In India 68.8% of the population resides in a rural area1. The public health system for formal health care in rural India consists of three tiers: Sub-Centres, Primary Health Centres (PHC) and Community Health Centres (CHC). There is a Sub-Centre with a male and female worker for every 5000 population; a PHC with a medical doctor and para-medical staff for every 30 000 population; and a 30 bed CHC with basic specialists for every 100 000 population2.
Even so, the rural health service is grossly inadequate. Rural areas have only 0.77 hospitals, 1.37 dispensaries, 3.2 PHCs and 44 hospital beds per 100 000 population, compared with the urban service of 4.48 hospitals, 6.16 dispensaries and 308 beds per 100 000 population3.
In India, allopathic doctors exceed 0.5 per 1000 population (one allopathic doctor for 1440 population) and if qualified Ayurveda, Unani, Siddha, Naturopathy and Homeopathy (AYUSH) doctors are included, the doctor-to-population ratio is more than to 1 per 1000 (one doctor for 750 population)4. Despite the large number of trained medical practitioners available in the country, the majority of medical graduates (74%) serve in urban areas5. In 2010 there was a shortfall in the total requirement for male health workers at Sub-Centres (64%) and allopathic doctors in PHC (10.3% of approximately one doctor per PHC)6. When considered according to Indian Public Health Standards which recommend two medical officers per PHC for adequate, quality health care7, the shortfall is more acute. This situation is compounded by endemic absenteeism among government health personnel in rural health centres8. As a result, unqualified private practitioners are likely to provide health care, especially to those living in urban slums, and remote rural and tribal areas9.
In rural areas, the private health sector provides approximately 81% of outpatient care and 56% of inpatient care10. The private health sector in rural areas consists mainly of unqualified medical practitioners11-13. There are few studies on the profile and practices of unqualified rural medical practitioners in India. This article presents the profile and medical practices of private rural health providers (PRHPs) in rural Ballabgarh, located in Haryana State.
The study was conducted at the Comprehensive Rural Health Services Project (CRHSP), Ballabgarh, located in Haryana, India. The CRHSP is an Intensive Field Practice Area (IFPA) under Centre for Community Medicine, All India Institute of Medical Sciences (AIIMS), New Delhi. The IFPA consisted of 28 villages catering for a population of 85 590 in 2008. Public healthcare services in these villages are provided via two PHCs.
Data were collected from July 2007 to June 2008. The study subjects included all PRHPs practicing in the study area for more than one year who had a healthcare facility (clinic or hospital). Private Rural Health Providers were defined as13:
...'qualified' if they had received a formal medical training in any system of medicine (Allopathy or Indian) from a recognised college/institution and 'unqualified' if they had not received any formal training in any system of medicine.
Traditional healers were excluded from the study. A list of the names, addresses and telephone numbers of all practicing PRHPs in the area was prepared with the assistance of key informants such as health workers and PHC medical officers.
The PRHPs were visited three times before they were classified unavailable. Written informed consent was obtained from all participating PRHPs. Interviews were conducted using a pre-tested interview schedule and data were entered and analysed using Microsoft Excel.
Ethics approval
Ethical clearance was provided by the ethical review committee of AIIMS, New Delhi (A-25/25.07.2007).
There were a total of 101 PRHPs in 28 villages, of which 87 were eligible. Of these, four declined participation and three PRHPs could not be contacted, giving a total of 80 PRHP participants (response rate 93%).
Approximately half the participating PRHPs had completed up to 12th standard education. Most were unqualified; however, three providers claimed that they had received formal training in one of the Indian systems of medicine (Table 1).
Table 1: Distribution of private rural health providers according to their profile (N=80)
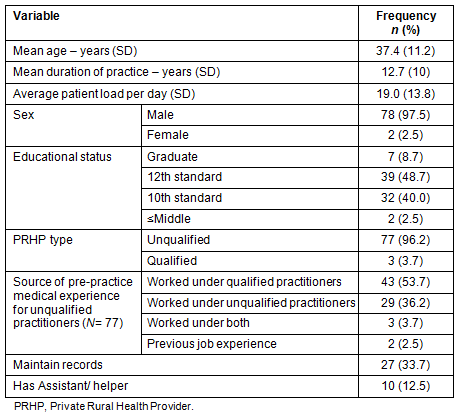
A half of the PRHPs had a separate space or a screened area for patient examination. Five (6%) had laboratory facilities and two (2.5%) had an X-ray facility. Three PRHPs had a separate labour room and a dressing room. One unqualified PRHP had an emergency room, an operation room and a 15 bed ward. The average patient load per day per PRHP was 19 (range 2-100). All PRHPs had a stethoscope (100%), and almost all had a thermometer (99%) and blood pressure apparatus (96%). A nebuliser, weighing machine and needle destroyer were available for 22.5%, 8.7% and 2.5%, respectively.
Most of the PRHPs prescribed and dispensed medicines (98.7%), administered injections (98.7%) and intravenous (IV) fluids (98.7%), and conducted minor surgical procedures (78.5%). Almost all PRHPs reported administering IV fluids in cases of diarrhoea, and 15% used IV fluids to treat fever (Table 2).
Table 2: Distribution of private rural health providers according to practice type
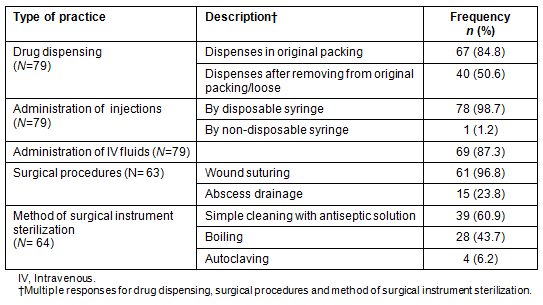
Two-thirds of the PRHPs reported that they disposed of infectious and pharmaceutical waste with the general waste. Dumping 'sharps' (eg needles, scalpels, broken vials and ampoules) was reported by 43.7% of the PRHPs. Other waste disposal practices were reported to be burial and burning. Nine (11.3%) mentioned that they sold used syringes and needles to junk dealers.
Seven PRHPs (8.7%) reported that they were involved in a national health program: three worked as DOTS (Directly Observed Treatment-Short Course) providers under the Revised National Tuberculosis Control Program, three worked as polio vaccinators under the National Polio Surveillance Program; and one provider had worked as both DOTS provider and polio vaccinator.
Most PRHPs (93%) expressed a need for training. For one-third this need was for information about new diseases and new medicines, and for 7% it was for training in injection practices (techniques) and medicine dosages.
Discussion
The finding that most of the PRHPs were unqualified is similar to that of past studies13-20. According to the 53rd Annual report of AIIMS in 2008-2009, the total number of patients seen by PHC under CRHSP Ballabgarh was 43 090 in one year, which is equivalent to approximately 60 patients per PHC/day21. In contrast, the PRHPs in the present study reported seeing approximately 19 patients per day (total for all 80 PRHPs = approximately 1520 patients per day [19 x 80]). Therefore, the average number of patients seen per day by PRHPs in the field practice area was much higher than the outpatient departments of the two PHCs in the area (1520 vs 120), demonstrating that PRHPs cater for the most of the patients in this rural area.
A majority of the PRHPs disposed biomedical waste with general waste, and the colour-coded dustbins recommended for biomedical waste disposal were not observed in any of the clinics. This lack of knowledge and incorrect biomedical waste disposal was also evident in the harmful practice of selling of used needles and syringes to junk dealers. The Ministry of Environment and Forests of India Bio-Medical Waste (Management and Handling) Rules, 201122, which apply to all persons who handle biomedical waste, recommends deep burial in rural areas22. In the present study, less than 15% of PRHPs reported burial of biomedical waste, and none of these complied with the standard of deep burial. Thus there is a need for education in biomedical waste management to bring PRHPs into compliance with the regulations.
The PRHPs were not actively involved in national health programs. Successful utilization of unqualified medical practitioners in implementing family planning and malaria programs, and AIDS awareness campaigns has been reported by health authorities in the Khammam District of Andhra Pradesh23, and also in the National Tuberculosis Control Program in Bangladesh24. The wide availability of rural PRHPs represents an untapped resource for supervised involvement in national health programs25.
Although most of the PRHPs were unqualified and worked with only basic health infrastructure, they provided a wide range of health services (eg consultation, prescription and dispensing of medicines, administration of injections and IV fluids, minor surgical procedures). While past studies have reported poor knowledge and skills among PRHPs in managing common ailments26-28, unqualified PRHPs are the preferred providers due to their wide availability13 and accessibility11. The Indian Medical Degrees Act, 1916, Section 6-A(1)29 and the Indian Medical Council Act1956, Sections 15 & 2530, have been enacted to punish those who impersonate qualified practitioners in western medical science, and those not registered with state medical councils. However, to date these acts have been unable to check the existence of unqualified private practitioners23, or to regulate their harmful practices. However, because they often serve as the first community contact in rural health care, it is recommended that unqualified PRHPs be utilized for disease surveillance, prevention and education programs.
Unqualified PRHPs do provide substantial outpatient healthcare services in rural Ballabgarh, India. This study revealed their inadequate biomedical waste disposal practices and the need for monitoring and training them in this and safe injection techniques. It is strongly recommended that they be utilised in important public health programs such as disease surveillance.
Acknowledgement
The authors acknowledge the staff and health workers of PHC Chhainsa and PHC Dayalpur who helped in approaching PRHPs in the villages at CRHSP Ballabgarh.
References
1. Office of the Registrar General & Census Commissioner, Government of India. Provisional Population Totals. Rural- Urban Distribution. Figures at a glance, India. (Online) 2012. Available: http://www.censusindia.gov.in/2011-prov-results/paper2/data_files/india/paper2_at_a_glance.pdf (Accessed 9 July 2012).
2. World Health Organization. India country health system profile. (Online) 2009. Available: http://www.searo.who.int/en/Section313/Section1519_10852.htm (Accessed 16 May 2009).
3. Duggal R, Gangolli LV. Introduction. In: LV Gangolli, R Duggal, E Shukla (Eds). A Review of Healthcare in India. Centre for Enquiry into Health and Allied Themes, 2005; 3-18. (Online) 2009. Available: http://www.cehat.org/publications/PDf%20files/r51.pdf (Accessed 26 February 2009).
4. Central Bureau of Health Intelligence. Directorate General of Health Services, Ministry of Health & Family Welfare, Government of India. Human resources in health sector. In: National Health Profile (NHP) of India, 2010. (Online) 2012. Available: http://cbhidghs.nic.in/writereaddata/mainlinkFile/Human%20Resources%20in%20Health%20Sector%202010.pdf (Accessed 10 April 2012).
5. Ministry of Health and Family Welfare, Government of India. Report: Task force on medical education for the national rural health mission. Chapter 1. Overview of the National Health System. (Online) 2011. Available: http://mohfw.nic.in/NRHM/Documents/Task_Group_Medical_Education.pdf (Accessed 24 December 2011)
6. Ministry of Health and Family Welfare, Government of India. Rural health care system in India, Rural health statistics in India 2010. Updated March 2010. (Online) 2012. Available: http://nrhm-mis.nic.in/UI/RHS/RHS%202010/RHS%202010/Rural%20Health%20Care%20System%20in%20India.pdf (Accessed 15 March 2012).
7. Directorate General of Health Services, Ministry of Health & Family Welfare, Government of India. Indian Public Health Standards (IPHS) for Primary Health Centres. Guidelines (Revised 2010). (Online) 2012. Available: http://mohfw.nic.in/NRHM/IPHS_Revised_Draft_2010/PHC_Revised_Draft.pdf (Accessed 15 March 2012).
8. Bajpai N and Goyal S. Primary Health Care in India: Coverage and Quality Issues. Center on Globalization and Sustainable Development (CGSD): Earth Institute, Columbia University, New York; June 2004. Working Paper Series, No. 15. (Online) 2012. Available: http://globalcenters.columbia.edu/southasia/files/mumbai/content/pdf/3._bajpai_primaryhealth_2004_15.pdf (Accessed 9 July 2012).
9. Planning Commission, Government of India. Tenth Five-Year Plan: 2002-2007. Sectoral policies and programs, Vol. 2. 2002. (Online) 2009. Available: http://planningcommission.nic.in/plans/planrel/fiveyr/10th/volume2/10th_vol2.pdf (Accessed 10 May 2009).
10. National Sample Survey Organisation (NSSO). Morbidity and treatment of ailments. Report no. 441. New Delhi: NSSO, Government of India; 1998. (Online) 2009. Available: http://mospi.nic.in/rept%20_%20pubn/441_final.pdf (Accessed 16 September 2009).
11. Gautham M, Binnendijk E, Koren R, Dror DM. 'First we go to the small doctor': First contact for curative health care sought by rural communities in Andhra Pradesh & Orissa, India. Indian Journal of Medical Research. November 2011; 134: 627-638
12. Banerjee A, Deaton A, Duflo E. Health, health care, and economic development: wealth, health, and health Services in rural Rajasthan. American Economic Review 2004; 94(2): 326-330.
13. Rhode JE, Viswanathan H. The rural private practitioner. New Delhi: Oxford University Press,1995.
14. Rao PH. Profile and practice of private medical practitioners in rural India. Health and Population: Perspectives and Issues 2005; 28(1): 40-49.
15. Alexander CA, Shivaswamy MK. Traditional healers in a region of Mysore. Social Science and Medicine 1971; 5(6): 595-601.
16. Bhat R. Private medical practitioners in rural India: implications for health policy. Report submitted to the Indian Institute of Management. Ahmedabad: Indian Institute of Management, 1999.
17. Neumann AK, Bhatia JC, Andrews S, Murphy AK. Role of the indigenous medicine practitioner in two areas of India, Report of a study. Social Science Medicine 1971; 5(2): 137-149.
18. Chuttani CS, Bhatia JC, Vir D, Timmappaya A. Study of private medical practitioners in rural areas of a few states in India. Indian Journal of Medical Education 1973; 12(3-4): 248-252
19. Kakar DN. Traditional healers in North India: a study. Nursing Journal of India 1983; 74(3): 61-63.
20. Nandraj S, Duggal R. Physical standards in the private health sector- a case study of rural Maharashtra. Mumbai: Centre for enquiry into health & allied themes (CEHAT), 1997. (Online) 2009. Available: http://www.cehat.org/infocentre/annot3.html (Accessed 10 May 2009).
21. Centre for Community Medicine, All India Institute of Medical Sciences. 53rd AIIMS Annual Report, 2008-2009. New Delhi: All India Institute of Medical Sciences, 2010; 177-204. (Online) 2011. Available: http://www.aiims.edu/aiims/annual-report/AIIMS%20Annual%20Repront%202008-2009.pdf (Accessed 20 December 2011).
22. Ministry of Environment and Forests, Government of India. The Gazette of India, Extraordinary (2011), Part II- Section 3, Subsection (ii). Notification (24 August, 2011). (Online) 2011. Available: http://moef.nic.in/downloads/public-information/draft-bmwmh.pdf (Accessed 21 December 2011).
23. Narayana K V. The unqualified medical practitioners: methods of practice and nexus with the qualified doctors. Working paper no.70. Begumpet, Hyderabad: Centre for Economic and Social Studies, 2006. (Online) 2009. Available: http://saber.eastasiaforum.org/testing/eaber/sites/default/files/documents/CESS_Narayana_2006.pdf (Accessed 16 May 2009).
24. Salim MAH, Uplekar M, Daru P, Aung M, Declercq E, Lönroth K. Turning liabilities into resources: informal village doctors and TB control in Bangladesh. Bulletin of the World Health Organizatio. 2006; 84: 479-484
25. Yadav K, Jarhyan P, Gupta V, Pandav CS. Revitalizing rural health care delivery: Can rural health practitioners be the answer? Indian Journal of Community Medicine 2009; 34: 3-5.
26. Alam S, Khan Z, Amir A. Knowledge of diarrhea management among rural practitioners. Indian Journal of Pediatrics 2003; 70: 217-219.
27. Kanjilal B, Mondal S, Samanta T, Mondal A, Singh S. A parallel health care market: rural medical practitioners in West Bengal, India. Future Health Systems (FHS) Research Brief No. 2: 4. Jaipur: Institute of Health Management Research, 2007. (Online) 2011. Available: http://www.research4development.info/PDF/Outputs/FutureHealth_RPC/ParallelHealthResBrief2.pdf (Accessed 10 January 2011).
28. Singh J, Bhatia R, Gandhi JC, Kaswekar AP, Khare S, Patel SB, Oza VB, Jain DC, Sokhey J. Outbreak of viral hepatitis B in a rural community in India linked to inadequately sterilized needles and syringes. Bulletin of the World Health Organization. 1998; 76(1): 93-98.
29. Medical Council of India. The Indian Medical Degrees Act, 1916 (ACT No. VII of 1916). Available: http://www.mciindia.org/acts/THE-INDIAN-MEDICAL-DEGREES-ACT.pdf (Accessed 16 March 2012).
30. Medical Council of India. The Indian Medical Council Act, 1956 (102 of 1956). 30th December, 1956 (As amended by the Indian Medical Council (Amendment) Acts, 1964, 1993 & 2001). Available: http://www.mciindia.org/ActsandAmendments/TheMedicalCouncilAct1956.aspx (Accessed 16 March 2012).



