Introduction
There were 88 398 new incidences of cancer detected in Australia during 2001, an increase from the 65 966 new cases in 1991, illustrating the large impact cancer has on society1. Over the past 30 years, the incidence of cancer in the Australian state of New South Wales (NSW) has risen substantially, and is predicted to rise another 25% by 20112.
The modern treatment approach to cancer care is multidisciplinary, with surgical, medical and radiation oncology treatments playing significant roles3. The literature suggests that 50% of cancer sufferers should receive radiation therapy (RT), either as a primary treatment or as an adjuvantive, combined approach, in both palliative and curative treatments4. Radiation therapy involves the use of ionising radiation to cause irreparable damage to tumour cells, while minimising the dose received by the normal tissue of surrounding structures. This maximises the therapeutic effect of RT and minimises treatment morbidity experienced by the patient5.
The radiation oncology team is largely multidisciplinary, consisting of medical, allied health and nursing staff. Radiation oncology departments require a large support network of medical physicists, biomedical engineers and information technology specialists to operate effectively. Because of this, radiation oncology departments are more often situated in metropolitan or large regional centres and rarely in rural or remote settings. For example, the referral base from the NSW rural and remote health sector of the Calvary Mater Newcastle (CMN) Department of Radiation Oncology exceeds 250 000 people. From the 1615 patients receiving treatment at the CMN in 2007, 27.7% of these were from rural and remote regions. This necessitates rural patients who require RT to relocate to the area of the nearest radiation oncology department for the duration of their treatment, which can be for between one and 7 weeks, or more in some cases. This relocation can have a large financial and psychosocial impact on patients and their families.
Following the completion of their RT course, rural patients return to their homes. Any acute side-effects of the RT will not have resolved on completion of the course, and may even increase in severity before beginning to resolve 10 to 14 days after treatment completion6,7. This means that the immediate after care of acute radiation reactions is often managed by GPs. In some cases the knowledge of GPs in rural and remote locations is not adequate enough to deal with patients' concerns. Mallinger, Griggs and Shields8 suggest that information may not be delivered effectively during this time, because physicians are not confident to discuss the issues relating to this specialist area. Compounding this, GPs may have very little support and training in the management of acute and long-term radiation induced side-effects. Currently, there is very little RT information readily available in the rural setting to patients and health professionals. This can impact on referrals and decision-making, and can potentially increase patient anxiety.
The project described aimed to:
- Define the current level of rural GP knowledge on RT information for patients.
- Explore the desire of rural GPs to receive education on general RT topics and post-RT patient management.
- Develop, implement and evaluate a educational resource to address identified areas of interest
All training and educational packages developed would be supported by an existing e-learning platform at the CMN Radiation Oncology Department called 'The Knowledge Tank'. The Knowledge Tank facilitates access to information and training for users anywhere and at anytime, as well as providing a constant and reproducible point of reference. In order to provide information and education to the target groups, adherence to educational design principles was necessary. A detailed educational design plan was required which included a needs assessment. This project report will discuss the development of a survey instrument and both quantitative and qualitative results.
Methods
Development of the survey instrument
The needs assessment was performed by a questionnaire (Appendix I) that included the following topics:
- GPs' previous experiences in caring for a patient involved in radiation therapy
- GPs' level of general knowledge on RT
- the information GPs view as important to provide to a patient considering or undergoing RT
- the information GPs feel important to have access to regarding RT
- what level of information on radiation induced skin injury is preferred by GPs
- how the information should be delivered and distributed to both patients and GPs.
The survey was based on quality assurance work previously conducted at the CMN that explored the issues important to patients as they begin their journey into the radiation oncology environment. Given the wide variety of potential RT treatment morbidities, radiation induced skin injury was targeted by the survey because it is a side-effect most patients will experience during their course of RT6,7.
Data collection
The survey was distributed to 1700 GPs via the NSW Rural Doctors Network. Data collection began in June 2007 and ceased in September 2007. All surveys were accompanied by an information sheet detailing the background of the project, and an addressed reply-paid envelope to return the completed survey. The information sheet informed GPs that return of the completed survey implied consent for the data in it to be used for the this project, resultant professional publications and conference presentations. A follow-up reminder notice was placed on the NSW Rural Doctors' Network website 1 month after distribution. No direct contact could be made with participants to prompt return of the surveys because access to the distribution database was not available to the researchers. All returned surveys were anonymous unless the participant chose to include personal details.
Data analysis
The quantitative data retrieved from the survey were entered in SPSS v15.0.0 (http://www.spss.com/products/). The GPs' responses for each survey section were examined descriptively. Qualitative data that were provided in open-ended questions and comments were subjected to a content analysis. The content analysis required the following steps:
- All qualitative data were analysed in MS Excel.
- The data weres read by the researcher to become familiar with overall content.
- The data were then re-read from hard copy, and common themes were identified.
- The identified themes were grouped into categories to illustrate key areas of interest within the data
Results
Response rate
Of the 1700 surveys distributed, 374 complete surveys were returned, providing a 22% response rate. The distribution of responses within the four major area health services in NSW is shoen (Table 1).
Table 1: Distribution and response rates of surveys by area health services
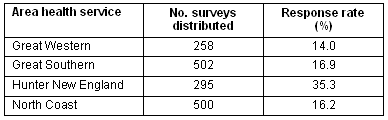
Information necessary to provide to patients
From the 374 GPs who responded, 93.9% had cared for a patient who had received RT, but only 23.3% of those felt they had sufficient information to discuss issues impacting on the patient's care (Fig1). The remaining 76.7% provided detailed responses regarding the type of information the GPs felt would be beneficial to provide to the patient (Fig2).
In addition to these responses, analysis of the open-ended questions revealed several themes that the GPs felt should also be included for the patient's benefit (Fig3), and for both the patient and GP's benefit (Fig4).
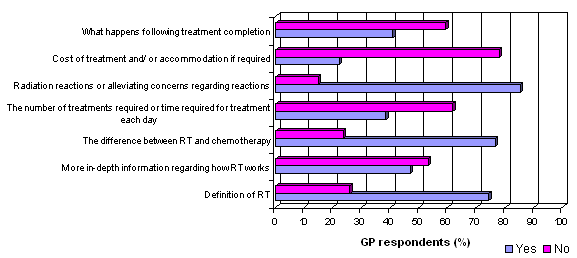
Figure 1: Whether or not GPs who reported having sufficient knowledge regarding radiation therapy (RT) informed their patients about specific RT topics.
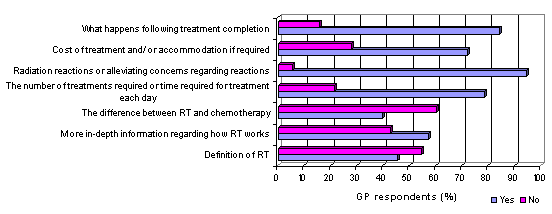
Figure 2: GPs' belief about whether specific patient radiation therapy (RT) information would be beneficial for patients or not.
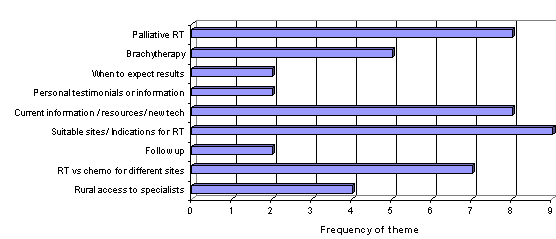
Figure 3: Emergent themes that GPs identified as important to be included in patient education resources. RT, radiation therapy; tech, technology.
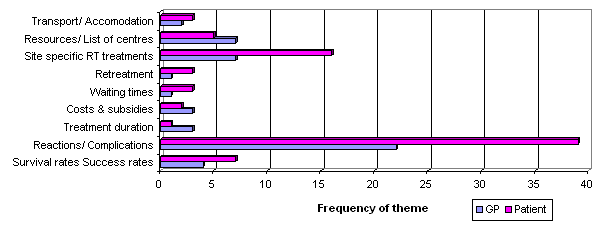
Figure 4: Emergent themes that GPs identified as important to be included in patient and GP education resources. RT, radiation therapy.
How to deliver the information
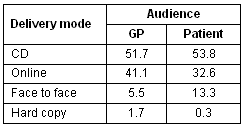
When the participants were asked which electronic media they would prefer for the delivery of information (for professional and patient use), there was no overwhelming majority for delivery via CD or online. However, many GPs indicated delivery preferences other than in electronic (Table 2).
Table 2: Delivery mode preferences for GP and patient distribution
Skin care management information
A total of 96.1% of the respondents indicated they would find information about acute and chronic radiation skin reactions useful in caring for a patient undergoing or completing a course of RT. Figure 5 shows the specific information they felt would be useful.
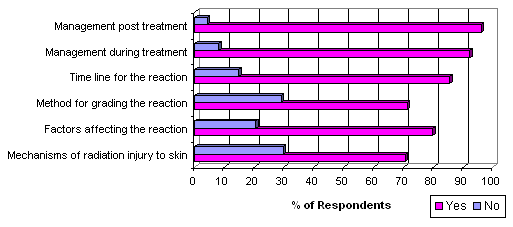
Figure 5: Specific information on radiation skin reaction that GPs nominated as a useful addition to the information package.
Content analysis
Analysis of the qualitative data indicated three main categories that GPs feel are beneficial for both their own professional development and as specific patient resources (Fig4). These include:
- site-specific treatments and reactions
- logistical information
- survival statistics.
In addition to this, GPs reported specific patient resources that need to be included (Fig3), all quite substantial and distinct topics not readily assimilated into groups. The majority of GPs also indicated the mechanisms and management of radiation-induced skin reactions was a topic that should be explored in the training material.
Discussion
The initial response rate to the surveys was encouraging; however, this was not sustained and the low (22%) overall response rate limits the generalisability of the study. There may be a number of reasons for the low response rate, such as the heavy workloads of rural GPs, and a perceived lack of need for further knowledge of RT. However, with well over 300 GPs responding from a cross-section of NSW, the sample was successful in representing the target audience. The distribution of responses within area health services were generally evenly distributed within larger populated regions.
The areas surveyed were key areas of importance identified by a quality assurance project completed within the CMN Radiation Oncology Department; this project involved patient, clinician and radiation therapist input. In interpreting the results of this study it is important to note that the instrument used was not a validated survey. While the domains investigated were generated from patient and clinician input, it is possible that not all areas were addressed. However, respondents were given the opportunity to raise other concerns in open-ended questions. The results were analysed qualitatively and will contribute to the design of the educational intervention to follow.
The results indicate that many rural and remote GPs have cared for a patient about to undergo RT, or one who has completed a course of RT. Most importantly, very few of the practitioners felt they had sufficient knowledge to inform and support such a patient. This indicates a need for information available to rural and remote GPs about the general concepts of and practical information on RT, for both professional use and distribution to patients.
This project identified a definite need for an educational strategy to be implemented that addresses all key areas explored in the survey, as well as site-specific treatment reactions and survival statistics. The next stage of this project will involve the development, distribution and evaluation of an educational strategy. The final stage of the project will include a post-intervention survey to assess if any improvement in GP knowledge has been sustained as a result of the educational package. Future projects could explore whether the planned educational strategy could have a measurable impact on patient care.
Although this project will endeavour to use all relevant data and comments in the design of the information packages for rural GPs and their patients, it must be noted that the needs of these groups vastly outweigh the resources of this project. This project will address the deficit of available resource material for rural and remote GPs in NSW. It will endeavour to provide an overview of RT practice for them and their patients, as well as information and training on assessing and managing radiation-induced skin reactions.
Acknowledgments
This study was funded by the New South Wales Institute of Rural Clinical Services and Teaching and NSW Health, Australia.
References
1. Australian Institute of Health and Welfare. Cancer in Australia 2001. Australian Institute of Health and Welfare & Australasian Association of Cancer Registries. Canberra, ACT: AIHW, 2004.
2. Tracey E, Roder D, Bishop J, Chen S, Chen W. Cancer in New South Wales Incidence and Mortality 2003. NSW Cancer Registry. Sydney, NSW: NSW Cancer Institute, 2005.
3. Rubin P, Williams JP. Clinical oncology: a multidisciplinary approach for physicians and students, 8th edn. Philadelphia, PA: WB Saunders, 2001.
4. Baume P. Radiation Oncology Inquiry. A vision for radiotherapy. Canberra, ACT: Commonwealth of Australia, 2002.
5. American Society of Radiologic Technologists. Introduction to Radiation therapy practice standards. Albuquerque, NM: American Society of Radiologic Technologists, 2004.
6. Perez C, Brady L, Halperin E, Schmidt-Ullrich R. Principles and Practice of Radiation Oncology, 4th edn. Philadelphia, PA: Lippincott, Williams & Wilkins, 2004.
7. Hymes S, Strom E, Fife C. Radiation dermatitis: clinical presentation, pathophysiology, and treatment 2006. Journal of American Academy of Dermatology 2006; 54: 28-46.
8. Mallinger J, Griggs J, Shields C. Patient-centered care and breast cancer survivors' satisfaction with information. Patient Education and Counseling 2005; 57: 342-349.
_________________________________
Appendix I: Distributed survey

