Context
Allied health service delivery in rural and remote areas of Australia is characterised by an increasing demand for allied health services, workforce shortages and a high turnover of staff1. Therapy assistants (TAs) can deliver allied health services to meet the needs of rural and remote communities2-5.
Rural and remote TAs deliver therapy programs to clients under the direction of allied health professionals (AHPs)5,6; however, their role varies from that of their metropolitan counterparts. Customarily, metropolitan TAs are aligned with one discipline7,8,9 and are based within that discipline in a hospital setting. In Western Australia (WA), many rural and remote TAs have a multidisciplinary role, are based at a different location to their supervising AHP, and work in schools or across a number of settings10.
Rural and remote TA programs have been attributed with providing ongoing client management between AHP visits (in the case of outreach services), giving continuity of services during AHP staff turnover, and building skills within the community11. For these reasons TAs are seen as an effective means of improving access to allied health services in rural and remote areas.
Therapy assistants have come to form a significant part of the rural and remote allied health workforce in WA10. (However, in other remote areas of Australia differing models of allied health service delivery exist. One established model is community co-workers, who work with AHPs delivering primary health care allied health services12,13). A census undertaken in 2005 identified 98 TAs in rural/remote WA who were supervised by AHPs employed by the WA Country Health Service (WACHS; Fig1), the state government health service provider10. The WACHS was the primary employer of TAs (63%). Disabilities Services Commission (DSC) (16%) and the Department of Education (13%) were also substantial employers10.
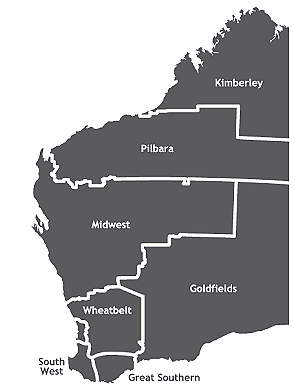
Figure 1: Map displaying Western Australia Country Health Service Regions
Training is essential in providing any health worker with the appropriate knowledge and skills for their work. Training for TAs in rural and remote WA has been identified as a priority in a number of projects developing the role of the rural and remote TA workforce3,14. Most training of rural TAs has occurred 'on-the-job' on an individual site-by-site basis, and typically provided by the supervising AHPs14. For AHPs, the demands of TA training sometimes competes for time in a busy clinical caseload14.
Although there is recognized training accredited through the Australian Vocational Education and Training sector (VET) (Certificate III in Health Service Assistance - allied health assistance), this does not reflect the role of rural TAs in WA 14. In 2005, only three of 98 rural and remote WA TAs had a recognized qualification for their work10.
Issue
This article reports on a project initiated to improve TA training in rural and remote WA: the WACHS/DSC TA Training Initiative.
The WACHS/DSC TA Training Initiative
The aims of the WACHS/DSC TA Training Initiative were to:
- develop an efficient and effective means of delivering TA training that reduced the training load placed on AHPs at a site level
- increase the skills and competencies of TAs
- increase the quality of services provided by TAs.
In order to achieve these aims, three objectives were identified:
- standardise the foundation competencies for TA across the WACHS
- develop a series of distance-learning training modules for TAs
- coordinate a schedule of TA training to be delivered via videoconferencing.
The WACHS/DSC TA Training Initiative formed part of a comprehensive model of training for TAs that includes statewide and localized training (Fig2).
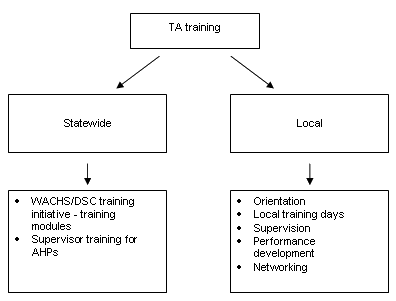
Figure 2: Features of a comprehensive training model for therapy assistants in Western Australia. AHPs, allied health professionals; WACHS/DSC, Western Australia Country Health Service/ Disabilities Services Commission.
Funding, project officer and steering committee: A part-time project officer (0.4 FTE) was employed to oversee the project, with funding provided by the WACHS and DSC. A steering committee was formed with AHP representatives from each WACHS Health Service Region (Fig1). The membership of this group expanded during the project to include two rural/remote TAs and a representative from DSC. The role of this group was to direct the overall development of the training program and the implementation of training modules.
Training priorities: A needs assessment survey was distributed to TAs and AHPs across the WACHS to identify training priorities within the workforce. This assessment confirmed a widespread need for training. Specifically, clinical training for TAs in the area of paediatrics was identified as a priority.
TA Training modules: Sixteen TA training modules were developed to meet identified needs (Table 1). Modules had a paediatric focus, covered a range of allied health disciplines (speech pathology, occupational therapy and physiotherapy) and were appropriate for delivery by videoconference. Small working groups were formed to develop a training package for each module. Working groups comprised the project officer and appropriate AHPs from different WACHS regions, who had relevant expertise in the topic, and experience working with TAs.
Table 1: Therapy assistant training modules developed for the Western Australia Country Health Service/ Disabilities Services Commission Therapy Assistant Training Initiative
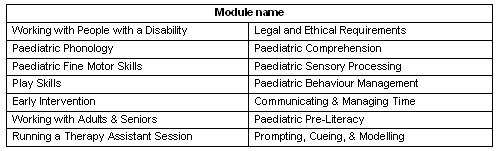
A comprehensive training package for each module comprised a 1.5 hour presentation delivered via videoconference, presenter notes and participant handouts. Each training package contained all the resources necessary for any AHP to present the module. Participant handouts included notes on the session content, learning activities, a TA assessment to be completed with on-site AHP supervisors, and module evaluation form. It was planned to adapt most training packages for delivery via VHS, DVD and CDROM for those unable to access scheduled videoconference training.
A priority of the initiative was the development of a training pathway for TAs toward a recognized qualification. A partnership between WACHS and the West Coast Technical and Further Education body (TAFE) linked elements of the training to the Certificate III Health Service Assistance (Allied Health Assistance). Where possible, training modules were matched to relevant units within the existing TAFE course and assessed against the required competencies. The completion of these modules contributed to the Certificate III qualification.
Evaluation
The reach of the training program was indicated by the number of participants and sites connecting to each module. An assessment of perceived quality of each module came from post-session evaluation forms submitted by participants immediately after each module. These forms asked about perceptions of the format and content of the training, and self-reported change in knowledge before and after the module (four point scale: poor, fair, good, excellent). Open-ended questions asked about strengths and areas for improvement.
To determine the longer-term impact of the training program, a purposive sample of five TAs and five AHPs was selected from across WACHS regions. Participants included AHPs from differing disciplines who work with TAs, and TAs with a variety of clinical experience and varying degrees of participation in the training program. The survey included demographic information and a series of open-ended questions exploring the perceived advantages, disadvantages and influence on work practices of the training program as a whole. Telephone interviews were conducted three months after completion of the training with participants' statements recorded by the interviewer. At the conclusion the content of the interview was reflected back to participants for verification.
Ethics
Exemption from formal ethical review on the basis of quality assurance was granted by the University of Western Australia Human Research Ethics Committee. The project was considered a part of usual WACHS quality assurance activities and did not involve any clients or client records. WACHS provided institutional approval.
Evaluation results
Participants: Fifteen training sessions were delivered: one was cancelled due to technical difficulties with videoconferencing. In total 30 different sites across rural and remote WA attended the training sessions with a total of 247 site link-ins (Fig3). An average of 16 sites attended each session. Numbers in each session ranged from 5-100 participants with an average of 44 participants per training session.
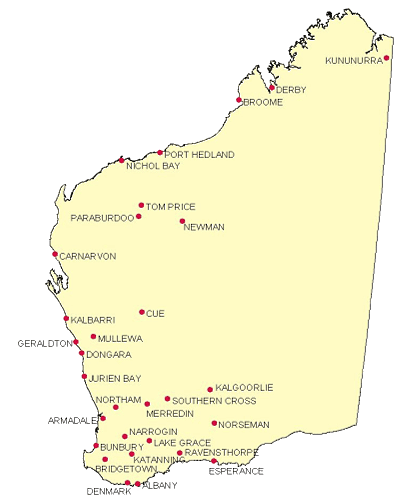
Figure 3: Map displaying sites attending training for the Western Australia Country Health Service/ Disabilities Services Commission Therapy Assistant Training Initiative
A total of 416 (67%) evaluation forms were returned from individual training sessions. Sixty-five percent of these participant evaluation forms were from Tas, and 20% were education assistants. (An education assistant is employed by the Department of Education and Training and assists the teacher in delivering planned education programs and encourages a supportive and inclusive learning environment. Education assistants often assist teachers in delivering programs to students including programs developed by speech pathologists, occupational therapists and physiotherapists). Of the remainder, 3% were parents, 2% were AHPs, 4% were other assistants, such as nursing and respite assistants, and 6% were unknown. Of those who returned participant evaluation forms, the majority (63%) were employed by the WACHS, followed by the Department of Education (20%) and DSC (6%).
Training: There was a high general level of satisfaction with the training. Overall 341 participant evaluation forms (82%) rated sessions as good or excellent, 42 (10%) as fair, four (1%) as poor, and 29 (7%) unknown. Three hundred and seventy-four participant evaluation forms (90%) agreed the length of the session was appropriate and 395 (95%) considered the activities and handouts within the training were useful. These sentiments were echoed in interviews with participants 3 months following the program. Participants also reported a reduced load for individual AHPs: 'it's statewide so the load is shared' (AHP 5); 'there is reduced need to develop training' (AHP 1); and '(there is) reduced training time for therapists' (AHP 2).
Sessions on clinical areas, and those that were practically focused, were rated above the non-clinical (eg legal and ethical requirements, running a therapy assistant session). Characteristics of sessions rated 'good' or 'excellent' were excellent presentation skills, a high level of preparedness, good supporting resources such as hierarchies and checklists, and interactive activities including case studies and problem solving scenarios completed during the session. Conversely, sessions rated 'fair' or 'poor' had poor presenter engagement (poor eye contact, reading from notes, lack of preparation), technological difficulties with videoconferencing, and poor pacing of the session; some topics could have been expanded and run over two sessions.
These themes were echoed in interviews. The most successful presentations had 'greater interaction and practical elements as well as feedback, as opposed to presentation' (AHP 3). Conversely, a lack of interaction during the sessions was viewed less positively: 'the style of some of the presenters was difficult to listen to. If they read from notes (or) information not practically grounded... boring' (TA 1).
Two hundred and eleven (51%) participant evaluation forms rated an improvement in their knowledge after training, 174 (42%) felt their knowledge was unchanged, 29 (7%) were unknown, and two (0.005%) felt they had less knowledge after training sessions. Of those with unchanged knowledge, 142 (82%) had rated their knowledge 'good' before attending the session.
Comments from respondents in interviews indicated that, for TAs with greater than 2 years' experience, the training validated their current practice. It was 'good for consolidating knowledge' (TA 1). For TAs with less experience, the training provided 'good basic information' (TA 4) and was a 'general introduction to everything' (AHP 3).
Videoconferencing: Three hundred and seventy-four (90%) participant evaluation forms indicated confidence in receiving training by videoconference, and 358 (86%) rated the sound and image quality as good. Most interview participants had found videoconferencing a positive way to access training; 'it saves time and money for isolated staff, it's convenient and easy to access' (TA 3).
While many interviewees found interaction with presenters and participants by videoconference positive, the level of experience was a factor; 'for some, videoconferencing is an unfamiliar medium; it's difficult to engage and pipe up' (AHP 2). The technical aspects of using videoconferencing were also a barrier at times: 'when there are technical glitches it is difficult to concentrate' (TA 1). As one participant also noted: 'not all areas have videoconferencing' (AHP 5) and '(there are) scheduling difficulties. It'll be better when DVDs are released' (AHP 4).
Networking: Networking opportunities were a further theme that emerged during interviews. The TAs strongly identified the benefit of networking with other TAs through the training as 'great for networking, feeling less isolated, (seeing the) bigger picture' (TA 1); 'being able to see other TA's, fantastic networking opportunity' (TA 2); and 'a nice sense of solidarity connecting to colleagues' (TA 5). The opportunity to network was also highlighted by one AHP: 'great networking opportunity for in-house and across WACHS' (AHP 4).
Lessons Learned
This project is a further step in the development of rural and remote TA practice and complements previous work undertaken to develop consistent standards for WA rural and remote TAs15. The WACSH/DSC TA Training Initiative is part of a comprehensive training system and is the first formal training system developed in line with the needs of rural and remote Tas, and accessible to those in rural/remote areas.
A number of key features of this project are relevant to the rural and remote context and for other services considering similar programs. First, the integral role of AHPs throughout the project has been important. Allied health professionals have had significant input to this project as participants on the steering group, in the development and delivery of the training, and the assessment of TA competency. As a result, training modules have been closely linked to needs 'on the ground'. This approach was validated by the significant numbers of TAs participating in training.
The development of training packages that 'stand alone' around each identified topic potentially allow any AHP to deliver TA training without too much effort. This has advantages in terms of sustainability of the program. In the situation of workforce turnover, any AHP is able to deliver a training module, which reduces reliance on external presenters or funding. To date, 14 modules have been produced as distance learning packages on VHS, DVD and CD, enabling those without access to videoconferencing to also access training.
Previously, the opportunity for career advancement and recognition of skills has been an important issue for TAs14. Articulating the WACHS/DSC TA Training Initiative with the existing training pathway through West Coast TAFE has been a central feature of this project. To date, eight TAs have enrolled and three have completed a Certificate III (Health Service Assistance - Allied Health Assistance). This is an important avenue for TAs. However, because most TAs work part-time (between one and 10 hours10), there are substantial costs associated with Certificate III enrolment, and recruiting TAs may be difficult10. It is not feasible for rural and remote health services to insist all TAs have a Certificate III level qualification.
The comprehensive training system for TAs includes a general level of knowledge for the role, as provided by training modules in the WACHS/DSC training initiative, and relevant local information provided through orientation processes, local training days, supervision, performance development, and networking with other TAs (Fig2). Therapy assistants are sometimes perceived to be a cheaper alternative workforce, or a panacea for allied health workforce shortages; however, as this work shows, this is not the case. Even though this project reduced the load on individual AHPs to train TAs, there are significant support requirements beyond Certificate III training or the WACSH/DSC TA Training Initiative in order to run successful TA programs2,14.
To sustain this model there is ongoing employment of a part-time project officer (0.4 FTE). The project officer will be responsible for coordinating further training by videoconference, adapting training modules for distance learning formats, and developing ongoing TA training modules in line with need. Areas identified to improve the delivery of training are the quality of presentation (organization, interactive learning activities, and supporting resources) and ensuring participants have had an orientation and training in the use of videoconferencing.
Conclusion
This training system is a further step in describing key aspects of a rural and remote model of TA allied health service delivery. The training resources produced during this project are relevant to health services employing, or looking to employ, similar models of service delivery. The method used to develop this training, utilizing a 'ground-up' approach, was important in ensuring training was directly tied to work requirement. An important aspect of this project is that TAs now have the opportunity to gain recognition for the training they are undertaking. Determining how similar models of allied health service delivery might be applied to other rural and remote populations, such as Aboriginal communities in WA, requires investigation. Further research is also needed to investigate the efficacy of the rural and remote TA model.
Acknowledgements
The authors would like to acknowledge members of the project steering group and training module working groups for their commitment to this project; interview participants for their time and considered input; Ann Larson and Tim Moss for reviewing copies of the manuscript; and Emma Birch for her input as the current WACHS TA project officer. This project was jointly funded by WACHS, Disabilities Services Commission, and the Australian Government Department of Health and Ageing. The Combined Universities Centre for Rural Health is funded by Australian Government Department of Health and Ageing.
References
1. O'Kane A, Curry R. Unveiling the secrets of the allied health workforce in Australia. In: Proceedings, 7th National Rural Health Conference. 1-4 March 2003; Hobart, TAS: National Rural Health Alliance, 2003.
2. Lin I, Birch E, Goodale B. Rural and remote therapy assistants in WA: the development of a statewide approach. In: Proceedings, 2nd NSW Rural Allied Health Conference: Allied Health Working Together. 28-29 October 2005; Sydney, NSW; NSW Health, 2005.
3. Lowe W. Rural Western Australian therapy assistant project report. Disabilities Services Commission and Combined Universities Centre for Rural Health; 2003.
4. Hall M. Integrated therapy assistants and video-conferencing. In: Proceedings, 7th National Rural Health Conference. 1-4 March 2003; Hobart, TAS: National Rural Health Alliance, 2003
5. Goodale B, Lin I. Therapy assistants - a model in rural/remote Western Australia. In: Walking Together - side by side. Proceedings, The National SARRAH Conference. 26-28 August 2004; Alice Springs, NT: Services for Australian Rural and Remote Allied Health, 2004.
6. Telfer J. Workforce planning-thinking outside the square for a flexible allied health workforce. In: Walking Together - side by side. Proceedings, The National SARRAH Conference 26-28 August 2004; Alice Springs, NT: Services for Australian Rural and Remote Allied Health, 2004.
7. Australian Physiotherapy Association. Physiotherapy assistants: policy statements and guidelines. Melbourne, VIC: Australian Physiotherapy Association, 2002.
8. Occupational Therapy Australia. Occupational therapy assistants: policy statements and guidelines. Perth, WA: OT Australia WA Inc; 2005 March.
9. Stevens A. Speech pathology Australia position statement on therapy assistants. Melbourne, VIC: Speech pathology Australia, 2004.
10. Lin I, Villaneuva K, Goodale B, Spitz S. Therapy assistants in WA: where, who and what does it mean? In: Proceedings, 2nd WA Rural and Remote Allied Health Forum. Health Communities: Closing the Gap. 24-25 June 2005; Fremantle, WA; Country Health Services, 2005.
11. Battye KM, McTaggart K. Development of a model for sustainable delivery of outreach allied health services to remote north-west Queensland, Australia. Rural and Remote Health 3: 194. (Online) 2003. Available: www.rrh.org.au (Accessed 21 August 2007).
12. O'Rourke K, Galligan K. North and West Queensland primary health care community-based workers. In: Proceedings, Building Bridges Crossing Borders: the National SARRAH Conference. 13-16 September 2006; Albury, VIC: Services for Australian Rural and Remote Allied Health, 2006.
13. Kokinos M. Developing partnerships with Indigenous community co-workers - the implementation of an innovative allied health model in the Katherine region. In: Proceedings, 2nd WA Rural and Remote Allied Health Forum. Health Communities: Closing the Gap24-25 June 2005; Fremantle, WA; Country Health Services, 2005.
14. Goodale BG, Lin I. Midwest Murchison region therapy assistant project - final report. Perth, WA: Western Australian Country Health Service and Combined Universities Centre for Rural Health, 2005.
15. Lin IB, Goodale BJ. Improving the supervision of therapy assistants in Western Australia: the Therapy Assistant Project (TAP). Rural and Remote Health 6: 479. (Online) 2006. Available: www.rrh.org.au (Accessed 21 August 2007).



