Colorectal cancer is the second leading cause of death from all malignancies and the seventh most common cause of death from all causes1. An efficient, safe and high quality colonoscopy service aims to reduce the impact of Colorectal Cancer (CRCa) on the community and minimise the financial and personal costs to the community. These costs include missed or advanced pathology, complications, repeated and increased frequency of procedures, subsequent radiological examinations such as barium enema or computed tomography (CT) colonography.
The need for appropriate services is increasing with the roll-out of the National Bowel Cancer Screening Program (NBCSP) in Australia2. In rural Australia, endoscopic services are provided by procedural GPs or specialists. Caecal intubation, colonoscopy withdrawal time, polyp detection rates, carcinoma detection rates, and perforation and haemorrhage rates are recognized quality and safety parameters. Located on the river Murray on the border of the states of Victoria and New South Wales, Australia, Echuca is a small rural town classified as 'inner regional' Victoria (inner regional [RA] 2; major/capital cities are classified RA1). Echuca was previously classified as 'Rural and Remote Metropolitan Areas 4' (RRMA4), where RRMA1 was a capital city and RRMA7 was extremely remote. General practitioners in Echuca care for approximately 18 000 people. Travel times by car are approximately 50 min (70 km) to the nearest regional centre (Shepparton) and 3 hours to state capital Melbourne; public transport options are extremely limited. This study aimed to assess the quality and safety of a rural GP proceduralist service, and to evaluate current GP procedural training requirements, in the context of service shortages.
Colonoscopy was performed on all patients referred via an 'open access' system whereby the patient's GP could directly refer the patient for the procedure. The GP proceduralist did not clinically assess patients prior to the procedure. Patients received English instructions outlining the procedure and associated risks as well as a list of dietary restrictions and sodium picosulfate solution for preparation.
Standard pre-procedure consent and colonoscopy were performed by the first author whose training is recognised by the Australian Conjoint Committee for Recognition of Training in Gastrointestinal Endoscopy. Training required performing a minimum of 100 unassisted, supervised, complete colonoscopies to the caecum, preferably to the ileum, and successful snare polypectomies on a minimum of 30 patients, in patients with intact colons (eg with no prior colonic resection). Trainees must achieve a 90% or greater caecal intubation rate.
On the day of the procedure the initials, date of birth, UR number, findings, caecal intubation and time to completion were recorded for each patient immediately following colonoscopy (Table 1). Light general anaesthesia with a combination of propofol, fentanyl and/or midazolam was provided by GP anaesthetists.
Caecal intubation was determined by ileoscopy (visualizing the ileum) or failing this, identification of the ileocaecal valve, appendix orifice and confluence of Tinea coli. The proceduralist was contacted if any patients were subsequently re-admitted following endoscopy. Echuca and Moama are sister towns with the Murray River between them; they share a single regional health service. As a 'closed' rural community, subsequent complications were easily identified (Tables 1, 2).
Ethics approval
The hospital waived ethics approval and classified the 'study' as an 'audit' because it involved only the first author's patients.
Table 1: Rural GP colonoscopy safety and quality for 3000 serial
colonoscopies, comparison with international studies3-21
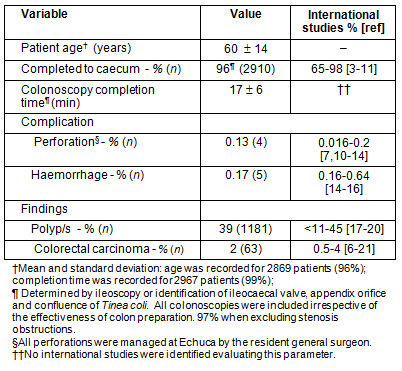
Table 2: Summary of complications' outcomes: N=9 (0.3%)
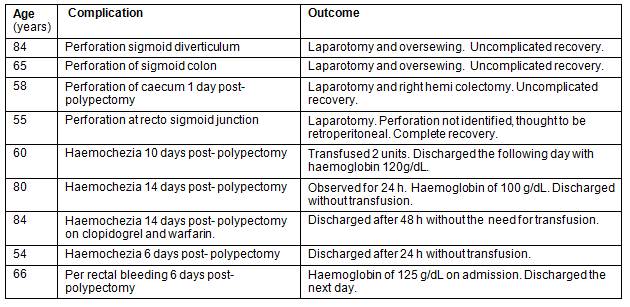
Quality and safety measures and complication details for 3000 serial colonoscopies performed between 1995 and 2011 are summarized (Tables 1, 2). The caecal intubation rate was 97% excluding stenosing lesions; polypectomy detection rate was 39%; carcinoma detection rate was 2%; and colonoscopy completion time was 17 min. Re-admission rates were 1.6/1000 for haemorrhage and 1.2/1000 for perforation. There were no deaths. Performance improved with completed colonoscopies and time to completion was stable at approximately 1000 colonoscopies.
Discussion
The GP proceduralist caecal intubation rate (96%) and detection rates (polyp 39%; CrCa 2%) reported in this study compare favourably with international standards set by the United Kingdom's National Health Service Bowel Cancer Screening Programme (NHSBCSP) in 201121, the United States Multi-Society Task Force on Colorectal Cancer in 200622, Cancer Care Ontario Colonoscopy in 200723 and current recommendations of the Australian NBCSP in 20092: caecal intubation rate greater than 90% and adenoma detection rate greater than 20%.
The quality and safety of colonoscopy are inter-related and this audit validates the use of the specific data set presented here as appropriate for service quality and safety assessment. The ideal practitioner should have a high caecal intubation rate, a high detection and removal rate of polyps with significant pathology, and a low complication rate.
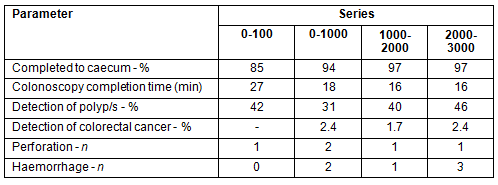
Improved completion rates were associated with a decrease in completion time and improved adenoma detection rates occurred over the sequential 1000 case intervals (Table 3). This 'learning curve' should be considered when assessing acceptable colonoscopy standards for practitioners at differing stages of development.
Table 3: Change in performance parameters over colonoscopy series
Evaluation for pathology is performed during colonoscopy and detection rates for polyps are reduced among practitioners with a 'normal' colonoscopy withdrawal time of less than 6 min. This finding has generated a recommendation of 8 minutes as the minimum standard withdrawal time24. Increases in colonoscopy withdrawal times, within limits, should lead to increased polyp and CRCa detection. However, there are no current recommendations regarding the ideal total colonoscopy completion time relative to polyp and cancer detection rates. 'Completion time' (from insertion to complete withdrawal) was recorded for this series because it better reflected the time required to negotiate the colon and include all procedures undertaken during colonoscope withdrawal. Recording completion time adds to quality and safety analysis in a meaningful way by acting as a cross-validation measure for difficulty and low detection rates. Importantly, detection, and therefore increased lesion biopsy or removal rates, would be expected to increase the risk of perforation and haemorrhage, and this corresponding complication rate should be accounted for in quality and safety audits. Conversely, reductions in adenoma detection rate would theoretically lead to fewer polyp removals and therefore reduced perforation and haemorrhage rates. Without consideration of adenoma (and CRCa) detection rates, such practitioners would appear to be of a high quality and safety. Thus, measuring quality and safety in colonoscopy should include the successful detection and removal of adenomas. Performing complex polypectomies also affects time to completion and complication rates. Although this series includes the performance of large polyp removal with base injections, the data collection did not specifically identify these more complex cases. Given the relative infrequency of such cases they are unlikely to have a significant impact on average time to completion over a large series but may significantly impact on complication rates, which are in the order of 1 in 1000. Therefore an associated increase risk of bleeding and/or perforation can be expected with complex cases. Identifying which practitioners undertake complex polypectomies may assist in determining acceptable complication rates for that subgroup. The 17 min average completion time in this study (including polypectomy time), combined with a high detection rate, compared with international standards, provide a new quality benchmark for proceduralists.
The major limitation of this study, which had a high detection and low complication rate, is that all colonoscopies were performed by a single GP proceduralist whose skill level might not be predictive of GP skills in general; however, the favourable outcomes comparisons suggest that the current international standards, generally for medical and surgical specialists, could and should be generally achievable with current Australian GP training requirements.
While the cost-effectiveness of this service versus a larger more centralised service has not been addressed, avoiding the transfer of patients to and from larger centres would result in significant savings. Patients would need to travel 70 km to Shepparton (50 min) or 92 km to the next nearest regional centre (Bendigo, 77 min), or utilise a train or bus service (indirect, lengthy travel times, 3 times a day). Since the average age in this series was 60 years, many patients would need to arrange an overnight stay to travel to larger centres, incurring additional costs (eg time off from work). The National Bowel Cancer Screening Program is gradually becoming established as public awareness of the importance of screening and early detection of bowel cancer and polyps increases. This in turn will increase the demand for colonoscopy services. Targeted funding for an extension of the GP proceduralist service model described in this article would help address the shortage of appropriate rural (or urban) proceduralists. Finally, as quality and safety become increasingly important to the public, this study provides a validated model for assessing the safety and quality of a colonoscopy service. This model could be extended to other procedures.
This audit shows that rural GP proceduralists can provide high quality, safe colonoscopies with the current Australian training requirements. With appropriate training, and the establishment of clear performance parameters, local rural GP proceduralists could address the current inequity between rural and urban communities and address increased demands on colonoscopy services as effective screening programs are established in the near future. It is recommended that the data collection methods used in this study become standard for GP, and other, proceduralists.
References
1. Australian Bureau of Statistics. 3303.0 - Causes of Death, Australia, 2009. Overview, Table 2.1. (Online) 2009. Available: http://abs.gov.au/ausstats/abs@.nsf/Products/B6940E9BF2695EE1CA25788400127B0A?opendocument (Accessed 31 August 2011).
2. St John J, Dodd E, Ellard K, Foreman L, Jones D, Luck A et al.,The National Bowel Cancer Screening Program Quality Working Group. Improving Colonoscopy Services in Australia. Canberra, ACT: Australian Government Department of Health and Ageing, 2009. Table 2, Page 19. Available: http://www.cancerscreening.gov.au/internet/screening/publishing.nsf/Content/3FD09B61D2B4E286CA25770B007D1537/$File/Improving%20col%20serv0709.pdf (Accessed 31 August 2011).
3. Nelson DB, McQuaid KR, Bond JH, Lieberman DA, Weiss DG, Johnston TK. Procedural success and complications of large-scale screening colonoscopy. Gastrointestinal Endoscopy 2002; 55: 307-1422.
4. Rathgaber SW, Wick TM. Colonoscopy completion and complication rates in a community gastroenterology practice. Gastrointestinal Endoscopy 2006; 64: 556-562.
5. Dafnis G, Granath F, Påhlman L, Ekbom A, Blomqvist P. Patient factors influencing the completion rate in colonoscopy. Digestive and Liver Diseases 2005; 37: 113-118.
6. Bowles CJA, Leicester R, Romaya C, Swarbrick E, Williams CB, Epstein O. A prospective study of colonoscopy practice in the UK today: are we adequately prepared for national colorectal cancer screening tomorrow? Gut 2004; 53: 277-283
7. Church JM. Complete colonoscopy: how often? and if not, why not? American Journal of Gastroenterology 1994; 89: 556-560.
8. Cotton PB, Connor P, McGee D. Colonoscopy: practice variation among 69 hospital-based endoscopists. Gastrointestinal Endoscopy 2003; 57: 352-357
9. Froehlich F, Harris JK, Wietlisbach V. Current sedation and monitoring practice for colonoscopy: an International Observational Study (EPAGE). Endoscopy 2006; 38: 461-469
10. Singh H, Penfold R, DeCoster C, Kaita L, Proulx C, Taylor G et a.. Colonoscopy and its complications across a Canadian regional health authority. Gastrointestinal Endoscopy 2009; 69(3): 6653.
11. Gatto N, Frucht H, Sundararajan V, Jacobson J, Grann V, Neugut A. Risk of perforation after colonoscopy and sigmoidoscopy: a population-based study. Journal of the National Cancer Institute 2002; 95(3): 230-236.
12. Levin T, Wei ZM, Conell C, Seeff L, Manninen D, Shapiro J. Complications of colonoscopy in an integrated health care delivery system. Journal of Internal Medicine 2006; 145: 880-886.
13. Rabeneck L, Paszat LF, Hilsden RJ, Saskin R, Leddin D, Grunfeld E, Wai E, Goldwasser M, Sutradhar R, Stukel TA. Bleeding and perforation after outpatient colonoscopy and their risk factors in usual clinical practice. Gastroenterology 2008; 135(6): 1899-1906.
14. Korman L, Overholt B, Box T, Winker C. Perforation during colonoscopy in endoscopic ambulatory surgical centers. Gastrointestinal Endoscopy 2003; 58(4): 554-557.
15. Ko C, Riffle S, Michaels L, Morris C, Holub J, Shapiro J et al. Serious complications within 30 days of screening and surveillance colonoscopy are uncommon. Clinical Gastroenterology and Hepatology 2010; 8(2): 166.
16. Leffler DA, Rakhi Kheraj MS, Bhansali A ,Yamanaka H, Neeman N, Sheth S et al. Adenoma detection rates vary minimally with time of day and case rank: a prospective study of 2139 first screening colonoscopies. Gastrointestinal Endoscopy 2012; 75(3): 554-560.
17. Williams J, Holub J, Douglas F. Polypectomy rate is a valid quality measure for colonoscopy: results from a national endoscopy database. Gastrointestinal Endoscopy 2012; 75(3): 576-582.
18. Millan MS, Gross P, Manilich E, Church J Adenoma detection rate: the real indicator of quality in colonoscopy. Diseases of the Colon and Rectum 2008; 51(8): 1217-1220.
19. Kaminski M, Regula J, Kraszewska E, Polkowsk M, Wojciechowska U, Didkowska J et al. Quality Indicators for colonoscopy and the risk of interval cancer. New England Journal of Medicine 2010; 362: 1795-1803.
20. Bair D, Pham J, Seaton MB, Arya N, Pryce M, Seaton TL. The quality of screening colonoscopies in an office-based endoscopy clinic. Canadian Journal of Gastroenterology 2009; 23(1): 41-47.
21. Chilton A, Rutter M. NHS BCSP Quality Assurance Guidelines for Colonoscopy.NHS BCSP publication 6 February 2011. (Online) 2011. Available: http://www.cancerscreening.nhs.uk/bowel/publications/nhsbcsp06.pdf (Accessed 31 August 2011).
22. The American Society for Gastroenterology (ASGE) and The American College of Gastroenterology (ACG) Task Force on Quality Endoscopy. Quality Indicators for Colonoscopy. American Journal of Gastroenterology 2006; 101: 873-885.
23. Rabeneck L, Rumble RB, Axler J, Smith A, Armstrong D, Vinden C et al, Cancer Care Ontario's Colonoscopy Standards Expert Panel. Cancer Care Ontario Colonoscopy Standards: standards and evidentiary base. Canadian Journal of Gastroenterology 2007; 21(Suppl D): 5D-24D.
24. Barlcay RL, Vicari JJ, Doughty AS, Johanson JF, Greenlaw RL. Colonoscopic withdrawal times and adenoma detection during screening colonoscopy. New England Journal of Medicine 2006; 355: 2533-2541.

