Cancer treatments can impose significant psychological and financial burdens on patients for a number of reasons. Financial issues are a common problem for cancer patients, because support is required for medical procedures, services such as physiotherapy and counselling, prostheses, aides, travel and accommodation, along with other practical issues such as child care and 'home help', to name a few. These increased financial requirements may also be coupled with a loss of income, and concerns about financial issues and how to access relevant information, which may influence a patient's treatment and wellbeing.
Such concerns are exacerbated for cancer patients from rural and remote areas, where treatment requires frequent travel to the city. While metropolitan and rural cancer patients have similar needs, higher cancer-related burdens and geography has been identified as a factor for rural patients1. A substantial financial burden accompanies the relocation for treatment, including unexpected costs such as telephone calls, laundry services and pharmaceutical products2. In addition to the financial costs of temporary relocations during treatment, rural families often need to maintain households in two locations while facing a loss of income when a family member is unable to work3. Because rural patients are no longer at home, the patients' (or carers') responsibilities fall to other family members, imposing additional stress and burdens on the family members who have stayed behind. Patients may also experience difficulties if they travel alone, including paying medical expenses and coping with treatment side-effects in a new environment4. The isolation of being in a new environment is also a challenge, and although patients may be able to build a network during their stay in the city, it is lost on their return to the rural area, leading to new feelings of isolation5. Relocation for treatment causes significant disruption in the lives of rural patients6,7.
In order to avoid the difficulties associated with relocation, or because they cannot afford relocation, some rural patients travel back and forth on a daily basis8. Additional travel can cause fatigue and stress8, and the treatment side-effects may also make travelling especially difficult and stressful9. Travel and time costs have been identified as factors in rural women having comparatively lower rates of use of breast-conserving therapy10, and mastectomy may be chosen over adjuvant therapy in order to accelerate the woman's return home11.
Although financial assistance may be available to mitigate the impact of relocation, patient awareness about such support is not always high7,12 and financial assistance may not fully cover the substantial costs associated with treatment relocation12. Rural patients also report other practical needs, including the need for information2 and medical support13. These issues are of concern for large, sparsely populated countries such as Australia, in which 29% of the population lives in rural and remote areas.
In this article, the results of a large survey of the supportive care needs of cancer patients in Western Australia (WA), a large, sparsely populated Australian state, are reported. At the time of the study, the state capital Perth was the only major centre in the state providing cancer services. The geography of WA impacts on residents' access to services and the travel costs associated with this access. This article explores the relationship between the unmet psychological and practical support needs of WA cancer patients and geographic location. Other aspects of the survey, including the identification and comparison of unmet needs across cancer sub-groups (eg lung, breast, prostate), will be reported elsewhere.
Participant recruitment
A random sample of 2079 potential participants was generated at the Western Australian Cancer Registry (WACR). The sample was structured to include all cancer types and geographical areas and with both sexes and randomised within these groups. Participants were considered eligible if they had been diagnosed with cancer between 6 months and 2 years previously. Throughout the recruitment process, a number of death registry checks were undertaken to ensure there was no attempt to contact deceased patients. Treating doctors for the potential participants were identified from WACR records and mailed a letter, a brief précis of the study, a list of their patients to be contacted and a reply paid envelope, as per ethics committee requirements. After the initial mail-out, doctors who did not respond (51%) were sent a reminder letter, with an accompanying list of patients and a reply paid envelope. In this letter, doctors were advised that the research team regarded non-response as indication that they could contact the doctor's patients.
Following these steps, 1770 participants were mailed a letter of invitation, information sheet, 2 questionnaires, WACR pamphlet and a reply paid envelope. The WACR pamphlet explained the function of the registry, how their names were included on the registry, and the process that WACR had undertaken to identify their name for an invitation to participate in the study.
All participants were fully informed of the purpose and procedures of the study and consent was assumed where surveys were returned. Ethics approval for the study was obtained from the Edith Cowan University Ethics Committee and the Confidentiality of Health Information Committee (CHIC).
Survey measures
The Long Form Supportive Care Needs Survey: The Long Form Supportive Care Needs Survey (SCNS-LF59) was used in this survey. The SCNS-LF59 is a reliable (Cronbach's α of 0.87-0.97 for the 5 scales identified with principal components analysis) and valid (face, content and construct validity)14 self-administered instrument for measuring global needs in cancer patients. The SCNS-LF59 needs assessment tool was developed in Australia and is widely used within the Australian context15-17. It takes approximately 20 min to complete and can be understood by people with minimal reading ability15.
The SCNS-LF59 consists of 59 items with 5 domains: (i) psychological; (ii) health system and information; (iii) physical and daily living; (iv) patient care and support; and (v) sexuality. For each item, participants are asked to circle their level of need for help over the last month on a scale of 1 to 5 (1 = not applicable, 2 = satisfied, 3 = low need, 4 = moderate need, 5 = high need). The questionnaire distinguishes 'some need' by combining scores for low, moderate and high needs, as opposed to 'no need' (the combination of scores for not applicable and satisfied).
Needs assessments offer advantages over other methodologies because they address both quality of life and quality of care issues, and enable direct evaluation of patients' perceived needs for help, thus providing indication of needed resources14. Identification of the magnitude of the needs is also possible, thereby allowing individuals and subgroups with higher levels of needs to be identified and targeted with appropriate early intervention, reduction of problems and prioritisation of support.
Demographic questionnaire: A demographic questionnaire was also administered to ascertain participant characteristics including sex, cultural background, educational attainment and employment status.
Assessment of remoteness: To determine metropolitan, rural and remote areas within the study, the Australian Bureau of Statistics (ABS) remoteness classes were adapted18 using the ABS classifications which range from 0 to 4 (0 = major cities, 1 = inner regional, 2 = outer regional, 3 = remote, 4 = very remote). For this study, these classifications were collapsed into 3 categories: (i) metropolitan (ABS classification 0); (ii) rural/regional (ABS classifications 1 and 2); and (iii) remote (ABS classifications 3 and 4). Because numbers were comparatively smaller in the rural and remote categories, the suitability of collapsing the categories into metropolitan/rural/remote rather than metropolitan/rural and remote was checked by re-running the analyses with the latter approach to categorisation. This re-categorisation did not change any of the findings and so the original categorisation was retained.
Data analysis
Only participants who had returned a completed demographic questionnaire and the SCNS-LF59 were included in the final analysis. Missing data were dealt with by imputing the mean score for the variable to replace the missing values. Basic frequencies and percentages were tabulated. The primary analysis was a comparison of proportions reporting 'some need' versus 'no need' across groups for the 15 highest-rated items for 'some need', undertaken with χ2-tests with a p-value of 0.05 used as the measure of significance. Because other researchers have suggested dichotomising the variables to 'moderate to high need' and 'low to no need'15,19, proportions were compared using this dichotomy but with a corrected p-value of 0.01 due to the number of tests undertaken. Finally, although the 15 highest-rated items across the sample were generally the highest-rated items for each geographical group, some items appeared in some groups that did not appear elsewhere, and so χ2-tests for these items (with p = 0.01 as the α value) were undertaken.
Participants
Of the 1770 individuals sent a letter, information sheet, WACR brochure and questionnaires, 829 (47%) returned questionnaires, implying consent. Only participants who returned both the completed demographic questionnaire and the SCNS-LF59 (n = 786; 94.8%) were included in the final analysis. The sample consisted of 382 males and 398 females (6 demographic questionnaires had these data missing); demographic data for participants are provided (Table 1).
Table 1: Participant characteristics (valid percentage in parentheses)
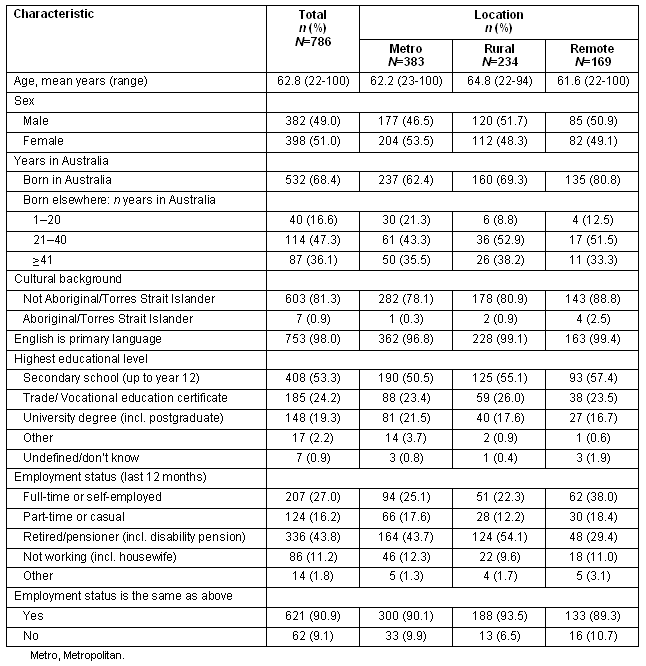
The proportions of participants who were male of Aboriginal/Torres Strait Islander background and spoke English as their primary language were similar across geographic groups. A majority of participants in each group were born in Australia, although this proportion was highest in the remote location group. Proportions were also similar in terms of educational attainment, with a majority in each group completing some form of secondary schooling. Although nearly all participants in each group held the same employment status as they had held for the previous 12 months, this varied across groups with the remote group having the largest proportion of self-employed or full-time workers and the smallest proportion of retirees or pensioners.
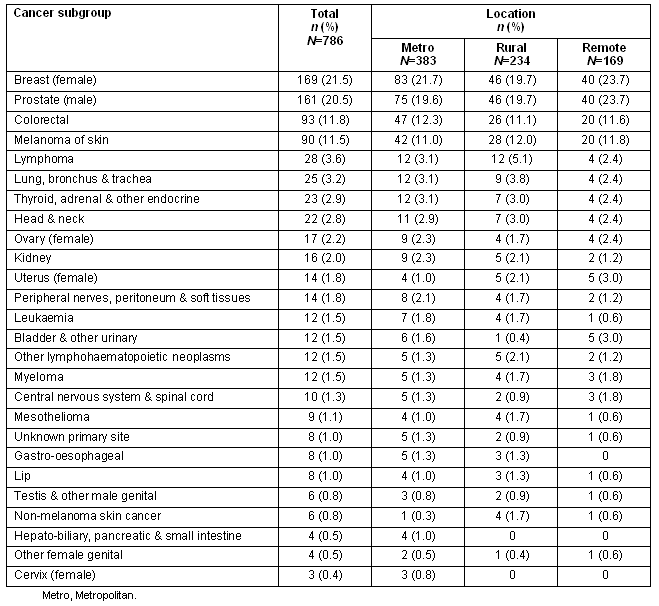
The distribution of cancer subgroups across the sample is presented (Table 2). The percentage of participants reporting each cancer type was similar across metropolitan, rural and remote areas.
Table 2: Number of participants in each cancer subgroup for the total sample and according to location (valid percentage in parentheses)
Unmet needs
As reported elsewhere, at least 20% of the participant sample identified 15 items where they had 'some needs' and the item with the highest number of participants (41%) reporting 'some needs' was 'fears about the cancer returning'20. The 15 items with the highest frequency on the SCNS-LF59 survey for 'some needs' were compared according to participants' location (metropolitan, rural or remote; Table 3).
Table 3: Frequencies for fifteen highest 'some needs' items reported according to participants' location (valid percentage in parentheses)
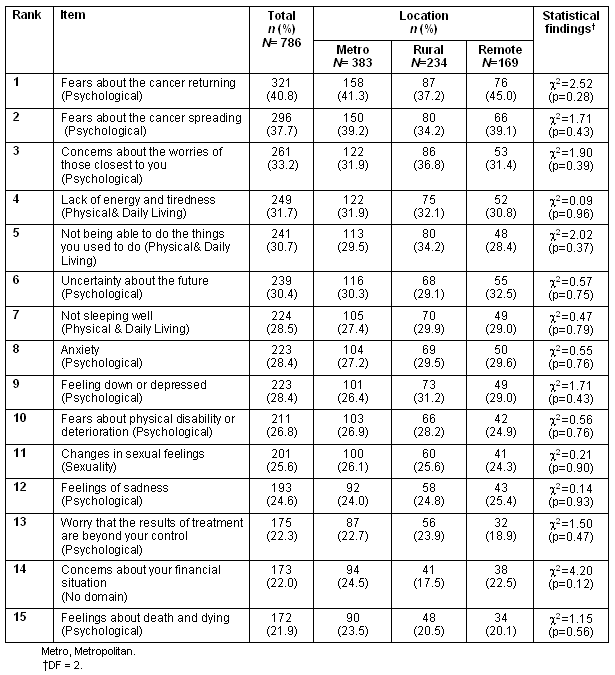
There were no statistically significant differences between the response from individuals in the metropolitan, rural and remote areas for any of the top 15 'some needs' items, with p-values of at least 0.20 seen for all items except 'concern about financial situation' (p = 0.12).
As noted, the top 15 'some needs' items were then compared in terms of 'moderate to high need' against 'low to no need'. No significant differences were found among individuals in metropolitan, rural and remote areas with this comparison (Table 4).
Table 4: Comparison of proportions reporting moderate to high needs on top fifteen 'some needs' items, according to participants' location (valid percentage in parentheses)
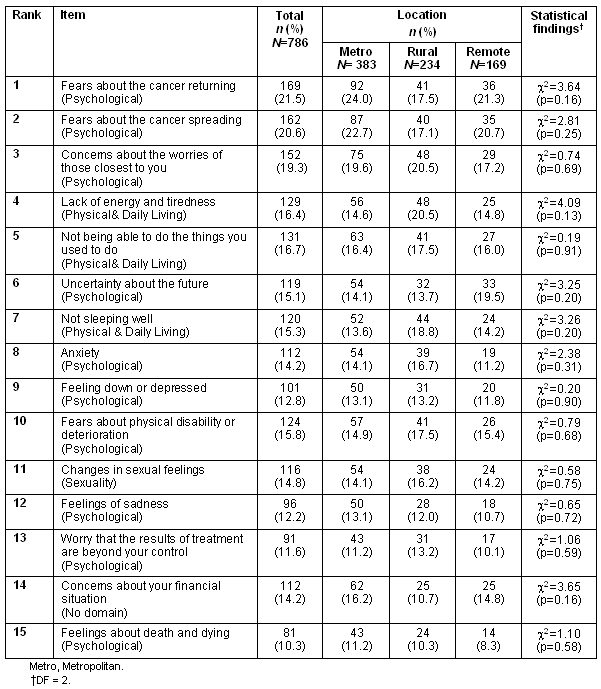
No statistically significant differences were found, and although p-values were smaller than when the variables were dichotomised as 'some to high need'/'no need', all p-values exceeded 0.10.
Finally, the top 15 'some needs' were listed and compared across each geographical group of participants and 5 additional needs (not included in the original list) were identified. These were 'Being informed about things you can do to help yourself get well', 'Work around the home', 'Changes to your usual routine and lifestyle', 'Anxiety about having any treatment' and 'Changes in your sexual relationships'. No significant differences were identified for the proportion of participants reporting 'some needs' for each of these items (Table 5).
Table 5: Comparison of proportions reporting 'some needs' for select items according to participants'location (valid percentage in parentheses)
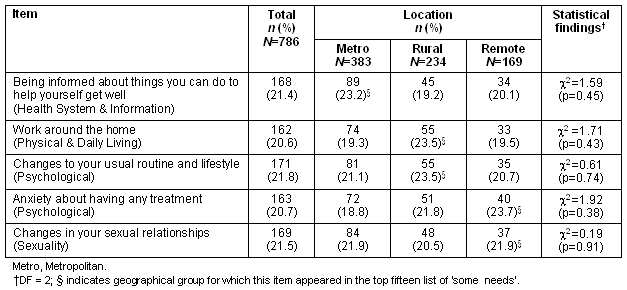
Although there was some variation in terms of which items appeared on the list of top 15 items for each geographically divided group of participants, the differences were small and all p-values exceeded 0.30.
Discussion
The perceived unmet needs of participants in the current study did not differ significantly according to geographical location. This finding is surprising, as it might have been expected that the lower levels of primary health care and supportive-care services in rural and remote WA would adversely impact the unmet needs of cancer patients2. Furthermore, a previous study assessing the needs of breast cancer patients found that location was predictive of higher needs for the 'physical' and 'daily living' domains21. A possible explanation is that the informal support structures (eg friends and families) that exist in rural communities provide a significant source of support to rural cancer patients22,23 and may contribute to reducing patients' unmet needs.
Although needs did not differ among metropolitan, rural and remote participants, our study identified that 'fear regarding the recurrence of cancer', 'psychological concerns' and 'financial concerns' were areas of need for Australian rural patients, and this is consistent with previous research24. Our findings are also consistent with a survey of rural women with breast cancer in Tasmania employing the Supportive Care Needs Survey which found moderate to high needs in the psychological and physical domains and few needs in the health system and information domain25. The authors of the Tasmanian study suggested this was because breast nurses improved supportive-care access and thus met patient needs in that domain25. Similarly, a 2008 study of rural and metropolitan cancer patients in WA found that both groups were satisfied with the quality of care, although rural patients wanted more information26. In another study, cancer nurse coordinators and cancer support workers were identified as playing a key role in improving care for rural WA cancer patients, specifically by improving patients' information and knowledge regarding accessible services and by decreasing the fragmentation of care27. Thus, another explanation for the present study finding of lack of difference in unmet needs across rural and urban populations may be that cancer services in WA were meeting the needs of patients in rural and remote areas.
Study strength and limitations
One of the strengths of this study is that it directly compared the unmet needs of rural, remote and metropolitan populations using a validated and reliable measure. However, this study also had several limitations. Participant numbers for some of the cancers were small and therefore results cannot be generalised to all cancer populations. Only participants who had English literacy skills sufficient to enable them to read and respond to a written questionnaire were considered eligible, potentially resulting in a non-representative sample of the socioeconomic population in WA. This may have particular implications for the findings relating to financial needs. Other limitations relating to the SCNS have been discussed elsewhere20.
The results of the present study provide important information about perceived unmet needs among remote, rural and metropolitan cancer patients in WA, which can guide the development of interventions to meet those needs. The lack of discrepancy among the three populations provides a positive message regarding the state of WA cancer services in rural areas, and the level of support provided to rural WA residents. In light of previous studies identifying high levels of need among remote carers, particularly in terms of health systems and information16, conducting a survey of the unmet needs of rural and remote carers would be an appropriate next step to ensure that cancer services are well equipped to meet the needs of all individuals involved in a patient's cancer journey.
References
1. Hughes PM, Ingleton MC, Noble B, Clark D. Providing cancer and palliative care in rural areas: a review of patient and carer needs. Journal of Palliative Care 2004; 20(1): 44-49.
2. Wilkes LM, White K, Mohan S, Beale B. Accessing metropolitan cancer care services: practical needs of rural families. Journal of Psychosocial Oncology 2006; 24(2): 85-101.
3. McGrath P. "It's horrendous - but really, what can you do?" Preliminary findings on financial impact of relocation for specialist treatment. Australian Health Review 2000; 23(3): 94-103.
4. Fitch MI, Gray RE, McGowan T, Brunskill I, Steggles S, Sellick S et al. Travelling for radiation cancer treatment: patient perspectives. Psychooncology 2003; 12(7): 664-674.
5. Gray RE, James P, Manthorne J, Gould J, Fitch MI. A consultation with Canadian rural women with breast cancer. Health Expectations 2004; 7(1): 40-50.
6. Davis C, Girgis A, Williams P, Beeney L. Needs assessment of rural and remote women travelling to the city for breast cancer treatment. Australian and New Zealand Journal of Public Health 1998; 22(5): 525-527.
7. Davis C, Williams P, Redman S, White K, King E. Assessing the practical and psychosocial needs of rural women with early breast cancer in Australia. Social Work in Health Care 2003; 36(3): 25-36.
8. Hegney D, Pearce S, Rogers-Clark C, Martin-McDonald K, Buikstra E. Close, but still too far. The experience of Australian people with cancer commuting from a regional to a capital city for radiotherapy treatment. European Journal of Cancer Care (England) 2005; 14(1): 75-82.
9. Payne S, Jarrett N, Jeffs D. The impact of travel on cancer patients' experiences of treatment: a literature review. European Journal of Cancer Care (England) 2000; 9(4): 197-203.
10. Bettencourt BA, Schlegel RJ, Talley AE, Molix LA. The breast cancer experience of rural women: a literature review. Psychooncology 2007; 16(10): 875-887.
11. Martin-McDonald K, Rogers-Clark C, Hegney D, McCarthy A, Pearce S. Experiences of regional and rural people with cancer being treated with radiotherapy in a metropolitan centre. International Journal of Nursing Practice 2003; 9(3): 176-182.
12. McGrath P, Seguerra J. The patient transit assistance scheme: a consumer's perspective. Australian Journal of Rural Health 2000; 8(4): 232-238.
13. McGrath P. Returning home after specialist treatment for hematological malignancies: an Australian study. Family & Community Health 2001; 24(2): 36-48.
14. Bonevski B, Sanson-Fisher R, Girgis A, Burton L, Cook P, Boyes A. Evaluation of an instrument to assess the needs of patients with cancer. Supportive Care Review Group. Cancer 2000; 88(1): 217-225
15. Sanson-Fisher R, Girgis A, Boyes A, Bonevski B, Burton L, Cook P. The unmet supportive care needs of patients with cancer. Supportive Care Review Group. Cancer 2000; 88(1): 226-237.
16. Clavarino AM, Lowe JB, Carmont SA, Balanda K. The needs of cancer patients and their families from rural and remote areas of Queensland. Australian Journal of Rural Health 2002; 10(4): 188-195.
17. Aranda S, Schofield P, Weih L, Yates P, Milne D, Faulkner R et al. Mapping the quality of life and unmet needs of urban women with metastatic breast cancer. European Journal of Cancer Care (England) 2005; 14(3): 211-222.
18. Australian Bureau of Statistics. ASGC Remoteness Classification: purpose and use. Census paper no 03/01. Canberra, ACT: ABS, 2003.
19. Janda M, Steginga S, Dunn J, Langbecker D, Walker D, Eakin E. Unmet supportive care needs and interest in services among patients with a brain tumour and their carers. Patient Education and Counseling 2008; 71(2): 251-258.
20. White K, D'Abrew N, Katris P, O'Connor M, Emery L. Mapping the psychosocial and practical support needs of cancer patients in Western Australia. European Journal of Cancer Care 2011; DOI: 10.1111/j.1365-2354.2011.01270.x.
21. Girgis A, Boyes A, Sanson-Fisher RW, Burrows S. Perceived needs of women diagnosed with breast cancer: rural versus urban location. Australian and New Zealand Journal of Public Health 2000; 24(2): 166-173.
22. McGrath P, Patterson C, Yates P, Treloar S, Oldenburg B, Loos C. A study of postdiagnosis breast cancer concerns for women living in rural and remote Queensland. Part II: Support issues. Australian Journal of Rural Health 1999; 7(1): 43-52.
23. McGrath P. Post-treatment support for patients with haematological malignancies: findings from regional, rural and remote Queensland. Australian Health Review 2000; 23(4): 142-150.
24. McGrath P, Patterson C, Yates P, Treloar S, Oldenburg B, Loos C. A study of postdiagnosis breast cancer concerns for women living in rural and remote Queensland. Part I: personal concerns. Australian Journal of Rural Health 1999; 7(1): 34-42.
25. Minstrell M, Winzenberg T, Rankin N, Hughes C, Walker J. Supportive care of rural women with breast cancer in Tasmania, Australia: changing needs over time. Psychooncology 2008; 17(1): 58-65.
26. Hall SE, Holman CD, Threlfall T, Sheiner H, Phillips M, Katriss P et al. Lung cancer: an exploration of patient and general practitioner perspectives on the realities of care in rural Western Australia. Australian Journal of Rural Health 2008; 16(6): 355-362.
27. Drury VB, Inma C. Exploring patient experiences of cancer services in regional Australia. Cancer Nursing 2010; 33(1): E25-31.
