The Alma-Ata Declaration of 1978 defines primary health care (PHC) as that which is essential and affordable, and made available to individuals where they live and work1. Many communities in Sub-Saharan Africa are far from this ideal due to patients' low access to limited and often unaffordable PHC facilities. In Namibia, with its large landmass, difficult terrain, and sparse population, access to health care is particularly difficult. Rural dwellers such as farm workers and their dependents must travel long distances for care. A 2007 survey conducted among 1414 Namibian commercial farm owners showed that the average one-way distance to a clinic was 63.6 km2. The resultant health burden falls on the most vulnerable populations, particularly women of childbearing age and children, who generally require more health care.
Children require basic preventive services such as immunization against major illnesses, de-worming, health education for their care givers, and curative services such as early diagnosis and prompt treatment of common childhood ailments. Orphans and vulnerable children (OVC) may be placed at even greater risk of poor health outcomes in areas with poor access to PHC. According to the Demographic and Health Survey (DHS), from a total population of 1.83 million people, Namibia has approximately 250 000 OVC, of whom 155 000 are single (lost one parent) or double (lost both parents) orphans under the age of 18 years3,4. Approximately 37% of all orphans have lost one or both parents to HIV5.
Studies examining health indices in children have shown mixed results when comparing OVC to children who are neither orphaned or vulnerable (non-OVC). Some studies have shown that OVC were more likely to self-report morbidity6, develop a fever, diarrhea or acute respiratory tract symptoms; less likely to have complete vaccinations7; and have lower weight-for-height Z-scores than non-OVC8. In contrast, other studies have not found a difference in the prevalence of fever, malaria parasitemia, hemoglobin level or height-for-age Z-scores9. Very few studies have evaluated the impact of an intervention on important health indices.
Mobile clinics have been used for programs such as family planning, surgical interventions, dental and eye clinics and immunization campaigns, and the literature suggests they have been effective in disease screening (eg for cervical cancer and infectious diseases)10,11. In general, mobile clinic systems are vertical in approach, focusing on one disorder or public-health problem, with few of these clinics providing comprehensive primary healthcare services. Publicly available studies on the cost-effectiveness of mobile clinics are scant; however, one of these studies demonstrated that for HIV testing, a mobile multi-testing unit was more cost-effective and reached more males than traditional fixed-site, voluntary counseling and testing12. Studies on the health outcomes of target populations are few because most only report on the number of beneficiaries served, or the number of clinics or outreach clinics held. The commencement of a mobile clinic service in rural Namibia provided a unique opportunity to examine the health of rural Namibian children, compare OVC to non-OVC, and to assess the outcomes from regular provision of mobile PHC services.
Study site and sample size
The study was conducted in rural areas of Otjozondjupa and Omaheke regions of Namibia between June 2011 and January 2012. Included in the study were children aged 0-18 years who lived on farms participating in the 'Mister Sister' mobile health service13, or attended primary schools around those communities; also included were children from Ileni Tulikwafeni, a nutritional support program located within the Five Rand camp settlement. Findings from a previous pilot study conducted in the same region projected that approximately 1500 children could be served by a mobile clinic, many of them OVC.
Orphans were defined as children who had lost at least one parent to death from any cause, or were abandoned by at least one parent. Vulnerable children were defined as those who did not fit into the orphaned categories but were regarded as being vulnerable under the categorizations of the Namibia Ministry of Gender, Equality and Child Welfare14. These included HIV-positive children and children deemed to be at economic, cultural or social disadvantage (ie children whose parents were alive but who lived with other relatives, children whose parents were out of work, and children with disabilities). Non-OVC were children who were not orphaned and did not fit into the described categories of vulnerability. At primary schools, OVC were identified by teachers and other school staff, and from a registration database at the feeding programs. Where caregivers were available or the children were old enough to explain, family information, orphan status and other information on vulnerability was obtained. This was the means of identifying OVC at the farms. All children were offered clinic services regardless of their OVC status.
Mister Sister mobile health services (Mister Sister clinics)
In Namibia, the Mister Sister clinics, a mobile PHC service, was implemented primarily to provide affordable health care to hard-to-reach populations, with the intent of improving health by reducing the physical barrier to preventive and basic curative services. The target population for the mobile clinic is predominantly employees and their dependents on rural and remote commercial enterprises (farms, mines, tourism establishments). In addition, vulnerable groups such as women and children, the elderly and people residing at significant distances from health facilities which the mobile clinics encounter en-route also receive clinic services. The Mister Sister clinics, an offshoot of a mobile multi-disease screening clinic (Bophelo!), are a unique public-private partnership in Namibia conducted by PharmAccess Foundation Namibia and the Ministry of Health and Social Services (MOHSS)13. The program is funded by monthly fees paid by the employers, plus national and international contributions. The Namibian government provides all vaccines and essential medicines for the PHC services as well as treatment for referred patients. The first Mister Sister clinic on which this study was conducted, was funded by Heineken Africa Foundation with technical assistance for operations, and donor funding for vulnerable communities provided by the Dutch Health Insurance Fund and USAID.
The mobile clinic is staffed by a nurse practitioner with diagnostic skills and prescription privileges, as well as a nurse and a multi-purpose driver. Detailed information about the mobile clinic has been published previously15. In this study, all diagnoses were made by the nurse practitioner, interventions such as administration of drugs or vaccines were carried out by both the nurse and nurse practitioner, referrals were written by the nurse practitioner and other administrative duties (ie registration of clinic patients and collection of fees) were conducted by all clinic staff, including the driver.
Outcome measures
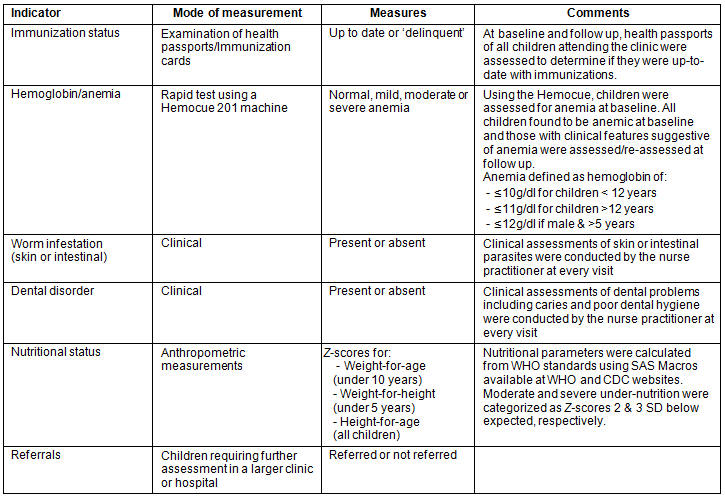
Prior to the study commencement, six outcome measures were chosen, based on previous experience and in consultation with the mobile clinic nurse practitioner: (i) immunization status assessed by examining children's health records; (ii) number and frequency of referrals; (iii) clinical and laboratory presence of anemia (all children had blood tests for anemia at base line and at follow up only those anemic at baseline or who had clinical features of anemia in the follow-up months were reassessed with blood tests); (iv) clinical diagnosis of skin and/or intestinal parasitic infections; (v) presence of dental disorders; and (vi) nutritional status. Details of the assessment of these health conditions are provided (Table 1). At each visit, children were assessed for all six health indicators. The first assessment (referred to as 'baseline') occurred in the first 2 months of the mobile clinic's visit to the sites (June and July 2011), while 'follow up' occurred during the last 2 months (December 2011 and January 2012).
Mobile clinic staff were trained to look for the presence or absence of the outcome measures and to document them.
Table 1: Explanation of health indices' assessment
The longitudinal group
Outcomes in a subset of the children who attended the clinic at baseline and at follow up were assessed. This cohort, referred to as the 'longitudinal group' were followed up for at least 4 months. As with the larger group, their baseline is identified as the first assessment in the first two visits, while follow up is their last assessment in the last two clinic visits.
Statistical analysis
Patient baseline characteristics were summarized with descriptive statistics stratified by orphan status. For nutritional parameters, Z-scores were generated using SAS macros available at WHO and Centers for Disease Control and Prevention websites16-18. Chi-squared tests of independence were used to assess significant differences between indicators at baseline and follow up. All analysis was conducted using SAS software v9.3 (www.sas.com).
Ethical approval
The study was approved by the Boston University institutional review board (#H31172) and by MOHSS in Namibia.
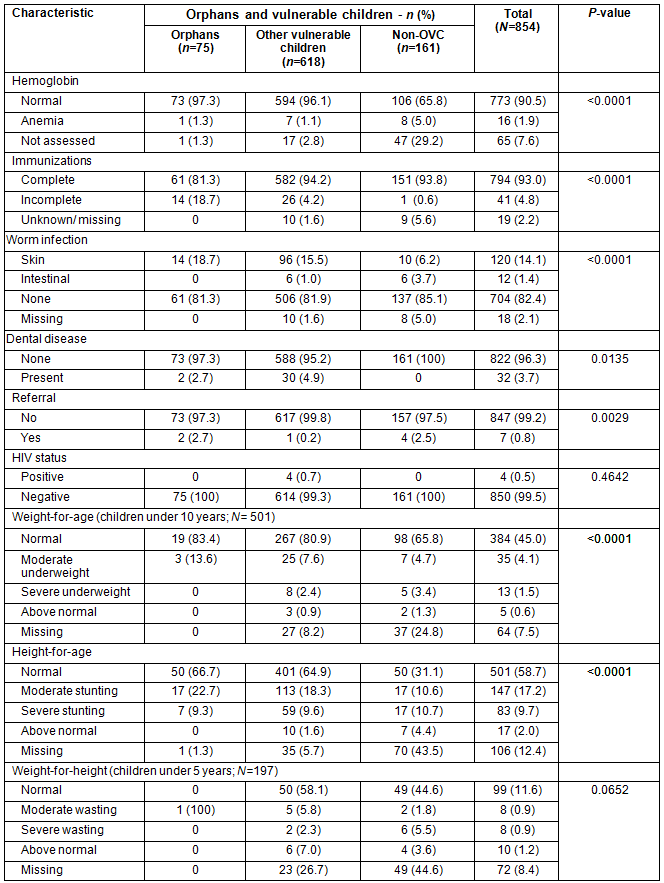
Over the 7 month period, a total of 1210 children visited the mobile clinic, with a median of 2 visits per child (interquartile range [IQR] 1-3 visits). At baseline, 854 children presented. Of these, the majority were identified at Otjozondu School (48.5%), female (50.8%), HIV-negative (99.5%), and had a median age of 8.7 years (IQR 5.5-12.3 years). Of these children, 8.8% (n=75) were defined as orphans, 72.4% (n=618) were defined as vulnerable but not orphaned, and 18.9% (n=161) were non-OVC (Table 2). Most of the orphans (98.7%) and other vulnerable children (86.1%), were at least 5 years of age, compared with 31.7% of non-OVC (p<0.0001). The vast majority of orphans or otherwise vulnerable children (95%) were identified at Ileni and Otjozondu primary schools, while virtually all the non-OVC were identified on the farms (p<0.0001).
Table 2: Baseline clinical and anthropomorphic characteristics stratified by orphans and vulnerable children status
Overall study group
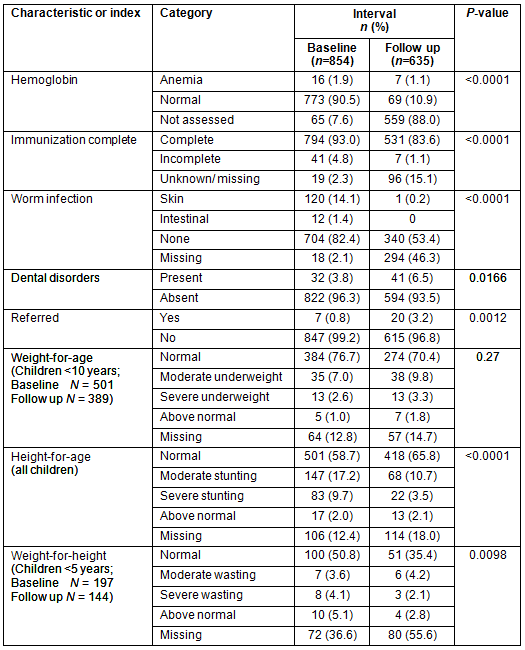
The overall study group at baseline (n=854) was reduced to 635 at follow up. Over the study period there was considerable reduction in children with outstanding immunizations (from 5% to 1% [p<0.0001]), and the prevalence of skin and intestinal parasites (from 15% to 0.2% [p<0.0001]) (Table 3). There was also an increase in identified dental disease (4% to 7%; p=0.0166) and in the proportion of children referred to a larger healthcare facility (1% to 3%; p=0.0012). While there was no significant change in weight-for-age (p=0.27) in children under the age of 10 years, there was a significant reduction in stunting (height-for-age) (p<0.0001) for all children. A reduction in moderate and severe stunting was also observed (from 17.2% to 10.7% & 9.7% to 3.5%, respectively), as well as an increase in normal height-for-age (from 58.7% to 65.8%). Additionally, there was a decline in severe wasting (from 4.1% to 2.1%), though significant data on weight-for-height were missing.
Table 3: Comparison of health indices of clinic attendees at baseline and follow up
Longitudinal group
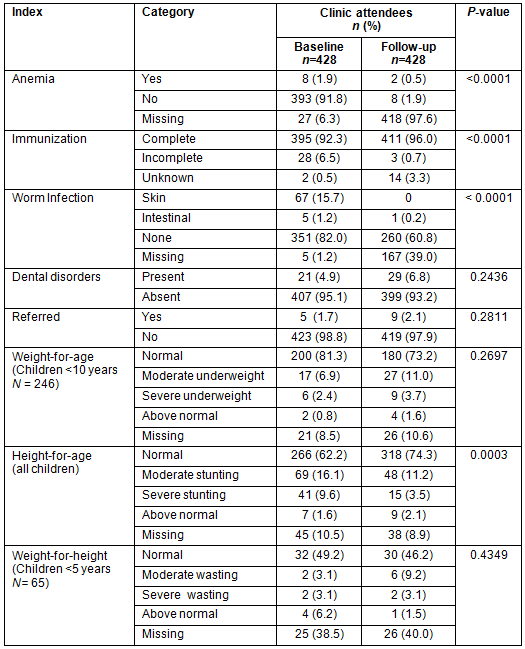
Among the 428 children who were seen at least once at baseline and also at follow up, there was a reduction in the prevalence of anemia from 1.9% to 0.5% (p<0.0001) and of incomplete immunizations from 6.5% to <1% (p<0.0001) (Table 4). None of the 67 children with skin parasites at baseline had skin parasites at follow up, and there was a modest but significant reduction in the intestinal parasites (from 1.2% to 0.2% [p<0.0001]). There was no significant change in the frequency of dental disorders or of children requiring referrals. There was a significant change in height-for-age (p=0.0003), with less children showing moderate and severe stunting at follow up compared with baseline; however, no significant change in the weight-for-age for <10 year olds and weight-for-height for <5 year olds was observed (Table 4).
Table 4: Comparison of health indices of clinic attendees at baseline and follow up in longitudinal cohort
Longitudinal group: comparison within and between vulnerability status
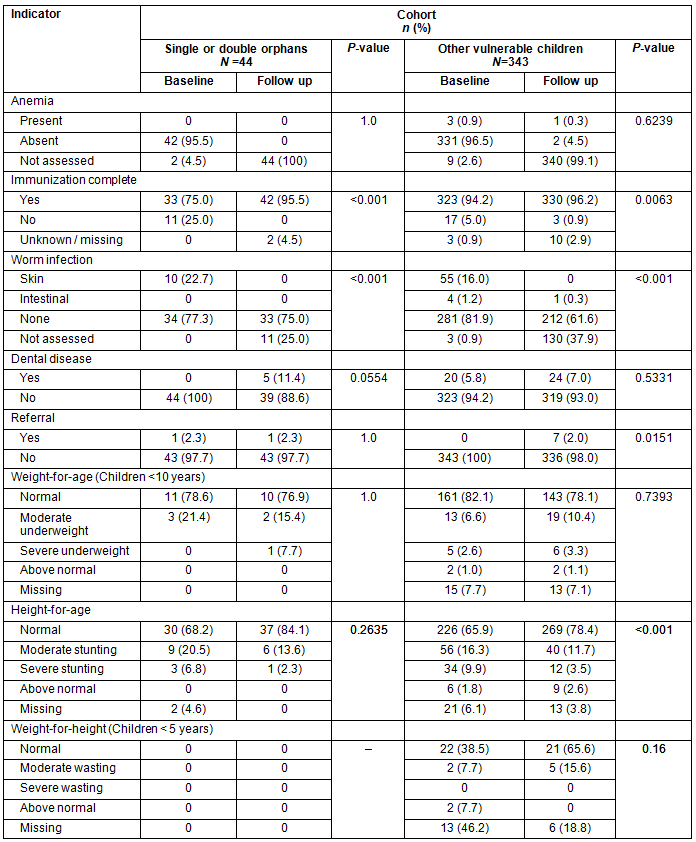
When comparing change from baseline within vulnerability status it was found that among orphans the prevalence of incomplete immunizations reduced from 25% to 0 (p<0.001), and parasitic infections decreased from 22.7% to 0 (p<0.001), while there was a non-significant reduction in the proportion of stunted children (from 27% to 16% [p= 0.195]). Among vulnerable children, the frequency of incomplete immunizations declined from 5% to 1% (p=0.002), as did skin and parasitic infestations (17.2% to 0.3% p<0.001) over the study period. Although not significant, there were similar reductions in anemia, incomplete immunizations, parasitic infections, and the height-for age parameters for the non-OVC (Table 5).
When comparing across vulnerability groups there were significantly more orphans having incomplete immunization (25%) compared with other vulnerable children (5%) and non-OVC (0%) (p<0.001) at baseline (Table 2). Orphans also had a higher proportion of skin and intestinal parasites at baseline compared with the other two groups (22.7% vs 17.2% vs 6.9% p=0.072). In contrast at baseline, none of the orphans were found to be anemic while up to 12% of the non-OVC was found to be anemic (p<0.0001). There were also significantly more non-vulnerable children requiring referral at baseline. There was no significant difference in the distribution of nutritional parameters among children's groups.
Table 5: Baseline and follow-up frequencies according to vulnerability in the longitudinal cohort
Discussion
This study, the results of which are largely consistent with previous findings (orphaned children are sick more often than non-orphaned children6, have greater risk of diarrheal disease, acute respiratory infection or malnutrition7,8), adds to existing evidence that health indices are potentially worse for OVC compared with non-OVC. Compared with non-orphans, orphans have been shown to be less likely to access health care and other services, accounting in part for the increased risk of illness19. The present study findings indicate that the provision of a comprehensive mobile primary healthcare program in hard-to-reach regions can help to improve the health of children and reduce the existing health disparity between OVC and non-OVC.
Among the children attending the clinic (n=1210), there was a relatively low burden of disease with the exception of skin or intestinal parasitic infection (12%) and malnutrition (stunting 23%; underweight 10%). The number of disorders outside the scope of a PHC facility and for which children were referred was particularly low, implying that most disorders encountered could be managed effectively by the Mister Sister mobile clinic. Though the proportion of children with incomplete immunization records at first clinic visit was relatively small, this population had been through one round of vaccination in a pilot trial by the Mister Sister clinic which ended 6 months before this study began; hence, the 4% prevalence of under-immunization does not reflect baseline in this population20.
In the study population, OVC had comparatively worse health indices than non-OVC. At baseline for both collective and longitudinal follow-up groups, incomplete immunization rates and the prevalence of parasitic infections in orphans and other vulnerable children were higher than for those in the non-OVC group. The results of other studies agree with the present findings of diminished immunization rates among OVC. In North India, significantly fewer orphans had complete immunizations compared with non-orphans (p<0.05)21, while in Kenya the risk of being unimmunized was almost 3 times higher in double orphans compared with non-orphans22. The findings of the present study show that immunization rates were lower among OVC and that the provision of regular PHC using a mobile clinic reduced the proportion of under-immunized children, with the greatest improvement seen among the orphans.
Nutrition is one of the most widely examined health indices of OVC, and studies almost uniformly agree that OVC have worse nutrition that non-OVC8,21,23-27; the Namibian 2006 DHS also agrees with this general finding4.Higher rates of poverty and food insecurity in OVC have been blamed for this disparity26 because households with HIV-affected orphans are more likely to suffer food insecurity, and are more malnourished children23,28. Maternal HIV infection has also been associated with increased risk of infant under-nutrition24. This nutritional disadvantage is not exclusive to orphans as it has been demonstrated in other vulnerable children, such as those in foster care or living with single mothers29. Mobile clinics providing food supplementation demonstrated significant reduction in acute and chronic under-nutrition27. Over the study period there was no change in nutritional parameters, except for a reduction in the proportion of children presenting to the clinic with stunting. This finding was probably due to chance because the mobile clinic did not provide any form of nutritional supplementation.
Anemia, an established public health problem among children in developing countries was particularly low at baseline in the present study (1.9% for all children). Only 6.1% preschool age children in the present study were anemic at baseline, compared with the national preschool age anemia prevalence of 40.5%30. The Mister Sister clinic definition of anemia was hemoglobin less than 10 g/L, compared with 11 g/L used in the national survey and this may have accounted for the difference in prevalence. During the follow-up months, the clinic conducted hemoglobin assessment only in children whose clinical features were suggestive of anemia and those who were anemic at their first visit (baseline). The prevalence of anemia declined from 1.9% at baseline to 1.1% at follow up in the entire (collective) population, and from 1.9% to 0.5% in the longitudinal group. Regular visits by the clinic reduced the prevalence of anemia in both the otherwise vulnerable and non-OVC groups. No mobile clinic studies with childhood anemia interventions were found for comparison.
Limitations
This study has some limitations. First, there was a significant amount of missing data, especially for the nutritional parameters in the non-OVC; however, considering the operational nature of this study and the difficulties with obtaining such information, this was not unexpected. With greater than 50% missing, the weight-for-height data was most affected and this made it difficult to draw conclusions about this index. Second, at follow up the vast majority of children did not have their hemoglobin tested; however, they were clinically assessed for anemia and only those who appeared anemic or who had anemia at baseline were offered a rapid hemoglobin test at follow up. Therefore, a reduction in the frequency of anemia is suspected. Third, the values at baseline for immunization in this study represents an improvement from an earlier pilot of the mobile clinic program that provided wellness screening and vaccinations only to children at the school, camp and farms. At the beginning of the first mobile clinic program, up to 32% of children were deficient in their immunization20, a more accurate reflection of the baseline status for immunization. So, when follow-up data is compared with the baseline from the mobile clinic pilot program, the effect of the mobile clinic on immunizations is even greater (a decrease from 32% to 2.7%, or 91.7% reduction). Fourth, significant inter-observer differences at baseline and follow up may have occurred with the clinical assessment of dental disease. The nurse practitioner assessed the children for dental disorders at baseline, while a dental hygienist made the assessment at follow up, increasing the probability of diagnosis. Fifth, the study period of 6 months may have been too short to see the effects of the clinic's interventions on some indices, particularly the nutritional. Studies with longer duration are required to assess sustained improvement in these parameters. Sixth, due the nature of the study there were significant demographic differences between the orphans, other vulnerable children and the non-OVC, such as the age and location of the children. This difference may have accounted for the difference in some of the outcome measures at baseline such as anemia, nutrition status and immunization. In particular, anemia prevalence was higher in the non-OVC, who had the highest percentage of children under 5 years of age. The demographic differences, however, cannot account for the broad improvement in outcomes. Finally, due to limited funds and resources, conducting general population surveys to determine indices at baseline and follow up were not possible. Neither was there comparable computerized data available for populations served at fixed sites. As such, modifying the Mister Sister's already available data system for the purposes of the study was the most cost-efficient way to conduct this study, although a community-based approach would have been desirable.
Update
Since the conclusion of the study, the Mister Sister clinic continues to operate in the region where the study was conducted and provides routine PHC services to OVC and other children. The organization has acquired three more mobile clinics and has expanded to two additional regions with the support of the MOHSS. It also continues to enjoy donor support (USAID through strengthening health outcomes through the private sector [SHOPS], Dutch Health Insurance Fund) and is increasingly attracting private sector funding in Namibia. Unit costs of treatment are declining with increasing volumes of participants, and operational experience improving efficiencies. Continuous marketing of the services to employer groups, as well as health insurance and medical aid funds has increased private sector funding. However, continuing to serve the OVC population with Mister Sister will require continued partial subsidization by foreign or local public funds.
Namibia's HIV epidemic and socioeconomic consequences have created significant issues surrounding orphanhood and childhood vulnerability. In rural Namibian children, the health of OVC is generally worse than non-OVC, a situation that is exacerbated by poor access to health care. Provision of regular preventive and therapeutic mobile clinic services can help to reduce the overall morbidity in children and bridge the health disparity between OVC and non-OVC. Careful planning of these programs in areas with similarly identified barriers may help correct the health disparities among Namibian OVC and could be a first step in improving child morbidity and mortality in difficult-to-reach rural areas.
Acknowledgments
The authors acknowledge the help and support of the members of the PharmAccess Namibia Mister Sister team without whom this work would not have been possible. In addition they thank the Ministry of Health and Social Services in Namibia for their valued assistance and input by critically reviewing this manuscript. The work of all the authors was funded by the USAID Project SEARCH, Orphans and Vulnerable Children Comprehensive Action Research (OVC-CARE) Task Order, under Contract No. GHH-I-00-07-00023-00, beginning on 1 August 2008. The OVC-CARE Task Order is implemented by Boston University. The opinions expressed herein are those of the authors and do not necessarily reflect the views of the funding agency.
References
1. UN. Declaration of Alma-Ata, (Online) 1978. Available: http://www.who.int/publications/almaata_declaration_en.pdf (Accessed 15 July 2013).
2. De Beer I, Coutinho HM, Guariguata L, Fortsch HHT, Hough R, Rinke de Wit TF. Health care options for commercial farm workers in Namibia. Rural and Remote Health 11: 1384. (Online) 2011. Available www.rrh.org.au (Accessed 13 April 2012).
3. Namibian Ministry of Gender Equality and Child Welfare. National Plan for Orphans and Vulnerable Children in Namibia: Annual Progress and Monitoring Report for 1 April 2007 to 31 March 2008. Windhoek: Ministry of Gender Equality and Child Welfare Namibia & UNICEF, 2008.
4. Namibia Ministry of Health and Social Services, Macro International. Namibia Demographic and Health Survey 2006-2007. Windhoek & Calverton, MD: MOHSS and Macro International, 2008.
5. UNICEF. Namibia: Statistics. (Online) 2012. Available: http://www.unicef.org/infobycountry/namibia_statistics.html (Accessed 13 April 2012).
6. Sarker M, Neckermann C, Müller O. Assessing the health status of young AIDS and other orphans in Kampala, Uganda. Tropical Medicine & International Health 2005; 10(3): 210-215.
7. Amoako Johnson F, Padmadas SS, Smith PWF. Orphanhood and vulnerability: a conduit to poor child health outcomes in Rwanda. AIDS Care 2010; 22(3): 314-323.
8. Watts H, Gregson S, Saito S, Lopman B, Beasley M, Monasch R. Poorer health and nutritional outcomes in orphans and vulnerable young children not explained by greater exposure to extreme poverty in Zimbabwe. Tropical Medicine & International Health 2007; 12(5): 584-593.
9. Lindblade KA, Odhiambo F, Rosen DH, DeCock KM. Health and nutritional status of orphans <6 years old cared for by relatives in western Kenya. Tropical Medicine & International Health 2003; 8(1): 67-72.
10. Swaddiwudhipong W, Chaovakiratipong C, Nguntra P, Mahasakpan P, Tatip Y, Boonmak C. A mobile unit: an effective service for cervical cancer screening among rural Thai women. International Journal of Epidemiology 1999; 28(1): 35-39.
11. Guyatt H, Evans D, Lengeler C, Tanner M. Controlling schistosomiasis: the cost-effectiveness of alternative delivery strategies. Health Policy Plan 1994; 9(4): 385-395.
12. Feeley F, Bindels E, Rinke deWit TF, De Beer I. Comparison of Key Unit Costs and Outcomes for Mobile and Fixed Site. (Online) 2010. Boston University Center for Global Health and Development. Available: http://www.bu.edu/cghd/files/2010/12/Bophelo-Report-FINAL-for-CGHD.pdf (Accessed 15 July 2013).
13. Mister Sister Mobile Health Service. Background. (Online) 2012. Available: http://www.mistersisterclinics.org/aboutClinic.php (Accessed 15 July 2013).
14. Namibia Ministry of Education. Education Sector Policy for Orphans and Vulnerable Children. Windhoek: Namibia Ministry of Education, 2008.
15. PharmAccess Foundation. Mister Sister Mobile Health Service - Information Brochure. Heineken Africa Foundation. (Online) 2011. Available: http://africafoundation.heineken.com/downloads/mister-sister-information-brochure.pdf (Accessed 15 July 2013).
16. WHO. Application tools. World Health Organization. (Online) 2012. Available: http://www.who.int/growthref/tools/en/ (Accessed 13 April 2012).
17. WHO. WHO Anthro. (Online) 2012. Available: http://www.who.int/childgrowth/software/en/ (Accessed 13 April 2012).
18. CDC. Growth Chart Training: Resources: SAS Program. (Online) 2012. Available: http://www.cdc.gov/nccdphp/dnpao/growthcharts/resources/sas.htm (Accessed 13 April 2012).
19. Andrews G, Skinner D, Zuma K. Epidemiology of health and vulnerability among children orphaned and made vulnerable by HIV/AIDS in sub-Saharan Africa. AIDS Care 2006; 18(3): 269-276.
20. PharmAccess Foundation Namibia. Report of Pilot project in Hochfeld. Windhoek: PharmAccess Foundation, 2010.
21. Bhattacharya M, Rajeshwari K, Saxena R. Demographic and clinical features of orphans and non-orphans at a pediatric HIV centre in North India. Indian Journal of Pediatrics 2010; 77(6): 627-631.
22. Radcliff E, Racine EF, Brunner Huber LR, Whitaker BE. Association between family composition and the well-being of vulnerable children in Nairobi, Kenya. Maternal and Child Health Journal 2012; 16(6): 1232-1240.
23. Ndirangu M, Wariero JO, Sachs SE, Masibo P, Deckelbaum RJ. Nutritional status of under-five children in HIV-affected households in western Kenya. Food and Nutrition Bulletin 2011; 32(2): 159-167.
24. Magadi MA. Household and community HIV/AIDS status and child malnutrition in sub-Saharan Africa: Evidence from the demographic and health surveys. Social Science and Medicine 2011; 73(3): 436-446.
25. Magadi MA. Cross-national analysis of the risk factors of child malnutrition among children made vulnerable by HIV/AIDS in sub-Saharan Africa: evidence from the DHS. Tropical Medicine & International Health 2011; 16(5): 570-578.
26. Kimani-Murage EW, Holding PA, Fotso J-C, Ezeh AC, Madise NJ, Kahurani EN et al. Food security and nutritional outcomes among urban poor orphans in Nairobi, Kenya. Journal of Urban Health 2011; 88(Suppl2): S282-297.
27. Parikh K, Marein-Efron G, Huang S, O'Hare G, Finalle R, Shah SS. Nutritional status of children after a food-supplementation program integrated with routine health care through mobile clinics in migrant communities in the Dominican Republic. American journal of Tropical Medicine and Hygiene 2010; 83(3): 559-564.
28. Rivers J, Mason JB, Rose DD, Eisele TP, Gillespie S, Mahy M et al. The impact of orphanhood on food security in the high-HIV context of Blantyre, Malawi. Food and Nutrition Bulletin 2010; 31(Suppl3): S264-271.
29. Mishra V, Arnold F, Otieno F, Cross A, Hong R. Education and nutritional status of orphans and children of HIV-infected parents in Kenya. AIDS Education and Prevention 2007; 19(5): 383-395.
30. Bruno de Benoist, Erin McLean, Ines Egli, Mary Cogswell (Eds). Worldwide prevalence of anaemia 1993-2005. Geneva: World Health Organization, 2006.



