Parkinson's disease (PD) is a debilitating neurological condition that occurs in more than three in 1000 people living in Australia1. In the United Kingdom and the USA, the estimated prevalence of PD ranges from 125 to 550 in 100 000 individuals2,3. The motor and non-motor symptoms associated with PD can result in the individual experiencing substantial activity limitations and participation restrictions4,5. This may compromise their health-related quality of life (HRQOL), which is concerned with the impact of health, disease and treatment on physical function, social and emotional wellbeing, and cognition6. As the population in Australia increases and ages, it is predicted that more individuals will be diagnosed with PD in the coming decades1,7. This is likely to place an increased economic and social burden on society as these individuals may have other conditions or diseases that further impair their HRQOL.
Growing evidence suggests that idiopathic PD is more prevalent in rural areas7-9, with several studies reporting a higher prevalence in rural communities compared to metropolitan areas7. Population-based studies in Taiwan have also reported idiopathic PD to be more common in rural areas8. The association between rural living and increased risk of PD may be attributed to the increased likelihood of exposure to agricultural agents - such as pesticides, solvents and metals - in rural areas10. Despite idiopathic PD being more common in rural areas, there is little information about the HRQOL of individuals with PD living in rural communities. A recent systematic review found only one study had examined the relationship between rural living and HRQOL11, with a rural life setting identified as an independent negative predictor of HRQOL12. Individuals with PD living in rural communities in Croatia were more likely to experience poor HRQOL in comparison to their urban counterparts12. Negative associations between rural living and HRQOL may be related to inadequate access to healthcare services and a limited number of PD specialists10,12,13. Individuals in rural areas may also have to travel longer distances to access primary or specialist care services, which can further contribute to poor HRQOL13.
This study aims to describe and quantify the different dimensions of HRQOL in an Australian sample of people with PD living in rural Victoria. Differences in the HRQOL of Australians with PD living in metropolitan Melbourne and rural Victoria will also be examined, including the contribution of rural living towards the variance in HRQOL.
Participants
The metropolitan sample consisted of individuals with idiopathic PD who were recruited as part of a rehabilitation trial that sampled from outpatient movement disorder clinics, PD support groups and community rehabilitation programs in Melbourne14. A separate sample of people with PD was also recruited from rural Victoria. Participants were classified as living in a rural area according to the Australian Standard Geographical Classification - Remoteness Areas system, where the defining difference between 'city' and 'country' is physical remoteness from goods and services15. This classification system divides Australia into five broad geographical categories (major city, inner regional, outer regional, remote and very remote), which are defined according to the road distance to the nearest urban centre based on population size15. In order to ensure adequate representation of the population of individuals with PD living in rural communities, participants were recruited from a variety of sources. This included people with PD attending community-based rehabilitation programs and support groups in Ballarat, Benalla and Shepparton. These areas are classified as inner regional areas in Victoria according to the Australian Standard Geographical Classification - Remoteness Areas system15.
Inclusion criteria were informed consent and a diagnosis of idiopathic PD confirmed by a neurologist. Participants were excluded if they scored less than 24 (age-adjusted) on the Mini-Mental State Examination (MMSE)16. Individuals living in metropolitan Melbourne were also excluded if they were unable to walk and/or safely participate in therapy as advised by their medical practitioner. This included individuals with a disease severity of Stage 5 according to the modified Hoehn and Yahr (HY) scale because they could not complete the treatment protocol17. This exclusion criterion was not applied to the rural sample, as participants were not required to participate in a physiotherapy intervention program.
Measures
Structured interviews by trained assessors were conducted to obtain information on demographic characteristics such as age, sex and PD duration. Cognitive function was assessed using the MMSE16 while disease severity was assessed using the modified HY scale17. The Parkinson's Disease Questionnaire-39 (PDQ-39) was used to quantify HRQOL because it is a highly reliable and well-validated disease-specific measure of health status18. It correlates strongly with clinical measures of PD such as the modified HY scale19,20 and there is evidence supporting its content, construct and discriminative validity20,21. The PDQ-39 comprises 39 items in eight different dimensions: mobility (10 items), activities of daily living (ADL) (six items), emotional wellbeing (six items), stigma (four items), social support (three items), cognition (four items), communication (three items) and bodily discomfort (three items). It addresses issues that are important to people with PD such as feeling worried about the future; experiencing painful muscle cramps and having difficulties getting around in public; cutting up food; and communicating with other people18. All items are scored from 0 (never) to 4 (always). Summary indices can be calculated for each dimension as well as the total scale to describe the impact of PD on physical, emotional and social functioning. Higher scores indicate poorer perceived health status18.
Statistical analysis
Descriptive statistics were used to summarise the demographic data and scores derived from the PDQ-39 for participants living in metropolitan Melbourne and rural Victoria. Differences in demographic characteristics and HRQOL ratings between the metropolitan and rural samples were explored using the Mann-Whitney U-test of significant due to skewed distribution of the data. Two models of multivariate regression were examined to determine whether rural living contributes to HRQOL in people with PD. The first model included rural living as the only predictor variable (HRQOL=f[rural living]). The determinants examined in the second model were rural living, age, sex, disease duration, employment status, living situation and disease severity (HRQOL=f[rural living, age, male, disease duration, unemployed, lives with others, moderate disease severity]). Age and disease duration were treated as continuous variables while sex, living situation, employment status and rural living were coded into categorical variables. Disease severity was also classified as mild (Stages ≤2) and moderate severity (Stages ≥2.5) given the ordinal nature of the modified HY scale22. Statistical interaction between the independent variables was assessed by including the product of these variables in the model. Interactions were examined between rural living and disease severity as measured by the modified HY scale and rural living and disease duration. An initial evaluation of the assumptions of the regression analysis led to a powered transformation of the PDQ-39 summary index (SI) score. A square-root transformation was used to reduce skewness and the number of outliers, as well as to improve the normality and linearity of residuals. All analyses were conducted using Statistical Package for Social Sciences v17 (SPSS Inc, www.spss.com).
Ethics approval
Ethics approval for this study was obtained from The University of Melbourne (HREC 0931917.1).
The characteristics of the participants with idiopathic PD living in metropolitan Melbourne and rural Victoria are presented (Table 1). In order to ensure that the characteristics of individuals living in rural Victoria were comparable to the metropolitan sample, one individual with a modified HY Stage 5 was excluded from the analysis. Two rural participants were also excluded because they scored less than 24 on the MMSE. There were no significant differences in age, sex, employment status, living situation and disease severity between participants in the rural and metropolitan samples. Nevertheless, participants with PD in rural areas had a significantly longer mean disease duration compared to participants living in metropolitan Melbourne.
Table 1: Participant characteristics from metropolitan Melbourne and rural Victoria
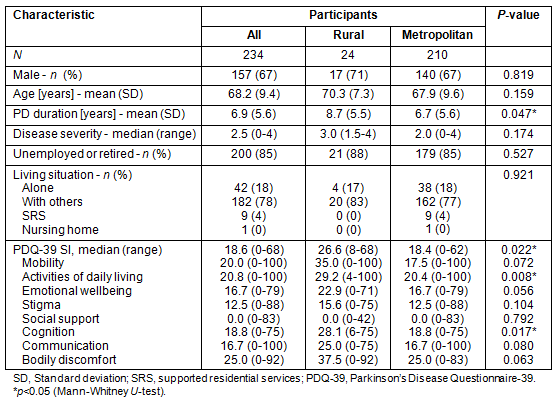
The median PDQ-39 SI score for participants living in rural Victoria was 26.6 (range 8-68) compared to a median of 18.4 (range 0-62) for people living in metropolitan areas. The ratings for the different dimensions are shown (Table 1). Participants in both rural Victoria and metropolitan Melbourne had the most difficulties with the dimensions related to:
- bodily discomfort (rural median 37.5; metropolitan median 25.0)
- mobility (rural median 35.0; metropolitan median 17.5)
- ADL (rural median 29.2; metropolitan median 20.4)
- cognition (rural median 28.1; metropolitan median 18.8)
- communication (rural median 25.0; metropolitan median 16.7)
- emotional wellbeing (rural median 22.9; metropolitan median 16.7)
- stigma (rural median 15.6; metropolitan median 12.5).
Both groups reported less impairment in the dimension of social support. Given that participants in the rural sample had significantly longer PD duration, a one-way analysis of covariance with disease duration as a covariate was conducted to determine whether there was a significant difference in HRQOL. After controlling for disease duration, there was a statistically significant difference in overall HRQOL as measured by the PDQ-39 SI (Table 2). A significant difference was also observed between the two samples for the PDQ-39 dimensions of ADL, emotional wellbeing and cognition.
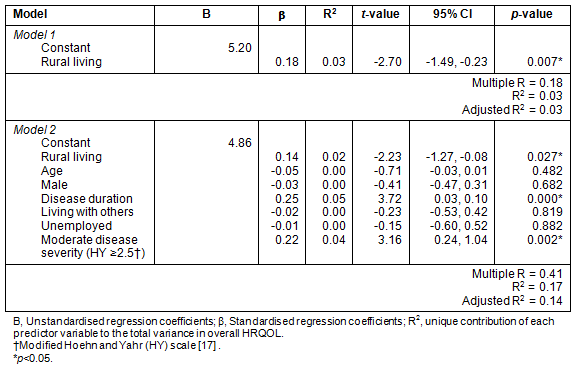
Rural living was found to be a significant negative predictor of HRQOL (β=0.14; 95% CI -1.27 to -0.08; p=0.027). It significantly contributed to the variance in HRQOL in both models, although it had a smaller contribution (2%) when other predictor variables were included. The final model accounted for 14% of the variance in HRQOL. The most important predictive factor was disease duration, which accounted for 5% of the variance in PDQ-39 SI scores. Moderate disease severity (modified HY Stage ≥2.5) was also a contributing factor, accounting for a further 4% of the variance in HRQOL. None of the interaction effects that were examined were significant at an alpha level of 0.05. As the interaction effects contributed less than 1% of the variance in HRQOL, the results for the regression analyses without the interactions between rural living, disease severity and disease duration have been presented (Table 3).
Table 2: Differences in health-related quality of life (HRQOL) between rural
and metropolitan participants after controlling for disease duration
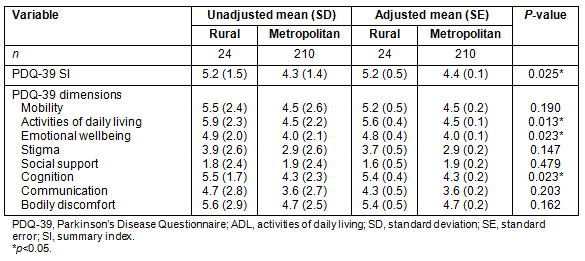
Table 3: Standard multiple regression of factors associated with health-related quality of life (HRQOL)17
This sample of people with PD living in rural Victoria rated their HRQOL at lower levels relative to individuals living in metropolitan Melbourne. Rural participants recorded higher mean scores for the PDQ-39 SI even after controlling for differences in disease duration, which indicated they had poorer HRQOL. This parallels findings by Klepac and colleagues, who found that living in a rural area in Croatia was associated with poor HRQOL in people with PD12. Similar findings have also been observed in veterans and elderly individuals living in rural settings13,23. The disparity in HRQOL that was observed in this small sample suggests that rural living may be negatively associated with HRQOL in some individuals and further research focusing on larger population samples from rural and remote areas is required.
The correlation between HRQOL and rural living was consistent with other HRQOL studies in PD, where rural life setting was associated with higher PDQ-39 scores. A variety of factors may explain this negative correlation12. Individuals with PD living in rural areas have reported experiencing difficulties with issues relating to their diagnosis, medications, and access to PD specialists and allied health professionals10. Consideration of such factors may therefore be useful when assessing individuals with PD who live in rural and remote areas. Further research is warranted to investigate how factors such as access to specialist healthcare programs and different service delivery models may play a role in determining the HRQOL of these individuals.
In this study, disease duration and moderate disease severity (modified HY Stage ≥2.5) were also found to predict HRQOL, which is consistent with previous reports4,5. It is widely accepted that people with long-standing PD may have poor HRQOL4 and those with more severe PD are more likely to experience poor HRQOL5. Nevertheless, disease duration and disease severity could be strongly correlated because as the disease progresses over time, the severity and associated disability of the disease may also increase24. Further investigations of the relationship between these two factors using statistical techniques such as path analysis would be useful to examine the implications of this covariance in relation to HRQOL. This information may assist clinicians to identify individuals at risk of experiencing poor HRQOL.
The main limitation of this study was the small sample of participants who were recruited from rural Australia. Another limitation was that the sample from metropolitan Melbourne may have perceived their HRQOL differently compared to the broader population of Australians with PD as they volunteered to participate in a physiotherapy exercise trial. In order to validate the findings of this study, further investigations with significantly larger sample sizes are required. Participants were also sampled predominantly from communities classified as inner regional areas in accordance with the Australian Standard Geographical Classification - Remoteness Areas system15. Thus, the rural sample might not have reflected the true population of people with PD living in rural Victoria. Further sampling of individuals living in outer regional or remote areas and other parts of Australia are needed to confirm and extend the generalisability of the current findings. Additionally, the same inclusion criteria were not applied to both samples because participants living in rural Victoria were not required to participate in a physiotherapy intervention program. No previous studies, however, have examined the HRQOL of Australians with PD living in rural communities. The significant association between rural living and poor HRQOL in Australians with PD highlights the need for further work in this area. Recommendations for future research are summarised, and include basic, applied and translational research (Fig1).

Figure 1: Recommendations for further research identified from this study.
PD, Parkinson's disease; HRQOL, health-related quality of life.
Quality of life is a multi-dimensional construct that takes into account global issues and the health, personal characteristics, social relationships and socioeconomic status of an individual25. This study did not examine the contribution of factors such as the quality of the rural healthcare system, access to PD-specialist services, presence of social support networks and individual coping styles. It may, therefore, be possible that these environmental, social and personal factors facilitated the disparity in HRQOL observed between individuals living in rural Victoria and those living in metropolitan Melbourne. Further studies are required to investigate whether factors such as access to specialist neurologists and allied health staff play a role in determining HRQOL in people with PD. The length of time rural participants have resided in a rural area also warrants further investigation in future studies in order to develop a better understanding of the contribution of rural living towards HRQOL in people with PD.
References
1. Access Economics. Living with Parkinson's disease: challenges and positive steps for the future. Canberra, ACT: Parkinson's Australia Inc, 2007.
2. Lees AJ, Hardy J, Revesz T. Parkinson's disease. Lancet 2009; 373(9680): 2055-2066.
3. Wright Willis A, Evanoff BA, Lian M, Criswell SR, Racette BA. Geographic and ethnic variation in Parkinson disease: a population-based study of US Medicare beneficiaries. Neuroepidemiology 2010; 34(3): 143-151.
4. Gómez-Esteban JC, Zarranz JJ, Lezcano E, Tijero B, Luna A, Velasco F et al. Influence of motor symptoms upon the quality of life of patients with Parkinson's disease. European Neurology 2007; 57(3): 161-165.
5. Global Parkinson's Disease Survey Steering Committee. Factors impacting on quality of life in Parkinson's disease: results from an international survey. Movement Disorders 2002; 17(1): 60-67.
6. Wood-Dauphinee S. Assessing quality of life in clinical research: from where have we come and where are we going? Journal of Clinical Epidemiology 1999; 52(4): 355-363.
7. Peters CM, Gartner CE, Silburn PA, Mellick GD. Prevalence of Parkinson's disease in metropolitan and rural Queensland: a general practice survey. Journal of Clinical Neuroscience 2006; 13(3): 343-348.
8. Chen CC, Chen TF, Hwang YC, Wen YR, Chiu YH, Wu CY et al. Different prevalence rates of Parkinson's disease in urban and rural areas: a population-based study in Taiwan. Neuroepidemiology 2009; 33(4): 350-357.
9. Walker RW, Hand A, Jones C, Wood BH, Gray WK. The prevalence of Parkinson's disease in a rural area of North-East England. Parkinsonism & Related Disorders 2010; 16(9): 572-575.
10. Duncan GF, Rositano P. Parkinson's disease in regional Australia. Rural and Remote Health 11: 1658. (Online) 2011. Available: www.rrh.org.au [Acessed 14 November 2012].
11. Soh S-E, Morris ME, McGinley JL. Determinants of health-related quality of life in Parkinson's disease: a systematic review. Parkinsonism & Related Disorders 2011; 17(1): 1-9.
12. Klepac N, Pikija S, Kraljic T, Relja M, Trkulja V, Juren S et al. Association of rural life setting and poorer quality of life in Parkinson's disease patients: a cross-sectional study in Croatia. European Journal of Neurology 2007; 14(2): 194-198.
13. Weeks WB, Kazis LE, Shen YJ, Cong Z, Ren XS, Miller D et al. Differences in health-related quality of life in rural and urban veterans. American Journal of Public Health 2004; 94(10): 1762-1767.
14. Morris ME, Menz H, McGinley J, Huxham FE, Murphy AT, Iansek R et al. Falls and mobility in Parkinson's disease: protocol for a randomised controlled clinical trial. BMC Neurology 2011; 11: 93.
15. Australian Bureau of Statistics. Australian Standard Geographical Classification (ASGC). cat. no. 1216.0. Canberra, ACT: ABS, 2006; 1.
16. Folstein MF, Folstein SE, McHugh PR. Mini-mental state: practical method for grading cognitive state of patients for clinician. Journal of Psychiatric Research 1975; 12(3): 189-198.
17. Hoehn MM, Yahr MD. Parkinsonism: onset, progression and mortality. Neurology 1967; 17(5): 427-442.
18. Peto V, Jenkinson C, Fitzpatrick R, Greenhall R. The development and validation of a short measure of functioning and well-being for individuals with Parkinson's disease. Quality of Life Research 1995; 4(3): 241-248.
19. Jenkinson C, Fitzpatrick R, Peto V, Kafantari A, Apostolidou E, Peitsidou E. The PDQ-8: development and validation of a short-form Parkinson's Disease Questionnaire. Psychology & Health 1997; 12(6): 805-814.
20. Peto V, Jenkinson C, Fitzpatrick R. PDQ-39: a review of the development, validation and application of a Parkinson's disease quality of life questionnaire and its associated measures. Journal of Neurology 1998; 245(1Suppl): S10-S14.
21. Damiano AM, McGrath MM, Willian MK, Snyder CF, LeWitt PA, Reyes PF et al. Evaluation of a measurement strategy for Parkinson's disease: assessing patient health-related quality of life. Quality of Life Research 2000; 9(1): 87-100.
22. Goetz CG, Poewe W, Rascol O, Sampaio C, Stebbins GT, Counsell C et al. Movement Disorder Society Task Force report on the Hoehn and Yahr staging scale: status and recommendations. Movement Disorders 2004; 19(9): 1020-1028.
23. Mainous AG, Kohrs FP. A comparison of health status between rural and urban adults. Journal of Community Health 1995; 20(5): 423-431.
24. Schrag A. Quality of life and depression in Parkinson's disease. Journal of the Neurological Sciences 2006; 248: 151-157.
25. Soh S-E, McGinley JL, Morris ME. Measuring quality of life in Parkinson's disease: selection of an appropriate health-related quality of life instrument. Physiotherapy 2011; 97(1): 83-89.
