Those who live in rural and remote areas experience a myriad of systemic barriers to accessing health care. These include a limited healthcare supply, difficulty recruiting and retaining healthcare professionals, and disparities in the number and distribution of GPs and specialist doctors. Expansive geography exacerbates these and other systemic barriers1. Moreover, inclement weather and inadequate infrastructure often make medical travel even more difficult in rural and remote regions2-7 . The terrain of British Columbia (BC) is especially challenging as it is largely characterized by forested and mountainous topography, making transportation between communities hazardous and time-consuming, especially in winter8.
Limited availability and accessibility of transportation is a well-known barrier to access health care in rural and remote regions1,3,9-14. Yet non-emergency medical transportation service programs are scarce. Such programs usually provide transportation services for a specific clientele, such as those who are elderly and physically disabled, and are designed to operate within a single community or its immediate periphery15.
A few medical transportation programs operate in Canada, such as the Care Cruiser Program operated by the BC and Yukon chapter of the international charitable organization Shriners, providing free non-emergency medical transportation with a focus on helping physically challenged and burned children. Also notable is Hope Air, a national charity that helps Canadians finance airfare for medical travel. Since 1986, Hope Air has helped pay for more than 58 000 flights with Air Canada, West Jet and Provincial Airlines16. Flight requests are accepted from all ages, illness groups, provinces and territories, but clients must demonstrate financial need. Another example is the Ontario Community Transportation Action Program (CTAP). The CTAP is a provincially-funded initiative to stimulate greater coordination of local transportation services, based on the needs of elderly and disabled people17. This program is not limited to transportation for medical reasons and covers other general purpose transportation.
To fill the gaps in this area, the Northern Health Authority (NHA) of BC established the 'Connections' service in the spring of 2006. This is a low-cost, publicly subsidized non-emergency medical transportation service for northern BC residents needing to visit a specialist or receive other healthcare services not available in their home community. Through a fleet of customized buses (equipped with wheelchair lift and toilets), patients from 41 rural and northern communities can travel all year to medical appointments in northern BC, Vancouver, Kamloops, and Grand Prairie (in the neighboring province of Alberta). Since its commencement, the Northern Health (NH) Connections users base has grown, and many have used the service multiple times, accounting for over 25 000 bus rides by August 200918.
Compared with the other examples of medical transportation, the NH Connections service is wider in geographic scope, provides a greater frequency of availability, covers diverse populations, and entails a higher subsidy, making it a unique medical transportation program in Canada.
This article examines the demographic, socioeconomic, and health profiles of the typical users of the Connections service to assess the reach of the program and determine the factors that contribute to greater frequency of service use.
Sample selection and data collection
Information on the demographic, socioeconomic and health profiles of the clients using the NH Connections service was obtained through a questionnaire administered to an initial sample of 500 users (of a population of >2000 users) using 3 methods:
- Random en-route survey of users while traveling in NH Connections vehicles to and from medical appointments (n=150), via a simple draw of 2 (of 5) short distance and 3 (of 8) long distance routes and inviting passengers to complete the questionnaire voluntarily.
- Mail-out survey administered to a randomly selected sample of past service users (n=350).
- Computer assisted phone interviews of selected past clients unwilling or unable to fill out the questionnaire they received in the mail (n=63).
A common questionnaire approved by the Ethics Committees of the University of Northern British Columbia and Northern Health Authority was used in all 3 types of survey. The questionnaire asked respondents about their demographic, socioeconomic, and health status, and their experience with the service using multiple-choice questions with an open 'other' category. The questionnaire was piloted with 30 clients before being applied to the entire sample.
To ensure the sample was representative of the communities, sample weights were applied to different communities. Such weights were calculated based on the relative shares of past users from different communities in the NH Connections database of all registered users. The number of cases suitable for final analysis was 297. Therefore, the overall response rate for the entire survey was about 60%. However, the response rate from the en-route survey was expectedly much higher (76%). In contrast, the combined rate for the mail-out and phone interviews was 52%.
Method of analysis
All data collected were pooled and linked to administrative data available from the NH Connections users' database, which includes data on personal demographics, contact numbers, postal addresses, and medical appointments. The statistical software Eviews v 5.1 (http://www.eviews.com/) was used to provide descriptive analysis of the data and estimate a 'censored ordered independent variable' regression (Tobit) model that measured the contribution of different determinants to the frequency of service use. The users were asked about the number of times they had used the service, which was top coded with 3 or more. Hence a right-censored Tobit model was deemed appropriate19. The model considers a latent variable 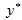 that is behind the observed responses
that is behind the observed responses 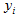 and depends linearly on a vector of explanatory variables
and depends linearly on a vector of explanatory variables 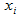 :
:
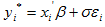 [1]
[1]
where 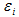 are independent and identically distributed random variables and
are independent and identically distributed random variables and 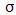 is a scale parameter. The observed
is a scale parameter. The observed 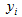 is determined from
is determined from 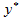 using the rule:
using the rule:
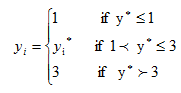 [2]
[2]
The vector of explanatory variables consists of users' demographic (eg sex, age), socioeconomic (eg income, education, employment status) and health (eg self-rated health status, number of health problems) attributes. The parameters 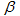 and
and 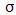 are estimated by the Maximum Likelihood method.
are estimated by the Maximum Likelihood method.
Sample descriptive results
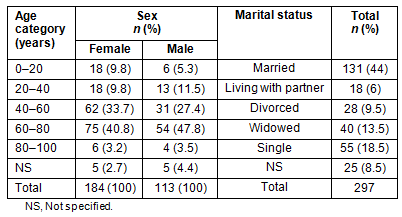
Demographic profile of the clients: Of the 295 respondents who revealed their sex, the majority were female accounting for 62% of the respondents. As well, the majority of clients (over 78%) were at least 40 years old with a mean age of approximately 55 years. Such a high proportion of older clients is, to an extent, a reflection of our ageing society; however, it is more likely to be due to a greater prevalence of health problems among older people (Table 1).
Data on the marital status of the users indicate that half of the clients were married or living with a partner; the other half were divorced, widowed and single (Table 1).
Table 1: Age and marital profiles of users
Of those who revealed their racial background (approximately 70%), approximately 18% were of Aboriginal (First Nations and Metis) background. Although the proportion of Aboriginal clients appears to be commensurate with the proportion of Aboriginal people living in northern BC, an over-representation of such users could be expected due to their greater burden of health problems and inadequate economic means. One possible reason for this lower than expected service usage among Aboriginal people is that the service is not well known among the Aboriginal population. Another is a lower response rate to mail-out and en-route surveys by Aboriginal users, because the number of Aboriginal users in the sub-sample of phone interviewees was almost double their proportion of the entire sample.
Socioeconomic profile of the users: The socioeconomic profile of users was captured by three indicators: education, employment and income status. The educational level of the majority of clients (approximately 63%) was high school or less (Table 2). Among those with more education, only 17% had graduated from a college or university. Such data are consistent with the nature of the economies and limited opportunities for more educated people in rural and northern areas.
In terms of employment status, less than half the users were retired, 21% were unemployed and 3% were disabled. More than half of those who were economically active worked part time. Such data strongly indicate that the vast majority (approximately 72%) of users were economically inactive and, therefore, in greater need of the subsidized medical transportation service.
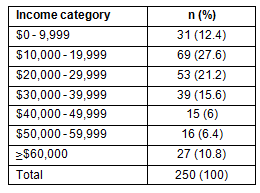
To establish income status, users were placed into 7 household income categories, with the lowest income category being $10,000 or less, and the highest $60,000 or more. A number of users (n=47) did not indicate their income category, but the income category of those who did was distributed as is shown (Table 3).
A significant proportion (61%) of the users who revealed their income had household incomes of less than $30,000 per year (Table 3). More than two-thirds of the users had incomes of less than $40,000. Unexpectedly, approximately 11% of users had incomes of $60,000 or more. While users in the latter category may have had a non-economic reason for using the service, most users were in the very low to moderate income categories, which is consistent with the employment status of the users.
Table 2: Educational and employment profiles of users
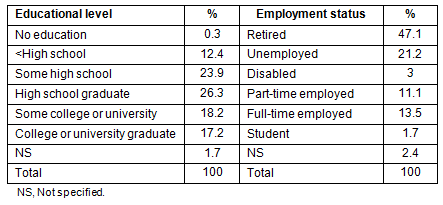
Table 3: Income profile of users
Health profile of users: To assess use of the Connections service by communities most in need, data were collected on service users' self-assessed health profile, including health conditions and the variety and frequency of health problems for which the users were seeking treatment. Users rated their health as poor, fair, good, and excellent (Fig1). Over half of the users (52%) rated their health as either poor or fair; of those with better health, 40% rated their health as good; only 7% assessed their health as excellent, indicating that the majority of clients were not in good health.
In terms of health problems reported by users (Fig2), the majority (76%) reported at least one health problem, including those who rated their health as good or excellent; and over half (55%) had at least 2 health problems, indicating that those using the service are not generally in good health.
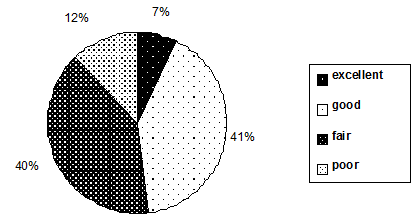
Figure 1: Self-assessed health profile of the users.
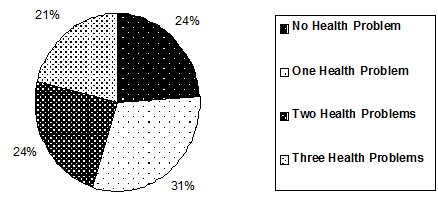
Figure 2: Distribution of self-reported health problems.
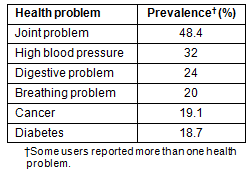
Users' reported health problems and their prevalence are shown (Table 4). It is notable that approximately half the clients with health problems suffer from joint problems, which would make driving difficult, hence their use of the Connections service. The prevalence of various health problems among users presumably reflects the absence of or inadequate appropriate healthcare services in their local communities.
Table 4: Prevalent health problems of users
Medical reasons for travel: Users indicated a wide range of medical reasons for their travel. Such reasons have been broadly classified as: (i) seeing a doctor for examination; (ii) non-surgical treatments; (iii) surgical procedures; and (iv) post-treatment follow up (Table 5).
Table 5: Medical reasons for traveling
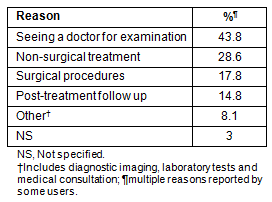
Consistent with frequency of service use, most clients presumably used the service for the first time to receive a medical examination. Non-surgical treatment, surgical procedures and post-treatment follow up were reported more often by clients who had used service before.
Estimation results
The descriptive results provide a good sense of typical service users' attributes. Some of theses attributes are most likely correlated. As a result, simple descriptive associations may not be conclusive. To determine the contribution of users' attributes to the frequency of service use (the dependent variable) considering most attributes simultaneously, a Tobit model was initially estimated for a larger set of explanatory variables or attributes (Table 6).
The set of explanatory variables includes sex (a binary variable), age (measured in years), education (measured as an ordered categorical variable with 1=lowest level of education and 6=highest), income (also measured as an ordered categorical variable with lowest income category=1 and highest=7), 5 dummy variables for the employment status of users (retired, disabled, student, unemployed, and part-time employed) with the full-time employed users taken as the reference category, and the 2 health status variables self-rated health (an ordered categorical variable with poor health=1; excellent health=4) and the number of health problems (from 1 to 6) (Table 6).
Based on the 5% level of significance, the explanatory variables sex, income, retired, disabled, student, part-time employed (among the demographic and socioeconomic attributes) and self-rated health were not statistically significant. This may be, in part, due to correlations among the variables. Moreover, two attributes (disabled and student) applied to a very small fraction of the users in the sample. Therefore, a more restricted specification of the model by dropping the statistically insignificant variables from the model was estimated. The Likelihood Ratio Test on the joint significance of the insignificant variables was 2.92 with a p-value of 0.82, meaning that such variables can be dropped safely from the model without affecting its overall fit. The Tobit model assumes a normal distribution for the errors. However, assuming a logistic distribution for the errors produced similar results. The estimation results for the restricted version of the model are reported (Table 7).
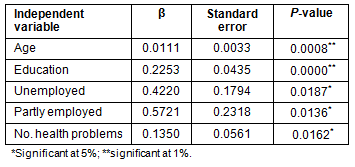
Age, education, unemployment, part-time employment and the number of health problems were statistically significant predictors or contributors to frequency of service use (Table 7). The marginal contribution of age compared with other predictors was very small, however. An extra year of education increased the frequency of use by 22.5%. Whereas, being unemployed or partly employed (compared with being fully employed) increased the frequency of service use by 42% and 57%, respectively. Likewise, an extra health problem increased the frequency of use by 13.5%. It must be noted, however, that unlike in the ordinary regressions, the interpretation of the coefficients as measures of the marginal effects of independent variables on the mean value of the dependent variable was not straightforward. Here, changes in the independent variables (users attributes) not only affected the mean value of the censored dependent variable (frequency of service use), but also its probability. The marginal effects can be decomposed into portions related to the change in the mean value of frequency of use and those related to the change in the probability of using the service20. Such decomposition was not critical because the question of whether the respondents used the service at all is irrelevant.
Table 6: Estimation results for the frequency of service use - the unrestricted model (estimated using 236 observations, 66 of which were right censored)
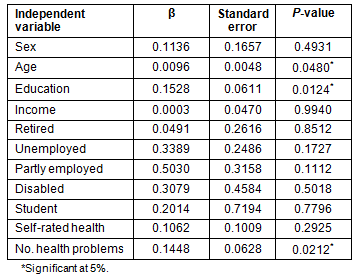
Table 7: Estimation results for the frequency of service use - the restricted model (estimated using 278 observations, 79 of which were right censored)
Discussion
The results are based on a relatively low sample response rate of approximately 60%, and this may have been due to mailed surveys not reaching intended recipients due to misreporting or change of address. However, what is critical is whether this rate reflects any systematic under-representation of certain groups with divergent traits from those captured in the sample. Aside from the concern about potential under-representation of Aboriginal users already discussed, it does not appear that the sample was systematically biased.
The descriptive sample results indicate the typical users of the Connections service. In terms of their demographic background, the majority are females of older age. This is not surprising given the higher prevalence of health problems among women in general, and those of older age in particular. Approximately half of the users were divorced, widowed, or single and need to rely on others for traveling purposes, unlike couples. A sizable portion of the users were Aboriginal but this was lower than expected, indicating Aboriginals may have been underrepresented in the sample. In terms of socioeconomic background, a significant majority of users had formal education up to high school level, approximately half were retired, and over one-fifth were unemployed, amounting to nearly three-quarters being economically inactive. Moreover, the vast majority of users reported annual incomes of less than $30,000 with a greater majority reporting less than $40,000, which adds to the evidence that typical service users are socio-economically in need. Regarding medical need, the results for self-reported health and health problems (few users in good health and the majority suffering from at least one chronic health problem) indicate that those in medical need are typical service users. Therefore, the Connections service has reached deserving users and enhanced their access to medical care.
The estimation results focus on the restricted model (Table 7), and show age, education, unemployment, part-time employment, and the number of health problems to be statistically significant (p-values ranging from 0.000 to 0.019) contributors to the frequency of service use. As such, older age, higher education level, being unemployed or partly employed, and more health problems are associated with more frequent use of the service by users. While age and the number of health problems capture the medical need of the users for the service, unemployment and part-time employment may indicate the economic need for using the service. It could also be argued that those unemployed and partly employed have more time or lower opportunity cost of time that would lead to more frequent use of the service.
Regarding the effect of education, if education is an indicator of social status, the results show that users of higher social status are using the service more frequently. This interpretation is not plausible for at least two reasons. First, the income variable, which is often highly correlated with social status, did not affect the frequency of service use (Table 6). Second, the educational level of a significant majority of users was at or lower that high school education, hardly a measure of social status. A more convincing interpretation of the effect of education on frequency of service use is that users with higher levels of education are more informed citizens who are more likely to use the services or opportunities available in their communities.
By construction, the individuals in our sample were all service users, which has limited the analysis and its implications. Data on those who were aware of the service but did not use it would have provided a better understanding of usage factors. Also, as a relatively new service, repeated use by individual users is likely to increase over time, which may yield greater observed variation in frequency of use to assist discrimination among significant predictors.
This study examined the success of the NH Connections service in enhancing rural and northern communities' access to healthcare services, in particular among those with limited means and resources. Overall, the Connections service appears to have reached to people with medical need and those of lower economic status in terms of employment, who may otherwise have found it difficult to access healthcare services outside their communities. Therefore, as an innovative healthcare policy, the Connections service model may be useful in other rural and remote jurisdictions.
Ultimately, however, enhanced access to needed health care should result in improved health. Therefore, a follow-up study on actual health improvement among the Connections service clients would be valuable. An equally important analysis yet to be undertaken is a cost-effectiveness assessment of this service compared with available alternatives.
Acknowledgements
Funding was obtained from the Northern Health Authority of British Columbia for an evaluation of the service. This article uses some of the data collected for that evaluation.
References
1. Leipert BD, Reutter L. Developing resilience: how women maintain their health in northern geographically isolated settings. Qualitative Health Research 2005; 15(1): 49-65.
2. Bellamy GR, Stone K, Richardson SK, Goldsteen RL. Getting from here to there: evaluating West Virginia's Rural Nonemergency Medical Transportation Program. Journal of Rural Health 2003; 19(Suppl): 397-406.
3. Goins RT, Williams KA, Carter MW, Spencer M, Solovieva T. Perceived barriers to health care access among rural older adults: a qualitative study. Journal of Rural Health 2005; 21(3): 206-213.
4. Kornelsen J, Grzybowski S. Rural Women's Experiences of Maternity Care: Implications for Policy and Practice Ottawa: Status of Women Canada. (Online) 2005. Available: http://www.ruralmatresearch.net/documents/FinalReport.pdf (Accessed 11 June 2009).
5. Ministerial Advisory Council on Rural Health. Rural Health in Rural Hands: Strategic Directions for Rural, Remote, Northern and Aboriginal Communities. (Online) 2002. Available: http://dsp-psd.pwgsc.gc.ca/Collection/H39-657-2002E.pdf (Accessed 21 November 2009).
6. Procyk A, Tobin P, Goodenough R, Cudmore M, Halseth G, Hanlon N. Integrated Study of the Social Determinants of Rural Health: 2005 Interim Report. Prince George, BC: Geography Program, University of Northern British Columbia. (Online) 2005. Available: http://web.unbc.ca/geography/faculty/greg/publications/Rural_Health_Interim_Report.pdf (Accessed 15 June 2010).
7. Triller D, Triller M, Donnelly J, Rugge J. Travel-related savings through a rural, clinic-based automated drug dispensing system. Journal of Community Health 2005; 30(6): 467-476.
8. Government of British Columbia Ministry of Health. Enhancing Health Services in Remote and Rural Communities of British Columbia: An Update on Former Recommendations. (Online) 2002. Available: http://www.health.gov.bc.ca/library/publications/year/2002/rapupdate.pdf (Accessed 21 December 2009).
9. Arcury TA, Preisser JS, Gesler WM, Powers JM. Access to transportation and health care in a rural region. Journal of Rural Health 2005; 21(1): 32-38.
10. Leipert BD. Rural women's health issues in Canada: an overview and implications for policy and research. Canadian Woman Studies 2005; 24(4): 108-116.
11. Nemet GF, Bailey A. Distance and health care utilization among the rural elderly. Social Science & Medicine 2000; 50: 1197-1208.
12. Schopp L, Johnstone B, Merrell D. Telehealth and neuropsychological assessment: new opportunities for psychologists. Professional Psychology: Research and Practice 2000; 31(2): 179-183.
13. Sherwood KB, Lewis GJ. Accessing health care in a rural area: an evaluation of a voluntary medical transport scheme in the English Midlands. Health & Place 2000; 6(4): 337-350.
14. Wardman D, Clement K, Quantz D. Access and utilization of health services by British Columbia's rural Aboriginal population. Leadership in Health Services 2005; 18(2): xxvi-xxxi.
15. Herold M, Gordon T, Kaye K, Brockie E, Fuller T. Rural Transportation Series No. 4. Elderly and Disabled Rural Residents: a continuing transportation issue. Ottawa: Government of Canada, 2002.
16. Hope Air. Hope Air History. (Online) 2008. Available: http://www.hopeair.org/pages/about_us/about_us_history.html (Accessed 20 December 2009).
17. Fuller T, Herold M. Community-based Responses to Rural Transportation Issues in Ontario: a review of the Ontario Community Transportation Action Program (CTAP) 1998-2000. (Online) 2002. Available: http://www.rural.gc.ca/researchreprots/transport/no1_e.pdf (Accessed 22 September 2008).
18. Northern Health Authority. Welcome to Northern Health Connections. (Online) no date. Available: http://www2.northernhealth.ca/Your_Health/Programs/NH_Connections/default.asp (Accessed 12 September 2010).
19. Greene WH. Econometric analysis, 5th edn. Upper Saddle River, NJ : Prentice Hall, 2003.
20. McDonnald JF, Moffitt RA. The uses of Tobit analysis. Review of Economics and Statistics 1980; 62(2): 318-321.
