Pakistan is amongst the five countries that contribute to 49% of global childhood deaths. Each day almost 500 newborns die in Pakistan, ranking its neonatal mortality close to that of Afghanistan and Iraq amongst developing countries. Neonatal mortality constitutes more than 70% of the infant mortality rate. In Pakistan, neonatal mortality has been static for two decades1. It is not possible to reduce the under-five and infant mortalities without addressing the stagnating neonatal mortality rate.
Given limited funding and the short time to the Millennium Development Goals deadline of 2015, the imperative to invest in the most effective interventions is clear. Cultural beliefs and practices, more common amongst women, often lead to delayed healthcare seeking for neonates in rural communities2. Simple and low-cost community and home-based neonatal interventions have the potential to bring about drastic reduction in neonatal morbidity and mortality3. In Bangladesh, the mother's knowledge of essential newborn-care practices, such as drying and wrapping the baby immediately after birth, initiating breast milk within 1 hour of birth and having early postnatal newborn checkups, improved neonatal health outcomes4. With Azad Jammu and Kashmir (AJK)'s urban-rural ratio of 12:88 and mainly mountainous topography5, health care provision to the scattered rural communities of the Azad Jammu and Kashmir (AJK) has been a big challenge. Moreover, disaggregated data on the patterns of neonatal morbidity and mortality is not available in AJK. Among the various causes and determinants of neonatal mortality in Pakistan, most emerge from behaviors and inappropriate practices of women and caregivers6. Therefore, reasonable gains can be made for newborn health and survival by addressing various myths, fallacies and misconceptions related to health-seeking practices. The objective of this research was to study household-based practices amongst mothers regarding healthcare seeking for their neonates in rural and urban settings of district Muzaffarabad, AJK.
This community-based cross-sectional study was carried out in rural and urban settings of district Muzaffarabad, AJK. The study was conducted during the 6 months from July to December 2011. Situated in the upper reaches of the Indian subcontinent and the Pakistani side of the Line of Control, AJK is a unique politico-legal territorial entity of unresolved status. Unlike Indian-administered Kashmir, AJK has not been formally annexed by Pakistan. The word Azad in AJK derived its inspiration from the political character of freedom movement launched by native Kashmiris for liberation of this state. Although AJK has its own constitution and elected government, the territory has no international legal status7.
The population of AJK was 4.059 million in 2011. AJK is divided into three divisions and 10 administrative districts with Muzaffarabad as the capital of the state5. Infant mortality rate in AJK is estimated at 62 per 1000 live births while the probability of dying under five years of age is around 96 per 1000 live births. Infant and under-five mortality rates are higher in rural areas than in urban ones8.
Inclusion criterion for this study was mothers who had a neonate with current illness or illness within the previous 2 weeks. Mothers who had 'too sick neonates' were excluded from the study. For the purpose of this study, 'too sick neonates' were considered as the ones having non-preventable diseases such as congenital conditions that might present as gross cyanosis, pallor and failure to thrive. 'Too sick neonates' were excluded from the study to avoid the risk of effect modification because there is increased probability of healthcare utilization for them compared to the 'neonates with common illness'. Neonates with preventable and curable illness such as respiratory, gastrointestinal, umbilical cord or eye infections were taken as 'neonates with common illness' in this study. A newborn of less than 28 days of age was considered to be 'neonate'.
For the purpose of this study, socioeconomic status of each household was categorized as low, middle or high. According to the Household Integrated Economic Survey (HIES) of 2007-089, household income is divided into five quintiles. In this study, first and second quintiles of the HIES 2007-08 were categorized as low, third and fourth quintiles as middle, and fifth quintile as high income (Table 1). Average household size in AJK is approximately 6.7 members8.
Sample size was calculated by using the formula of two samples to estimate the difference between two population proportions with specified precision10. Precision required on either side of the true value of the population proportions was taken as 10% (0.1). Disaggregated data on household-based practices of urban and rural mothers for their neonates is not available in AJK. Therefore, proportions for both the rural and urban mothers were taken as 50% (0.5) in order to obtain the largest sample size. Confidence level was set at 95% with significance level at 5% (0.05).
A multi-stage sampling technique was used for selection of 104 mothers each from urban and rural settings of district Muzaffarabad. In Pakistan, administrative boundaries are used to define urban areas, with designations of municipal corporation, municipal committee or cantonment board11. An urban area having a population exceeding 30 000 is considered to be a municipal committee12. A cantonment board is responsible for administering the military lands whose functions are synonymous to the municipal committee of the civil setup13. The population of a municipal corporation exceeds 5000 000. A rural area is any area that is not an urban area12.
Basic Health Units (BHUs) were taken as the entry points into household that they cover. BHU is the first-level care facility where a lady health worker (LHW) reports and submits data of the population that she covers by visiting them at their households. In the first stage of sampling, a list of the BHUs of district Muzaffarabad was taken as the sampling frame. In the second stage, two BHUs for the rural population and two for the urban populations were randomly selected. Study was conducted on the mothers at the household level within the catchment populations of these BHUs and LHWs. In the third stage of sampling, the LHWs facilitated identification of the study population in the community.
Recruitment of the mothers having neonates was done, with study objectives explained and informed consent taken. Thereafter, interviews were conducted at the level of household by LHWs for assessing household-based practices and service utilization patterns of mothers regarding early neonatal care. Inclusion criteria were strict; it was not feasible to randomly select from the population. Therefore, all mothers having less than 28-day-old neonates with current or past (within 15 days) illnesses were interviewed. A high response rate was expected because 60 LHWs facilitated recruitment of mothers. LHWs have an established rapport with mothers in their respective areas of urban and rural settings.
A close-ended pre-coded questionnaire was used for data collection. This tool was developed after extensive literature review regarding household-based practices and service utilization patterns of mothers with early neonates in Pakistan, and in neighboring and some developing regional countries4,6,14-16. Questionnaire and consent form were translated into Urdu (the national language of Pakistan) before administering them in the study population. The questionnaire was pre-tested and necessary changes were made such as a detailed explanation of the categorization of socioeconomic status; inclusion and exclusion criteria were included in the questionnaire.
Data was collected for variables related to sociodemographic characteristics and household-based practices. Quantitative statistical analysis of variables was carried out using the Statistical Package for the Social Sciences v16.0 (SPSS Inc., http://www.spss.com). Inferential analysis was carried out using the χ² test along with cross-tabulation to assess the level of association. Binary logistic regression was utilized to control the effect of confounders. Selected outcome variables from household-based practices were regressed against a set of predictor variables including mother's age and education, father's education, family system, socioeconomic status and place of residence of the household.
Ethics approval
Research was initiated upon acceptance of the proposal by the Ethical Review Board of the Health Services Academy, Islamabad. Upon written approval from the Ethical Review Board, liaison was established with the administration of district Muzaffarabad and the LHW program of AJK. During processing and analysis of the data, strict confidentiality was maintained.
Table 1: Socioeconomic status of household

Response rate was 100% in this study. The predominant proportion of the study population (53%) belonged to the middle socioeconomic group. Thirty five per cent of the mothers in this study were found to be illiterate (Fig1). In cross-tabulation, more rural mothers were found to be illiterate compared to the urban ones (p=0.004, χ² test).
The majority of the neonates (55%) were delivered at the public health facility. The number of deliveries conducted at homewas 34% (Table 2). Elderly experienced ladies attended 53% of deliveries at home; traditional birth attendants were called for 27% of home deliveries. Most neonates (77%) in this study had received vaccination. In cross-table analysis, more neonates were found to be delivered at home (p<0.001) and left unvaccinated (p=0.008) in rural settings compared to urban ones (Table 2).
Statistically significant association was found in cross-table analysis between the rural place of residence and the practices of tying (p<0.001) and cutting (p<0.001) a newborn's umbilical cord with unsterilized items (Table 3). Similarly, more urban neonates (p<0.001) were found to be dried and wrapped immediately after birth compared to the rural ones (Table 4).
In 50% of cases of sick neonates, healthcare seeking was immediate. Out of the remaining cases, there was delay of 1 day for 28% of sick neonates, a delay of 2 days in 16% and delay of 3 days in 6% of the cases. In cross-tabulation, delay in seeking neonatal health care was more common in rural settings compared to urban ones (p<0.001) (Table 5). The main reason for delay in seeking health care for the neonates was found to be non-availability of transport followed by 'need of permission from elders'.
The most preferred healthcare provider of mothers in both the urban (29%) and rural (27%) settings of this study was medical doctor (Fig2) either privately or in a public facility. Fifteen per cent of the mothers preferred taking their neonate directly to a district level hospital. There were 12% of the mothers who preferred seeking health care from the traditional birth attendant, while 10% preferred peer sahib (faith/spiritual healer), and 7% preferred LHWs.
Findings of the logistic regression analysis showed that residing in rural settings reduced chances of delivery at a health facility. Masters level education of the neonate's father increased chances of childbirth at the health facility (Table 6). Newborns delivered in rural areas had reduced chances of having their umbilical cords tied with commercially available strings (Table 7). Therefore, stratum-specific analyses concluded rural place of residence as a predictor of the inappropriate household-based practices of mothers for their neonates.
Table 2: Place of residence, place of delivery and neonate's vaccination?

Table 3: Place of residence, practices of tying and cutting umbilical cord?
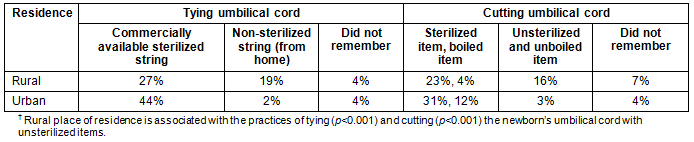
Table 4: Place of residence, practice of drying and wrapping newborn immediately after birth?
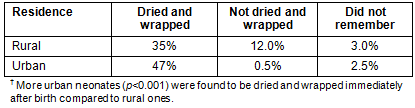
Table 5: Place of residence, delay in decision-making and duration of delay?
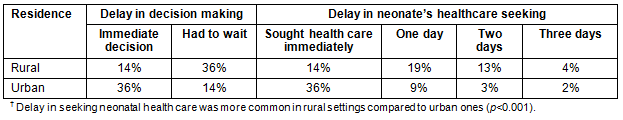
Table 6: Logistic regression analysis for examining predictors of childbirth at home or in health facility
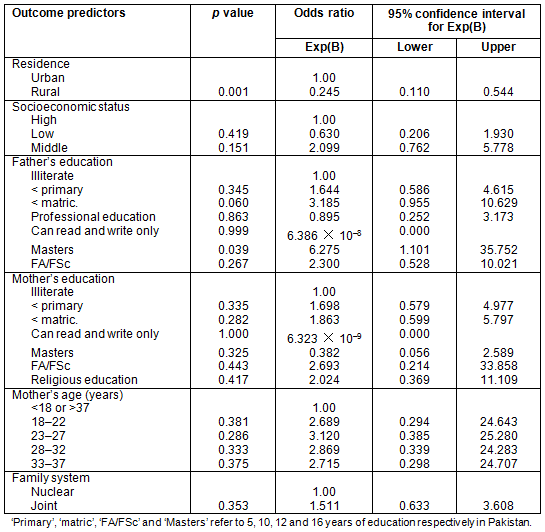
Table 7: Logistic regression analysis for examining predictors of tying the umbilical cord with home-made or commercially available string
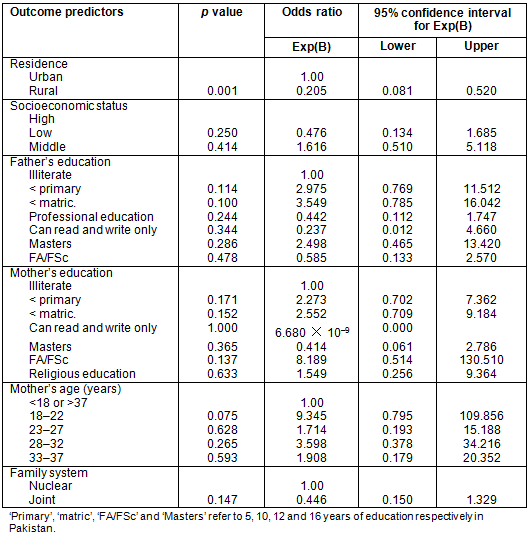
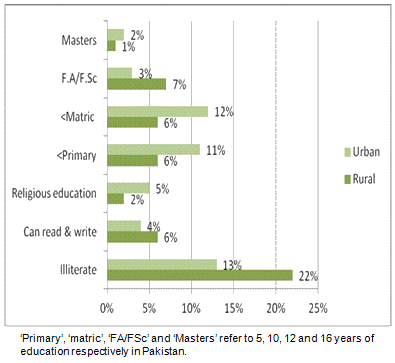
Figure 1: Education of neonate's mother and place of residence.
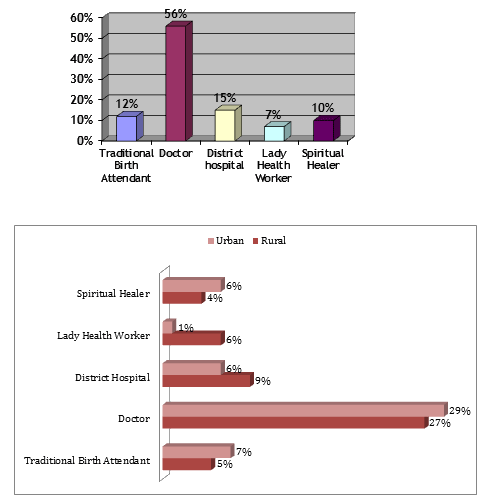
Figure 2: Preferred healthcare provider.
Discussion
Universal access to basic education is the second Millennium Development Goal. Education is a vital prerequisite for empowering women. Inferential statistics utilized in this study concluded that out of the illiterate mothers (35%), most were in rural settings. According to the AJK Demographic Health Survey of 2010, 40% of the female population in AJK have no education17. Only 29% of girls of primary school age are actually in school; the proportion of boys is considerably higher, at 40%8.
After adjusting for the effect of confounders, findings of the present research showed statistically significant association of the rural place of residence with inappropriate household-based practices of the mothers for neonates. Findings of this research are in concordance with the AJK Multiple Indicator Cluster Survey (MICS 2007-08)8, AJK Demographic Health Survey17 and the research conducted in northern areas of Pakistan and urban and rural areas of other countries in the south Asia region15 regarding household-based practices of healthcare seeking for children.
In the present study more urban neonates were found to be immunized compared to the rural ones. According to the MICS survey in AJK, children of urban settlements and the wealthiest households are more likely to be fully vaccinated than other children8. Findings of the AJK DHS show that 41% of the population in urban areas is in the richest wealth quintile in contrast to 16% of the rural population. On the other hand, almost 20% of the rural population is in the poorest quintile, compared with only 3% of the urban population17.
Use of health services is known to depend on the physical, economic and social accessibility of the offered services. Traditional community practices and the conservative norms drastically affect neonatal health outcomes6. As per the findings of this research, tying the umbilical cord with home-made unsterilized string was more likely with newborns of mothers residing in rural settings compared to the urban ones. Similarly, delivery at home was more likely to occur for mothers residing in rural settings compared to those in urban areas. Evidence suggests that families might view out-of-home care-seeking during the neonatal period as risky because it potentially exposes the newborn to cold winds, malevolent spirits, and the gaze of jealous people, and the treatment itself may be seen as too strong for a young child16. There is evidence to suggest that participatory health education interventions coupled with community-based primary health care in rural regions can improve maternal and child health18,19.
In the present research, delay in seeking neonatal health care was more common in rural settings compared to urban ones. The main reason for delay was found to be non-availability of transport followed by 'need of permission from elders'. Results of the AJK Demographic Health Survey showed that half (51%) of the births in AJK are delivered in health facilities, while 47% of births take place at home. The main reasons given for not delivering in a health facility included the facility being too far away or non-availability of transport (41%)17.
Average distance to a reproductive health facility in rural areas of AJK is almost four times the distance in urban areas, making access to services for rural women without transportation or funds extremely difficult20. Evidence from another study conducted in the northern areas of Pakistan suggests that the effect of long distance on the use of health services becomes stronger when combined with the dearth of transportation, and poor roads, which contribute towards increased costs of visits. As in all other developing countries and restricted cultures, lack of social mobility is a barrier to women seeking health care for themselves and their children, even in matters of utmost importance14.
The most preferred healthcare provider of the mothers in both the urban and rural settings of this study was a medical doctor. Some mothers preferred seeking health care from traditional birth attendants and peers sahib. Factors behind such service utilization preferences include crucial shortages of trained health staff at primary care level. As in other provinces of the country the number of LHVs and nurses is not sufficient for the population health needs of the AJK20. The gender of the healthcare provider is a longstanding issue; there are not enough female healthcare practitioners, particularly in rural areas of Pakistan. Since access to the health care of women is defined by societal norms, most of the time it is constrained because of the non-availability of female healthcare providers6.
Achieving the fourth Millennium Development Goal may be delayed unless the prospective range of child survival interventions are scaled up, with a strong focus on the production and deployment of a critical mass of community midwives along with LHWs linked to the health system, and supported by strong partnerships and active community participation. In Pakistan, no more than 20% of people consult a government first-level care facility, and this has been unchanged for the past 10 years14. There is an urgent need to equip the referral facilities, to scale up integrated management of newborn and child illness and to ensure effective newborn delivery in first-level care facilities21.
Findings of this research conclude that inappropriate household-based practices regarding neonatal care are more common in rural settings compared to urban ones. It is imperative to formulate a comprehensive behaviour change and advocacy campaign for promoting appropriate practices for neonatal healthcare seeking. Collaboration for action on social determinants ought to be considered, with particular emphasis on girls' education with the long-term objective to improve decision-making power and health-seeking behaviours of mothers for their neonates.
References
1. Bhutta ZA, Cross A, Raza F, Zahir Z. Infant and child mortality in Pakistan demographic and health survey 2006-07. Pakistan: National Institute of Population Studies and Macro International Inc., 200; 89-100.
2. Nyamongo IK. Health care switching behavior of malaria patients in a Kenyan rural community. Social Science and Medicine 2002; 54: 377-386.
3. Ganatra HA, Zaidi AKM. Neonatal infections in the developing world. Elsevier Seminars in Perinatology 2010; 34(6): 416-425.
4. Syed U, Asiruddin S, Helal MSI, Mannan II, Murray J. Immediate and early postnatal care for mothers and newborns in rural Bangladesh. Journal of Health, Population and Nutrition 2006; 24: 508-518.
5. AJK Planning and Development Department. Azad Kashmir at a glance. 2011-12. Muzaffarabad: AJK Planning and Development Department, 2012.
6. Ejaz I, Shaikh BT. Social marketing for early neonatal care: saving newborn lives in Pakistan. World Health & Population 2010; 11(3): 18-24.
7. Pakistan Institute of Legislative Development and Transparency (PILDAT), Pakistan. Pakistan-Azad Jammu & Kashmir politico-legal conflict. Background Paper. (Online) 2011. Available: http://www.pildat.org (Accessed 22 June 2011).
8. AJK Planning and Development Department, Federal Bureau of Statistics, UNICEF Pakistan. Multiple Indicator Cluster Survey (MICS) 2007-08. Muzaffarabad: AJK Planning and Development Department, 2008.
9. Federal Bureau of Statistics. Household Integrated Economic Survey 2007-08. Islamabad.
10. World Health Organization. Sample size determination in health studies, a practical manual. (Online) 1991. Available: http://apps.who.int/iris/handle/10665/40062‎ (Accessed 23 July 2011).
11. Haider M, Haider I. Urban development in Pakistan (Online) 2006. Available: http://www.docstoc.com/docs/159603496/Pak_chapter_ADB (Accessed 4 July 2013).
12. Provincial assembly of the Punjab. Punjab Local Government Bill 2012. Bill No. 23 of 2012.
13. CSS Forum. Civil Service of Pakistan. Military Lands & Cantonments Group (Online). Available: http://www.cssforum.com.pk/css-cadres-training-programmes/specialized-training-program-stp/military-lands-cantonments-group/54592-military-lands-cantonments-group.html (Accessed 6 August 2013).
14. Shaikh BT, Haran D. Treating common illnesses among children under five years: a portrayal of health-seeking behaviours and practices in the northern areas of Pakistan. World Health & Population 2011; 12(4): 24-34.
15. Moran AC, Choudhury N, Khan NZ, Karar ZA, Wahed T, Rashid SF, et al. Newborn care practices among slum dwellers in Dhaka, Bangladesh: a quantitative and qualitative exploratory study. BMC Pregnancy and Childbirth 2009; 9: 54.
16. Winch PJ, Alam MA, Akther A, Afroz D, Ali NA, Ellis AA, et al. Local understandings of vulnerability and protection during the neonatal period in Sylhet district, Bangladesh: a qualitative study. Lancet 2005; 366: 478-485.
17. National Institute of Population Studies, Pakistan. AJK Demographic Health Survey. Islamabad: National Institute of Population Studies, Pakistan, 2010.
18. Bhutta ZA. Community-based interventions for improving perinatal and neonatal health outcomes in developing countries: a review of the evidence. Pediatrics 2005; 115: 519-617.
19. Rosato M. Community participation: lessons for maternal, newborn, and child health. Lancet 2008; 372: 962-71.
20. Maternal and Newborn Health Programme Research & Advocacy Fund. How far can I go? Social mobility of community midwives in Azad Kashmir. Research report. Pakistan: 2012.
21. Bhutta ZA, Ali S, Cousens S, Ali TM, Haider BA, Rizvi A, et al. Interventions to address maternal, newborn, and child survival: what difference can integrated primary health care strategies make? Lancet 2008; 372: 972-989.
