Preparing for the aging of society has remained a common, serious policy challenge among developed countries since the late twentieth century. As the baby-boomer population ages, the demand for healthcare services will rise steeply over the next three decades1.
With the rapid aging of the Japanese population, the number of elderly individuals who require long-term care (LTC) has increased. Many of these individuals do not have, or only have, aged family members to care for them. Against this backdrop, Long-Term Care Insurance (LTCI), a social insurance system that supports LTC for the elderly, was established in 20002-5. In this system, those eligible for LTCI (ie persons aged 40 years or older who pay monthly LTCI premiums) receive a certification of long-term care need based on the judgment of the LTC approval board, which includes a physician. The certification of long-term need is issued by municipalities (villages, towns, cities, and wards of metropolitan cities) which serve as insurers of LTCI.
An insured person requiring LTC can choose either in-home services or in-facility services. In-home services include home-visits by helpers and nurses, day services at care facilities, home-visit bathing services, home-visit rehabilitation, day rehabilitation services, welfare device leasing, and short-stay services at care facilities. In-facility services include institutional care at a LTC welfare facility, which may be regarded as a nursing home for the elderly in other countries, or LTC medical facility, which is a sanatorium-type hospital ward for elderly patients with dementia. Out-of-pocket payment at a fixed rate (10% of the cost of the insured services) and a standard charge for meals are imposed on users of in-facility services, although there is an upper limit to this payment. The amounts of services provided are determined according to the LTC level authorized by the municipality. For example, the limit of monthly benefits provided for in-home services is $2,073 (1 US dollar = 80 yen in 2011) for those classified as Level 1, and $4,479 for those classified as Level 5. For in-facility services, costs are determined based on the facility type and LTC level.
Total expenditure for LTCI has grown from $45 billion in 2000 to $99 billion in 20102. Accordingly, the Japanese government announced plans to eliminate LTC medical facilities and reduce the number of chronic care hospitals by 2011 due to increasing LTC costs and the medical care costs incurred these facilities6. This plan, however, has been temporarily halted due to a change of government. To reduce LTC expenditure, the government currently promotes a shorter hospital stay and discharge of patients to their homes, but not the transfer to other hospitals or LTC facilities7. Even overseas, public policy has shifted over time such that a larger share of resources is allocated to support home-care services given that home care is a lower-cost alternative to institutional care1, which accounts for a large part of government expenditures1,8. However, a review that assessed the effects of institutional versus at-home care for functionally dependent elderly individuals on health outcomes, satisfaction, quality of care, and costs, reported that the results obtained thus far are inconclusive9.
Rural areas have higher proportions of elderly individuals, higher rates of poverty, and less availability of health care due to barriers to care faced by low-income and elderly residents10, as well as a shortage of medical care providers11. If the government promotes in-home LTC services, can disabled elderly living in rural areas be discharged from institutions to their home? This study examines the effectiveness of the deinstitutionalization of disabled elderly individuals for the purpose of cost reduction, and clarifies the policy issues surrounding an aging society.
Setting
This study was conducted in Town A in rural Hokkaido. Town A has a population of 9600, of which 25% are elderly individuals. This is higher than the national average of 21.5% as of 2007.
There is also a shortage of LTCI services, and the residents of Town A do not have access to home-rehabilitation or home bathing services. The alternatives to these services are day services, home-visit helper services, and home-visit nursing; however, the provision of these services is insufficient due to a shortage of specialist personnel in rural areas. Furthermore, a short-stay respite service has only seven beds available, with just two beds available for accepting patients who need medical care. In addition, there is a constant waiting list of 20-30 people for admission to LTC welfare facilities.
Population
A survey was conducted of residents of Town A, who were staying at any of two LTC welfare facilities, one LTC medical facility, and two chronic hospitals as of 1 July 2007.
All participants were aged over 65 years and classified as having a Care Needs Level of 1 to 5. Individuals classified as Level 1 require partial care, whereas those classified as Level 5 are unable to conduct daily activities without extensive assistance5.
Complete data were obtained for all 139 individuals in the study population (mean age, 85.3 years). Of these, 30% were men, 20% were living alone, and 40% were classified as Care Needs Level 5. The mean length of hospital or facility stay was 2.6 years (range 1-15 years). 'Patient's or family's hope' and 'Having no caregivers at home' were indicated as the primary reasons for long-term stay.
Data collection
Data were collected from LTCI claim records from July 2007 for LTC welfare/medical facilities, and medical care claim records from July 2007 for chronic hospitals. The LTCI claim records included monthly information regarding age, sex, Care Needs Level, utilization of services, and LTC costs. Medical care claim records included monthly information regarding age, sex, illness, length of hospital stay, and hospital costs.
An original questionnaire survey was conducted among institutional staff to obtain information about basic demographics, Activities of Daily Living (ADL) and Instrumental Activities of Daily Living (IADL), and medical care. In addition, respondents were asked to predict potential issues at home regarding patients' behavioral problems should they be discharged to their homes. Each item of ADL, IADL, and medical care had two answer choices: 1 for 'without assistance', and 0 for 'need assistance'. For a response of 'need assistance', three additional questions were asked: (i) How many times a day/week? (ii) How long does it take? and (iii) How many personnel are required?
Retrospective data were also collected on existing home care costs for disabled elderly individuals living at home in Town A, which included costs for welfare equipment rentals and guidance on management of in-home medical LTC, and care manager fees. These LTCI services are commonly utilized by elderly individuals irrespective of the degree of disability.
Selection of candidates for discharge/deinstitutionalization
Candidates were selected for deinstitutionalization among the participants, excluding those who were considered unable to stay alone at home, that is, those with behavioral problems, at risk of falling, or requiring medical care that could only be provided at a hospital. Exclusion criteria were evaluated by home care specialists such as visiting nurses or care managers who coordinate LTCI services provided in the community for most disabled elderly individuals living at home. A total of 52 patients were excluded for reasons such as high risk of falling (n=14), catheter removal (n=2), behavioral issues (n=12), prowling (n=13), possibility of sudden change in condition (n=3), severe cognitive disorder (n=4), threat to life (n=16), and ongoing medical care at a hospital (n=12).
Formulation of post-discharge home care plans
Based on the questionnaire responses regarding ADL, IADL, and medical care, nurses and care managers formulated post-discharge home care plans for the selected participants.
In formulating the care plans, regularly used services were focused on, and informal care services or services that take less than 20 min were excluded, given that the utilization of informal care varies significantly among individuals, and that only nursing care services that require at least 20 min are included in LTCI services. Also included were at-home bathing services, since bathing is an important custom for the Japanese and the elderly in particular prefer baths to showers.
The LTCI provides three types of bathing services for elderly who require bathing assistance: (i) home-visit helper services; (ii) home-visit bathing services; and (iii) day services. Home-visit helper services involve home helpers visiting the elderly and assisting with bathing at home. These services, however, are only available to partially handicapped individuals. It is also worth noting that most bathtubs in Japanese households are too small for the provision of extensive bathing assistance. Therefore, LTCI provides home-visit bathing services in which a vehicle equipped with a portable bath is brought to the home, or day services, which provide the elderly with transportation to a facility where they can receive bathing, meal, and exercise services. These services are available to individuals with a severe physical disability. As there are no home-visit bathing services available in Town A, either home-visit helper services or day services for bathing were included in care plans.
Next, with home-visit nurses and care managers, the manpower necessary for adequately providing care services were assessed, and the time and frequency of utilizing the services. For example, if a person required two helpers at a facility due to his/her weight when changing a diaper, a care plan was formulated that included two home-visit helpers. The time of day for utilizing services is dependent on the participant's needs, so if a participant required services at night, early evening, or early morning, these were added to the day services. The frequency of utilizing bathing services was set at 2-3 times a week because the results from the questionnaires revealed that most participants bathed 2-3 times per week at institutions.
Consequently, four patterns of post-discharge home care plans were formulated for the selected participants. For the purpose of this study, four patterns were chosen that utilized home-visit helper services alone, or in combination with day services. The first pattern utilized home-visit helper services during the day and evening hours without utilization of day services. The second pattern utilized home-visit helper services during the day, evening hours, and night, without utilization of day services. The third pattern utilized home-visit helper services during the day in combination with day services three times a week. Finally, the fourth pattern utilized home-visit helper services during day, evening hours, and night, in combination with day services three times a week. Disabled elderly people living at home usually require home care services during the day and evening hours, but not so much during the night. Participants who required night care, such as aspiration or safety confirmation, were assigned to either the second or fourth pattern.
Figure 1 illustrates the four weekly post-discharge home care plans for the selected participants. This schedule applied to the majority of participants with severe disabilities who required assistance for ADL and IADL (eg diaper change, bathing, dressing, food preparation, shopping) but not medical care.
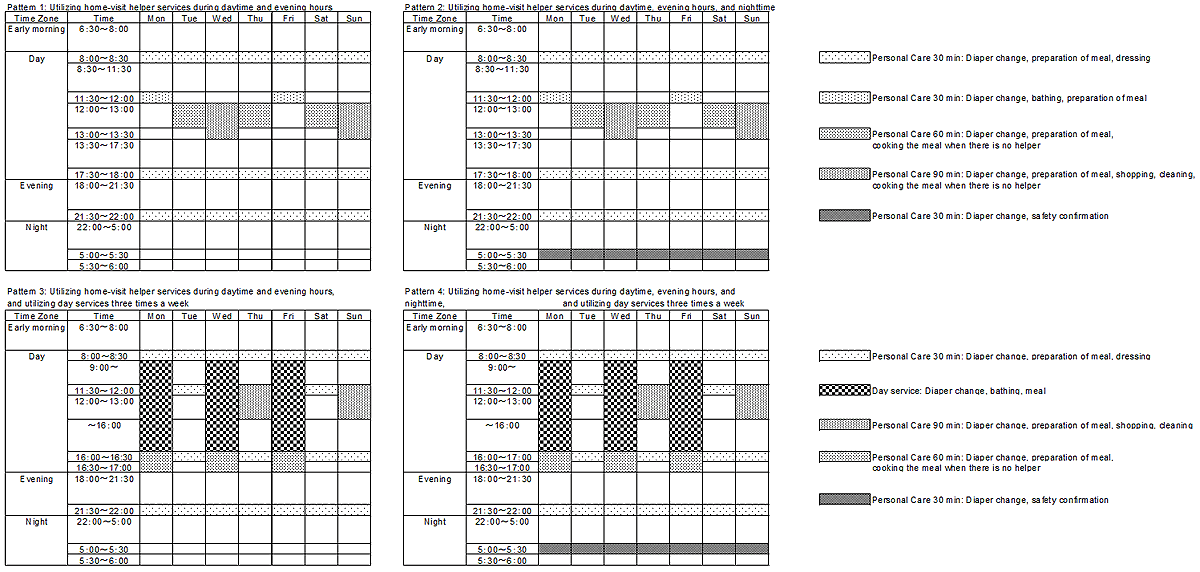
Figure 1: Proposed post-discharge home care plans. Plans are for participants classified as 'Care Needs Level 4', who require assistance
for ADL and IADL (eg diaper change, bathing, dressing, food preparation, shopping), but not medical care.
Calculation of existing institutional care costs and estimated home care costs
The existing costs of LTC welfare facilities and LTC medical facilities were determined based on LTC costs stated in LTCI claim records, which included insurance burden and co-payments. Medical care costs for participants institutionalized in the chronic hospital also included insurance burden and co-payments. Existing LTC costs included LTC facility fees and meals and extra room charges; whereas, medical care costs included medical administration fees and meals and extra room charges.
Total LTC costs for home care were then estimated for participant populations according to the formulated home care plans. Total estimated costs were calculated based on the following requirements: participants pay 10% of home care costs (90% is covered by the insurer); when service costs exceed the limit of benefits, participants must pay the excess. The LTC costs for home care were then estimated according to service reimbursements determined by LTCI. These estimated costs included the service costs of home-visit helpers, home-visit nurses, and day services. In addition to the estimated LTC costs, mean costs for welfare equipment rentals and guidance on management of in-home medical LTC for participants living at home were also included, as well as care manager fees for July 2007. These are services commonly used by those who receive home care services. Outpatient treatment fees, doctors' visiting fees, or pharmaceutical administration costs were not included because these costs differ among individuals.
Examination
The existing costs were examined and estimated home care costs calculated assuming that participants would be discharged from institutions to their homes. Existing costs were expressed as median (min-max), and for each, a percentage was obtained. The estimated home care costs were then compared with the existing institutional costs through stratification of Care Needs Level and facility type using the Wilcoxon signed ranks test, and p<0.05 was considered statistically significant. Existing costs and estimated home care costs are presented using the exchange rate for 2007 (ie 121 yen to the dollar).
Existing costs were converted to monthly costs using the median daily cost in cases where the length of facility stay was less than 31 days.
Ethics approval
This study was approved by the Ethics Committee of the University of Tokyo. Protection of personal information was ensured by keeping the data in a locked cabinet with restricted access. Consent was obtained and based on a comprehensive explanation of the study's purpose via a poster in the town office.
Participant characteristics
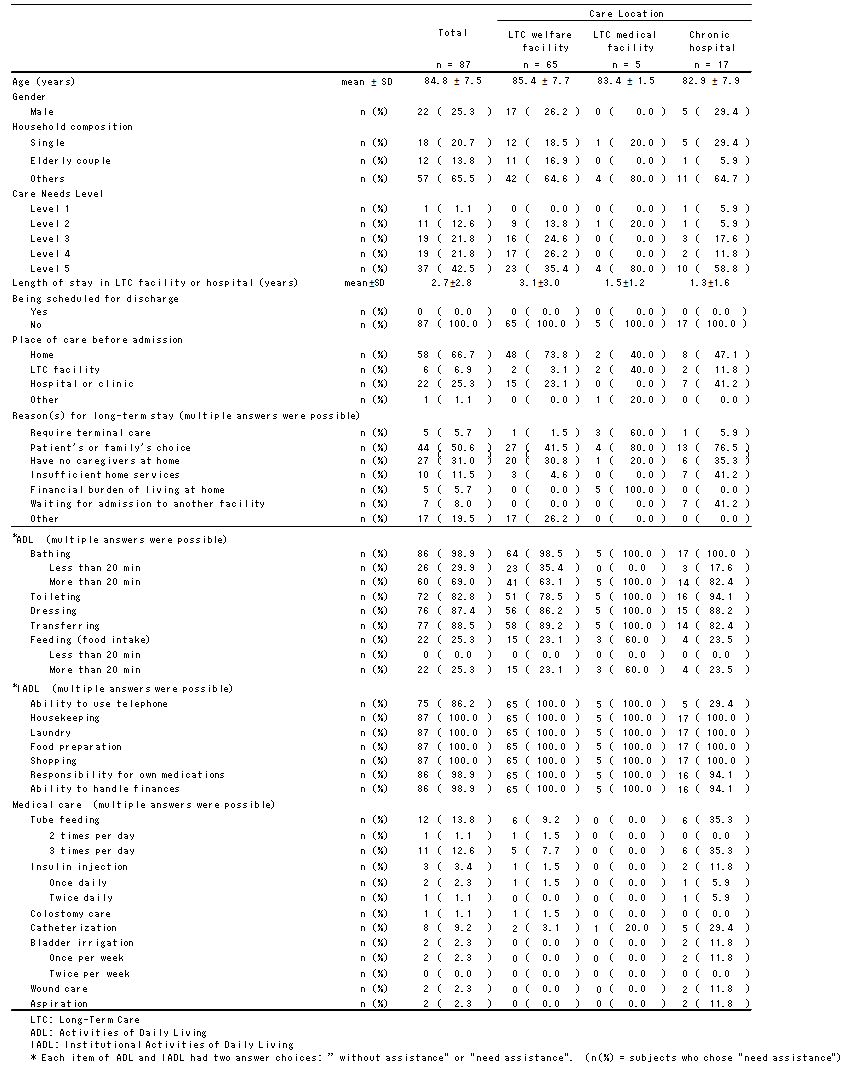
Table 1 summarizes participant characteristics. The mean age of participants was 85 years; 25% were men, 21% were living alone, and the majority was classified as Care Needs Level 5.
Thirty-seven of 87 participants who were candidates for deinstitutionalization were able to take a bath in their home bathtubs, while others required utilization of day services for bathing. As for ADL and IADL, most participants needed assistance with bathing, housekeeping, laundry, food preparation, and shopping. Some participants required medical care, although 12 required tube feeding. The law states that, with the exception of some special cases, tube feeding can only be performed by medical care personnel. Accordingly, the provision of medical care by home-visit nurses was incorporated into the home care plans.
Table 1: Participant characteristics
Comparison of existing institutional care costs and estimated home care costs
Thirty-seven participants who were able to take baths at home were assigned to patterns 1 and 2. Eighty-seven participants, including 50 who could not take baths at home, were assigned to patterns 3 and 4. Patterns 3 and 4 utilized a combination of home care and day services.
Table 2 shows the comparison of the median of existing institutional care costs and estimated home care costs for patterns 1 and 2. The median of existing costs for the 37 participants was $2,495/month (range $2,306-3,743/month), whereas the medians of estimated costs were $3,449/month (range $782-4,222/month) for pattern 1 (p=0.345) and $4,422/month (range $782-5,245) for pattern 2 (p=0.004) (data not shown). When Care Needs Level was considered by facility type, the median of existing costs was $2,300-2,700/month at LTC welfare facilities, $3,700/month at the LTC medical facility, and $2,500-2,600/month at chronic hospitals. The median of estimated costs for pattern 1 was $1,800-3,500/month at LTC welfare facilities, $3,500/month at the LTC medical facility, and $800-4,200/month at chronic hospitals. The median of estimated costs in pattern 2 was approximately $1,000 higher than pattern 1 because pattern 2 utilized home-visit helper services during the night. The higher the Care Needs Level, the larger the estimated costs were, reflecting the greater degree of professional care needed. The medians of estimated home care costs for patterns 1 and 2 were higher than those of existing institutional costs, except for the following participants: those classified as Care Needs Level 2 in LTC welfare facilities, Care Needs Level 5 in the LTC medical facility, Care Needs Level 1 in chronic hospitals, and Care Needs Level 3 in chronic hospitals (pattern 1 only).
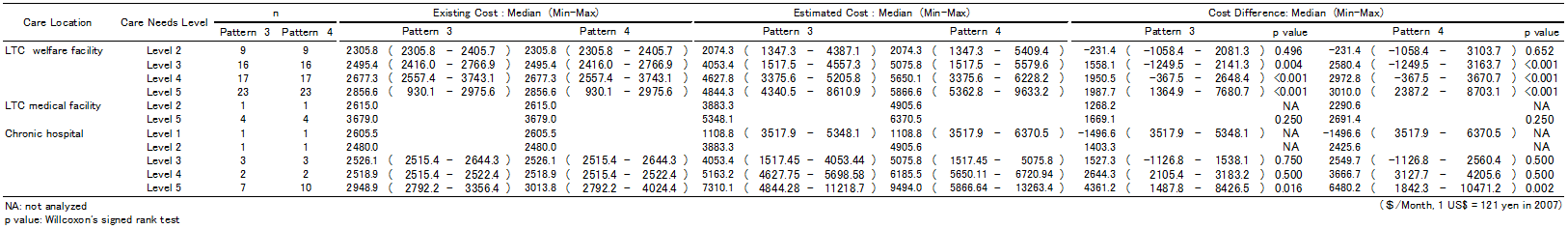
Table 3 shows the comparison of median existing institutional costs and estimated home care costs for patterns 3 and 4. The median of existing costs for all 84 participants, excluding three who needed care at night, was $2,677/month (range $930-3,743/month), whereas the median of estimated home care costs for pattern 3 was $4,593/month (range $1,109-11,219/month) (p<0.001) (data not shown). The median of existing costs for all 87 participants was $2,677/month (range $930-4,024/month), whereas the median of estimated costs was $5,650/month (range $1,109-13,263/month) for pattern 4 (p<0.001) (data not shown). When Care Needs Level was considered by facility type, the median of existing costs for pattern 3 was $2,300-2,900/month at LTC welfare facilities, $2,600-3,700/month at the LTC medical facility, and $2,500-3,000/month at chronic hospitals. However, the median of estimated costs for pattern 3 was $2,000-4,800/month at LTC welfare facilities, $3,900-5,300/month at the LTC medical facility, and $1,100-7,300/month at chronic hospitals. The median of estimated costs for pattern 4 was $1,000-2,200 higher than that of pattern 3 because pattern 4 utilized home-visit helper services and nursing care services at night. Compared with the median of existing institutional care costs, the median of estimated costs was higher, except for participants classified as Care Needs Level 2 in LTC welfare facilities and Care Needs Level 1 in chronic hospitals. For both patterns 3 and 4, estimated costs also increased with increasing Care Needs Level; estimated costs for Level 5 participants were 1.5- to 3.2-fold higher than existing institutional costs.
Table 2: Comparison of the median (min-max) of existing institutional care costs and estimated home care costs (Patterns 1 and 2)
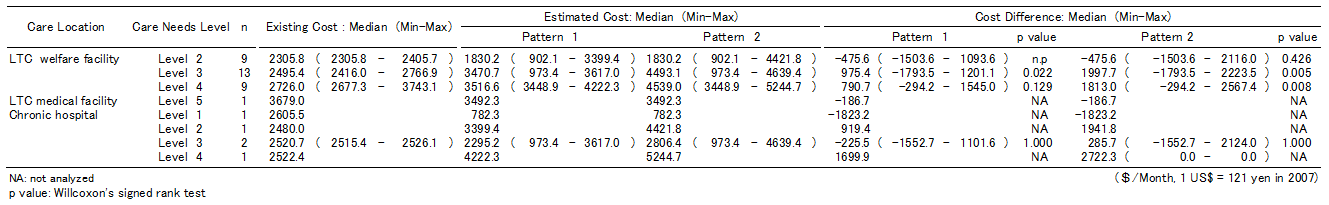
Table 3: Comparison of the median (min-max) of existing institutional care costs and estimated home care costs (Patterns 3 and 4)
Discussion
This study found that estimated home care costs are higher than institutional care costs. The results indicate that deinstitutionalization of the elderly would not contribute to the reduction of healthcare costs.
In this study, 87 of 139 patients were considered candidates for deinstitutionalization at the discretion of care managers and home visiting nurses. Participants had been institutionalized for a long period, and one-third of participants consisted of single elderly or elderly couples with no caregivers at home. Residents in rural areas utilize fewer informal sources of assistance12, and due to the rapidly aging population in these areas, only a minority can receive sufficient informal care. In this regard, the serious shortage of healthcare facilities for the disabled elderly should be taken into consideration, as well as shortages of medical care and LTCI service providers in rural areas such as Town A. Hokkaido's population is aging rapidly and there are climate problems, such as heavy snowfall, and geographic issues, such as a long distances between houses to consider. Thus, providing care to elderly living at home is challenging given the limited access to medical care and availability of in-home LTCI services. As a result, the elderly face a barrier to receiving adequate care9.
The study revealed that estimated monthly home care costs per person were higher than existing monthly institutional care costs; estimated costs increased with increasing Care Needs Level. Estimated home care costs were higher than existing institutional care costs in 24 of 37 participants assigned to patterns 1 and 2, 74 of 84 assigned to pattern 3, and 77 of 87 assigned to pattern 4. Some studies suggest that home care is less costly than institutional care12-15. In contrast, the present results were in agreement with other reports claiming that home care costs are higher than in-facility care costs16,17. Consistent with this, Lian et al reported that home care for a patient with a high degree of dependence could be more expensive than care provided at a nursing home facility when both family costs and provider costs are considered18,19.
The ratio of care facilities which provide care for people with mild disabilities to the elderly population in Japan is low compared with other developed countries20. The present results suggest that more institutions and support facilities are needed that provide care for elderly people who have severe disabilities or live in sparsely populated areas.
Limitations
There are a number of limitations to this study. First, cross-sectional data were used to estimate costs; it was not possible to use actual home care costs. Accordingly, there is a possibility that estimated costs may have been overestimated. Some studies have performed cost comparisons between in-home care and nursing home care15,21, in which costs for care between those living at home and those living in nursing homes were compared. However, there were differences in both disability levels and the existence of informal caregivers between the two care settings18,19. In this study, nurses and care managers formulated post-discharge home care plans, and thus the data should accurately reflect the real state of the community. Second, the study was conducted in only one town, so care must be used in generalizing the results to a larger population. However, Town A is located in a typical rural area in Japan, so a similar cost trend may be found in areas with similar populations. Third, this study only compared costs and did not evaluate quality of care or improvements in physical or mental function, mortality, satisfaction, and quality of life. A more detailed future study should be conducted to address these issues.
Despite these limitations, the results contribute greatly to the identification of characteristics of LTC facility residents, and provide meaningful insights into the healthcare system in aging societies.
Almost all the study participants residing in institutions required assistance with ADL, IADL, and medical care. The estimates revealed that LTC costs would be higher if facility residents were to be deinstitutionalized, compared with existing costs of institutional care. The finding suggests that elderly individuals with severe disabilities may add a social and financial burden if they were to be discharged and received home care.
Acknowledgements
The authors extend their appreciation to the staff of the town office, the hospital offices, and the LTC institution in Town A for their assistance in data presentation. The authors also acknowledge and thank the individuals who reviewed the manuscript.
References
1. OECD Health Project. Long-term care for older people. Paris, OECD, 2005;1-137.
2. Ministry of Health, Labour and Welfare. Overview of the Long-Term Care Insurance System. (Online) 2008. Available: http://www.mhlw.go.jp/english/wp/policy/dl/03.pdf (Accessed 25 June 2012).
3. Naoki Ikegami. Rationale, design and sustainability of Long-Term Care Insurance in Japan - In Retrospect. Social Policy & Society 2007; 6(3): 423-434.
4. Crocker Houde S, Gautam R, Kai I. Long-term care insurance in Japan implication for US Long-term Care Policy. Journal of Gerontological Nursing 2007; 33(1): 7-13.
5. Tsutsui T, Muramatsu N. Care-Needs Certification in the Long-Term Care Insurance System of Japan. Journal of the American Geriatrics Society 2005; 53(3): 521-527.
6. Ministry of Health, Labour and Welfare. [Reorganization of a convalescent bed and assistance measures for switching from a convalescent bed to healthcare facility]. (Online) 2010. Available: http://www.mhlw.go.jp/stf/shingi/2r9852000000xgrs-att/2r9852000000xgy5.pdf (Accessed 4 September 2012). (In Japanese)
7. Ministry of Health, Labour and Welfare. Plan for proper medical care costs. (Online) 2008. Available: http://www.mhlw.go.jp/bunya/shakaihosho/iryouseido01/pdf/info02_21.pdf (Accessed 25 June 2012). (In Japanese)
8. Stewart KA, Grabowski DC, Lakdawalla DN. Annual Expenditures for Nursing Home Care Private and Public Payer Price Growth, 1977 to 2004. Medical Care 2009; 47(3): 295-301.
9. Mottram P, Pitkala K, Lees C. Institutional versus at-home long term care for functionally dependent older people. Cochrane Database Systematic Review 2007; 17(4): CD003542.
10. Ormond BA, Wallin S, Goldenson SM. Supporting the Rural Health Care Safety Net. Occasional Papers 2000; 36: 1-50.
11. Hart LG, Salsberg E, Phillips DM, Lishner DM. Rural Health Care Providers in the United States. Journal of Rural Health 2002; 18: 211-232.
12. Weissert WG, Lesnick T, Musliner M, Foley ka. Cost Savings from Home and Community-Based Services: Arizona's Capitated Medicaid Long-Term Care Program. Journal of Health Politics, Policy and Law 1997; 22(6): 1329-1357.
13. Bachelard B, Tinturier G. Long-term institutional care or home care? What is the best solution for the Canton of Vaud? Health Policy 1988; 10: 57-63.
14. Chappell NL, Havens E, Hollander MJ, Miller JA, McWilliam C. Comparative Costs of Home Care and Residential Care. The Gerontologist 2004; 44(3): 389-400.
15. Charles KK, Sevak P. Can family caregiving substitute for nursing home care? Journal of Health Economics 2005; 24: 1174-1190.
16. Thornton C, Dunstan SM, Kemper P. The Evaluation of the National Long Term Care Demonstration: 8. The Effect of Channeling on Health and Long-Term Care Costs. Health Services Research 1988; 23(1): 129-142.
17. Weissert WG. Seven Reasons Why It Is So Difficult To Make Community-Based Long-Term Care Cost-Effective. Health Services Research 1985; 20(4): 423-433.
18. Chiu L, Tang K-Y, Shyu W-C, Huang CL, Wang SP. Cost Analyses of Home Care and Nursing Home Services in the Southern Taiwan Area. Public Health Nursing 2000; 17(5): 325-335.
19. Chiu L, Tang K-Y, Shyu W-C. Cost comparisons between family-based care and nursing home care for dementia. Journal of Advanced Nursing 1999; 29(4): 1005-1012.
20. Ministry of Health, Labour and Welfare. Plan for Community Care Improvement. (Online) 2007. Available: http://www.mhlw.go.jp/bunya/shakaihosho/iryouseido01/pdf/04-2c_59-122.pdf (Accessed 25 June 2012). (In Japanese)
21. Weissert WG, Scanlon WJ. Determinants of Nursing Home Discharge Status. Medical Care 1985; 23: 333-343.
