Context
The Australian rural experience indicates that there is a long-term problem in attracting medical practitioners1. In particular, access to psychiatrists in rural areas has been seen as uniformly a major problem2.
Latrobe Regional Hospital (LRH) is located within Gippsland, 2 hours from Melbourne, the state capital of Victoria. The Gippsland region stretches from the eastern edge of Melbourne to the far-eastern Victorian/New South Wales border. It has a unique combination of socio-economic groups and demographic spreads, including urban coastal areas, industrial centres and remote rural towns.
Mental health services are provided to approximately 3500 clients per year in a geographical area of over 40 000 km2. The LRH mental health model is based on 'Victoria's Mental Health Service - the Framework for Service Delivery'3 and is aimed at providing accessible care in a least restrictive environment. The service has been divided into three geographical sectors in which there are a total of eight community mental health centres covering adult, aged and child and adolescent programs. The centrally located inpatient services comprise 25 adult beds, 2 child and adolescent beds, 6 secure extended-care beds, and a 20 bed aged mental health unit.
In 2006, the equivalent of 11 full-time psychiatrists were employed across the three programs, working within community and inpatient settings.
Issue
Difficulties in recruiting
Difficulties in recruiting in the early 1990s led to a crisis in 1994. With just one psychiatrist employed, the service relied on the assistance of metropolitan-based psychiatrists in an outreach model. The number of psychiatrists employed at LRH over the last 12 years is plotted in Figure 1, which demonstrates a gradual increase in numbers.
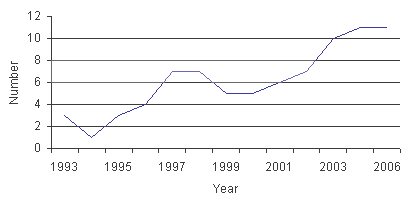
Figure 1: The number of psychiatrists employed at Latrobe Regional Hospital, 1994-2006.
In 1994, despite extensive advertising in Australia, little or no interest in positions was received. Reasons for the exodus of Australian-trained psychiatrists from the public sector have been described as multiple and coincided with the First National Mental Health Plan and associated reduction in mental hospital beds by 42%. The private sector proved very attractive, with perceived increased control over work, capacity to work one-to-one rather than within a team, and exposure to a broader range of psychiatric disorders4.
During the periods of low numbers of psychiatrists the workload was untenable and problems numerous. These included:
- lack of specialist expertise in the treatment of clients
- existing psychiatrists seen as prescription officers
- lack of psychiatrist input into service planning
- lack of peer interaction, support and scrutiny
- existing psychiatrists required to be on-call almost continually
- difficulty in covering periods of leave
- pressure of work preventing adequate orientation of new staff
- pressure of work preventing academic activities
- cancellation of accredited psychiatry registrar program.
It became essential to give priority to the recruitment and retention of psychiatrists - for the benefit of both clients and staff. A recruitment and retention strategy was implemented in 1995, resulting in an increase of appointments (Fig1). Success was not achieved overnight, and it came about through a combination of factors.
Profile and publicity
A concerted effort was made to raise the profile and credibility of the service. Presentations at conferences, show-casing of aspects of the model of care, the development of state-wide protocols with the Victorian Department of Human Services, and stronger linkages with other rural mental health services were important aspects.
Establishing Individual rapport
Advertising in international psychiatry journals achieved significant interest from psychiatrist international medical graduates (IMGs) who had specialist qualifications gained outside Australia. The service concentrated on presenting a professional impression to all potential applicants, including the provision of information packages covering the service and Gippsland. Prompt responses to enquires and providing information on the recruitment process were other important factors in establishing rapport with applicants.
Applications received were predominantly from India. The Victorian employment process included: review of the applicant's curriculum vitae by the state chief psychiatrist; registration with Victorian Medical Practitioner Board; and a temporary working visa until fellowship of the Royal Australian and New Zealand College of Psychiatrists (RANZCP) was achieved.
The recruitment process was managed within LRH mental health services and took between 3 and 6 months. It commenced with individual telephone interviews, an important element in the process of building rapport. Experience showed that the greater the rapport between the service and the psychiatrist during this long and often frustrating process, the more likely the recruitment would ultimately succeed. Up-to-date knowledge of visa requirements through contacts within the Australian Government Department of Immigration and Citizenship also assisted in faster visa approvals.
Multifaceted orientation program
The transition of psychiatrist IMGs and their families to a new country and culture is important5. Assistance was provided with housing, schooling options and getting established in a new environment.
Considerable effort was taken with the induction and orientation of new psychiatrists. While most services have well-developed professional orientation to the organisation, it is equally important to maintain a supportive environment as well as address differences between cultures and countries6. Some of the matters discussed include:
- family structure and values in Australia
- community values
- behaviour which is seen as acceptable and that which is not
- colloquial use of language, especially swearing or slang.
Improving retention rates
By 1997, LRH had full psychiatrist staffing with seven psychiatrists IMGs employed. However retention rates were still relatively low with a number of psychiatrist IMGs passing their fellowship exams and moving to private practice or more senior positions within the public hospital sector. Others moved from Victoria to other Australian states.
Once again, psychiatrist IMGs filled this gap. Word of mouth proved to have an increased impact, with psychiatrist IMGs recruited who were already working in more junior roles within Australia.
Retention of staff is as important as staff recruitment7. Retention rates of psychiatrists employed by LRH improved from an average of 18 months in 1994 to an average of 4 years 2006 (Fig2). There were a number of important contributing figures.
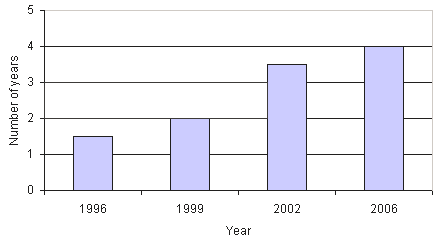
Figure 2: Retention rates of psychiatrists.
Medical staff structure: The sectorised medical staff structure implemented in 2001 is outlined in Figure 3. The model provides for sector psychiatrists to have responsibility for the overall care of sector clients both in the community and as inpatients, with the further support of medical officers and registrars (doctors appointed to accredited specialist training position or who hold a position designated as such by the hospital). The continuity of patient care and less demanding travel requirements resulting from clear division of responsibilities and shared workloads proved particularly attractive to the psychiatrists.
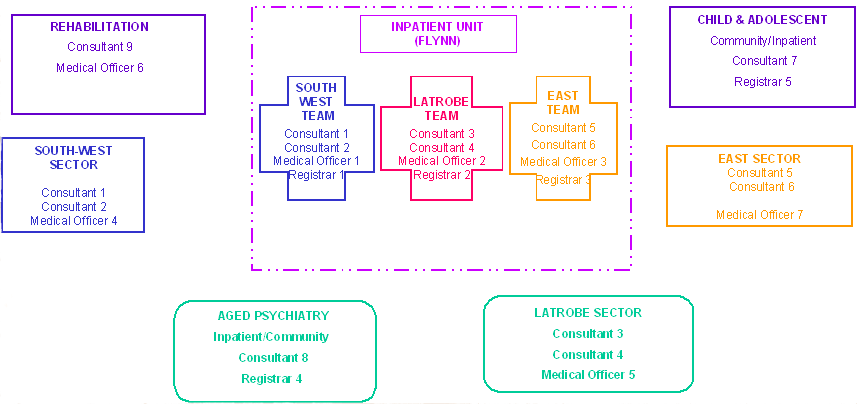
Figure 3: Medical staff structure.
Registrar Program: Another essential element associated with improved recruitment and retention is the RANZCP Southern Region Training Committee Psychiatry Registrar Program. The program effectively provides two full-time equivalent registrars with four, three-month, compulsory rural rotations per year, in addition to the psychiatrist staff profile. The registrars provide important supervision to the more junior medical officers and vital support to the psychiatrists. A positive 'rural experience' is the aim for the Melbourne-based registrars. Some of the ways in which this has been approached are:
- registrars are not on-call over weekends
- one day per week is allocated to attend academic activities in Melbourne and pursue studies (usually a Friday)
- rent-free accommodation is provided (a furnished house).
Academic developments: In 2002 a greater emphasis on rural psychiatry led to the establishment of a Professorial Chair in Rural Psychiatry with Monash University. This conjoint appointment between LRH and the Department of Psychological Medicine, School of Psychology, Psychiatry and Psychological Medicine, and School of Rural Health, Monash University, significantly increased the profile of research and academic activities at LRH. The impact on both recruitment and retention has been positive.
Other improvements: Greater internal flexibility and support came through the development of the sub-speciality areas of aged psychiatry and child and adolescent mental health - the areas of greatest need.
The recruitment of a Psychogeriatrician enabled the creation of an aged psychiatry registrar position. Significant funding for this position was received from the Commonwealth Government through the Advanced Specialised Trainee Post in Rural Areas (ASTPRA).
A Child and Adolescent registrar position was offered with this two-year course being undertaken consecutively by two full-time registrars, with supervision from Melbourne-based child and adolescent psychiatrists. The service's profile remained high and this, together with a relatively close proximity to Melbourne assisted in securing the additional part time services of an Australian trained child and adolescent psychiatrist.
Recent challenges
The registrar supervision is undertaken at two levels within the service. Consultant psychiatrists who are approved non-college supervisors provide supervision at a one-on-one level. In addition, the Professor of Rural Psychiatry/Director of Clinical Services provides regular group registrar supervision. Recent RANZCP regulations have, however, become stricter, creating some issues. The LRH is working towards a 'train the trainer' model, with the aim of being better able to facilitate the approval of psychiatrist IMGs as supervisors.
Changes in the requirements of the RANZCP for both aged mental health and child and adolescent registrars also impacted on the previous strategy of recruiting psychiatrist IMGs to these positions. Applicants for the advanced trainee positions are now required to have achieved RANZCP fellowship status. An important factor in improving retention rates has been the linking of these specialist training positions with currently employed psychiatrists who are interested in specialising after achieving fellowship status.
The Psychiatrist Training Initiative
An area of current concern for many psychiatrist IMGs in Australian, and one that does impact significantly on their recruitment and retention, is the difficulty that many experience in passing RANZCP exams. This led to an increased focus at LRH on educational support, including exam preparation workshops. A specific program, the Psychiatrist Training Initiative (PTI) was developed. Described in a companion paper8, PTI takes a holistic approach to designing and developing an educational program. Specifically tailored for psychiatrist IMGs, the program incorporates strong elements of communication skills, acculturation issues and exposure to the Australasian model of psychiatry8.
In recent months there has been significant success with two LRH candidates passing the final clinical component of the RANZCP fellowship exams. The candidates attribute achieving their fellowship largely to this program.
Lessons learned
A review of our performance
Individual interviews were recently undertaken with past and present psychiatrists with a response from 14 out of 19 previously and currently employed psychiatrists.
To be described in more detail in a future article, a number of themes emerged from these interviews. Initial recruitment and commencement issues were generally viewed very positively. It was suggested, however, that further introductory materials should be supplied prior to commencement with LRH. The official orientation program also came under scrutiny. It was felt that the program was too quick, and not sufficiently in-depth. Additional information and training in leadership, team dynamics and cultural aspects of Australian and Gippsland were also identified as areas for improvement.
Professional isolation was highlighted as a concern, with requests received for additional linkages to city based psychiatrists and services. Feedback was also received on the need for increased peer supervision.
Conclusion
Significant progress has been made in the successful recruitment of psychiatrists to LRH. While the majority of psychiatrists recruited are IMGs, there is now a significant component of Australian trained psychiatrists who are attracted to the service. It appears that the previous situation of low numbers of psychiatrists employed is in the past. In addition, service systems have improved to the extent that the retention rates for recruited psychiatrists have increased dramatically.
The key elements of this success can be seen as:
- a focus on building individual rapport with new psychiatrists at the time of their recruitment
- an extensive and multifaceted orientation program
- working to meet individual and family needs, both professionally and within the wider context
- a sectorised medical staff structure, with both community and inpatient elements
- the provision of ongoing educational support with a specific focus on preparing for RANZCP fellowship exams.
While these achievements can be seen as the result of changes to recruitment processes and the ability of LRH to better meet the needs of psychiatrists, there is still room for improvement. An increased focus on cultural issues, family support, educational opportunities and additional linkages to city based psychiatrists and services are areas that would further increase work satisfaction and, in turn, result in further improved retention rates.
Acknowledgement
The authors acknowledge M Haines, Gippsland Regional Clinical School, School of Rural Health, Monash University, Traralgon, Victoria, Australia, who undertook the survey of psychiatrists - 'Attracting psychiatrists to a rural area', and clustered information.
References
1. Australian Medical Workforce Advisory Committee. The medical workforce in rural and remote Australia. AMWAC report 1996.8. (Online) 1996. Sydney, NSW: AMWAC. Available: http://www.health.nsw.gov.au/amwac/amwac (Accessed 20 June 2007).
2. Australian Medical Workforce Advisory Committee. The specialist psychiatry workforce in Australia. AMWAC report 1999.7. (Online) 1999. Sydney, NSW: AMWAC. Available: http://www.health.nsw.gov.au/amwac/amwac (Accessed 20 June 2007).
3. Department of Health and Community Services. Victoria's mental health service: the framework for service delivery. Melbourne, VIC: Psychiatric Services Division Victorian Government, 1994.
4. Barton D, Hawthorne L, Singh B, Little J. Victoria's dependence on overseas trained doctors in psychiatry. People and Place 2003: 11: 54-64.
5. Lau T, Kumar S, Thomas D. Practising psychiatry In New Zealand's rural areas: incentives, problems and solutions. Australasian Psychiatry 2002; 10: 33-38.
6. Han GS, Humphreys, JS. Overseas-trained doctors in Australia: community integration and their intention to stay in a rural community. Australian Journal of Rural Health 2005; 13: 236-241.
7. Storer D. Recruiting and retraining psychiatrists. British Journal of Psychiatry 2002; 180: 296-297.
8.Haines M, Oakley Browne M. Developing an educational framework for international medical graduates in rural psychiatry: The Psychiatrists Training Initiative. Australasian Psychiatry 2007; 15(6): 499-503.
Modified on 3 April 2008: the correction "Manager, Ambulatory Care, Latrobe Regional Hospital, Traralgon, Victoria, Australia" was made to the institutional affiliation of the third author.

