Introduction
Healthcare providers in rural areas face challenges in providing coherent and integrated services. A growing political trend in planning health services for rural and remote populations, is to take rurality into account in order to ensure greater equity in health services and health outcomes1,2. Rural health research is flourishing, especially in the United Kingdom, Australia and North America, but findings from these areas may not be transferable to the geography and demography of other regions or continents, such as Africa or Asia.
A special challenge in rural areas is that the proportion of older people often is higher than that of the general population. As a consequence, rural health practitioners often have to deal with older patients with multiple and chronic diseases. In addition, unfavourable health outcomes have been linked to rural populations, such as higher asthma mortality rates and a more advanced stage at diagnosis of some cancers3-6.
We conducted a literature study to explore evidence on how to promote continuity and integration in healthcare services in order to meet the special demands of populations in rural areas. Concepts and terms commonly used in the literature related to these issues are presented. Policy documents and strategies from northern European regions are also presented in some detail.
Rurality
There is a lack of internationally agreed-upon definitions of what rurality entails, how it is measured and how it is used in research and healthcare policy and planning. Researchers usually employ their own definition according to the study area of interest. This makes it difficult to interpret and compare study results internationally and to establish an evidence base for these issues1,2,7.
According to the Organisation for Economic Co-operation and Development (OECD), the definition of rurality is fewer than 150 persons per km27. In the UK, authorities have recently developed a methodology to define rural and urban areas which is now being used as a national statistic8. Another initiative to describe and delineate rurality is the 'Clinical peripherality index' from Scotland's health service9. This index reflects characteristics of rural and remote general practices and the communities they serve, including their access to secondary care facilities, to centres of decision- making and to professional education and support.
In this study our understanding of rurality relating to health care entails some or all of the following elements: isolated and dispersed communities, low density populations, limited public transport and road infrastructure, long distances to hospitals and health care services, and the difficulties in attracting and recruiting qualified personnel.
Method and Results
Search strategy
Electronic database searches were performed in Pubmed, MEDLINE and EMBASE using controlled vocabulary and text words. Definitions of search terms are presented (Table 1). The first search was in PubMed for the period 1995-2005, resulting in 214 hits. The abstracts were reviewed, and 21 were selected. Then searches for systematic reviews were made in MEDLINE for the period 1966-2005 and in EMBASE for the period 1980-2005, resulting in 507 hits in total, of which 18 were selected. Supplementary searches of MEDLINE and EMBASE for the period 2005-October 2006 resulted in the selection of 10 of 139 articles. In addition, some studies were identified from desktop searches and some from reference lists. Only one Cochrane systematic review was found10. The selection of articles was based on the authors' estimate of what was relevant to providing continuous and integrated services in rural areas from review of the abstracts, and articles published in recent years.
National public health strategies and policy documents relating to the needs for more integrated and decentralised health services in rural areas from some northern European countries were also identified.
Table 1: Definitions of MeSH search terms
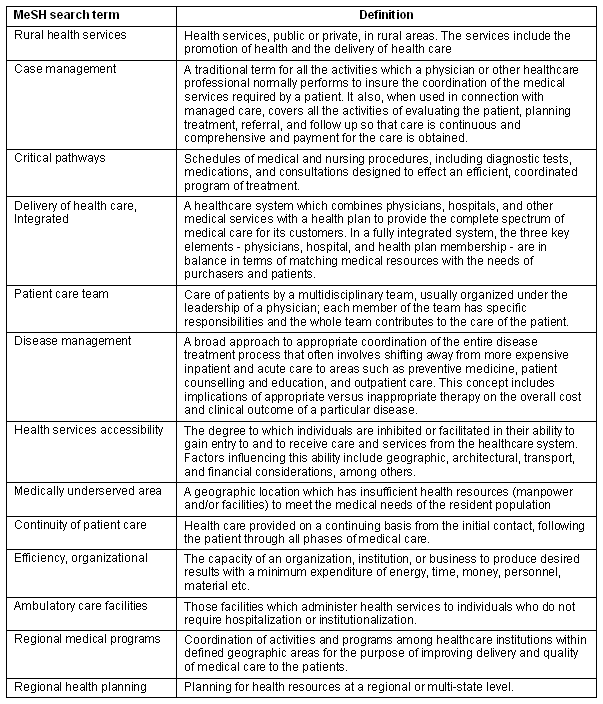
Data analysis
On the basis of the collected literature, using an editing analysis style11, we identified units in the material that were indicators of organisational forms and programs that would lead to more continuous and integrated services, such as access to services, delegation, cooperation and teamwork. Some of these were specific to rural areas, but some were not. From these units we synthesised five common themes:
- Trends in public health strategies and policy documents.
- Delegation and substitution of tasks, team-based working, flexibility of roles and cultural adjustments.
- Integrated care programs and managed care.
- Intermediate care, shared care and specialist outreach.
- Telemedicine.
Trends in public health strategies and policy documents
Health policy documents in many countries focus on the need for integrated, continuous and decentralised health services, but many fail to take into account the special context of rurality. According to the Board of Science of the British Medical Association, rurality will increasingly be recognised as an issue worthy of its own health policies2. Their report Health care in a Rural Setting2 is a policy update on rurality, healthcare delivery to local areas, acute and emergency services, local provision of facilities for disabled people, interprofessional work and education, and expert patient programs.
Another report from the UK, Keeping the NHS local - A New Direction of Travel, outlines modernisation strategies for models of care 'closer to home' that suit the demands of populations in rural areas1. The goal is to work with local communities and staff to rebuild local services around local needs. The service modernisation proposed includes new and extended roles for doctors, nurses and other clinical staff, a shift towards team-based work, an appropriate balance in care from generalists and specialists, networking between hospitals, and using telemedicine.
The report from NHS Scotland9 states:
The Scottish Executive's report (2002) on the availability of services in rural Scotland identified poor access to public services as one of the main causes of social exclusion for rural areas. The loss of local health services can have a significant knock-on effect to the sustainability of fragile local communities and recruitment and retention of healthcare professionals in remote and rural areas presents particular challenges.
A report from northern Norway on the rural dimensions in decentralisation of health services recommends the use of outreach/ambulatory services, community hospitals, enhanced use of telemedicine solutions and better counselling and guidance from specialists to primary care workers12.
A key impression gained from our review is that there is a growing emphasis on the rural dimensions in health planning, calling for a shift of services from secondary care to community-based care, and from community-based to home-based care or self-management programs.
Delegation and substitution of tasks, team-based work, flexibility of roles and cultural adjustments
Greater flexibility in traditional professional roles and responsibilities, such as nurse practitioners or community pharmacists managing common conditions, is proposed in order to alleviate a scarcity of personnel and resources13. Empowering primary-care practitioners by training and education combined with support and supervision is described in studies dealing with diabetes and mental health14,15. Other examples include generalist providers, particularly community and home-care nurses, playing a greater role in the delivery of primary palliative care16,17. Primary-care professionals may also substitute for secondary care in hospitals' acute and emergency departments18.
Substitution of health personnel with lay health workers or paraprofessionals, often in combination with interdisciplinary teams, is among measures proposed to alleviate staff shortage and to overcome cultural barriers19. The Kansas Health Education Training Center describes the role of the 'community health worker' as 'partners for health'20: 'Working in health promotion and self-management programs they assist in bridging culture, language and patterns of health behaviour in underserved populations.' While the working conditions in remote areas are characterised by: 'Geographical, professional and, often, social isolation of practitioners; a strong multidisciplinary approach; overlapping and changing roles of team members; a high degree of general practitioner substitution; and practitioners requiring public health, emergency and extended clinical skills'21.
The literature reveals that working in remote and rural areas calls for flexibility of roles and responsibilities, delegation of tasks, and cultural adjustments by the healthcare practitioners.
Integrated care programs and managed care
Integrated care implies coordinated programs in all phases of medical care. An integrated care pathway (ICP) is an outline of planned care for a specific patient group. Much of the focus on patient pathways has been related to clinical pathways in hospital settings, or to the gate-keeping and case-management mechanisms used by managed care organisations. But a broader approach is emerging, where ICP are multiprofessional documents designed to embed locally accepted, evidence-based, patient-centred guidelines in everyday use for the individual patient22,23. A design for implementing integrated pathways into rural health services implied identifying patient pathways for patient groups and the planning of multidisciplinary, comprehensive care on a timescale, not only for those needing isolated episodes of care, but also for chronically ill patients24.
An analysis of systematic reviews carried out in the Netherlands evaluating the effectiveness, definitions, and components of integrated care programs for chronically ill patients25 found that:
The most common components were self-management support and patient education, often combined with structured clinical follow up and case management; a multidisciplinary patient care team, multidisciplinary clinical pathways and feedback, reminders and education for professionals.
Such integrated care programs appeared to have positive effects on the quality of care.
Both integrated patient care and managed care are intended to improve access, continuity and coordination of care. But managed care also takes into account payment and economic elements, and the cost-effectiveness of care. One definition of managed care26 is:
Any system that manages healthcare delivery with the aim of controlling costs. Managed care systems typically rely on a primary care physician who acts as a gatekeeper through whom the patient has to go to obtain other health services such as specialty medical care, surgery, or physical therapy.
It is proposed that rural case management depends on a locally based case manager, rather than a regular case manager who travels to rural areas from an urban centre27. This is illustrated in a US study describing the nurse's role as case manager in rural settings28. The highest ranked essential skills for rural case managers were identified as: the ability to be creative in the coordination of resources, multidimensional nursing skills, excellent communication skills, high-calibre computer skills and excellent driving skills. The authors28 found the emphasis on technology and telemedicine somewhat surprising and offered the following conclusion:
Case management in a rural environment requires a much broader and generalist knowledge base, it covers all levels of prevention and traverses all age groups. Rural case management is a distinct specialty area of practice, with a distinct knowledge base and skill level, and nurses should be prepared at the advanced practice level.
Our review revealed that planned care programs such as integrated care and managed care must be adjusted to the context of rural areas, and that they also require of rural health professionals special knowledge and skills.
Intermediate care, shared care and specialist outreach
Many of the initiatives to improve health services in rural and remote areas are attempts to better the interaction and communication between primary and specialist levels. The Rural Access Action Team of Scotland offers the following definitions9:
- Intermediate care describes the expansion of primary health care and social care services to bridge the interface with secondary care.
- The rural general hospital is a locally based, consultant-led service that provides emergency medical care such as triage, resuscitation and stabilisation. It also provides locally based elective care, diagnosis, treatment or transfer. It handles care for the elderly and for those with chronic illness such as stroke and diabetes, and support for renal dialysis patients.
- The community hospital varies as to what services are provided, but usually has a core of GP inpatient beds, while some have consultant long-stay beds, primary care nurse beds or delivery beds run by midwives. Community hospitals may also play a role in palliative care, outpatient functions including day case surgery, specialist clinics and in telemedicine including teleradiology.
In Norway, community hospital functions are often placed in small units with 2-3 beds within a nursing home. Others are part of district medical centres, combining primary health care and specialist outreach services. A recent political trend in Norway is to strengthen such services, mostly in rural areas29,30.
In Scandinavia, GPs are often engaged as advisors to the hospital staff, acting as facilitators of cooperation between generalists and hospitals. They participate in the development of clinical guidelines for shared care and also conduct multidisciplinary patient pathway analyses in order to identify areas of quality improvement31. A patient pathway may be defined as the route that a patient will take from their first contact with their GP, through referral, to the completion of treatment. It also covers the period from hospital admission to discharge. It may, thus, be illustrated on a timeline, on which every event relating to treatment can be entered32.
The formal liaisons between GPs and specialist teams were evaluated in a systematic review33. Patient retention rates within treatment programs improved with GP involvement, as did patient satisfaction. With such cooperation, the behaviour of both GPs and specialists changed. More rational use of diagnostic tests, improved clinical skills, increased use of appropriate treatment strategies, and more frequent clinical behaviours designed to detect disease complications were reported. Cost-effectiveness could not be determined.
In a literature review of shared care at the primary-secondary interface, one of the most fundamental aspects identified was the need for improved data transfer relating to discharge planning, shared prescribing and shared management of disease34. Although information technology may provide solutions to this, it was concluded that a culture change compelling health professionals to share patient information in a more timely and efficient way should be given higher priority.
Specialist outreach clinics in primary care and rural hospitals were studied in a 2004 Cochrane systematic review, providing an assessment of effectiveness in terms of access, quality, health outcomes, patient satisfaction, use of services and costs10. Most comparative studies came from urban non-disadvantaged populations in developed countries. Specialist outreach as part of more complex multifaceted interventions involving collaboration with primary care, education or other services was associated with improved health outcomes, more efficient and guideline-consistent care, and less use of inpatient services. The additional costs of implementing outreach may be offset by improved health outcomes. The benefits of simple outreach models in urban non-disadvantaged settings, however, appeared to be small10.
A study from Australia's northern Aboriginal communities evaluated a specialist outreach service, confirming the findings of the Cochrane study in that specialist outreach is dependent on a well-functioning primary healthcare system35. It also states that 'according to the way in which outreach is conducted and the service is organised, it can either support primary care or it can hinder primary care and, as a result, reduce its own effectiveness.'
Our study found evidence that collaboration at the interface between primary and secondary sectors may improve access, continuity of care and the quality of service delivery in rural areas. These measures are dependent on a well-functioning primary healthcare system as a base.
Telemedicine
Telemedicine may be defined as 'Medicine practiced at a distance. It therefore encompasses diagnosis, treatment and medical education'36. The benefits of telemedicine involve the facilitation of access to health services and medical information regardless of time and place. In this context, there is abundant literature on applications in rural settings; however, there is a lack of evidence supporting its clinical and cost advantages relative to traditional services37.
One report of well-functioning telemedicine services comes from the state of Maine, USA, where there has been rapid a growth in state-wide telemedicine systems in rural, economically disadvantaged areas38. Here telemedicine is used in a broad array of interactive videoconferencing applications, including mental health and psychiatry, diabetes management, primary care, paediatrics, genetics, and dermatology. An article from Tennessee, USA, describes an integrated telehealth network linking three hospitals, a healthcare clinic and patient homes39. Outcomes from the disease management program for diabetes showed an increase in the number of diabetic patients who had managed to control their blood glucose levels. In Scotland, remote nurse practitioners in a community hospital staffed accident and emergency services, supported by telemedicine advice from a regional hospital by videoconference and a document camera which allowed transmission of still images of wounds and radiographs40. Both professionals and patients reported high levels of acceptance and satisfaction.
It is also reported that telemedicine may contribute to acceptable services in palliative care and cancer treatment programs in remote and rural areas41. The use of telemedicine to facilitate thrombolytic therapy for patients with acute stroke, by providing stroke consultative services to remote-site hospitals, has also been shown to be reliable42,43. There is good evidence that systemic thrombolysis can be employed in remote sites with telemedical consultation44.
This review found that telemedicine can be a valuable tool in achieving access to healthcare services in remote and rural areas, but that documentation of its cost-effectiveness has been limited.
Conclusion
The findings of this literature review indicate that continuous and integrated healthcare services may be achieved in rural areas by decentralisation of services, delegation and substitution of tasks, interdisciplinary and team-based working, flexibility of roles, and cultural adjustments. In addition, it was found that programs such as integrated and managed care pathways, outreach programs and shared care were relevant measures. Telemedicine may also be a useful tool to achieve access to services in remote areas. Most of the literature comes from industrialised countries in Europe, USA, Canada and Australia; much of it reflects a lack of evidence and indicates the need for future research. There is also a need for further studies on the relevance and validity of these findings in other regions, such as in the southern hemisphere.
References
1. UK Department of Health. Keeping the NHS local - A new direction of travel. (Online) 2003. Available: http://www.dh.gov.uk/PublicationsAndStatistics/Publications/PublicationsPolicyAndGuidance/PublicationsPolicyAndGuidanceArticle/fs/en?CONTENT_ID=4010316&chk=H%2BFDrS (Accessed 3 March 2007).
2. British Medical Association; Board of Science. Healthcare in a rural setting. (Online) 2005. Available: http://www.bma.org.uk/ap.nsf/AttachmentsByTitle/PDFrural/$FILE/rural.pdf (Accessed 3 March 2007).
3. European Rural and Isolated Practitioners Association, EURIPA. A collaborative analysis of public health and health service issues in rural areas. (Online) 1999. Available: http://www.euripa.org/research.htm (Accessed 3 March 2007).
4. Campbell N, Elliot A, Sharp L, Ritchie L, Cassidy J, Little J. Rural and urban differences in stage at diagnosis of colorectal and lung cancers. British Journal of Cancer2001; 847: 910-914.
5. Jones A, Bentham G, Horwell C. Health service accessibility and deaths from asthma. International Journal of Epidemiology 1999; 28: 101-105.
6. Ryan-Nicholls KD, Racher FE. Investigating the health of rural communities: toward a framework development. Rural and Remote Health 4: 244. (Online) 2004. Available: www.rrh.org.au (Accessed 13 November 2006).
7. Public Health Agency of Canada. Definitions of 'rural' summary. (Online) 2002. Available: http://www.phac-aspc.gc.ca/rh-sr/paper_e.html (Accessed 3 March 2007).
8. UK Online National Statistics. Rural and Urban Area Classification 2004 (Online) 2004. Available: http://www.statistics.gov.uk/geography/nrudp.asp (Accessed 3 March 2007).
9. Scottish Executive Health Department. A National framework for service change in the NHS in Scotland. (Online) no date. Available: http://www.sehd.scot.nhs.uk/nationalframework/Reports.htm (Accessed 3 March 2007).
10. Gruen RL, Weeramanthri TS, Knight SE, Bailie RS. Specialist outreach clinics in primary care and rural hospital settings. Cochrane Database of Systematic Reviews 2004; (1):CD003798. DOI: 10.1002/14651858.CD003798.pub2
11. Malterud K. Qualitative research, standards, challenges, and guidelines. The Lancet 2001; 358: 483-487.
12. Desentralisering av spesialisthelsetjenester i Helse Nord. Rapport fra prosjektgruppe oppnevnt av Helse Nord RHF. (Online) 2005. Available: http://www.helsenord.no/category5929.html (Accessed 3 March 2007).
13. Chapman JL, Zechel A, Carter YH, Abbott S. Systematic review of recent innovations in service provision to improve access to primary care. British Journal of General Practice 2004; 54: 374-381.
14. Maddigan SL, Majumdar SR, Guirguis LM, Lewanczuk RZ, Lee TK, Toth EL et al. Improvements in patient-reported outcomes associated with an intervention to enhance quality of care for rural patients with type 2 diabetes: results of a controlled trial. Diabetes Care 2004; 27: 1306-1312.
15. Donoghue A, Hodgins G, Judd F, Scopelliti J, Grigg M, Komiti A et al. Training case managers to deliver focused psychological strategies. International Journal of Mental Health Nursing 2004; 13: 33-38.
16. Phillips JL, Davidson PM, Jackson D, Kristjanson L, Bennett ML. Enhancing palliative care delivery in a regional community in Australia. Australian Health Review 2006; 30: 370-379.
17. Kelley ML, Habjan S, Aegard J. Building capacity to provide palliative care in rural and remote communities: Does education make a difference? Journal of Palliative Care 2004; 20: 308-315.
18. Roberts E, Mays N. Can primary care and community-based models of emergency care substitute for the hospital accident and emergency (A & E) department? Health Policy 1998; 44: 191-214.
19. Breedlove G, Lamping B, Smith JA. The Kansas Health Education Training Center: caring for the underserved. Kansas Nurse 2006; 81: 1-3.
20. Minore B, Boone M. Realizing potential: improving interdisciplinary professional/paraprofessional health care teams in Canada's northern aboriginal communities through education. Journal of Interprofessional Care 2002; 16: 139-147.
21. Wakerman J. Defining remote health. Australian Journal of Rural Health 2004; 12: 210-214.
22. Mirando S, Davies PD, Lipp A. Introducing an integrated care pathway for the last days of life Palliative Medicine 2005; 19: 33-39.
23. National Library for Health. About integrated care pathways. (Online) 2005. Available: http://www.library.nhs.uk/pathways/page.aspx?pagename=ICPS (Accessed 3 March 2007).
24. Hicks LL, Bopp KD, Winter F. Integrated pathways for managing rural health services. Health Care Management Review 1996; 21: 65-72
25. Ouwens M, Wollersheim H, Hermens R, Hulscher M, Grol R. Integrated care programs for chronically ill patients: a review of systematic reviews. International Journal for Quality in Health Care 2005; 17: 141-146.
26. MedicineNet.com. Definition of managed care. (Online) 2007. Available: http://www.medterms.com/script/main/art.asp?articlekey=4270 (Accessed 3 March 2007).
27. Kelley ML, MacLean MJ. I want to live here for rest of my life. The challenge of case management for rural seniors. Journal of Case Management 1997; 6: 174-182.
28. Stanton MP, Dunkin J. Rural case management: nursing role variations. Lippincott's Case Management 2002; 7: 48-55.
29. Garaasen H, Kaasa S, Roesstad T, Broen P. Specialised short-term wards in nursing homes: a professionally and financially sound solution. Tidsskrift for Den Norske Legeforening 2005; 125: 1503-1505.
30. Aaraas I, Langfeldt E, Ersdal G, Haga D, Sykestuemodellen, nøkkel til bedre samhandling i helsetjenesten - la sykestuene leve! Tidsskrift for Den Norske Legeforening 2000; 120: 702-705.
31. Olesen F, Jensen PB, Grinsted P, Henriksen JS. General practitioners as advisers and coordinators in hospitals. Quality in Health Care 1998; 7: 42-47.
32. Department of Health. Patient pathways. (Online) 2007. Available: http://www.dh.gov.uk/PolicyAndGuidance/OrganisationPolicy/SecondaryCare/TreatmentCentres/TreatmentCentresArticle/fs/en?CONTENT_ID=4097263&chk=RGATY4 (Accessed 3 March 2007).
33. Mitchell G, Del M, Francis D. Does primary medical practitioner involvement with a specialist team improve patient outcomes? A systematic review. British Journal of General Practice 2002; 52: 484.
34. Hampson JP, Roberts RI, Morgan DA. Shared care: a review of the literature. Family Practice 1996; 13: 264-279.
35. Gruen R, Bailie R. Specialist clinics in remote Australian Aboriginal communities: where rock art meets rocket science. Journal of Health Services & Research Policy 2004; 9Suppl 2: 56-62.
36. Journal of Telemedicine and Telecare e-journal. Guidelines for authors. (Online) no date. Available: http://www.rsmpress.co.uk/jtt_gfa.htm (Accessed 3 March 2007).
37. Wootton R, Jebamani LS, Dow SA. E-health and the Universitas 21 organization: Telemedicine and underserved populations. Journal of Telemedicine and Telecare 2005; 11: 221-224.
38. Edwards MA, Patel AC. Telemedicine in the state of Maine: a model for growth driven by rural needs. Telemedicine and e-Health 2003; 9: 25-39.
39. Dimmick SL, Burgiss SG, Robbins S, Black D, Jarnagin B, Anders M. Outcomes of an integrated telehealth network demonstration project. Telemedicine and e-Health 2003; 9: 13-23.
40. Brebner EM, Brebner JA, Ruddick-Bracken H, Wootton R, Ferguson J, Palombo A et al. Evaluation of an accident and emergency teleconsultation service for north-east Scotland. Journal of Telemedicine and Telecare 2004; 10: 16-20.
41. Campbell NC, Ritchie LD, Cassidy J, Little J. Systematic review of cancer treatment programs in remote and rural areas. British Journal of Cancer 1999; 80: 1275-1280.
42. Levine SR, Gorman M. 'Telestroke'. The application of telemedicine for stroke. Stroke 1999; 30: 464-469.
43. Audebert H. Telestroke: effective networking. Lancet Neurology 2006; 5: 279-282.
44. Hess DC, Wang S, Gross H, Nichols FT, Hall CE, Adams RJ. Telestroke: extending stroke expertise into underserved areas. Lancet Neurology 2006; 5: 275-278.

