Introduction
There is a critical shortage of doctors in rural Australia1,2. In response to this, the Australian Government supported South Australia's Flinders University to develop the Flinders University Parallel Rural Community Curriculum (PRCC). The PRCC was the first community based medical education program in Australia to teach a full academic year of medicine based in rural general practice, and was constructed on the hypothesis that increased rural practice exposure during undergraduate medical education would influence students to pursue a rural career path3-11.
The PRCC is undertaken by medical students for the entire third year of their four-year graduate entry medical program at Flinders University. The first cohort of eight students commenced in 1997 in the Riverland region of South Australia. At the time this was a radical departure from the standard medical curricula in Australia, where accepted practice was for medical students to undertake only short 2-6 week rural clinical placements.
The PRCC places are open to rural and urban applicants. In order to gain a PRCC place, students apply voluntarily and are selected by interview. Between 50% and 60% of PRCC places are filled by rural background students annually.
The PRCC has been considered an outstanding academic and workforce success12-16. However, there is no data on how the PRCC exerts this workforce effect. The success of the initial program has resulted in replication of this approach to other rural regions of South Australia. In 2008 there were 30 medical students participating annually in PRCCs across four rural regions of South Australia.
The graduates in the present research undertook their PRCC placements in the Riverland and the Greater Green Triangle regions of South Australia. This research explores how the PRCC has influenced their career choices as graduates of the program.
Methods
Between 1997 and 2005 a total of 98 students had participated in the PRCC. By 2007, all these students had graduated and were working as doctors.
A comprehensive search for current contact details of all graduates was undertaken. This included searches of alumni data bases, websites and telephone directories, rural doctor workforce agencies, medical registration boards and local contacts. This resulted in 86 graduates being contacted with an invitation to participate in this research.
A retrospective survey of all contactable graduates of the PRCC was undertaken in 2007. Those surveyed were between one and 9 years post-graduation.
Ethics approval was granted by the Flinders University Social and Behavioural Research Ethics Committee.
Definition of rurality
Within Australia there is no agreed definition of 'rural'. In this study, the Rural, Remote and Metropolitan Areas (RRMA) classification system was used, as is used by the Australian Medical Workforce Advisory Committee (AMWAC) in its national medical careers longitudinal studies17. In this research 'rural' was defined as 'a regional city or large town, a smaller town or a small community'17, which included the RRMA 3-7 classifications. This definition of rural was used to determine the study participants' current training or practice location, identification of self and spouse as having a rural background, and self-identification as being on a 'rural career pathway'.
Definition of rural career pathway
In this research, rural career pathway is defined as the intention or actual practice in a rural area as described in the definition of rurality. The PRCC graduates in intern training were asked to self-identify as being on a rural or urban career pathway, that is the intention to undertake further training or practice in an urban or rural area. Graduates in vocational training or vocationally qualified were assumed to be on a rural career pathway if they were practising in a regional city or large town, a smaller town or a small community, which included RRMA 3-7.
Survey design and administration
Survey questions were based on known factors that may be associated with rural medical career choice1,3-10,17-24. All questions relating to geographic location were based on previously validated questions used in the AMWAC national medical careers longitudinal studies17. The survey was conducted either by telephone interview or on-line completion using Perseus Software Solutions, according to the preference of the participant. Telephone interviews were recorded and transcribed, and the transcript was returned to the interviewee for verification. The survey instrument was piloted with the 2007 cohort of PRCC students who were not included in the research sample. The pilot resulted in changes to one question.
Anonymity was maintained because each responder was given a unique identifier at the point of submission of the survey at the central IT repository of the Flinders University Rural Clinical School.
Analysis
The data set was exported into SPSS 14.0 for Windows v14 (SPSS Inc; Chicago, IL, USA; www.spss.org) and QSR International NVIVO v7(QSR International; Melbourne, VIC, Australia; www.qsrinternational.com) for analysis. Statistical data were analysed using t-tests with Fisher's exact test. Content analysis was used to identify themes that emerged from the qualitative data, and to construct conclusions about the meanings in the text.
Results
Responses were received from 49 of the 86 graduates invited to participate. Three respondents did not identify a definite career choice. These responses were removed from the analysis, resulting in useable data from 46 respondents, which represented a 53% response rate. The representativeness of the responders to the whole cohort is strengthened because the gender balance of responders and non-responders was similar, and a search of records identified a comparable rural/urban background ratio of responders and non-responders. The age profile of responders and non-responders was between 19 and 53 years.
Analysis found that 54% of respondents indicated they were on a rural career pathway. These respondents were equally divided between those with a rural background and those with an urban background. A further 24% of survey respondents identified as having a rural background reported being on an urban career path. These respondents reported that limited rural options influenced them to practise in a non-rural location. The remaining 22% of respondents identified as having an urban background and being on an urban career path.
Data on the specialty choice of graduates were analysed by career stage (internship, vocational training, fully qualified) and career pathway (Table 1). In Australia, medical graduates intending to pursue a career in any specialty, including general practice, must undertake further formal training (known as vocational training) in an accredited training program.
Table 1: Specialty choice of graduates by career stage and career pathway
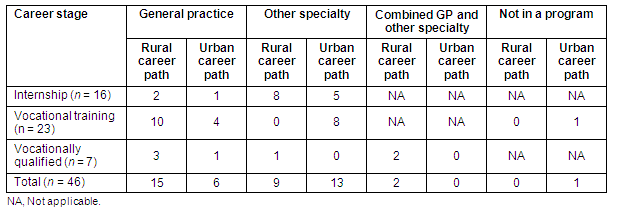
The PRCC graduates in intern training were asked to self-identify as being on a rural or urban career pathway. Only two graduates (12%) in internship reported choosing general practice and being on a rural career pathway, while eight graduates (50%) reported choosing a career specialty other than general practice and being on a rural career pathway. Conversely, in vocational training (the next stage of training) graduates in a general practice vocational training program were more likely to be on a rural career pathway than graduates in any other specialty training program (p = .003).
Data were analysed to identify when graduates made their definitive career choice (Table 2). A positive relationship existed between being on a rural career pathway and making the decision prior to or during medical school (p = 0.027). There were no significant associations for graduates on an urban career pathway and making the decision prior to or during medical school. A positive relationship existed between graduates in vocational training on an urban career path and making their decision on career specialty after graduation from medical school (p = .004). There were no significant associations for graduates in internship or those who were fully qualified and when they made their career choice.
The literature identifies rural background as the predominant variable influencing a rural career choice, along with undergraduate rural exposure18-20,24. Further analysis of graduates' career pathway choice (rural/urban) and geographic background (rural/urban) was conducted to construct a four quadrant (Q) model (Fig1). The distribution of survey respondents among the quadrants was similar. This was unexpected. Therefore, further analysis of the data was undertaken to explore the characteristics of graduates in each quadrant (Table 3).
Table 2: Graduates' time of career choice, by career stage and career pathway
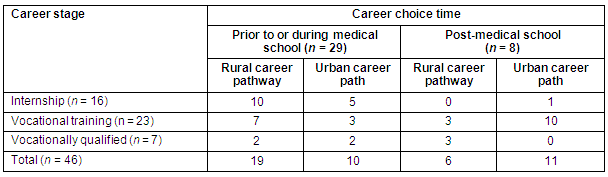

Figure 1: The four combinations of graduate background and career pathway choice.
Table 3: Data clusters in each of the four quadrants
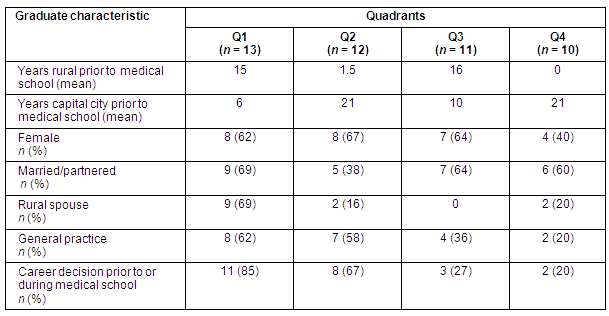
Analysis of data in each quadrant
Quadrant 1. Rural background and rural career pathway: Respondents in Q1 were predominantly female (n = 8/13; 62%) and nine (69%) were either married or in a partnership. A positive relationship was found between these respondents (all rural origin) and having a rural spouse (p = 0.002), with 100% of partners identified as rural origin. The Q1 respondents had lived in small communities for a long period of time (mean years = 15) prior to admission to medical school. The Q1 respondents reported family relationships (returning to family, children and partner needs) as influencing their career location choice. Eight had chosen general practice as their specialty choice (62%). The Q1 respondents were more likely to make a career decision either prior to or during medical school than were non-Q1 respondents (p = 0.034). Twelve respondents (92%) reported that the PRCC experience confirmed their existing career decision. Reported PRCC program positive influences were rural clinical mentors and the rural general practice experience. The Q1 respondents said:
There really wasn't any consideration of not taking a rural training pathway. I would never see myself as working in the city. I don't want to sound condescending of city GPs it is important but it's not what interests me. R12
Decided on rural general surgeon or Obs & Gyn as opposed to rural GP which I think is because of my positive exposure to specialists. R28
I was affected personally by the past influence of living in a rural town and my family prefers to live in a small rural town. R36
Quadrant 2. Urban background and rural career pathway: Respondents in this quadrant were again predominantly female but the majority, 7 (62%) were single. There were no single males in this quadrant. Eleven (92%) of Q2 respondents had an almost entirely city based background prior to entry to medical school, with a median of 21 years lived in a capital city. Seven (58%) had chosen general practice as their specialty choice and 8 (67%) made their career specialty decision during medical school. Respondents reported as influential in career decision-making: the extended rural general practice experience, small hospital experience, patient interaction, opportunities for skill building, and rural specialists. Personal reasons influencing their career choices concerned the themes: dislike of cities, dislike of city hospitals, wanting to be close to friends, preference for a rural lifestyle despite coming from an urban background. The Q2 respondents said:
GP training promised to be intellectually stimulating and diverse, it also seemed like a good 'lifestyle' choice, as it is easier to work part time, choose convenient hours etc. R58
It [the PRCC] showed me the benefits of general practice and the ability to practise obstetrics in a meaningful way, rather than 'shared care' in the city. R57
I wanted to work in a smaller friendly hospital. I decided rural GP was for me. R42
Quadrant 3. Rural background and urban career pathway: The majority of respondents in this quadrant were female. None of the 7 partnered graduates in this quadrant had a partner with a rural background. These respondents lived in small communities for a long period of time (median years = 16) prior to admission to medical school. More of these respondents chose a career specialty other than general practice (7 vs 4, respectively) and eight (73%) reported making their specialty decision after graduation from medical school. Seven respondents (63%) reported as influencing their choice of vocational training program: limited rural pathway options or limiting choices related to lifecycle stage, such as working conditions, flexibility of and length of time to complete training programs. The Q3 respondents said:
There isn't a rural pathway for psychiatry; there are various rural options when I finish. R10
A rural tract in the geriatric psychiatry program didn't exist. I have created one as part of my fellowship. R19
Currently have no choice of location as in rotational training program which sets my roster and training locations. No opportunity for rural anaesthetics training in South Australia. R37
There is no rural pathway but there is the opportunity to do rural rotations. There will be rural aspects to it as there will be future opportunities for rural rehab as it is an expanding field both in the city and country. R55
Quadrant 4. Urban background and urban career pathway: This is the only quadrant in which the gender split was biased towards males (6 vs 4, respectively). All respondents in this quadrant lived in a capital city for all of their life prior to medical school. The majority (80%) were undertaking a specialist career other than general practice, and the majority (80%) made their career specialty decision after graduation from medical school. Influences affecting career decision-making in this quadrant were more likely to be family, such as children's schooling and spouse employment, rather than personal preferences. Half of this quadrant's respondents reported having limited rural career options, and training program constraints. The Q4 respondents said:
I decided to pursue a surgical career following my surgical experiences in the PRCC, very positive. R35
Ultimately [my] vocational choice is primarily one of professional interest. At this point my location is governed 100% by vocational training opportunities. No rural pathway offered. R47
It [the PRCC] did result in an increased interest in rural issues and although I am not based rurally, I visit rural South Australia each week for work and this is likely a result of PRCC increased interest. R11
Discussion
The distinctive clustering that emerged from the data resulted in each quadrant being re-named: (Q1) 'The True Believers'; (Q2) 'The Convertibles'; (Q3) 'The Frustrated'; and (Q4) 'The Metro Docs'. This led us to the development of a new model called the Four Qs Model (Fig2) which may be a useful model to test for predictability in further studies.
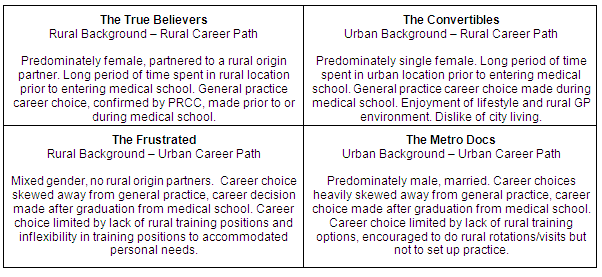
Figure 2: The Four Qs Model (PRCC, Flinders University Parallel Rural Community Curriculum).
The concordance of these data with previously published data on career choice3-11 is encouraging, given the small sample size. The literature supports the findings that medical graduates with a rural background and a spouse with rural background are more likely to choose rural general practice (The True Believers)3,7,8,16.
New information is contained in the analysis of The Convertibles who report the extended rural undergraduate experience as influencing them to undertake a rural career path, despite a city based upbringing. This is important for curriculum planners to understand, and further research is recommended in this area.
Of concern is the number of rural background graduates identified as The Frustrated who report barriers to undertake training to follow a rural career pathway. This requires further investigation on a larger scale because it has implications for postgraduate training providers and rural scholarship holders.
The Metro Docs appear to be influenced by the PRCC experience differently from the other PRCC graduates, choosing different specialties and making this decision later in their careers. This may still be seen as a positive outcome of the rural based program because these city doctors may have more empathy with rural patients and referrals from rural doctors as a result of their rural experiences.
Limitations
The small sample size combined with the low response rate exerts a limiting effect on the validity of the results. Limitations could result from a self-selection bias of students because the researcher was known to the study participants who were volunteers in this research. In addition, because this research was undertaken in one medical school, caution should be used in generalising findings to other institutions.
Conclusions
The PRCC was established in 1997 as an intervention to help address the rural doctor workforce shortage. That over half responding PRCC graduates in this study were on a rural career path supports the results of previous PRCC outcome studies that found the PRCC is helping to address the rural medical workforce shortage.
Importantly, many graduates in this research reported being frustrated in their endeavours to undertake rural-based postgraduate training programs. This emphasizes the need to establish more rural career pathways for current graduates, and for the planned increase in medical graduates in 3 years time. Additional rural postgraduate training places, including rural internships, coordinated by Rural Clinical Schools, would build on the successful undergraduate community based educational programs, such as the PRCC, to significantly reduce the Australian rural doctor workforce shortage.
Equally important are the urban background respondents who selected a rural career path. These respondents (named The Convertibles) provide valuable insights into the experiences that 'converted' them into rural practitioners.
The Four Qs Model provides a potentially useful model that demonstrates consistent themes in the characteristics of graduates of the PRCC and why they choose a rural medical career. The model could be usefully applied to the selection of medical students into rural medical education programs, and it could assist in the construction of rural curricula. The model also offers a useful framework for further research in this field.
References
1. Australian Medical Association. Training and workplace flexibility. Canberra, ACT: Australian Medical Association, 2001.
2. Access Economics Pty Ltd. An analysis of the widening gap between community need and the availability of GP services. Canberra, ACT: Australian Medical Association, 2002.
3. Wilkinson D, Beilby J, Thompson DJ, Laven GA, Chamberlain NL, Laurence C. Associations between rural background and where South Australian general practitioners work. Medical Journal of Australia 2000; 173: 137-140.
4. Kamien M, Buttfield IH. Some solutions to the shortage of general practitioners in rural Australia, Part 1. Medical School Selection. Medical Journal of Australia 1990; 153: 105-106.
5. Strasser R. Attitudes of Victorian rural GPs to country practice and training. Australian Family Physician 1992; 21(7): 808-812.
6. Rolfe IE, Pearson S, O'Connell D, Dickenson J. Finding solutions to the rural doctor shortage: the roles of selection versus undergraduate medical education at Newcastle. Australian New Zealand Journal of Medicine 1995; 25: 512-517.
7. Western J, Makkai T, McMillan J, Dwan K. Issues for rural practice in Australia. In: General Practice Evaluation Program Department Of Health Aged Care. Canberra, ACT: National Information Service, 2000; 1-30.
8. Laven G, Beilby J, Wilkinson D, McElroy J. Factors associated with rural practice among Australian-trained general practitioners. Medical Journal of Australia 2003; 179(2): 75-79.
9. Laven G, Willikinson D. Rural doctors and rural backgrounds: how strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11: 277-284.
10. Ward AM, Kamien M, Lopez DG. Medical career choice and practice location: early factors predicting course completion, career choice and practice location. Medical Education 2004; 38(3): 239-248.
11. Australian Medical Workforce Advisory Committee. Career Decision Making by Postgraduate Doctors, Key Findings. Sydney, NSW: Australian Medical Workforce Advisory Committee, 2005.
12. Worley P, Silagy C, Prideaux D, Newble D, Jones A. The parallel rural community curriculum: An integrated clinical curriculum based in rural general practice. Medical Education 2000; 34: 558-565.
13. Worley PS, Prideaux D, Strasser R, Sialgy C, Magarey JA. Why we should teach undergraduate medical students in rural communities. Medical Journal of Australia 2000; 172(12): 615-616.
14. Worley PS, Esterman A, Prideaux D. Cohort study of examination performance of undergraduate medical students learning in community settings. British Medical Journal 2004; 328: 207-209.
15. Worley PS, Prideaux D, Strasser R. Can medical students learn specialist disciplines based in rural practice: Lessons from students' self reported experience and competence. Rural and Remote Health 4: 338. (Online) 2004. Available: www.rrh.org.au (Accessed 10 November 2009).
16. Worley P, Martin A, Prideaux D, Woodman R, Worley E, Lowe M. Vocational career paths of graduate entry medical students at Flinders University: a comparison of rural, remote and tertiary tracks. Medical Journal of Australia 2008; 188(3): 177-178.
17. Australian Medical Workforce Advisory Committee. Career decision making by postgraduate doctors - AMWAC medical careers surveys, 2004. Report no AMWAC 2005.3. Sydney, NSW: Australian Medical Workforce Advisory Committee, 2005.
18. Veitch C, Underhill A, Hays RB. The career aspirations and location intentions of James Cook University's first cohort of medical students: a longitudinal study at course entry and graduation. Rural and Remote Health 6: 537. (Online) 2006. Available: www.rrh.org.au (Accessed 10 November 2009).
19. Orpin P, Gabriel M. Recruiting undergraduates to rural practice: what students can tell us. Rural and Remote Health 5: 412. (Online) 2005. Available: www.rrh.org.au (Accessed 10 November 2009).
20. Dunbabin J, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. Rural and Remote Health 3: 212. (Online) 2003. Available: www.rrh.org.au (Accessed 10 November 2009).
21. Humphreys J, Jones J, Jones M, Hugo G, Bamford E, Taylor D. A critical review of rural medical workforce retention in Australia. Australian Health Review 2001; 24(4): 91-102.
22. Australian Medical Workforce Committee. Career Decision Making by Postgraduate Doctors, Key Findings. Sydney, NSW: Australian Medical Workforce Committee, 2005.
23. Harris MG, Gavel PH, Young JR. Factors influencing the choice of specialty of Australian medical graduates. Medical Journal of Australia 2005; 183(6): 295-300.
24. Somers GT, Strasser R, Jolly B. What does it take? The influence of rural upbringing and sense or rural background on medical students' intention to work in a rural environment. Rural and Remote Health 7: 706. (Online) 2007. Available: www.rrh.org.au (Accessed 10 November 2009).


