Sub-Saharan Africa remains the epicenter of the global HIV and AIDS epidemic with 22 million people presently living with HIV1. Southern African Malawi has an HIV prevalence of 11.9% among those aged 15-49 years, with over 930 000 people living with HIV from the population of 13.1 million1,2. By 2007, approximately 68 000 Malawian adults and children had died of AIDS-related illnesses and life expectancy had fallen to 50 years3.
The majority of Malawians are impoverished and primarily dependant on subsistence farming, with 85% of the population living in a rural area4. Health care in rural areas is provided from government and church-owned health centers and small community hospitals, each of which serves an average population of 35 000. However, many villagers have poor access to health care due to distance to health centers and a lack of transportation for those who are ill. Health centers are under-resourced in materials (eg equipment and medications) and staff, especially nurses5-8.
In 2004 the Government of Malawi and its Ministry of Health created an ambitious 6 year national health program and considerable progress has been made in achieving its goals5. Free antiretroviral therapy (AVT) has been made available to 200 000 citizens and the number of healthcare workers has increased9,10. Despite this important progress, villagers in remote areas are not being tested. Additionally, those who test positive to HIV have to travel great distances to be evaluated for care and treatment11.
The Mulanje District in Malawi's south is particularly under-resourced. It consists of 3309 km2 (2056 miles2) and has a population of 540 000, 48% of whom are aged under 15 years. Land is scarce due to the mountainous terrain and foreign-owned tea estates, making even subsistence farming difficult12. Two district areas, Muloza and Chitakale, were identified by the Mulanje District Health Office in 2008 as particularly underserved and distant from government health centers.
The purpose of this report is to describe the work of two mobile clinics to fill the identified service gap in the remote areas of Mulanje District. The program was developed by an international non-governmental organization, Global AIDS Interfaith Alliance (GAIA), and the Mulanje Health District Office, with funding from the Elizabeth Taylor HIV/AIDS Foundation.
The Global AIDS Interfaith Alliance has worked in Malawi since 2001. Its 2003 major village program, funded by the Bill and Melinda Gates Foundation, trained local women in HIV prevention and care strategies. The women educated and encouraged villagers to access voluntary HIV counseling and testing services, and provided care to home-based patients and orphaned children.
In 2007, GAIA obtained funding from the Elizabeth Taylor HIV/AIDS Foundation to deploy two mobile clinics in Malawi to increase access to:
- rapid HIV testing and referral for treatment
- diagnosis and treatment of malaria
- sputum collection for suspected TB
- diagnosis and treatment of STIs and opportunistic infections
- pre-natal care.
Using an integrated primary health care model, GAIA developed clinical protocols with the Mulanje District Health Office (DHO). The mobile clinics were designed to provide the kinds of entry-level services normally available at community-based government health centers. Data collection processes were devised to link the mobile clinics to the Health Management Information System (HMIS) in use in Malawi.
Two four-wheel drive utility vehicles were outfitted for this service. The roads in this district are unpaved, and this type of vehicle is needed to traverse the rugged terrain and reach distant villages. The vehicles were equipped with a stretcher, storage for medical and laboratory supplies, and seating for the clinical team of clinical officer, nurse and nurse's aide. As well as carrying clinical supplies and healthcare personnel to care sites, patients requiring urgent care are transported to the district hospital in the vehicle.
Healthcare providers and development experts reviewed applications and interviewed for drivers and mobile clinic staff, who were then trained in the Mulanje DHO's clinical protocols. As well as equipping the vehicle, the DHO requires that each mobile clinic team maintains an office in the area of service with locked safe storage for medications and supplies, and overnight secure garaging for the vehicle. So after training, staff were dispatched to visit service sites, identify potential clinic locations (eg churches, schools or other community buildings), and determine circuits for visiting the selected villages. As part of this process, staff meet with village headmen and women to introduce the project, promote local understanding and gain cooperation, a strategy used successfully by GAIA in previous community-based projects. The clinic sites were then chosen by clinic staff in consultation with community leaders. Because each mobile clinic returns to the same location on the same day each week, villagers are able to anticipate the timing and location of local health care.
It was intended that the project would be operational within 6 months of funding (ie by August 2008), but delays in shipping the vehicles from other countries and then adapting them for clinic use, hiring clinical staff, solidifying the partnership with the Ministry of Health, and meeting official requirements meant that this was not possible. For example, while GAIA received permission for the clinics from the Ministry of Health, additional approval was required from the Medical Council of Malawi, a para-statal professional regulatory body. Although this delayed the program, it ensured robust support from multiple stakeholders once the project was launched.
The two mobile clinics were deployed on 13 October 2008. On the first day of operation, both were overwhelmed with patients, with the 100 patients at each site more than double the anticipated number. Because of the overwhelming number of patients, the vehicle drivers assisted staff to deploy a crowd control strategy to maintain a calm and orderly environment (Fig1). To ensure the sickest patients were seen first, staff prioritized patient 'health passports' (the patient-held ongoing medical record used in Malawi), identifying the patients who required priority. In a community participation strategy, GAIA encouraged village health committee members to take on triage and other duties, for which they trained.
The clinic staff developed a routine of giving 'health talks' on a variety of issues (Fig2). As similar projects have found, this strategy assists in crowd management by engaging with waiting patients and communicating important health information13.

Figure 1: Villagers waiting for clinic services.

Figure 2: Mobile Clinic Health Talks Topics 2009.
Because the clinics' operations commenced at the start of the rainy season, many patients presented with the clinical symptoms of malaria. Because of this and other acute presentations, HIV testing and referral services took 3 months to become operational but were fully established in January 2009.
Data
The GAIA clinic project constructed a data collection system under the direction of the DHO, with data points selected to match those already being used by the rural health centers of Malawi's HMIS. Consistent with this, data were collected manually using handwritten reports which were later entered into MS Excel by GAIA and HMIS personnel.
During the first 18 months of data collection, some data points were refined to facilitate comparison between HMIS and mobile clinics; however, some mobile clinic data remains broad, in non-specific diagnostic categories, affecting comparability across clinical sites. For example, in the HMIS system some sites distinguish between dysentery and diarrhea; in other systems, including the GAIA clinics, diarrhea data are collated in a broad diagnostic category. In addition, in Malawi the diagnosis 'clinical malaria' encompasses a broad range of symptoms without laboratory confirmation. Consequently, malaria may be over-diagnosed and other illnesses with similar symptoms may be under-diagnosed14.
The GAIA clinics follow Ministry of Health protocols for malaria. When the clinics began operation, patients were treated presumptively with sulfadoxine and pyrimethamine (Fansidar®), based on clinical symptoms. Patients who did not improve were given a rapid diagnostic test (RDT) and, if positive, were treated with artemisinin therapy (lumefantrine and artemether; LA). Subsequently, LA became the standard treatment, and at the present time, all children under 5 years presenting with the clinical symptoms of malaria are given an RDT and treated with LA if positive. Adults and children aged 5 years and over are treated on the basis of clinical symptoms alone, except if the diagnosis is in doubt, in which case an RDT is performed. If LA treatment is not effective, the second line treatment is quinine.
Another challenge to data collection and analysis is the difficulty of providing patient care while collecting data accurately under emergent conditions. This is especially the case in areas where the number of patients is very high and many are acutely ill and in need of urgent services.
In 2009, the two mobile clinics 'Muloza' and 'Chitakale' (named after the hubs where they are based) had 38 647 client contacts (both new and returning patients). Because the patient-held health passports comprise individual out-patient records in Malawi, individual patient data are not captured at clinic level. Of the 38 647 contacts, 1160 patients were referred to a higher level of care. The most common illnesses seen in the clinics were:
- those under 5 years with clinical malaria (n=11 924)
- upper respiratory infections among patients of all ages (n=6528)
- those over 5 years with clinical malaria (n=3264)
- those under 5 years with clinical pneumonia (n=3141)
- diarrhea among patients of all ages (n=2610).
These disease patterns are consistent with the most common causes of morbidity and mortality in sub-Saharan Africa (Fig3).
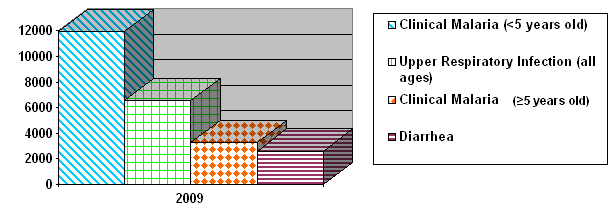
Figure 3: The most common illnesses seen by the Global AIDS Interfaith Alliance (GAIA) mobile clinics.
A total of 714 pregnant women were seen in 2009 at the two clinics and counseled for HIV testing, and 536 (75%) consented to HIV testing. Of these, 20% tested positive. Although referrals for HIV follow up are not captured in the data, mobile clinic protocols require that all patients who test positive for HIV are referred to a health center for treatment and follow up.
As described, patients waiting to see a healthcare provider are likely to participate in educational 'health talks' on a variety of topics, including malaria, sanitation, family planning, HIV and sexually transmitted infections. In 2009 the health talks facilitated 30 887 client contacts.
To assess the impact of the mobile clinics on the catchment areas, collected data were examined on visits from children under 5 years with clinical malaria at both the GAIA mobile clinics in the period April to December 2009. This data point was well-matched with HMIS data collected from health centers designated to served these same catchment areas and reflects the sixth UN millennium development goal (to combat malaria and other diseases). The number of children seen by the health centers and by the GAIA mobile clinics show similar trends, including seasonal impacts; however, the number of children seen by health centers did not decrease after deployment of mobile clinics (Fig4). It may be that the GAIA mobile clinics are providing care to children in remote areas who would otherwise not receive care. The mobile clinics closed for staff leave for 2 weeks in December of 2009, and this is reflected in a drop in the number of children seen for malaria. In the same month, the number of children seen at the health centers increased, and it may be that parents who had been educated about the dangers of malaria sought assistance at the health centers when the mobile clinics were closed.
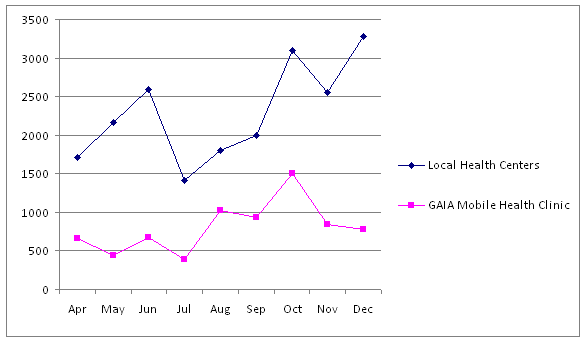
Figure 4: Seasonal variation in the number of children seen for clinical malaria by mobile Global AIDS Interfaith Alliance (GAIA) clinics and at local health centers (April-December 2009).
A number of implementation challenges to deploying mobile clinics in rural Malawi were identified. Initially, medication, supply chain and infrastructure issues as well as government/non-governmental requirements can affect implementation and scheduling. Timelines should be flexible to accommodate unexpected delays.
The scheduling of services should be adapted to local circumstances. Although the primary purpose of these clinics was HIV testing and treatment referral, commencing services during the rainy season demanded a focusing on malaria first and HIV second. Priorities should reflect the exigent needs of the communities.
Assessing the impact of health delivery in Malawi, including that from mobile clinics, remains challenging. Although mobile clinic data points were matched with HMIS variables, gaps in data from both sources and inconsistent variables among sites made direct comparisons difficult. Because each patient visit is recorded separately, it is not possible to determine the true number of patients treated; therefore, drawing conclusions about disease prevalence and co-morbid disease states is constrained.
Data collection is further hampered by existing infrastructure: shortages of personnel, handwritten data-recording, and the competing demands of high patient volume.
Conclusions
Future directions for the mobile clinics include enhanced HIV/AIDS services. As Malawi prepares to meet new WHO guidelines for ART, it has set the ambitious goal of training 4000 healthcare workers in the new protocols. At the same time GAIA is evaluating the feasibility of providing ART through the mobile clinics, especially the monitoring and management of stable patients who have completed the initiation stage of therapy. As the clinical symptoms of malaria is the most common presentation at the clinics, GAIA is considering adding the preventative intervention of bed-net distribution at clinic sites, with education about their use and care. Because clinic staff are fully occupied by existing services, this would require an additional vehicle with dedicated staff.
Despite the challenges, the GAIA mobile clinics have been successfully integrated into catchment area health services, using a community participation model that has worked well in GAIA Malawi village projects. Over the 18 months, the mobile clinic project has provided point-of-care primary health services to thousands of people, incorporated health education, urgent care, disease management, HIV testing, and prenatal services to remote rural villagers (Fig5).

Figure 5: A pregnant woman receives antenatal care at a GAIA mobile clinic.
Finally, strong relationships have been forged with local community leaders and with Malawi Ministry of Health officers. These form the foundation for long-term sustainable engagement and eventual integration of services into Health Ministry programs.
Acknowledgements
The authors gratefully acknowledge the Elizabeth Taylor HIV/AIDS Foundation for its continuous financial support of this project, and note with sadness Dame Elizabeth's death on 23 March 2011. Her support of so many in the struggle against HIV since the early 1980s showed her to be a faithful and persistent soldier for research, inclusiveness, disease prevention and treatment, and a person with overall compassion and respect for all.
References
1. UNAIDS. 09 Epidemic update. (Online) 2009. Available: http://data.unaids.org/pub/Report/2009/JC1700_Epi_Update_2009_en.pdf (Accessed 17 May 2010).
2. National Statistics Office. Population and Housing Census: Preliminary Report. (Online) 2008. Available: www.nso.malawi.net (Accessed 14 March 2010).
3. CIA. World Factbook Malawi. (Online) 2009. Available: https://www.cia.gov/library/publications/the-world-factbook/geos/mi.html (Accessed 17 February 2010).
4. United Nations Malawi. Discover Malawi. (Online) no date. Available: http://www.unmalawi.org/on_mal_discover.html (Accessed 17 May 2010).
5. Ministry of Health. A joint programme of work for a health sector wide approach [2004-2010]. Lilongwe, Malawi: Department of Planning, Ministry of Health, 2004.
6. Government of Malawi. Government of Malawi Ministry of Health Malawi Health Sector Employee Census. Zomba, Malawi: Centre for Social Research, University of Malawi, 2007.
7. Dugger CW. An exodus of African nurses puts infants and the ill in peril. The New York Times, 12 July 2004; A-1.
8. Manafa O, McAuliffe E, Maseko F, Bowie C, Machlachlan M, Normand C. Retention of health workers in Malawi: perspectives of health workers and district management. Human Resources for Health 7: 65. (Online) 2007. Available: http://www.human-resources-health.com/content/7/1/65 (Accessed 17 May 2010).
9. UNAIDS. Malawi. (Online) 2009. Available: www.unaids.org/en/Regionscountries/Countries/Malawi/ (Accessed 24 March 2011).
10. Management Sciences for Health. Evaluation of Malawi's Emergency Human Resources Programme. (Online) 2010. Available: www.msh.org/news-bureau/upload/Evaluation-of-Malawi-s-Emergency-Human-Resources-Programme.pdf (Accessed 24 March 2011).
11. International Treatment Preparedness Coalition. Rationing funds, risking lives: the world backtracks on HIV treatment. (Online) 2010. Available: http://www.who.int/pmnch/ITPCMTT8report.pdf (Accessed 17 May 2010).
12. National Statistical Office. Malawi Demographic and Health Survey (MDHS) 2004. Calverton, MD: NSO and ORC Macro, 2005.
13. Stillman PC, Strong PC. Pre-triage procedures in mobile rural health clinics in Ethiopia. Rural and Remote Health 8: 955. (Online) 2008. Available: www.rrh.org.au (Accessed 8 April 2010)
14. Nankabirwa J, Zurovac D, Njogu JN, Rwakimari JB, Counihan H, Snow RW et al. Malaria misdiagnosis in Uganda - implications for policy change. Malaria Journal 2009: 8: 66.






