Leptospirosis is a widespread zoonotic disease that is recognized as an emerging global public health problem due to its increased incidence in both developed and developing countries1,2.
There is evidence that leptospirosis exists as an endemic disease in temperate countries like Germany and in Asian countries such as China, Korea, Vietnam, Cambodia, Laos, India, Indonesia, Bangladesh, Nepal and Thailand. Major recent outbreaks of leptospirosis have been reported from India and Indonesia3-9.
Traditionally a disease of farmers10, leptospirosis was formerly considered a disease affecting adults. However, cases of leptospirosis have also been reported in children, particularly in agricultural countries where children are involved in rice farming11-13.
Leptospirosis has become a major public health problem in Sri Lanka. The first human case was reported in 195314. Despite implementation of many strategies to prevent and control the disease among high risk groups, cases have been increasing. In 2008, Sri Lanka experienced its largest outbreak of leptospirosis in history with 7423 cases and 207 deaths14. In 2011, 6613 cases and 89 deaths were reported by the Epidemiology Unit of Sri Lanka. The most severely affected area was the district of Kurunegala, where 1574 cases and 10 deaths were reported15. Surveillance data showed that of the 686 cases detected in 2011, 8 (1.2%) were among 0-9-year-olds, 21 (3.1%) were among 10-19-year-olds and 65 (9.5%) were among 20-29-year-olds16.There is evidence that children from farming families drop out of school to help with farm work, especially during the harvest season17. This information suggests that more attention should be paid to the risk of leptospirosis among children living in rural agricultural areas.
Leptospirosis has been a grossly neglected disease and increasing awareness is essential to identify the disease burden in a society18. Knowledge of the disease and healthy behaviours are crucial in preventing leptospirosis. Thus, there is a direct need to assess the level of knowledge and extent of risky practices among the Sri Lankan population, particularly in rural areas. Previous studies have shown a lack of such knowledge among adult populations19,20. A formal assessment of awareness and knowledge of leptospirosis among Sri Lankan school children has yet to be carried out.
Kurunegala is a prominent agricultural district in Sri Lanka21 that is affected by leptospirosis throughout the year. The highest reported case load in 2011 was observed in Galgamuwa, a rural area within the Kurunegala district. The total population of Galgamuwa is 54 910, which includes 15 371 children under the age of 15 years. A majority of the population consists of Sinhala (50 668), Buddhists (50 351) followed by Muar and Tamils22. The potential risk for disease is high among children in this area due to recreational and high risk water activities. In addition, many of these adolescents will eventually become farmers. This study was conducted to assess the knowledge and high risk practices regarding leptospirosis among school children in Galgamuwa, Sri Lanka.
This was a descriptive cross-sectional study conducted in Galgamuwa educational division during the period 1 May 2011 to 31 December 2011. The study population included all school children in grades 9 and 10 from any of the three categories of government school in Galgamuwa educational division: Type 1 AB, 1C and Type 2 schools.
Sample size was calculated as 384 using the following Lwanga and Lemeshow formula23:
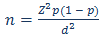
where:
n = sample size
Z = standard normal deviation for specified alpha error, usually set at 1.96 which corresponds to 95% confidence limit, alpha error considered as 5%
p = expected prevalence of 'good' level of knowledge regarding leptospirosis among grades 9 and 10 school students (In the absence of this information, this was taken as 50% to get the maximum sample.)
d = degree of accuracy (precision), which was set at 0.05.
A sample size of 384 would allow estimation of the prevalence of 'good' level of knowledge, with 95% confidence and precision of 0.05. As cluster sampling was used, the sample size was multiplied by the design factor, taken as 1.1 to overcome the design effect. With the correction, calculated sample size was 422. A non-response rate of 5% was allowed. Therefore, the final sample size was 422 + 21 = 443 students.
A stratified cluster sampling technique was used. In the first stage of sampling, two schools from each of the three school categories were selected randomly. A class with 20 students in grade 9 or 10 was considered as a cluster, considering the minimum number of students in a class of grade 9 or 10. The number of clusters allocated to the schools was based on the proportion of grade 9 and 10 students in each type of school. An equal number of clusters were allocated to similar types of schools. In the next stage, the classes of grade 9 and 10 were listed and the required number of clusters was selected randomly from the list. In classes with more than 20 students, random selection was done from the class register. Once the cluster was selected, all the students in that class were invited to participate in the study. Out of the 2054 targeted students in the region 460 (22.4%) students were selected for the study. Parents were provided with an explanation of the purpose and the nature of the study, and asked to consent to their children's participation. As a population affected by leptospirosis, the parents were generally interested in the study. All parents contacted gave informed consent to their children's participation. All students in the sample were present on the days of data collection.
A structured, pretested, self-administered questionnaire with three sections was used. The first section collected basic demographic and social data. The second section had questions about knowledge of leptospirosis, including the distribution of the disease and trends, the disease agent, animals that can transmit the disease, mode of transmission, high risk groups, basic clinical features, complications of the disease, and methods of prevention and control. The students were also asked about the sources of their information. High risk behaviour related to leptospirosis was assessed in the third section; questions related to the respondent's involvement in agriculture work, use of protection wear, personal hygiene, rodent control, handling of cattle, pattern of recreational activities, prophylaxis, perceived barriers for the current practices and health seeking behaviour regarding leptospirosis. The Government of Sri Lanka offers doxycycline prophylaxis treatment free of charge to the farmer families in this study setting. In the questionnaire students were asked whether they knew the method of taking a 'drug' to prevent leptospirosis. This was taken as awareness of prophylaxis treatment.
'Frequently' was defined as involvement in paddy cultivation or use of gloves and boots or washing and bathing in stagnant water pods once or more than once a week and 'rarely' was defined as being involved in these activities less than once a week. For the purposes of logistic regression analysis, students who were involved in paddy cultivation 'rarely' and 'frequently' were amalgamated as one category against the category of students who had 'never' got involved in paddy cultivation activities. The decision to combine the 'frequently and 'rarely' categories together was to create a category of 'involved' against 'non-involved'.
All the questions related to practices were limited to the practices at the time of data collection or during the recent past. The life events inquired into were major events of a life of an adolescent. These precautions were to minimize any recall bias in the information collected. Social-desirability bias was unlikely because all participants were rural children from farming villages. However, the questionnaire included a statement stating that farming is an accepted practice in rural Sri Lanka, prior to the questions about participants' involvement in farming.
The test-retest method was used to assess the reliability of the questionnaire. One week after data collection in the first school, selected significant questions with responses in categorical form were administered again to a group of randomly selected 50 adolescents who participated in the main study. Test-retest reliability of these categorical variables was assessed using Cohen's kappa coefficient24, and the minimum was 0.76 for the variables included.
Data was collected during the period of July and August 2011, when students had completed their second term examinations.
The Statistical Package for Social Sciences v17.0 (SPSS; http://www-01.ibm.com/software/analytics/spss) software was used for data analysis. Sociodemographic characteristics of the study population were described using frequency distributions. Knowledge level was assessed by scoring each question. The minimum score was 0 and maximum 91. Each correct response to knowledge questions received one mark, while incorrect responses or 'do not know' were given a score of zero. Prior to data analysis an expert panel defined a 'good' level of knowledge about leptospirosis as a score of 60% or more. A respondent accurately responding to all the questions assessing 'core' knowledge would have obtained a score of 60% and that was the basis for this cut-off. Core questions related to the main animal responsible for transmitting leptospirosis, the modes of entry of the organism to the human body, population groups at higher risk of getting leptospirosis and the places that are likely to promote transmission of leptospirosis, common initial symptoms of leptospirosis, practices to be adopted to prevent the disease occurring including prophylactic drugs and what one should do if a person is suspected to have leptospirosis. The non-core questions related to the type of causative agent, distribution and trend of rat fever in the country, distribution and trend of rat fever in their own area and to complications of leptospirosis.
Involvement of parents and other family members in paddy cultivation, involvement of students in paddy cultivation and use of personal protective practices by students with the student's knowledge on leptospirosis was assessed using the χ2 test. Logistic regression analysis was performed to assess adjusted odds ratios (OR) and 95% confidence intervals (CI) of factors predicting leptospirosis preventive practices among students.
Ethics approval
Prior to data collection written authorization was obtained from the Zonal Education Director, Maho. The school principals gave verbal permission. An information sheet about the study was given to every parent or guardian. They were informed of their right to decline their child's participation or withdraw from the study, the measures to maintain confidentiality, and that all information would be used only for research purposes. The parents gave informed written consent. Ethical clearance was obtained from the Ethical Review Committee, Faculty of Medicine, Ragama, Sri Lanka; ethics approval number FWA00013225.
Sociodemographic characteristics and involvement in paddy cultivation
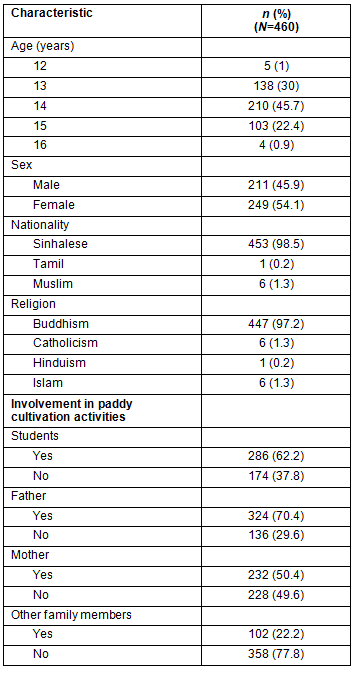
The study included 460 subjects with a response rate of 100% (460/460). Sociodemographic characteristics of the study population and details of involvement in paddy cultivation activities by the students themselves, their parents and other family members are presented in Table 1. A total of 271 students (58.9%) were studying in grade 9 and 189 (41.1%) in grade 10. The mean age of the study population was 13.9 years (standard deviation (SD) 0.8 years) and 249 (54.1%) were female. The majority were Sinhalese (98.5%, n=453) and Buddhists (97.2%, n=447). A total of 286 (62.2%) students were involved in paddy cultivation activities either frequently or rarely. A total of 102 (22.2%) students reported that their family members were involved in paddy cultivation. Most fathers (70.4%, n=324) were involved in paddy cultivation, while half of the mothers (50.4%, n=232) were also involved.
Table 1: Sociodemographic characteristics of the sample and details of involvement in paddy cultivation activities
Prevention knowledge and practices at the personal and household level
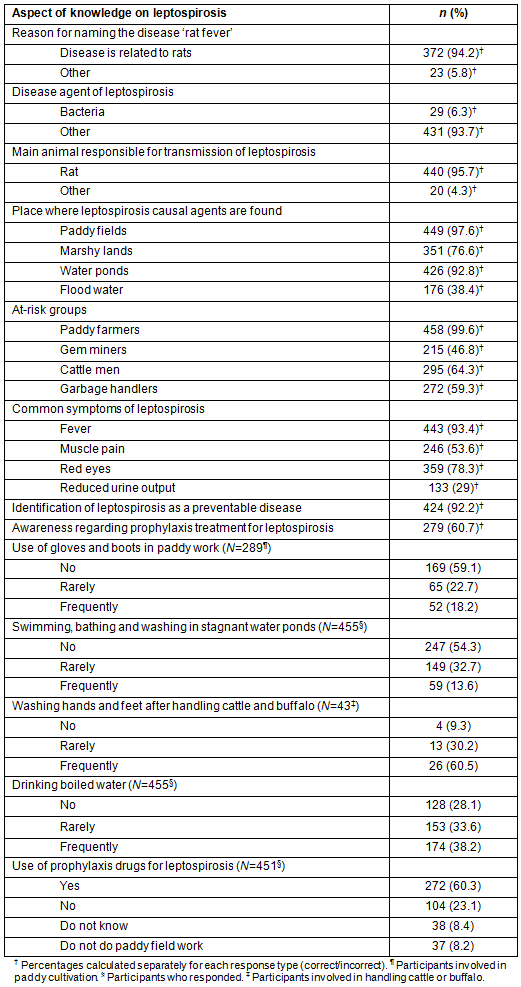
The students were asked about several aspects of knowledge regarding leptospirosis as well as practices regarding prevention of leptospirosis at the personal level and household level. The frequency distributions are presented in Table 2. All students had heard of leptospirosis (100%, n=460) and 99.6% (n=458) identified paddy farmers as a high risk population. The question on 'reason for naming the disease as rat fever' was answered only by 395 students with 65 students not responding to this question (94.2%). Only 29 (6.3%) students identified bacteria as the disease agent. The other question asked was about the main animal responsible for transmission of leptospirosis. This was answered by 460 students, and 440 (95.7%) identified the rat as the main animal. A total of 449 (97.6%) identified paddy fields as a place where leptospirosis transmission occurs while 351 (76.6%) identified marshy lands. A total of 99.6% (n=458) had identified paddy farmers as a high risk population. The majority (93.4%, n=443) identified 'fever' as a common symptom of leptospirosis. Almost all (92.2%, n=424) identified leptospirosis as a preventable disease, and a majority (60.7%, n=279) was aware of prophylaxis treatment for leptospirosis.
Among the students who were involved in paddy cultivation, only 117 (40.9%) had used gloves and boots when engaged in paddy cultivation and only 18.2% (n=52) used them 'frequently'. Moreover, 209 (45.7%) students reported that they swim, bath and wash in stagnant water ponds either frequently or rarely. The respondents were also asked whether they handled cattle or buffalo. The majority (77.0%, n=354) did not have cattle or buffalo at home; only 43 (9.3%) ever handled cattle or buffalo. Among the students who did, 13 (30.2%) reported that they wash their hands and feet with soap 'rarely', and 26 (60.5%) reported that they wash 'frequently'. Most households (61.7%) were either not or rarely boiling their drinking water, and either not using or rarely using rodent control methods (88.7%). Regarding the use of prophylaxis for leptospirosis, a majority of the students (60.3%, n=272) reported that their family members have used prophylaxis drugs.
Table 2: Aspects of knowledge about leptospirosis and prevention practices at the personal and household level
The score for knowledge about leptospirosis ranged from 18 to 78. The mean knowledge score was 54 (SD 11.1). About half had a 'good' level of knowledge regarding leptospirosis (52.0%, n=239).
Among the students, 20 (4.3%) had stated that a family member had suffered from leptospirosis. Of these, 13 (65%) had taken the patient to the nearest hospital as soon as their symptoms appeared. This information was verified by contacting parents of these adolescents using the identification number. Family members of 11 students had diagnostic cards indicating laboratory investigations confirming leptospirosis. Family members of the other two had misplaced the diagnosis cards but inquiries into symptoms and signs indicated that the diagnosis was very likely to be leptospirosis.
Sources of information about leptospirosis and perceived barriers to using protective boots and clothing in paddy work
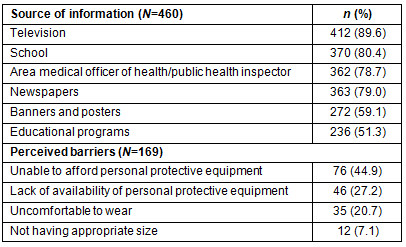
Common sources of information regarding leptospirosis were television (89.6%, n=412), school (80.4%, n=370), newspapers (79.0%, n=363), the medical officer of health or public health inspector (78.7%, n=362), banners and posters (59.1%, n=272), and educational programs (51.3%, n=236) (Table 3).
Students were also asked about barriers to the use of gloves and boots in paddy work. The commonest barriers mentioned were cost (44.9%, n=76), lack of availability (27.2%, n=46), discomfort (20.7%, n=35), and lack of appropriate sizes of protective clothing or boots (7.1%, n=12) (Table 3).
Table 3: Sources of information about leptospirosis and perceived barriers
Factors associated with knowledge about leptospirosis
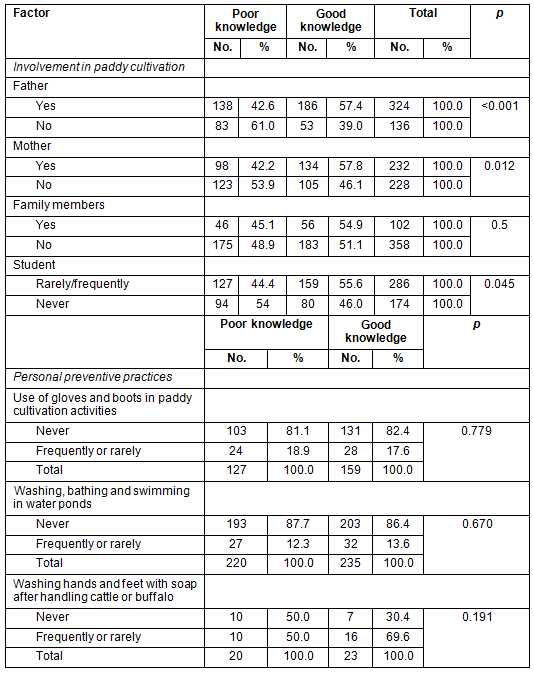
Factors significantly associated with a 'good' level of knowledge regarding leptospirosis are shown in Table 4. Results were based on the χ2 test. Among the students whose fathers were involved in paddy cultivation, 57.4% had a 'good' level of knowledge, while only 39.0% of the students whose fathers were not involved in paddy cultivation had a 'good' level of knowledge. Father's involvement in paddy cultivation was a factor associated with a 'good' level of knowledge among students (p<0.001). Similarly, mother's involvement in paddy cultivation was a factor associated with a 'good' level of knowledge among students (p=0.012). Among the students whose mothers were involved in paddy cultivation, 57.8% had a 'good' level of knowledge, while only 46.1% of the students whose mothers were not involved in paddy cultivation had a 'good' level of knowledge. Furthermore, 54.9% of the students who were involved in paddy cultivation showed a 'good' level of knowledge compared to 46.1% of the students who were not involved in paddy cultivation, indicating that student involvement in paddy cultivation was also a factor associated with 'good' knowledge (p=0.045). None of the personal protective practices were significantly associated with level of knowledge.
Table 4: Factors associated with a 'good' level of knowledge regarding leptospirosis
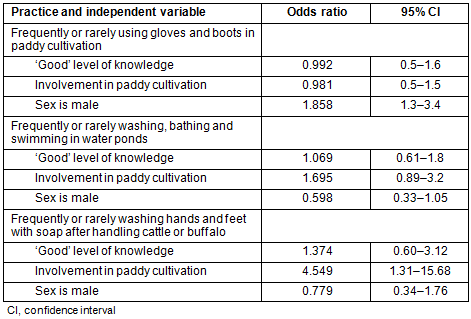
The results of logistic regression analysis for evaluating associations between selected variables and practices for preventing leptospirosis are shown in Table 5. Being a male (OR 1.9, 95% CI 1.3-3.4) was significantly associated with frequent use of gloves and boots in paddy cultivation, while being involved in paddy cultivation was significantly associated with frequent washing of hands and feet with soap after handling cattle and buffalo.
Table 5: Logistic regression analysis for evaluating associations
between selected variables and practices for preventing leptospirosis
Discussion
A majority of the students, fathers and mothers in this study population were involved in paddy cultivation activities. Though knowledge among many of the students was at a 'good' level, there were gaps in important areas of knowledge. The study identified factors that were associated with good knowledge. In contrast, findings related to knowledge and personal prevention practices were neglected by many adolescents.
The high level of involvement in paddy cultivation by the students and their parents is not surprising, given that Kurunegala district is an area of high paddy production21. In a cross-sectional descriptive study to assess knowledge regarding leptospirosis among rural villagers in a highly endemic area in Thailand, a majority of the villagers (84.0%) were farmers19. The fact that a high proportion of the population in the endemic areas are involved in paddy cultivation suggests that farmers are a high risk occupational group.
The high awareness of leptospirosis (100%) in this study contrasts with the findings of other studies25-27. Some of the results in the study are consistent with other studies such as identification of the disease agent28, identification of the rat as the main animal responsible in transmission of leptospirosis25, identification of paddy farmers as an at-risk group25, identification of 'fever' as a common symptom and awareness regarding prophylaxis treatment25. The identification of paddy farmers as an at-risk group in the present study can be attributed to the high level of involvement in paddy cultivation by the study population. The high proportion able to identify the common symptoms of leptospirosis in this study can be attributed to the high likelihood of them receiving education, as the study setting was an endemic area and the study population was at high risk of leptospirosis.
Among the study population, a 'good' level of knowledge regarding leptospirosis was found in 52% of the study population. A pilot test was performed using the same questionnaire with a sample of 50 students in a non-endemic area. A 'good' level of knowledge regarding leptospirosis was found only in 24% of the non-endemic sample, suggesting that the level of knowledge regarding leptospirosis among the school adolescents in this rural endemic area was satisfactory.
Among the participants, 4.3% of respondents reported that one of their family members had been afflicted with leptospirosis and of them 65% had received immediate care from the nearest hospital. This information, which was verified clinically and through review of medical records, can be used as evidence of high incidence of leptospirosis in the study setting. As shown in Table 2, preventive practices for leptospirosis were unsatisfactorily conducted compared with other studies26. Only 60% were using prophylaxis, which is less than the ideal usage rate for preventing leptospirosis. This highlights the need for improving the compliance to prophylactic treatment in the study area, as 99% coverage is needed for an intervention to be effective, such as immunization for preventable diseases28.
Level of knowledge about leptospirosis was significantly associated with parents' involvement in paddy cultivation, which is consistent with other studies19,25. These findings may indicate that education programs may be reaching only families involved in cultivation. This should be rectified because it is accepted now that those not involved in farming may also be at risk of the disease, especially in cultivation areas.
None of the personal prevention practices of the sample were significantly associated with level of knowledge. This suggests that knowledge alone is not sufficient to improve personal preventive practices. In this study the students were asked about barriers to the use of gloves and boots in paddy work. Unavailability of such equipment mostly due to cost was highlighted as a barrier. Lack of appropriate size and discomfort were the other barriers highlighted. Overcoming these requires actions at individual, local and government levels. Other than providing knowledge, the individuals would need to be motivated through behavioural change communication methods to promote use of gloves and boots in paddy cultivation activities. At local level, a mechanism to supply equipment of suitable sizes to adolescents, either free of charge or on a concessionary basis, would improve the situation. At national level, manufacturing boot and gloves of sizes that match the adolescents and suit the local weather conditions may improve practices.
In the present study, knowledge and practices about leptospirosis were assessed only among school-going adolescents. Non-school-going adolescents, who have a higher probability of being exposed to the disease due to paddy cultivation, were not assessed, limiting the ability to generalize these findings. Additionally, sources of drinking water were not assessed and personal prevention practices were obtained through self-report. Ideally, practices need to be evaluated through observation, which would have increased the internal validity of the study. Nevertheless, the data were validated and steps were taken to minimize biases.
The overwhelming majority of the adolescent school children in the rural paddy farming area of Galgamuwa, Sri Lanka, consider leptospirosis to be a preventable disease. However, this knowledge is not translated into preventive practice at an individual or household level. Some of the practices could be improved by the relevant authorities by addressing the perceived barriers, such as availability and affordability of protective clothing and boots.
References
1. Bharti AR, Nally JE, Ricaldi JN, Matthias MA, Diaz MM, Lovett MA, et al. Leptospirosis: a zoonotic disease of global importance. Lancet Infectious Diseases 2003; 3(12): 757-771.
2. Vijayachari P, Sugunan P, Shriram A. Leptospirosis: an emerging global public health problem. Journal of Bioscience and Bioengineering 2008; 33(4): 557-569.
3. Liverpool J, Francis S, Liverpool C, Dean G, Mendez D. Leptospirosis: case reports of an outbreak in Guyana. Annals of Tropical Medicine and Parasitology 2008; 102(3): 239-245.
4. Mcbride A, Athanzio D, Reis M, Ko A. Leptospirosis. Current Opinion in Infectious Diseases 2005; 18(5): 376-386.
5. David A, Robyn M, Richard A, Bradly A, Robbin S, Sandra L. Asymptomatic Infection and Risk Factors for Leptospirosis in Nicaragua. American Journal of Tropical Medicine and Hygiene 2000; 63(5,6): 249-254.
6. Jansen A, Schöneberg I, Frank C, Alpers K, Schneider T, Stark K. Leptospirosis in Germany, 1962-2003. Emerging Infectious Diseases 2005; 11(7): 1048-1054.
7. Victoriano A, Smythe L, Gloriani-Barzaga N, Cavinta L, Kasai T, Limpakarnjanarat K, et al. Leptospirosis in the Asia Pacific region. BioMed Central Infectious Diseases 2009; 9: 147.
8. Tangkanakul W, Smits L, Jatanasen S, Ashford A. Leptospirosis: an emerging health problem in Thailand. Southeast Asian Journal of Tropical Medicine and Public Health 2005; 36(2): 281-288.
9. Sehgal C, Sugunan P, Vijayachari P. Leptospirosis disease burden estimation and surveillance networking in India. Southeast Asian Journal of Tropical Medicine and Public Health 2003; 34(2): 170-177.
10. Cachay R, Vinetz J. A global research agenda for leptospirosis. Journal of Postgraduate Medicine 2005; 51(3): 174-178.
11. Karande S, Bhatt M, Kelkar A, Kulkarni M, De A, Varaiya A. An observational study to detect leptospirosis in Mumbai, India. Archives of Disease in Childhood 2003; 88(12): 1070-1075.
12. Everard COR, Hayes RJ, Edwards CN. Leptospiral infection in school-children from Trinidad and Barbados. Epidemiology and Infection 1989; 103(1): 143-156.
13. Jones L. Farm Child UK, a report on the nature and incidence of accidents and zoonoses to children under sixteen years on farms and in the countryside. Powys, Wales: HSE Books, 2003.
14. Epidemiology Unit, Ministry of Healthcare and Nutrition. New challenges in controlling leptospirosis. Colombo: Ministry of Healthcare and Nutrition, 2011.
15. Epidemiology Unit, Ministry of Healthcare and Nutrition. Prevention and control of leptospirosis. Colombo: Ministry of Healthcare and Nutrition, 2011.
16. Epidemiology Unit, Ministry of Health and Nutrition. Leptospirosis 2011 Special Surveillance Kurunegala. Colombo: Ministry of Healthcare and Nutrition, 2011 (in press).
17. Arunatilake N. Education participation in SriLanka. International Journal of Educational Research 2005; 45(3): 137-151.
18. Hartskeerl R. Leptospirosis: current status and future trends. Indian Journal of Medical Microbiology 2006; 24(4): 309.
19. Wiwanitkit V. A note from a survey of some knowledge aspects of leptospirosis among a sample of rural villagers in the highly endemic area, Thailand. Rural and Remote Health 6(1): 526. (Online) 2006. Available: www.rrh.org.au (Accessed 30 September 2013).
20. Agampodi S, Peacock S, Thevanesam S. The potential emergence of leptospirosis in Sri Lanka. Lancet Infection Disease 2009; 9(9): 524-526.
21. Department of Census and Statistics Sri Lanka. Paddy statistics - extent, sown, harvested, average yield and production by district - 2010 Yala season. Colombo: Department of Census and Statistics Sri Lanka, 2010.
22. Department of Census and Statistics Sri Lanka. Population and housing - population by DS division. Census of Population and Housing - 2011. Colombo: Department of Census and Statistics, Sri Lanka, 2011.
23. Lwanga S, Lemeshow S. Sample size determination in health studies. A practical manual. Geneva: World Health Organization, 1991.
24. Blackman N, Koval J. Interval estimation for Cohen's kappa as a measure of agreement. Statistics in Medicine 2000; 19(5): 723-741.
25. Agampodi S, Agampodi T, Thalagala E, Perera S, Chandraratne S, Fernando S. Do people know adequately about leptospirosis? A knowledge assessment survey in post-outbreak situation in Sri Lanka. International Journal of Preventive Medicine 2010; 1(3): 158-163.
26. Brown P, Mckenzie M, Pinnock M, Mcgrowder D. Environmental risk factors associated with leptospirosis among butchers and their associates in Jamaica. International Journal of Occupational and Environmental Medicine 2011; 2(1): 47-57.
27. Bipin V, Abhay K, Patel P, Sushil P, Shaishav P. Educational interventions to increase knowledge of leptospirosis in Navasari district. National Journal of Community Medicine 2010; 1(1): 30-32.
28. World Health Organization. Managing programmes to improve child health. Module 1 Introduction. Geneva: WHO, 2009.

