Introduction
Healthcare funding is an important issue in developing countries. The healthcare sector is one of India's largest public sectors in terms of revenue and employment, with approximately one-fifth of public expenditure1.
In recent times, India has experienced a steady decline in infant mortality and also in some major communicable diseases, such as hepatitis and poliomyelitis among infants. These improvements have helped the Indian population increase at an annual rate of 2%2. In July 2007, of India's population of 1 027 015 247 (males: 531 277 078 and females: 495 738 169), some 300 million were living on less than one dollar per day (below the poverty line)3. The overall situation in healthcare facilities in India is unfavorable, especially for the economically disadvantaged4. It has often been stated that public healthcare is a basic service that will assist in combating poverty
In spite of economic growth and demographic transition, the Indian healthcare system is burdened by a rise in infectious and chronic degenerative diseases6. Infectious, contagious and waterborne diseases such as dengue fever, diarrhea, typhoid, viral hepatitis, measles, malaria, tuberculosis, whooping cough and pneumonia are major contributors to disease, especially among poor and rural Indians2. Communicable diseases once thought to be under control (eg dengue fever, viral hepatitis, tuberculosis, malaria, and pneumonia) are still in existence in India, having reappeared with high levels of drug resistance, to the disadvantage of the poor2,4. The wealthy and middleclass sectors of Indian society have better access to public/private healthcare facilities and are less affected2-4,6.
India's healthcare infrastructure has failed to keep pace with the nation's economic growth. Emerging market conditions and a poor public healthcare system has encouraged a shift from public to private healthcare4, with private healthcare facilities now constituting more than 80% of healthcare expenditure, including that of those who are poor1,7. Ranson found that the burden of such high expenditure on private healthcare had catastrophic effects on the household financial situation of those who are poor8.
It has been shown in developing countries that existing public healthcare facilities are most effective for the poor4. India has an existing widely distributed public healthcare system but it is ailing and unresponsive6. Indian policy-makers complain of a lack of funds needed to manage the public healthcare system. However it has been shown that problems in healthcare financing can be solved in a number of ways, such as a community based health insurance scheme8. However, the Indian public healthcare system suffers from problems other than financial9. It is important to explore these other contributing factors, and identify major issues that may be corrected, subject to budgetary constraints.
It is has been established that the number of public health facilities in India is inadequate2. A national study identified that the majority of the population (urban 46% and rural 36%) mainly use private doctors or clinics, with only 16% visiting public and private hospitals10. The same study identified that urban Indians prefer private hospitals, while the rural population prefers public healthcare facilities10. However, the reasons for healthcare users not utilizing existing public healthcare facilities has not been determined.
Millennium development goals (MDG), particularly MDG 3 and 5 (promote gender equality and empower women; and improve maternal health, respectively) emphasized the healthcare of women. Women and their children are more frequent users of healthcare facilities than men11,12 and, apart from the provision of basic medical care, Indian health planning has concentrated on maternal and child health and family planning services9. It is therefore important to analyze the opinions of women regarding the quality of public healthcare facilities. Using a nationally representative sample, the current study has attempted to examine women's reasons for non-utilization of public healthcare facilities (supply of healthcare) according to the type of healthcare they are seeking (demand for healthcare).
Indian National Family Health Survey
The Ministry of Health and Family Welfare of the Government of India initiated the National Family Health Surveys (NFHS) to provide reliable, quality data on population and health indicators. Following NFHS-1 (1992-1993) and NFHS-2 (1998-1999), NFHS-3 (2005-2006) has recently been completed.
Methods
The present study used secondary data from the Indian NFHS-3. A large number of women (n = 124 385) of reproductive age (15-49 years) were interviewed from India's 29 member states of.
NFHS-3 sampling and data collection
Fieldwork for NFHS-3 was conducted in two phases from November 2005 to August 2006. In the first phase, fieldwork was conducted in 12 states (Andhra Pradesh, Assam, Chhattisgarh, Delhi, Gujarat, Maharashtra, Meghalaya, Orissa, Punjab, Rajasthan, Uttar Pradesh, and West Bengal), with the second phase being conducted in the remaining 17 states (Arunachal Pradesh, Bihar, Goa, Haryana, Himachal Pradesh, Jammu and Kashmir, Jharkhand, Karnataka, Kerala, Manipur, Madhya Pradesh, Mizoram, Nagaland, Sikkim, Tamil Nadu, Tripura, and Uttaranchal). The 2001 population census was used to determine the sample size of each area.
The initial targeted sample size (for completed interviews) was 4000 ever-married (married at any time in their lives) women in states with a population of more than 30 million; 3000 ever-married women in states with a population between 5 and 30 million; and 1500 ever-married women in states with a population of less than 5 million. The NFHS-3 followed a uniform sample design procedure using probability proportional to population size (PPS). Rural sample selections were made in two stages: (i) the selection of Primary Sampling Units (PSUs; villages) with PPS; and (ii) random selection of households within each PSU. The urban sample selections were made in three stages: (i) selection of PSUs (municipal wards) with PPS; (ii) random selection of one census enumeration block (CEB) from each PSU; and (iii) random selection of households within each selected CEB. A more detailed description of the sampling procedure is available in the NFHS-3 final report 200710.
Questionnaire
The NFHS-3 was intended to provide information on important emerging health and family welfare issues. It was also intended to provide essential state- and national-level data for improved monitoring of health and family welfare programs and policies implemented by the Ministry of Health and Family Welfare and other ministries and agencies. The NFHS-3 used three types of questionnaires: the household questionnaire; the women's questionnaire; and the men's questionnaire. The questionnaires provided detailed data on: women's background, reproductive history, use of family planning methods, fertility preferences, antenatal and delivery care, child care and nutrition, child mortality, adult mortality, awareness of and precautions against sexually transmitted diseases, AIDS, marriage and sexual behavior, empowerment and social indicators, domestic violence and healthcare.
Dependent variables
The respondents were asked why they did not utilize public healthcare facilities when members of their households were ill, identifying their reasons with a yes/no choice. Five reasons for non-utilization of public healthcare were offered: (i) 'there is no nearby facility'; (ii) 'facility timing is not convenient'; (iii) 'health personnel are often absent'; (iv) 'waiting time is too long'; and (v) 'poor quality of care'.
Independent variables
The study attempted to identify the services sought by the respondents. The respondents were asked to indicate their reasons (yes/no response) for visiting public healthcare facilities for the following 11 services types: family planning, immunization, antenatal care, delivery care, postnatal care, disease prevention, self medical treatment, treatment for child, treatment for other person, growth monitoring of child, and health check-up.
Respondents' demographic characteristics collected included: age, residential area, education, economic status and standard of living. Age was collected as a continuous variable and then modified into a categorical variable with seven groups at 5 year intervals (15-19 years, 20-24 years etc). Residential areas were indicated as either rural or urban. Economic status was categorized according to a wealth index ranging from 'poorest' to 'richest' (poorest, poorer, middle, richer and richest). Respondents' standard of living was categorized as low, medium or high.
Wealth index is a widely used measurement of economic status used to ascertain the equity of health programs in publicly or privately provided services. The main objectives of a wealth index are to measure ability to pay for health services and the distribution of services among the poor. The wealth index used in India was introduced by Rutstein and Johnson13 and includes any item that may reflect economic status, specifically most household assets and utility services, including country-specific items.
Statistical analyses
To control for confounders, independent associations between dependent and independent variables were assessed using logistic regression. The magnitude and direction of associations were expressed as odds ratios (OR). Due to the large size of the sample, a significance level of p<0.001 was used in all analyses.
Results
The majority of the women in India (58%) said that their family members did not use public healthcare facilities, and this was because: there were no nearby facilities (27%); service times were inconvenient (9%); health personnel were often absent (5%); waiting times were too long (17%); and the care was of poor quality (32%).
Among the 118 777 women respondents, 54% lived in rural areas; 53% had secondary or higher education; 25% were poor; 55% were rich; and 52% had a high standard of living. The women's demographics and their reasons for non-utilization of public healthcare facilities follow.
Age
Women aged 15-29 years were approximately 1.5 times more likely than the reference group (45-49 years) to say that there were no nearby public health facilities, and the quality of care in the public health facilities was poor.
Residential area (rural/urban)
Women in urban areas were 1.26 times more likely than those in rural areas to say that there were no nearby healthcare facilities, 1.13 times more likely to say that the service times in public facilities were inconvenient, approximately twice (1.82 times) as likely to say that the waiting time was too long, and 1.21 times more likely to say that public healthcare facilities were of poor quality. However, only 4.4% (OR = 0.66) of women in urban areas agreed that health personnel were often absent (Table 1).
Table 1: Participants' demographics according to opinion category regarding non-utilization of public healthcare facilities
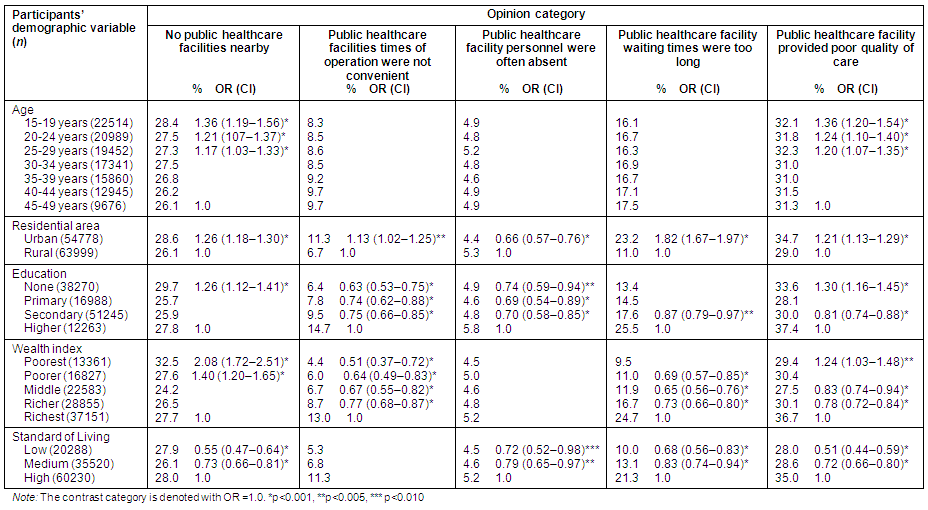
Education
Of the 38 270 women who had no education, only 6.4% agreed that service times of public healthcare facilities were inconvenient, and 4.9% agreed that health personnel were often absent. Women with no education were 1.26 times more likely than the richest women to agree that there were no nearby healthcare facilities, and 1.30 times more likely to agree that the quality of public healthcare was poor (Table 1).
Of those women who had primary education, 7.8% agreed that service times of public healthcare facilities were inconvenient, and only 4.6% agreed that health personnel were often absent.
Women who had secondary school education were less likely than those with higher education to agree that the service times of public healthcare facilities were inconvenient (OR = 0.75), health personnel were often absent (OR = 0.70), the waiting time was too long (OR = 0.87), and the quality of care was poor (OR = 0.81).
Wealth index
The poorest people were more likely than the richest to say that there were no nearby public healthcare facilities (OR = 2.08) and were 1.24 times more likely to agree that the quality of care in public healthcare facilities was poor (Table 1).
Of all the people in the 'poorer' category, only 6% (OR = 0.64) agreed that the service times of public healthcare facilities were inconvenient, while 11% (OR = 0.69) agreed that the waiting time was too long. In this category, women were 1.4 times more likely to agree that there were no nearby public healthcare facilities. Women belonging to the 'middle' wealth index, were less likely than the 'richest' women to agree that the service times of public healthcare facilities were inconvenient (OR = 0.67), waiting time was too long (OR = 0.65), and the quality of care in public health facilities was poor (OR = 0.83). Women in the 'richer' range were less likely than those in the 'richest' range to agree that the service times of public healthcare facilities were inconvenient (OR = 0.77), the waiting time was too long (OR = 0.73), and the quality of care was poor (OR = 0.78).
Standard of living
Women with a low standard of living were less likely than those with a high standard of living to agree that there was no nearby facility (OR = 0.55), the health personnel were often absent (OR = 0.72), the waiting time too long (OR = 0.68), and the quality of care was poor (OR = 0.51). Women with a medium standard of living were less likely than those with a high standard of living to agree that there was no nearby facility (OR = 0.73), health personnel were often absent (OR = 0.79), the waiting time was too long (OR = 0.83), and the quality of care was poor (OR = 0.72).
Service seeking
As reported, women who did not use the public health service for the immunization of children were less likely (OR = 0.85) to agree that the waiting time was too long (Table 2). Women who did not use the public health service for the delivery of care were less likely (OR = 0.60) to agree that health personnel were absent.
Women who did not seek the service of disease prevention, were 1.52 times more likely to agree that the waiting time was too long, and were 1.43 times more likely to say that the quality of care was poor.
Women who did not seek self medical treatment from public health services were less likely to agree that there were no nearby facilities (OR = 0.88), service times of public healthcare facilities were inconvenient (OR = 0.84), the waiting time was too long (OR = 0.80) and the quality of care was poor (OR = 0.84).
Women who did not seek child medical treatment from public health services were less likely to agree that there were no nearby facilities (OR = 0.84), the waiting time was too long (OR = 0.78) and the quality of care was poor (OR = 0.80).
Women who did not seek another person's treatment from public health services were less likely to agree that the waiting time was too long (OR = 0.81) and the quality of care was poor (OR = 0.80).
Women who did not seek child growth monitoring service from public health services were less likely to agree that the service times of public healthcare facilities were inconvenient (OR = 0.49) and the waiting time was too long (OR = 0.70).
Women who did not seek health check-up service from public health services were less likely to agree that there were no nearby facilities (OR = 0.81), the service times of public healthcare facilities were inconvenient (OR = 0.69), health personnel were often absent (OR = 0.78), the waiting time was too long (OR = 0.74) and the quality of care was poor (OR = 0.89).
Table 2: Participants' opinion category regarding non-utilization of public healthcare facilities according to service seeking
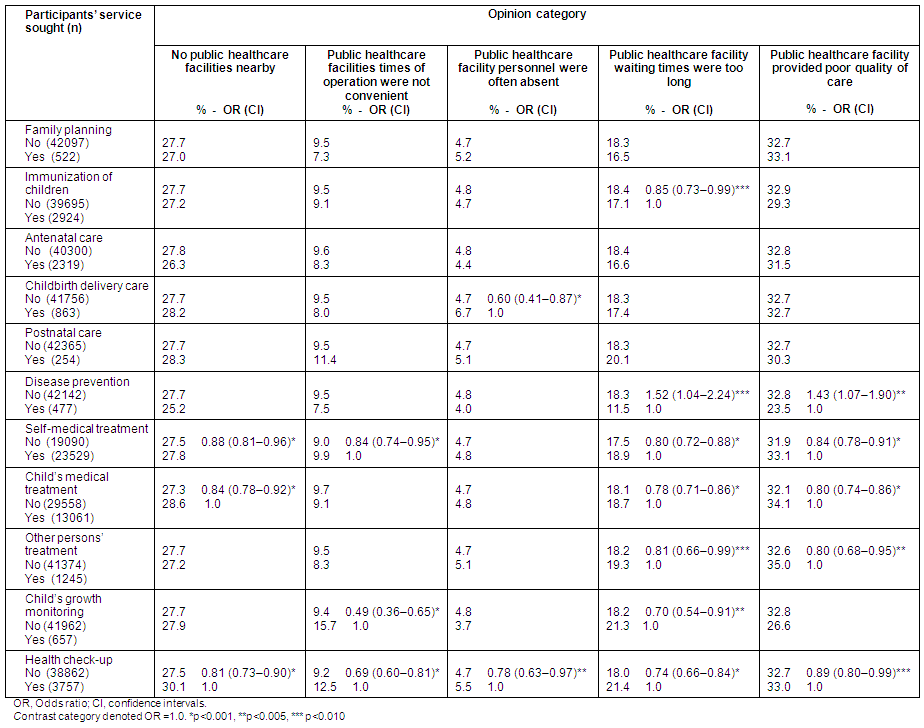
Discussion
The majority of Indian families do not use public healthcare facilities. The study indicates some important relationships between non-utilization of public healthcare, demographics and the demand categories (service seeking) of public healthcare. For instance, when mothers sought public health services for immunization of their children, they found that waiting times were too long or health personnel were absent. Service seeking for respondents' self-medical treatment and health check-ups emerged as a strong predictor for identifying the drawbacks associated with public health facilities (except for the absence of healthcare personnel).
This study is probably the first to identify the inadequate supply of public healthcare according to basic demand categories (service seeking) in the Indian context using users' opinions. Because the study analyses data from a nationally representative sample, its outcomes should be considered in any reform of the Indian public healthcare system, especially concerning distance to public healthcare outlets and the quality of care provided.
An earlier study from India's Madhya Pradesh identified disparities between the healthcare facilities in rural and urban India2. The current study concurs with this, using a nationally representative sample. Urban Indian women report a number of problems in using public healthcare facilities. They found the service times to be inconvenient, which could be due to urban women's increased likelihood of being occupied with household activities during the day when public healthcare facilities are open. It is therefore recommended that the opening hours of public healthcare facilities be revised, according to the convenience of users. Urban women also reported longer waiting times than rural women, which could be a perception influenced by their greater time pressure related household activities. Alternatively, the higher population density associated with urban public clinics may increase urban women's sense of urgency to leave the clinic. Increased urban population density may also lead to higher expectations of public health facilities, which result in perceptions of poor quality care.
However rural women are concerned about the frequent absence of healthcare staff, and this may be the result of 75% of healthcare infrastructure (including medical personnel and other resources) being concentrated in urban India where less than one-third of the population lives14. With rural Indians experiencing two-fold barriers to public healthcare (fewer healthcare facilities and lower presence of medical staff), the government should increase the number of rural health clinics and provide improved regulation of staff presence. Greater administrative follow up and a higher concentration of patients using rural clinics may also ensure the compulsory presence of healthcare staff.
Respondents' education, economic status and standard of living emerged as significant predictors for non-utilization of public healthcare facilities. Higher education, economic status and standard of living indicate greater dissatisfaction with public healthcare facilities. Therefore, it is recommended that attention is given to the distribution public healthcare facilities and the convenience of their opening times. Improved use of these services may also be encouraged by the application of stringent rules for the presence of staff, and effective planning to reduce waiting times.
Consideration of demands for public healthcare (categories of healthcare service seeking) yielded some interesting findings. Public services sought for child immunization, child growth monitoring, and treatment and health check-ups for family members were affected by perceived long waiting times and/or poor quality of care at public facilities.
Public healthcare delivery was repeatedly perceived as affected by an absence of staff. In India, economically disadvantaged mothers usually deliver babies in the traditional way, without the assistance of ineffective public healthcare or expensive private health facilities. This situation was also described in a Zambian study that found ineffective healthcare facilities resulted in low use of maternal healthcare services15, and an Indian study that found poor quality healthcare is likely to reduce its utilization16. Low usage of public services childbirth care may impact on maternal health problems, including the high rate of maternal mortality17. This important issue in resource-poor settings is reflected in the UN MDGs concerning the reduction of maternal mortality18. In this context, Mavalankar and Rosenfield analyzed healthcare policies using examples from rural India and recommended the expansion of professional roles to improve the supply of healthcare18. However, the present study recommends greater investment in public healthcare facilities and regulation of staff presence, the availability of convenient opening times and an improvement in the quality of care.
WHO's World Health Report 2006 and others have identified a shortage of qualified staff in public health sectors, especially in developing countries6,19,20. Therefore, policy-makers are encouraged to ensure the regular presence of health personnel, and their optimal use in meeting MDGs. To reduce maternal and child health issues, careful monitoring of policies relating to waiting times for service users, the redistribution of healthcare facilities and improvement in service quality is advised.
The present study has some limitations, including the use of a cross-sectional design to assign causality. In addition, the study examined public healthcare problems using only 5 categories (dependent variables). In acknowledgement of the many other problems existing in the system, the inclusion of other 'problem' variables (such as maternal healthcare) is recommended for future studies. The results of this study can, however, be used to influence policy-making in India because it used representative samples from all states.
Almost a decade ago (in 1999) an overview was made of health equity in India21,22, with the marked difference in health status of those in rural and urban areas linked to poverty, social status and the disproportionate growth of health infrastructure. It has been argued subsequently that withdrawing public money from healthcare facilities used by those who are economically disadvantaged results in increased out-of-pocket payments, which ultimately creates more poverty23. And in the absence of effective, affordable public healthcare facilities, it has been found that the poor (especially poor rural populations) are likely to consult with 'quacks' or traditional health practitioners, which ultimately extends their period of morbidity24. With the findings of the present study highlighting public health services as inconvenient, unfriendly and ineffective, the Indian poor and rural populations are likely to face medical poverty traps and prolonged morbidity.
Conclusion
The current study concludes that the redistribution of public healthcare facilities will help address established rural disadvantage. In addition, user-friendly opening times, the regular presence of staff, reduced waiting times and improved quality of care are necessary steps to assist in reducing morbidity and poverty in India.
Acknowledgements
The authors acknowledge the Ministry of Health and Family Welfare, Government of India and Measure DHS for their permission to use the data; and Gloria Macassa for her comments on the manuscript.
References
1. National Sample Survey Organization. NSS 60th Round. New Delhi: Govt. of India, 2006.
2. Healthcare in India. Emerging market report 2007. (Online) 2007. Available: www.pwc.com/globalhealthcare (Accessed 29 July 2008).
3. Dollar D. Globalization, poverty, and inequality since 1980. The World Bank Research Observer 2005; 20(2): 145-175.
4. Duggal R. Poverty & health: criticality of public financing. Indian Journal of Medical Research 2007; 126: 309-317.
5. Castro-Leal F, Dayton J, Demery L, Mehra K. Public spending on healthcare in Africa: do the poor benefit? Bulletin of the World Health Organisation 2000; 78(1): 66-74.
6. De Costa A, Diwan V. Where is the public health sector? Public and private sector healthcare provision in Madhya Pradesh, India. Health Policy 2007; 84: 269-276.
7. Government of India. National Health Accounts of India 2001-2002. New Delhi: Ministry of Health and Family Welfare, 2005.
8. Ranson MK. Reduction of catastrophic healthcare expenditures by a community-based health insurance scheme in Gujarat, India: current experiences and challenges. Bulletin of the World Health Organisation 2002; 80(8): 613-621.
9. Qadeer I. Healthcare systems in transition III. India, Part I. The Indian experience. Journal of Public Health Medicine 2000; 22(1): 25-32.
10. Government of India. National Family Health Survey (NFHS) III (2005-06), India Report. Bombay: International Institute for Population Sciences, 2007.
11. Haas J. The cost of being a woman. New England Journal of Medicine 1998; 338: 1694-1695.
12. Mustard CA, Kaufert P, Kozyrskyj A, MayerT. Sex differences in the use of healthcare services. New England Journal of Medicine 1998; 338: 1678-1683.
13. Rutstein SO, Johnson K. The DHS wealth index. DHS Comparative Reports no. 6. Calverton, MD: ORC Macro, 2004.
14. Patil AV, Somasundaram, KV, Goyal, RC. Current health scenario in rural India. Australian Journal of Rural Health 2002; 10(2): 129-135.
15. Stekelenburg J, Kyanamina S, Mukelabai M, Wolffers I, van Roosmalen J. Waiting too long: low use of maternal health services in Kalabo, Zambia. Tropical Medicine and International Health 2004; 9(3): 390-398.
16. Rani M, Bonu S, Harvey S. Differentials in the quality of antenatal care in India. International Journal for Quality in HealthCare 2008; 20(1): 62-71.
17. Maine A, Rosenfield A. The safe motherhood initiative: why has it stalled? American Journal of Public Health 1999; 89(4): 480-482.
18. Mavalankar D, Rosenfield A. Maternal mortality in resource-poor settings: policy barriers to care. American Journal of Public Health 2005; 95(2): 200-203.
19. WHO. The World Health Report 2006 - working together with health. Geneva: WHO, 2006.
20. WHO. Human Development Report 2005. New York: United Nations Development Program, 2005.
21. Anon. Equity raises questions. Health Millions 1999; 25(2): 10-1.
22. Anon. Equity in health - an overview. Health Millions 1999; 25(2): 2-5.
23. Chinai R. Getting healthcare to vulnerable communities. Bulletin of the World Health Organization 2005; 83(11): 804-805.
24. Dalal K, Rahman A. Out-of-pocket payments for unintentional injuries: a study in rural Bangladesh. International Journal of Injury Control and Safety Promotion 2008; 8: 1-7.
Abstract
Introduction: This article examines women's opinions about their reasons for the non-utilization of appropriate public healthcare facilities, according to categories of their healthcare seeking in India.
Methods: This cross-sectional article uses nationally representative samples from the Indian National Family Health Surveys NFHS-3 (2005-2006), which were generated from randomly selected households. Women of reproductive age (15-49 years) from the 29 states of India participated in the survey (n = 124 385 women). The respondents were asked why they did not utilize public healthcare facilities when members of their households were ill, identifying their reasons with a yes/no choice. The following five reasons were of primary interest: (1) 'there is no nearby facility'; (2) 'facility timing is not convenient'; (3) 'health personnel are often absent'; (4) 'waiting time is too long'; and (5) 'poor quality of care'.
Results: Results from logistic regression analyses indicate that respondents' education, economic status and standard of living are significant predictors for non-utilization of public healthcare facilities. Women who sought the services of care delivery and health check-ups indicated that health personnel were absent. Service seekers for self and child's medical treatments indicated that there were no nearby health facilities, service times were inconvenient, there were long waiting times and poor quality healthcare.
Conclusions: This study concludes that improving public healthcare facilities with user-friendly opening times, the regular presence of staff, reduced waiting times and improved quality of care are necessary steps to reducing maternal mortality and poverty.
Key words: India, National Family Health Surveys, public healthcare, women's health.
You might also be interested in:
2020 - Organophosphate exposure and the chronic effects on farmers: a narrative review
2012 - Maternal rib fracture after manual uterine fundal pressure
2005 - The quality of procedural rural medical practice in Australia

