There is a longstanding strong gender imbalance in the medical workforce. Increasing female entry to medical school is redressing this issue worldwide1, with the consequence that the proportion of female junior medical officers in hospitals is approaching that of medical school enrolments2. But in specialty training, and college membership thereafter, the imbalance persists: internationally workforce ratios of women to men drop precipitously for all but primary care2. In Australia also, the specialties have significant differences in gender representation. Though all Australian medical school enrolments have been roughly equivalent for some decades3, entry into the vocational colleges is uneven: at best 56-66% for general practice, obstetrics & gynaecology, paediatrics, palliative medicine, rehabilitation medicine, and at worst 14-24% for surgery, radiology, environmental medicine and intensive care4.
The gradual entry of women into the medical workforce has brought a suite of work-related topics to the forefront of discussion, and these include working hours (eg being required to work hours that are difficult for a mother); exit and re-entry criteria (having lost position advantages after exiting the workforce); ceilings for seniority (fewer women in positions of medical leadership); specialisation skew; and geographical skew (not all disciplines allow flexible work arrangements). It should be noted that all are workforce- rather than gender-specific issues2,5. Some argue that these issues describe workforce discrimination1,6.
Although a number of these issues could be considered costs that women deal with personally, others are costs borne by the system. So, for example, the public cost of training a basic graduate may be considered to be well invested in a doctor who pursues long hours in full-time work without a break, but less well invested in a doctor who does not spend continuous years in service or is working part time and has been described as 'retreat from work'7.
Other costs are borne by the population. There are fewer female than male doctors in rural practice and this means that rural women have less opportunity to discuss intimate issues with a female doctor than their urban peers8. Such a reality may underlie the lower reporting rates, and higher morbidity and mortality for presentations such as women's cancers in the bush9.
The specific and continuing shortage of women doctors in rural medicine is an important topic for discussion. Indeed rural female doctors' views on workforce planning are already expressed and include such sensible measures as on-call cover, flexible work arrangements, child care, as well as increasing opportunities for peer-support, and new ways of offering continuing medical education (CME)10,11.
It is of interest that much of the rural discussion to date has considered the way women's workforce priorities negatively impact the sustainability of present and projected workloads, and how to manage this impact through workforce modelling12. Less frequently discussed positives include the particular contributions made by women doctors, including differences that may enhance patient health outcomes. Women, for example, are considered to practice more patient-centred care13; and while female GPs engage in longer consultations, they also have more consultations with mental health billing codes14. The relative paucity of rural female GPs may contribute to mental health under-management in rural and remote locations.
A further positive, which has not received the discussion it deserves, is the specific benefit of women in the workforce with respect to part-time work. This is usually cited as a negative factor associated with having a family6; however, this study aimed to examine the positive aspects of having part-time female doctors in the rural academic workforce, asking:
- Are there significant numbers of women relative to men in this workforce?
- How does this female rural academic workforce compare with the female medical workforce at large?
- How sustainable is this rural female academic workforce, using years in employment as the proxy for sustainability?
Context
The Rural Clinical School of WA (RCSWA) is a workforce initiative with the long-term aim of recruiting new rural doctors by training undergraduates in rural locations, so students live and study for one academic year in the country. The RCSWA includes every major and some smaller towns in WA as educational sites - 13 sites in all. Its staff is entirely local, and teaching appointments specify part-time teaching and part-time clinical work to ensure continuity of teaching from the classroom to the clinic.
Intervention
Given the known social and cultural priorities that women doctors bring to the workplace15, a number of relevant employment characteristics developed in RCSWA are described. First, the instigation of rural teaching networks where potential new teachers are recognised and identified then mentored has emphasised the development of teaching skill and confidence, reflecting the priorities of rural female practitioners15. Peer support is also key to rural women practitioners, particularly networking with female colleagues15. To this end, RCSWA's focus on, and funding for, collaborative cross-site communication by email, quarterly meetings, variously convened working groups and interest groups has been pivotal to networked practice. Family-friendly policies are also critical. The commitment to pay for a whole family to join an annual meeting and the provision of child-care for travelling doctors are two examples of policies specially negotiated through university regulators, reflecting the mutual choice of family alongside career15.
Study data
Human resource records were obtained from The University of Western Australia dating from The RCSWA inception in 2002 to 30 June 2012. Teachers who were full-time employees of WA Country Health Services Hospitals or casually paid were not included. The RCSWA staff lists produced internally each year were also consulted. Further administrative data relating to gender, reason for leave (maternity or other) and location of practice were added manually from Rural Clinical School administrative registers.
Data were maintained in Excel v14.1.4. The total months each staff member worked from their employment to June 2012 were tabulated. Relative risk and χ² statistics were calculated using male RCSWA employees and workforce data published by Rural Health West as the comparators.
As the study used general administrative data relating to ongoing operation of the program, it qualified as an evaluation exercise was ethics-exempt.
Background development of Rural Clinical School of Western Australia
Most of the doctors who set up the 13 RCSWA sites were male, reflecting the predominantly male composition of local general practices (primary care clinics). Women set up three sites. This statistic (23%) is lower than the overall proportion of female GPs in the rural Western Australian workforce, and is probably an indication of the time investment required to house, staff and resource a new university teaching centre, that is, mature male practitioners whose level of time commitment has traditionally formed part of the argument for a male workforce16. But where men were key instigators in starting up sites, women have contributed to sites' expansion and development, as is described in this study.
Characteristics of entry as academic staff
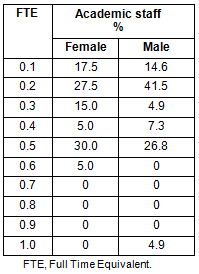
Many women entering the RCSWA were initially recruited as student mentors and supervisors on a casual basis. Based on an attraction to teaching, and the workability of flexible arrangements, a proportion of these women progressed to university appointments as part-time medical coordinators (MCs). As academic staff, female MCs taught full-time equivalents (FTE) that were indistinguishable from their male counterparts (t=1.0 p=0.295), as is shown (Table 1). Their time committment contributed to the development and expansion of The RCSWA.
Table 1: Percentage of male and female academic
Rural Clinical School of Western Australia
staff according to full time equivalent fractions
Characteristics of on-going academic workforce
Since its inception The RCSWA has employed 40 women specifically as site medical coordinators, compared with 41 men employed as MCs. The majority of both were GPs/ primary-care doctors. The current proportion of female to male GPs in rural Western Australia is 36.5%17. The RCSWA ratio of female to male academics was significantly higher than the rural workforce at large (χ²=4.0 p=0.046), with a relative risk of 1.28, CI 1.0-1.64.
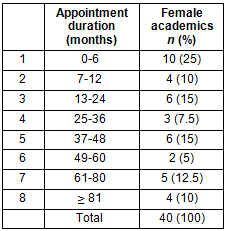
The average period worked by female MCs was 34 months (2.8 years). Shorter-duration appointments have accrued as The RCSWA continued to grow; nevertheless, 50% of women worked more than 2 years, and nearly one-quarter, 22.5%9 were employed for five or more of the 10 years The RCSWA has been in operation (Table 2). The period of tenure was indistinguishable between male and female MCs (t=1.19, p=0.24).
Table 2: Duration of women's appointments since
commencement of the Rural Clinical School of
Western Australia (June 2002-January 2012)
Of the women employed, 28% temporarily exited the workforce to have a child11. Of these, three exited more than once. All female doctors have returned to work in The RCSWA following parental leave. Most returned to their original appointment; however, two returned to a new, adjusted role. A number retained their RCSWA roles while taking leave from other work, allowing on-going participation in the workforce.
Vocational characteristics
Given that the rural workforce is strongly biased towards general practice, it is not surprising that 80.5% of female academic staff in RCSWA were GPs. However, a selection of disciplines more commonly found in rural practice were also represented by RCSWA women: district medical officer (general hospital doctor), paediatrics, obstetrics & gynaecology, and emergency medicine.
Local origin
The surveyed Western Australian rural GP workforce consisted of 48% Australian-trained medical graduates in 201117. In contrast, 78% (31 of 40 women) of The RCSWA's female academic staff was Australian trained. Relative to the workforce at large, the likelihood of being Australian trained in The RCSWA was 1.62 (CI 1.3-2.0), χ²=19.3, p=0.000. Of these Australian-trained women, most of whom were GPs and belonged to the surveyed demographic, 42%13 were even more locally trained, being graduates of The University of Western Australia. Of these local women, three had been educated in The RCSWA as undergraduates.
Site leadership
Leadership was divided equally between male and female doctors, with 7 of 13 RCSWA sites headed by a woman doctor who employed local colleagues to assist with teaching. Large, medium and small towns and health services, including work in Aboriginal Medical Services, were equivalently represented by this female leadership. The concentration of female-led sites in the most remote northern service areas in Western Australia is shown (Fig1).
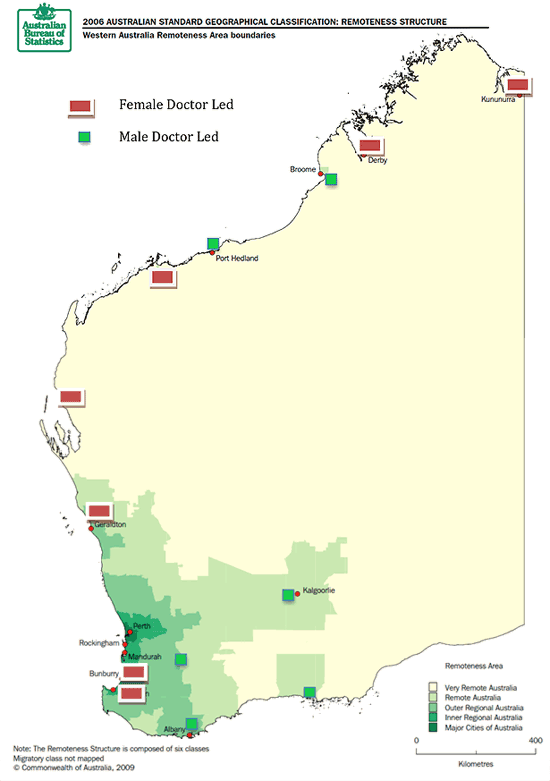
Figure 1: Geographical Distribution and Remoteness of Female-led sites, 2009. Map reproduced
with the permission of Australian Bureau of Statistics Australian Statistical Division)18.
Discussion
The single outstanding point of this workforce data is the confirmation of significant numbers of women relative to men in rural academy. This is in contrast to the shortage of female rural doctors generally practising in Western Australia, and indicates that female doctors have enabled teaching to develop in a work environment that is significantly underserviced. In this context of rural and remote workforce shortages, the Rural Clinical School appears to be providing a viable female workforce model. The dominance of female-led sites in the most remote regions of Western Australia is particularly indicative of this success.
The ideals of flexibility and part-time arrangements are part of the design of The RCSWA workforce model. Part-time practice is central to rural female rural doctors' satisfaction, as described in a Delphi study inquiry into sustainable practice15. Of successful strategies for female doctors, 'establishing personal and professional boundaries' was found to be key. The part-time Rural Clinical School contract, intended to enable clinical practice alongside teaching, was clearly consistent with these women's priorities.
The workforce model stands in contrast to the usual academic research and teaching workload, which is generally added to full-time practice, an arrangement which is particularly untenable for mothers2. For this reason women have been categorised as 'least-promoted' in academic medicine1. However, given the funding arrangements for Rural Clinical Schools to appoint at the appropriate level of seniority, and the particular equity principles at the university, there are no appointment differentials in either pay or seniority between male and female academic staff for The RCSWA. Here, the idea of women being part of the workforce mainly to do 'the grunt work'13 is clearly not applicable, since women head RCSWA sites in proportion to their rates of employment.
The leadership equity observed in The RCSWA is in agreement with a British study which demonstrated that, in the UK hospital system, women assume positions of leadership in proportion to their ratio in the workforce19. While elsewhere, child-bearing and family commitments systematically reduce this ratio6, the present study has showed that women were well retained in The RCSWA workforce. This enabling of women to be retained in the rural workforce has clear implications for rural female leadership. Strong female headship in the most remote areas of Western Australia suggest that there are no geographical limitations to women doctors being leaders.
The fact that operation of a Rural Clinical School represents promotion in rural practice should also be considered an important distinguishing characteristic, particularly for general practice where promotional characteristics are otherwise very 'flat'.
Women and men appear to have developed different roles in The RCSWA. Where men have been key instigators in the time-intensive effort of starting up sites, women have participated in sites' ongoing development. This may be concordant with an American study of part-time female physicians, which identified women to be 'working differently', particularly focusing on quality rather than quantity of work. In this sense, the attraction of high proportions of locally trained female academics augers well for the on-going sustainability of a quality-focussed teaching workforce.
The fact that women are attracted to the essential characteristics of general practice - its flexible, private arrangements and relational focus - make general practice a key collaborative partner in increasing the representation of women in Rural Clinical School teaching. But insofar as part-time work is attractive to female practitioners, more thought must be given to developing the same flexible engagement in hospital-based disciplines. For as in general practice, women in hospital-based disciplines are under-represented in regional Australia.
Women in the rural workforce have embraced the part-time teaching role. Their participation as academics is high relative to the low percentage of female rural doctors. They have assumed responsibility for site leadership, including at the most remote sites. They have played a critical role in developing the reputation of the Australian Rural Clinical Schools as a high quality teaching initiative. In short, female doctors who are willing to take on part-time work are supporting the rural teaching workforce.
References
1. Reichenbach L, Brown H. Gender and academic medicine: impacts on the health workforce. BMJ 2004; 329(7469): 792-795.
2. Allen I. Women doctors and their careers: what now? BMJ 2005; 331: 569-72.
3. Joyce CM, Stoelwinder JU, McNeil JJ, Piterman L. Riding the wave: current and emerging trends in graduates from Australian university medical schools. Medical Journal of Australia 2007; 186: 309-312.
4. Flanagan KC. Medical Training Review Panel Fifteenth Report. Canberra, ACT: Commonwealth of Australia, 2012.
5. Quadrio C. Women and men and the medical workforce in Australia. Medical Journal of Australia 1997; 166: 7.
6. Buddebery-Fischer B, Stamm M, Buddeberg C, Bauer G, Hammig O, Knecht M et al. The impact of gender and parenthood on physicians' careers - professional and personal situation seven years after graduation. BMC Health Services Research 2010; 10: 40-50.
7. Wainer J. What is it about women doctors? (Online) 2011. Australian Review Of Public Affairs. Available: http://www.australianreview.net/digest/2011/10/wainer.html (Accessed 12 June 2013).
8. Young AF, Dobson AJ, Byles JE. Access and equity in the provision of general practitioner services for women in Australia. Australian and New Zealand Journal of Public Health 2000; 25(5): 474-480.
9. Jong KE, Smith DP, Yu XQ, O'Connell DL, Goldstein D, Armstrong BK. Remoteness of residence and survival from cancer in New South Wales. Medical Journal of Australia 2004; 180: 618-622.
10. Ozolins I, Greenwood G, Beilby J. Keeping women doctors in the country. Rural and Remote Health 4:268. (Online) 2004. Available: www.rrh.org.au (Accessed 12 June 2013).
11. Tolhurst H, Talbot JM, Baker L. Women in rural general practice: conflict and compromise. Medical Journal of Australia 2000; 173: 119-120.
12. AMWAC. Toward gender balance in the Australian medical workforce: some planning implications. Australian Health Review 2000; 23(4): 27-42.
13. Levinson W, Lurie N. When Most Doctors Are Women: What Lies Ahead? Annals of Internal Medicine 2004; 141(6): 471-474.
14. Harrison CM, Britt HC, Charles J. Sex of the GP - 20 years on. Medical Journal of Australia 2011; 195: 192-196.
15. Wainer J, Strasser R, Bryant L. Sustainable practice: successful strategies from male and female rural doctors. Melbourne, VIC: Monash University School of Rural Health, 2004.
16. Heiligers P, Hingstman L. Career preferences and the work-family balance in medicine: gender differences among medical specialists. Social Science & Medicine 2000; 50: 1235-1246.
17. Rural Health West. Minimum Data Set Report and Workforce Analysis Update. Perth, WA: Rural Health West, 2011.
18. Australian Bureau of Statistics. Australian Standard Geographical Classification: Remoteness Structure, Western Australia Remoteness Area Boundaries. Map. Canberra, ACT: ABS, 2006.
19. Kvaerner K, Aasland OG, Botten GS. Female medical leadership: cross-sectional study. BMJ 1999; 318(7176): 91-94.

