Lack of access to health care, especially in early childhood, is one of the major determinants of inequality in health1. While there are many studies describing problems and barriers in access to care among Indigenous patients2-4, there are few quantitative studies that assess disparities in the utilization of healthcare services between Indigenous groups and the majority population. A study in Australia found a higher rate of hospitalization among Aboriginal people5. This article explores the utilization of health care among the Indigenous Sami people in Norway.
Variations in healthcare expenditure has been an issue in health service research for many years6. Variations in hospital rates are often described in the literature using aggregated data and small area analysis6-8, or in studies of access to services9. Regarding geographic access, it is widely acknowledged that the nearer one is to services the better is one's access10. When considering health-delivery system characteristics, it has been established that those living in areas with more services (eg more physicians) have superior access to health care7,9. Hospital use is also related to the characteristics of the patient and population. This is often based on qualitative studies, and this socio-cultural literature examines cultural access and the way linguistic problems and cultural differences shape barriers for effective communication and treatment11-13. However in studies based on aggregated data, information revealing linguistic and cultural barriers to care is not easy to include in a model.
Political and professional concerns related to health services for Sami people
Since the 1960s in Norway there have been political and professional concerns about persistent health gradient differences between the northernmost county (Finnmark) where many Sami people live, and the counties further south. In 1980, a study of a Sami village observed a gap between Sami people and other Norwegians in their primary healthcare utilization14,15. While the average consultation rate in Norway was 3 times a year, subjects who considered themselves to be Sami had 0.5 visits per year, and other villagers 1.4 visits. Fugelli suggested that linguistic and cultural barriers prevented Sami patients from consulting a doctor. A more recent study suggested ethnic barriers to Sami youths accessing health services, although Sami and non-Sami youths were found to use health services with equal frequency16. Apart from these studies there is little documentation of health service utilization among the Sami people.
Health policy and Sami population today
Norway's health services are founded on the principle of equal access. Norwegian health policy is more ambitious, implying that equal results require a disproportionate distribution of health services. This is because equal rights re-create existing social differences17. Therefore, a main objective of Norwegian Sami health policy is to provide a better quality health service for Sami patients, and so government initiatives are based on the assumption that barriers result in an under-utilization of health services among Sami patients18-20.
Objective
The objective of this study was to explore whether somatic hospital services and specialist care are under-utilized among Sami people by comparing health expenditure in predominantly Sami municipalities and non-Sami municipalities.
Data on the expenditure of hospitals and specialist services were retrieved from the Norwegian Patient Registry (NPR) for the period 2002-2006. However data from 2008 was used to ascertain the number of specialists in private practice, the number primarily public funded and attached to hospitals, and the specialist service level (data from 2002 to 2006 were not available). Mean annual expenditure rates express the number of out-patient contacts and hospitalizations. Each individual may have more than one out-patient contact or more than one hospitalization.
Geographical delimitation
In Norway there are no official health-related or other statistics for people in the ethnic group Sami. Even the number of Sami who live in Norway is unknown, and no clear ethnic border between Sami and Norwegians has been established. However a geographical delimitation is often used in Sami policy instruments. In 1992, six rural Sami municipalities in Northern Norway (Kautokeino, Karasjok, Porsanger, Tana, Nesseby and Kåfjord) were described as the administration area for those who speak the Sami language. For the purposes of the present study, these were considered the main area of Sami habitation (Fig1).
Three different data sources confirmed that the proportions of Sami in these areas are significantly higher than in the neighbouring municipalities of Finnmark and Northern Troms. First, the proportion of the population in the Sami municipalities who had registered in the 2005 Sami Census21 was between 20% and 68%, compared with 5% in Finnmark and 4% in the remaining municipalities of Northern Troms. Second, the Sami language is a proxy for Sami identity. The Saminor study revealed that between 14% and 86% of the population in the 6 Sami municipalities speak Sami, compared with 4% in the neighbouring municipalities (available data from the neighbouring area consisted of only 5 of the 17 surrounding municipalities, which were considered to be 'mostly Sami')22. Third, a survey from the Sami Parliament found that between 35% and 96% of the population in the 6 Sami municipalities were able to understand the Sami language, compared with 10% in the neighbouring municipalities23, although this survey has been criticized for methodological flaws24. While the proportion of Sami varies among the 3 sources, all demonstrate high Sami populations in the 6 municipalities selected, and low numbers in neighbouring municipalities.
Comparison areas
No municipalities have the same background population characteristics (educational standards, income, and employment in primary industries), healthcare supply and delivery, and access (distance) to care. However the neighbouring municipalities were chosen for comparison (in addition to the national average) because they were judged to be most similar to the Sami municipalities. The host municipalities of hospitals were excluded from the neighbouring comparison areas because other studies have proved such municipalities to have higher expenditure on hospitals25. 'Comparison Area Finnmark' is the study term for the remaining municipalities in Finnmark County, with the exclusion of the 3 municipalities with hospitals (Sør-Varanger, Kvalsund and Hammerfest). 'Comparison Area Northern Troms' is the study term for municipalities that collaborate with the Sami municipality Kåfjord on health care in the northern part of Troms County (Kvænangen, Skjervøy and Nordreisa) (Fig1).
Municipalities are well defined population units and valid constituencies for studying variations in the use of hospitals and specialist services across the country.
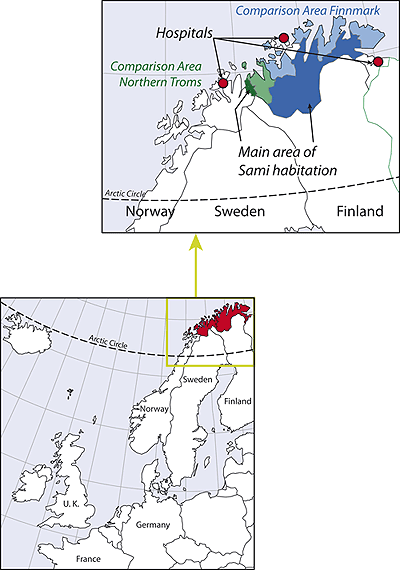
Figure 1: Map of the main area of Sami habitation, including comparison areas and hospital locations.
Statistical methods
Age- and sex-adjusted expenditure rates at the municipality level were calculated using a direct method of standardization, with the Norwegian population of 1 January 2004 as standard, and comparison age groups of 0-19, 20-34, 35-49, 50-64, 65-79 and 80 years and older.
When using aggregated data from the NPR alone, it is not possible to distinguish patient characteristic effects such as linguistic or cultural barriers, on the supply of care, access to care, or substitutes for hospital care. When controlling for structural variables, the objective was include explanatory variables and confounders, and discuss direction in which those variables influenced/affected the results. Travelling time to care from the centre of the municipality to the hospital was used as a simple measure of access to care, and expressed as short, medium or long (<1 hour, 1-2.5 hours, >2.5 hours, respectively).
Data from the NPR were provided as an SPSS Windows v15.0 (www.spps.com) data file, with SAS statistical software for Windows v9.1 (www.sas.com) used for calculations.
Purpose and ethical approval
This study is a part of the project 'What creates different expenditure rates for hospital services in Norway', and was approved by the Norwegian Social Science Data Services. The purpose of the project is to investigate whether variation in the rate of health expenditure among municipalities can be associated with municipalities' characteristics or primary health care.
The yearly expenditure rates for both out-patient treatment and hospitalization measured at municipality level vary from year to year. In 3 of the 6 municipalities in the main area of Sami habitation, out-patient treatment expenditure ranged from above to below the national average during the period 2002-2006. The annual variation is largest in the smallest municipality, where the range (highest-lowest yearly rate) is 17 % of the mean annual rate. The annual rates of hospitalization varied even more (up to 33% of the mean annual rate). Taking yearly variation into consideration, the results are presented using mean annual rates for the 5 year period.
Expenditure rates within the main area of Sami habitation vary
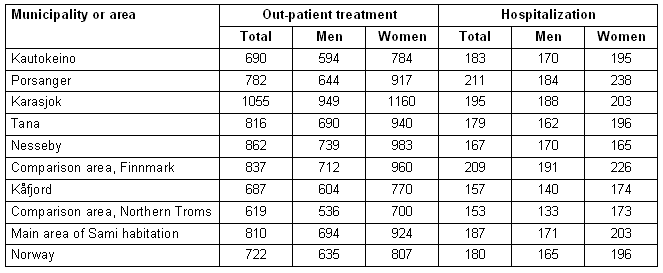
The mean annual expenditure rates in the Sami municipalities vary considerably (Table 1). The rates in 4 of the 6 Sami municipalities are above the national mean for out-patient contact. The rates in 3 of the 6 Sami municipalities are above the national mean for hospitalization. The average expenditure for the six Sami municipalities is also above the national average. Compared with neighbouring municipalities, expenditure in Sami municipalities is higher in 3 of 6 municipalities for out-patient treatment, and 2 of 6 for hospitalization. Karasjok stands out from the other Sami municipalities in having the highest expenditure on out-patient treatment. Kåfjord is the only Sami municipality lower than the national average for both out-patient treatment and hospitalization expenditure; however it is a high-expenditure municipality compared with the neighbouring area.
Table 1: Mean annual rate of expenditure on out-patient treatment and hospitalization per 1000 inhabitants 2002-2006
Highest expenditure in the middle-aged population in Sami municipalities
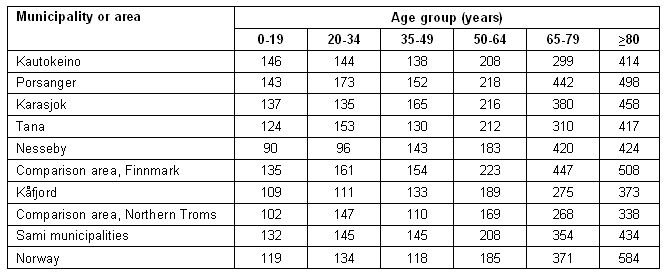
The expenditures on both out-patient treatment and hospitalization for the age groups 35-49 and 50-64 years in all Sami municipalities are higher than the national average, with one exception (Tables 2,3). The expenditure on out-patient treatment for these two age groups are lower than in the comparison areas in 2 and 3 Sami municipalities, respectively. Comparison area Finnmark has even higher expenditure than the Sami municipalities for hospitalization, except for one age group in one Sami municipality.
Lowest expenditure in the oldest population in Sami municipalities
The expenditure for out-patient treatment among the elderly (≥80 years) is below the national average in 4 of the 6 Sami municipalities, and below the comparison area in three of the 6 municipalities. The expenditure for hospitalization is below the national average for this age group in all of the Sami municipalities, and below the comparison area in 5 of the 6 municipalities.
Table 2: Age specific rate of expenditure on out-patient treatment per 1000 inhabitants (5 year average) 2002-2006
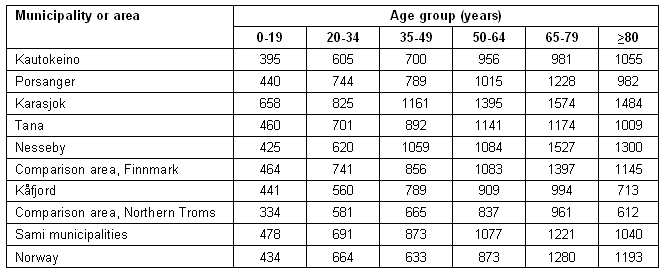
Table 3: Age specific expenditure rates on hospitalization per 1000 inhabitants (5 year average) 2002-2006
Considerable volume of private practice specialist health care in two Sami municipalities
In addition to public sector services, there is a considerable volume of private practice specialist health care that is mainly public funded, and mostly in urban parts of Norway. Very few of the specialists in private practice work in Finnmark or the northern part of Troms. Nevertheless, in 2 of the Sami municipalities the expenditure for private practice specialist health care is almost equal to the national level (Fig2). Except for Karasjok, which has the highest public expenditure but also considerable private expenditure, this makes the total out-patient expenditure more even among the Sami municipalities; the municipalities with the lowest public expenditure, have the highest private practice expenditure.
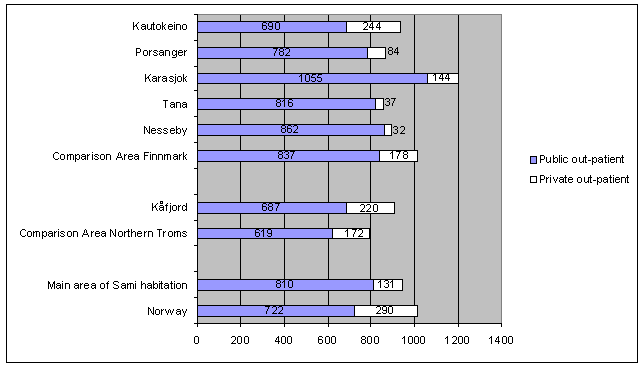
Figure 2: Out-patient expenditure rates per 1000 inhabitants in private practice (2008) and the public sector (5 year average 2002-2006).
Discussion
The main finding of the present study is that the overall healthcare use in Sami municipalities is higher than the national average and the same as in corresponding municipalities in that geographic area. However, there remains a considerable variation in expenditure among the Sami municipalities. This is consistent with the rest of the municipalities in Norway.
Data and methods
The study aim was to explore whether there is an under-utilization of somatic hospitals and specialist service among Sami people, based on the rate of health expenditure of Sami municipalities. A major limitation in a geographical analysis like this is that aggregated data may be misleading when the population studied is heterogeneous14, as is the case in the main area of Sami habitation which contains a Sami population and other inhabitants. Inhabitants of the main area of Sami habitation who are not Sami have been included, while Sami people living outside the main area of Sami habitation (including those in cities) have been excluded. However, there is no reason to believe that the heterogeneity of this area challenges our main conclusion, for what is under discussion is the Sami municipalities with the largest proportion of Sami people. Regarding the Sami municipalities with the lowest proportion of Sami people (Porsanger and Kåfjord), a marginal under-utilization of health care among the Sami would be more difficult to detect.
Limitations
There are, however, two potential limitations to the study. First, the NPR data contains very little information on the background of those consuming healthcare services. Second, only one year (2008) of out-patient expenditure on private practice was available for analysis, so these data are less reliable than the 5 year average for public expenditure.
Explanatory variables and confounders
In the following discussion of the results, consideration is given to the modernization of Sami people, supply and access to care (supply of GPs and distance to care), and the characteristics of the healthcare delivery system (replacements for general hospital beds). Variables such as out-of-pocket payment for services and insurance coverage were not considered in the present study because minimum variance can be expected due to the Norwegian publicly-funded universal healthcare system.
Consequences of modernization and assimilation of the Sami on healthcare consumption: The reduction in the earlier observed differences in healthcare expenditure between the Sami and the rest of the population is probably closely related to the modernization and assimilation of the Sami people. The traditional Sami way of life is rarely followed now, and many Sami people do not speak the Sami language. As the Norwegian Sami population has become modern and heterogeneous, the Sami people have integrated into the Norwegian social system26. High levels of education and good health among the Sami people are the consequences of this assimilation, with no health differences between Sami people and other Norwegians today27. This is in contrast to other Indigenous peoples, for in North America, Australia and New Zealand, the healthcare barriers of poor communication, rural location and low socio-economic status continue to disproportionately affect indigenous populations2.
Explaining varying hospital rates - supply of and access to care: Supply factors to be considered include the supply of primary health care, hospital beds and out-patient clinics. The supply of primary health care is likely to be a confounder of great importance. While there is no evidence of systematic differences in the local primary health care for the proportion of Sami inhabitants in the municipalities studied, data are lacking concerning the supply of primary health care for the whole period 2002-2006. However, a Finnmark study from 2002-2004 classified the Sami municipalities Kautokeino and Porsanger as 'unstable' with respect to primary health staffing, finding many GP positions vacant due to high staff turn-over, leaving many inhabitants without a physician28. There is instability in Comparison Area Finnmark too, with 6 out of 11 municipalities classified 'unstable'. In Norway, GPs have a gatekeeper role, being responsible for all referrals to hospitals and specialist care29, thus reduced access to GPs may result in fewer referrals to hospitals30. However the relationship between the supply of primary health care and hospital rates can be ambiguous, for other studies have claimed that a lack of primary care providers increases hospitalization, including an Australian study where a higher rate of hospitalization among Aboriginals was thought to be due, in part, to their delayed presentation to primary health care5,31.
Are cottage hospital beds a replacement for general hospital beds for the oldest patients? Differing types of health services can sometimes be interchangeable, for example general hospital beds and cottage hospital beds (in Norway small medical institutions or 'general practitioner hospitals' called cottage hospitals are between primary care and general hospitals). Cottage hospital beds were not included in the present data. Therefore, the characteristics of the healthcare delivery system at the municipality level will affect the hospital expenditure rates. It has been estimated that up to 45% of treatments in cottage hospital beds may be substitutes for treatment in a general hospital32. Each of the Sami municipalities studied had between one and 4 cottage hospital beds (2002-2006). Because one of the present findings is that the expenditure on the elderly (≥80 years) in Sami municipalities was far below the national average, this may have been attributable, at least in part, to their access to cottage hospital beds. In 2006 there were 40 beds in cottage hospitals in Finnmark of a total of only 89 in Norway, although only 1.6% of the Norwegian population resides in Finnmark33. It is known that the cottage hospital beds in particular are used by elderly patients34. This may explain the lower expenditure on the elderly in the comparison areas, as well as in the Sami municipalities.
Travelling time to care: It is widely acknowledged that medical care is easier to access when it is located nearby. Therefore 'travelling time to care' as a proxy for access to care is often considered an important factor when explaining differences in healthcare expenditure. None of the Sami municipalities had access to a hospital within 1 hour of travelling time; however, Karasjok is one of 2 municipalities in Finnmark that hosts an out-patient clinic. The location of this clinic might explain the very high out-patient expenditure in Karasjok. Kautokeino is the Sami municipality located furthest from a hospital (>2.5 hours) and this may explain its lower expenditure on public out-patient services. However the use of specialists in private practice in Kautokeino was equal to the national level. While specialists in private practice are located mainly in the urban areas of Norway, there are some specialists located within 2 hours' travel of Kautokeino.
Studying the current healthcare expenditure among Sami people in Norway is relevant because former studies have concluded that linguistic and cultural barriers prevent Sami people from using healthcare services, and recent official 'white papers' have assumed an under-utilization of health services among Sami patients. The present study results on the healthcare services expenditure of 6 Sami municipalities do not indicate that barriers prevent the inhabitants from using somatic hospital and specialist services. However the fact that cultural differences and linguistic problems often shape communication failure between patients and providers must still be taken into consideration. Although this study does not support that being an inhabitant of a Sami municipality is significant in terms of expenditure on health services, it cannot be excluded that Sami patients experience a patient-physician relationship of lesser quality than other Norwegians.
Implication
Concerns related to somatic hospital services for Sami people should concentrate on the quality of care, rather than assumed under-utilization.
References
1. Mackenbach J, Bakker M (Eds). Reducing inequalities in health: a European perspective. London: Routledge, 2002.
2. Marrone S. Understanding barriers to health care: a review of disparities in health care services among indigenous populations. International Journal of Circumpolar Health 2007; 66(3): 188-198.
3. Cass A, Lowell A, Christie M, Snelling PL, Flack M, Marrnganyin B et al. Sharing the true stories: improving communication between Aboriginal patients and healthcare workers. Medical Journal of Australia 2002; 176: 466-470.
4. Kelly L, Brown JB: Listening to native patients. Changes in physicians' understanding and behaviour. Canadian Family Physician 2002; 48: 1645-1652.
5. Healy J, Sharman E, Lokuge B. Australia Health system review. Health systems in Transition 2006; 8(5): 1-158.
6. Wennberg J, Gittelsohn A. Small area variations in health care delivery. Science 1973; 182(4117): 1102-1108.
7. Gittelsohn A, Powe NR. Small area variations in health care delivery in Maryland. Health Services Research 1995; 30: 295-317.
8. Joines JD, Hertz-Picotto I, Carey TS, Gesler W, Suchindran C. A spatial analysis of county-level variation in hospitalization rates for low back problems in North Carolina. Social Science & Medicine 2003; 56: 2541-2553.
9. Rosenberg MW, Hanlon NT. Access and utilization: a continuum of health service environments. Social Science & Medicine 1996, 43(6): 975-983.
10. Joseph AE, Phillips DR. Accessibility and utilization: geographical perspectives on health care delivery. New York: Harper and Row, 1984.
11. Wang L. Immigration, ethnicity, and accessibility to culturally diverse family physicians. Health & Place 2007; 13; 656-671.
12. Carrillo JE, Green AR, Betancourt JR. Cross-cultural primary care: a patient-based approach. Annals of Internal Medicine 1999; 130: 829-834.
13. Zhang J, Verhoef MJ. Illness management strategies among Chinese immigrants living with arthritis. Social Science & Medicine 2002; 55: 1795-1802.
14. Fugelli P. Den norske lege i Sameland. Etiske og etniske problemer ved Skoganvarreprosjektet. [The Norwegian doctor in Sami areas. Ethical and ethnical problems regarding the Skoganvarre-project]. In: M Aikio, K Korpijaakko (Eds). Samesymposium. Rovaniemi: Förvaltningsembetet publikationer 15, 1991. (In Norwegian).
15. Fugelli P. Morbidity and health service among the women in a Lappish-Norwegian village. Nordic Council for Arctic Medical research Report 1982; 33: 141-142.
16. Turi AL, Bals M, Skre IB, Kvernmo S. Health service use in indigenous Sami and non-indigenous youth in North Norway: a population based survey. BMC Public Health 2009; 9: 378.
17. Lian O, Westin S. Bidrar helsetjenesten til sosiale ulikheter i helse? [Does health care contribute to health disparities?]. In: JG Mæland, JI Elstad, O Næss, S Westin (Eds). Sosial epidemiologi - Sosiale årsaker til sykdom og helsesvikt. Oslo: Gyldendal Akademisk, 2009; 315-335. (In Norwegian).
18. Norwegian Government. NOU 1995:6 Plan for helse- og sosialtjenester til den samiske befolkning i Norge. [Long-term plan for health and social services for the Sami people in Norway]. Oslo: Government Administration Services, 1995. (In Norwegian).
19. Ministry of Social Services and Health. Mangfold og likeverd: Regjeringens handlingsplan for helse- og sosialtjenester til den samiske befolkningen i Norge 2002-2005 [Diversity and equality - The Government's long-term plan for health and social services for the Sami people in Norway]. (Online) 2001. Available: http://www.regjeringen.no/upload/kilde/shd/pla/2001/0001/ddd/pdfv/140454-mangfold_og_likeverd.pdf (Accessed 9 November 2009). (In Norwegian).
20. Norwegian Ministry of Health and Care Services. [The Coordination Reform]. Report no.47 (2008-2009). Oslo: Government Administration Services, 2009. (Report in Norwegian, English summary).
21. Sami Parliament. Sami Census 2005. (Online) 2005. Available: http://www.sametinget.no/Artikkel.aspx?AId=236&back=1&MId1=3461&MId2=&MId3=& (Accessed 18 October 2010).
22. Lund E, Melhus M, Hansen KL, Nystad T, Broderstad AR, Selmer R et al. Population based study of health and living conditions in areas with both Sami and Norwegian populations - The Saminor study. International Journal of Circumpolar health 2007; 66(2), 113-128.
23. Sami Trade and Development Centre. Undersøkelse om bruken av samisk språk [Investigation on the use of Sami language]. Tana: SEG, 2000.
24. Nordic Sami Institute. [Sami Social Science Database]. (Online) 2008. Available: http://www.sami-statistics.info (Accessed 18 October 2010).
25. Heiberg I, Berntsen G. Finnmarksbefolkningens bruk av sykehustjenester, med særlig fokus på Alta kommune [Use of hospitals in Finnmark county]. Tromsø: Center of Clinical Documentation and Evaluation, Regional Health Authority of Northern Norway 2009. (Online) 2009. Available: http://www.helse-nord.no/getfile.php/SKDE/Dokumenter/Rater%20sykehusforbruk%20Finnmarkskommuner%202003-2007_versjon2.pdf (Accessed 18 October 2010). In Norwegian).
26. Selle P, Straumsnes K. Marginalisering eller integrering? Samisk politisk interesse og deltakelse. [Marginalization or integration? Sami political interest and participation]. In: I Helgøy, J Aars (Eds). Flernivåstyring og demokrati. Bergen: Fagbokforlaget, 2008; 189-220. (In Norwegian).
27. Special Study Group of Sami Statistics. Samiske tall forteller 2. Kommentert samisk statistikk 2009 [Sami figures 2. Annotated Sami statistics 2009]. Guovdageaidnu: Sámi University College, 2009. (Online) 2009. Available: http://www.regjeringen.no/upload/AID/publikasjoner/rapporter_og_planer/2009/Samiske_tall_forteller_II_Norsk.pdf (Accessed 16 October 2010). (In Norwegian and Sami).
28. Abelsen B, Baeck UDK (Eds). Lav stillingsstabilitet som utfordring for fastlegeordningen i Finnmark og Nord-Trøndelag. [Turnover and locums: a challenge for the list-doctor system in Finnmark and Nord-Troendelag] Alta and Tromsø: Norut, 2005. (In Norwegian).
29. Carlsen B, Norheim OF. Introduction of the patient-list system in general practice: Changes in Norwegian physicians' perceptions of their gatekeeper role. Scandinavian Journal of Primary Health Care 2003; 21(4): 209-213.
30. Fylkesnes K. Determinants of health care utilization - visits and referrals. Scandinavian Journal of Public Health 1993; 21: 40-50.
31. Shea S, Misra D, Ehrlich MH, Field L, Francis CK. Predisposing factors for severe, uncontrolled hypertension in an inner-city minority population. New England Journal of Medicine 1992; 327: 776-781.
32. Aaraas I. The Finnmark general practitioner hospital study. Scandinavian Journal of Primary Health Care 1995; 13: 250-256.
33. Statistics Norway. [Beds in hospitals, cottage hospitals and maternity homes]. (Online) 2009. Available: www.ssb.no/histstat/tabeller/4-20.html (Accessed 23 February 2010). (In Norwegian).
34. Aaraas I, Førde OH, Kristiansen IS, Melbye H. Do general practitioner hospitals reduce the utilisation of general hospital beds? Evidence from Finnmark county in north Norway. Journal of Epidemiology & Community Health, 1998; 52: 243-246.



