Physiotherapy practice in Africa faces a number of challenges, one of which is the limited number of therapists in most public hospitals. In 2000 the ratio of physiotherapists to the local population was estimated as 1:550 000 in most of the public hospitals in Africa1. A survey conducted in Ghana identified no rehabilitation doctor or occupational therapist in the country2. In Kenya the ratio was estimated as 1:20 0003 and it was observed that physiotherapy services are limited by few trained personnel and funding4. The lack of general funds for service development and equipment could indicate that physiotherapy is still regarded as less important for development than others in health care, such as medicine and nursing5.
The physiotherapy profession has a long history of advocating for self-management between consultations, which has the potential to assist in the move to more community care6. Self-management is concerned with enabling a person who has a chronic condition to manage the day-to-day impact of the condition themselves7. It involves forming a patient-healthcare provider relationship which empowers and enables the person with a chronic condition to make choices and decisions about the activities they engage in to manage the condition7. Such activities can include utilisation of healthcare services, or adherence to therapeutic activities performed by themselves or others, in their home or work environments. Self-management may lead to efficient use of health services and meet the needs of people with chronic conditions or disability8. These processes would seem particularly important in countries where there is a shortage of health professionals.
Skilled and appropriate communication underpins effective practice in physiotherapy9-11, is a key professional ability12, and is highly valued by users of physiotherapy13-15. Positive communication between physiotherapists and users has socio-affective elements that help to provide social support, inspire cooperation and generate a positive emotional atmosphere16. Studies have revealed that positive feedback and consideration of service users' own conceptions of their problems and strategies for solving most problems could exert an important influence on recovery, improving both adherence to recommendations and outcome17,18. For effective self-management to occur there must be effective two-way communication and interaction between the physiotherapist and service user. However, absconding from institutional-based rehabilitation services by users has been highlighted in Kenya19, where children's carers thought hospital staff underestimated their emotional distress. This led carers to seek an alternative treatment for their child's disability from traditional and spiritual healers. A recent study in Kenya revealed the potential of a home-based intervention20. It revealed the opening up of communication between a caregiver and child with little or no communication. This communication recognised the child's strength and re-established social support systems that had earlier collapsed.
Despite this evidence, little qualitative research has examined the experiences of physiotherapy users in rural facilities in Africa. Many studies into users' perceptions of physiotherapy have been primarily quantitative. There have been a few qualitative studies, and these have been mainly in developed countries21-23.
Currently, physiotherapy services in Africa are offered in hospitals, which could pose challenges to the users. The aims of this study were to explore service users' experiences of the physiotherapy service in a rural Kilifi District general hospital in Kenya, and to evaluate whether current practice fosters self-management of chronic conditions.
This study aimed to answer the following questions:
- What is the user's perception of physiotherapy practice in Kilifi?
- What are the challenges faced by physiotherapy service users in Kilifi?
- Does current physiotherapy practice in Kilifi foster self-management of chronic conditions?
- What are the possible options for improved management of chronic conditions?
The research was predominantly qualitative with a component of observational data to triangulate the qualitative data.
Study site
Participants from this study came from the Kilifi Health Demographic and Surveillance System (KHDSS) area. The KHDSS is in Kilifi District in Kenya and stretches from the Mida Creek in the north to the Mtwapa Creek in the south. It borders the Indian Ocean in the east and the Arabuko-Sokoke Forest in the west and covers an area of 900 km2. It has a population of approximately 250 000 and the Mijikenda ethnic group predominates.
Study participants and sampling procedure
Study participants were drawn from a pool of 549 patients (284 males) attending physiotherapy as recorded in the 2009 outpatient attendance register. The department attends to patients from Kilifi and neighbouring districts. From the 549 cases, 78 patients (44 males) resided in the KHDSS area. The KHDSS is a demarcated research area controlled by the Kenya Medical Research Institute for research purposes. A purposive-convenience sample of 32 participants was selected from these 78 patients. Inclusion criteria included availability of time to participate, regular attendance for therapy and residing in the KHDSS area. Exclusion criteria included unwillingness to take part in the study, not being a regular attendee, and coming from outside the KHDSS area. Geographical representation and sex balance were considered. Eight participants from the sampled 32 who came from the furthest distance were identified for interviews (Table 1). Due to poor infrastructure, those who live in close proximity were sampled for focus group discussions (Table 2).
Table 1: Details of patients interviewed
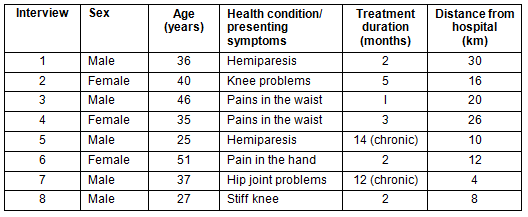
Table 2: Details of patients in focus groups
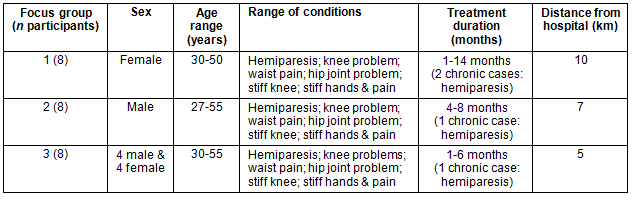
Methods of data collection and analysis
Interviews, focus groups and participant observations were used as data collection methods. Interviews and focus group discussions have different dynamics and therefore may reveal different information; they are also used for comparison and triangulation. Participant observation was considered appropriate as it gave a close familiarity with the given group of individuals through intensive involvement with the given group, and it conceals the status of the researcher.
Eight in-depth interviews and three focus group discussions using open-ended questions were conducted to elicit information from study participants giving a total sample size of 32. All the interviews and focus groups were conducted in Swahili and within the hospital environment by a trained fieldworker. The Swahili language was chosen because all participants were fluent in that language. Written field notes were taken by a trained fieldworker during both individual interviews and focus group discussions. All the interviews and focus group discussions were recorded using a digital recorder, transcribed in Swahili language and then translated into English language. The transcriptions were imported to NVivo 9 (www.qsrinternational.com) for management and storage. The NVivo program assists the researcher to organise the data in a systematic way for easy retrieval, management and analysis. With software assistance, inductive analysis as described by Patton24 was used to analyse the data. According Patton, the first step of data analysis is the creation of 'free nodes'. Transcripts are read and re-read for familiarisation and then coded as free nodes. The second step is when the free nodes with similar or thematically linked content are identified and grouped together to form 'tree nodes', each bearing a name of a theme. The third step is the identification of connections within the themes and making interpretations. Two authors shared and cross-checked analysis of the transcripts. Conflicting ideas were discussed and analysis was utilised to clarify interpretation for consensus.
Participant observations were conducted by the first author (JKG). In these observations, the researcher status is not known to the observed groups, and the observer takes part in activities of the observed group. The observations were conducted in four different areas of the physiotherapy department at different times: in the gym where the physical exercises were conducted; in the electrotherapy room; in the waiting bay where patients waited for their treatment; and in an area where lying and standing exercises were conducted. Observations were made on: type of treatment and how long patients waited for treatment; how the treatment was administered; the time the therapist allocated to a patient; patients' reactions during and after treatment; and clients' general mood. Field notes were taken in each observation. Field notes act as both data and analysis25.
Observed participants were different from those who consented for interviews. No participant had to stay overnight to receive therapy. The length of therapy for most of the participants was between 10 and 15 min with therapist, and approximately 20 min alone. Although the conditions of the focus group participants tended to be similar, each focus group had different respondents.
Ethical considerations
The study was approved by the National Ethics and Review Committee in Nairobi (SSC #1406).
All sampled users were given letters of invitation by a fieldworker, in which the purposes of the study were indicated. It was emphasised that participation in the study was voluntary and that there would be no adverse consequences if one opted not to attend. The fieldworker who presented the invitation letters obtained each participant's verbal and signed consent. Re-imbursement of fares to and from the hospital was provided to all participants.
The results are presented in four broad themes: perception of treatment; challenges to treatment; options for long-term conditions; and self-management.
Perceptions of treatment
Perceptions of treatment was found to have two sub-themes: effective and regular monitoring.
Effective: The majority of the users viewed the physiotherapy treatment to be effective and felt that it had helped them improve significantly. Being shown the procedures of the therapy and applying those procedures regularly facilitated faster recovery:
According to me the treatment is good. If you go there they show you what to do and after a while you see the problem fading away. (FGD with women)
I feel that the treatment is so good in that my condition is improving by each passing day. (FGD with men)
It is good because the part that was paining and stiff is gaining back flexibility and recovering gradually. (FGD mixed)
I came here when I could not walk. But as you can see now I can walk. (Interview, male client)
The treatment is good and helpful because the condition I came isn't the same condition I am today; the condition is improving and getting better each day. (Interview, female client)
Regular monitoring: Respondents felt that there was a need for continuous assistance from the therapists whenever therapeutic visits were made. The therapy users were left alone with little assistance from the therapists. Even young users tended not to attract the attention of the physiotherapists:
I think since she is still a young girl she should be assisted by a therapist anytime she is doing the exercises. (Interview, carer [sibling])
I have observed and seen that most clients are struggling alone. They need assistance. (Interview, male client)
I don't think they are doing enough to assist clients during therapy sessions. (Interview, female client)
Observations showed participants sharing positive remarks on the effectiveness of the therapy process. There were indications of satisfaction in terms of their improvement, although there were signs that continuous assistance was not provided by therapists. Most patients were observed to be on their own during exercises.
Perceptions of therapists
There were mixed reactions concerning the patients' relationships with the therapists. Some were critical of the therapist whom they felt did not keep them informed or listen to their concerns, or lacked empathy. However most of the users had positive therapeutic experiences with the majority of the therapists.
Positive experiences: Positive experiences were highlighted in all the focus groups and interviews (Table 3). Some participants viewed the physiotherapists as dedicated to their work. Such physiotherapists were viewed as possessing virtues that were acceptable in the community context.
Table 3: Positive experiences with therapist
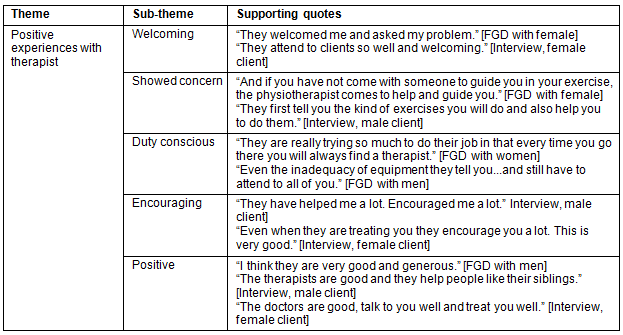
Negative experiences: Some participants reported negative experiences with a few of the therapists, whom they felt were not sensitive to their needs and tended not to be duty conscious. Details are provided (Table 4).
Table 4: Negative experiences with therapist

Challenges to treatment
Challenges reported by users were divided into a number of sub-themes (Table 5). Distance from the hospital, shortage of staff and lack of equipment in the therapy facility were major impediments to accessing therapy. Lack of proper information on prognosis led to disappointments.
These experiences were supported by the observational data of patients talking freely among themselves. It was observed that therapists came late. In one instance, a patient was observed complaining to a therapist after being burnt by a hot pack which appeared to have resulted into a large wound. Shortage of staff and equipment was also observed. Most of the time one therapist was observed to be left in the department, moving up and down attending to the patients. Patients were observed to share experiences of the long distances they had to cover to get to the hospital and were also observed to discuss about fellow patients who had absconded due to travelling expenses. Most of the patients who had absconded had chronic conditions and had run out of money.
Table 5: Challenges to physiotherapy treatment

Possible options for long-term conditions
Most users expressed the need for rehabilitation options due to problems in accessing the physiotherapy services at the hospital. There were suggestions for community- or home-based services to facilitate easy and affordable accessibility for patients with chronic conditions:
There is need for community or home-based physiotherapy services for those with long-term conditions. Many times they fail to come because the exercises take a long time and can't afford. (FGD with women)
I am not sure if these services can be brought to our homes or villages like what Association for Physical Disabled of Kenya does. (Interview, male patient)
Self-management of long-term conditions
The results indicate that the current physiotherapy practice at the hospital does not foster self-management of chronic conditions. Users complained of travelling long distances without being introduced to self-management skills for use at home. There were no other options for users who failed to report for therapy.
We are from Chumani at Charo Kiringi stage, then we go towards the ocean. It's far. So if we can't make it, that's the end. (FGD with women)
Our problem is just we are from far and have to come here daily for a long time and we spend a lot of money for fare and I am not improving fast. (FGD with men)
So if one does not have a relative near the hospital then he will need to rent a room if he has money, but if he does not have money then he will not attend as required. We need to be taught how to do it ourselves at home. (Interview with female patient)
Observations revealed users' desire for self-management at their home environments. Users, especially those with chronic conditions, were observed to engage in talk that suggested a wish for better options for managing their conditions. Observations further showed that physiotherapy practice in the department did not encourage self-management as there was greater emphasis by the therapists on regular attendance, rather than self management of their conditions.
Discussion
This study reflects the views and experiences of physiotherapy users in a rural government hospital. The majority of users interviewed had positive perceptions of most of the therapists and the treatment given. As much as the treatment was effective, most users appeared to benefit from a good relationship with the therapist whom they perceived as taking a personal interest in their wellbeing. Users valued a therapist who was welcoming, concerned, conscientious and encouraging. This further encouraged them to strive for improvement as a way of expressing their appreciation to the therapist. In rural communities users' perceptions of a health professional influences their commitment to the treatment provided.
Though most users perceived the physiotherapy treatment as effective, it presented challenges in terms of travelling long distances to attend the therapy. Other challenges were lack of staff and equipment in the hospital, which overshadowed the expectations of most patients. This finding is in line with a WHO disability report3 which found a patient : therapist ratio in Kenya of 1:20 000. Issues relating to inadequate therapist skills or training and equipment have been highlighted in other studies as a common phenomenon in rural Africa1. For users with chronic conditions and who struggle to reach physiotherapy facilities, a shift to community-based practice, which would be more responsive to user requirements and needs in rural area, may be indicated. For the enhancement of rehabilitation health services in rural communities, community based rehabilitation (CBR) has the potential to facilitate easy access26. The potential of the therapists and community-based workers in the management of chronic conditions must be emphasised. The CBR framework emphasises empowerment of community-based workers to provide easy access to and sustainability of services through affordable mechanisms.
Though treatment was perceived as effective by many, dissatisfaction with continued assistance during the treatment process was common. The expectation of continued assistance may represent several key, yet differing, issues relevant to fostering self-management of chronic conditions. The aspect of self-management was mentioned by a number of users, and could have been facilitated by lack of emphasis from the therapists. Self-management is a necessary aspect of physiotherapy6, and has been shown to lead to efficient use of health services that meets the needs of people with chronic conditions8.
Lack of user supervision during rehabilitation may indicate inadequate staffing of the department. Alternatively, it may reflect differences in therapist and user expectations and indicate the need for improved communication. While therapists may believe that they are fostering self-management and enabling user rehabilitation by minimising or reducing supervision, the expectation that users will take an active role in therapy appears to be inadequately communicated. Positive communication between physiotherapists and users has many beneficial effects16, and in the present case could have led to efficient physiotherapy practice. This supports the idea that satisfaction in physiotherapy, as in other health processes, is multidimensional and may be influenced by underlying tensions. Researchers have identified ten different dimensions of satisfaction26-29. The dimension of effective treatment outcome highlighted in this study is similar to the findings of other studies conducted in the USA30-32.
The results also revealed that scant information about treatment procedures was given to users, with most users indicating dissatisfaction with information about the duration of the treatment. This is similar to the findings of Deyo and Diehl, who found that users indicated most dissatisfaction over inadequate explanation of the problem and the following treatment procedure32. In an attempt to provide clear prognostic information, therapists may under- or over-estimate the likely rate of progress and amount of treatment required.
However, for many conditions, particularly those that are chronic, prognosis and the optimum type and length of treatment are difficult to determine at the initial consultation. Therapists who lack access to current research findings have to rely on their own or their colleagues' clinical experience. However, clinical experience is prone to bias and should be supported with current evidence on effective management strategies33. For many conditions, or where such information is lacking, it may be most appropriate to use clinical reasoning in a user-centred approach34. Such an approach can include setting short- and long-term goals which are negotiated and agreed with the user prior to commencing therapy, along with planned times for review of progress with user participation. Such a dialogue opens communication about variability in healing times and responses to therapy. It can empower users to take an active role in decision-making with regard to usage of therapy services35. It may also encourage therapists to evaluate the need for frequent therapy sessions at a centralised location, and identify ways to enable patients to continue therapy in their home environment. The element of empowerment is crucial in rural communities as it enhances full participation and ownership of the therapy activities.
Community- or home-based services were viewed more appropriate for patients, especially those with chronic conditions because they were easily accessible and affordable. This is in line with the WHO recommendation that community-based approaches should be utilised as options for delivering rehabilitation services in rural communities with low resources36.
It is not clear from the present study what underlying mechanisms may lead to a problematic therapist-user relationship. Performance appraisal, continuing professional development and reflective practice approaches are used in the therapy professions to ensure that high quality, patient-centred care is provided37. However, where staffing levels are insufficient and funding is limited, it is likely that staff management reviews and service improvement processes are inadequate or absent38. Staff may lack support or skills to honestly and openly reflect on, appraise and improve their own practice. For quality service provision that meets the needs and expectations of service users, such issues require further consideration and research. For example, action research can be used to understand service providers' views of existing opportunities and challenges, and how they can best support users in the self-management of long-term conditions in rural communities.
Limitations
The participants in the study were not given the opportunity to verify the transcriptions before they were translated to English. The exclusion of the physiotherapy absconders was also a major limitation due to the likelihood of their greater insights into the challenges of accessing physiotherapy when one had a chronic condition.
Conclusion
Users' experiences of physiotherapy treatment in this rural hospital indicate that a host of challenges exist. In the face of these challenges, the needs of users may be compromised, especially for those with chronic conditions. Rehabilitation services that are easily accessible and affordable could be better options in rural areas and resource-low settings. There is therefore a need for community-based services that place emphasis on the self-management of chronic conditions in order to foster better health outcomes in rural communities.
Acknowledgements
The authors thank the Director Kenya Medical Research Institute (KEMRI) for permission to publish these data. This work was supported by the Cerebral Palsy Foundation (UK) and KEMRI/Wellcome Trust Collaborative Research Programme. Prof Charles Newton is supported by Wellcome Trust UK (no. 083744).
References
1. Twinble R, Henley E. Preparing occupational therapists and physiotherpaists for community based rehabilitation. Asia Pacific Disability Rehabilitation Journal 2000; Selected Readings Series 1, s.109-26, Jan (17 s).
2. Tinney MJ. Medical rehabilitation in Ghana. Disability & Rehabilitation 2007; 29: 921-927.
3. World Health Organisation. World Report on Disability. Geneva: WHO, 2001.
4. Hard J, MacKay C, Okidi C. Volunteer Clinical Placements for Canadian Physiotherapist and Physiotherapy Students in a community-based rehabilitation programme in rural Kenya. World Congress of Physiotherapy; 24 June 2007; Vancouver (Poster presentation) 2007.
5. Frantz J. Challenges facing physiotherapy in Africa. Internet Journal of Applied Health Sciences and Practice 2007; 5(4): 1-5.
6. Kenyon J, Kenyon K. The physiotherapists pocket guide: essential facts at your fingertips. Melbourne, VIC: Churchill Livingstone, 2004.
7. Lorig KR, Holman H. Self-management education: history, definition, outcomes and mechanisms. Annual Behavioural Medicine 2003, 26: 1-7.
8. Wilson P.M, Kendall S. Brooks F. Nurses responses to expert patients: the rhetoric and reality of self-management in long-term conditions: a grounded theory. International Journal of Nursing Studies 2006; 43(7): 803-818.
9. Anon. European Region, European physiotherapy benchmark statement. World Conference of Physical Therapy, 2003. (Online) 2003. Available: http://www.physio-europe.org/pdf/Benchmark.pdf (Accessed 15 July 2013).
10. Jensen G, Gwyer J, Hack L, Shepard K. Expertise in physical therapy practice. Boston, MA: Butterworth Heinemann, 1999.
11. Reynolds F. Communication and clinical effectiveness in rehabilitation. Boston, MA: Butterworth Heinemann, 2005.
12. Health Professionals Council. Standards of Proficiency-physiotherapist. (Online) 2007. Available: http://www.hpc-uk.org/assets/documents/10000DBCStandards_of_Proficiency_Physiotherapists.pdf
13. Partridge C. Evaluation of physiotherapy for people with stroke: report of a workshop on appropriate outcomes of physiotherapy for people with stroke. London: King's Fund Centre, 1994.
14. Johnson R. Attitudes don't just hang in the air: disabled people's perception of physiotherapists. Physiotherapy 1993, 7: 619-627.
15. Pound P, Bury M, Gompertz P, Ebrahim S. Views of survivors of stroke on benefits of physiotherapy. Quality Health Care 1994, 3: 69-74.
16. Lundvik-Gyllensten A, Gard G, Salford E, Ekdahl C. Interaction between patient and physiotherapist: a qualitative study reflecting the physiotherapist's perspective. Physiotherapy: Research International 1999, 4: 89-109.
17. Westman-Kumlin I, Kroksmark T. The first encounter: Physiotherapists' conceptions of establishing therapeutic relationships. Scandinavian Journal of Caring Science 1992; 6: 37-44.
18. Sluijs EM, Kok GJ, van deer Zee J. Correlates of exercise compliance in physical therapy. Physical Therapy 1993, 73: 771-782.
19. Gona JK, Mung'ala-Odera V, Newton CR, Hartley S. Caring for Children with Disabilities in Kilifi, Kenya: what's the carer's experience? CHILD: Care, Health & Development 2011; 37(2): 175-183.
20. Gona JK, Newton C, Hartley S, Bunning K. Home-based intervention using augmentative and alternative communication (AAC) techniques in rural Kenya: what are the caregivers' experiences? CHILD: Care, Health & Development. (Online) 2013. Available: http://onlinelibrary.wiley.com/doi/10.1111/cch.12031/full (Accessed 24 July 2013).
21. Johnson RJ. Low-back pain in sports: Managing spondylolysis in young patients. Physician and Sports Medicine 1993; 21(4): 53-59.
22. Thomas C, Parry A. Research on users views about stroke survivors: Towards an empowerment Research paradigm or more of the same? Physiotherapy 1996; 82(1): 6-12.
23. May SJ. Patient satisfaction with management of back pain. Physiotherapy 2001; 87(11): 4-20.
24. Patton MQ. Qualitative evaluation and research methods, 2nd edn. Newbury Park, CA: Sage, 1990.
25. Dewalt KM, Dewalt BR. Participant observation: a guide for fieldworkers. Walnut Creek, CA: AltaMira, 2002.
26. World Health Organisation. Community-based Rehabilitation Guidelines. Geneva: WHO, 2010.
27. Fitzpatrick R. Surveys of patients' satisfaction. 1: important considerations. BMJ 1991; 302: 887-889.
28. Linder-Pelz S. Towards a theory of patients' satisfaction. Social Science and Medicine 1982; 16: 577-582.
29. Hall JA, Dorman MC. What patients like about their medical care and how often they are asked: A meta-analysis of the satisfaction literature. Social Science and Medicine 1988; 27: 935-939.
30. Ware JE, Snyder MK, Wright R, Davies AR. Defining and measuring patients' satisfaction in medical care. Evaluation and Programme Planning 1983; 6: 247-263.
31. Greenfield S, Anderson H, Winickoff RN, Morgan A, Komaroff AL. Nursing protocol management of low back pain: Outcomes, patients' satisfaction and efficiency of primary care. Western Journal of Medicine 1975; 123: 350-359.
32. Deyo RA, Diehl AK. Patients' satisfaction with medical care for low-back pain. Spine 1986; 11(1): 28-30.
33. Cherkin DC, Mac Cormack FA. Patients' evaluation of low back pain care from family physicians and chiropractors. Western Journal of Medicine 1989; 150: 351-355.
34. Sackett D L, Rosenberg WMC, Muir-Gray JA, Haynes BR, Richardson WS. Evidence Based Medicine. What it is and what it isn't. BMJ 1996; 321: 71. Available: http://www.bmj.com/content/312/7023/71.full
35. Kook K. User-centred design and evaluation of affected interfaces. In: Z Ruttkay, C Pelachaud (Eds). From Brows to Trust: Evaluating Embodies Conversational agents. Philadelphia, PA: Kluwer, 2004.
36. Stephenson R. Clinical reasoning as a tool for CPD' in Tools for Continuing Professional Development, 2nd Edn. London: Quay, 2012.
37. UN. Declaration of Alma-Ata, 1978. (Online) no date. Available: http://www.who.int/publications/almaata_declaration_en.pdf (Accessed 15 July 2013).
38. Wells C. Practice education and CPD' in Tools for Continuing Professional Development, 2nd Edn. London: Quay, 2012.



