Introduction
Recognition of vaccine use through history has shown to be a significant intervention assisting in the reduction in childhood morbidity and mortality due to infectious diseases1-4. The paradox of this success is that as the risk of vaccine-preventable diseases drops, parents' attention turns to the perceived risk of vaccines5-10. Fine et al.3 stated that the very success of these programs brings new problems. No intervention is entirely without risk, and even very rare adverse reactions to a vaccine increase in importance as the target disease itself disappears3.
In years past, public health nurses in Alberta provided provincially standardized information on routine public-funded child immunizations. This information was what was to be given to parents, and assumptions may have been made that this information was adequate for the parents to make a decision.
However, since the 1980s, information calling into question the effectiveness, safety, and long-term effects of vaccines has become readily available, causing some parents to question the status quo11,12. Although the healthcare community has responded by providing additional sources of information, the reluctance of some parents to immunize their children has continued13.
Historically, health professionals have used information, developed for parents, to promote child immunization. Few studies have specifically looked at how effective and helpful this information is in meeting the needs of parents5,11,12,14,15. Although the literature stresses the importance of parents receiving clear, thorough and unbiased information about immunization so they can make an informed decision, limited attention has been given to how parents would, themselves, describe what clear, thorough, and unbiased information means to them.
The purpose of this study was to gain insight into parents' need for information about child immunization, in order to improve and/or optimize information shared by rural health professionals. More specifically we explored: (i) whether information contributed to their decision; and if so, how (ii) what types of information and content parents required; (iii) the sources of information considered helpful and trusted; and (iv) parents' suggestions on how information could be conveyed to them more effectively.
Methods
Given the limited amount of information available in this area of research14,15 and the exploratory nature of the study objectives, a qualitative study using semi-structured interviews was determined to be the best method to search out the information required from those participating in this study. These interviews were with mothers of children aged two years and under who had been eligible for routine immunizations in Alberta in the previous year.
Recruitment of study participants
Public health nurses working in the Rural South Area of Calgary Health Region assisted with recruitment of parents for this study. They had access to parents from a variety of settings, such as postpartum visits, 'Baby and Me' groups, breastfeeding support groups, community activities, and pre-natal classes.
Local public health nurses were asked to offer an information package to parents they had contact with who met the following criteria:
- were of legal age
- had faced making a decision about immunizing their infant in the past year (1 January to 31 December 2002). The child would be aged 2 years or less at the time of recruitment.
- were living in the rural area south of Calgary, within the boundaries of Calgary Health Region. This included small rural towns and villages serving the surrounding ranching and farming communities.
- could be fathers or mothers with varied ages, education levels, and family sizes
- were making different decisions in regard to vaccinating their children.
This information package included an information sheet, a reply card, and a stamped envelope. Interested parents filled out the reply card and returned it to the sealed drop box in each health unit office or directly mailed it to the investigator. Confidentiality was discussed in the information sheet assuring potential participants of their anonymity.
Recruitment was open for one month and the aim was to find as many eligible parents as possible over that month. Of the thirty-nine parents who volunteered and filled out reply cards, two were ineligible according to the study criteria.
The investigator contacted all but two of the respondents by phone (those two were set aside after numerous attempts to reach them by phone). This allowed respondents to ask questions about the study and gave the investigator an opportunity to gather socio-demographic information. It was hoped this would assist in drawing a purposive sample that represented as broad as possible a variety of ages, education levels, and different decisions about immunization (Table 1). While it was hoped that fathers would be included in the sample, no fathers responded to the call for participation. One potential reason for this was that mothers were more likely to bring their children to classes and clinics without the fathers.
Table 1: Characteristics of participants (n = 11)
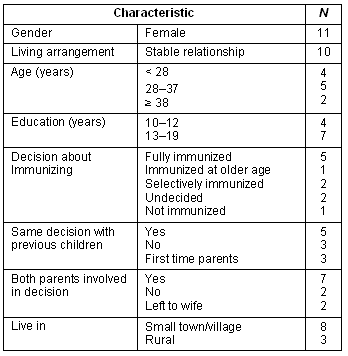
The rural communities in this area included one minority group, namely the Hutterites. Those eligible parents living on local colonies were asked if they would be interested in participating but declined. Apart from this, the participants appeared to reflect the socio-demographic variables of the majority of mothers in this geographical area. This was confirmed by senior management working with the public health nurses in this area.
Data Collection
Data were collected using semi-structured interviews of no longer than one hour in length. An interview guide was developed specifically for the interviews. Questions explored four different areas of interest: (i) whether information contributed to their decision; and if so, how (ii) what types of information and content parents required; (iii) sources of information considered helpful and trusted; and (iv) parents' suggestions on how information could be conveyed to them more effectively. The interview guide is provided (Fig1). While the intent was to audiotape all interviews, one tape was damaged which made transcription impossible; however, notes were made by the interviewer during this interview.

Figure 1: Interview guide.
Qualitative content analysis was used to identify themes and concepts16,17. This study was exploratory in nature and specific to assisting local public health nurses to better support parents on their decisions about child immunization. The focus was on identifying major themes and concepts, not in studying them in depth.
Data collection and analysis occurred simultaneously, so that when themes/concepts emerged during the interview process they were documented, coded, and compared with previously established categories16. This also allowed adjustments to be made to the interview guide, as needed, prior to the next interview18. Despite minor changes to the wording of questions, the initial intent of the questions was not changed.
Participants were chosen from the thirty-five eligible and available respondents. After 11 interviews two of the investigators had identified the same themes and concepts reoccurring in the interviews. Therefore, it was decided that saturation had been achieved and recruitment was stopped.
The principal investigator was responsible for all coding of transcription text. All coding was done by hand and many safeguards were present to ensure credibility and quality of the data19. These safeguards included: (i) reflective notes written on interviews as needed; (ii) one of the co-investigators reviewed parts of all transcripts and the other co-investigator independently coded all transcripts; (iii) every participant was given the opportunity to review the transcript of her interview (all declined to do so); and (iv) verbatim quotes of participants were used to support conclusions and demonstrate how categories were developed.
After the analysis was completed, findings were shared with the public health nurses. To begin assessing the usefulness of the results, the principal investigator met with most of the nurses from each of the six offices within months of the study's completion and collected feedback from them. Approximately 16 nurses participated during this process. In order to see what long-term effects this study may have had on their practice, feedback was asked of some of the nurses at a later date.
The design of this study and all tools used, including the participant information package and the interview question guide, were reviewed and given ethical clearance by the Community Research Ethics Board of Alberta (CREBA), Canada.
Results
Mothers' immunization decisions, about routine child vaccinations provided by the Alberta government, were classified as: (i) fully immunized with all routine vaccinations administered at recommended age in Alberta; (ii) immunized at an older age; (iii) selectively immunized by choosing certain vaccines for administration and rejecting others; (iv) undecided; and (v) not immunized.
The content analysis of the 11 participant interviews revealed five themes and numerous sub themes (Table 2). The themes found in the transcriptions of these interviews provided a rich body of information that could then be helpful in fulfilling the purpose of this study.
Table 2: Outline of results section

Theme 1: Factors influencing mothers' decisions
Role of information: Virtually all participants found that information from a variety of sources played at least one of the following roles in their decisions about immunization: helping to make the decision; confirming the decision; causing confusion and making the decision difficult; and stimulating more questions.
Regarding 'causing confusion' and 'making the decision difficult', Respondent 3 said: 'I don't really know what to believe'.
Other influential factors: Most participants discussed the other influences they felt had contributed to their decision about child immunization. Such influences included past experiences of themselves or others; perceived risks of vaccines; not being aware they had a choice with regard to vaccinating; personal beliefs coloring their attitudes and decisions; and relationships with health professionals.
Regarding past experiences, Respondent 8 said: '...I knew that it was going to be a tough decision for me at the start because my brother had problems with his immunizations....'
Theme 2: Mothers' concerns in making their decision
During the interview process, participants shared some of the worries they faced while making their decision about immunizing their child. These worries have been categorized into three sub-themes: making the right decision; being respected for making a decision; and being given all the information.
Making the right decision: 'Either way, whether I decided to do it or not to do it, I was potentially putting them in harm's way. I needed to stop and think about it'. (Respondent 7)
Being respected for making a decision: 'They need to have respect that the parent is the one making the decision and sometimes they don't get that'. (Respondent 9)
Being given all the information: '...the health nurse did, in the beginning, give me some books on immunization shots, but they were only one-sided...they didn't explain the other side'. (Respondent 5)
Theme 3: Perceptions of 'good' information
During the interviews, an obvious pattern developed as participants described what 'good' information meant to them. The 'characteristics of information' and the 'credibility of information' were two recurring sub-themes in discussion of the definition of good information. Responses pertaining to credibility - specifically, sources which were believed and why - were notably varied.
Characteristics of information: The majority of participants made comments which outlined two basic characteristics of good information. First, information should be comprehensive, that is, current, accurate, and balanced in its presentation. Second, information needed to be logical, clear, and understandable so that parents could feel satisfied they truly understood the information. Respondent 6 said, 'You know...nobody really explains anything easily, you know? ...all these big words...'.
Credibility of information sources: Most participants shared their views on who they perceived to be trusted information providers and why. The opinions expressed were varied and underscore the impact of parents' experiences and feelings with regard to perception of credibility. Some parents found it essential to have official health sources from which to obtain information. Some required an established, trusting relationship with the information source, for example the doctor-patient relationship. Others found they had confidence in information sources they could relate to, whether someone acknowledged their concerns or had walked in their shoes previously. This was very powerful in establishing credibility.
I want it from my trusted people in my community...from my doctor and ...health nurses.... (Respondent 4)
I guess...it depends on their credentials a little bit.... (Respondent 8)
I get counsel from other people - they are people that are receptive and you know make thoughtful decisions...I know they've made thoughtful decisions...when sorting through the information I'm looking for facts versus blanks...I try to assess them as best that I can.... (Respondent 9)
Theme 4: Mothers' information needs
In discussing their experiences and views about the information presently available to parents, every participant contributed to some key recommendations for future development and distribution of the information on child immunization. These recommendations, although diverse, were organized into the following categories: presentation, quantity, availability, timing, and contents of the information.
Presentation of information: The participants' responses indicated that a varied presentation of information is necessary to meet all parents' needs (eg written, oral, visual).
Quantity of information: A few participants addressed the issue of how much information was enough. It became obvious that parents' needs regarding the quantity of information, differ and must be met individually.
Availability of information: Some participants shared where they had found information and offered ideas on where they felt information should be available. The suggested places included doctors' offices, hospitals, health units, prenatal classes, libraries, and the internet.
The timing of receiving information: Many participants agreed that information on child immunization should be available well before parents must make a decision. Some felt this information should come during the pre-natal period so the information could be considered without the additional stress of welcoming the new arrival. Most felt post-delivery was not an optimal learning time for this decision-making process.
Content to be covered: The quotes below elucidate some of the topics/concerns mothers mentioned during the interviews (Fig2).

Figure 2: Participant identified topics/concerns helpful in making informed decisions.
...their immune system has never worked yet...they've never had the chance to fight anything off... there needs to be more study on that and...you know...how much benefit is there to letting their immune system start working on its own before you start injecting into it.... (Respondent 3)
...like I said...research studies...with dates on the publication or specific numbers-information that's as specific as possible. (Respondent 1)
I guess statistics would be what I would be looking for...how many years have they been giving this and the kids that have been followed along and they had no problems.... (Respondent 4)
Most participants emphasized the importance of having current information that addressed all sides of the immunization issue. The following remarks reflect this:
Both sides of the story. I got only the medical side...what the doctors have been taught...what the nurses have been taught. I only got the side that they've been taught in medical school...It works for some...What about the children who have problems? And what they didn't tell me was the other side of the coin...so that I could weigh it out for myself. (Respondent 5)
...everyone's got a right to know...it's just like when you get a prescription at the drugstore, they give you two sheets of what might happen to you if you take this pill and it's just worse-case scenario and I don't think it would frighten, I think it would just inform. (Respondent 4)
Theme 5: Recommendations to health professionals who convey information
During the interviews, each participant provided a perspective on how well health professionals convey information to parents. Their perceptions and observations pertaining to this final topic provided better understanding of the effect health professionals have on parents in the simple act of sharing information. Participants suggested that health professionals strive to provide an environment which welcomes questions and open discussion so each parent's questions and concerns can be addressed adequately. Furthermore, health professionals need to demonstrate that they are well informed and up to date with current research and practices relating to child immunization. Last, health professionals should recognize that parents can be affected by their demeanour and attitude. Being clear on where the health professional's allegiance lies can also be helpful to parents.
...some nurses are better than others. There was a nurse that I had...I could go in there and feel like I was visiting an old friend...but there are other nurses that I couldn't wait to get out of there! I am there to be respected and someone caring for my children and one way that I handled that...is that I choose who I see. (Respondent 9)
The fact that they thought to explain things and exactly what they were going to do and what impact it might have or what side-effects...was reassuring. It made me feel like they were well informed and I've always had confidence in them. (Respondent 1)
Participants had other ideas that could improve how information was delivered to parents. These ideas included: (i) being willing to locate resources for parents; (ii) using teachable moments to prepare parents for the immunization process; (3) speaking in terms parents can understand; (iv) respecting parents as the decision makers; (v) providing overviews of diseases and vaccines; (vi) pointing out information specific to immunization when given at postpartum visits; and (vii) working together with alternative health communities in providing information. The following response illustrates this last idea:
I would actually be very, very happy if, um, the two health communities...the homeopaths and the MDs, would work together, because they both have a tremendous amount of information...um...they both, uh, I think are very, um, credible. I think they both carry a lot of weight and they both have some very valid points, but I think they need to work together. (Respondent 7)
A final comment illustrates both the recommendation to address parents' concerns and the suggestion to willingly locate resources for parents.
...and to have the answers, you know, or if...if they don't know, that maybe they could suggest where I might be able to find that information, you know...where I might look...you know? I'd like it to be validated that, you know, it is a concern...even though, to them, this one child in a million, right? But to me, it's my child. (Respondent 3)
In order to begin assessing the value of this study, it was important to know whether local public health nurses gained greater understanding of what parents needed from them when making decisions about child immunization. Initial feedback indicated that the nurses realized there was room to improve their practice. Feedback given later indicated that the nurses had now incorporated these ideas and were using them in their practice.
Two particular words described the feedback from those nurses: enlightenment and confirmation. Here are a number of thoughts shared by some of the nurses:
Enlightenment: Nurses commented:
My practice changed as a result of the study.... I used to push for vaccination so that the stats would look good. Since the study, I spend more time making sure that the parents are feeling comfortable with immunization....I believe in the long term, this approach will yield an improved immunization rate as well as improved respect for other public health initiatives. (Nurse 1)
...I certainly give a lot more information than I might have in the past. I don't push vaccines, but offer as much info as possible to try to help parents make a decision. I don't skirt the issue of side effects and will offer to find more info if I can. I have also started letting people know that it is never too late to start vaccinations.... I think I try to give a balanced view, even though I am pro-vaccine. I find that arguing with people never gets you anywhere. (Nurse 2)
I am more ready to listen to parents' concerns. (Nurse 3)
...parents are not passive consumers - we need to be better prepared to answer their questions intelligently instead of just 'it is the right thing to do because we say so'. Also to respect the parents' right to make that choice. (Nurse 4)
What I learned is how important it is to acknowledge and respect a parents concerns around immunization. Give them the information and give them the time to make an informed decision. Parents are only acting out of concern for their children and it is important to recognize this. (Nurse 8)
Confirmation: Nurses commented:
...it confirmed my belief that one of my roles is to help parents access the info they need to be comfortable making a decision re: immunization. ...parents need to be able to trust the nurse: that s/he will not judge them for questioning the safety and need of vaccines, and that s/he will provide them with non-biased information sources. (Nurse 5)
...confirmed my belief that people need to be totally comfortable with their decision to vaccinate themselves or their children. (Nurse 6)
...reminded me that every parent makes the decisions about their child's health and immunization and it is my job to provide information and support and the rest is up to them! (Nurse 7)
Discussion
During the 1990s, local public health nurses began to notice a shift in how accepting parents were of child immunization. The nurses had observed reluctance of some parents to accept the information routinely provided as the only source they would use in making their decision. Other sources of information, which questioned the effectiveness, safety, and long-term effects of the vaccines, seemed readily available to these parents. They began to question whether it was safe and necessary to vaccinate their children, and local nurses found it increasingly difficult to know how to respond when confronted about these issues.
The fact that parents were seeking alternative sources of information for this decision showed an increasing need to look at the situation with new eyes. What were parents looking for that the standardized information was not providing? What did they need to know in order to make an informed decision? How were parents deciding whom to believe among the sources of information they encountered? Thus, this study explored these questions and a veritable wealth of information was gathered during the interview process.
Most participants confirmed that the use of information had played some role in their decision about immunizing their children. However, other factors were seen at times to have greater influence on those decisions. Other factors identified were: personal/others experiences; beliefs; perceived risks to the child; parents were unaware of their right in Alberta to make the decision; and relationships with health professionals.
Mothers expressed worries about making the decision to vaccinate their children. First, were they making the right decision? Second, would they be respected for the decision they had made? Third, had they received complete and balanced information on which to base their decision?
Study participants defined what 'good' information meant to them. Full disclosure about vaccines in a language easily understood was important to them. Mothers also determined what they considered credible sources of information. This criterion seemed to be based on their experiences and feelings.
The study results also identified participants' perceived information needs. Certainly it was important that information on child immunization address all sides of the issue and answer questions thoroughly. However, it was also important to address the needs of parents individually in such areas as how information was to be presented, where it would be most available, and when would it be most helpful.
Beyond the information itself, most participants felt that how health professionals conveyed information had a major impact on them. Comments referring to trust and respect were often heard in the interviews. These mothers wanted to feel respected and supported in whatever decision they made. They did not always feel that health professionals could do this because of their professional role and bias toward promoting immunization.
The findings of this study were limited by the following factors: (i) the design meant that only parents living in a specific rural Alberta area were included and, thus, the results cannot be generalized; (ii) the size of sample was small; and (iii) only mothers volunteered to participate. It should, however, be noted that some mothers indicated that fathers were actively involved in making decisions about immunizing their children.
While limited, the results were comprehensive and provided much information to improve practice. The significance of this study was found to be in the ideas and concerns these mothers shared during the interviews, which were relevant to the local public health nurses, as confirmed in interviews with the nurses about the utility of the results. Some of the nurses were able to identify improved ways to broach the subject of child immunization with their parents. Others felt confirmed in the way they were supporting parents and conveying information.
As a result of this study, the nurses also recognized that not all parents wanted to immunize their children and that they may not be receptive to information offered to them. The nurses saw that persuading or intimidating these parents into vaccinating their children was unlikely, and that in Alberta parents have the right to chose.
This study clearly suggests parents simply wanted to make the right decision for their children. Sporton et al. has said that parents perceive themselves as having the roles of protector and decision-maker, and being responsible for any consequences resulting from those decisions20. Immunization requires parents to take a small but active risk with their children for the benefit of the community, and some may see that risk as unnecessary21. The nurses were able to gain a better understanding of how important it was to acknowledge parents' concerns, articulate a balanced presentation on the benefits and risks of immunization, encourage questions and thoughtful reflection about the issue, and support parents in the decision they make.
Future investigation on this subject, using a larger, more diverse population from both urban and rural areas to ascertain if there are any differences between rural and urban parents' perspectives, would further add to the knowledge base on this subject for front line health professionals.
Conclusion
While not all the information generated in this study may be new, its strength was that the need for it arose in practice, and that nurses appeared to take ownership of the results because this was about parents in their region. Nurses' feedback on this study and its findings demonstrated a high likelihood that the results would be used and lead to changes in practice.
Acknowledgement
This research was supported by a grant from the Alberta Heritage Foundation for Medical Research.
References
1. Poland GA, Jacobson RM. Understanding those who do not understand: a brief review of the anti-vaccine movement. Vaccine 2001; 19: 2440-2445.
2. Jaroff L. Vaccine jitters. Time 1999; 154(11) : 64-65.
3. Fine PEM, Chen RT. Confounding in studies of adverse reactions to vaccines. American Journal of Epidemiology1992; 136: 121-135.
4. Lemonick MD, Park A. Vaccines stage a comeback. (Online) 2002. Available: www.time.com (Accessed 5 March 2008).
5. NewsRx. Childhood immunizations: parents must get more information to counter immunization fears. Medical Letter on the CDC&FDA. (Online) 14 March 2004. Available: http://www.newsrx.com/newsletters/Medical-Letter-on-the-CDC-and-FDA/2004-03-14/0314200433322DC.html (No date of access).
6. Asch-Goodkin J. When parents say "No" to immunizing their child. Contemporary Pediatrics 2005; 22 : 80,78,76.
7. Duffell E. Attitudes of parents toward measles and immunisation after a measles outbreak in an anthroposophical community. Epidemiology and Community Health 2001; 55: 685-686.
8. Gellin BG, Maibach EW, Marcuse EK. Do parents understand immunizations? A national telephone survey. Pediatrics 2000; 106: 1097-1102.
9. Halperin SA. How to manage parents unsure about immunization. Canadian Journal of CME 2000; 12: 62-74.
10. Evans G, Bostrom A. Vaccine risk communication. American Journal of Preventive Medicine 1998; 14: 237-239.
11. Levi BH. Addressing parents' concerns about childhood immunizations: a tutorial for primary care providers. Pediatrics 2007; 120: 18-26.
12. Smailbegovic MS, Laing GJ, Bedford H. Why do parents decide against immunization? The effect of health beliefs and health professionals. Child: Care, Health & Development 2003; 29: 303-311.
13. Alberta Health and Wellness. Table B-11: Immunization coverage. (Online) 2004. Available: http://www.health.alberta.ca/regions/b11.htm Accessed 10 March 2008.
14. Austin H. Parents' perceptions of information on immunization. Journal of Child Healthcare 2001; 5: 54-59.
15. Lochhead YJ. Failure to immunize children under 5 years: a literature review. Journal of Advanced Nursing 1991; 16: 130-137.
16. Creswell JW. Qualitative inquiry and research design. Choosing among five traditions. Thousand Oaks, CA: Sage, 1998.
17. Polit DE, Hungler BP. Nursing research. Principles and methods, 6th edn. Philadelphia, PA: JB Lippincott, 1999.
18. Rothe JP. Undertaking qualitative research. Edmonton, AB: The University of Alberta Press, 2000.
19. Norwood SL. Research strategies for advanced practice nurses. New Jersey, NY: Prentice Hall Health, 2000; 147-168.
20. Sporton RK, Francis SA. Choosing not to immunize: are parents making informed decisions? Family Practice 2001; 18: 181-88.
21. Leask JA, Chapman S. An attempt to swindle nature: press anti-immunisation reportage 1993-1997. Australian and New Zealand Journal of Public Health 1998; 22: 17-26.


