The mobilization and strengthening of human resources for health is central to building sustainable health systems. This will assist in meeting the UN's health Millennium Development Goals (MDGs) and improving health outcomes1. Many low and middle income countries suffer from severe health staff shortages and/or maldistribution which weakens the health system. The African region, compared with other WHO regions, is particularly affected by severe health staff shortages, having only 150 708 physicians (2/10 000 population)2. Sub-Saharan Africa is estimated to need at least 1 million additional health workers in order to offer the basic services consistent with reaching the MDGs1. Low and middle income countries face the challenges of producing adequate numbers of heath workers, retaining those workers in the country after graduation, and distributing them rationally within country.
West African Ghana was recently re-classified from low- to a lower-middle-income country3. The UN lists Ghana as a medium human development country, ranked 135th of 177 countries, based on life expectancy, adult literacy, educational enrolment, and per-capita income4. Official estimates of working physicians in Ghana range from 2442 to 32402,5. However, Ghana has one of the highest physician emigration rates in the world6, with 61% of medical school graduates between 1985 and 1994 leaving the country7. It has been estimated that up 30% of Ghana's potential medical workforce is practicing in the USA8. The migration of physicians from Ghana represents a lost investment of significant training costs, which are heavily subsidized by the Ghanaian Government7.
Health worker shortages and maldistribution are comprise significant threats to the Ghanaian health system9,10. Recruitment and retention of staff for rural facilities has been particularly problematic, with the Ministry of Health (MOH) citing problems with accommodation, children's education, and workload as major challenges11. Over two-thirds of physicians practicing in Ghana work in one of the country's two largest cities, Accra and Kumasi5, while almost two-thirds of Ghana's 24.2 million citizens live in rural areas, with doctor-to-population ratios ranging from 1:5000 in Greater Accra to 1:92 000 in the rural North12. One study revealed that most doctors posted to rural sites either failed to report to their stations or moved out of the country soon after reporting7.
There are relatively few proven strategies to recruit and retain physicians in rural areas, particularly in low income countries13. Research in the area has identified a number of factors that affect healthcare workers' motivation to work in rural/deprived areas or emigrate, including wages, working conditions, career development, equipment and infrastructure, colleagues in the workplace, management, spousal satisfaction, educational opportunities for children, and proximity to extended family and social groups14-17. It has been shown that to reduce migration, improving working and living conditions may be more effective than increasing wages18-20.
In addition to work-related issues, factors across the lifecourse may contribute to a physician's decision to move to a rural area. For example, medical students of rural origin are more likely to choose rural careers21-27. However, the decision to practice in a rural location is likely to be the result of a complex interaction of many factors14,28. Research from high-income nations suggests that parental education may play an important role. For example, a Canadian study found that students interested in rural family medicine were more likely to have graduated from a rural high school or to have family in a rural location and were less likely to have university-educated parents than those interested in another specialty29,30. However, little is known about the impact of childhood experiences and socioeconomic background on the likelihood of rural service in Africa. Such information could be valuable to medical schools in low-income countries aiming to produce an equitable physician workforce.
This study was part of a broad study into factors contributing to the rural practice and emigration of health workers in Ghana that utilized survey data from all fourth year medical students. Earlier analyses demonstrated that improved equipment, supportive management, shorter contracts and salary bonuses were associated with a higher probability of choosing a rural posting31. However, neither intrinsic motivational factors (such as a desire to help others) nor extrinsic motivational factors (such as social status/prestige) contributed to a willingness to work in a rural area32. The current study examined how lifetime exposure to rural areas, international travel and parental circumstances affect willingness to work in a rural/deprived area and consideration of emigration.
Setting and sample
Ghanaian medical education consists of 3 years of basic science/para-clinical studies, 3 years of clinical training at a teaching hospital, and a two-year rotating housemanship. There are four medical schools in Ghana: the University of Ghana (UG); Kwame Nkrumah University of Science and Technology (KNUST); University for Development Studies (UDS); and University of Cape Coast (UCC). At the time of this study, all fourth-year UDS students were training at UG or KNUST teaching hospitals, while the UCC medical school, which began accepting students in 2007, had no fourth-year students.
Fourth-year medical students were selected for this study because they had experienced the clinical environment, but had not yet made placement decisions. All fourth-year students in the country were recruited to participate; no sampling was conducted. The survey was administered and completed during the month of May, 2009, at UG in Accra and KNUST in Kumasi.
Ethics approval
Ethics approval was obtained from the Ghana Health Service Ethical Review Committee; the UG Medical School; the KNUST Committee on Human Research, Publications, and Ethics; and the University of Michigan Institutional Review Board (HUM00029101). Informed consent was obtained from respondents prior to their participation.
Survey and statistical analysis
To develop the survey instrument, seven focus groups were conducted with third and fifth year medical students at UG and KNUST in an approach previously described by Kruk et al31. The survey instrument generated was self-administered in campus computer labs with study personnel available to answer questions. Data were collected on flash drives and then merged into the study database. The instrument collected information about respondents' demographic background, international and rural experiences, and future career plans. Where appropriate, similar response options to the Ghana Demographic and Health Survey were included. Variables of interest included: university, sex, marital status, birth location, pre-studies location, rural and international living experience, and parental professional and educational status (PPES). High (vs low) PPES was defined as having (vs not having) a mother and/or father who is a university-trained professional (eg doctor, lawyer, engineer, accountant, technical). Rural exposure was measured by examining respondents' birth location, the location where they lived prior to their medical studies, and by asking if they had ever lived in a rural area from the age of 5 years. Given the authors' interest in exploring the joint influence of rural and international exposure on the dependent variables, international living experience (in any country outside Ghana and at any age) and rural living experiences (from age five years) were combined into a single four-category variable for this analysis.
Outcomes of interest included willingness to work in a deprived area and considering emigration following graduation. 'Deprived area' is a term used by the Ghanaian MOH to describe a rural area that is distant from large cities and has few social amenities such as schools, roads, pipe-borne water. Students were asked to rate how likely they were to work in a deprived area at some point in the future. Those responding 'I will definitely work in a deprived area' or 'I am likely to work in a deprived area' were coded as willing, while those responding 'I will definitely not work in a deprived area' or 'I am unlikely to work in a deprived area' were considered unwilling to work in a deprived area. Finally, students were asked if they had considered emigrating to another country to work after graduation (yes/no).
The software STATA v10.1 (www.stata.com) was used for the statistical analyses. Bivariate associations and 95% confidence intervals (CI) were estimated using logistic regression. Characteristics associated with an outcome in bivariate analyses at the level p<0.05 were included in multivariate logistic regression.
Of 310 fourth-year medical students, 307 students (99%) participated in the survey. Five survey files were corrupted or lost due to equipment malfunction during survey administration. Of the 302 respondents with complete data, 40 were international students and 34 had missing data on the outcomes of interest, resulting in a final sample of 228 students. The mean survey time was 32.2 min (SD 13.0).
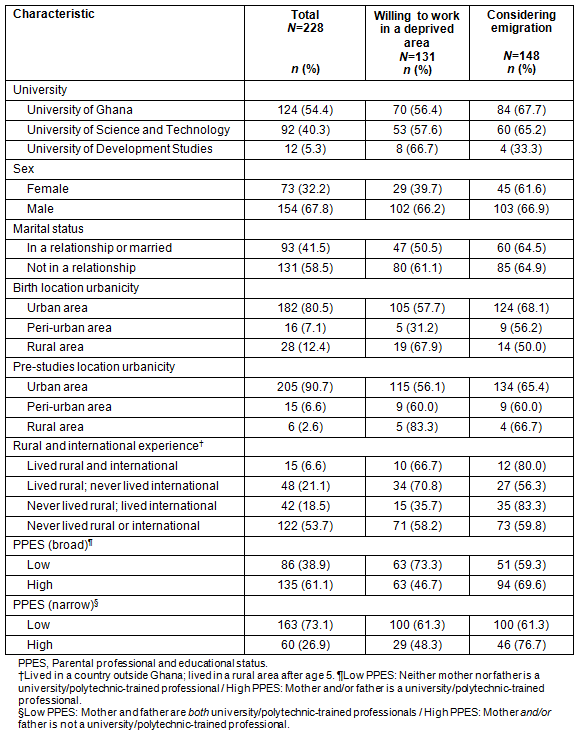
Demographic characteristics and rural and international experiences are shown (Table 1). Approximately two-thirds of students were male (67.8%) and few students were born in a rural area (12.4%). Most students had never lived in a rural or international setting (53.7%) and few students had lived in both (6.6%). Most respondents (>60%) came from high PPES families. Over half were willing to work in a deprived area (57.4%) and almost two-thirds had considered emigration (64.9%).
Table 1: Ghanaian medical students' demographic characteristics and willingness to work
in a deprived area and consideration of emigration after graduation, N=228
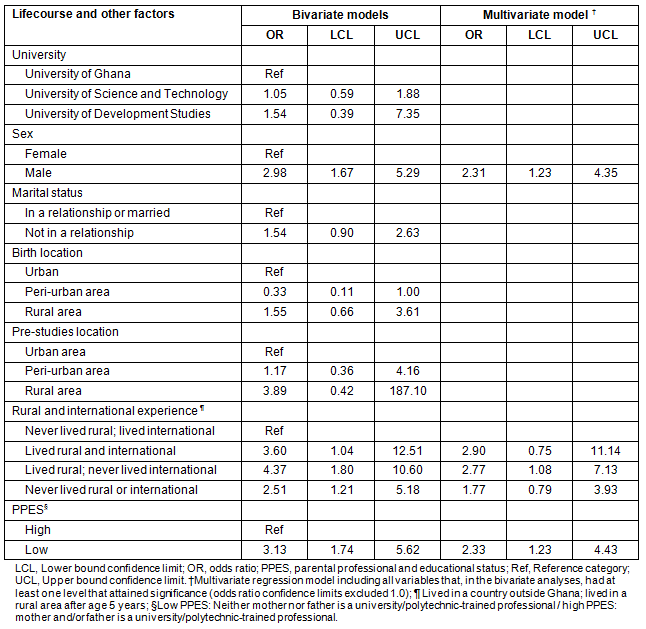
The results of the bivariate analyses of lifecourse factors and willingness to work in a deprived area are shown (Table 2). Male students were almost three times as likely to report willingness to work in a deprived area (OR 2.98, 95%CI: 1.67-5.29). Students with rural but no international experience were most likely to report willingness to work in a deprived area (OR 4.37, 95%CI: 1.80-10.60), followed by those with both rural and international experience (OR 3.60, 95%CI: 1.04-12.51), and those with neither rural nor international experience (OR 2.51, 95%CI: 1.21-5.18). Those with a lower family PPES were three times more likely to report willingness to work in a deprived area (OR 3.13, 95%CI: 1.74-5.62), compared with those with a higher family PPES.
The results of the multivariate model, controlled for gender, family PPES, and rural and international experience, are also shown (Table 2). The effects of gender and family PPES on willingness to work in a deprived area were attenuated, but still significant at 95% CI. Students with rural but no international experience were almost three times as likely to report willingness to work in a deprived area, compared with those with international but no rural experience (OR 2.77, 95%CI: 1.08-7.13). Those with neither rural nor international experience and those with both rural and international experience were no different from students with international but no rural experience with regard to willingness to work in a deprived area.
Table 2: Ghanaian medical students' regression models of willingness to work
in a rural area on graduation in relation to lifecourse and other factors, N=228
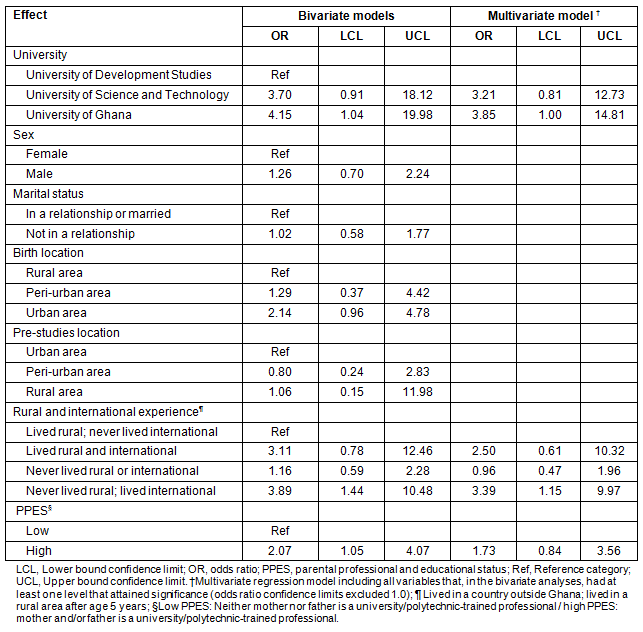
The results of the bivariate analyses of lifecourse factors and considering emigration after graduation are shown (Table 3). Students from UG were more than four times as likely to have considered emigration as those from UDS (OR 4.15, 95%CI: 1.04-19.98). Those with international but no rural experience were almost four times as likely to have considered emigration, compared with those with rural but no international experience (OR 3.87, 95% CI: 1.44-10.48). Those with a higher family PPES were more than twice as likely to have considered emigration (OR 2.07, 95%CI: 1.05-4.07) compared with those with a lower family PPES.
The results of the multivariate model, controlled for university, family PPES, and rural and international experience, are shown (Table 3). Those with international but no rural experience were more than three times as likely to have considered emigration, compared with those with rural but no international experience (95%CI: 1.15-9.97). PPES was not a significant predictor emigration consideration in this model.
There was a sub-set of 80 individuals (35%) who reported being both willing to work in a deprived area in Ghana and considering emigration. This group contained more men than women (41% vs 23%), but there were no other major differences in their covariates (data not shown).
Table 3: Ghanaian medical students' regression models of considering emigration
after graduation in relation to lifecourse and other factors, N=228
Discussion
In this study of 228 fourth-year Ghanaian medical students, it was found that male students, those who had lived in rural areas and never lived abroad, and those from a low PPES family were more willing to work in a deprived area after graduation. Students from UG and those who had lived abroad but not in a rural area were more likely to have considered emigrating after graduation. These results add to those from a recent, discrete, choice experiment of the present authors, which assessed how Ghanaian medical students' stated preference for certain rural postings was influenced by various job attributes31.
This study differs from previously published research in that it investigates factors influencing both emigration and rural practice in Ghana, a low-middle income country, and in that the entire class of fourth year medical students in Ghana was interviewed, avoiding self-selection bias. Nevertheless, the present findings regarding rural living experience and willingness to work in a rural area are consistent with the literature14,21,22. Students with exposure to rural life (after the age of 5 years) may be more willing to return due to family connections in rural areas, identification with their home communities, greater appreciation of the rural lifestyle, or a desire to serve as a role model for or representative of their community33-36. Comprehension of the health needs of rural areas and a desire to be a positive role model may further encourage the return of students to a rural area35. Rural students also understand the nuances and intricacies of rural life and therefore may be more at ease with living and working in a small community36. Students without rural living experience may have negative stereotypical views of rural environments which may be magnified by international experience.
The present finding that students from a lower socioeconomic background were more willing to work in a deprived area is consistent with several studies that have suggested students interested in rural practice are less likely to have university-educated parents than those interested in a specialty29,37. Matsumoto et al found that the parental academic background of rural medical students in Japan tended to be lower than that of urban students37. Although family PPES is often tied to rural origin, this factor persisted even after controlling for rural exposure. Students of a lower PPES may be more willing to practice in deprived areas due to a greater understanding of poverty or a motivation to help the poor17.
It was found that female students were less willing to work in a rural area. This is consistent with studies in other countries36 and reflects the international predominance of males in rural practice34,35,38. This may be explained by fewer job opportunities for spouses and a lack of appropriate educational opportunities for children in rural areas39. Studies in the USA and Australia demonstrated that doctors with rural-origin spouses were significantly more likely to practice in a rural setting40. Other factors may include cultural standards regarding women and travel, and the tendency for women to follow their husbands' jobs, rather than the reverse. Women may also be more integrated into social networks during their studies.
The finding that UG students were more likely to consider emigration is also consistent with research on graduates from other elite institutions41. For example, graduates from All India Institute of Medical Sciences account for a disproportionately large share of emigrating physicians41. The referent institution, the UDS, is located in the northern city of Tamale, which has a lower representation of students with international experience than KNUST or UG (17% vs 26% and 23%, respectively). Even after controlling for rural and international experience, however, UG students were more likely to have considered emigration than UDS students. Because Accra is the capital city of Ghana and an international travel hub, it is likely that the UG students were more exposed to international travellers in social and professional settings than those from UDS. Given the remote location and community medicine focus of UDS, students choosing to attend UDS may also be self-selected into a more community-minded cohort.
It was also found that students with international experience were more likely to have considered emigration than students without international experience. International living experiences expose Ghanaians to a higher standard of living in high-income nations such as the UK and USA, both primary destinations for emigrants. Students with international experience may also have friends and family overseas, which would ease the emigration process.
The bivariate analysis showed that, compared with students who had international but no rural experience, students with all other combinations of rural/international experience were more willing to work in a rural area. Similarly, students who had international but no rural experience were the only group more likely to have considered emigration in both bivariate and multivariate analyses. These results show that students' international experience without rural experience is a potent driver away from rural practice and towards emigration.
The significant number of students who reported both willingness to work in deprived areas as well as consideration of emigration should be noted. The predominance of males in the group may indicate their greater willingness to relocate and/or greater social acceptance of males relocating for work).
Strengths and limitations
A potential limitation of this study is its reliance on students' self-reports. Students may have felt a strong social pressure to remain in Ghana and work in deprived rural areas. Although participants were assured that their responses were anonymous and that they could omit any question they preferred not to answer, these results may be subject to social desirability bias. Future research is needed to compare students' stated intentions with actual career choices after graduation. In addition, the study population was naïve regarding career planning: they had not yet practiced medicine and had no experience in seeking or evaluating employment options. Most of these students were yet to experience the pressures of parenthood; therefore it is likely that their motivation and perspectives are likely to change substantially over time. Thus, this study's findings should not be applied to practicing physicians or health students of a different age group. Finally, these results may not be generalizable to future classes of students. The Ghanaian medical education system is rapidly evolving and as this system changes, the student population will also change.
A major strength of this study is that it captures an entire population of medical students (no sampling was conducted). In addition, a high response rate (99%) assures very little self-selection for participation. Future studies could attempt to combine multiple classes of students in order to improve generalizability and power to detect effect size.
The study population is a source of both strength and weakness. Medical students are younger and more naïve than practicing physicians. At the same time, inexperienced graduating students are the primary MOH targets for recruitment to rural posts. In addition, the study population represents an entire graduating class of Ghanaian medical students, including those who will emigrate soon after graduation. A survey of practicing physicians, on the other hand, would miss those who had emigrated.
Finally, to the authors' knowledge there have been no studies with the diversity of lifecourse investigated here, or that have looked simultaneously at the likelihood of rural practice and emigration in a lower-resource setting.
Policy implications
Students who have previously lived in rural areas are more likely than their urban peers to contribute to addressing physician maldistribution34. Fewer applications to medical schools come from candidates raised in rural areas; consequently, rural individuals are under-represented in incoming medical classes42,43. A university admission policy giving preference to students who have previously lived in rural areas, as part of a balanced selection process, should be considered21,22,37,44,45. At schools where this strategy has been implemented, the academic performance of students given preferential admission did not differ from their urban peers44,46,47. In Japan, a rural recruiting scheme was successful in recruiting and retaining medical professionals in medically underserved areas41. Similarly, recruitment and/or selective admission of students of a lower PPES should also be considered.
Evidence for the strategy of exposing students to rural practice early in their medical training is mixed14,34,35,48. For example, studies in South Africa suggested that requiring inexperienced doctors to perform community service in rural areas without adequate guidance and support may have a negative effect on rural practice49,50. However, the perceived quality of the rural educational experience is associated with an increased interest in a rural career51. It is therefore important that Ghanaian health science faculties provide rural training of sufficient duration and quality to make a positive impact on future rural recruitment.
The association between emigration consideration and the university attended supports the notion that the location of a training program has an impact on the practice location of its graduates. Medical schools outside urban areas produce graduates who are more likely to practice primary care and in rural areas, while urban medical schools encourage specialization38. Expanding medical training programs outside large urban areas and those focusing on family medicine and general practice may increase rural physician concentration. In addition, in countries where in-country postgraduate training programs are limited, students may see emigration as a way to obtain specialized medical education. Expansion of in-country specialist training is therefore a potential method of increasing physician retention.
More than half of the fourth-year medical students in Ghana were willing to work in a deprived area and almost two-thirds had contemplated emigration after graduation. Selective admission policies based on medical student lifecourse factors, combined with the strategic location of medical schools in more rural areas, and high-quality rural electives during training are suggested to increase the number of rural physicians in Ghana. Policy experiments should be rigorously evaluated and adapted as future cohorts with different backgrounds and expectations enter medical training. A commitment to health services research and a healthy collaboration between academic, governmental, non-governmental, and regulatory agencies are essential elements of such an investigation.
Acknowledgements
The authors thank Provost Aaron Lawson of the University of Ghana College of Health Sciences and Provost Peter Donkor of the Kwame Nkrumah University of Science and Technology (KNUST) School of Medical Sciences as well Dean Christine Ntim-Amponsah (University of Ghana Medical School) and Dean Kwabena Danso (KNUST Medical School). The authors appreciate the logistical assistance of Mr Perry Ofosu and Ms Nadia Tagoe from the Ghana-Michigan CHARTER. They also thank Ms Akosua Serwaa and Ms Mawunyo Belinda Akakpo for their capable management of study fieldwork and computer laboratory managers, Mr Aggrey (University of Ghana), Ms Helen Agyei (KNUST), and Mr Charles Donkor (KNUST) whose support was essential to the completion of the computer-assisted interviews. Lastly, the authors acknowledge the medical students at the University of Ghana and KNUST for their enthusiastic participation in this research, and especially the class leaders who ably assisted with participant recruitment. This study was funded by the Bill and Melinda Gates Foundation.
References
1. Chen L, Evans T, Anand S, Boufford J, Brown H, Chowdhury M et al. Human resources for health: overcoming the crisis. Lancet 2004; 364: 1984-1990.
2. WHO. World Health Statistics 2009. Geneva: WHO, 2009.
3. World Bank. Data. Changes in Country Classifications. (Online) 2010. Available: http://data.worldbank.org/news/2010-GNI-income-classifications (Accessed 2 August 2012).
4. Watkins K, Ugaz C, Carvajal L, Coppard D, Nieva RF, Gaye A et al. Fighting climate change: Human solidarity in a divided world. In Human Development Report 2007/8. New York City: United Nations Development Programme, 2007.
5. Ghana Ministry of Health. Regional Distribution of doctors in Ghana. Accra: Ghana Ministry of Health, 2009.
6. Mullan F. The metrics of the physician brain drain. New England Journal of Medicine 2005; 353: 1810-1818.
7. Dovlo D, Nyonator F. Migration by graduates of the University of Ghana Medical School: A preliminary rapid appraisal. Human Resources for Health 1999; 3: 40-51.
8. Hagopian A, Thompson MJ, Fordyce M, Johnson KE, Hart LG. The migration of physicians from sub-Saharan Africa to the United States of America: measures of the African brain drain. Human Resources Health 2004; 2: 17.
9. Asante AD, Zwi, AB; Ho, MT. Equity in resource allocation for health: A comparative study of the Ashanti and Northern Regions of Ghana. Health Policy 2006; 78: 135-148.
10. Asante AD, Zwi AB. Factors influencing resource allocation decisions and equity in the health system of Ghana. Public Health 2009; 123: 371-377.
11. Ghana Ministry of Health. Independent review: Health sector programme of work 2007. Accra: Ghana Ministry of Health, 2008.
12. Ghana Ministry of Health. Facts and figures: Human resources for health. Accra: Ghana Ministry of Health, 2009.
13. Wilson N, Couper I, De Vries E, Reid S, Fish T, Marais B. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health 9: 1060. (Online) 2009. Available: www.rrh.org.au (Accessed 7 July 2012).
14. Henry J, Edwards B, Crotty B. Why do medical graduates choose rural careers? Rural and Remote Health 9: 1093. (Online) 2009. Available: www.rrh.org.au (Accessed 7 July 2012).
15. Humphreys J, Jones M, Jones J, Mara P. Workforce retention in rural and remote Australia: determining the factors that influence length of practice. Medical Journal of Australia 2002; 176: 472-476.
16. Lehmann U. Staffing remote rural areas in middle- and low-income countries: a literature review of attraction and retention. BMC Health Services Research 2008; 8: 19.
17. Serneels P, Lindelow M, Garcia-Motalvo J, Barr A. For Public Service or Money: Understanding Geographical Imbalances in the Health Workforce. Oxford: World Bank, 2005.
18. Vujicic M, Zurn P, Diallo K, Adams O, Dal Poz MR. The role of wages in the migration of health care professionals from developing countries. Human Resources for Health 2004; 2: 3.
19. Willis-Shattuck M, Bidwell P, Thomas S, Wyness L, Blaauw D, Ditlopo P. Motivation and retention of health workers in developing countries: a systematic review. BMC Health Services Research 2008; 8: 247.
20. Couper I, Hugo J. Management of district hospitals - exploring success. Rural and Remote Health 5: 433. (Online) 2005. Available: www.rrh.org.au (Accessed 7 July 2012).
21. de Vries E, Reid S. Do South African medical students of rural origin return to rural practice? South African Medical Journal 2003; 93: 789-793.
22. Laven G, Wilkinson D. Rural doctors and rural backgrounds: how strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11: 277-284.
23. Rabinowitz HK. A program to recruit and educate medical students to practice family medicine in underserved areas. JAMA 1983; 249: 1038-1041.
24. Silagy CA, Piterman L. Attitudes of senior medical students from two Australian schools towards rural training and practice. Academic Medicine 1991; 66: 417-19.
25. Rabinowitz HK, Diamond JJ, Hojat M, Hazelwood CE. Demographic, educational and economic factors related to recruitment and retention of physicians in rural Pennsylvania. Journal of Rural Health 1999; 15: 212-218.
26. Azer SA, Simmons D, Elliott SL. Rural training and the state of rural health services: effect of rural background on the perception and attitude of first-year medical students at the University of Melbourne. Australian Journal of Rural Health 2001; 9: 178-85.
27. Somers GT. What does it take? The influence of rural upbringing and sense of rural background on medical students' intention to work in a rural environment. Rural and Remote Health 7: 706. (Online) 2007. Available: www.rrh.org.au (Accessed 7 July 2012).
28. Schofield D, Fletcher S, Fuller J, Birden H, Page S. Where do students in the health professions want to work? Human Resources for Health 2009; 7: 74.
29. Feldman K, Woloschuk W, Gowans M, Delva D, Brenneis F, Wright B et al. The difference between medical students interested in rural family medicine versus urban family or specialty medicine. Canadian Journal of Rural Medicine 2008; 13: 73-79.
30. Hancock C, Steinbach A, Nesbitt T, Adler S, Auerswald C. Why doctors choose small towns: a developmental model of rural physician recruitment and retention. Social Science & Medicine 2009; 69: 1368-1376.
31. Kruk ME, Johnson JC, Gyakobo M, Agyei-Baffour P, Asabir K, Kotha R et al. Preferences for rural practice incentives among medical students in Ghana: a discrete choice experiment. Bulletin of the WHO 2010; 88: 333-341.
32. Agyei-Baffour P, Kotha SR, Johnson JC, Gyakobo M, Asabir K, Kwansah J et al. Willingness to work in rural areas and the role of intrinsic versus extrinsic professional motivations - a survey of medical students in Ghana. BMC Medical Education 2011; 11: 56-63.
33. Daniels ZM, VanLeit BJ, Skipper BJ, Sanders ML, Rhyne RL. Factors in recruiting and retaining health professionals for rural practice. Journal of Rural Health 2007; 23: 62-71.
34. Woloschuk W, Tarrant M. Does a rural educational experience influence students' likelihood of rural practice? Impact of student background and gender. Medical Education 2002; 36: 241-247.
35. Couper I, Hugo J, Tumbo J, Harvey B, Malete N. Key issues in clinic functioning - a case study of two clinics. South African Medical Journal 2007; 97: 124-129.
36. Peach HG, Bath NE. Comparison of rural and non-rural students undertaking a voluntary rural placement in the early years of a medical course. Medical Education 2000; 34: 231-233.
37. Matsumoto MI, Inoue K, Kajii, E. Characteristics of medical students with rural origin: Implications for selective admissions policies. Health Policy 2008; 87: 194-202.
38. Horner RD, Samsa GP, Ricketts TC. Preliminary Evidence on Retention Rates of Primary Care Physicians in Rural and Urban Areas. Medical Care 1993; 31: 640-648.
39. Dussault G, Franceschini M. Not enough there, too many here: understanding geographical imbalances in the distribution of the health workforce. Human Resources for Health 2006; 4: 12.
40. Laven G, Beilby J, Wilkinson D, McElroy H. Factors associated with rural practice among Australian-trained general practitioners. Medical Journal of Australia 2003; 179: 75-79.
41. Kaushik M. High-end physician migration from India. Bulletin of the WHO 2008; 86: 40-45.
42. Rourke JT, Strasser R. Education for rural practice in Canada and Australia. Academic Medicine 1996; 71: 464-469.
43. Craig M, Jackel C, Gerrits P. Selection of medical students and the maldistribution of the medical workforce in Queensland, Australia. Australian Journal of Rural Health 2008; 1: 17-21.
44. Rabinowitz H. Evaluation of a selective medical school admissions policy to increase the number of family physicians in rural and underserved areas. New England Journal of Medicine 1988; 319: 480-486.
45. Rolfe IE, Pearson SA, O'Connell DL, Dickinson JA. Finding solutions to the rural doctor shortage: the roles of selection versus undergraduate medical education at Newcastle. Internal Medicine Journal 1995; 25: 512-17.
46. Willoughby TL. Personal characteristics and achievements of medical students from urban and nonurban areas. Journal of Medical Education 1981; 56: 717-726.
47. Longo DR, Gorman RJ, Ge B. Rural medical school applicants: do their academic credentials and admission decisions differ from those of nonrural applicants? Journal of Rural Health 2005; 21: 346-50.
48. Ranmuthugala G, Humphreys J, Solarsh B, Walters L, Worley P, Wakerman J et al. Where is the evidence that rural exposure increases uptake of rural medical practice? Australian Journal of Rural Health 2007; 15: 285-288.
49. Marais BJ, de Villiers M, Kruger J, Conradie H, Jenkins L, Reuter H. The role of educational strategies to reverse the inverse performance spiral in academically-isolated rural hospitals. South African Family Practice 2007; 49(7): 15.
50. Nemutandani MS, Maluleke FRS, Rudolph MJ. Community service doctors in Limpopo province. South African Medical Journal 2006; 96(3): 180-182.
51. Shannon C, Baker H, Jackson J, Roy A, Heady H, Gunel E. Evaluation of a required statewide interdisciplinary rural health education program: student attitudes, career intents and perceived quality. Education for Health Journal 2005; 18: 395-404.








