Introduction
There is a shortage of doctors in rural practice across the developed world1-3. The professional and social isolation that accompanies a rural placement is seen as unattractive, and the maintenance of professional skills and development is also an issue4. Furthermore, increased or perceived increased hours of work combined with dependence on locum cover to allow annual leave is unappealing in a society where lifestyle is as important as professional satisfaction5.
Why some individuals choose rural practice is less clear than the issues that instigate a departure from rural medicine. Previous exposure to a rural environment appears to be pivotal. Those who originate from a rural area are most likely to return to work there5. Time spent in rotation as an undergraduate also appears to be influential6. The influence of exposure is possibly related to an increased ability to integrate into the community. This community integration with opportunity for development of personal interests is vital; those individuals and families who struggle to do so being much more likely to leave the rural area7,8. Professionally, some practitioners are attracted to the truly general nature of the job and the satisfaction of providing continuity of care9.
To date, most research into remote and rural recruitment and retention has been conducted in Australia, the US and Canada. While there may be some similarities, differences in training and recruitment of medical students across countries, as well as cultural, social and geographical differences, mean that these studies are unlikely to identify all of the factors relevant to local settings. Thus, work is required to identify the aspects of rural exposure that may influence the take up of rural practice in other, usually smaller, countries.
Scotland makes up one-third of the UK land mass and has one-tenth the population. The Highlands of Scotland have a population density of 8 per km2 compared with the UK norm of 246 people per km2, and accounts for one-fifth of the Scottish population (approximately 1 million people). Although the remote areas of Scotland, and indeed those of other UK regions, are geographically less isolated than some of the remote communities in Australia and Canada, the same problems with recruitment and retention of healthcare professionals apply1-3,10. These difficulties are reflected in applications for posts in the early stages of medical training. Recent Medical Training Application Service (MTAS) documentation revealed that the NHS Education for Scotland (NES) North Deanery (which consists of Grampian, Highland, Shetland, Orkney and Western Isles) is the least popular in the country. Furthermore, general practice training data for specialist training (ST) posts indicates that, of Grampian, Moray and Highland, Highland is the least popular place to train (K Walker, Education Director, NES, North Deanery, pers. comm., 2007).
This pilot study looks at the determinants of fourth-year medical students studying at the University of Aberdeen, Scotland, opting for an extended remote and rural placement within a degree program where all students must take at least one 5 week remote medicine rotation. As this extended option was new, faculty was also keen to review the performance of the first cohort of students to ensure quality control of the teaching and learning.
Thus, the aims of this pilot study were twofold. First, to identify student factors, including perceived benefits, which contributed to the students self-selecting for an innovative, extended remote and rural placement, and their experience of this placement. Second, it was aimed to compare student performance with their outcomes from the previous year of medical school (3rd year).
Methods
Setting
Aberdeen University Medical School is spread over two campuses: Foresterhill in Aberdeen and Raigmore Hospital in Inverness. Students spend their first 3 years exclusively in Aberdeen. The 4th year consists of 9 clinical blocks, each lasting 5 weeks, covering all major specialities. Eight of these are within the hospital and the ninth is in general practice. All 4th year students are given the opportunity to go to Inverness for one clinical block, in order to experience medicine in an alternative environment.
The extended remote and rural option was introduced in 2006. This allowed 14 students to gain wider experience of rural medicine by completing all nine 4th year clinical blocks in the Highlands. The majority of clinical teaching took place in Inverness but each student also carried out a general practice placement in a remote and rural location. Block co-ordinators at Raigmore Hospital were requested to provide students with at least one specific remote and rural experience in each of the other eight blocks.
Data collection
In the absence of prior UK empirical work, we selected a mixed methods approach to data collection.
First, students were asked to complete a brief, 5 point Likert scale questionnaire, to help identify the student and teaching program factors which lead students to opt for an extended rural option. The questionnaire (Table 1) was developed on the basis of discussion with the key stakeholders in the remote and rural option. Demographic details were collected from students, including gender, place of birth and environment of origin11. Questions followed on student perceptions of the experience, specifically whether they felt they had received a 'remote and rural experience', and if this had influenced their choices for foundation year posts.
Second, in the absence of prior UK empirical work, we selected qualitative methodology (focus group) to explore why students selected the placement, their experiences of it, and their views of remote and rural medicine generally. We chose a focus group because they are able to generate data regarding perceptions, values and beliefs and can be particularly useful as group participants act as challengers, supporters and negotiators12. The group setting can make people more confident in sharing information13.
Finally, we also examined routine assessment data. The cohort of students who selected the extended option undertook the same end-of-year degree examinations as the other 4th year students. Thus we looked at the students' performance in the end-of-year examinations, and compared these with their 3rd year exam results.
Note that assessment marks are collected in the form of the common assessment scale (CAS), a 21 point scale from 0 to 20, used for all assessments at the University of Aberdeen to allow students to compare more easily their level of performance in different courses. On the scale 9 represents the minimum level of performance needed to pass and 20 indicates the best performance which can be expected from a student at the relevant level. The CAS is not a linear scale.
Participants
Fourteen students who had reached the end of the extended remote and rural option were invited to participate in the study. Invitations and information outlining the study background and purpose, and the commitment required, were sent by email. The students were told that they did not need to give a reason for declining to participate, and there would be no penalty for doing so.
Analysis
The focus group was taped, transcribed verbatim, and analysed using grounded theory14. Analysis was carried out by JC, using an inductive, data-based approach.
The software SPSS for Windows, v 15.0 (SPSS Inc; Chicago, IL; USA) was used for quantitative data storage and analysis. Questionnaire data were analysed using descriptive statistics. The cohort's 3rd and 4th year assessment marks were compared using marginal homogeneity tests. Marks were compared with similar assessments. Medians and inter-quartile ranges are presented for these data.
Ethics permission
The North of Scotland Research Ethics Committee stated that full ethics permission was not required for the study. However, to ensure ethical assurance, written, informed consent for data collection and publication of anonymous data was obtained from all participants.
Results
Fourteen (8 female and 6 male) students completed the extended option and all students took part in the study. The students were slightly older than the year mean, with an average age of 23 years compared with the year average of 21 years. The majority were not originally from Scotland, and most were from major cities or urban centres (classified using the Scottish Executive Urban/Rural classification). Two of the 14 students had a partner. Both partners were from a rural area. The students had had a mean of three remote and rural trips to remote GPs, or to clinics in the Islands, Caithness or Fort William.
Questionnaire data
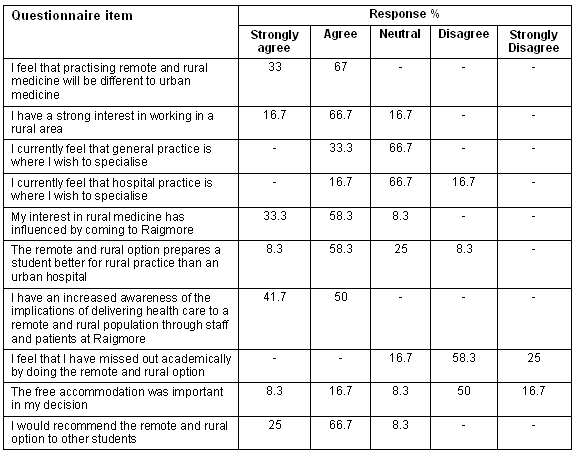
Students on the remote and rural extended option expressed the view that the practice of remote and rural medicine was different from that of urban medicine. Most had a strong interest in working in a rural area. Most did not have definite plans about a future choice of specialty, but did have a slight preference for general practice. Their placement had influenced their interest in rural medicine. Most agreed that the extended option had prepared them better for rural practice. All students agreed or strongly agreed that they had an increased awareness of the implications of delivering health care to a remote and rural population as a result of the extended option. Most did not think they had missed out academically by being away from the main campus (but see later for the focus group data). All but one of the students said that they would recommend the experience to other students (Table 1).
Table 1: Student questionnaire responses
Focus group data
Analysis of the focus group data identified four main themes relating to the students' decision to opt for the extended remote and rural option:
- The reputation of the teaching
- To experience remote and rural medicine
- A change from Aberdeen
- Lifestyle.
The reputation of the teaching: The quality of teaching in Inverness was a significant draw for the participants. It was apparent that students had been encouraged by students a year or two ahead of them to have 'as much time as possible in Inverness'. Smaller teaching group size was an attraction. There was no consensus as to why the teaching was better, other than it was felt that perhaps they were more a part of the team simply because there were fewer of them, they were known by the tutors, and thus the individual feedback they received was more meaningful. The relationships formed meant that the students felt that they adopted a professional mindset and were more aware of 'not disappointing' their tutors (Fig1).
Experience remote and rural medicine: The students regarded the practice of medicine in the Highland and Islands of Scotland as different from that delivered in urban environments, and this had been confirmed by their experiences over the year. Their views of remote and rural practice were positive, due mostly to feeling part of a community health team and part of the wider community (Fig1). Inverness itself, a small city, was not viewed as remote or rural, and they seemed to have a rule of thumb that more than approximately 50 miles (80 km) north of the city counted as remote. Many of the students had chosen the extended option so that they could gain experience of living and working in a remote and rural area on their GP placement. Many of them had spent a large proportion of their life in large cities and were keen to experience life in other settings.
A change from Aberdeen: Some of the students expressed a wish for a change from a large teaching hospital to a smaller district general hospital, so they could experience another hospital. Many of them were also keen to live somewhere else, having spent several years in Aberdeen (Fig1). This had a negative side also: they were no longer part of university life or living in a university city, thus they missed the social aspects of university life. Students also worried about not being as prepared for the end-of-year exams as their colleagues in Aberdeen. Their impression was that 4th year students in Aberdeen had been studying much more than they had. This seemed due to a feeling that, while they had gained more clinical experience than their Aberdeen colleagues, they had had less time for book learning as they were too tired to study after a full clinical working day (Fig2).
Lifestyle: The 'healthier and more out-doorsy' lifestyle of the Highlands was an attraction. Many of the participants were involved in clubs at the university, such as the mountaineering club and the Wilderness Society, and these interests had been fuelled further by spending the year in Inverness (Fig1).

Figure 1: Focus group data - positive aspects of the extended placement.

Figure 2: Focus group data - less positive aspects of the extended placement.
Outcome data: academic performance
The students involved in this experiment were a self-selected group with a wide range of academic abilities. This was reflected in their third-year, end-of-year exam results, which showed that their average mark varied from 10.8 (pass) to 17.2 (very good).
Analysis of routine assessment databases indicated that the students' assessment outcomes in 4th year (ie at the end of the extended option) were consistent with their previous years' marks. There was no significant difference in performance across the 3rd year and 4th year in terms of the following comparisons: 3rd year OSCE (median [M] 14; IQR 13-16) and 4th year OSCE (M 14; IQR 13.75-15.5) (p = 0.79); the 3rd year special study module (M 16; 15-17) and the 4th year ethics assessment (M 17; IQR 15.75-17.25) (p = 0.10); the first of two 3rd year written exams (A: M 13.5; IQR 10.75-15.5) and the 4th year written exam (M 12; IQR 10.00-14.25) (p = 0.10); or the second 3rd year written exam (B: M 12; IQR 9.75-16.00) and the 4th year written exam (M 12; IQR 10.00-14.25) (p = 0.49). Comparison of 3rd year (M 14; IQR 12.34-15.25) and 4th year average marks (M 14; IQR 12.83-15.91) also identified no significant differences in performance (p = 0.48) over time, although the cohort's average CAS mark rose from 14 in 3rd year to 14.3 in 4th year. This reflects a pattern seen in for the year as a whole (14 to 14.4).
Discussion
The results indicate that the extended remote and rural option offered was a valuable and academically successful experience for the cohort of 4th year students who participated. The students reported that they had enjoyed, and benefited from, the intimacy of working and learning in a district general hospital and a remote and rural general practice. They had positive attitudes to remote and rural medicine, and remote and rural lifestyles.
In terms of outcomes, the students' performances were consistent with their marks from the previous year (3rd year) on all forms of assessment. Thus, while their fears about not having done as much book study as their Aberdeen colleagues may well have been accurate, this did not affect their performance in the end-of-year exams. However, their perception of better clinical teaching did not translate into an improved performance on OSCE exams. Other local work has indicated that students' performances on written exams and clinical assessments remain reasonably consistent across time15.
The mixed methods approach we used in this small study proved useful. While most students responded that they did not think they had missed out academically by being away from the main campus in the questionnaire, this issue was raised by the students themselves in the focus group as a possible disadvantage to opting for the extended placement.
We see this small study as having several main important outcomes. First, medical students who spent all of 4th year off the main campus on the one-year remote and rural placement did not suffer academically. Second, the cohort maintained their interest and enthusiasm for long-term remote and rural practice, as demonstrated by all but one student stating that they would recommend it to other students. Furthermore, it was clear in the focus group discussion that even at this early stage of training, participants did regard remote and rural medicine as different from urban medicine, even in a relatively small country such as Scotland. This has implications for training doctors throughout the UK and in smaller European countries with distinct rural communities.
It does seem, however, that we were preaching to the converted. Those students who choose the extended remote and rural option were those who had an existing interest in this aspect of medicine, as has been identified in previous studies6-9. How we attract those without an existing interest is likely to require more ingenuity. It is unclear from the existing literature if this has been examined in other studies - how do we make remote and rural medicine attractive to those who have never considered it an option? Furthermore, our results may not be generalizable to other UK medical schools who offer remote and rural rotations or placements because much of the students' decision-making was based on the good reputation of teaching at the Inverness campus and the lifestyle benefits of living in the Scottish Highlands and Islands.
Interestingly, while previous research has found that students who originate from remote and rural areas are more likely to return to work there5, most of our cohort of students were not originally from Scotland, and most were from major cities or urban centres. It may be that ensuring all students experience remote and rural medicine at undergraduate level attracts students from urban backgrounds to such practice. We need to carry out longitudinal research on all our students (ie not only the small cohort who selected the extended option) to see how the take up of remote and rural training places and practice compares across our medical students and those from UK medical schools who do not offer even brief remote and rural rotations.
This pilot study presents only the short-term outcomes of a remote and rural extended option delivered by the University of Aberdeen Medical School. Thus, we are unable to comment on whether this extended option influenced student selection for training posts, or choosing the Highlands and Islands as a place to live and work long term. We hope to follow up this cohort, and their successors, to examine long-term and monitor short-term outcomes. Such a longitudinal database should also provide information which may aid selection of participants for future cohorts. We believe our results are of interest to those designing methods of teaching delivery that might attract medical students to remote and rural medicine in the UK.
Acknowledgements
The authors thank Professor Malcolm Laing, Associate Dean for Undergraduate Medicine (Inverness) for supporting this research; thanks also to Professor Amanda Lee, Head of Statistics, Public Health, University of Aberdeen, for her advice on analysis.
References
1. Tholl WG. Rural and Remote Healthcare in Canada. Presentation to Standing Social Committee on Social Affairs, Science and Technology, 31st May 2001. (Online) no date. http://www.cma.ca/multimedia/staticContent/HTML/N0/l2/working_on/Kirby/rural.pdf (Accessed 7 August 2008).
2. Australian Institute of Health and Welfare. Medical Labour Force 2004. National health labour force series no 38. Canberra, ACT: Australian Institute of Health and Welfare, 2006. Available: http://www.aihw.gov.au/publications/hwl/mlf04/mlf04.pdf
3. British Medical Association Board of Science. Healthcare in a rural setting. London: BMJ Publishing Group, 2005. Available: http://www.bma.org.uk/ap.nsf/Content/healthcarerural.
4. Richards HM, Farmer J, Selvaraj S. Sustaining the rural primary healthcare workforce: survey of healthcare professional in the Scottish Highlands. Remote and Rural Health 5: 365. (Online) 2005. http://www.rrh.org.au/assets/article_images/article_print_365.pdf (Accessed 5 August 2008).
5. World Organisation of Family Doctors (WONCA) working party on rural practice (2001). Policy on rural practice and rural health. (Online) 2004. Available: www.globalfamilydoctor.com (Accessed 5 August 2008).
6. Williamson M, Gormley A, Bills J, Farry P. The new rural health curriculum at Dunedin School of Medicine: how has it influenced the attitudes of medical students to a career in rural general practice? The New Zealand Medical Journal; 116 (1179). (Online) 2003. Available: http://www.nzma.org.nz/journal/116-1179/537/ (Accessed 5 August 2008).
7. Mayo E, Mathews M. Spousal perspectives on factors influencing recruitment and retention of rural family physicians. Canadian Journal of Rural Medicine 2006; 11: 271-276.
8. Cutchin MP, Norton JC, Quar MM, Bolt D, Hughes S, Lindeman B. To stay or not to stay: issues in rural primary care physicians' retention in Eastern Kentucky. Journal of Rural Health 1994; 10: 273-278.
9. James R, Cormack D, Dowell A. Rural General Practitioners: 1999 Survey part 4: analysis of specific sub-groups. New Zealand Medical Journal; 118(1028). (Online) 2005). Available: http://www.nzma.org.nz/journal/118-1208/1256/ (Accessed (Accessed 5 August 2008).
10. Temple J. Securing future practice: shaping the new medical workforce for Scotland. Report of a Short Life Working Group Commissioned by the Scottish Executive. (Online) 2004. Available: http://www.scotland.gov.uk/Publications/2004/06/19454/38410 (Accessed 5 August 2008).
11. Eley D, Baker P. Does recruitment lead to retention? Rural Clinical School training experiences and subsequent intern choices. Remote and Rural Health 2006; 6: 511. (Online) 2006. Available: http://www.rrh.org.au/assets/article_images/article_print_511.pdf (Accessed 5 August 2008).
12. Stringer E. Action research in education. Upper Saddle River, NJ: Pearson Education, 2004.
13. Farquhar C. Are focus groups suitable for 'sensitive' topics? In: R Barbour, J Kitzinger (Eds). Developing focus group research: Politics, theory, and practice. London: Sage, 1999; 47-63.
14. Strauss A, Corbin J. Basic of qualitative research: grounded theory procedures and techniques. London: Sage; 1998.
15. Cleland JA, Milne A., Sinclair HK., Lee AJ. Predicting performance cohort study: is performance on early MBChB assessments predictive of later undergraduate grades? Medical Education 2008; 42: 676-683.

