Introduction
The mental healthcare system in Victoria, Australia has evolved over the past two decades. Significant changes to policy and service delivery have followed since the introduction of the first National Mental Health Strategy in 1992. Since this time, there have been two subsequent revisions to the plan. A major change in service delivery was introduced by the 1992-1998 plan1. Previously, mental healthcare service delivery relied heavily on services provided by long-term psychiatric hospitals. The first plan saw a significant reduction in institution-based care and a shift towards community-based services. With the second plan (1997-2003) a key focus area was addressing high prevalence disorders. The current plan for the period 2003-2008 states four priorities: (i) mental health promotion and illness prevention; (ii) better service responsiveness; (iii) strengthening service quality; and (iv) encouraging research, innovation and sustainability.
Child and Adolescent Mental Health Services (CAMHS) provide services for children and adolescents who have a serious emotional disturbance1. The CAMHS clients are aged between 0 and 18 years. The CAMHS service components comprise: Intensive Mobile Youth Outreach Services (IMYOS); continuing care, which includes assessment, treatment, case management, parental support and consultancy to other services; acute inpatient services; day programs; and conduct disorder programs.
Social features of health sector workplaces
Social support in health workplace settings may include emotional as well as instrumental support from colleagues and supervisors. Consideration of the literature examining social support reveals that emotional and instrumental social support are generally not distinguishable in the findings. While some studies define social support in terms of practical support offered by co-workers and managers, others considered workplace social support as emotional support. Research findings indicate the positive effects of good social support in the workplace for health professionals in the areas of intrinsic motivation, job satisfaction, health, and wellbeing2-5. Results from these studies illustrate the significance of social relationships at work and demonstrate that social relationships in healthcare organizations represent both sources of emotional and instrumental support for employees.
Service delivery in rural areas
Rural mental health service delivery operates according to the same age-based structure as metropolitan settings, with specialist mental health services comprising clinical and Psychiatric Disability Rehabilitation Support Services (PDRSS). There are currently eight Area Mental Health Services (AMHS) in rural Victoria. However, notable differences exist between urban and rural public mental health service delivery.
One major difference in rural service delivery compared with urban service delivery concerns co-location of services6. Larger regional services generally provide 'single-services' to each of the three age groups at separate locations. In contrast, rural AMHS tend to base CAMHS, Aged Psychiatric Mental Health Services (APMHS) and adult psychiatric services in the same setting. Often all three mental health services will be co-located at community health centres. These community health centres provide a variety of other community services in addition to specialist mental health services.
Another distinguishing feature of rural mental health service delivery is the variation in service configurations6. Co-location of services is one model of service delivery. Alternatively, some central rural service hubs may provide satellite services as a cost-effective approach to service delivery for communities who face great travel distances to larger population centres. Up to seven satellite services can be offered, based at central rural service hubs. Also, certain rural communities operate mental health crisis services from local hospitals, where individuals presenting with severe mental distress may be admitted.
Significant differences exist in service usage between rural and metropolitan AMHS6. Rural mental health services respond to a higher percentage of the population compared with urban mental health services. From 2004 to 2005, 1.56% of the population accessed a rural AMHS versus 1.04% who accessed an urban AMHS. With regard to inpatient services, the average length of stay was predominantly lower in rural areas than statewide and urban averages. In six rural areas the average length of stay was less than 10 days. However, similarities existed between urban and rural AMHS for the 2004 to 2005 timeframe in relation to increases in clientele and high occupancy levels of inpatient services.
Other factors to consider in rural mental health service delivery result from the limited availability of alternative service providers6. Due to less PDRSS, and few GPs, psychiatrists and psychologists, public mental health service providers tend to fulfil a broader range of roles. Greater geographical travel distances also impact on service delivery. More time is needed for travelling, meaning less time is spent delivering services.
Although the rural public mental healthcare system operates according to the same structure statewide, there are clear differences in service delivery between rural and urban areas. One such difference is the co-location of psychiatric services, a common practice in rural areas7. Often rural AMHS take on a wider variety of responsibilities compared with AMHS in urban areas due to a lack of available services. Rural AMHS providers travel greater distances than their urban counterparts, which impacts upon service delivery. In addition rural AMHS clinicians may face a greater responsibility for service provision due to a lack of feasible alternative providers.
The present study
According to the National Mental Health Strategy's Mental Health Statement of Rights and Responsibilities, 'children and adolescents admitted to a mental health facility or community program have the right to be separated from adult patients and provided with programs suited to their developmental needs'8. Although this statement represents the ideal, the realities of child and adolescent mental health service delivery in rural areas include a lack of healthcare services, financial constraints, greater service delivery areas and fewer mental healthcare specialists7. As such, several community-based mental healthcare services exist in rural Australia in which child and adolescent services are co-located with adult services.
Until recently, the CAMHS studied in regional Victoria, Australia, was co-located with the adult mental healthcare outpatient service. This meant that services to CAMHS clients were delivered from the same setting as the mental health services provided to adult clients with mental health problems. In 2005, this CAMHS relocated and became a stand-alone service. Consequently, the location from which service delivery was provided for existing CAMHS clients and clinicians changed. Therefore, this group of clinicians and their clients had the unique experience of service delivery provided from both a co-located and a stand-alone setting.
The present study aimed to explore the perceptions of service providers on the impact of different settings on service delivery. The following research questions were explored within a qualitative framework:
- What effect did the relocation of the service (stand alone vs co-located) have on utilization of the service from the clinicians' perspective?
- What was the impact on clinicians of the relocation of this CAMHS from a co-located to stand alone service?
Method
Participants
Participants comprised one male and five female CAMHS clinicians ranging in age from early thirties to late forties. The disciplinary backgrounds of the participants were psychology, social work, and psychiatric nursing, with two participants representing each discipline. Experience in a CAMHS setting ranged from 5 to 20 years. The research was discussed at a CAMHS staff meeting and clinicians were invited to participate. Inclusion criteria specified that clinicians needed to have experienced service delivery both from the co-located and the current stand-alone CAMHS settings. All of the eight eligible participants were invited to participate. One declined participation and the other was unable to complete the interviewing within the timeframe of the study.
Data analysis
Recorded data were transcribed verbatim and de-identified by the first author. A thematic analysis was carried out on the transcribed data based on an interpretative phenomenological analysis approach, with a focus on participants' experiences and perceptions9. To begin with, the first case was read several times and initial impressions of the data were noted in the transcript margin. These first insights were then re-examined and given preliminary thematic labels. Themes were listed and organized into clusters to reflect connections between categories. Once clustering of themes had occurred superordinate labels were assigned to each cluster. Subsequent transcripts were then analysed using the initial thematic structure from the first case as a guide to coding. As new themes emerged across cases the superordinate thematic structure was refined.
Rigour
Validity of the results was enhanced by utilization of the qualitative data analysis techniques described by Goodrick10. During analysis consideration was given to how the data could be organized to support different thematic categories. This seeking of rival explanations resembles Karl Popper's notion of refutation, whereby more confidence in the validity of results follows when rival explanations are sought and not found. Validity was also enhanced through peer debriefing with the study's co-authors. This process involved discussing preliminary ideas of thematic categories to help identify alternative ways of coding the data. Special ethical approval was granted for de-identified transcripts to be presented to the research group for this purpose.
Procedure
The CAMHS manager initially approached the second author with a request to conduct research into the effects of the service relocation. Meetings were held with CAMHS management to discuss aims of the project and methodological considerations. Ethical approval was obtained from both the Department of Human Services through the hospital ethics committee and the university ethics committee. Clinicians who consented to participating in the study contacted the first author and an interview time was arranged. Participants who decided to take part were individually interviewed about their experiences of service provision from the old and new settings. The first author conducted all the interviews.
Interviews were digitally recorded. Data files were subsequently transferred to the student researcher's computer and password protected. All data was de-identified and transcribed verbatim by the student researcher according to qualitative data transcription guidelines described by McLellan, Macqueen, and Neidig11. Transcribed data files were password protected and stored exclusively on the student researcher's computer.
Results
Interview data were organized into three core thematic domains: (i) negative impact of co-location on clients; (ii) physical features of settings; and (iii) social capital. Under each core theme, sub-themes were identified that provide more specific detail around the core theme. Thematic descriptions are accompanied by select quotes from participants to provide an illustration of the concepts. A matrix display of the results is presented (Table 1).
Table 1: Matrix display of results
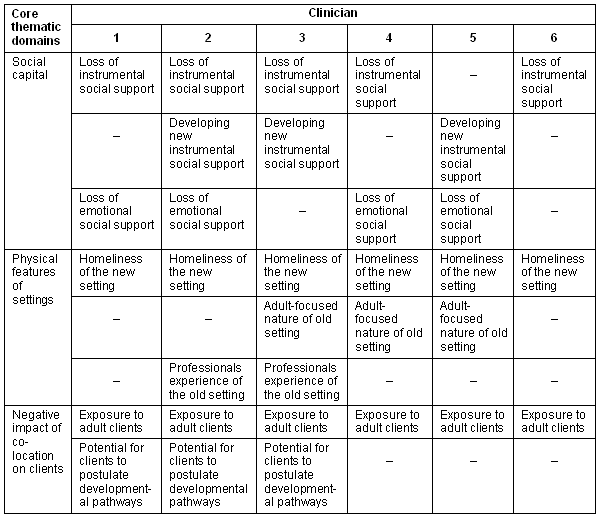
Negative impact of co-location on clients
Service delivery from a co-located setting with adult psychiatric clientele was viewed as potentially harmful for CAMHS clients and their families. Placing young clients within physical proximity to older clients with serious mental illnesses was suggested to increase the risk of CAMHS clients witnessing disturbed behaviours or postulating a developmental pathway from child emotional difficulties to adult psychiatric illness.
Exposure to adult clients
All participants expressed concern over the possibility of young clients and their families coming into contact with clients from the adult psychiatry service at the co-located setting. Exposure of CAMHS clients to adult psychiatric clients was seen as a major problem due to the severity of mental illness in the adult client population. Although efforts were made to keep adult clients separate from CAMHS clients, clinicians explained how, by virtue of service delivery from the same location, there was a risk that the two groups would encounter each other. Interviewees recognized how their clients could experience the behaviours of clients from the adult service to be frightening. For example:
...people just coming to the front door or families with young children might be sitting in the waiting room and then you've got an adult client who is increasingly uncontained and then of course when they're confronted with a whole bunch of clinicians standing there saying 'Is there anything we can do to help?'...it's still incredibly confronting to see a person having a psychotic episode and you know isn't fully alert and aware of objective reality. It can be experienced as a frightening and confronting situation and yeah you can get quite uncontained and aggressive behaviour and that ... is not appropriate to have a children's waiting room anywhere near that vicinity.
Potential for clients to postulate developmental pathways
Another consequence of young clients and their families receiving services from the same setting as adult psychiatric services mentioned by some clinicians was the potential for families to make a link between their child's current emotional difficulties and adult mental illness. Clinicians were concerned that CAMHS clients might have difficulty distinguishing child and adolescent mental health difficulties from long-term psychiatric illnesses and reach the conclusion that childhood mental health problems always lead to mental illness in adulthood. Participants discussed how this association was more likely to occur when children and adult psychiatric services were delivered from the same setting. For example:
I think the other point would be a fear coming into a centre like that, seeing the other clients, adult clients with very chronic schizophrenia and chronically disabling conditions and the question 'Will that be me?'.
...basically the difference with the adult clientele that a mental health service deals with is the very severe mental illness. And often that can be really confronting and frightening for families of young children, who might be presenting with you know emotional disturbance or ADHD or um an eating disorder or something like that and then the association between does that mean my child's going to go on and have these difficulties. So, and those are the thoughts that I think sometimes will come to families.
Physical features of settings
Clinicians offered their perspective on the impact of the physical characteristics of each setting on clients. Characteristics of the new location were viewed as contributing to a better experience for clients and visiting professionals while features at the co-located setting were seen to be inappropriate for a younger client group.
Homeliness of the new setting
Clinicians perceived that receiving services at the new location was a more positive experience for clients due to the welcoming and family-friendly atmosphere that resulted from coming to a setting that resembled a home. All of the interviewees recognized the house set-up at the new location as a significant strength of the service relocation. Examples of remarks from clinicians include:
...it's more child-friendly, it's not as intimidating. Kids come in here and their eyes are just lit up...It's more homely, it's not, you know um like walking into a doctor's office.
Adult-focused nature of old setting
In contrast participants viewed the physical characteristics at the old service location as potentially frightening for clients and their families. There was a common perception that the old setting was designed for an adult clientele and that the physical features of the environment at the old location might have contributed to a less positive experience of service delivery. For instance:
...some of the other difficulties were that because adult and child were in together you had them coming into the one building and it's quite an intimidating building.
...you should never have to bring a child to a mental health service that says 'adult psychiatric services' on the front, or that says 'inpatient unit this way'. Or a huge sign on the front that says we will not tolerate violence and those kind of very confronting things for parents bringing a child in.
Professionals' experiences of the old setting
A few clinicians commented on the possible effects of the physical features of the service location on the experiences of visiting professionals. Their comments suggested that the old setting was not only possibly frightening for clients and families but that professionals also felt uncomfortable visiting the service at the old location. They stated:
It's only really been since we moved here that people feel comfortable coming to lectures here.
Well I've had a number of other clients other professionals say to me it was terrifying going in there [old setting].
Social capital
All participants commented on the significance of social relationships with staff from adult psychiatric services at the old setting. Resources obtained from these social networks included instrumental and emotional support. Relocation was perceived to have resulted in a weakening of social connections with adult psychiatric staff and a consequent loss of social capital contained in those relationships.
Loss of instrumental social support
Interviewees discussed practical benefits arising from relationships with staff in adult psychiatric services in the old setting. Familiarity with the adult psychiatric staff and being within close physical proximity was perceived as helpful when CAMHS staff needed assistance from members of the adult psychiatric team. Participants commented:
...sometimes it's good to get an adult's perspective, especially if we've got older adolescents because they may actually be transferring over to the adult system. So just with the transfer of cases I mean usually more just of a straight paperwork thing but I mean even just knowing that the adult clinician's room was you know just through the sliding door was helpful sometimes... you could catch up with things you had in common with clients.
Quite often we'd go 'what' and you'd get a referral and there's the medication you weren't familiar with and you'd just pop your head around the corner into the adult services and ask them and they had a lot of a lot more access to um psychiatrists than we did. We only had a CAMHS consultant psychiatrist one day a week... so you were able to talk to their psychiatrists as well and to clarify any sort of more tricky um clinical or you know pharmacological questions that you might have, which is handy.
Loss of emotional social support from the old setting
In addition to benefits obtained from more formal professional relationships with members of the adult psychiatric service, participants discussed the value of informal social relations with adult psychiatric staff at the co-located setting. Interviewees explained how relationships with staff at the adult service functioned as emotional support for CAMHS clinicians. To illustrate:
Initially I missed being around the adult services because I just it was nice to just see some of the people over there and obviously you have some friendly people. And sometimes it was nice to be able to turn around and sort of say you know come and have a coffee and just sit in the lunchroom altogether and that was the time where we'd all sort of talk.
Developing sources of social support at the new setting
Some participants mentioned the development of new working relationships with mental health clinicians at the hospital directly across the road from the new CAMHS location. This was viewed as a positive development for CAMHS. For example:
...we're linking in with them [the hospital clinicians] more formally like say for supervision and things like that. And [manager] has worked with their manager and stuff like that.
It's just across the road [the hospital] and we've developed closer links with people like [clinicians]. Not the rest of allied health but certainly [clinicians] and the psychology team. We're more connected to them than we used to be over there. And we need to be cos we're the ones that work more with kids...
Discussion
This study explored two research questions regarding the recent re-location of a regional CAMHS from co-located to stand alone premises; these were: (i) what effect did the relocation of the service (stand alone versus co-located) have on utilization of the service from the clinicians' perspective?; and (ii) what was the impact of the relocation of the CAMHS from a co-located to stand alone service on clinicians? Three core themes emerged for the analysis of interviews with six CAMHS clinicians who had experienced service delivery at both settings. These were: (i) the negative impact of co-location on clients; (ii) physical features of settings; and (iii) social capital.
Clinicians expressed strong views regarding potential negative impact of the co-located service on clients. They argued that by virtue of placing child and adolescent clients in the same setting as adult clients there was increased risk that young clients could witness disturbing behaviour exhibited by unwell adult clients. Clinicians also expressed concern about the potential for CAMHS clients and families to make an association between childhood emotional/behavioural difficulties and progression to severe psychiatric illness. This connection was viewed as being more likely to occur at the old setting where psychiatric services for children and adolescents were located with adult psychiatric services.
There was a strong consensus that physical characteristics of the new setting were better for clients compared with the physical features of the old setting. Clinicians described the new setting as child-friendly and homely. While the physical attributes of the new setting were viewed as facilitating a more positive experience of service delivery for clients and their families, the physical characteristics of the old location were perceived as potentially having the opposite effect. Clinicians expressed their opinions that the old setting was designed for an adult client population and that the building could be frightening and intimidating for younger clients. Some clinicians noted that, in their experience, even visiting professionals felt uncomfortable when coming to the old setting.
Themes related to the social capital available at the older setting reflected the importance of professional social relationships for clinicians. Participants discussed a loss of social connections with adult psychiatric service clinicians as a major disadvantage of the relocation. Clinicians perceived the co-location of adult psychiatric services and CAMHS as helpful for facilitating communication, and sharing of expertise and resources between the two services. In addition to the perceived benefits of social support from clinicians at the old setting, CAMHS clinicians described emotional benefits resulting from more informal social relationships with clinicians at the co-located setting. Despite a sense of loss regarding relationships with adult psychiatric service staff, there was acknowledgement that the relocation had facilitated development of new instrumental social support from mental health clinicians located at a centre within close physical proximity to the new CAMHS.
Methodological limitations
It is important to also acknowledge the methodological limitations of the present study. Not all clinicians who experienced service delivery at the two settings agreed to participate in the research. There may have been some differences of opinion between clinicians who participated in the study and those who chose not to.
Another limitation was that only the clinician perspective was obtained. There was a group of CAMHS clients and their families who experienced service delivery at the old and new settings but their views were not obtained. Due to the nature of the present study, findings cannot be generalized to other CAMHS settings. There is a need to replicate results utilizing quantitative techniques and a representative sample to make conclusive statements about the impact on mental health service delivery of co-located and stand-alone settings across the entire service system.
Implications of the findings
Although the relocation of CAMHS from a co-located setting to a stand-alone setting was perceived as beneficial for clients, the loss of social capital experienced by clinicians was identified as a negative outcome of the relocation. Research consistently indicates the benefits of social and instrumental support for healthcare professionals in the areas of job satisfaction, perceived ability to cope with work demands and emotional wellbeing2-5. The findings of the present study indicate that organizations need to be mindful of possible effects on employees in addition to clients when relocating services from a co-located service delivery model to a stand-alone setting. This study highlighted the importance of strategies such as facilitating development of new professional connections, consultation with staff, and monitoring of employee emotional wellbeing and job satisfaction to assist employees with a successful transition to a new service location.
Clinicians interviewed in the present study speculated about the potential for clients and their carers to draw associations between childhood mental health problems and adult mental illness when the two services were located at the same setting. However, past research clearly indicates that the likelihood of children and adolescents involved in the mental healthcare system progressing into the adult mental healthcare services is small9,10. Therefore, if this view is widely adopted by clinicians and their clients, and evidence suggests it is a myth, then education about this may also be needed.
Although the nature of this research means that findings should not be generalized to other populations, the results may be considered by other rural CAMHS that are currently based at co-located settings. Contemplation of relocation of rural or regional CAMHS from a co-located to a stand-alone setting could be informed by these findings, thus facilitating a smoother transition for clinicians and their clients.
Conclusions and recommendations
This study investigated clinician perspectives of the impact of a rural CAMHS relocation from a co-located setting to a stand-alone service on service delivery. A key finding was that while the relocation was perceived as positive for clients, clinicians experienced a loss of emotional and instrumental social support due to the physical separation of the CAMHS team from the same setting as the adult psychiatric services clinicians. Perceived advantages of the relocation for clients related to the child-friendly, homely environment of the new setting and separation from the adult psychiatric service. Results of the present study provided insight into effects of co-located versus stand-alone CAMHS on service delivery from a group of clinicians who have experienced service delivery from both settings. In conclusion, consistent with the 'National Mental Health Statement of Rights and Responsibilities', CAMHS clients may benefit from service delivery at stand-alone setting, compared with a co-located setting. Importantly, however, the impact of relocation from a co-located to a stand-alone setting on clinicians should be taken into consideration.
References
1. Department of Human Services. An introduction to Victoria's public clinical mental health services, 2006. Available: http://www.health.vic.gov.au/mentalhealth/services/intro-mhservices.pdf (Accessed 10 January 2007).
2. Bradley JR, Cartwright S. Social support, job stress, health, and job satisfaction among nurses in the United Kingdom. International Journal of Stress Management 2002; 9: 163-182.
3. Escriba-Aguir V, Tenias-Burillo JM. Psychological well-being among hospital personnel: the role of family demands and psychosocial work environment. International Archives of Occupational Environmental Health 2004; 77: 401-408.
4. Van Yperen NW, Hagedoorn M. Do high job demands increase intrinsic motivation or fatigue or both? The role of job control and job social support. Academy of Management Journal 2003; 46: 339-348.
5. Wallace, JE, Lemaire J. On physician well being - you'll get by with a little help from your friends. Social Science & Medicine 2007; 64: 2565-2577.
6. Department of Human Services. Planning framework for public rural mental health services, 2006. Available: http://www.health.vic.gov.au/mentalhealth/publications/pubs (Accessed 10 January 2007).
7. Boyd CP, Aisbett DL, Francis K, Kelly M, Newnham K, Newnham K. Issues in rural adolescent mental health in Australia. Rural and Remote Health 6: 501 (Online) 2006. Available: http://www.rrh.org.au (Accessed 6 February 2007).
8. Mental Health Consumer Outcomes Taskforce. Mental health statement of rights and responsibilities, 1991. Available: http://www.health.act.gov.au/c/health?a=dlpol&policy=1150870722 (Accessed 10 January 2007).
9. Smith JA, Osborn M. Interpretive phenomenological analysis. In: JA Smith (Ed.). Qualitative psychology: a practical guide to research methods. London: Sage, 2003; 50-79.
10. Goodrick D. Qualitative research: principles and practice. In: Proceedings, Australian Consortium for Social and Political Research Incorporated (ACSPRI) Workshop. 21-25 January, 2004; Melbourne, Australia; 2004.
11. McLellan E, Macqueen KM, Neidig JL. Beyond the qualitative interview: data preparation and transcription. Field methods 2003; 1: 63-84.



