Latin America is undergoing rapid demographic and nutritional transitions with the accompanying tendency to overweight, as is common in countries emerging from poverty. This change in weight can be explained by changes in eating habits and an increase in sedentary leisure activities. In Brazil, population weight changes due to the nutritional transition have been independent of socioeconomic status, and obesity is one of the greatest public policy challenges1. Being overweight is now the most common health issue that affects children in Brazil2.
Although the nutritional status of children living in urban areas has been widely studied few studies have sought to understand the nutritional perspective of children in rural environments. A study of school children aged 5-9 years old in a rural state school in the Federal District of Brazil found a low prevalence of overweight when compared with the urban population, and none of the children were underweight3. Among specific populations in the rural regions of other countries, similar or even more severe situations were observed, some affecting 20% of children between 7 and 9 years of age4,5.
Objective
The object of this study was to estimate the prevalence of nutritional extremes among school children aged between 7 and 10 years, living in a rural municipality in the Brazilian southeastern region.
A cross-sectional study of children from primary schools was conducted in 2009-2010 in the municipality of Santa Maria de Jetibá, Espírito Santo (ES). Santa Maria de Jetibá is located in the mountainous region of ES and is 87 km from the capital Vitória (Fig1). The approximately 34 000 population of this rural municipality are of European origin and 70% live in rural areas where poultry farming and agriculture are the main economic activities. The municipality is known nationally for its organic agricultural produce (www.pmsmj.es.gov.br).
Figure 1: Map of the locations of the study Santa Maria de Jetibá-ES, Brazil.
The sample was planned for this study in order to geographically cover the whole municipality, and the following criteria were used: 2385 school children between 7 and 10 years, an anticipated prevalence of 10% excess weight (overweight and obesity), an error of 3%, design effect of 2, and 5% level of significance. Randomized stratification was used for sampling in two stages. Firstly the total number of children in the regions schools (urban and rural) was considered, subsequently the school size (small: up to 50 students; medium: from 51 to 200; large: more than 200 students). This was proportional to quotas and based on the number of students enrolled in 2008. The minimum number of students calculated was 662 and in order to achieve this, 1000 school children were randomly selected and invited to participate. Children younger than 7 or older than 10 years at the time of data collection were excluded from the study, as were those without an informed consent form signed by their parents or guardians.
A pilot study was performed in a state school with 40 children prior to data collection. Trained undergraduate health discipline students who lived in the region collected data for the main study. During data collection each trainee was responsible for the measurements or questionnaire in order to reduce variability among evaluators.
Anthropometric measurements were performed at schools. Weight was measured in kilograms to 100 g precision using Tanita scales (Family BWF model; Tanita, IL, USA). All children were measured wearing minimal clothes and without shoes, standing at the center of the scales, facing forward and with their arms along their bodies. Height was measured in centimeters to 1 mm precision using a SECA mobile stadiometer (model 206; Seca, Hamburg, BRD) fixed on a flat wall without a baseboard. All children were measured facing forward, barefoot, with loose hair and their back and heels touching the wall. The BMI was calculated and WHO anthropometric standards were used as reference6. The following cut-off points were used: BMI for age < 3rd percentile = underweight and BMI per age > 97th percentile = obesity.
Information on the child's eating habits and physical activity in the school environment was obtained using a standard questionnaire which included: eating breakfast (yes or no); number of meals per day (≤ 4 or > 4); ate lunch with other people (yes or no); school location (urban or rural); sex (female or male); age (7, 8, 9 or 10 years) and skin color. The last variable was obtained by two interviewers who were trained to classify skin colors as white, black, brown or yellow. When the two interviewers disagreed, a third internee would evaluate and the skin color was classified as 'white' or 'not white'.
To assess differences between proportions a X2 was performed with a statistical significance of 5%, using SPSS statistical software v18.0 for Windows (www.spss.com).
Ethics approval
The research project was approved by the Research Ethics Committee from the Center for Health Sciences at the Federal University of Espírito Santo (no. 060/90).
Data were collected from 901 children, 445 male (49.4%) and 456 female (50.6%), most of whom lived in a rural location (58.4%) and were white (78.3%). No significant differences were found when comparing sex to the variables of age (p=0.90), location (urban/rural; p=0.22) and skin color (p=0.22). The distribution of socio-demographic variables and nutritional status is provided (Table 1).
Table 1: Distribution of the studied sample according to socio-demographic variables and nutritional status, Santa Maria de Jetibá, Brazil
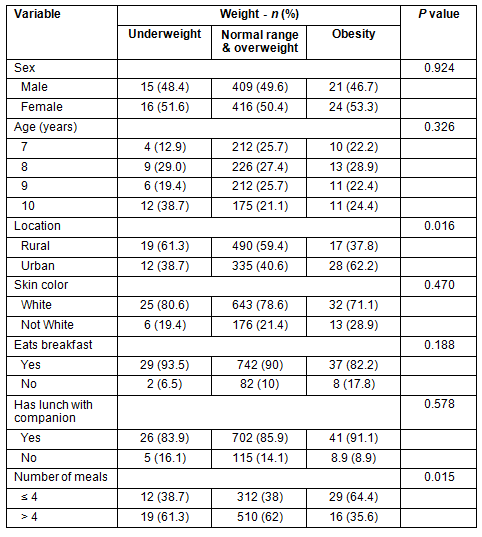
Regarding eating habits, 81.6% ate lunch with a companion, 60.7% ate more than 4 meals a day and 90% ate breakfast every day. The prevalence of nutritional extremes according to socio-demographic variables is also provided (Table 1).
A prevalence of 3.4% underweight and 5% obesity was found, with no statistically significant differences observed for sex, age, skin color or for the presence or not of a companion during meals. School children who were classified as obese were less likely to eat breakfast but this was not statistically significant.
However a significant difference was found in the children's home location (urban or rural area) with 7.5% obesity found among the urban children, which was approximately twice that of obese rural dwellers. Among the school children who ate 4 or fewer meals a day the prevalence of underweight and obesity were 3.4% and 8.2%, respectively. However, the prevalence of those who ate more than 4 meals 3.5% and 2.9%, respectively.
Discussion
The nutritional transition in Brazil, as in other developing countries, has presented a public health problem in the coexistence of malnutrition and overweight in the same social group, contributing to an increase in non-communicable diseases1. In this study the percentage of underweight was found to be relatively low both in urban and rural areas of the region studied. The phenomenon of reduction in the incidence underweight has been observed throughout Brazil in the past three decades. This change has been associated with an increase in purchasing power among the poorest of the population, and also the public investments that allow universal access to essential services such as education, health and sanitation7.
The prevalence of obesity found in the municipality of Santa Maria de Jetibá is lower than the 10.9% observed in a study of the rural municipality of Arapotí, Paraná state8 with 1647 school children. Triches and Giugliani9 performed a study in Rio Grande do Sul with school children aged 8-10 years and found a similar prevalence of obesity, in the rural region (3.9%), and 8% in the urban region. In the present study, children who lived and studied in the urban area had twice the chance of being classified as obese, compared with rural dwellers. Furthermore, obesity was associated with a low frequency of eating breakfast, which is in accordance with a sample of children and teenagers that showed those who eat breakfast to be less prone to overweight10. The authors also suggested that an inadequate or no breakfast can contribute to poor food choices during the day, thus promoting obesity10. Another plausible hypothesis is that not eating breakfast interferes with appetite control, leading to obesity11. Regarding the number of meals, the results of this study were similar to those found among German school children, in which obesity prevalence was more frequent among those who eat 4 or fewer meals each day12.
Limitations
In the present study BMI was used as an indicator to diagnose nutritional status; however, the cut-off points used in studies with children vary and this hindered the comparison with prevalences reported in other studies.
Eating four or fewer meals a day was associated with obesity, possibly due to alterations in biological mechanisms, such as insulin and lipogenesis, as well as being a probable indicator of low diet quality12, although the possibility of biased information cannot be discounted.
We conclude that underweight, as an historical problem in Brazil, has been reduced, possibly due to improvements in health access and living conditions, even in rural areas. The other extreme, that is obesity, was associated with home location. This could be explained by lower socioeconomic conditions and greater physical activity in daily tasks in the rural area studied.
Promoting physical activity, mainly in the urban location of the municipality studied, is an important way to reduce obesity and improve quality of life among school children. Nutritional education to improve eating habits is suggested in urban and rural regions of the municipality, especially in the urban area.
References
1. Coutinho JG, Gentil PC, Toral N. Malnutrition and obesity in Brazil: dealing with the problem through a unified nutritional agenda. Cad de Saúde Pública 2008; 24(Suppl 2): S322-S340.
2. Brasil. Ministério da Saúde. Secretaria de Atenção à Saúde. Departamento de Atenção Básica. Obesidade. Ministério da Saúde, Secretaria de Atenção à Saúde, Departamento de Atenção Básica, Brasília: Ministério da Saúde, 2006.
3. Rivera FSR, Souza EMT. Perfil nutricional e econômico de escolares de uma comunidade rural. Revista de Saúde do Distrito Federal 2005; 16(3): 23-31.
4. Núñez-Rivas HP, Monge-Rojas R, León, Roselló M. Prevalence of overweight and obesity among Costa Rican elementary school children. Rev Panam Salud Publica/Pan American Journal of Public Health 2003; 13(1): 24-32.
5. Montgomery-Reagan K, Bianco JA, Huston RS. Prevalence and correlates of high body mass index in rural Appalachian children aged 6-11 years. Rural and Remote Health 9:1234. (Online) 2009. Available: www.rrh.org.au (Accessed 26 September 2012).
6. WHO. Growth reference data. (Online) 2012. Available: http://www.who.int/growthref/ (Accessed 1July 2012).
7. Monteiro CA, Benício MHD, Konno SC, Silva ACF, Lima ALL, Conde WL. Causes for the decline in child under-nutrition in Brazil, 1996-2007. Rev de Saúde Pública 2009; 43(1): 35-43.
8. Salomons E, Rech CR, Loch MR. Estado nutricional de escolares de seis a dez anos de idade na rede municipal de ensino de Arapotí, Paraná. Rev Bras de Cineantropom. & Desempenho Hum 2007; 9(3): 244-249.
9. Triches RM, Giugliani ERJ. Obesity, eating habits and nutritional knowledge among school children. Rev de Saúde Pública 2005; 39(4): 541-547.
10. Rampersaud GC, Pereira MA, Girard BL, Adams J, Metzl JD. Breakfast habits, nutritional status, body weight, and academic performance in children and adolescents. Journal of American Dietitians Association 2005; 105: 743-760.
11. Giovannini M, Verduci E, Scaglioni S, Salvatici E, Bonza M, Riva E et al. Breakfast: a good habit, not a repetitive custom. Journal of International Medical Research 2008; 36: 613-614.
12. Toschke AM, Küchenhoff H, Koletzko B, von Kries R. Meal frequency and childhood obesity. Obesity Research 2005; 11(13): 1932-1938.



