Introduction
Diabetes is a significant health issue in the USA. It is the leading cause of kidney failure, lower-limb amputations, and adult-onset blindness, and is the seventh leading cause of death for adults1. The disease affected an estimated 34.1 million people in the USA in 2018, and grew in prevalence from 9.5% to 12% between 1999 and 20161. Diabetes prevalence is expected to increase an additional 54% by 2030, affecting more than 54.9 million Americans and resulting in more than US$622 billion in medical and societal costs2.
Type 2 diabetes accounts for the majority of the cases of diabetes, and is characterized by a decrease in insulin action with relative insulin insufficiency3. Risk for developing type 2 diabetes may go undiagnosed for years, and increases with age, as well as the modifiable lifestyle factors of obesity and lack of physical exercise4. As an increasing number of the US population are affected by diabetes, effective care approaches that address diabetes management at the population level are urgently needed5. Population-based diabetes care coordination by multidisciplinary teams improves quality of care, patient outcomes, and overall population health6,7. Effective diabetes care should include a range of providers across clinic and community settings that provide the self-management education and support required for adequate disease management8.
The Cooperative Extension System (CES) is a nationwide education network that provides research-based information and programs in nearly 3000 counties in the USA to improve the health and wellbeing of rural and urban communities. Chronic disease prevention and management is one of six priority program areas identified in the CES National Framework for Health published in 20149. As such, many state CESs are conducting lifestyle management programs for people with diabetes. Virginia Cooperative Extension (VCE) has developed the Balanced Living with Diabetes (BLD) program for this purpose.
Virginia’s diabetes prevalence was slightly higher than the national average in 2018 (9.5% v 9.1%)10. The impacts of diabetes on health in Virginia, as in the nation as a whole, are significant. In 2014, 27% of the hospitalizations for myocardial infarction, 46% for congestive heart failure, and 85% for lower extremity amputations in adults with diabetes were attributable to diabetes. Forty percent of cases of end-stage renal disease were diabetes related11. Virginians with diabetes were also more likely to report a physical, mental, or emotional disability11. Of significance, rural counties in Virginia have higher prevalence rates of diabetes compared with non-rural counties12.
According to Rural Healthy People 2020, diabetes is the third highest-ranking health priority in rural communities, following healthcare access, and nutrition and weight status13. In rural communities, diabetes is 8.6% more prevalent, and diabetes-related morbidity and mortality rates are higher compared to metropolitan areas14-17. Many factors are responsible for the higher diabetes prevalence and poorer health outcomes in rural communities. These include higher uninsured rates, decreased access to health care, lower economic and educational status, lack of transportation, and complex factors associated with increased overweight and obesity16,18-22. Importantly, 62% of rural communities lack diabetes self-management education programs, which are effective at improving diabetes management23.
To address the relative disparity in diabetes prevalence, outcomes, and access to self-management support, rural Virginia counties with high diabetes prevalence were targeted to provide community-based education in diabetes life style management through the VCE. Family and Consumer Sciences (FCS) extension educators serving these counties offered the BLD, an evidence-based lifestyle management program for people with type 2 diabetes, to community residents over 2 years. The goal of the project was to create sustained capacity for VCE to provide effective diabetes lifestyle management education in resource-limited rural communities. This article describes the BLD implementation process, including barriers and facilitators to implementation, and the impact of community context on adoption and maintenance. It also presents the BLD outcomes, including change in blood glucose control, self-management, and lifestyle behaviors. Evaluation outcomes are reported using the RE-AIM (Reach, Effectiveness, Adoption, Implementation, Maintenance) implementation framework and discuss the potential public health impact of the BLD conducted by CES24-26.
Methods
Rural counties in Virginia were targeted for dissemination of the BLD program between September 2015 and October 2017. All counties designated ‘non-metro’ according to the 2013 Rural–Urban Continuum Codes (RUCC) of the US Department of Agriculture Economic Research Service27, and that had an FCS extension educator, were selected for program dissemination. The Virginia Tech Institutional Review Board approved the implementation of the BLD through CES, and extension educators and BLD participants provided informed consent.
Description of the Balanced Living with Diabetes program
The BLD program is a group-based lifestyle intervention program for adults with type 2 diabetes. The BLD was developed by VCE through an iterative process of testing and modification in Virginia, and is conducted by extension educators in collaboration with community partners. The BLD is grounded in social cognitive theory and includes strong modeling and experiential components of healthy meal preparation and physical activity. It has shown efficacy to modify dietary and physical activity behaviors that result in improved glycemic control as measured by glycosylated hemoglobin (A1C). The BLD program consists of four consecutive weekly classes and a reunion class held 2 months after the last weekly class. The classes include an interactive presentation by a registered dietitian nutritionist or certified diabetes educator, a food demonstration by the FCS educator, and personal goal setting, sharing, and practice.
Training for family and consumer sciences extension educators
Counties that met the rural designation inclusion criteria and had an FCS educator providing community programming who could participate in the project were identified. FCS educators serving the counties that agreed to participate were trained on the BLD program. Participating educators received 8-hour, in-person training on the BLD program in October 2015. The training reviewed the types, etiology, prevention and control of diabetes, provided an overview of the BLD program components and theoretical underpinnings, and detailed the program conduct and key implementation components of each lesson.
Trained BLD educators were asked to conduct the BLD program in their county/counties twice during the project period (2015–17). Upon completion of the first BLD programs, feedback was solicited from the BLD educators through a group discussion to query their experience with the program, the systems for accessing program materials, the role of CES Master food volunteers, and recommendations for improving the program. Recommendations were incorporated into the program prior to the second BLD. An orientation to the updates to the BLD program was conducted in the second year.
Evaluation data
Process and outcome data were collected to evaluate the program. Process data included the number of targeted counties that participated in the BLD and characteristics of participating/non-participating counties; BLD training evaluation, BLD participant demographics and retention rates, type and number of community partners; implementation fidelity; and FCS educator semi-structured interviews at study conclusion to assess facilitators and barriers to BLD implementation and intentions for future programs.
Trained research personnel conducted participant assessments at baseline and 12 weeks to evaluate program outcomes. Assessments included anthropometrics (height and weight), A1C, and pre- and post-program questionnaires. The A1C test, also called hemoglobin A1C, can be used to diagnose type 2 diabetes and pre-diabetes, and is a primary test for diabetes management4. A1C measures the amount of glucose attached to hemoglobin in the red blood cells and was reported as a percentage. Higher blood glucose results in a greater amount of glucose bound to hemoglobin. Because the lifespan of red blood cells is 110–120 days on average, A1C provides information about glycemic control over the previous 3 months. This coincides with the length of the BLD program, providing sufficient time for lifestyle changes resulting in improved glycemic control to be reflected in the A1C. For purposes of analysis, an A1C less than 7 was considered a metric of appropriate glycemic control for participants with diabetes based on the recommendations of the American Diabetes Association in their Standards of Medical Care in Diabetes for non-pregnant adults without significant hypoglycemia4 The A1CNow+ system is used to test A1C, which generates results in 5 minutes using capillary whole blood from a finger stick. The system is certified by the National Glycohemoglobin Standardization Program, and is waived by the Clinical Laboratory Improvement Amendments due to its simplicity and low risk of an incorrect result.
Questionnaires consisted of 47 questions that gathered sociodemographic data and data on diabetes history, diabetes self-management (five questions), dietary knowledge (three questions), diabetes management (two questions), lifestyle behaviors (five questions on nutrition and physical activity) and diabetes lifestyle management self-efficacy (five questions). The questionnaire was adapted from the Foods Beliefs Survey, a valid and reliable tool for measuring nutrition behavior and physical activity using social cognitive theory constructs28-31.
Program evaluation
The potential public health impact of the BLD was evaluated using the RE-AIM framework24,25. This approach has been used to evaluate diabetes self-management interventions26. The components of the RE-AIM framework were applied as follows: Reach (program participation, participant demographics and retention), Efficacy (mean change in BLD outcome measures including glycemic control, knowledge, lifestyle behaviors and self-efficacy), Adoption (educator participation rate), Implementation (context, implementation fidelity, facilitators and barriers to implementation), and Maintenance (educator intentions for future programs, organizational support) was evaluated.
Descriptive statistics of the BLD participants in all programs were calculated and compared to the population statistics for the counties in which the programs were conducted. Statistical analysis was conducted using the Statistical Package for the Social Sciences v25 (IBM; https://www.ibm.com/products/spss-statistics). Paired t-tests were used to evaluate change in anthropometrics, glycemic control (A1C), diabetes self-management and dietary knowledge, diabetes management and lifestyle behaviors (nutrition and physical activity), and self-efficacy for participants that had both pre- and post-program data. Mean composite scores for diabetes self-management knowledge, dietary knowledge, and self-efficacy were calculated for this purpose, with higher scores representing higher levels of knowledge and self-efficacy.
Ethics approval
This study was approved by the Virginia Tech Institutional Review Board, VT IRB #150771.
Results
Fifty-three of the 134 counties and incorporated cities in Virginia were designated rural according to the 2013 RUCC codes. Of these, 18 counties/incorporated cities were served by an FCS extension educator with several counties served by a single educator. One educator served three counties, two educators served two counties and one educator served a rural county and an incorporated city. This resulted in 12 FCS extension educators eligible for participation in the project. All 12 educators agreed to conduct two BLD programs in the counties/incorporated cities they served during the project period. There were two exceptions. One educator served three counties, so was only able to commit to conducting the program in two of these. Another educator served a county and incorporated city contained within the county. This educator agreed to conduct a program within the city, but recruit for the program in the county as well.
All educators received training on the BLD program at the beginning of the project. Results from satisfaction surveys completed by the educators after the BLD training showed that all 12 attendees were satisfied with the training, felt it provided the information and materials needed, and were confident in their knowledge and capacity to conduct the program.
Process outcomes
Extension educators conducted 30 BLD programs during the project period, with a total of 291 participants. Of these participants, 169 self-reported that they had diabetes, 48 self-reported pre-diabetes, 44 reported neither, and 30 people did not report their diabetic status. Programs had an average of nine participants (range: 3–19) with an average age of 63 years (21–90 years). The average retention rate, as defined as participants returning for the final reunion session, was 58% (range: 13–100%). Compared to the combined demographic characteristics of the participating counties, there was a higher proportion of women and people with college degrees in the BLD programs. The racial make-up of BLD participants was also different from the county demographics, with fewer white participants, and a greater proportion of black participants in the program. The one eligible county that did not conduct a program (non-participating county) had a population that was predominantly white, a lower percentage of college graduates, and lower median income (Table 1). The BLD program was conducted in 16 counties during the first half of the project.
Five counties did not conduct a second program. Reasons for not conducting a second program varied, as did the location and demographics of these counties. Two counties were unable to provide a second program due to loss of the FCS extension educator position. These counties were in far Southwest Virginia, had a population that was predominantly white (94% and 99%), and had the lowest median household incomes (US$26,204 and US$28,296) of all of the counties. The ratio of staffing to population was lower or equal to the mean of all counties (all-counties mean ratio=0.03; county ratios=0.02 and 0.03). One county did not have enough interest from community members despite broad advertising to conduct a second program. This county was in Central Virginia, had a median income (US$40,776) slightly higher than the average of all the counties (mean=US$39,885), and a diverse population with 56% white and 50% African-American. The ratio of staffing to population was similar to that in other counties (0.03).
The final two counties were served by the same extension educator, who did not conduct a second BLD program due to a decision to prioritize her time in a different area. These counties had relatively higher median incomes (US$43,435 and US$47,364), had a predominantly white population (95% and 96%), and a staff-to-population ratio equal to or higher than the mean of the counties (0.03 and 0.05). In contrast to this, three of the original counties had substantial interest in the program and chose to conduct the BLD three times, and an educator from an additional rural county not included in the original project requested to be trained on the BLD and implemented the program twice in the second half of the project.
Table 1: Sociodemographic characteristics of participants in the Balanced Living with Diabetes programs with combined characteristics of the 16 participating counties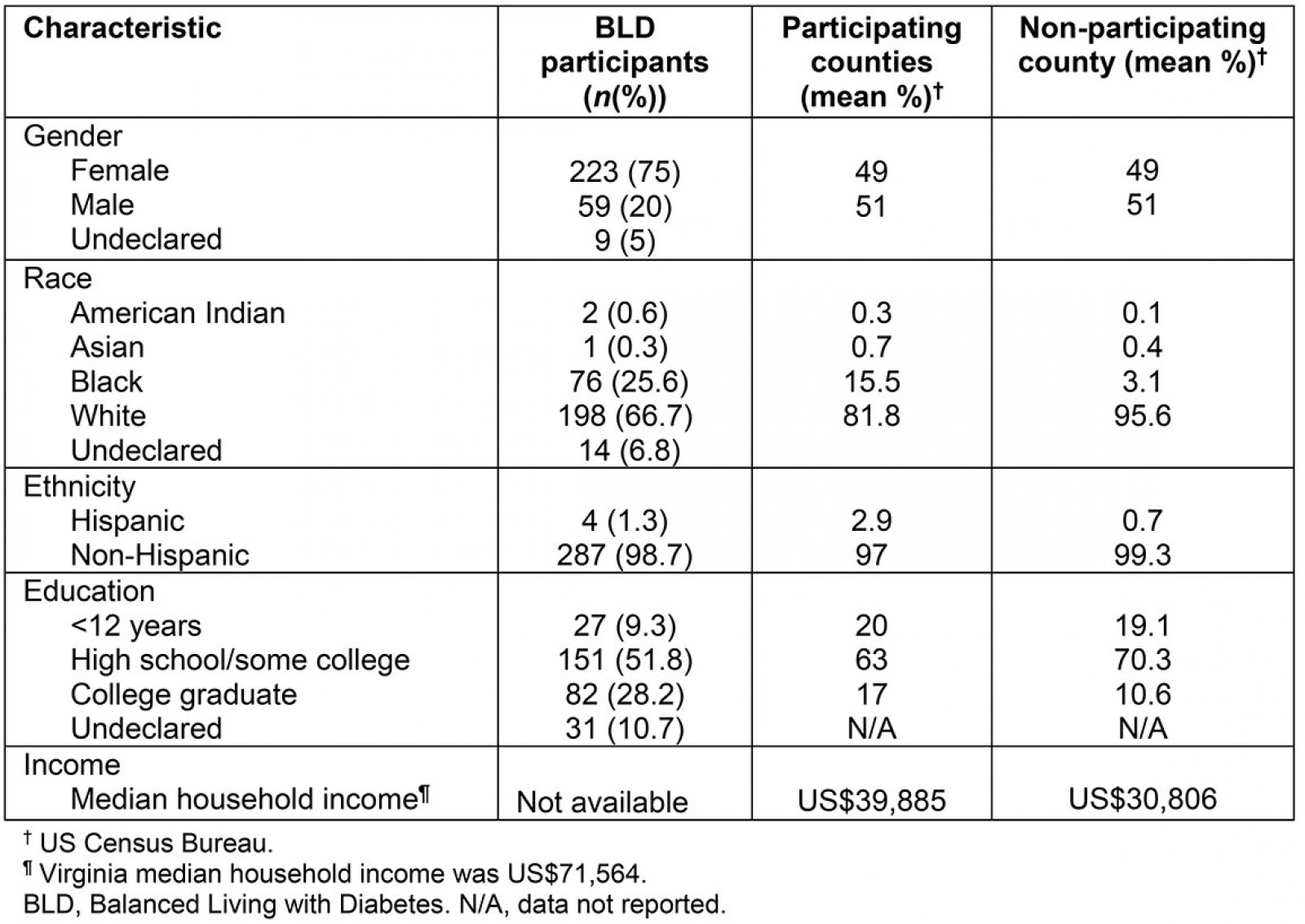
Discussion group and educator interview findings
Principal findings from the discussion conducted with educators after completion of their first BLD program were that there was a need for recruitment materials for the program, and for communication materials for ongoing contact and reinforcement of key messages with participants. Two educators who had difficulty recruiting participants indicated that commonly used recruitment methods for extension programs were less successful for this disease-specific program. Educators found relative success by advertising through faith-based organizations, and two identified senior nutrition sites as a good site for recruitment. In addition, to maintain participant engagement, educators highlighted a need for communication with program participants in the 8-week period before the reunion session. In response to these comments, the research team created marketing materials for print and multimedia use. The materials were created with input from the BLD educators. A draft of the marketing material was created (flier and social media post) and distributed to the BLD educators. Input from the BLD educators was incorporated in the final material. BLD educators were able to adapt the materials to their target audience. In addition, the team developed an 8-week communication plan with concomitant communication disease-specific materials that could be distributed weekly to participants via email or postal service.
During the discussion, all but one of the educators indicated that they used extension volunteers called master food volunteers to assist in the food demonstration component of the program sessions. A web-based continuing education module was developed in the first year of the project to train master food volunteers planning to assist educators with food demonstrations for the BLD program. The training module is web-based with audio-recorded lessons and post-lesson self-assessments. The process of its development is described elsewhere32. There was unanimous agreement among the educators that master food volunteers were very helpful to the sustained conduct of the BLD program. They assisted primarily with the food demonstrations associated with each lesson. When asked about the utility of the food demonstrations as part of the BLD program, all educators felt participants enjoyed and were interested in the information presented through the food demonstrations. One educator commented that some of the recipes did not lend themselves to effective demonstration. In response to this, the research team gave educators the option to go beyond the recipes that are part of the BLD program materials and use recipes from a diabetes cookbook given to participants at the final reunion lesson33.
Semi-structured interviews were conducted with extension educators after completion of the second BLD program at the conclusion of the project. Nine of the 12 extension educators who participated in the project provided feedback through these interviews. Two educators were no longer employed with VCE, and one educator declined to be interviewed despite repeated solicitations. The themes and recommendations resulting from the extension educator interviews fit into two categories.
Program facilitators:
- The program requirement of having a registered dietitian nutritionist or certified diabetes educator provide the diabetes and health-related information as part of the program was helpful. In general, FCS extension educators did not have a clinical background, and did not feel qualified to provide medical-related instruction.
- Master food volunteers were very useful. They conducted food preparation for the food demonstrations, and some conducted the food demonstration and related food preparation and safety information to the participants. This allowed educators to dedicate their time to facilitate the lessons and manage program logistics.
- The food demonstrations were engaging and promoted active learning. Educators indicated that choosing recipes culturally acceptable to the audience was important.
Barriers to program sustainability:
- Finding a registered dietitian nutritionist or certified diabetes educator to co-facilitate the program was the most difficult task. Developing systems for consistent access to these professionals was identified as important to program sustainability.
- Cost of the program is relatively high for the target audience of extension educators. Sustainable funding for program materials to ensure program access to all was identified as an important issue.
- Broader awareness of the program being offered by VCE would help support sustained program attendance. There is a need for effective marketing systems that reach individuals most in need of the program. A system for referral of patients from healthcare providers to the program was identified as a need.
All educators were able to engage a variety of local collaborators to support the program, and had ideas for additional collaborations. Collaborating organizations included local hospital systems (six counties), local departments of health (two counties), local Area Agencies on Aging (two counties), a dietetic internship program, a local grocery store chain, the YMCA, a religious organization, community college, and public library (one county each).
Three models of collaboration to increase program sustainability showed promise. The first was a collaboration with a state university dietetic internship program that provided dietetic interns as co-facilitators for the BLD. This provided a rich experience for the interns in community nutrition education, and a consistent source of qualified educators for the BLD in two underserved communities. The second was a formal relationship between VCE, a healthcare system, and a local Area Agency on Aging to provide the BLD program in their senior nutrition sites. The Area Agency on Aging provided funding to cover the material costs of the program, the healthcare system provided a certified diabetes educator as co-facilitator, and VCE provided the program to their clients with diabetes. The third model was a collaboration between a local hospital rehabilitation center and VCE for the conduct of the BLD program in their center. The hospital system provided the certified diabetes educator, location, and patient referrals to the program, and the VCE educator conducted the program.
Program outcomes
A total of 169 program participants had both pre-program and post-program data, and were included in the outcome analysis. One-hundred had diabetes, 47 had pre-diabetes, and 22 were caregivers or family of a person with diabetes. The program resulted in significant improvements in glycemic control, diabetes self-management and healthy lifestyle behaviors, and self-efficacy. The greatest improvement of glycemic control was seen in those with poorer control at the beginning of the program.
Twenty-two percent (n=14) of participants with poorly controlled diabetes (defined as A1C≥7.0) reduced their A1C into the clinical goal range of <7.0. There was a significant reduction in A1C for all participants with diabetes determined by having a baseline A1C of 6.5 or greater (mean reduction=0.345±1.013; p=0.001). Greater reduction in A1C was seen in participants with a baseline A1C≥7.0 (mean reduction=0.384±1.182; p=0.014). Twenty-three percent (n=11) of participants with pre-diabetes, determined by having a baseline A1C between 5.7 and 6.4, reduced their A1C into the normal range of <5.7. Of significance, 14% (n=21) of participants with either diabetes or pre-diabetes had a clinically significant reduction in their A1C (reduction of ≥1.0). Although the BLD program is not specifically designed to result in weight loss, this is often an outcome of the change in diet and physical activity recommended in the program. Sixty-one percent (n=103) of the BLD participants providing follow-up data lost weight, with an average weight loss of 2.71% of body weight (5.4±6.3; range=900 g–20 kg) (Table 2).
Table 2: Program outcomes: change in A1C and weight in Balanced Living with Diabetes participants†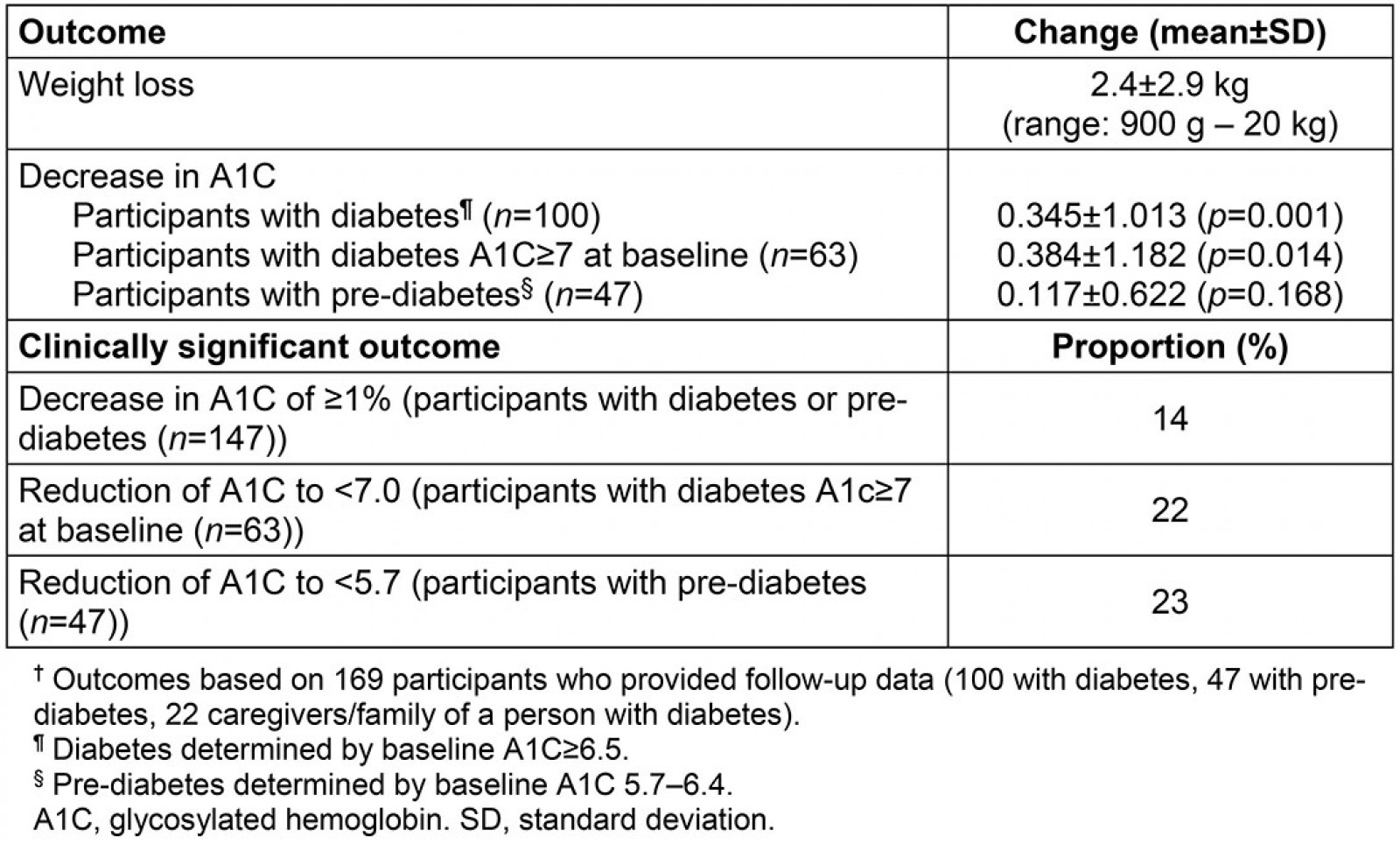
Changes in health behaviors, knowledge, and self-efficacy: Significant improvements occurred in diet and physical activity behaviors, including an increase in the daily portions of fruits and vegetables and whole grains, use of the plate method as a tool for diet management34, and days a week of at least 30 minutes of physical activity (Table 3). Diabetes self-management knowledge and behaviors also improved significantly, as did dietary knowledge. Importantly, participants reported a significant increase in self-efficacy to implement the diabetes self-management recommendations made during the program (Table 3).
Table 3: Program outcomes: change in behavior, knowledge, and self-efficacy of participants in the Balanced Living with Diabetes program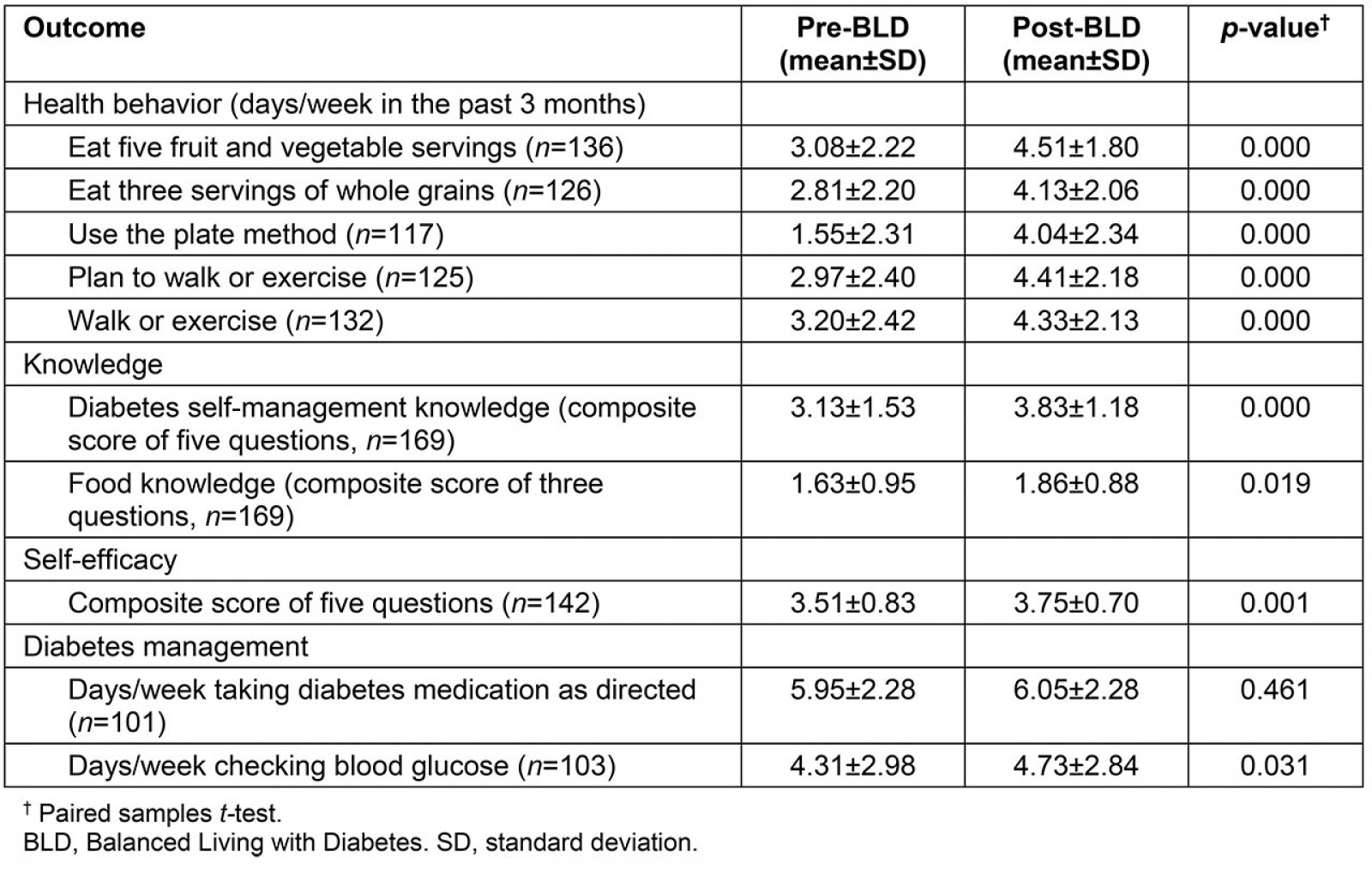
Discussion
The high prevalence of type 2 diabetes and the looming expansion of the proportion of the US population who will develop the disease requires a multi-sector response. As an increasing number of the US population are affected by diabetes, effective healthcare approaches that address diabetes management at the population level are urgently needed5. Population-based diabetes care coordination by multidisciplinary care teams improves quality of care, patient outcomes, and overall population health; however, this model has rarely been tested with community service providers as part of the care team6,7. Effective diabetes care teams should include a range of providers across clinic and community settings that provide the diabetes self-management education and support required for adequate disease management8.
The CES is a nationwide network of community education providers that has chronic disease prevention and management as a priority program area. The goal of the project reported here was to harness the educational resources of VCE to provide effective, sustained lifestyle management education to people with type 2 diabetes in resource limited-rural communities. The process and outcome evaluation of the implementation of the BLD program by Virginia extension educators resulted in the development of supporting materials and systems important to program sustainability and effectiveness, identified three models of collaboration for program sustainability, and indicated that the program is highly acceptable and effective at improving diabetes self-management by program participants.
The individuals reached through the BLD programs were over-represented in minority groups and women, and under-represented by men and those at the lowest education levels. Additionally, participants were not exclusively people with diabetes, but included those with pre-diabetes, family members of people with diabetes, and persons with a family history of the disease who hoped to reduce their risk. This is partially due to the normal recruitment policies and practices of VCE that distribute recruitment materials to the public and do not exclude anyone from programs and resources offered in community. To focus recruitment to reach the people most at need for the program, recruitment materials with targeted messages were developed, and key locations and methods for distribution in areas with high diabetes prevalence and risk were identified (Area Agencies on Aging, healthcare facilities). Furthermore, efforts to establish direct referral systems from healthcare providers to the BLD programs are under way.
The program is effective at improving glycemic control and changing lifestyle behaviors. Over a quarter of attendees with diabetes who returned for the reunion session had a significant improvement in their glycemic control. This is as a result of the changes in diet, physical activity, and self-management behaviors in BLD participants. Because the BLD program is a group-based diabetes lifestyle management program offered in community to the general public, a target A1C of less than 7.0 was used as the metric for adequate glycemic control. This is based on the recommendations of the ADA Standards of Medical Care in Diabetes4.
The American Diabetes Association standards encourage a patient-centered approach to setting treatment goals and intensity of glycemic control based on several factors including risks associated with hypoglycemia, disease duration, life expectancy, established vascular complications and comorbidities, and patient preference, among others4. Better glycemic control is associated with reduced rates of development and progression of microvascular complications in both type 1 and type 2 diabetes, and landmark trials have been conducted to test the effects of near normalization of blood glucose on cardiovascular outcomes in individuals with long-standing type 2 diabetes and cardiovascular disease35-40. The intense efforts required to achieve the more stringent glycemic goals, and findings of increased mortality in the Action to Control Cardiovascular Risk in Diabetes (ACCORD) trial, have warranted caution in applying the stricter glycemic goals4.
Beyond these tangible outcomes, anecdotal evidence in the form of participant testimonials show that people enjoy the program and would like to have ongoing supportive sessions. Extension educators also expressed personal satisfaction from the impact the program had on participants behavior and health. This has driven adoption and maintenance of the program by VCE educators. Of the nine educators that conducted two BLD programs during the project, seven continue to conduct the program. The two educators who are not conducting the program are no longer working with VCE in those counties. In addition, four educators that were not involved in the original project requested training, and are now conducting the program in their counties. The slow process for replacing FCS extension educators who leave the service poses a challenge to health program sustainability within VCE.
Significant barriers to program maintenance included the difficulty in having regular access to a registered dietitian nutritionist or certified diabetes educator as co-facilitator, covering program costs, and recruitment of priority populations for participation. Three collaborations formed by extension educators in the conduct of the BLD program that show promise in addressing these difficulties were described:
- Linking the BLD with a local dietetic internship program ensured availability of a dietetic intern to co-facilitate the program and was mutually beneficial to both programs. The model is being expanded to other areas where dietetic internship programs exist.
- In order to ensure equitable access to VCE programs, these are offered either free of charge or at a nominal cost. Because Area Agencies on Aging have a responsibility to provide evidence-based chronic disease education to their patrons and have a funding stream for this, combining the resources of the two organizations to address their aligned goals enhances the effectiveness and sustainability of each. Conducting programs at Area Agencies on Aging is also an effective way of accessing older adults, who have a higher prevalence of diabetes and may lack transportation or other resources required for participation in other existing community or hospital-based programs. Engaging the local healthcare provider in the education provided by the Area Agencies on Aging and VCE collaborative affords the additional opportunity to link participants to a primary care provider if they do not already have one.
- Conducting the BLD program in a community wellness center that is used as a resource by local physicians and patients is a model for increasing program awareness, accessibility, and patient referrals by physicians.
Linking the needs of patients in the healthcare setting with community education and support resources is an important component of comprehensive care models, like the Chronic Care Model and the Expanded Care Model5,41,42. These models use a systematic approach to restructuring medical care to create partnerships between health systems and communities. The Expanded Care Model includes elements of population health promotion that emphasize prevention, social determinants of health, and enhanced community participation. Although there are examples of community-level partnerships pooling human and fiscal resources to provide diabetes management services43-46, there is a need for more information about the community resources component of these models47.
The present study was limited in scale, lacking a sufficiently large sample size to draw robust statistical conclusions about the impact of the BLD program. Having said that, a significant mean reduction in A1C was demonstrated, particularly among those with poor glycemic control at the beginning of the program. In addition, significant changes in self-reported health behaviors, diabetes knowledge, and self-efficacy in the self-management of diabetes were demonstrated. Future research should be conducted with a larger sample size, and validation of the modified diabetes behavior, knowledge, and self-efficacy survey.
The CES is a national network of community educators in the USA well positioned to serve as an effective partner for the provision of chronic disease education in general, and diabetes education and lifestyle management specifically. Public–private partnerships between providers and community organizations are needed to address barriers to diabetes care and to provide culturally appropriate community-based services (eg lifestyle self-management classes, cooking classes and exercise programs) particularly for underserved populations and communities47. This study demonstrated that CES can effectively implement an evidence-based diabetes lifestyle-management program, the BLD, in underserved communities through collaboration with a variety of community partners. Included among the partners were those providing healthcare and social service support to the most vulnerable. Future research will focus on implementation strategies to enhance the BLD program retention and effectiveness, efficacy of care coordination models and systems between the CES and healthcare partners, and the effectiveness of these models at improving diabetes self-management practices and health outcomes.
Conclusion
Healthcare organizations and diabetes care specialists serving under-resourced rural communities should seek to create partnerships with community-based organizations as part of their comprehensive care model for their patients with diabetes. National organizations providing public health education, such as CES, are available in almost every community and are natural partners for this purpose. These organizations have the local presence, networks, and cultural understanding to provide ongoing support for patients with diabetes. Combining the knowledge and resources of healthcare and community organizations through effective systems will improve diabetes management and outcomes.
Acknowledgements
We thank the extension educators who conducted the Balanced Living with Diabetes program in their service communities and provided valuable information about the implementation of the programs. The study was conducted through funding from the National Institute of Food and Agriculture/USDA (#2015-46100-24197).
References
You might also be interested in:
2006 - Comparison of stroke among Christians and Muslims in Thrace, Greece





