Cigarette smoking is the leading risk factor for mortality in the USA1. It also poses a serious health threat to non-smokers exposed to secondhand smoke2. Two public health policies that can potentially reduce smoking and smoking-related disease are smoke-free laws (at either the state or local level) and the placement of graphic warning labels on cigarette packages3. As of December 2010, 25 states and the District of Columbia had comprehensive statewide smoke-free laws, which prohibit smoking in the indoor areas of worksites, restaurants, and bars4. An additional 18 states had less restrictive statewide laws, while seven states had no statewide smoking restrictions4. Most recently, the US Food and Drug Administration (FDA) revealed nine graphic warning labels that will be required on all cigarette packages no later than September 20125.
Both smoke-free laws and the use of graphic warning labels on cigarette packages have produced encouraging public health results. Statewide comprehensive smoke-free laws have been associated with fewer deaths from acute myocardial infarction6, while non-statewide laws have reduced smoking-related disease, smoking prevalence and cigarette consumption among adults, and smoking initiation among youths7-9. Data also suggest that graphic warning labels, which have been used on cigarette packages for some time in other countries10, serve as a source of information about the risks of smoking, discourage smoking initiation, decrease cigarette consumption, and promote smoking cessation10-13.
The Appalachian region of the USA consists of more than 400 counties in 13 states extending from New York to Mississippi14. Appalachia is mostly a rural region, with approximately 70% of its counties considered non-metropolitan, and just under half of its residents living in rural areas15. Compared with the rest of the USA, the residents of Appalachia have higher rates of poverty, lower levels of education, and poorer health15,16. Smoking is also more prevalent in the Appalachian region16, which may be partly attributable to the region being a primary producer of tobacco in the USA17. Appalachian residents therefore have the potential to benefit greatly from tobacco-related public health policies. At the time of this study, however, only two Appalachian states (Ohio in 2006 and New York in 2003) had passed comprehensive statewide smoke-free laws4. A third Appalachian state (Maryland in 2008) has since passed a comprehensive statewide smoke-free law, while six have limited smoking restrictions and four have no statewide smoking restrictions4. In Appalachian states without comprehensive statewide laws, few communities have local smoke-free ordinances18.
Ohio Appalachia is a mostly rural 32 county region (29 counties at the time of this study) in the southern and eastern parts of the state, and its characteristics are similar to those of the entire Appalachian region15. For example, approximately 31% of adults in Ohio Appalachian counties are smokers, compared with only approximately 21% in non-Appalachian counties in Ohio19. The smoke-free law in Ohio was passed on 7 November 2006, took effect on 7 December 2006, and began being enforced on 3 May 200720.
Although previous research has examined US residents' views about smoke-free laws21-24 and graphic warning labels on cigarette packages25-27, the present authors are not aware of studies addressing these issues among Appalachian residents. Given that smoking is more prevalent in this geographical region and that the unique Appalachian culture has pro-tobacco beliefs and attitudes, the authors believe this to be an important gap in the existing literature. The current study addresses this gap by examining the beliefs and attitudes about smoke-free laws and the addition of graphic warning labels to cigarette packages among the residents of Ohio Appalachia. Results provide early feedback from one of the few Appalachian states with a statewide comprehensive smoke-free law, as well as an initial insight into Ohio Appalachian residents' views on graphic warning labels for cigarette packages.
This focus group study was conducted with the support of the Community Awareness, Resources and Education (CARE) Project, one of eight Centers for Population Health and Health Disparities (P50) funded by the National Institutes of Health28. The study was primarily designed to assess Ohio Appalachian residents' beliefs, attitudes, and acceptability of the human papillomavirus (HPV) vaccine, results that have been reported previously29. During the focus groups, risk factors for cervical cancer, including smoking, were mentioned by participants. Since the smoke-free Ohio law was recently passed, residents' beliefs and attitudes about this new law and the graphic cigarette labels being used in Canada at that time were also explored. The resulting data form the basis of this report. The Institutional Review Board at The Ohio State University approved the study.
Participants
As described previously29, participants were recruited from Ohio Appalachian counties with assistance from members of local community-based cancer coalitions associated with the Ohio Appalachian Community Cancer Network (ACCN). The ACCN coalition members posted flyers at various locations (eg health departments, libraries) in Ohio Appalachian counties and sent flyers to local community-based agencies. Four types of community members were targeted for the study: healthcare providers, community leaders, parents with adolescent daughters, and young adult women (18-26 years). Separate focus groups were conducted for each type of community member. In-depth interviews were conducted on occasions when only one person arrived for a focus group.
A total of 23 focus groups were conducted with 112 participants, as well as in-depth interviews with two individuals. The focus groups and interviews occurred in nine of the 29 Ohio Appalachian counties with participants (n=114) from 14 Ohio Appalachian counties. Participants included 37 healthcare providers (nurses, pediatricians, pharmacists, and a gynecologic surgeon) in six focus groups and one in-depth interview; 31 community leaders (church leaders, health agencies) in six focus groups; 19 parents in six focus groups; and 27 young adult women aged 18-26 years in five focus groups and one in-depth interview.
Procedures
An experienced female moderator (MLK) led the focus groups with an additional staff member recording field notes and group dynamics. Focus groups were held in various community locations (eg libraries, clinics), with all sessions audio-recorded. Audio-tapes were later transcribed verbatim and transcripts reviewed for accuracy. Focus groups lasted approximately 1 hour and were conducted during the summer of 2007. Participants received a $25 gift card for participating in the focus group and a $5 gasoline gift card for travel expenses. Prior to the start of each focus group, participants completed written consent forms and short self-administered surveys that collected socio-demographic information.
During focus groups, the moderator probed on community members' beliefs and attitudes about two specific tobacco-related issues: (i) the comprehensive statewide smoke-free law that had been recently enforced in Ohio; and (ii) the possibility of the USA adding graphic warning labels to cigarette packages, similar to the labels used in Canada. The moderator showed pictures of Canadian cigarette packages with graphic warning labels indicating that cigarettes cause oral disease and lung cancer.
Data analysis
Two research team members (MLK, PLR) read all focus group transcripts and developed a coding tree. One team member (PLR) coded the tobacco-related sections of data and consulted another member (MLK) on any issues that arose during this process. NVivo qualitative software (www.qsrinternational.com) was used to code the data and aid in classifying, sorting, and categorizing data. Data were compared across the four community member types using cross-group comparisons with a matrix30. Since there were no differences and similar themes emerged from the different groups, all data were combined in this report. Quotations were selected to illustrate prevalent themes.
Participant characteristics
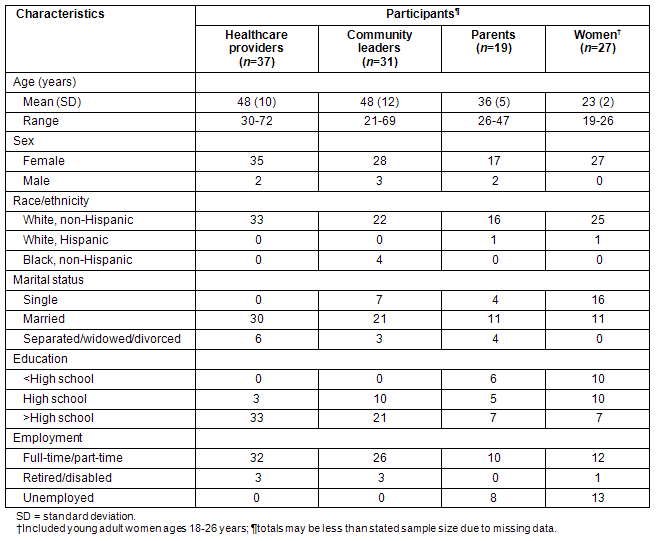
Most participants were female (94%), non-Hispanic White (94%), and married (65%); Table 1. All healthcare providers and community leaders reported having at least a high school education, but 36% of parents and young adult women indicated they had not completed high school. Almost all healthcare providers (91%) and community leaders (90%) were employed full-time or part-time, with fewer parents (56%) and young adult women (46%) indicating current employment.
Table 1: Characteristics of focus group participants from Ohio Appalachia
Smoke-free law
Participants reported that the recently enforced statewide smoke-free law had been discussed a great deal in their communities. Themes that emerged concerning the law included support from non-smokers in participants' communities, opposition from smokers in these communities, and general compliance among residents and local businesses (Table 2). A parent who supported the law stated, 'I like that when I go to a store or when I go to a restaurant and it's non-smoking'. Participants felt that one of the main reasons smokers opposed the law was the perception that it was an infringement of their rights. As one parent indicated, 'Oh, a lot of them smoke and they're like "You aren't going to tell me I can't smoke a cigarette".' A healthcare provider expressed a similar viewpoint:
....that feel, you know, that they have an inalienable right to smoke, and if they want to smoke, they ought to be able to do it and it should be made where they can do it, inside a restaurant also.
Despite some opposition, participants believed that most residents and local businesses were abiding by and enforcing the smoke-free law. As one community leader pointed out, 'Oh, they grumble. No one is defying the law, I don't think, but they're not happy with it'. However, some groups indicated that certain types of businesses (eg bars and private clubs) may not be strictly enforcing the law or that some had already designated outside areas for smoking (which, if appropriately designated, are allowable under the smoke-free law). A few participants expressed doubt that the smoke-free law has promoted smoking cessation in their region:
All the smoking law did was kept us non-smokers, ex-smokers, from having to deal with it in the community, but smoking is still pretty prevalent.
I don't think it's deterred them in any way.
Table 2: Focus group themes concerning Ohio's smoke-free law and cigarette warning labels
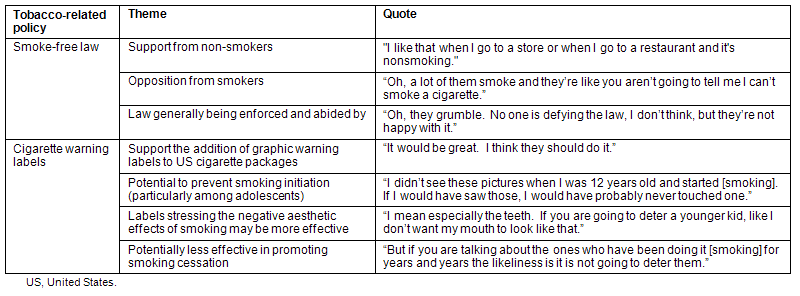
Cigarette warning labels
Overall, most participants were surprised by the graphic nature of the warning labels and that the labels were already being used in Canada. Themes expressed during discussions of these labels included support for adding them to US cigarette packages, their potential to prevent smoking initiation (particularly among adolescents), how labels stressing the negative aesthetic effects of smoking may be more effective, and their potential lack of effectiveness in promoting smoking cessation (Table 2).
Participants from all focus groups supported the possibility of US cigarette packages containing graphic warning labels. One young adult woman expressed her support for adding the warning labels, 'It would be great. I think they should do it'. Participants especially believed these types of warning labels could help deter adolescents and adult non-smokers from smoking initiation, many of whom were believed to lack knowledge about the health risks from smoking. One community leader commented on why the labels may deter adolescents:
The kids I see, they don't see the long-term effects. They are more right at the moment type. They don't see 25 to 30 years down the road, what it's [smoking] going to do to them.
A young adult woman also described the images' potential positive effects on adolescents:
I didn't see these pictures when I was 12 years old and started [smoking]. If I would have saw those, I would have probably never touched one.
Some participants thought graphic warning labels stressing the negative aesthetic effects of smoking (eg oral disease) may be more effective among adolescents than labels stressing other smoking-related diseases (eg lung cancer). One young adult woman stated, 'I mean especially the teeth. If you are going to deter a younger kid, like "I don't want my mouth to look like that".' A healthcare provider made a similar suggestion, 'Focusing on some of the aesthetic things does seem to make a difference with young people'. Multiple healthcare providers indicated that posters depicting the negative aesthetic effects of smoking have been effective in their clinics. A few participants, however, expressed concern that adolescents may be desensitized to graphic smoking-related images because they have already seen them in school health classes or that peer pressure will remain the strongest influence on adolescents' smoking behaviors in this region, despite the presence of graphic warning labels on cigarette packages.
Participants generally felt that graphic warning labels would be less effective among older individuals in this region, particularly current smokers. They believed that smokers were already too addicted for the labels to have any effects. One parent noted:
But if you are talking about the ones who have been doing it [smoking] for years and years the likeliness is it is not going to deter them.
A young female participant echoed this viewpoint, 'Well it's an addiction, I mean it's not going to stop people from smoking'. A few participants felt many people in the region have a fatalistic view of their health, limiting their interest and motivation to stop smoking. As one participant stated:
I think it would upset the older generation that have done it all their life because they already have the mind frame set that whatever is going to happen is going to happen.
Suggestions that smokers would simply avoid the labels were also made, with one participant (a current smoker) stating, 'I would just cover up the package with a piece of paper'.
Discussion
Smoke-free laws and the addition of graphic warning labels to US cigarette packages represent public health policies that can potentially reduce smoking and smoking-related disease. Appalachia is a large geographic region in the USA with approximately half of its residents living in rural areas15. Appalachia is also a tobacco-producing region where smoking is more prevalent and statewide comprehensive smoke-free laws are less prevalent compared with the rest of the USA4,16,17. Thus, it is of great public health importance to examine Appalachian residents' views about these policies. Using qualitative data from focus groups throughout Ohio Appalachia, a mostly rural region, it was found that participants tended to support both tobacco-related health policies.
Ohio began enforcing its comprehensive statewide smoke-free law just prior to the present study (in May 200720), and thus the results indicate mostly positive early feedback. Focus group participants indicated the law was generally accepted in their communities, with opposition from some smokers. These findings coincide with those from other US studies, where support for smoke-free laws or smoking restrictions was typically high and greater among non-smokers21,23,24. Although one of these prior studies was in a non-Appalachian Kentucky county that produces tobacco24, the authors believe the present results represent the first evidence that Appalachian residents are generally supportive of such laws. As importantly, focus groups participants believed that most residents and local businesses were abiding by and enforcing the law. Given the benefits of smoke-free laws to both smokers and non-smokers6,7,31-33, it is important that such laws are properly enforced after they are passed. Compliance with smoke-free policies among businesses has generally been high (over 90% following policy enactment), although most previous studies have been conducted in urban or suburban locations34,35. Future quantitative research is needed to further examine support for and enforcement of these laws in the Appalachian region. With only three Appalachian states currently having statewide comprehensive smoke-free laws4, such data could help inform future tobacco policies in this region.
The FDA will require all US cigarette packages to contain graphic warning labels no later than September 20125, although tobacco companies recently filed a lawsuit to prevent this change from occurring36. In the present study, high levels of support were found for adding such labels to US cigarette packages, similar to past research conducted in the US25,26. Focus group participants felt that graphic warning labels could be especially effective at preventing adolescents and adults from smoking initiation. This could be partly attributable to participants believing that most adolescents and young adults in their region are not well-informed about the risks of smoking, and graphic warning labels may be more effective in communicating these risks10,13. Participants believed that labels stressing the negative aesthetic effects of smoking would be more influential among adolescents compared with other label types. These findings coincide with data from other countries10 and prior US focus groups, where young adult non-smokers thought graphic warning labels stressing gum disease would be most influential among young people who do not smoke or have recently started smoking26. If labels stressing the negative aesthetic effects of smoking are used, those that are highly graphic may be more influential than less graphic labels37. The findings presented offer an early insight into Ohio Appalachian residents' support for graphic warning labels and suggest such labels represent a possible strategy for reducing smoking initiation in this region.
Participants felt that graphic warning labels would be less successful in promoting smoking cessation in their region. Participants' skepticism was based on a few factors: the strength of addiction, avoidance of the labels, and fatalistic beliefs. They believed that many smokers in their region were too addicted for the labels to have any effect on smoking cessation. While this belief is consistent with past research examining the use of large text on cigarette package labels38, studies have demonstrated that graphic warning labels actually decrease cigarette consumption, promote intentions to quit, and enhance smoking cessation efforts10-12. Participants also believed that smokers may simply avoid the labels. To help smokers in other countries avoid graphic warning labels, tobacco companies have utilized split packs that divide in half so that one side doesn't show the label, and have also produced sleeves to cover the warning labels39. Most current smokers, however, do not make an effort to avoid the labels and avoidance is not associated with smoking cessation11,25. Finally, participants believed that many residents have a fatalistic view of their health. Fatalism, the belief that events are determined by fate and are out of human control, is a value traditionally associated with the Appalachian region. Although there is some evidence to suggest fatalism influences the health behaviors of Appalachian residents40,41, other studies have found it is not a major barrier to health care in this region42. Future research is needed to determine the effects of graphic warning labels on smoking cessation in Appalachia and whether these potential barriers affect behavior.
The strengths of the present study included the large number of focus groups conducted in a geographic region with high smoking prevalence, targeting four types of community members, the collaboration with local community-based cancer coalitions for recruiting participants, and the timing of the focus groups in relation to the enforcement of Ohio's comprehensive statewide smoke-free law. The focus groups were conducted throughout the Ohio Appalachian region but the generalizability to other Appalachian states is not known. Most participants were female and non-Hispanic White, so additional research among more diverse populations is needed. The smoking status of participants was not collected. Some participants did, however, volunteer their smoking status during focus groups, giving the authors confidence that many groups contained both smokers and non-smokers. It is also possible that participants' responses may have been influenced by the focus group discussions, although this possibility was likely to be reduced by the use of an experienced moderator.
The Ohio Appalachian residents in this study, most of whom were female, generally held positive views about smoke-free laws and the addition of graphic warning labels to US cigarette packages. These tobacco-related public health policies offer possible strategies for reducing smoking and its associated diseases in this mostly rural region with high smoking prevalence among its residents. Future research is needed to monitor the continuing effects of and support for statewide smoke-free laws and to determine the influence of graphic warning labels once they appear on US cigarette packages.
Acknowledgement
This research was supported by the National Cancer Institute grants: P50CA105632, K07CA107079 (MLK), CA114622 (Appalachia Community Cancer Network), and the P30 CA016058 (Behavioral Measurement Shared Resource at The Ohio State University Comprehensive Cancer Center).
References
1. Danaei G, Ding EL, Mozaffarian D, Taylor B, Rehm J, Murray CJ et al. The preventable causes of death in the United States: comparative risk assessment of dietary, lifestyle, and metabolic risk factors. PLoS Medicine 2009; 6(4): e1000058.
2. US Department of Health and Human Services. The health consequences of involuntary exposure to tobacco smoke: A report of the Surgeon General. (Online) 2006. Available: http://www.surgeongeneral.gov/library/secondhandsmoke (Accessed 5 December 2011).
3. US Department of Health and Human Services. (Online) 2000. Reducing tobacco use: A report of the Surgeon General. 2000. Available: http://www.cdc.gov/tobacco/data_statistics/sgr/2000/index.htm (Accessed 5 December 2011).
4. Centers for Disease Control and Prevention. State smoke-free laws for worksites, restaurants, and bars - United States, 2000-2010. MMWR Morbidity and Mortality Weekly Report 2011; 60(15): 472-475.
5. US Food and Drug Administration. FDA unveils final cigarette warning labels. (Online) 2011. Available: http://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm260181.htm (Accessed 5 December 2011). .
6. Dove MS, Dockery DW, Mittleman MA, Schwartz J, Sullivan EM, Keithly L et al. The impact of Massachusetts' smoke-free workplace laws on acute myocardial infarction deaths. American Journal of Public Health 2010; 100(11): 2206-2212.
7. Fichtenberg CM, Glantz SA. Effect of smoke-free workplaces on smoking behaviour: systematic review. BMJ 2002; 325(7357): 188.
8. Klein EG, Forster JL, Erickson DJ, Lytle LA, Schillo B. The relationship between local clean indoor air policies and smoking behaviours in Minnesota youth. Tobacco Control 2009; 18(2): 132-137.
9. Siegel M, Albers AB, Cheng DM, Hamilton WL, Biener L. Local restaurant smoking regulations and the adolescent smoking initiation process: results of a multilevel contextual analysis among Massachusetts youth. Archives of Pediatrics and Adolescent Medicine 2008; 162(5): 477-483.
10. Hammond D. Health warning messages on tobacco products: a review. Tobacco Control 2011; 20(5): 327-337.
11. Hammond D, Fong GT, McDonald PW, Brown KS, Cameron R. Graphic Canadian cigarette warning labels and adverse outcomes: evidence from Canadian smokers. American Journal of Public Health 2004; 94(8): 1442-1445.
12. Hammond D, Fong GT, McDonald PW, Cameron R, Brown KS. Impact of the graphic Canadian warning labels on adult smoking behaviour. Tobacco Control 2003; 12(4): 391-395.
13. Hammond D, Fong GT, McNeill A, Borland R, Cummings KM. Effectiveness of cigarette warning labels in informing smokers about the risks of smoking: findings from the International Tobacco Control (ITC) Four Country Survey. Tobacco Control 2006; 15 Suppl 3: 19-25.
14. Appalachian Regional Commission. The Appalachian region. (Online) no date. Available: http://www.arc.gov/appalachian_region/TheAppalachianRegion.asp (Accessed 5 December 2011).
15. Pollard KM. Appalachia at the millennium: an overview of results from Census 2000. (Online) 2003. Available: http://www.arc.gov/research/researchreportdetails.asp?REPORT_ID=42 (Accessed 5 December 2011) .
16. Halverson JA. An analysis of disparities in health status and access to health care in the Appalachian region. (Online) 2004. Available: http://www.arc.gov/research/researchreportdetails.asp?REPORT_ID=82 (Accessed 5 December 2011).
17. Wood LE. The economic impact of tobacco production in Appalachia. (Online) 1998. Available: http://www.arc.gov/research/researchreportdetails.asp?REPORT_ID=59 (Accessed 5 December 2011).
18. Ferketich AK, Liber A, Pennell M, Nealy D, Hammer J, Berman M. Clean indoor air ordinance coverage in the Appalachian region of the United States. American Journal of Public Health 2010; 100(7): 1313-1318.
19. Anon. Ohio Behavioral Risk Factor Surveillance System. Columbus, OH: Ohio Department of Health 2008.
20. Ohio Department of Health. Smoke-free workplace program. (Online) 2008. Available: http://www.ohionosmokelaw.gov/ (Accessed 5 December 2011).
21. Linnan LA, Weiner BJ, Bowling JM, Bunger EM. Views about secondhand smoke and smoke-free policies among North Carolina restaurant owners before passage of a law to prohibit smoking. North Carolina Medical Journal 2010; 71(4): 325-333.
22. Borland R, Yong HH, Siahpush M, Hyland A, Campbell S, Hastings G et al. Support for and reported compliance with smoke-free restaurants and bars by smokers in four countries: findings from the International Tobacco Control (ITC) Four Country Survey. Tobacco Control 2006; 15(Suppl 3): 34-41.
23. Tang H, Cowling DW, Lloyd JC, Rogers T, Koumjian KL, Stevens CM et al. Changes of attitudes and patronage behaviors in response to a smoke-free bar law. American Journal of Public Health 2003; 93(4): 611-617.
24. Wilson R, Duncan DF, Nicholson T. Public attitudes toward smoking bans in a tobacco-producing county. Southern Medical Journal 2004; 97(7): 645-650.
25. Peters E, Romer D, Slovic P, Jamieson KH, Wharfield L, Mertz CK et al. The impact and acceptability of Canadian-style cigarette warning labels among US smokers and nonsmokers. Nicotine and Tobacco Research 2007; 9(4): 473-481.
26. O'Hegarty M, Pederson LL, Yenokyan G, Nelson D, Wortley P. Young adults' perceptions of cigarette warning labels in the United States and Canada. Preventing Chronic Disease 2007; 4(2): A27.
27. O'Hegarty M, Pederson LL, Nelson DE, Mowery P, Gable JM, Wortley P. Reactions of young adult smokers to warning labels on cigarette packages. American Journal of Preventive Medicine 2006; 30(6): 467-473.
28. National Institutes of Health. Centers for Population Health and Health Disparities. (Online) 2002. Available: http://grants2.nih.gov/grants/guide/rfa-files/RFA-ES-02-009.html (Accessed 5 December 2011).
29. Katz ML, Reiter PL, Heaner S, Ruffin MT, Post DM, Paskett ED. Acceptance of the HPV vaccine among women, parents, community leaders, and healthcare providers in Ohio Appalachia. Vaccine 2009; 27(30): 3945-3952.
30. Miles MB, Huberman AM. Qualitative data analysis: an expanded sourcebook, 2nd edn. Thousand Oaks, CA: Sage, 1994.
31. Repace JL, Hyde JN, Brugge D. Air pollution in Boston bars before and after a smoking ban. BMC Public Health 2006; 6: 266.
32. Bohac DL, Hewett MJ, Kapphahn KI, Grimsrud DT, Apte MG, Gundel LA. Change in indoor particle levels after a smoking ban in Minnesota bars and restaurants. American Journal of Preventive Medicine 2010; 39(6Suppl 1): S3-9.
33. Centers for Disease Control and Prevention (CDC). Reduced secondhand smoke exposure after implementation of a comprehensive statewide smoking ban - New York, June 26, 2003-June 30, 2004. MMWR Morbidity and Mortality Weekly Report 2007; 56(28): 705-708.
34. Weber MD, Bagwell DA, Fielding JE, Glantz SA. Long term compliance with California's Smoke-Free Workplace Law among bars and restaurants in Los Angeles County. Tobacco Control 2003; 12(3): 269-273.
35. Hyland A, Cummings KM, Wilson MP. Compliance with the New York City Smoke-Free Air Act. Journal of Public Health Management and Practice 1999; 5(1): 43-52.
36. Associated Press. Tobacco companies file lawsuit over warning labels. (Online) 2011. Available: http://www.foxnews.com/us/2011/08/17/tobacco-graphic-federal-warnings-arent-fair/ (Accessed 5 December 2011).
37. Kees J, Burton S, Andrews JC, Kozup J. Understanding how graphic pictorial warnings work on cigarette packaging. Journal of Public Policy & Marketing 2010; 29(2): 265-276.
38. Devlin E, Anderson S, Hastings G, Macfadyen L. Targeting smokers via tobacco product labelling: opportunities and challenges for Pan European health promotion. Health Promotion International 2005; 20(1): 41-49.
39. Felberbaum M. Grisly labels not so scary for cigarette sales. (Online) 2011. Available: http://abcnews.go.com/Business/wireStory?id=14021292 (Accessed 5 December 2011).
40. Walker R, Lucas W, Crespo R. The West Virginia Rural Cancer Prevention project. Cancer Practice 1994; 2(6): 421-426.
41. Deskins S, Harris CV, Bradlyn AS, Cottrell L, Coffman JW, Olexa J et al. Preventive care in Appalachia: use of the theory of planned behavior to identify barriers to participation in cholesterol screenings among West Virginians. Journal of Rural Health 2006; 22(4): 367-374.
42. Coyne CA, Demian-Popescu C, Friend D. Social and cultural factors influencing health in southern West Virginia: a qualitative study. Preventing Chronic Disease 2006; 3(4): A124.
