Indigenous people have a similar or lower incidence of total cancer compared with other Australians, though patterns of incidence vary by site1-4. Cancer mortality is generally higher for Indigenous people than for non-Indigenous people. While cancer survival for non-Indigenous Australians has increased, this has not been shared by their Indigenous counterparts5. Cancer survival in South Australia, Queensland (QLD) and the Northern Territory is lower for Indigenous people than non-Indigenous people2,3,6. The under-ascertainment of Indigenous status in censuses, health surveys, and administrative datasets across some jurisdictions is likely to mean that the burden of cancer in Indigenous people is underestimated7,8.
In QLD, Indigenous people have an overall 21% lower incidence of cancer9. Indigenous people are more likely to have aggressive cancers and be diagnosed at a later stage2,8. They are also more likely to have higher rates of co-morbidities, wait longer from diagnosis to surgery, have interrupted treatment patterns and reach death earlier2. Indigenous people are 36% more likely to die from cancer in comparison with the total QLD population9.
Given the disproportionate rate of survival between Indigenous and non-Indigenous people, and the multi-faceted reasons for this, the need for systematic delivery of cancer control programs and services is important10. Systems of belief and perception about cancer directly impact on the care-seeking behaviour of Indigenous people5. Age, socioeconomic status, race, language and culture, attitudes and family composition are consistently identified as likely factors that may result in inequitable access to cancer services10. Additionally, a higher proportion of Indigenous people live in more rural and remote areas and thus also experience the difficulties associated with distance from their homes to major treating centres, including travel time, cost, accommodation and separation from support networks which have been documented as possible reasons for inadequate and interrupted treatment in other Indigenous populations10,11. Specific cultural barriers may also exist, including history of racism, lack of Indigenous staff, limited to no culturally appropriate information available, isolating hospital environments, differences in communication styles between patients and health professionals, and lack of understanding about Indigenous culture and life circumstance12. Thus the role that support services can play in facilitating these difficulties cannot be understated.
The aim of this study was to identify and describe the cancer support services available to all cancer patients in QLD. In particular, the suitability or potential cultural appropriateness of these services for Indigenous cancer patients were examined and considered their location relevant to the population.
Study design and sample
The data reported here were collected in 2009 from a cross-sectional questionnaire of cancer support services in QLD. Support services were considered to be those that had the resources to help cancer patients with their physical, emotional, psychological and social needs, as well as providing information and practical support. The Cancer Council Queensland (CCQ) is considered to be the peak cancer advocating agency in QLD. The CCQ provides support and refers patients to support for their cancer, particularly through the cancer helpline. The cancer helpline database of all cancer support services and groups in QLD (n=344) was ascertained. All services which met one of the following inclusion criteria were included: (i) had in their name or description included the word 'cancer' or an 'Indigenous term'; or (ii) included the words 'transport', 'accommodation' and/or 'financial'.
A snowball-sampling recruitment strategy was followed whereby services contacted from the CCQ list were asked to identify and provide details for other potential participants from among their own networks and acquaintances.
The manager from each service was contacted initially via telephone, a brief overview of the study was provided, and permission gained to forward a copy of the study questionnaire. The questionnaire was developed online using SurveyMonkey (www.surveymonkey.com) which also acted as a data collection and storage tool. The questionnaire was forwarded either by email (with a web link and attached copies of the information sheet and survey), fax or post (at the discretion of the interviewee). Questionnaires completed via post, fax or email were entered into SurveyMonkey.
After 3 days from the initial point of contact, a follow-up phone call was made to ensure that the service had received the questionnaire and to remind them it was due back within 7 days. At 7 days from the second contact a follow-up reminder phone call was made and, if requested, a second questionnaire was sent.
Questionnaires were completed by the Manager or relevant position (eg president etc) of the service.
Service classification
The selected services were considered 'Indigenous-specific' if they only provided a service to Indigenous clientele or 'Indigenous-friendly' if they had provided a service to 10 or more Indigenous clients in the previous year or had a specific staff member available for Indigenous clients.
Analyses
Data was downloaded from SurveyMonkey into Microsoft Excel 2007 and imported for analysis into SPSS v17.11 (www.spss.com). Means were calculated, as were standard deviation (normally-distributed data), medians, range (non-normally-distributed data), inter-quartile range (IQR) and proportions. Using the service address (postcode), and Google Earth, the longitudinal and latitudinal coordinates of each service were derived. These coordinates were used to map the service location against 2008 population data reported for local government areas (LGA) to assess distribution of services in relation to the Indigenous population using ArcGIS v9.3. (http://www.esri.com/software/arcgis/index.html). Responses from open-ended questions were analysed separately by two investigators performing manual thematic analysis, and then cross-checked and combined to develop an overall interpretation of the data13.
Ethical approval
Ethical approval for this study was obtained from the Human Ethics Committees of the Queensland Institute of Medical Research (#P1219) and the Australian National University (#2009/314).
There were 121 eligible services identified (five from snowballing), two were ineligible (did not service cancer patients), 113 agreed to participate in the study, and 83 completed a questionnaire. Eighty-three were included in the study (response rate 73.6% [83/119]) of which 36.1% of services returned the survey via the online option (SurveyMonkey).
Service characteristics
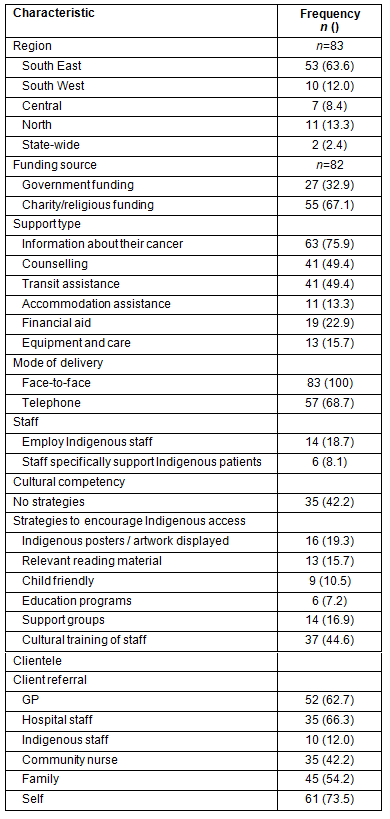
The characteristics of participating services are summarised (Table 1). The majority of services were located in the South-east QLD region. Over two-thirds (67.1%) of the services were funded by a charity and/or religious organisations, and 32.9% were government funded (state, federal or both). All 83 services provided support to cancer patients, and some also supported their families and friends. The type of support offered by the participating services included providing information about cancer (75.9%), counselling (49.4%), transport (49.4%), financial aid (22.9%), assistance with equipment and care (15.7%) and accommodation assistance (13.3%; this could be paying for accommodation, providing accommodation or helping to locate suitable accommodation). All services delivered support face to face, 68.7% (n=57) also delivered support by telephone and 50.6% (n=42) provided support through information (eg pamphlets or brochures about cancer). Of the services included, 44% (n=36) targeted specific cancer types, with the most common being breast cancer. The median number of staff employed was 1.5 (n=75, range 0-300 and IQR 0.0-16.0); however, 37.3% (n=28) reported no employed staff (ie services were run entirely by volunteers). The median number of volunteers in a service was 17.5 (n=58, range 1-2500 and IQR 4.4-70.0).
Table 1: Characteristics of cancer support services in Queensland
Indigenous specific characteristics
No 'Indigenous-specific' services were identified. Eleven services (13.8%) were considered 'Indigenous-friendly'. In the preceding 12 months, eight of the 'Indigenous-friendly' services saw a median of 28 Indigenous clients (range 10-500 and IQR 12.5-63.8) and five services saw a median of 10 Indigenous cancer clients (range 3-20). Six services (8.1%) had at least one specific staff member designated to supporting Indigenous clientele; all of these staff were non-Indigenous. The service positions held by these staff were diverse (breast cancer nurse, psychologist, community development worker, president and secretary of support group). Only these 11 services of the 83 saw either Indigenous clientele or had a staff member specific for Indigenous clients.
Fourteen services indicated that their service employed an Indigenous staff member (range 1-10) although four of those did not identify the number employed. The use of strategies to encourage Indigenous clientele to use their services was reported by 32.5% of services. The most common strategy used was displaying Indigenous posters and artwork followed by the provision of support groups and targeted reading material. Thirty-five services (42.2%) had no strategies in place.
Services were also asked if their staff participated in cultural training ('Have your staff participated in cultural training/awareness/competency? If yes, please describe'), of which staff from 37 services (44.6%) reported they did. This training varied from general multicultural training, awareness days, mandatory training in cultural diversity from Queensland Health and workshops with Indigenous people and or Elders. There was a general consensus from services that did not provide cultural training to staff that 'all cultures are treated the same' or that they did not have the capacity to undertake this training. Additionally, services were asked to report if they had established working relations with local Indigenous organisations. Thirty-six services (43.4%) reported never having contact with an Indigenous organisation, 26 (31.3%) sometimes did, and seven (8.4%) frequently had contact. Fourteen services did not report on having contact with an Indigenous organisation. One-third of services (33.7%) had provided a service to an Indigenous person in the previous 12 months. The number of Indigenous cancer patients reported by these services ranged from 1 to 20.
Services in this study documented a number of perceived barriers to Indigenous people accessing their specific cancer support service. A range of themes emerged including: a lack of awareness or knowledge about their service, lack of referral, limited culturally appropriate resources including Indigenous staff, lack of confidence by Indigenous people described as 'shyness', and the cost involved in accessing their service.
Regarding client referral to the participating services, most were self-referral (73.5%), hospital staff (66.3%), GPs (62.6%), community nurse (42.2%) and families (54.2%). Fewer referrals were received from Indigenous health workers' (ILOs; 12.1%).
Mapping revealed services were located where the majority of the QLD population resides, in the south-east of the state. The services identified as 'Indigenous-friendly' were also located in the south-east, with fewer located in the northern and western parts of the state. The percentage of Indigenous people per LGA for all services and Indigenous-friendly services are presented (Figs 1 & 2, respectively).
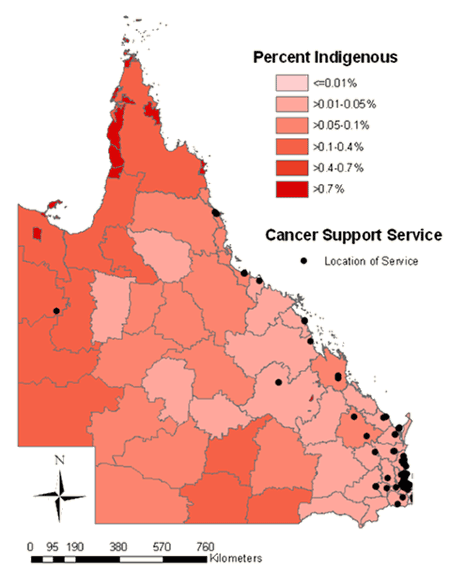
Figure 1: Location of all cancer support services in Queensland
and Percentage of Indigenous Australians by Local Government Area (2008).
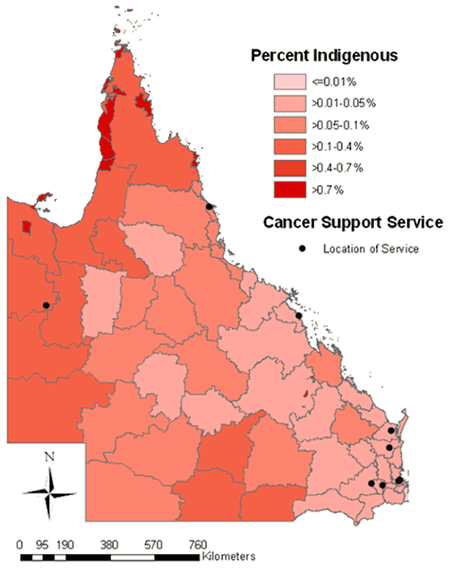
Figure 2: Location of 'Indigenous Friendly' cancer support services in Queensland
and Percentage of Indigenous Australians by Local Government Area (2008).
Discussion
The majority of cancer support services are located in South-east QLD, including those services identified as 'Indigenous-friendly'. Services were located in areas where the greatest absolute number of Indigenous people are, but were lacking in more remote areas where the percentage of Indigenous people is higher. Access to medical practitioners, health services and allied health professionals are limited for persons who live in rural and remote areas1. A recent review by van Schaik et al found that during cancer diagnosis and treatment stress is increased by a lack of social support networks if the patient must travel to and from hospital for treatment and with deliberation of costs, logistics, social obligation, emotional and physical distance and community isolation14,15. Areas identified by mapping where the proportion of Indigenous people is high tend to be more rural (and thus would have to travel for treatment) and without cancer support services. Indigenous cancer patients living in these rural areas will continue to suffer from the health, social and transport inequalities if a lack of support services is not available.
Most services were charity funded, indicating a potentially unstable source of support for cancer patients in QLD. Almost half the services target specific cancer types (eg breast cancer), further restricting access to support to those patients with less common cancers.
There were no 'Indigenous-specific' services identified and only a handful of services were classed as 'Indigenous-friendly', and most did not have Indigenous staff. There were no strategies to encourage Indigenous clientele or cultural training for staff in over one-third of the services. Most referral was by self-referral or hospital staff and GPs, with fewer referrals from ILOs.
Utilization of official support services by cancer patients is generally low, which has also been reflected here by low numbers of Indigenous clientele accessing the support services in the preceding 12 months16,17. Support services should consider utilising ILOs and engaging with Indigenous community organisations to increase referral of Indigenous cancer patients. This may especially be useful to overcome any issues of distrust Indigenous people often experience regarding westernized medical systems by having an ILO refer the patient to a service that may not be Indigenous-specific12,15.
Information was the most commonly reported form of support; however, while providing information is highly valuable, it is unknown how relevant or appropriate this information is for Indigenous people. To ensure that the information provided is beneficial to Indigenous cancer patients, it should be easy to understand, culturally appropriate, and contextualised5,18. It is likely that the information currently provided by these support services is not culturally relevant to Indigenous patients due to the large proportion of services having no contact with local Indigenous groups and the considerable numbers of staff within services not participating in cultural training. This is an area that, if addressed, could vastly improve the support and knowledge for Indigenous cancer patients provided by these support services. This could be achieved by implementing and fostering relationships with local Indigenous groups to ensure the cultural adequacy of the information provided19.
Other barriers reported in the literature that affect Indigenous patients uptake of services include lack of Indigenous staff, lack of understanding about culture, language barriers, failure to establish ongoing relationships and differences in communication style12. The present study shows that fewer services offered practical support such as transport, financial assistance and accommodation and more information based support, information that may not be culturally appropriate for Indigenous cancer patients. Most services could identify barriers to Indigenous patients accessing support but were restricted by capacity and funds to make changes that would address these barriers.
It is likely that these identified barriers can influence treatment decisions14,20. Appropriate support services have the capacity to improve Indigenous cancer patients experiences by supporting and assisting better access to care. Further research into the use of support services by Indigenous cancer patients is vital to understanding gaps which currently exist in the lack of Indigenous clientele using existing services demonstrated in this study. Furthermore, increasing culturally safe environments in mainstream support services is recommended as an important step. Fostering relationships with ILOs, local Indigenous health organisations and Elder groups in community and hospital settings is central to supporting Indigenous cancer patients.
Limitations
A notable limitation of this study is the selection of services from the CCQ database, which may mean some services were not included in the study. The CCQ is the central place for cancer patients' referral for support services; therefore, its database of services is likely to be comprehensive. In addition, given the use of snowballing, it is anticipated that selection bias has been limited. Some services did not complete the questionnaire and were not included in the study. There is no way of knowing how these non-responders differed from participating services. Recall bias should also be considered when interpreting these results because the numbers of staff and volunteers may have been reported from the manager's memory rather than from official records. Furthermore the number of Indigenous clients who accessed the service should be interpreted with caution because most services did not identify Indigenous status. Thus it is unclear as to how those estimates were made.
There is much room for improvement in supporting Indigenous patients in QLD who have cancer. The known barriers documented in this study should be addressed. Greater emphasis should be placed on providing support services where a high percentage Indigenous population resides to ensure support is maintained in rural and remote settings. Further efforts should be placed on establishing and developing relationships between Indigenous organisations and mainstream support services, and also in encouraging referrals from ILOs. Further research should be undertaken into the best models for providing culturally appropriate cancer support services to Indigenous people. These improvements are essential to ensuring that Indigenous patients are well supported throughout their cancer journey, in order to achieve higher rates of survival for Indigenous cancer patients in QLD.
Acknowledgements
Author LJ Whop was a Master of Applied Epidemiology (MAE) scholar at the National Centre for Epidemiology and Population Health, at The Australian National University and the Queensland Institute of Medical Research at the time this study was undertaken. The MAE program is funded by the Australian Government Department of Health and Ageing. PC Valery was supported by an Australian Research Council Future Fellowship (#FT100100511). National Health and Medical Research Council (Project Grant #1004643) partially funded this study.
References
1. Australian Bureau of Statistics and Australian Institute of Health and Welfare. The Health and Welfare of Australia's Aboriginal and Torres Strait Islander Peoples. Canberra, ACT: AIHW, 2008.
2. Valery PC, Coory M, Stirling J, Green AC. Cancer diagnosis, treatment, and survival in Indigenous and non-Indigenous Australians: a matched cohort study. Lancet 2006; 367(9525): 1842-1848.
3. Condon JR, Barnes T, Cunningham J, Armstrong BK. Long-term trends in cancer mortality for Indigenous Australians in the Northern Territory. Medical Journal of Australia 2004; 180(10): 504-507.
4. Miller J, Knott V, Wilson C, Cunningham J, Condon J, Roder D et al. Aboriginal and Torres Strait Islander Cancer Control Research Project. Canberra, ACT: Commonwealth of Australia, 2010.
5. Shahid S, Finn L, Bessarab D, Thompson SC. Understanding, beliefs and perspectives of Aboriginal people in Western Australia about cancer and its impact on access to cancer services. BMC Health Services Research 2009; 9: 132.
6. South Australian Cancer Registry. Cancer incidence, mortality and case survival in the South Australian Aboriginal Population. In: Epidemiology of Cancer in South Australia. Adelaide, SA: South Australian Cancer Registry, 1997.
7. Anderson I, Crengle S, Kamaka ML, Chen TH, Palafox N, Jackson-Pulver L. Indigenous health in Australia, New Zealand, and the Pacific. Lancet 2006; 367(9524): 1775-1785.
8. Cunningham J, Rumbold AR, Zhang X, Condon JR. Incidence, aetiology, and outcomes of cancer in Indigenous peoples in Australia. Lancet Oncology 2008; 9(6): 585-595.
9. Moore SP, O'Rourke PK, Mallitt KA, Garvey G, Green AC, Coory MD et al. Cancer incidence and mortality in Indigenous Australians in Queensland, 1997-2006. Medical Journal of Australia 2010; 193(10): 590-593.
10. Sanson-Fisher R, Carey M, Mackenzie L, Hill D, Campbell S, Turner D. Reducing inequities in cancer care: the role of cancer registries. Cancer 2009; 115(16): 3597-3605.
11. Kanekar S, Petereit D. Walking forward: a program designed to lower cancer mortality rates among American Indians in western South Dakota. South Dakota Medicine 2009; 62(4): 151-153, 155-157, 159.
12. Shahid S, Finn LD, Thompson SC. Barriers to participation of Aboriginal people in cancer care: communication in the hospital setting. Medical Journal of Australia 2009; 190(10): 574-579.
13. Patton MQ. Qualitative research and evaluation methods, 3rd edn. Thousand Oaks, CA: Sage, 2002.
14. van Schaik KD, Thompson SC. Indigenous beliefs about biomedical and bush medicine treatment efficacy for Indigenous cancer patients: a review of the literature. Internal Medicine Journal 2012; 42(2): 184-191.
15. Thompson SC, Shahid S, Bessarab D, Durey A, Davidson PM. Not just bricks and mortar: planning hospital cancer services for Aboriginal people. BMC Research Notes 2011; 4: 62.
16. Curry C, Cossich T, Matthews JP, Beresford J, McLachlan SA. Uptake of psychosocial referrals in an outpatient cancer setting: improving service accessibility via the referral process. Support Care Cancer 2002; 10(7): 549-555.
17. McDowell ME, Occhipinti S, Ferguson M, Chambers SK. Prospective predictors of psychosocial support service use after cancer. Psychooncology 2011; 20(7): 788-791.
18. Morgan DL, Slade MD, Morgan CM. Aboriginal philosophy and its impact on health care outcomes. Australian and New Zealand Journal of Public Health 1997; 21(6): 597-601.
19. Taylor KP, Thompson SC. Closing the (service) gap: exploring partnerships between Aboriginal and mainstream health services. Australian Health Review 2011; 35(3): 297-308.
20. Shahid S, Finn L, Bessarab D, Thompson SC. 'Nowhere to room ... nobody told them': logistical and cultural impediments to Aboriginal peoples' participation in cancer treatment. Australian Health Review 2011; 35(2): 235-241.




