Introduction
Unequal distribution of physicians has generated much political debate in Japan. Among the 47 prefectures of Japan (administrative regions equivalent to the states of USA or Australia), there exists a more than two-fold gap in the number of physicians per unit population between the highest and the lowest1. Regardless of financial and political support from the national and local governments to distribute doctors equally throughout the entire country, the uneven distribution of physicians has remained unchanged, or worsened2. In other countries, markedly high concentrations of physicians in urban areas and shortages in rural areas have been reported3-6.
It has been assumed that the distribution of doctors is largely dependent on market forces. Over-supply of physicians in urban areas was supposed to create economic competition among them and forced a substantial proportion of them to migrate to rural areas. Therefore, increasing the total number of physicians, which has been attempted in most industrialized countries, has long been considered one solution to this problem7. However, at least in Japan, such a political trial has not resulted in improvement but has led to exacerbation of the existing maldistribution2. A new way to redress the maldistribution of physicians is needed, one that is not dependent on market forces.
Jichi Medical University (JMU) was established in 1972 by the Ministry of Home Affairs and by Japan's 47 prefectural governments. The JMU has two missions to: (i) produce rural physicians; and (ii) distribute them evenly, nationwide. In order to attain these goals, JMU has applied a unique 'home prefecture recruiting scheme' to all JMU entrants8. The JMU recruits two or three high-school graduates per year from each of the 47 prefectures for a total of 100-110 entrants. On matriculation, all students sign contracts with their home prefectures and JMU. As a result, they are fully funded by their home prefectural governments for the entire 6 years of undergraduate medical education at JMU, and they commit to working for medical institutions in their home prefectures for 9 years after graduation. The nine-year obligation includes 3 or 4 years of postgraduate training and 5 or 6 years of rural dispatch. The rural areas to which JMU graduates are sent are determined by each prefectural government, which takes into consideration the demand/supply balance of physicians in the prefecture. Each prefecture office is responsible for checking that all JMU graduates from the prefecture has fulfilled their contractual obligation. Students who breach their contract must pay all their medical school expenses in one lump sum. The total expenses to be paid are 22,600,000 yen ($US183,333) plus 10% per year in interest. After completing the nine-year contract, JMU graduates can choose their workplaces freely. The cumulative rate of JMU graduates who completed the contract among all the graduates is over 95%9.
The uniqueness of the JMU system is derived from a combination of two elements: (i) obligatory rural service; and (ii) home prefecture recruiting. The outcomes of the first element of the JMU system have been reported previously8-10. The percentages of JMU graduates practicing in rural communities (villages, towns or cities) were approximately 13-times (under duty) and 4-times (after duty) higher than those of non-JMU graduates9,11. Also, in other countries (particularly in the USA), the successful outcomes of rural medical education programs have been reported12,13. The outcomes of the US programs were by and large comparable with that of JMU11.
However, the outcomes of the second element of JMU system (ie home prefecture recruiting and service), have not been assessed. The JMU is subsidized equally by the 47 prefectural governments of Japan, and its students are taken equally from the 47 prefectures. Indeed more than 95% of JMU graduates have completed their home prefecture service9, but it is unknown that what proportion of JMU graduates are retained in their home prefectures after the nine-year obligation. Among the retention rates of all prefectures, those of rural or medically underserved prefectures are particularly important for assessing the effectiveness of the equal distribution scheme. The equal distribution element of the JMU system is quite original. There is no other medical school or medical education program similar to JMU in this respect. The JMU is an unprecedented national-level experiment conducted under the cooperation of the Japanese government and local governments. The long-term effects of the equal distribution scheme may thus be beneficial for medical educators and policy makers in countries in which physicians in rural areas are in short supply, and where political interventions to the maldistribution of physicians are sought.
This study followed up all the JMU graduates after their nine-year obligation and assessed whether the home prefectural recruiting system worked effectively in the long term. This study also analyzed personal and prefectural factors associated with long-term retention to home prefectures after the completion of their obligatory work.
Methods
Study design and data collection
This is a retrospective cohort study. The baseline data on demographics, academic performance and other personal information at matriculation and graduation were collected from 1477 subjects who had graduated from JMU by 1991 (ie those who were expected to have completed their contract by 2000). All the baseline data were stored at JMU. Follow-up data were collected on whether the subjects still worked in their home prefectures. The follow-up survey was conducted in July 2000, 2004, and 2006.
Because of the binding and experimental nature of the JMU system, JMU has an administrative section which specializes in longitudinal monitoring of the contract compliance status and workplaces of each graduate. Officials of this section conducted the follow-up survey using a mail survey, and telephone survey when necessary. Follow-up rates were: 98.7% in 2000, 98.2% in 2002, and 98.0% in 2006. Of the 1477 subjects, 69 (4.7%) dissolved the contract, 127 (8.6%) were still under contract due to contract extensions (eg due to prolonging the training period), and 26 (1.8%) could not be followed in at least one of the 3 years. The remaining 1255 (85.0%) graduates who had completed their obligation by 2000, and whose information on workplace address were available for all 3 years, were included as study subjects. Among the subjects, those who worked in their home prefectures in all the 3 years (ie for at least 6 years after the nine-year requirement), were labeled as a 'home prefecture settler' in this study.
Of the baseline data collected, the prefecture of home address at the time of application to JMU was used as home prefecture. Academic rank at entrance was defined as the percentile ranked from the top of the entrance examination (paper test and interview) score. The academic rank at graduation was defined as the percentile from the top of the graduation examination score, or that of the grade point average in the final year when the former score was unavailable.
To evaluate characteristics of home prefectures, data excerpted from the 2004 National Population Census including population size, population density, number of physicians, number of residents who were aged 65 years or older, annual increase in population, number of medical institutions, number of inpatients and outpatients a day in each of the 47 prefectures were merged, through prefectural identification codes, with the baseline data1.
Of all the self-declared specialties registered in the follow-up data, internal medicine, surgery, pediatrics, community medicine, and general medicine were 'primary care specialties', and others were 'specialist subjects'. Those who engaged in any of the primary care specialties in 2000, 2004, or 2006 were 'primary care physicians' and others were 'specialists' in this study.
Statistical analysis
Statistical analyses were carried out using SPSS for Windows v 11.5 (SPSS Inc, Japan). Continuous variables were compared between home prefecture settlers and non-settlers using an unpaired t-test. Categorical variables were compared using the χ2 test or Fisher's exact test. The settlement rate of subjects in each prefecture was calculated as the proportion of settlers among all the subjects from the respective prefecture. Differences in settlement rates among the 47 prefectures were examined with the χ2 test. The associations between home prefecture settlement and various baseline/follow-up variables were examined using logistic regression analysis. The academic backgrounds of father and mother were separately incorporated in the logistic regression models because of their colinearity. For the same reason, academic ranks at entrance and at graduation were also treated separately in the models. Goodness-of-fit was confirmed through the Hosmer and Lemeshow method. Correlations between the settlement rates of all the prefectures and selected demographics of the prefectures were evaluated using Spearman's rank correlation coefficients. All p values shown were two-tailed. P<0.05 was considered statistically significant.
This study was conducted with permission from the Ethics Committee on Epidemiological Studies, Jichi Medical University.
Results
The baseline characteristics of the study subjects are shown in Table 1. Most of the graduates were male (97.5%), from public high schools (87.8%), had postgraduate training based in community hospitals (75.8%), and settled in their home prefectures (69.8%.)
Table 1: Characteristics of 1255 Jichi Medical University graduates who completed their nine-year obligation

The settlement rate of JMU graduates in each prefecture is shown (Fig1). The rates ranged from 45.5% to 93.3%, and the differences among the 47 prefectures were statistically significant (p<0.001.) The population density (Fig2) and physician : population ratio (Fig3) of each prefecture are also shown for comparisons. The settlement rate of JMU graduates tend to be higher in lower population density prefectures or in prefectures with lower physician/population ratio.
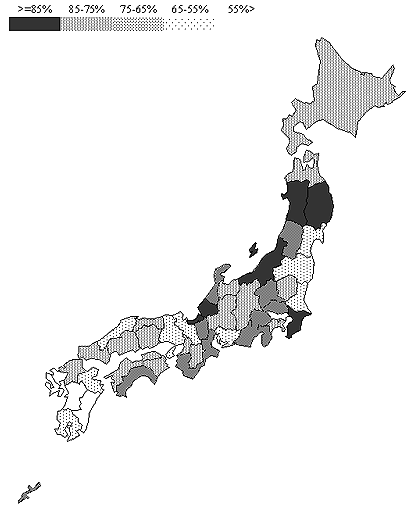
Figure 1: Settlement rate of post-obligation Jichi Medical University graduates in each prefecture.
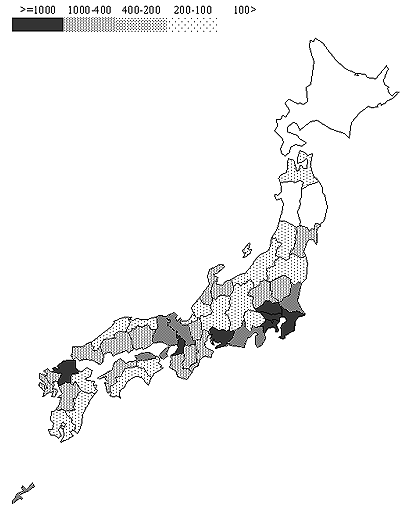
Figure 2: Population density in each prefecture (number of residents/km2).
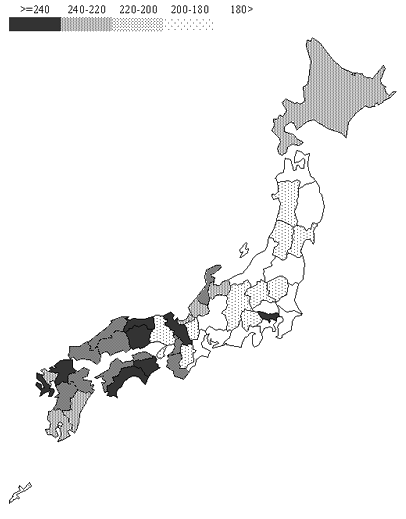
Figure 3: Physician : population ratio in each prefecture (number of physicians/100 000 residents).
Table 2 shows correlations between selected demographic factors and settlement rates of the prefectures. Among the prefectural variables, the number of physicians per 100 000 population (physician : population ratio) and the number of clinics and hospitals per 100 000 population (medical institution : population ratio) were negatively correlated with settlement rate of the prefecture (correlation coefficient -0.34 [p=0.020]; and -0.35 [p=0.017], respectively). The number of outpatient visits per physician a day was positively associated with settlement rate of the prefecture (correlation coefficient 0.32 [p=0.029]). In short, prefectures with a relative shortage of physicians had higher settlement rates.
Table 3 shows the results of univariate analysis comparing personal factors of settlers to those of movers. Home prefecture settlers were less likely to be female (1.7% vs 4.5%, p<0.004) and more likely to be primary care physicians (50.0% vs 32.5%, p<0.001). The academic backgrounds of settlers' mothers were more likely to be lower than those of movers, but the statistical significance was marginal (p=0.05).
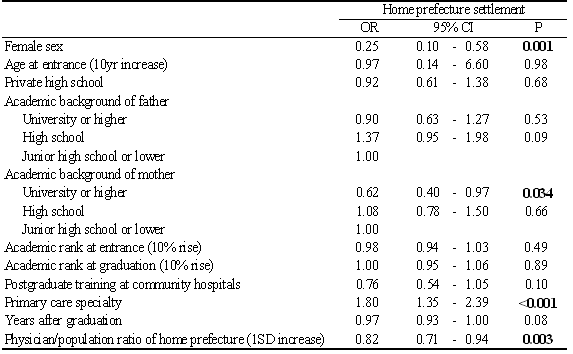
The results of the multivariate analysis are shown (Table 4). As was seen in the univariate analysis, female sex was negatively associated (odds ratio [OR] 0.25 [95% confidence interval {95%CI} 0.10-0.58]) and primary care specialty was positively associated with home prefecture settlement (1.80 [1.35-2.39]). A higher academic background of mother was negatively associated with settlement; when the mothers were university graduates the odds of the subjects for settlement were 0.62 times (95%CI 0.40-0.97) higher than those whose mothers had gone no further than junior high school. Physician : population ratio of home prefecture was also negatively associated with settlement (OR for 1 SD increase 0.82 [0.71-0.94], respectively).
Table 2. Correlations between settlement rates and selected demographics of prefectures (n = 47)
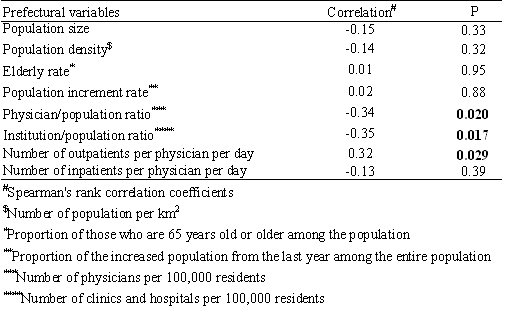
Table 3: Comparisons between those who settled in home prefectures after their 9 year obligation, and those who moved out
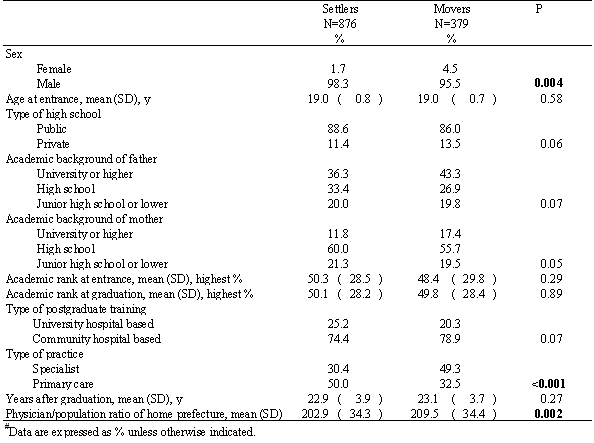
Table 4. Multivariable analysis of factors associated with settlement in home prefectures (n1255)
Discussion
On average, 69.8% of JMU graduates remained in their home prefectures for at least 6 years after their nine-year contractual obligation. According to a cross-sectional nationwide survey conducted by the Ministry of Education, 52.1% of Japanese physicians who had graduated from medical school in 1996 remained in the prefectures in which they attended medical school in 200614. The gap of the values between JMU graduates and the other physicians should be regarded as underestimated when the difference in definitions of retention is taken into account. This study employed a restrictive definition of retention, in which only those who were in their home prefectures at all the three follow-up time points were regarded as settlers. If the definition is made less restricted, the settlement rate rises accordingly. For example, when settlement is defined as being in a home prefecture at least one out of the three time points, the settlement rate of post-obligation JMU graduates rises to 76.3% (data not shown in tables). Although there were substantial gaps in settlement rates among prefectures, the gaps favored JMU's school mission because higher retention rates were achieved in more medically-underserved prefectures.
The higher retention rate of JMU graduates in prefectures that had shortages of physicians and medical institutions was understandable. The governments of these medically underserved prefectures are more likely to require their JMU graduates to work as generalists, and were more keen to persuade them to remain after obligation. Some of these prefectures arrange for jobs in public clinics and hospitals of the prefectures for their JMU graduates, and these jobs are more abundant in such prefectures than in medically over-served prefectures. In contrast, it is likely that the governments of urban prefectures are less keen on such job arrangement for their JMU graduates.
Low supply and maldistribution of physicians have been two of the most serious problems in post-war Japan15. Experience has shown that location of undergraduate medical education in Japan has an impact on practice location after graduation (ie physicians tend to remain in prefectures where they took undergraduate medical education). This empiric rule has led to an ambitious national project called 'One Medical School in Each Prefecture'. In the 1970s the national and local governments decided to establish at least one medical school in each prefecture in the hope of increasing the total number of physicians and distributing them evenly throughout the country16. As a result, 33 new medical schools were established between 1965 and 1980, and the number of newly certified physicians doubled from 3500 to 8200 per year16. The project has indeed succeeded in raising the number of physicians, but the maldistribution of physicians has remained unchanged, or even worsened15,2. One of the reasons for the lack of improvement is that medical schools in some prefectures produced more graduates than was expected. A survey revealed that 70% of medical school graduates in the five most medically underserved prefectures obtained training posts in other prefectures immediately after graduation17.
Because of this, 17 medical schools have now introduced non-contract type 'home quota' systems in which a small proportion of in-prefecture students are admitted with priority and are encouraged to work in the same prefecture18. The government supported this strategy18, and decided to increase capacity by 110 students per year in Jichi, and by 10 students in medical schools in other medically underserved prefectures19. Further, the national government recently announced that it would submit a budget to create 'rural quotas' with an obligatory work period for most of the 80 medical schools in Japan, accommodating 250 new students each year. The government explained that these rural quotas should be similar to the JMU system (ie graduates of the quotas will be obliged to work in their home prefectures for 10 years after graduation, including 6 or 7 years of rural service)20. The JMU graduates account for only 0.7% of all physicians in Japan9; therefore, in spite of the success of its home prefecture recruiting scheme, the impact of JMU on the nation-wide distribution of physicians will be small. However, the current reforms of medical education will dramatically increase the number of the JMU-like programs, and may have substantial impact on the physician distribution in Japan. As these reforms are recent, it is too soon to assess the long-term outcomes. The results of this study will be beneficial to medical schools and policy-makers who are beginning to establish such systems.
The probable reason for women's high attrition rate is marriage. In Japan it is still common for a wife to relocate to her husband's home. It is thus conceivable that a substantial number of female JMU graduates who married men from other prefectures moved from their home prefectures after their obligatory periods. It is also possible that female graduates in rural prefectures tend to move out on their own volition. Some past studies have indicated that female doctors are less likely to practice and live in rural areas than are male doctors, and even if they do practice and live there, they tend to be less satisfied than male doctors21-23. Further studies are needed to analyze the reasons for the gender difference in retention rates.
The high retention rate of graduates with primary care specialties was within our expectation24-27. This is probably due to the nature of primary care, which is more attached to the community in which it is delivered than is specialist care. Continuity of practice is needed more in primary than in specialized care. Primary care physicians thus are more likely than specialists to stay in one place once they have chosen their practice location.
The lower retention rate of physicians whose mothers had more education was surprising. The reason for the result is unknown, but may be related to the assumption that these graduates were from families of higher social class. In modern Japan, social class and income level is well correlated with the educational background of the individual28. Members of higher social classes tend to be more modernized and westernized in their ethos and lifestyle. The physicians whose mothers had a higher educational background might, thus, be more individualistic, have weaker emotional ties to other family members or relatives, and feel less attachment to their home places. Further analysis is needed to test this hypothesis.
There are some limitations to this study. The uniqueness of JMU's obligation system makes interpretation of the results of this study difficult. The JMU graduates are required not only to return to their home prefectures, but also to work in rural areas of the prefecture for 6 or 7 years. The rural experience may affect their retention in their home prefectures, although it is unknown whether this impact is positive or negative. In addition, the 'going home' system of JMU is binding, but the 'home quotas' of most of the other medical schools in Japan, and also most of the similar programs reported from other countries, are not based on any contractual obligation to work in target areas12,13. These programs either might or might not be similarly effective in retaining their graduates in their target areas, compared with JMU. Finally, this study focused on in-prefecture (equivalent to in-state in USA and Australia) retention of physicians, and thus municipality-level (county-level in USA and Australia) retention of the physicians is unknown. Past studies have revealed that various personal and education factors, such as rural background and primary care specialty, influenced the retention of physicians in rural areas10,11,29. These findings are mostly based on municipality/county-level retention studies, and thus cannot be compared directly with the results of this study.
References
1. Statistics Bureau, Ministry of Internal Affairs and Communications. Toukei de miru shikuchouson no sugata [Statistical observations of municipalities]. Tokyo, Japan: Japan Statistical Association, 2005.
2. Kobayashi Y, Takaki H. Geographic distribution of physicians in Japan. Lancet 1992; 340: 1391-1393.
3. Australian Medical Workforce Advisory Committee. The general practice workforce in Australia. (Online) 2000. Available: http://www.healthworkforce.health.nsw.gov.au/amwac/amwac/pdf/gp_2002.pdf (Accessed 12 December 2007).
4. Bureau of Health Professions. Rural health professions facts: supply and distribution of health professions in rural America. Rockville, MD: Health Resources and Services Administration, 1992.
5. Rivo ML, Kindig DA. A report card on the physician work force in the United States. New England Journal of Medicine 1996; 334: 892-896.
6. Bowman R. The world of rural medical education. Available: http://www.unmc.edu/Community/ruralmeded/indexRME.htm (Accessed 12 December 2007).
7. Newhouse JP, Williams AP, Bennett BW, Schwartz WB. Where have all the doctors gone? Journal of American Medical Association 1982; 247: 2392-2396.
8. Inoue K, Hirayama Y, Igarashi M. A medical school for rural areas. Medical Education 1997; 31: 430-434.
9. Inoue K, Matsumoto M, Sawada T. Evaluation of a medical school for rural doctors. Journal of Rural Health 2007; 23: 183-187.
10. Matsumoto M, Inoue K, Kajii E. Characteristics of medical students with rural origin: implications for selective admission policies. Health Policy 2008; 87: 194-202.
11. Matsumoto M, Inoue K, Kajii E. Contract-based training system for rural physicians: follow-up of Jichi Medical University graduates (1978-2006). Journal of Rural Health (in press).
12. Rabinowitz HK. Recruitment, retention, and follow-up of graduates of a program to increase the number of family physicians in rural and underserved areas. New England Journal of Medicine 1993; 328: 934-939.
13. Rabinowitz HK, Paynter NP. The role of the medical school in rural graduate medical education: pipeline or control valve? Journal of Rural Health 2000; 16: 249-253.
14. Ministry of Education, Culture, Sports, Science and Technology. Igakubuigakka sotugyousei no shinrojoukyou chousa [A survey report on medical school graduates]. (Online) 2006. Available: http://www.mext.go.jp/b_menu/shingi/chousa/koutou/029/siryo/06061613/001.pdf (Accessed 4 July 2007).
15. Jichi Medical School. Chiiki-iryo hakusyo [White paper on community healthcare]. Tochigi, Japan: Jichi Medical School, 2002.
16. Ministry of Health, Labour and Welfare. Ishi no jukyu ni kansuru kentoukai houkokusyo [Working party report on national supply of physicians]. (Online) 2006. Available: http://www.mhlw.go.jp/shingi/2006/07/dl/s0728-9c.pdf (Accessed 25 March 2007).
17. Mainichi Shinbun Newspaper. Sotsugyousei no 7-wari ga kengaibyouin ni syuusyoku [70 percent of medical school graduates outflow from their prefectures]. April 5 2007; 2.
18. Ministry of Education, Culture, Sports, Science and Technology. Igakukyouiku no kaizen/juujitsu nikansuru chousakenkyuukyouryokusya kaigi daiichijihoukoku [The first report from the Committee for Improvement of Medical Education]. (Online) 2006. Available: http://www.mext.go.jp/b_menu/shingi/chousa/koutou/029/toushin/07012321.htm (Accessed 4 July 2007)
19. Yomiuri Shinbun Newspaper. Igakubu tenin kei 110nin zou: ishibusoku 10ken to Jichiidai de [110 increase in medical school enrollment: Jichi and ten schools in medically underserved prefectures]. (Yomiuri Online) 31 August 2006. Available: http://www.yomiuri.co.jp/iryou/news/iryou_news/20060831ik08.htm (Accessed 25 March 2007).
20. Yomiuri Shinbun Newspaper. Igakubu ni hekichi iryou waku [Rural quota in medical schools]. (Yomiuri Online) 13 May 2007. Available: http://www.yomiuri.co.jp/iryou/news/iryou_news/20070513ik01.htm (Accessed 25 March 2007).
21. Wilkinson D. Selected demographic, social and work characteristics of the Australian general medical practitioner workforce: comparing capital cities with regional areas. Australian Journal of Rural Health 2000; 8: 327-334.
22. Incitti F, Rourke J, Rourke LL, Kennard M. Rural women family physicians. Are they unique? Canadian Family Physician 2003; 49:320-327.
23. Lee MC, Chou MC. Job and life satisfaction among remote physicians in Taiwan. Journal of Formosan Medical Association 1991; 90: 681-687.
24. Siboni K. Medical graduates (candidates) 1972-2001 from the University of Southern Denmark, Odense, 2nd edn. Geographical supply and distribution, length of study, postgraduate education, specialties and main occupation. Danish Medical Bulletin 2003; 50: 85-89.
25. Igras SM, Franklin RR, Samaha PA, Rice JC. Factors associated with retention of medical school graduates for in-state graduate medical education. Journal of Medical Education 1983; 58: 733-735.
26. Seifer SD, Vranizan K, Grumbach K. Graduate medical education and physician practice location: implications for physician workforce policy. Journal of American Medical Association 1995; 274: 685-691.
27. Burfield WB, Hough DE, Marder WD. Location of medical education and choice of location of practice. Journal of Medical Education 1986; 61: 545-554.
28. Policy Research Institute, Ministry of Finance. Syakai kaisou ishiki ni kansuru kenkyukai houkokusyo [Report on social class and class consciousness]. (Online) 2003; Available: http://www.mof.go.jp/jouhou/soken/kenkyu/zk064/zk064.htm (Accessed 29 April 2008).
29. Brooks RG, Walsh M, Mardon RE, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: a review of the literature. Academic Medicine 2002; 77: 790-798.


