Indigenous Australians experience poorer health than that of all other Indigenous cultures in developed nations1, and a greater burden of disease largely due to high levels of chronic illness and injury, that also contribute to developing functional disability at a younger age2 . The prevalence of dementia is almost 5 times that of non-Indigenous Australians, with high rates of self-reported falls, incontinence and pain3,4, and greater rates of hospitalisation and mortality for mental health illness5.
The provision of culturally appropriate community care services and support to Indigenous people, families and communities is challenging, with ongoing service gaps and unmet needs6-8. Aged and disability services in Australia have limited adaptation to differing cultural and remote locations, compounded by workforce issues, lack of infrastructure, education and the expense of transport8-10. Lack of communication and collaboration between diverse service providers engaging with communities can lead to a 'silo effect', resulting in isolation of resources, control and employment, leading to service gaps and confusion within the community about how to access services, and what individual services provide11. Lack of mutual cultural acceptance can lead to distrust of services for those living in communities, and on also a reluctance for service providers to relinquish control of funding and governance8,11.These issues were highlighted in a recent Australian Government document addressing effective practices for service delivery and coordination in Indigenous communities12. The document states that risk averse and inflexible organisations 'including silo based frameworks', and a 'one size fit all approach' do not work12. Further this report highlights the need for adequate evaluation of new models of care12.
Some innovative programs for the provision of services to older people, those with disabilities and mental illness and chronic disease management have been described12-14. The Family Well Being program in Far North Queensland is a 10 year research program15 initiated to focus on empowerment of community members to improve emotional wellbeing. This program aimed to foster personal transformation and a life tool of practical skills for dealing with day to day challenges with the secondary outcomes of improving social cohesion and advocacy through enhancement of resilience and self-worth. This program has been utilised as the basis for a range of health interventions including promotion of self-care in chronic conditions and men's health. The Yuendumu Old Peoples Programme based on a 'Family Model of Care' with underlying concepts of 'community control' and 'cultural comfort' allowed mainstream services to function in a complementary and supportive manner with professional services being accountable and responsive to local management that was governed by the structures and norms of community tradition16. Other initiatives such as the 'Troopy Respite Program' provide unique and culturally appropriate respite care and assistance17. The Katherine Health West Board is a larger, Aboriginal managed and facilitated organisation that aims to provide high quality collaborative care18.
The underlying principles needed for success of such programs include concepts of 'cultural comfort' and 'community control' and recognise mutual competence between traditional and mainstream services. Other essentials for remote health models include adequate funding, consultation, participation, leadership and quality assurance11,12, with the aim to enhance cultural resiliency, empowerment and assistance with education and advocacy. Research has strongly linked community development approaches with positive health outcomes, increased access to services and patient satisfaction7,19,20, tightly integrating mental, cultural and spiritual aspects of care.
Previous research by the present authors documented the methodology and outcomes describing specific areas of need and recommendations expressed by local community members and stakeholders in order to deliver appropriate care to the elderly and disabled living in remote communities6,21. These areas included the importance of local workforce engagement, the need for appropriate education and training, and improved service delivery.
Rationale for this research
This one-year pilot project arose from earlier work in the Kimberley6, that demonstrated barriers to accessing quality care, and provided recommendations on ways to improve care for elderly Aboriginal people with dementia in remote areas. This article describes the development and implementation of a locally responsive and culturally appropriate pilot model of care and respite for frail aged, extended to others with physical and mental disabilities, that was directed, applied and monitored by the community of Looma. The successes and shortcomings are explored and discussed.
Development of Lungurra Ngoora Model
The model structure was developed using a collaborative process with community members and council and relevant stakeholders, based on previous research6. Although the initial target group was older people with dementia, the steering committee determined a need for the inclusion of clients of all ages with all disabilities, including mental health, living in the community. The community care service model was named Lungurra Ngoora meaning Blue Tongue Lizard Home, in the Walmajarri language.
Community: Looma Community is a remote Aboriginal community in the Kimberley region of Australia, approximately 120 km south-east of Derby, in Nyikina country, with Nyikina, Walmajarri and Mangala the main language groups. There are approximately 350 people in the community. Looma was chosen because it has a high proportion of community members over the age of 45 years who had required residential care outside their community (14% aged >45 years in 2005-2007)22. This is a relatively large population for a remote community, and there was strong interest and support from the community council to improve care.
Funding: The initial funding for preliminary discussions, program set-up and external evaluation was made available in an NHMRC grant (458793). Subsequent negotiations with the Western Australian Department of Home and Community Care, Western Australian Country Health-Mental Health Service and the Disability Services Commission, resulted in 12 month funding for the employment of staff, education, transport and other accessories required for the provision of services.
Establishing governance structure: This project was co-managed by a steering committee consisting of representatives from the community council, government services and non-government organisations.
The model structure
The model structure (Fig1) consisted of the steering committee, a facilitator role, and a project coordinator who managed both community workers and the HACC support worker.
Steering committee The steering committee consisted of the Looma chairman, a Council member, and representatives of Disability, Aged Care Services, Population Health, Mental Health and others (Fig1). The committee provided guidance, expertise, resources, strategic management, and was accountable for financial and administrative tasks.
Facilitator: The facilitator role was developed to address the silo effect and facilitate partnership, collaboration and cooperation between services and the community. The facilitator's role was to manage the project coordinator, facilitate Steering Committee meetings, and report to the funding bodies. For the initial 6 months of the project this role was undertaken by the University of Western Australia, and then handed to Frontier Services, a non-government organisation experienced in remote Aboriginal health and aged care service delivery.
Local action group: The local action group consisted of community members and representatives from existing local service providers. Their role within the new model was to provide training and support to the community project staff, with the aim of developing independence in the program team to deliver services.
Project coordinator: The project coordinator managed the project on a day to day basis, supervising staff and facilitating training and administrative duties. The coordinator was the key contact for service providers, clients, family and community members. The coordinator managed: (i) community workers whose roles included the provision of education to community members, and respite activities such as fishing, visiting country and art; and (ii) a HACC (Home And Community Care) support worker who coordinated essential support for those in need of assistance with activities of daily living, assisting with respite care, meals, laundry and gardening. The latter role was an existing HACC funded role that was absorbed into the model. The coordinator and workers were employed within the community.
A service agreement was signed by all stakeholders with the objectives to: (i) identify appropriate clients the frail aged and people with physical and mental disabilities of all ages; (ii) identify their needs; (iii) administer services and support; (iv) employ a holistic, inclusive and creative approach to meet client and caregiver needs; and (v) develop a blueprint of the model that, along with the developmental process, is transferable to other Aboriginal communities.
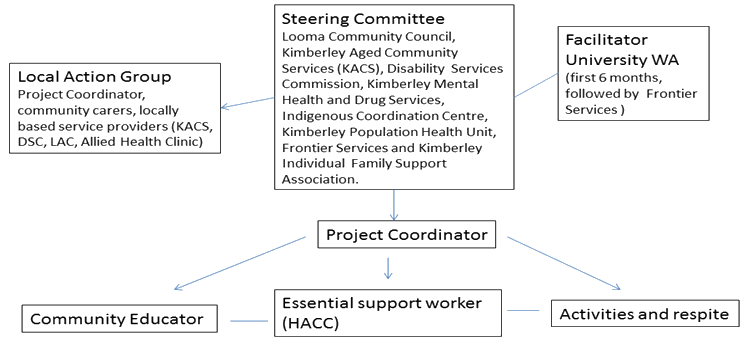
Figure 1: Community care service model structure.
Data collection and evaluation
Quantitative data were obtained from HACC performance of service records ('tick sheets', a simple attendance record utilised by HACC workers), weekly summaries of services showing service usage and the type and number of clients seen. In addition, data from staff diaries and letters received were abstracted (Table 1). Training sessions were documented.
External evaluation: An independent evaluation was conducted at baseline, 6 months and 12 months by qualitative methods. Baseline evaluation was conducted to determine the key needs of the community prior to the commencement of the project. These key factors focussed on service provision and access, cultural protection, accountability, partnerships and sustainability. Further evaluations were conducted at 6 and 12 months, on 11 clients and carers, six service providers, six project staff and two community council members, addressing service usage, advocacy, training and cultural considerations23. The information was transcribed, and thematically analysed. Finally, the project was evaluated by author RM against eight good practice principles in delivering services to Aboriginal people (Table 2). These principles include community participation and capacity building; resources; partnerships; workforce; evaluation; accountability; appropriate service delivery and cultural protection. Feedback to Steering Committee occurred at each point of evaluation. The independent consultant had family links to the community and substantial knowledge in the area. A summary of findings is described in Table 2, and full report is also available23.
Table 1: Use of services determined by tick sheets
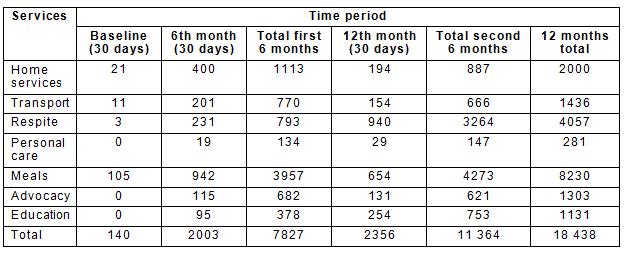
Table 2: Results of external evaluation including benefits and challenges to good practice guidelines (data source23)

Ethics approval
Ethics approval was obtained from the University of Western Australia (#RA/4/1/1686) and the Western Australia Aboriginal Health Information Ethics Committee (#153-02/07). Looma Community Council provided approval for the pilot program.
In the month prior to the pilot program, eight clients in Looma were receiving community care services (7 were frail aged and one had a disability/mental illness), and by 12 months this had increased to 22 (15 aged care, 3 mental health, 3 disability and 1 encompassing all three domains). Clients' ages ranged from 15 to 83 years; 11 (50%) were women.
There was an increase in services in all domains from 140 to 2356 per month (Table 1). Home services included cleaning, laundry, shopping, yard maintenance and social support. Respite included fishing, camping, art activities, hunting, BBQ picnic and others. Advocacy referred to assistance in accessing appropriate services and liaison between services. For example. Lungurra Ngoora staff liaised with occupational therapists and the community maintenance workers to improve the safety and independence of clients. Tasks completed included wheelchair maintenance, installation of handrails, provision of equipment to support activities of daily living equipment, and after much discussion, restoration of some footpaths. Transport was facilitated by the purchase of a second-hand vehicle with wheelchair access, which allowed greater access to activities such as fishing, and was supplemented by the HACC bus. Caregiver and wider community education needs were identified by Lungurra Ngoora staff members, and the education and training to meet these needs was organised by the community education officer. This education was delivered by the staff members, members of the local action group (including the clinic and allied health staff) or external educators such as the Dementia Behavioural Advisory Service who staff organised visits to the community and provide training to staff and caregivers. Staff education totalled 29 training sessions, including five staff completing Aged Care Certificate 3 part 1 courses, mental health first aid and dehydration training.
At 12 months, six local people were employed by the program, three (2 full-time equivalent [FTE]) funded through joint project funds, 1 FTE by HACC conversion monies, and 1.5 FTE by Federal Government Jobs Creation Packages. Two community CDEP (Federally funded Community Development Employment Project) workers assisted intermittently. There were an equal number of male and female staff and two were non-Aboriginal.
Discussion
This pilot program describes a model of community care service that was developed from widespread community consultation, and addresses the needs of the frail aged and those with disabilities and mental illness of all ages.
This collaboratively funded project resulted in a marked increase in the range of services available, which was welcomed by the community. Initially not all community referrals were appropriate and the project coordinator fielded these requests which resulted in more appropriate referrals for external services such as allied health. Improvement in services lead to an increase in community knowledge and expectation of what services could deliver, where previously there was limited services particularly for those with disability.
There was a marked increase in services overall. Initial data may have been underreported as staff addressed the importance of service reporting. Home services including cleaning, laundry, shopping, social support (such as assistance with paying bills, reading mail) and varied at times due to staff turnover and holidays and client cultural commitments, particularly in January. The peak use of home services occurred prior to Christmas with increased activities recorded. Personal care was focused on a few clients requiring more intensive showering and dressing and, therefore, accounted for fewer services. Meals were more reliably delivered and when fishing and hunting took place the food was shared with the clients. Frequent respite activities (eg fishing, barbeques) and transport accounted for a large increase in service usage, occurring on most days. Many clients were without easy access to transport and their transport needs included getting to clinic appointments, the local town and visiting relatives in residential care. Advocacy was identified as a key unmet need, with a lack of communication between service providers and family carers improving over the 12 month period. This included staff assisting with direction to and representation on services available, and follow up of services organised. For many clients this resulted in a number of contacts per day, diminishing isolation and increasing physical activity where possible.
One example of the effectiveness of the program was described by an allied health team professional who visited Looma monthly (p 64-65)21:
One particular client had [a] severe condition that limited his ability to walk or manage his personal hygiene...he had not walked for many months and was unable to access his toilet or shower, and his mental state was very low...however the project has enabled him to receive regular personal care services improving his personal hygiene, that enabled him to partake in valued activities such as fishing.
The visiting allied health professionals indicated:
We were able to utilise the Lungurra Ngoora employees to provide basic rehabilitation efficiently and effectively in our absence.
Apart from an increase in service delivery, other successes are discussed according to the principles of good practice11,12,19,20,23, as well the many challenges throughout program delivery (Table 2).
Community participation and capacity building
The development of the program resulted from extensive discussion with local caregivers, service providers and stake holders. The Steering Committee was a central mechanism for monitoring, decision-making and governance. There were pressures for members of the Steering Committee to play an increasing role in dispute resolution between staff and in other major decisions relating to the project. Although this occurred to some extent, the intention of the project was to increase local authority to make decisions about local services through the local action group and Looma Council. The Facilitator oversaw the steering meetings and the program became a standing agenda item on the Council meeting agendas. There was some sense of lack of ownership by Steering Committee service providers at times, that may have related to adjustment to relinquishment and the establishment of new roles. However, the service structure enabled members of the community to express their needs more easily. Having one service in place of the previous three separate services reduced duplication and led to improved working partnerships, with the potential to reduce service costs.
Resources and accountability
The additional resources were much appreciated by the community. However, this was complicated by unclear funding arrangements, and various financial providers were reluctant to combine project funds within one community budget, making monies difficult to track and allocate. Recommendations that simplification of the budget and access and accountability were not taken up. Stakeholders made differing contributions to the budget, resulting in different expectations of the outcomes. Some service providers insisted on very detailed financial reporting, markedly reducing flexibility in the employment of staff and service provision. The community recommended that project funds be held by the facilitator with support from the community, so that there was only one central budget. Eventually the mechanisms for financial reporting improved with the establishment of clearer reporting guidelines.
Partnerships
Establishing and maintaining partnerships was a key component of the project. The incorporation of a community based system of service provision that encompassed the client groups from three separate agencies (ie disability, aged care and mental health) was good sense in a community with limited infrastructure, and helped address the silo effect that is often a barrier to flexible care. Although the partnerships were generally respectful, there were some significant challenges caused by conflicts in relationships and understandings of roles. Key individuals can play an important role in driving new programs, but they can also have 'negative impacts'11. These difficulties resulted from lack of experience in new staff, and lack of adaptability in current service providers.
Workforce
There was a significant increase in community employment through the program, which ensured culturally sound practices. Council provided support to the project coordinator, and direct line management was provided through an independent facilitator. Education and training was provided reasonably freely because many of the staff had limited backgrounds in these services. There was a perception from some that too many training programs were undertaken in a short time, and that not all were appropriate for the skill set required. Many areas of development were requested, including numeracy, literacy and computer skills and potential for leadership development. Staff turnover did not disrupt service delivery because vacant positions were often quickly filled within the community. A more multiskilled approach was sought when employees were absent so others could step into their roles.
Delivery of appropriate services
A strength of the program was that it was a comprehensive community care service permanently based in the community that employed local people and reported to the community and the broader steering committee. Improved access and quality of services were provided, in particular regarding personal and respite care. Although it was perceived of as an aged care service by some, limiting service use by younger clients, education assisted in this regard. Families felt more confident in leaving their aged or disabled relatives for short periods knowing care was available. There were concerns that not all people receiving care had a level of unmet needs or the functional disability that required services, based on Governmental guidelines. However, overall there was a definite shift from service-led to needs-led care and support services.
Program challenges
There are many challenges in implementing a model of care in a remote community. The structure of this program enabled some of these challenges to be met; however, changes are recommended to reduce barriers18. Immediate challenges during the period of the pilot program included the absence of a community Chief Executive Officer for a number of months, changes in CDEP funding and a shortage of staff with driver's licences, among others. Many of these issues were overcome within the structure of the program (eg the coordinator assisted staff members to obtain drivers licences).
Other challenges included a complicated budget system, and clear determination of roles within the community with regard to decision-making. The latter, however, improved with the employment of an independent facilitator. It was considered that the local action group in this community setting added an unnecessary layer to the reporting structure, but it was an important inclusion during the developmental phases.
Existing external service providers need to be supported through a change in role from direct service provision to education and training. There were differences between key individuals who both facilitated and hindered progress and communication, a role that the facilitator would be required to manage to minimise any adverse impact on the program.
Although cultural partnerships and community control are espoused as best practice, there are challenges in accepting and relinquishing roles, governance and financial accountability. Service providers may be reluctant to hand over services to communities, often citing the need for financial accountability, although it is likely that other factors are also important. There is the danger that without formal partnerships, external providers will disengage their support.
A lack of stable and appropriate workforce may hinder functionality of community based services, although the experience of this pilot challenged this view, where services were maintained despite staff changes. Funding was provided predominantly through Home and Community Care, with smaller amounts from others, resulting in different expectations and inequality of status within the structure. Twelve months is a short period for a project of this nature to become embedded within a community. During the project, discussions were undertaken with all stakeholders and key funding organisations regarding on-going funding, with the initial understanding that current levels of funding would be maintained. Unfortunately this did not eventuate; however, some increase in the previous level of funding was maintained for those identified as requiring assistance in this program, and services reverted to initial providers with the major recommendations not maintained. A review of Kimberley state wide-services was initiated with the results of this program considered.
The major risk of limited term funding is the significant disappointment and disruption for communities and all those involved when programs cease; however, the documentation of programs that have been trialled and evaluated provides important information for future funding in a range of communities. The Lungurra Ngoora community care service model pilot project demonstrated a successful collaborative service model that addressed the care needs of older persons, those with disability and mental illness, and their carers in this remote community. The developmental approach, and model structure, could serve as a template for future delivery of services in remote Aboriginal communities.
Acknowledgements
The authors acknowledge the community members, carers, service providers and workers of Looma who participated in this program, and gave approval for publication of this work.
References
1. Hill K, Barker B, Vos T. Excess Indigenous mortality: are Indigenous Australians more severely disadvantaged than other Indigenous populations? International Journal of Epidemiology 2007; 36: 580-589.
2. Zhao, Y, Guthridge, S, Magnus, A, Vos, T. Burden of disease and injury in Aboriginal and non-Aboriginal populations in the Northern Territory. Medical Journal of Australia 2004; 180: 498-502.
3. Smith, K, Flicker L, Lautenschlager NT, Atkinson D, LoGiudice D et al. Dementia and cognitive impairment in remote Indigenous Australians - Evidence of different patterns of risk factors and increased prevalence. Neurology 2008; 71(19): 1470-1473
4. LoGiudice D, Smith K, Atkinson D Dwyer A, Almeida OA, Flicker L et al. The preliminary evaluation of the prevalence of falls, pain and urinary incontinence in remote living Indigenous Australians over the age of 45 years. International Medical Journal 2012; 42(6): e102-107. doi: 10.1111/j.1445-5994.2010.02332.x
5. Australian Institute of Health and Welfare 2009. Measuring the social and emotional wellbeing of Aboriginal and Torres Strait Islander peoples. Cat. no. IHW 24. Canberra, ACT: AIHW. http://www.aihw.gov.au/publication-detail/?id=6442468208 (Accessed 1 June 2010)
6. Smith K, Flicker L, Shadforth G, Carroll E, Ralph N, LoGiudice D et al. 'Gotta be sit down and worked out together': views of Aboriginal caregivers and service providers on ways to improve dementia care for Aboriginal Australians. Rural and Remote Health 11: 1650. (Online) 2011. Available: www.rrh.org.au (Accessed 5 December 2012).
7. Stewart S. Cultural competence in health care. Position Paper. Sydney, NSW: Diversity Health Institute, 2006.
8. Senior K. Testing the ICIDH-2 with Indigenous Australians: result of field work in two Aboriginal communities in Northern Australia. Canberra, ACT: Australian Institute of Health and Welfare, ICIDH Collaborating Centre and the Department of Health and Family Services, 2000.
9. O'Neill MK, Thomson N. A review of the literature on disability service for Aboriginal and Torres Strait islanders peoples. Australian Indigenous Health Bulletin 2004; 4(4): 1-26.
10. Alzheimer's Australia NT. Indigenous Dementia Project Report. Alzheimer's Australia 2002. (Online) 2002. Available: http://203.89.197.244/common/files/NT/Indigenous_Dementia_Project_Report_Dec02.pdf (Accessed June 2010).
11. Wakerman J, Chalmers EM, Humphreys JS, Clarence CL, Bell AI, Larson A et al. Sustainable chronic disease management in remote Australia. Medical Journal of Australia 2005; 183: S64-S68.
12. Stewart J, Lohoar S, Higgins D. Effective practices for service delivery coordination in Indigenous communities. Resource Sheet no 8. Closing the Gap Clearinghouse. Canberra, ACT: Australian Institute of Health and Welfare, 2011.
13. Shanley C. Developing more flexible approaches to respite for people living with dementia and their carers. American Journal of Alzheimer's Disease and Other Dementias 2006: 21(4): 234-241.
14. Fuller JD, Martinez L, Muyambi K, Verran K, Ryan B, Klee R et al. Sustaining an Aboriginal mental health service partnership. Medical Journal of Australia 2005; 183: S69-72.
15. Tsey K, Wilson A, Haswell-Elkins M, Whiteside M, Mc Calman J, Cadet-James Y et al. Empowerment-based research methods: a 10-year approach to enhancing Indigenous social and emotional wellbeing. Australasian Psychiatry 2007; 15(S1): S34-S38.
16. Smith K, Grundy JJ, Nelson HJ. Culture at the centre of community based aged care in a remote Australian Indigenous setting: a case study of the development of Yuendumu Old People's Programme. Rural and Remote Health 10: 1422. (Online) 2010. Available: www.rrh.org.au (Accessed 5 December 2012).
17. Working Carers Gateway. The Northern Territory's unique respite program. (Online) 2009. Available: http://www.workingcarers.org.au/index.php?option=com_content&view=article&id=976&Itemid=380 (Accessed 5 December 2012).
18. Katherine West Health Board. Something Special: A brief history of the Katherine West Health Board. Canberra, ACT: Aboriginal Studies, 2003.
19. Council of Australian Governments. National Partnership Agreement on Remote Service Delivery. (Online) 2009. Available: http://www.coag.gov.au/sites/default/files/remote_service_delivery_NPA_annual_report_COAG2010-11.pdf (Accessed 1 June 2010).
20. Australian Health Ministers' Advisory Council. Standing Committee on Aboriginal and Torres Strait Islander Health Working Party. AHMAC Cultural Respect Framework for Aboriginal and Torres Strait Islander Health, 2004-2009. Canberra, ACT: Australian Government, 2004.
21. Carroll E, Smith K, Flicker L, LoGiudice D, Shadforth G, Lindeman M et al. Indigenous Services Study: Lungurra Ngoora Community Care Final Report. (Online) 2010. Available: http://www.wacha.org.au/docs/misc/IDSS-Final-Report.pdf (Accessed 5 December 2012).
22. Smith K. Assessment and prevalence of dementia in Indigenous Australians. PhD thesis. University Western Australia, 2008.
23. Murphy R. Lungoora Ngoora Community Care Service. Evaluation Report. 2010. http://www.kamsc.org.au/research/downloads/Lungurra%20Ngoora%20Community%20Care%20Service%20Evaluation%20Report%20Aug10%20Final.pdf (Accessed June 2010).



