More than half a million women worldwide die annually from the complications of pregnancy and childbirth and approximately 20 million women suffer maternal morbidity. Approximately 4 million newborns die in their first month of life and approximately 9 million children die before their fifth birthday; an additional 4 million babies are stillborn. Most of these deaths among women and children occur in the world's poorest countries and malnutrition is a contributing factor1,2. These figures are a sign of the gap between developing and developed countries but there are also differences between urban and rural inhabitants within countries such as India3.
Improving maternal and child health are two of the Millennium Development Goals (MDG) of the World Health Organization (WHO). The goal specified in MDG 5 is to reduce the maternal mortality ratio by 75% between 1990 and 2015. This goal can be reached by improving healthcare interventions such as antenatal care (ANC) involving check-ups both during and after pregnancy, providing skilled care during delivery, family planning and safe abortion. Providing excellent ANC is critical, especially in the rural areas of developing countries, as many women face several risk factors such as nutritional deficiencies and anemia. The goal specified in MDG 4 is to reduce the under-five mortality rate among children by two-thirds. Strategies for reducing mortality during the first month of life and reducing malnourishment are considered to be the most effective ways to reach this goal4. To reach the goals of MDG 4 and 5 by 2015, greater efforts will be required with ANC and child health care (CHC)5.
Despite its economic development, India is one of the countries most burdened by maternal, newborn, and child deaths worldwide6. Since 2005, there has been a growing interest in giving political priority to safe motherhood7 and the Indian government is currently committed to reducing infant and maternal mortality rates8. However, India is one of the countries where progress towards meeting MDG 4 and 5 has been insufficient6.
This study is based on a collaboration between Pravara Medical Trust (PMT), Maharastra in India, Linköping University and Östergötland County Council in Sweden, to develop ANC and CHC in a remote rural area in India. The major objective was to improve maternal and child health by applying a nurse-based ANC and CHC program based on relevant parts of the Swedish model. The goals of the Swedish model are close to those specified in the policy of the WHO: to promote health, to find and correct adverse conditions, and to support parents in their transition to parenthood9,10. Participation is voluntary and free of charge and the nurse-based clinics are able to offer good availability and continuity.
The aim was to describe how families participate in the nurse-based ANC and CHC and the effect of this on referrals to specialist care, institutional deliveries and mortality figures. Furthermore, the staff's experiences of the healthcare model are described.
Setting
The project area includes approximately 450 000 inhabitants living in 235 underserved remote villages in the Ahmednagar district, Maharastra, India. In 125 of these so called tribal villages located in the mountains there are extremely sparse health services. The number of health workers in the project area was approximately 1 per 730 for the general population and approximately 1 worker per 460 for pregnant women and children.
Baseline survey
A baseline survey was performed in 2005 before the intervention and these data are until now unpublished. The data were collected by medical students in 150 randomly selected villages in the project area, according to a structured protocol. The results showed that approximately 55% of the families were living below the poverty level (<1000 Rupees/month). Approximately 90% of the families did not have access to latrines. The sex ratio was 945 female per 1000 male among newborns, indicating that selective abortion was being practiced. The prevalence of anemia in women during pregnancy was 65%. Only 51% of the women received antenatal care that included three check-ups. Almost 75% of deliveries took place at home. Maternal mortality was reported to be 478 per 100 000 live births, based on reports from 1250 randomly selected delivering women with an infant mortality 80 per 1000 live births. More than half of the children under 5 years of age were malnourished (78% of girls and 52% of boys). The rate of full immunization was 43%. Eigthy percent of girls and 40% of boys dropped out of school. Indian law permits marriage from the age of 18 in women and 21 years of age in men, yet in this area 61% of the women and 40% of the men married when they were younger, with girls' mean age at marriage being 16.1 (standard deviation 2.0) years in 2005. There were big differences within the project area with the worst conditions found in the tribal villages.
The healthcare system within the project area consisted of 29 governmental primary health centers, four governmental hospitals, one missionary hospital and one university hospital, Pravara Rural Hospital (PRH). The missionary hospital left the project in 2009.
Procedure
Intervention: The Indian program8 and applicable parts of the Swedish ANC and CHC nurse-based systems were considered when establishing the schedules for ANC and CHC. The ANC program was also strongly influenced by the recommendations of WHO11.
Antenatal care The goal was that women should present for their first ANC check-up before pregnancy week 16. Those with a normal pregnancy should have at least three check-ups and a postnatal visit. Women who were identified as high risk cases should have a minimum of 5 check-ups, be referred to a specialist in obstetric care and have a postnatal visit. At the first visit a nurse made a risk classification, using a classifying form based on WHO recommendations11. Women could also be identified as having a high risk pregnancy at a later stage.
Child health care The schedule for check-ups was inspired by the Swedish child health program and adjusted to the timetable for immunizations in India, as this might be of significant importance for influencing parents' preparedness for going to the clinic. The most important period for supervising the children was considered to be the period between birth and the age of 3 years with a higher frequency of check-ups in early life. For children from the age of 3 years there is the governmental system with anganwadi which provides a government sponsored child-care center for all children in the villages where growth, malnourishment and development are supervised. The clinic also provides food, vitamins and immunizations for children.
The focus was on the growth and development of the child. Growth was judged from weight and height continuously, head circumference from birth to 18 months and mid-arm circumference from the age of 12 months. The figures were plotted in diagrams so deviations were obvious. The child's development related to age, and specified tests were described. Breastfeeding, weaning, nutrition and prevention of accidents were compulsory subjects in the dialogues between parents and nurses. Much effort was also invested in the importance of parents having confidence in the nurses and creating a positive and friendly atmosphere during their meetings
Education program Approximately 385 Indian personnel worked actively in the project; approximately 150 nurses, mainly auxiliary nurses, medical officers (most of them practicing ayurweda but some with western medical education) and field workers such as social workers. Women (n=235) who were respected in the villages and able to read and write were recruited as local key persons or Female Health Volunteers (FHV). Their task was to motivate and educate the women and stress the importance of health check-ups and attending to issues such as nutrition, the need for rest and the prevention of accidental events. The FHV received small salaries.
The education of the co-workers was a collaborative effort of the Indian and Swedish teams. The Swedish team members educated experienced Indian nurses and medical officers. They then educated the Indian staff. A model called Training of Trainers (ToT) was established. Two tutorial groups with a total of 12 nurses and medical officers were formed and the training was inspired by Problem Based Learning (PBL)12. They worked as nurses and medical officers but they were also expected to educate and support the staff in the project as trainers. The aim of the education program was to increase theoretical knowledge, medical examining skills, and to promote patient-centered care and the friendly and attentive treatment of women and children. There was extensive teaching, training and monitoring of all nurses' and medical officers' performance, both in campus sessions and at the clinics.
The FHVs, Traditional Birth attendants (TBA; n=384) and traditional healers (n=126) were engaged in the project and taught by the Indian team working with campus-based education, including training and workshops. The TBAs also had training sessions at the delivery ward at PRH.
Establishing clinics Nine Primary Health Centers (PHC), and five mobile clinics were established in the project area. The mobile clinics visited remote villages once a month following a pre-arranged schedule providing ANC and CHC, and attending to others who were sick.
Health records and manuals for ANC and CHC were produced in a collaboration of the Indian and Swedish team. Flow charts were developed to provide reminders about what was required, step-by-step, at each visit in ANC and CHC.
The PHC and mobile clinics were equipped with easily handled instruments to make it possible for the nurses to make correct measurements. They also had toys that could distract children and be used in tests checking attentiveness and physical and mental development. Laboratory equipment for water testing, blood and urine analyses, sphygmomanometers, disinfectants and examination bunks were obtained.
Informational and educational materials were produced, including leaflets/handouts, flexi charts/billboards and wall calendars. Films/video documentaries were produced on various subjects (eg female feticide, water purification, HIV/AIDS, adolescent health). To promote hygienic home deliveries, special kits including paper sheets, gloves and a clean knife, were developed and produced. These kits were first given to the TBAs but subsequently also to the pregnant women to make them more independent.
Study design
A longitudinal, prospective study was conducted between 2006 and 2009, using quantitative and qualitative data.
Data collection and statistical analyses
Protocols were completed during the examinations of women and children. Pre-selected information from these protocols was entered at the computer centre at PMT, Loni. Descriptive statistics were used. Mortality figures for changes over time were compared using the χ2 test.
Qualitative data were assessed from a focus group discussion13,14. The dialogue was transcribed by one of the authors. The transcription was analyzed according to Kreuger14 by two of the authors. The transcription was read several times to obtain a deeper understanding of the interview. All text connecting to the study aims was selected and sorted into sub-categories and categories.
Ethical considerations
The study was financed and approved by the Swedish International Development Cooperation Agency and ethical aspects were considered in the application and approval (PIMS/CSM/RC/2006/1). The Research Committee of Pravara Medical Sciences approved the comparative study of the efficacy of healthcare services.
Family participation in antenatal care and child health care
The number of women and parents presenting with their children for check-ups increased year by year. More families in remote districts where the mobile clinics visited attended the service than those in the districts where there were other healthcare options.
Antenatal care and deliveries: In 2006, there were approximately 7100 deliveries in the area, the majority being unassisted deliveries at home. The total number of pregnant women in the project area was approximately 9000 per year. The amount of first check-ups before 16 weeks increased from 38% in 2006 to 63% in 2009. The corresponding figures for at least one check-up were 50 and 83%, respectively, and for at least three check-ups 30 and 60%, respectively. An increasing number of women were referred for further antenatal check-up or to PRH for delivery. Approximately 25% of women were referred in 2006 and 52% in 2009 of an estimated target population of approximately 7000. Thirty-eight percent of the referrals were acute cases. Pre-eclampsia was one common complication detected in 11% of pregnant women in 2009. Severe anaemia (haemoglobin < 7 g/dL) was found in 8% of the women.
The percentage of institutional deliveries increased considerably from 40% to 74% between 2006 and 2009. One example is that the number of deliveries at PRH doubled and instrumental deliveries and caesarean sections increased by 13%. Institutional delivery was defined as delivery in PHCs, in governmental rural hospitals, in private institutions or at PRH. The attendance of trained TBAs at home deliveries increased from 20 to 90% over the study period.
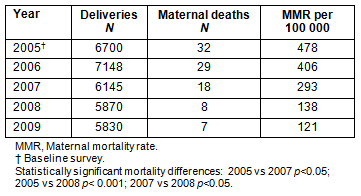
Maternal mortality decreased: The mortality figures showed a pronounced reduction from a baseline value of 32 in 2005 (calculated value) to 18 in 2007 and 8 in 2008. The decreases were statistically significant (Table 1). Figures for 2005 show a much higher mortality rate in tribal areas (650/100 000 women) but these figures were based on few cases.
As most of the mothers delivered outside the PRH, the causes of maternal deaths recorded were arbitrary. The most probable, major causes of death were post-partum haemorrhage, infections and pre-clampsia/eclampsia.
Table 1: Maternal mortality per year, absolute values and per 100 000 deliveries
Child health care: Children were grouped according to age (newborn-2 years and 3-5 years). There was a considerable increase in CHC attendance with higher attendance figures in the younger than the older group (Table 2).
Besides health check-ups, reasons for seeking advice or help were respiratory infections 39%, diarrhoea 24%, skin diseases 15%, accidents and injuries 7%, and other 15%. The total number of referrals from CHC to PRH increased by 55% from 2006 to 2009. Approximately 20% of children below the age of 1 year were referred to PRH in 2009 (58% were boys). The most frequent reasons for referral were respiratory infections, congenital anomalies and malnutrition. Almost one-third of all patients suffered from some degree of malnutrition, and 2% had grades 3 or 4 malnutrition according to the grade definition of Ghai15.
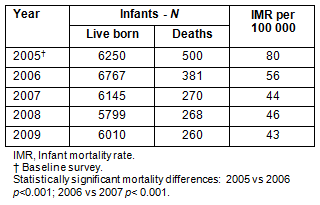
Infant (ie children below the age of 1 year) mortality decreased. There was a pronounced reduction in mortality from the baseline survey of 80 per 1000 live births to 56 in 2006 and 44 in 2007, and these were statistically significant (Table 3). There were marked differences among the three major districts in the project area, with the highest mortality rate in the poorest districts. It was not possible to identify the causes of infant deaths.
Table 2: Total number of children examined in the project, according to age
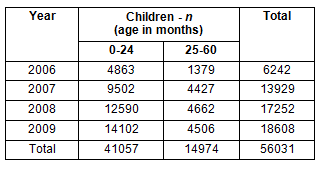
Table 3: Total number of infant deaths and infant mortality rate per 1000 live births
Staff's experience of participation in the new healthcare model
Three major categories were derived from the content of the focus group discussions, all focusing on aspects of the effect of establishing nurse-based ANC and CHC in a rural and remote area.
Influence on people's thoughts and actions: The nurses and medical officers stressed that in the process of the implementation of ANC and CHC they commonly encountered attitudes such as 'preventive health has low value and is just a waste of time and money'. However, during the intervention as there was an increasing interest in ANC and CHC and the number of patients attending the PHC and MC increased, there was an enlarged awareness of the benefits of preventive health care and confidence in nurse-based care.
'Blind-faith beliefs' was identified as an important issue affecting how people valued health. One example was the belief that a pregnant woman should eat as little as possible in order to give birth to a small baby and have fewer labour complications. Substantial efforts were made to improve women's and children's nutritional status; these efforts entailed educating women, farmers and the leaders in the villages about the crops that would provide the nutrition needed. Another aspect was the production of a nutritional support in the form of a powder developed during the intervention.
The necessity of paying attention to the tradition of joint families and the authority of the mother-in-law was stressed. The pregnant woman's situation concerning aspects such as her nutritional needs, working situation and her ability to attend ANC and a delivery ward, depended on the opinions and decisions made by her mother-in-law and the woman's husband. Therefore, the group stressed the significance of selling the message of the importance of health care during pregnancy to elderly women and patients' husbands. Since the mother-in-law often takes care of the small children while the parents are working, it is essential that she has knowledge about issues such as nutrition for children, including girls, the prevention of accidents and the importance of asking for care when there are health problems.
Intra- and inter-professional work: One of the challenges in establishing nurse-based ANC and CHC was the limited skills among available nurses and medical officers. Another problem was the turn-over of staff because working in a remote area was considered unattractive. In the discussion it was stressed that nurses educated in the program were likely to be attractive for recruitment by other health providers.
Several changes were mentioned regarding development of skills in the nurses and medical officers. These included new ways of meeting patients and making them feel welcome and more relaxed, new skills in examining women and children, improved counseling and a new ability to identify at-risk cases. This resulted in an increased confidence in their responsibilities even though they experienced the work as demanding.
Staff felt that they had come to know others in the team which facilitated learning from each other in their daily work, and striving for the same goals. The medical officers said that collaboration with the nurses decreased their work stress. The nurses highlighted the development of a supportive dialogue between members of staff.
Influence on collaboration between health care and society: There was a change in the way staff related health problems and the life situation of the patient. One medical officer felt the way he viewed himself as a doctor had changed, and that being a doctor also included being a social worker. A nurse pointed out that there was a feeling of increased responsibility for the whole of society.
The need for collaboration with other health actors was identified as important. A governmental organization was responsible for immunizations and therefore it was not possible to include this aspect of health in the project. However, the schedules for the mobile clinics and the governmental nurses were coordinated where possible so parents could have immunizations and health check-ups at the same time.
Schools and other institutions requested educational material produced in the project, such as information about nutrition, HIV and sexuality. This was interpreted by the group as indicating an increased awareness and value of preventive health care.
Discussion
The focus of this study is the result of the development of a nurse-based ANC and CHC in an economically disadvantaged and remote rural area in India where an estimated 55% of the families lived below the poverty line. The results suggest that it is possible to increase the awareness of the benefits of participation in health care in such a population and that it is possible to develop nurse-based health services with mostly local staff. In order to meet MDG 4 and 5, it is crucial to reach people in rural areas with ANC and CHC. However, the discrepancy between urban and rural areas is daunting. The Millennium Developments Goals Report5 stresses that ANC is important in reducing maternal mortality in rural areas. Key efforts identified for India6,16 are in line with the reported intervention, that is, encouraging institutional deliveries and training auxillary nurses to increase their competence.
The focus for CHC was on children from birth to the age of 3 years. It is reported that children under 5 years are at greater risk of dying in rural areas, even in regions with decreasing child mortality5. It is therefore essential that the development of nutrition policies and programs is focused on young children6.
The increased attendance of pregnant women for ANC and the availability of competent nurses were important factors in the increased number of referrals and institutional deliveries. High risk cases, such as pre-eclampsia and severe anemia, were identified and treated, which was probably the major reason for the reductions in maternal and infant mortality17.
Maternal mortality is still high in the project area but it is lower than the most recent average figures for India of 230 deaths per 100 000 live births3. India falls behind several other Asian countries in decreasing maternal mortality6. The changes were most pronounced in the tribal areas, that is the poorest areas with previously little access to medical care. The total numbers are low, however, so only limited conclusions can be drawn.
A relatively rapid initial decline in infant mortality was also seen. Infant mortality is still high but lower than the average for India of 53 deaths per 1000 live births6. Contributing factors to infant mortality are very low average birth weight, infections and malnutrition with related complications. During the intervention it was possible to identify and refer cases for treatment of, for example, infection; however, there were limited resources to prevent malnutrition in this disadvantaged, isolated population.
A strength of the intervention was the focus on the youngest children (newborn-3 years of age), for studies have shown that the first 2 years of life are the most important for future development and health6,18. However, the Indian organization with anganwadi, supporting children with immunizations, nutrition and education, commences when the child is 3 years.
The implementation was based on the principle of educating tutors who then trained nurses and medical officers working in the field with patients. The successively increasing attendance rate can probably be seen as an acceptance of the nurse-based system and also an increasing understanding of the importance of preventive health care. It was easier to introduce maternal health care than CHC. The reason for this may be that it is easier for families to understand the importance of check-ups during the limited time of pregnancy than throughout the longer period of childhood. The FHVs were crucial for motivating women to use the health service for themselves and their children. Several projects have revealed the importance of having a well-known person living among the families and taking part in daily life19,20.
The process of Swedish and Indian contributors cooperating on the design of the project was fruitful and rewarding. The Swedish partners contributed with experience from nurse-based ANC and CHC and the Indian partners knew the culture and which parts of Swedish health care could be considered relevant in this context. Nurse-based health care has been shown to be feasible and effective21.
At the beginning, project nurses were trained to work in both ANC and CHC. However, this was too demanding and it was decided that a focus on one area was enough for each nurse. The mobile clinics were small to begin with, and as patient numbers increased they were too small for both ANC and CHC. It also became necessary to run ANC and CHC in parallel to make it possible to accommodate all those who presented for check-ups. Therefore, more space was required. Generally it was found practical to use a school room or open place for CHC, and to consult with pregnant women in the mobile clinics. This arrangement contributed to higher quality care and greater efficiency.
Knowledge about the learning process improved among the trainers and influenced the staff training. The trainers came to feel more confident in teaching and monitoring clinical work. They developed new ways of evaluating the learning process and used other forms of education than lectures. At the end of the project it became obvious that nurses educated in the project were likely to be recruited by other health providers. While this indicates the quality of the education provided in the project and offered a way to spread the project work, it also increased costs because new nurses had to be recruited and educated for the project.
Also identified in the focus discussions as a result of the education provided was the development of a new patient-centered communication with patients and parents. Listening, having a dialogue and a presenting a less authoritarian image was advocated and emphasized by the trainers.
Because the aim of the collaboration was to develop nurse-based health care, it was important to have competent nurses and a functional team working in the field. Therefore, the limited skills of the available nurses (auxiliary nurse) and ayurweda-educated medical officers were a challenge. The high turn-over of staff related to the unattractiveness of working in remote areas was another problem. The strategy developed was to focus on staff already living in the remote area with education and training, which is in concordance with WHO guidelines16.
Promoting maternal and children health is a challenge worldwide, especially in rural and remotes areas, and efforts to develop ANC and CHC are stressed as being crucial5,6. This intervention of nurse-based ANC and CHC could contribute to the progress towards practical and effective health care as women and children are shown to be essential groups for influencing future public health5.
Limitations
Many lessons were learned during this intervention. One limitation was that the full scale intervention commenced without a pilot study. A smaller pilot study in one or a few villages would have made the full scale implementation easier, as well as the evaluation. Another limitation was the lack of a control group, which could not be recruited for practical reasons. However, the baseline survey was a strategy to solve this problem.
However, other factors might have contributed to the results. Mortality figures for 2005, both for mothers and infants, were calculated from the baseline survey and are probably less reliable than data from the project area. It is therefore of importance to note a continued decline during the project time.
The study results suggest it is possible in an economically disadvantaged, rural area to increase people's interest in and awareness of the value of preventive health care for pregnant women and children, and to promote the benefits of participation.
The results also suggest that it is possible to decrease maternal and infant mortality within 3 years by introducing nurse-based health care in a rural and remote area with limited resources.
It is also possible to influence the care encounter. The training of trainers was a successful way to implement new strategies, competence and attitudes in a large group of health workers and thus bridge cultural differences in an international collaboration.
Acknowledgements
The authors thank the Pravara Medical Trust, India, Swedish International Development Cooperation Agency, Sweden, Linköping University and County Council in Östergötland, Sweden for financing the project. Associate Professor Leif Mathiesen contributed in the ANC program, and Dr Prasanna Dhore was responsible for follow up of the ANC and CHC program.
References
1. World Health Organization. Women and health, today's evidence tomorrow's agenda. (Online) 2009. Available: http://whqlibdoc.who.int/publications/2009/9789241563857_eng.pdf (Accessed 28 March 2012).
2. World Health Organization. Children reducing mortality. Fact sheet No178. (Online) 2012. Available http://www.who.int/mediacentre/factsheets/fs178/en (Accessed 28 March 2012).
3. World Health Organization. World Health Statistics 2011. (Online) 2011. Available http://www.who.int/whosis/whostat/EN_WHS2011_Full.pdf (Accessed 2 February 2012).
4. United Nations. What will it take to achieve the Millennium Development Goals? (Online) 2010. Available: http://content.undp.org/go/cms-service/stream/asset/?asset_id=2620072 (Accessed 2 February 2012).
5. United Nations. The millennium Development Goals Report 2011. (Online) 2011. Available http://www.un.org/millenniumgoals/11_MDG%20Report_EN.pdf (Accessed 31 January 2012).
6. Paul VK, Sachdev HS, Mavalankar D, Ramachandran P, Sankar M J, Bhandari N et al. India: Towards Universal Health Coverage 2. Reproductive health, and child health and nutrition in India: meeting the challenge. Lancet 2011; 377: 332-349.
7. Shiffman J, Ved RR. The state of political priority for safe motherhood in India. British Journal of Obstetrics and Gynaecology 2007; 114: 785-790.
8. Government of India. Reproductive and Child health - Phase 2. (Online) no date. Available http://www.mohfw.nic.in/NRHM/RCH/Index.htm (Accessed: 2 February 2012).
9. Chalmers B, Mangiaterra V, Porter R. WHO principles of perinatal care: the essential antenatal, perinatal, and postpartum care course. Birth 2001; 28: 202-207.
10. Bhutta ZA, Ali S, Cousens S, Ali TM, Haider BA, Rizvi A et al. Rebirth and revision 6. Interventions to address maternal, newborn, and child survival: what difference can integrated primary healthcare strategies make? Lancet 2008; 372: 972-989.
11. WHO. Antenatal care randomized trial: Manual for the implementation of the new model. (Online) 2002. Available: http://whqlibdoc.who.int/hq/2001/WHO_RHR_01.30.pdf (Accessed 20 March 2010).
12. Marton F, Booth S. Learning and awareness. Mahwah, NJ: Erlbaum Associates, 1997.
13. Krueger RA, Casey MA. Focus groups. A practical guide for applied research, 4th edn. Thousand Oaks, CA: Sage, 2009.
14. Krueger RA. Analyzing & reporting focus groups results. In: Focus group kit, vol. 6. Thousand Oaks, CA: Sage, 1998.
15. Ghai OP, Gupta P, Paul VK. Ghai essentil pediatrics, 6th edn. Dehli: CBS, 2004.
16. World Health Organization. Increasing access to health workers in remote and rural areas through improved retention. (Online) 2010. Available: http://whqlibdoc.who.int/publications/2010/9789241564014_eng.pdf (Accessed 2 February 2012).
17. Kim SY, Rochat R, Rajaratnam A, Digirolamo A. Evaluating completeness of maternal mortality in rural health and social affairs unit in Vellore, India 2004. Journal of Biosocial Science 2009; 41: 195-205.
18. Victora CG, Adair L, Fall C, Hallal PC, Martorell R, Richter L et al. Maternal and child undernutrition study group. Maternal and child undernutrition: consequences for adult health and human capital. Lancet 2008; 371: 340-357. Erratum in 372: 302.
19. Bhim P, Shrestha BP, Bhandari B, Dharma SM, Osrin D, Costello A et al. Community interventions to reduce child mortality in Dhanusha, Nepal: study protocol for a cluster randomized controlled trial. Trials 2011; 12: 136.
20. Turan JM, Tesfagiorghis M, Polan ML. Evaluation of a community intervention for promotion of safe motherhood in Eritrea. Journal of Midwifery Women's Health 2011; 56: 8-17.
21. Van Griensven J, De Naeyer L, Uwera J, Asiimwe A, Gazille C, Reid T. Success with antiretroviral treatment for children in Kigali, Rwanda: Experience with health center/nurse-based care. BMC Pediatrics 2008; 8: 39.







