Introduction
Health care provision appears to be going through a defining transition in response to the combined, complex challenges of changing healthcare needs, improving knowledge, advancing technology, increasingly aware patients and chronic workforce shortages. One facet of this transition is that the way that health professionals should work is under pressure to change from a more individualist to a more collectivist approach. That is, healthcare delivery is now increasingly viewed as a team effort, rather than a collection of individual efforts. The quality of care received increasingly depends on the function of teams that may consist of members from several different professions, each contributing their particular expertise, ideally in such a way that 'the total is more than the sum of the parts'. Potential team membership now extends beyond the traditional groups to include newer professional groups, such as physician assistants and allied health therapy assistants1-3; and many health professionals will work in several teams, each with different membership, depending on the clinical task.
If this new vision of interprofessional teamwork is accepted, then it is logical to commence interprofessional activity during the education and training pathways that produce all health professionals. Interprofessional education (IPE) is currently defined as follows: 'Interprofessional Education occurs when two or more professions learn with, from and about each other to improve collaboration and the quality of care'4. However, while this definition may be easy to embrace philosophically and has a reasonably strong theoretical base5, there is as yet only limited evidence of success6. While education research design often poses challenges to proving effectiveness of any educational intervention, it may also be that converting IPE theory to action and outcomes is much more challenging at the level of educational design. Questions remain to be answered about just how to develop genuine interprofessional engagement, when in a curriculum to schedule interprofessional activities, and where to do it. An important question to ask is: are we expecting too much of IPE activities, particularly at undergraduate level? This article addresses these contextual and educational design issues, with a particular focus on how to achieve meaningful, high quality IPE in rural practice settings.
Contextual issues
Healthcare practice in rural and remote communities may be an ideal context in which learners can observe and participate in sound interprofessional clinical practices. Smaller, close-knit communities tend to have smaller, close-knit teams of health professionals consisting of both resident and visiting members, sometimes reliant on communications technology. Team members tend to know each other well and work together often. Many are relatively isolated professionally from their peers and so have to rely on each other more for professional support, often through active communication networks based on continuing professional development activities. Most are generalists and roles tend to blur at the margins as people just do what has to be done in a mutually supportive way. This is, of course, an idealized view because poor teamwork can happen anywhere; but as there are few alternatives to team membership in smaller communities, it is in the interests of all team members to work out how to work well together.
Rural health has been the context for some of the more pioneering IPE developments in Australia. The first multi-professional rural students' club was established in 19917, and now every Australian health professional education institution has one, albeit with varying membership of specific health professions. These clubs are student-led, and therefore are not necessarily well integrated with formal curricula, but they almost certainly achieve some degree of mutual awareness of professions and roles, in addition to increasing positive impressions of rural careers8. Further developments in rural IPE are likely, however, to require substantial effort from academic staff and their institutions9.
How?
Designing any IPE course or activity should follow the same educational design principles required for any educational activity10. The goal in IPE is ensure all learners are prepared and able to work in multi-professional teams in their future careers. A key strategy for achieving this is to expose learners to successful interprofessional teams of people who understand and respect each others' roles, and demonstrate sound healthcare outcomes that depend on teamwork. Role modeling is known to be a powerful influence on the development of individual learners11-12, and should be equally effective for teams of individuals learning how to work together. Precursors to this role modeling may well include knowledge and understanding of what roles the different professions can offer to teams, and respect for both the professional roles and contributions made by individuals within the teams. As for any important educational program, IPE learning objectives should be assessed, and results should contribute to pass/fail decisions if learners are to take it seriously13.
The limited impact of IPE activity may reflect flaws in design and implementation of IPE. For example, IPE is often managed by a different group to that responsible for the participating courses, thereby limiting its recognition as an integral part of each course. The function of the team of faculty who develop IPE activities has been shown to be a key to success14. If managed separately, IPE is then often provided as an additional, non-core curriculum component, rather than as a common strand integrated into the curricula of all participating health professional courses. One consequence may be that IPE sessions require additional attendance that conflicts with demands of the core curricula, part-time employment or other personal issues. In addition, IPE is often delivered as a predominantly theory-based course, with mostly lectures and seminars, when recent evidence shows that participation in clinical IPE activities improves achievement of learning objectives15. Further, there is a strong belief in placing together learners in all available health professions because the theory is common to all. However, this usually means large class sizes and significant logistic problems that may reduce the impact. Still further, when small group activities are planned, there is a mistaken assumption that these activities will foster teamwork in later professional life. The business and organizational psychology literature is full of examples of how to create effective teams, and there is general agreement that successful teams do not happen until relevant individuals are brought together for specific tasks16. One likely interpretation is that there may be no such thing as generic teamwork skills. The message is that learners should be in 'clinically relevant' small groups that reflect future professional tasks, rather than convenience or ideology. Finally, IPE is infrequently assessed in a way that failure to engage prevents progress, and students can choose to participate to a very minimal level, or perhaps not at all.
There are disturbing anecdotal reports that IPE sometimes reinforces negative attitudes to professional teamwork. Hence the stakes are high and 'getting it right' is a high priority. Some principles for improving the educational design of IPE activities have been elucidated10 and, although challenging to implement, are feasible.
When?
Interprofessional education should be regarded as a vertical curriculum theme throughout the entire curriculum of each participating professional course, at both undergraduate and postgraduate levels. As with any vertical theme, it could be debated that basic knowledge should come before experience, or vice versa, a replication of the debates about problem-based learning. There is little evidence to support either approach. What may be more important is that the approach to IPE is consistent, combines imparting of knowledge, development of understanding, role modeling by successful examples and experience in clinically relevant teams, with scope for variation in sequencing and timing. It may be logical to start early in all curricula; however it may be more important to mould IPE into the participating curricula in a way that best suits the goal. It is easier with postgraduate learners to develop clinically relevant teams with genuine clinical tasks; however senior undergraduate learners can still do this with appropriate supervision.
Where?
The more acute inpatient areas, such as emergency departments, operating theatres and intensive care units are difficult to use for IPE. Even though these often provide the best examples of inpatient interprofessional teamwork, it is possible that the involvement of more junior learners in clinical care could compromise patient safety. Hence, student IPE participation in these areas should be focused on observation and analysis of acute care teamwork. Indeed, many urban hospitals are becoming too acute and too busy for meaningful involvement of undergraduate students17. Participation in clinically-focused IPE sessions may be more easily managed in ambulatory care settings. There are many possible examples of such activities in both inpatient and ambulatory settings, as listed in Table 1 and detailed further elsewhere10.
Table 1: Examples of ideal clinical tasks for interprofessional education student learning
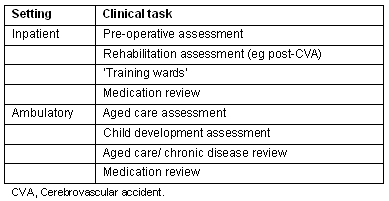
One of the major advantages of rural health care is that all of the inpatient and ambulatory tasks listed in Table 1 are often accessible within the local healthcare environment. Non-resident healthcare team members tend to visit the local health centre or hospital, which is also a base for video-conferencing and other communications technology. There is much less division between inpatient and ambulatory care, and generally the same individuals work in both contexts. Patients are more often discharged from urban hospitals for postoperative care closer to home, providing access to patients with a wide range of common and interesting conditions. Home visits are simpler to arrange. Students can more easily interact with the entire health professional team, both resident and visiting, by simply following patients through healthcare episodes. Students from different professions can, therefore, work together more often around a range of tasks, potentially developing a model of teamwork much closer to that required in later careers.
Conclusion
Health professionals should be exposed during training to effective professional teamwork that enhances the quality of patient care, but effective IPE has so far proven difficult to implement. There is, however, some evidence to guide the design of IPE activities. Early course content can include some theory, but the emphasis should be on role-modeling and engaging students in effective interprofessional health care. Clinical placements should include assignment to small, 'clinically relevant', multi-professional teams that conduct, and are assessed on, clinical tasks that contribute to improving patient care. Rural practice may be an ideal environment in which to provide a wide range of clinical tasks relevant to IPE, because learners in rural placements can more easily follow patients and work across professional boundaries on clinical care pathways.
References
1. O'Connor TM, Hooker RS. Extending rural and remote medicine with a new type of health worker: physician assistants. Australian Journal of Rural Health 2007; 15: 346-351.
2. Lin IB, Goodale BJ. Improving the supervision of therapy assistants in Western Australia: the Therapy Assistant Project (TAP). Rural and Remote Health 6: 479. (Online) 2006. Available: http://www.rrh.org.au (Accessed 30 April 2008).
3. Stirling CM, O'Meara P, Pedler D, Tourle V, Walker J. Engaging rural communities in health care through a paramedic expanded scope of practice. Rural and Remote Health 7: 839. (Online) 2007. Available: http://www.rrh.org.au (Accessed 30 April 2008).
4. Centre for the Advancement of Interprofessional Education. Defining IPE. (Online) 2002. Available: http://www.caipe.org.uk/about-us/defining-ipe/ (Accessed 1 December 2007).
5. Hammick M. Interprofessional education: concept, theory and application. Journal of Interprofessional Care 1998; 12: 323-332.
6. Hammick M, Freeth D, Koppel I, Reeves S, Barr H. A best evidence systematic review of interprofessional education: BEME Guide no 9. Medical Teacher 2007; 29: 735-751.
7. Hays RB, Acklin F, Chan P, Davis A, McAllister L, Murphy B et al. The University of Sydney Rural Careers Project. Australian Journal of Rural Health 1993; 1: 23-25.
8. Turner JV, Scott LM. University rural health clubs: nurturing the future Australian rural workforce. Rural and Remote Health 7: 649. (Online) 2007. Available: http://www.rrh.org.au (Accessed 30 April 2008).
9. Smith T, Stone N, Bull R, Chesters J, Waller S, Playford D et al. Australian Rural Health Education Network's position on interprofessional education and practice in health care. Rural and emote Health 7: 866. (Online) 2007. Available: http://www.rrh.org.au (Accessed 30 April 2008).
10. Hays RB. Interprofessional education in the community: where to begin. The Clinical Teacher 2007; 4: 141-145.
11. Lublin JR. Role modeling: A case study in general practice. Medical Education 1992; 26: 116-122.
12. Kenny NP, Mann KV, McLeod H. Role modeling in physicians' professional formation: reconsidering an essential but untapped educational strategy. Academic Medicine 2003; 78: 1203-1210.
13. Newble DI, Jaeger K. The effect of assessments and examinations on the learning of medical students. Medical Education 1983; 17: 165-171.
14. Stalmeijer RE, Gijselaers WH, Wolfhagen IHA, Harendza S, Scherpbier AJJA. How interdisciplinary teams can create multi-disciplinary education: the interplay between team processes and educational quality. Medical Education 2007; 41: 1059-1066.
15. Morison S, Jenkins J. Sustained effects of interprofessional shared learning on student attitudes to communication and team working depend on shared learning opportunities on clinical placement as well as in the classroom. Medical Teacher 2007; 29: 464-470.
16. West M. Effective teamwork. Oxford: Blackwell, 2004; 27-48.
17. Olsen LG, Hill SR and Newby DA. Barriers to access to patients in a group of teaching hospitals. Medical Journal of Australia 2005 183: 461-463.
Abstract
Interprofessional education (IPE) has been suggested as an answer to improving the effectiveness of health professional teamwork, which in turn is regarded as a key strategy for improving the delivery and outcomes of increasingly complex healthcare approaches. There is a strong theoretical base to support the implementation of IPE for all health professionals, and in response many training programs now do this, although in a wide variety of ways. There is, however, little evidence so far that IPE has the desired effect, and one reason for this may be the design of the IPE learning activities. This article presents some theory-based but practical advice for how to develop effective IPE activities. The focus is on rural practice, which is an ideal location for IPE because small teams must work together in small communities to provide optimal health care.
Key words: education, interprofessional education, multidisciplinary.
You might also be interested in:
2010 - Building capacity for acute care in developing countries
2007 - Long term regional migration patterns of physicians over the course of their active practice careers

