The chronic shortage of doctors in rural Australia has been well documented. Enabling medical students to undertake positive rural experiences during their undergraduate course is a well-supported long-term strategy to provide a sustainable solution to this problem1. The Riverland Parallel Rural Community Curriculum (PRCC) in South Australia is an innovative example of this undergraduate strategy supported by an Australian Commonwealth Government grant2.
The PRCC was developed in 1997 by Flinders University, South Australia, to enable senior medical students to undertake an entire clinical year based in rural general practice in the Riverland region of South Australia. The academic success of this program has been widely acknowledged3-5. Many institutions are planning to use this model as a basis for their own curriculum reform. However, questions have been asked as to how much of this success was due to the distinctive character of the Riverland region, and how well this program would translate to other regions of Australia.
In the Riverland PRCC program, students learn by taking an active longitudinal role in the care of patients who come through the door of the general practice and may, or may not, be admitted to hospital of referred for specialist care. The aim of this program is to allow students to work with a patient-centred focus, where they follow patients through the continuum of health services from presentation in primary care to hospital inpatient care and return to the community.
The Riverland PRCC evaluations identified several components that work particularly well. Students have improved their examination performance in relation to their peers in the tertiary hospital6. One study suggested that the initial time commitment of rural general practitioner (GP) supervisors reaches a level where investment in students becomes time-neutral by approximately 13 weeks, and creates a net time-benefit for the remainder of the year7. Feedback from the Riverland GPs was positive and this correlates well with a study from London, UK, which suggested that GPs who teach have a higher morale8. Community stakeholder feedback has shown good patient acceptance, and the Riverland community has embraced this project4. Community acceptance has been clearly linked with the expectation that this program will have a positive impact on local GP workforce9.
Methods
New program development
With the success of this initial programme, and further funding opportunities through the Commonwealth Government, Flinders University embarked on translating this program to the Greater Green Triangle (GGT) region. The GGT region, where the GGT PRCC program is based, is 450 km south-east of Adelaide, the South Australian capital city, and crosses the boarder between the States of South Australia and Victoria. The three towns of Millicent, Mt Gambier and Hamilton are involved in the program (Table 1).
Table 1: Greater Green Triangle towns involved in the Parallel Rural Community Curriculum
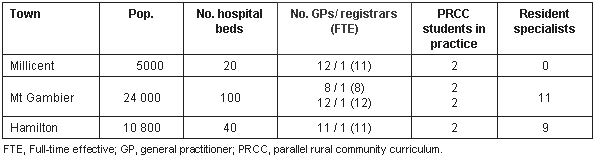
In 2002, Millicent was a town with a population of 5000, 50 km west of Mt Gambier. There was one general practice in the town with 11 full-time equivalent (FTE) doctors and one solo GP not involved in the PRCC program. Mt Gambier was the central town in the proposed GGT PRCC area and had a population of 24 000. There were two practices with 8 FTE and 12 FTE doctors respectively, each with capacity for two PRCC students. There was also one solo GP not involved in the PRCC program and 11 specialists (anaesthetists, general and orthopaedic surgeons, gynaecologists, physician and a paediatrician) with variable involvement. Hamilton, 110 km east of Mt Gambier, had a single medical practice which combined three physicians and 11 FTE primary care doctors. There were six other resident specialists with variable involvement in the PRCC program. There was a hospital in each of the three towns involved in the PRCC program.
The local academic (0.5 FTE) and administrative support staff (1.1 FTE) for the program were based in Mt Gambier. The local academic worked full time during the 6 month set-up phase and the first 6 months of the student program. Prior to this there had been 18 months of initial lead time when academics from Flinders University visited regularly to engage stakeholders.
As a consequence of the partnerships with the above mentioned general practices and hospitals, seven year-3 graduate-entry medical program students were based in the GGT in 2002. Their learning program was based on the Riverland model (Fig 1).

Figure 1: Greater Green Triangle, Parallel Rural Community Curriculum student activities.
Student activities amounted to approximately 6-8 structured sessions per week, depending on the nature of their on-call; as well as ad hoc clinical encounters in the remaining in-hours sessions. In some sites students were able to participate in existing regular educational and continuing professional development activities, for example journal clubs or radiology meetings. At one site, the PRCC was responsible for the commencement of a journal club for doctors, registrars and students.
Student results
The seven students in the 2002 program achieved five distinctions and two credits for their overall result in year-3 examinations. This represented a mean student rank improvement of 17 places out of a class of 90 from the end of year-2 examinations prior to the PRCC, to the end of year-3 examinations at the conclusion of the PRCC year. While there were numerous potential confounders that must be considered in interpreting these results, such as the Hawthorne effect of the first year of a program and selection biases, these results were similar to the trend obtained by the Riverland program over the previous 5 years.
Evaluation methods
In order to determine the significant events and issues involved in achieving the translation of the PRCC program from the Riverland to the GGT, a thematic analysis of the following data was undertaken using an action research approach. Data sources included the notes kept by the authors throughout the development phase and the first academic year of the program, the support resources developed during the recruitment process, and the annual work plans employed to establish the program. The three authors had different roles in the development of the GGT program: initiator of the Riverland program (PW), interim director in the GGT involved in stakeholder engagement (BM), and the local academic employed to establish and coordinate the program (LW).
Results
Establishing partnerships
General practitioners: General practitioners were initially recruited through personal networks following multiple visits to practices to meet with the doctors as a group and on an individual basis.

Figure 2: Agreed expectations of general practices and Flinders University.
GPs with previous teaching experience who indicated some enthusiasm for the program were initially approached with the view to finding a 'GP champion' in each of the four practices where the PRCC students were to be placed. In each practice, the GPs initial worries included concern about time, clinical exposure, the organization of the program, and the infrastructure needs of their practice in order to support students. Once these initial concerns were worked through, a letter of understanding was developed clearly stating the roles and responsibilities of both the GP and the University (Fig 2). The academic staff responsible for developing the program worked hard to acknowledge GP anxiety and then presented to GPs the evidence available regarding Community Based Medical Education programs and in particular the experience of the Riverland PRCC program. Enthusiasm for the program developed relatively quickly, and many GPs rapidly embraced the concept of the PRCC program.
Specialists: In a similar way to GPs, specialists were initially recruited through personal networks. The resident proceduralist specialists within the GGT were cautious about adopting the paradigm changes required in order to embrace the PRCC program. The specialists had previous experience of students shadowing them for periods of time ranging from one to 6 weeks. Specialist anxieties differed from GP anxieties (Fig 3).
The specialists also expressed concern regarding the transfer of loyalties to another university's students, but were anxious not to increase their total teaching time. Procedural specialists, in particular, expressed concern that their speciality area would not be given enough weighting if students, lead by GP supervisors, took responsibility for their own learning. Non-proceduralist engagement has paralleled more closely the partnership development of GPs.
The GGT PRCC has worked to remain flexible to allow for clinicians to move in and out of the program depending on clinical and personal commitments. Some but not all specialists embraced these opportunities to become involved in the program. Speciality area teaching not covered by local clinicians has been delivered by distance education or visits by city-based academic staff.

Figure 3: Initial concerns of regional specialists about the Parallel Rural Community Curriculum.
Local Hospitals: As medical students in the PRCC follow patients rather than doctors, there was some difficulty in working through the medical and legal implications of student access to local hospitals, particularly concerning clinical supervision and student indemnity. Hospitals in the region worked through these issues effectively allowing appropriate student access. One hospital in the region expressed the partnership with the university through creating a clinical academic position in internal medicine. Allied health professional (AHP) involvement included student attachments for half-day sessions with some of the hospital-based AHPs. These sessions where viewed with some concern by the AHPs, and feedback from students suggested they found many of these sessions lacked meaning due to the absence of clear learning objectives or opportunitites to be actively involved. Some AHPs expressed feelings of being undervalued and were keen to formalise their contribution with tutorials or other formal teaching sessions. It was agreed by the GP supervisors that more work was needed to provide meaningful AHP teaching/exposure within the patient-centred paradigm of the program.
Community stakeholders: Several of the local government councils in the GGT region embraced the PRCC program as an answer to the medical workforce crisis in their local rural area. One municipal council collaborated to develop sustainable student housing. It was important to be honest with the community regarding student commitments to the PRCC program. There was no binding requirement for the PRCC medical students to return to the region. Students reported that local community members supported the program at a social level by assisting them to settle in and become part of the broader community.
Successes and pitfalls
From the initial evaluation of the 2002 GGT PRCC program it is clear that some aspects worked well (Fig 4). In particular, the positive student feedback and examination performance in the initial year of the program was very important for all involved. There were some significant pitfalls, which are important to highlight for any region considering the development of a similar program. Partnership development took time. General Practitioners showed significant anxiety initially in regards to their teaching capacity, time commitment of students, and the infrastructure demands on their practices. Specialists' engagement was a challenge initially, requiring a significant change to their teaching paradigms. Horizontal and vertical integration of teaching was complex and required ongoing effort to maximize efficiency. The community had high expectations of the workforce outcome and these needed to be tempered with realistic expectations of the length of time required to train doctors, and the understanding of workforce mobility.

Figure 4: Successes and pitfalls of the Parallel Rural Community Curriculum.
Discussion
An account of issues faced and the measure of success of any community based medical education program will differ depending on the perspective of the stakeholder. The main stakeholders involved in developing the GGT PRCC included the university, the clinicians, and the broader community represented by organisations such as local health services and councils. The importance of the development of symbiotic relationships between the various stakeholders in community-based medical education has been described elsewhere10,11.
From the university's perspective, the major objective was the capacity for students to achieve a similar quality of medical education. Initial student results mirrored the success of the Riverland PRCC, however more work needs to be done to assess the student perspective, particularly as the student cohort changes and students begin to choose the PRCC option because of its reported academic success, rather that due to their own rural interest.
Partnership establishment with all clinicians relied on the University recognising that clinical service provision and other personal needs take precedence over teaching roles and responsibilities. Even for the GP champions within each clinic, the tension between their clinical and small business commitments, and the enjoyment of teaching must continue to be acknowledged by the university. Time-poor GPs who enjoyed teaching expressed concerns regarding the administrative burden the PRCC program could create, and so they saw the local program coordinating team's main role was to work to minimise this burden on their behalf. Financial constraints affected even the keenest clinical teachers who were required to balance their enthusiasm for the program development with the clinical, financial and contractual obligations they had with their practice business partners. Establishing partnerships between the university and GPs was less complicated where clinics had clear governance processes allowing clinic doctors to decide upon the extent of involvement in the program as a unit. Although some information is available regarding the financial and time impact of having medical students in a PRCC long-term mentorship model7, more research has to be undertaken to define the actual impact medical students have on their GP supervisors, rather than relying on GP perceptions.
Specialist proceduralists who have higher incomes relative to GPs expressed less concern regarding the financial implications of taking on students. Many resident specialists within the GGT were more cautious about adopting the paradigm changes required in order to embrace the PRCC program. The specialists had previous experience of students shadowing them for periods of time ranging from one to 6 weeks. During these attachments, specialists had been responsible for delivering the content of the curriculum and for the range of clinical exposure to which the students were presented. The PRCC model embraces adult education principles and required a pedagogical shift because students followed patients throughout the hospital and had patients from different clinical specialties in the hospital and clinics at any one time. Students described having multiple clinical opportunities at any one time and, like rural health professionals, needed to make choices about which opportunities they became involved in. They learned to keep committed appointments and to take advantage of other clinical opportunities as they presented. In the PRCC program, students, rather than clinicians, were responsible for covering the curriculum.
Community interest in the GGT PRCC program steadily increased with significant human and financial resource contribution in the first 12 months. These partnerships created significant challenges for the university. Transparency on future workforce deliverables was imperative, but local enthusiasm threatened, at times, to drown this cautionary message. Community ownership of the GGT PRCC was reflected in the financial contribution of health services and councils, the social inclusion of medical students at a personal level, and the high rates of patient acceptance. Patients not only consented to students being present during consultations, but on many occasions, sought out 'their' student as an active member of their healthcare team.
Conclusions
These data suggest that the Riverland PRCC is translatable. Successes, including student performance, GP acceptance and community ownership have been replicated in the GGT. Partnership development with local stakeholders was the key to successful development of this community based medical education program. Despite this success, there is a need for more research into the needs, expectations, and responses of GPs, specialists, health service organisations and the broader community involved in this and similar programs as medical schools increasingly move toward community-based initiatives to address both academic and workforce priorities.
References
1. Worley PS, Prideaux DJ, Strasser RP, Silagy CA, Magarey JA. Why we should teach undergraduate medical students in rural communities. Medical Journal of Australia 2000; 172: 615-617.
2. Worley P, Silagy C, Prideaux D, Newble D, Jones A. The Parallel Rural Community Curriculum: an integrated clinical curriculum based in rural general practice. Medical Education 2000; 34: 558-565.
3. Newble D, Sidford S. Flinders University School of Medicine Parallel Rural Community Curriculum Evaluation Report. Woodville, South Australia: Clinical Education Development Unit, Queen Elizabeth Hospital, 1998.
4. Oswald N. Flinders University of South Australia Parallel Rural Community Curriculum Final Evaluation Report to the Commonwealth. Mt Gambier, South Australia: Greater Green Triangle University Department of Rural Health, 2003; 2.
5. Lines DR, Forsyth K, Worley PS. Teaching undergraduate paediatrics in a rural community. Focus on Health Professional Education: A Multi-Disciplinary Journal 2000; 2: 25-30.
6. Worley P. The immediate academic impact on medical students of basing an entire clinical year in rural general practice. [PhD Thesis]. Flinders University, South Australia.
7. Worley P, Kitto P. A Hypothetical Model of the financial impact of student attachment on rural general practice. Rural and Remote Health 1 (online) 2001: no 83. http:rrh.org.au (accessed 31 October 2003).
8. Hartley S, Macfarlane F, Gantley M, Murray E. Influence on general practitioners of teaching undergraduates: qualitative study of London general practitioner teachers. BMJ 1999; 319: 1168-71.
9. Nelson J. The parallel rural community curriculum: what a mouthful. Commonwealth Department of Health and Aged Care, National Networks 2000; 9. [Newsletter]
10. Worley P. Relationships: A new way to analyse community-based medical education? Part 1. Education for Health 2002; 15: 117-128.
11. Worley P. Integrity: the key to quality in community-based medical education? Part 2. Education for Health 2002; 15: 129-138.
Footnote
Published 5 November 2003; modified 27 November 2003.
Abstract
Background: The chronic shortage of doctors in rural Australia has been well documented. Enabling medical students to undertake positive rural experiences during their undergraduate course is a well-supported long-term strategy to provide a sustainable solution to this problem. The Parallel Rural Community Curriculum (PRCC) was developed by Flinders University, South Australia, in 1997 to enable senior medical students to undertake an entire clinical year based in rural general practice in the Riverland region of South Australia. The academic success of this program has been widely acknowledged. Many institutions are planning to use this model as a basis for their own curriculum reform. However, questions have been asked as to how well this program would translate into another region. Due to the success of the Riverland program, Flinders University decided to commence a second PRCC program in 2002, this time in the Greater Green Triangle (GGT) region of South Australia and Victoria, Australia. This new program was developed collaboratively by the GGT University Department of Rural Health and the Flinders University Rural Clinical School.
Results and Discussion: The mean student rank improved by an average of 17 places out of a class of 90 students. Partnership development took time. General practitioners (GPs) initially showed significant anxiety particularly in regard to their teaching capacity, time commitment of students and the infrastructure demands on their practices. Specialists' engagement was a challenge, requiring a significant change to their teaching paradigms. Horizontal and vertical integration of teaching was complex and required ongoing effort to maximize efficiency. The community had high expectations of the workforce outcome and these needed to be tempered with realistic expectations about the length of time required to train doctors, and an understanding of workforce mobility.
Conclusions: The initial evaluation of the GGT PRCC suggests that the Riverland PRCC is translatable. Successes, including student performance, GP acceptance and community ownership have been replicated in the GGT community-based medical education program. A key to the success has been the recognition of the crucial role of partnerships in an environment where, for clinicians, clinical service provision and other personal needs take precedence over teaching roles and responsibilities.
Key words: community-based medical education, curriculum reform, general practitioners, Riverland, South Australia, undergraduate.



