Providing quality health services to people living in remote areas is central to global efforts to achieve universal access to health care1. In general, urban areas are better served in terms of distance to facility, health worker density and quality of care, compared with remote areas2.
One of the primary ways to improve services in remote regions is through an effective and efficient referral system. Referrals have considerable implications for patient outcomes, the healthcare system and healthcare costs3,4. Strong referral mechanisms consist of identification of appropriate cases, organisation of transport, formalised communication between facilities, supervision and accountability for provider performance, and prompt and appropriate care at the receiving facility5,6. Obstacles to an efficient referral system include inadequate skill capacity of health workers and insufficient availability of medical equipment at both the referring and receiving facility, and poor transport infrastructure7.
Much of the literature on referral practices in low-and middle-income countries (LMICs) focuses on emergency obstetric care referrals6. Other studies on referral systems note a high level of inappropriate referrals and a failure to adhere to accepted guidelines. One study in Cambodia described road traffic injury referrals, finding that 60% of road traffic injury referrals made contact with the referral facility in advance5. Another descriptive study conducted in Honduras described the frequency of use of a referral form from primary care to tertiary care and found that a referral form was used in 70-80% of hospital referrals8. A third publication regarding referrals in LMICs estimated that most patients attending the highest level referral facility could have been treated at a lower level of care at one-sixth the cost9. There are a number of gaps in the literature regarding referrals within small island states and with regard to the financial burden of referrals between health facilities.
Effective referral systems are especially critical in resource-limited countries where small populations are separated by considerable distances. Much of the Pacific region faces these constraints. The Solomon Islands is a country of approximately 500 000 people in the Southwest Pacific consisting of approximately 1000 islands spread over approximately 1500 km. The urban population is only 18.6% of the total, with the vast majority of people living in outer islands10. The lack of user fees for accessing health services has led to the Solomon Islands having the lowest annual out-of-pocket spending on health in the world at approximately US$1 per year11. Its Human Development Index is 142 out of 187 countries and territories12.
Given these development and geographic challenges, the Solomon Islands' Ministry of Health and Medical Services (MHMS) aims to better understand and thus improve their referral system to improve quality of care and manage costs. Despite this, the evidence base on how the referral mechanism functions is very limited. This article aims to build an evidence base on inter-island referrals in the Solomon Islands, in particular regarding the number of referrals, reasons for referrals, and cost, to ultimately provide recommendations regarding referral practice effectiveness and efficiency.
Setting
The Solomon Islands' health system includes nurse aid posts, rural and area health centres, provincial hospitals and the National Referral Hospital (NRH) in the capital Honiara. There are seven provincial hospitals and four privately funded hospitals as well as 37 area health centres and more than one hundred rural health clinics13. As of December 2010, there were a total of 2728 health workers in the public sector including 153 medical doctors/dentists; 936 nurses; and 524 nurses' aides13. There is only one anaesthetist and due to power outages, lack of running water and other constraints, only two of the provincial hospitals are able to provide surgical care beyond very basic procedures14.
The Solomon Islands' Ministry of Health released patient referral guidelines in 2005. The guidelines aim to facilitate a coordinated, appropriate, patient-centred, yet economically sustainable system for referring patients to higher-level health facilities when healthcare needs cannot be managed at a lower level15. In support of the system, printed referral guidelines, and a patient referral form were created for provincial hospital use for referrals to the NRH16. In general, referral is meant to take place to the next highest level of care. For example, referral from an area health centre should go to the provincial hospital, except in emergency cases or where referral to the provincial hospital is not possible due to geography and ease of transport.
Data collection and analysis
The data for this study arose from the referral database collected and maintained by the NRH administrative office in Honiara. The database collects information on age, sex, ward or department visited, date of travel back to home port, home port and province for each individual whose travel back to home province was paid from the NRH budget. Information on patients referred to the NRH but who died in hospital was not available and thus mortality data were not able to be included in the analysis. The dataset was obtained in August 2011 in Honiara with the approval of the MHMS and the NRH. Travel costs were taken from NRH administrative information. The study was a retrospective study of routinely collected data.
Data were available for all of 2008, 6 months of 2009, all of 2010 and 1 month of 2011; a total of 31 months. All data available over the 31 month study period were included. The variables analysed for this study were largely complete. Of the 10 340 entries, the following information was missing: for province 27 (0.3%); for age 14 (0.1%); for sex 8 (0.1%); and for ward/department 565 (5.5%).
In addition, 10 qualitative interviews were conducted with staff at the NRH and MHMS as well as at one provincial hospital (Gizo Provincial Hospital, chosen due to its large size and remote location from Honiara). The interviews were semi-structured and were designed to elicit information from clinicians and policy-makers regarding inter-island referrals, the process for referral, decision-making, referral appropriateness and challenges faced. Quantitative data were analysed using Microsoft Excel. Qualitative data from interviews were grouped by interview question and analysed for key themes and illustrative quotations.
Ethics approval
Ethics approval for the qualitative interviews was obtained from the University of Sydney Human Research Ethics Committee (approval numbers 05-2009/11688 & 05-2009/11702).
Number of referrals
The NRH paid for the return of 3472 patients in 2008, 1889 over a 6 month period in 2009, 4645 in 2010 and 334 in January 2011. This amounted to 10 340 patients over the 31 months of data available; 330 referrals per month on average. In addition to the patients, the NRH paid for the one-way travel of a large number of accompanying family members. In 2008, 3199 accompaniers were funded, 1807 in 2009, 4088 in 2010 and 321 in 2011. Therefore, over the study period, the NRH paid for the return of 19 755 passengers to their home province.
The NRH policy states that 'one relative may accompany a patient who is less than 18 years of age or above 60 years of age' and approval for the relative's travel must be obtained from the referral provincial director prior to travel16. Despite this, over the study period 77.3% of referred patients aged 18-59 years had an accompanying relative funded for travel.
The return referrals per month are shown (Fig1), excluding accompanying family members. Referral patterns over 2008 were relatively flat while peaks can be seen in mid- and late 2010. November 2010 was the month with the highest number of returned referral patients (599).
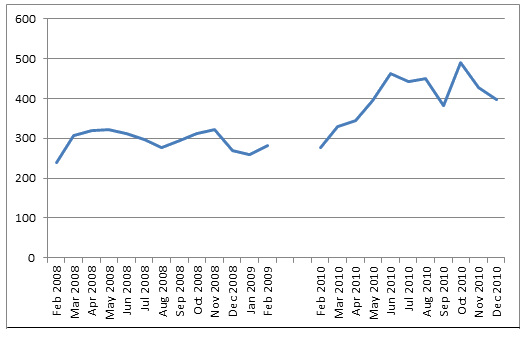
Figure 1: Patient referrals from the national referral hospital to home province by month.
Over the study period 3342 patients (32.4%) were returned to Malaita Province and 1916 to Western Province (18.6%; Table 1). Provinces with smaller populations such as Isabel, Choiseul and Temotu had fewer referrals in absolute terms.
Children under 10 years of age comprised 15.1% of all referrals over the study period despite representing 28.1% of the total Solomon Islands population (Table 2)17. Young adults aged 15-34 years comprised 29.7% of those referred. Just over 10% of respondents were classified as being 'adults' without a specified age. Of the patients under 10 years of age, 59.4% were male. Among young adults of 15-34 years, 63.8% were female while among older adults aged 50 years and older, the majority of referred patients were male.
The most common inpatient ward or outpatient clinic to which patients were referred over the study period was orthopaedics with 1238 (12.7%) of all referrals following by obstetrics and gynaecology (1109; 11.3%) and the medical outpatient clinic (1013; 10.4%; Table 3). Accident and emergency comprised 5.4% of referrals. A number of departments including the tuberculosis, dental and psychiatric departments all received fewer than 5% of referrals.
Examining referrals by department for each province demonstrated that 30% of all orthopaedic department referrals came from Malaita with an additional 18% from Western and 13% from Makira. Similarly, 31% of referrals to obstetrics and gynaecology were from Malaita, 19% from Western, 11% from Guadalcanal and 10% from Choiseul. From the perspective of each province, 19% of Choiseul's referrals were for obstetrics and gynaecology, the highest from any province. From Makira, 23% of referrals were to orthopaedics, as were 21% of Temotu's. Isabel referred more commonly for surgical reasons with 12% of referrals going to the surgical outpatient clinic and 10% to the surgical ward.
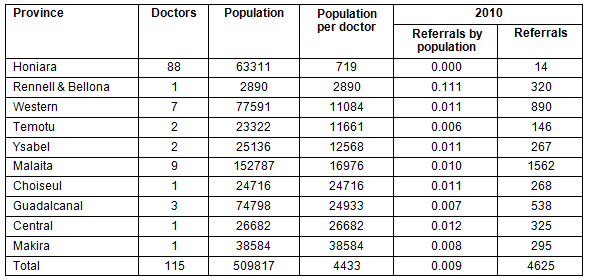
There was no consistent pattern at the provincial level between availability of doctors and rate of referrals. Provinces with the largest ratios of population size per doctor wre not those with the highest rates of referrals (Table 4). Makira, which has only one doctor serving its 38 584 people, had the third lowest rate of referral (0.008 referrals per person) of any province in 2010. Western province, with seven doctors for its 77 591 people (or one doctor per 11 084 people), had a higher referral rate of 0.011 referrals per person in 2010. Central, on the other hand, with only one doctor for 26 682 population (second highest population per doctor ratio), was the highest referring province after Rennell and Bellona.
Table 1: Patient referrals from the National
Referral Hospital by province, 2008-2011
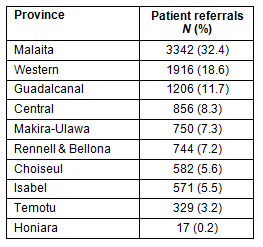
Table 2: Patient referrals from the National
Referral Hospital to home province by age and sex, 2008-2011
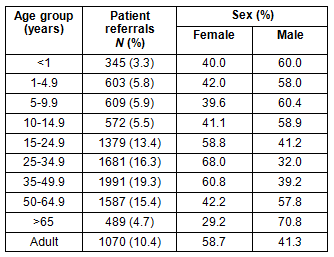
Table 3: Patient referrals by department (top ten only), 2008-2011
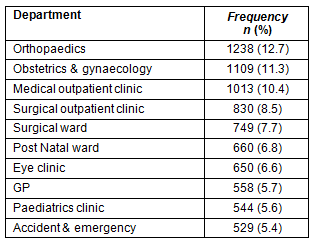
Table 4: Doctors by province and population, and 2010 referrals by population
Cost analysis
Patient transportation is most often undertaken by inter-island ferry. Outboard motorboat canoe, inter-island flights and military helicopter are additional options. The cost of transport for referred patients and accompanying family members from the location of referral to NRH is covered by the provincial health budget and the cost of transportation from NRH to home is paid for using the NRH budget.
The majority of individuals referred for medical care travel by boat to the capital city, Honiara, with only the most urgent referrals to the NRH being undertaken by plane or occasionally by military helicopter provisioned by the Australian-led Regional Assistance Mission to the Solomon Islands. The lowest cost one-way trip to or from Honiara for each province as of 2010 were used for estimates. For example, the lowest cost to travel from Central province to Honiara was Samoan (S)$150 (US$ 21) from the port of Tulagi. From remote Temotu, the cheapest boat trip was S$570 (US$80) from Lata with trips from Vanikoro costing S$720 (US$101). Trips from Western were calculated at S$380 (US$53) (price from Gizo) and from Malaita S$170 (US$24) (price from Auki).
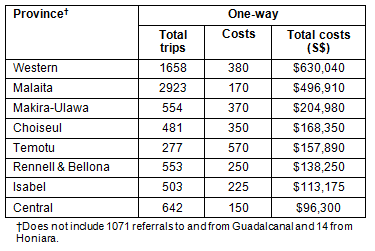
Using 2010 data only to derive annual costs, the total number of trips per province including patients and all accompaniers is presented (Table 5). Using the lowest one-way boat trip cost, total spend by province, in 2010, was at least S$630,040 (US$88,598) for Western and S$496,910 (US$69,877) for Malaita. These figures are likely to be significant underestimates. Each provincial health budget covers referrals to the NRH and the NRH covers the return trip. More than 46% of the total referral cost was spent on accompanying travellers. The analysis assumed zero mortality among patients referred to the NRH because information on in-hospital mortality was not available from the referral dataset. The analysis below is therefore likely an underestimate of true figures.
Table 5: Costs for referrals one-way by province, in Solomon Islands dollars, 2010
According to MOHMS figures, in 2010, the real cost of patient transport from the NRH back to provinces amounted to S$2,481,777 (US$348,994). In 2009, the cost of patient transport had been S$1,170,460 revealing that patient transport costs more than doubled in 2010 despite only a limited increase in the number of patients referred. In 2011, S$1,101,998 had been spent by end of June on patient referral travel. Patient transport accounted for 15.6% of the NRH annual budget in 2011.
The 2011 MOHMS budget only allocates S$630,000 to patient transport for all provincial hospitals ranging from S$100,000 for each of Kilufi and Atoifi Hospitals in Malaita to S$30,000 for Tulagi Hospital in Central. Given the data shown in Table 5, this is likely to be a gross under-allocation. Referral costs for Central in 2010 were estimated to be almost S$100,000 and almost S$500,000 for Malaita. The S$630,000 figure allocated for all provincial patient travel to NRH would cover only the costs borne by Western Province. This represents a considerable budget shortfall.
In addition to the costs described above, Regional Assistance Mission to Solomon Islands (RAMSI) has provided helicopter referrals for emergency cases over the past few years with no charge to the MHMS budget. The MHMS has now budgeted S$1.1 million (US$154,685) under the assumption that the free RAMSI trips might not be sustained for much longer. The S$1.1 million would cover emergency plane and helicopter charters as needed.
Findings from stakeholder interviews
Based on interviews with key stakeholders, a number of additional findings emerged about the referral system in the Solomon Islands. Clinicians and administrators working at the NRH mentioned a perceived high level of inappropriate referrals, although they conceded that no systematic study of the topic had been conducted. They suggested that a high percentage (one interviewee cited 50%) of referrals were inappropriate and that the individual should not have been sent to Honiara because either the care needed was not available at the NRH or was available at the outer island facility.
According to MHMS guidelines, patients should only be referred after consultation between the outer island facility individual in charge and the chief executive officer of the NRH; yet it was agreed by all interviewees that this procedure is not often followed. Additionally, there is a patient referral form to be signed by the referring health worker for the patient to carry to the NRH. The guidelines state that those who do not have the form are to be considered self-referrals and are not eligible to have transport costs covered, but again interviewees noted that this was rarely applied. One interviewee noted that many patients arrive saying they have lost their documents.
Additionally, a number of NRH staff and administrators noted that, despite the name of the hospital, not all patients seen at the NRH are referrals. Many residents of Honiara use the NRH as their primary care health facility, representing a potentially poor use of resources and scarce tertiary care physician expertise. Interviewees estimated that only 5% to 20% of those seen at the NRH were referred patients presenting for specialist care. Primary care complaints comprised 50-70% of all cases seen at the NRH. Due to this high level of self-referral and inappropriate referrals from outer islands, NRH resources are unnecessarily strained.
Discussion
In the Solomon Islands, referrals from outer islands to the NRH are substantial and are gradually increasing over time. The two most populous provinces outside the capital, Western and Malaita, represented 51% of all referrals over the study period. Of those referred, 21% were under 15 years of age (even though 40% of the country's population is under 15) with 30% being young adults of 15-24 years. Orthopaedic conditions comprised the largest number of referrals in this study, with obstetric and gynaecological conditions a close second. The cost of referrals is rapidly increasing and is now almost US$350,000 per year for the NRH alone. The amount budgeted for patient travel from the provinces to the NRH is a fraction of what is needed to cover the current number of referrals leading to a substantial budget shortfall.
The proportion of referrals by province generally mirrored the population for that province as might be expected. For example, 30% of referrals to the NRH's orthopaedic department were from Malaita which has 30% of Solomon Islands' population. Other provinces were over-represented: Rennell and Bellona had 320 referrals in 2010 for a population of 2890, equivalent to 11.1 referrals per 100 population. However, more work is required to elucidate reasons for trends in the different provinces' referral rates, given available human resources. There does not appear to be a clear link between number of doctors in each province and the rate of referrals.
The findings of other studies provide possible explanatory factors for the data found in this study. Research on referral practices in other settings highlights that the lack of user fees was seen to promote the overuse of hospitals8 which might impact referrals in the Solomon Islands as well. Other work on referrals has similarly highlighted the need for management incentives to improve the quality and appropriateness of referrals18. Another study from rural Niger conversely found a low willingness to refer patients as that is seen as a loss of power and prestige19.
Despite the lack of success in the Solomon Islands, a Cochrane review on interventions to improve referrals found that guidelines with structured referral sheets were generally effective3. The same review found that introducing fee-for-service models reduced referral rates.
The high rates of self-referral cited by interviewees were also seen in a Tanzanian study: of the 11 412 patients seen at Tanzania's national referral hospital, 72.5% were self-referrals20. Many referral systems are burdened by excessive self-referral where individuals by-pass appropriate levels of care to access higher level facilities21.
Data used for this study were taken from routine data collected in Honiara, thus the data are relatively complete except for missing data in 2009 which limits the completeness of the trend analysis. The use of an existing database ensured that data were collected without a bias toward study objectives. The exact destination port was not available for all respondents meaning that exact costs could not be calculated from the database. In these instances our research team estimated the lowest-cost estimates. Thus, overall results are conservative values. Further limitations include the lack of data on mortality among referred patients and the lack of in-depth data on condition and severity to help assess the appropriateness of the referral. Lastly, the lack of interviews with patients limits understanding of the patients' experience of the referral system.
In summary, this research highlights the need for greater policy attention to referrals from a number of different perspectives: equity of access, quality of care and cost. In general, referral of patients is costly and resource intensive and travelling when ill or injured is not the optimal situation for patients. The research makes clear the impact of human resource limitations in outer island facilities with Natuzzi and colleagues stating that the 'most common reason given for referring patients is the provincial doctor's lack of skills'14. There is a marked need for up-skilling of existing health staff, as well as more surgeons and doctors in peripheral facilities. The fact that more than 75% of the country's doctors work at the NRH means that provincial facilities will necessarily have to refer a large number of patients to the capital.
There is however a light at the end of the tunnel. The Government of the Solomon Islands has committed to increasing its human resources for health with 75 young Solomon Islanders being trained as doctors in Cuba as part of a bilateral agreement between the two countries22. Although there is still debate as to where these doctors will be posted, it is hoped that at least some will work in provincial facilities including the large new provincial hospital at Gizo in Western Province. The task-shifting literature has also highlighted that certain procedures can be performed by lower level cadres in order to address shortages in human resources23.
Beyond human resources, other efforts are needed to strengthen peripheral facilities in terms of infrastructure and supplies24. Spiegel and colleagues provide a useful template for assessing facilities' capacity to provide surgical care25, one key component that would reduce referrals. Over the longer term, strengthening information systems could allow some elements of the referral system to be conducted electronically thus simplifying communication and record-keeping and potentially reducing unnecessary referrals26. Furthermore, the referral guidelines themselves need review to ensure that they are practical and appropriate given the health system constraints in the Solomon Islands.
Future research could focus upon an evaluation of referral guidelines using clinical and psychosocial outcomes. It would also be useful to collect information from patients to explore their first-hand experiences of the referral system. Future research should also aim to monitor the effectiveness of any changes to the referral system. Changes to referral systems are likely to have very context-specific outcomes. An effective evaluation system for any interventions to improve referrals in the Solomon Islands is therefore required.
Improving the appropriateness of referrals can have a substantial impact on access, quality of care and costs. Improvements in equipment in remote facilities, in human resources for health and in information technology can strengthen the quality of care in outer islands. Reducing the burden on referral facilities will allow them to provide appropriate care to those most in need while building public trust in all layers of the health system.
Acknowledgements
Author JN was partly funded by an Australian National Health and Medical Research Council capacity building grant. Author AM was in-part funded by an unrestricted educational Fellowship from Merck Inc during the writing of this manuscript. Funding for travel to the Solomon Islands was received from Rotary International Sydney Cove and from the Nossal Institute for Global Health's Health Policy and Health Finance Knowledge Hub. The authors thank Alanna Fitzgerald-Husek for her contributions.
References
1. World Health Organization. The World Health Report 2008. Primary Care-Now More Than Ever. Geneva: WHO, 2008.
2. World Health Organization. The World Health Report 2006. Working Together for Health. Geneva: WHO, 2006.
3. Akbari A, Mayhew A, Al?Alawi MA, Grimshaw J, Winkens R, Glidewell E et al. Interventions to improve outpatient referrals from primary care to secondary care. Cochrane Database of Systematic Reviews 2008; iss4. art. no: CD005471.
4. Barnett ML, Keating NL, Christakis NA, O'Malley AJ, Landon BE. Reasons for choice of referral physician among primary care and specialist physicians. Journal of General Internal Medicine 2011; 27(5): 505-512.
5. Nakahara S, Saint S, Sann S, Ichikawa M, Kimura A, Eng L et al. Exploring referral systems for injured patients in low-income countries: a case study from Cambodia. Health Policy and Planning 2010; 25(4): 319-327.
6. Murray SF, Pearson SC. Maternity referral systems in developing countries: current knowledge and future research needs. Social Science & Medicine 2006; 62(9): 2205-2215.
7. Levine AC, Presser DZ, Rosborough S, Ghebreyesus TA, Davis MA. Understanding barriers to emergency care in low-income countries: view from the front line. Prehospital Disaster Medicine 2007; 22: 467-470.
8. Ohara K, Meléndez V, Uehara N, Ohi G. Study of a patient referral system in the Republic of Honduras. Health Policy and Planning 1998; 13(4): 433-345.
9. Sanders D, Kravitz J, Lewin S, McKee M. Zimbabwe's hospital referral system: does it work? Health Policy and Planning 1998; 13(4): 359-370.
10. United Nations Statistics Division. UN data Solomon Islands. (Online) no date. Available: http://data.un.org/CountryProfile.aspx?crName=Solomon%20Islands (accessed 13 December 2011).
11. World Health Organization. Spending on health: a global overview. Fact sheet 319. Geneva: WHO, 2007.
12. United Nations. UNDP Human Development Report 2011. Explanatory note on 2011 development indices Solomon Islands. (Online) 2011. Available: http://hdrstats.undp.org/images/explanations/SLB.pdf (Accessed 13 December 2011).
13. Asante A, Robert G, Hall J. A review of health leadership and management capacity in Solomon Islands. Sydney, NSW: Human Resources for Health Knowledge Hub, University of New South Wales, 2011.
14. Natuzzi ES, Kushner A, Jagilly R, Pickacha D, Agiomea K, Hou L et al. Surgical care in the Solomon Islands: a road map for universal surgical care delivery. World Journal of Surgery 2011; 35(6): 1183-1193.
15. Ministry of Health and Medical Services (Solomon Islands). General Referral Guidelines. Honiara: MHMS, 2005.
16. Ministry of Health and Medical Services (Solomon Islands). Guideline for Patient Referral to the NRH. Honiara: MHMS, 2007.
17. Population Division of the Department of Economic and Social Affairs of the United Nations Secretariat. World Population Prospects: the 2010 revision. (Online) 2011. Available: http://esa.un.org/unpd/wpp/index.htm (Accessed 27 January 2011).
18. Marinker M, Wilkin D, Metcalfe DH. Referral to hospital: can we do better? BMJ 1988; 297(6646): 461-464.
19. Bossyns P, Van Lerberghe W. The weakest link: competence and prestige as constraints to referral by isolated nurses in rural Niger. Human Resources for Health 2004; 2(1): 1.
20. Simba DO, Mbembati NA, Museru LM, Lema LE. Referral pattern of patients received at the national referral hospital: challenges in low income countries. East African Journal of Public Health 2008; 5(1): 6-9.
21. Negin J, Roberts G, Lingam D. The evolution of primary heath care in Fiji: past, present and future. Pacific Health Dialogue 2010; 16(2): 13-23.
22. Asante AD, Negin J, Hall J, Dewdney J, Zwi AB. Cuban health assistance program and human resources for health challenges in the Pacific: analysis of policy implications. Human Resources for Health 2012; 10(1): 10.
23. Gessessew A, Barnabas GA, Prata N, Weidert K. Task shifting and sharing in Tigray, Ethiopia, to achieve comprehensive emergency obstetric care. International Journal of Gynaecology and Obstetrics 2011; 113(1): 28-31.
24. Westcott M, Martiniuk ALC, Fowler RA, Adhikari NKJ, Dalipanda T. Critical care resources in the Solomon Islands: a cross-sectional survey. BMC International Health and Human Rights 2012; 12: 1.
25. Spiegel DA, Choo S, Cherian M, Orgoi S, Kehere B, Price RR et al. quantifying surgical and anesthetic availability at primary health facilities in Mongolia. World Journal of Surgery 2011; 35: 272-279.
26. Martiniuk A, Negin J, Hersch F, Dalipanda T, Jagilli R, Houasia P et al. Telemedicine in the Solomon Islands: 2006 to 2009. Journal of Telemedicine and Telecare 2011; 17(5): 251-256.




