Identifying medically underserved areas, in which people have less access to medical services than in other areas, is essential for planning policy that distributes health resources evenly. Traditionally, some areas have been labeled rural or remote based on available area variables, and subsequently seen as a focus of resource redistribution. Area variables often used for defining rural/remote are population size, population density, main industry, and distance to a large city1-5. In Hiroshima Prefecture, Japan, for example, some municipalities (or parts of municipalities) are administratively designated rural based on their rate of population decrease, economic status, and industry structure. The prefecture government financially supports hospitals that cover rural areas and assigns doctors to these hospitals6. Different definitions of 'rural' are used in other countries for policy-making6. The rural/remote designation created by these definitions is a useful and convenient concept not only for health policy, but also for industry development policies and environmental resources management.
It is not clear, however, how much 'rural' overlaps with 'underserved'. There are several types of rural areas whose nature depends on the variables used for its definition, the cut-off point in each variable, and the size of the geographical unit on which the definition is based3,4. Even a rural area defined in a highly sophisticated manner can still contain areas that are not medically underserved. It is also possible that truly underserved communities are excluded from defined rural areas.
It is not easy to demonstrate how much geographic 'rural' overlaps with medical low-access. Although identifying rural areas is easy when the rural definition is clear, measuring accessibility for people in these areas is quite difficult. In order to measure access to health care, it is necessary to know who had what diseases and how far is it between the community and each facility to which the patients must commute. It is unusual to have such data in a complete form. In patients with some diseases, however, access data can be obtained from public registration systems.
Therefore, this study focused on hemodialysis patients in Hiroshima Prefecture, and evaluated the association between the rurality of the community in which a patient lives and his/her geographic accessibility to dialysis facilities. Dialysis patients usually need to undergo treatment three times a week, and access data of all dialysis patients in the prefecture is available from the municipal registration system. Thus, to what degree 'rural' and 'remote' areas (defined by community-level parameters) actually accords with 'low-access' areas (defined by driving time of dialysis patients) can be determined. Also demonstrated is how the accuracy of the term 'low-access' changes when the size of a geographic unit in analysis is expanded. Based on the results of the analyses, the extent to which the concepts rural and remote can be used to develop effective outreach strategies to underserved populations is revealed.
Study area
Hiroshima, one of the 47 prefectures in Japan, is located in the western part of the country (Fig1). Its population was 2 860 750 according to the 2011 census. For area-based analysis, the second-smallest census block (community) was used as the geographic unit smaller than a municipality (city, town or village). There are 1869 communities in Hiroshima, and two communities were excluded due to lack of age- group population data. In this study, data on all the communities, dialysis patients, and dialysis facilities in Hiroshima Prefecture were used for analyses.
Community-level rurality/remoteness and accessibility parameters
Data on community-level population, area, and the number of primary industry workers were obtained from the 2005 National Census. Primary industries are agriculture, forestry, and fisheries according to the Japan standard industrial classification7.
The following five variables were employed as community-level rural/remote parameters: (i) population size; (ii) population density (/km2); (iii) elderly rate (proportion of residents aged ≥65 years); (iv) agriculture rate (proportion of primary industry workers among the residents ≥15-years); (v) distance to the nearest city with population >50 000. Population size, population density, elderly rate and agriculture rate were used as rural-ness parameters, and distance to the nearest city was the remoteness parameter, based on various Japanese and international rural definitions1-4,6,8-10.
Distance to the nearest city was calculated as driving minutes between the centroid point of a community and the city hall of the nearest city with population >50 000. In this process, network analysis was conducted (ie the shortest travel-path was discerned between two locations on a road network including highways), to find the travel time (in min) by car using geographic information systems (GIS) software ArcGIS v10.0 (http://www.esrij.com/products/arcgis/) and ArcGIS Data Collection Road Network 2011(http://www.esrij.com/products/data/data-collection/). In the latter, the driving speeds of all road segments were classified into 14 categories, according to the type and width of the segment.
As a community-level accessibility parameter, the average one-way driving time (in min) of dialysis patients in the community was employed. Details of the data collection and calculation methods are shown in the next section.
Dialysis patients, facilities, and calculation of driving time
Collection of location information on dialysis patients and dialysis facilities has been described previously11,12. Briefly, postal code information as of August 2011 of all the 7374 patients certified by municipality governments as having first or third grade 'renal disability' were collected (capture rate 100%). Information on postal code and the maximum number of outpatients (capacity) of all 98 dialysis facilities was also collected (capture rate 100%). For a person to be certified as having renal disability, the serum creatinine level must be higher than 5.0 mg/dL or creatinine clearance less than 20 mL/min13. Most patients with renal disease in Japan apply for certification of renal disability when they begin dialysis therapy in order to obtain public financial assistance for the medical treatment. As a preliminary survey, the certified disability status among all the dialysis patients was checked as of June 2011 at seven randomly sampled medical institutions in Hiroshima. Of the 486 dialysis patients, 483 (99.3%) were certified as having a first- or third-grade renal disability11.
For each dialysis patient, one-way driving time to the nearest available facility was calculated in the capacity-distance model11,12. First, patients and facilities were geocoded in GIS according to their addresses. Next, the shortest road-driving minutes for each patient was calculated based on an algorithm programmed for this study. In the algorithm, each facility accepted patients in order of shorter travel time until it reached the limit of its capacity. If a patient was not accepted by the facility in the first step, the patient approached the next-nearest facility in the same manner. The first and second steps were followed until all patients were accepted by one of the facilities. The process was conducted based on the network analysis.
Among the 1867 communities included in this study, 497 did not contain any dialysis patients. However, driving time needed to be calculated for these communities as well as those with dialysis patients. Thus, the shortest travel time between the centroid point of each of the communities and its nearest available facility was calculated as the patient driving time in the community. The nearest available facility was identified in the capacity-distance model in which the request from each no-patient community did not occupy the facility capacity.
Analysis
Correlation analysis was conducted between the rural/remote parameters and the access parameter. Most of the parameters have a skewed distribution in values, so Spearman's rank correlation coefficient was employed.
Next, receiver operating characteristic (ROC) analysis was conducted to evaluate the predictive power of rural/remote to identify low access areas. Communities were dichotomized into low-access and high-access, according to the average driving time of dialysis patients in each community. Three degrees of low-access category were then created by setting the cut-off point for driving time at 20, 30, and 40 min. The 30 min interval was used because most past studies on geographic accessibility to dialysis therapy have used this value14-16; values 10 min shorter and longer were then added. Sensitivity, specificity, positive predictive value, negative predictive value, and area under curve were calculated for each rural/remote definition with regard to its power to identify the low access area defined at each driving time cut-off. The optimal cut-off value of each parameter was determined using the Youden Index17. Area under curve was calculated using the Delong method18.
The predictive power was evaluated not only for each parameter but also for combinations of all the five parameters. For this purpose, a multivariate logistic regression equation was formulated, and the optimal sensitivity and specificity of the combination were calculated. Based on the maximum likelihood method, following logistic regression equation was built:
Probability (low-access) = 1/[1 + exp(-X)], where X = -3.912899 - 0.0000584 * (population) - 0.0002194 * (population density in /km2) + 0.0116272 * (agriculture rate in %) + 0.0047531 * (elderly rate in %) + 0.0586207 * (distance to nearest city in min).
The equation provides the best estimate of a community's likelihood of being low access expressed as a probability between 0.0 and 1.0. All five parameters were used in the regression equation as continuous variables. This method has been utilized, for example, to examine the combined power of multiple risk factors to predict diabetes19,20.
Finally the effect was examined of expanding the geographic unit on the proportion of low-access communities within the unit. Four levels of geographic unit were used: (i) community; (ii) municipality; (iii) secondary healthcare area (niji-iryo-ken); and (iv) administrative 'rural' area (chu-sankan-chi). The area and population sizes increase in this order. Hiroshima Prefecture consists of 1869 communities, 35 municipalities, 7 secondary healthcare areas, and two administrative 'rural'/'urban' areas. The administrative rural area is defined by combination of five national laws and has been used for resource redistribution policies in the prefecture (as mentioned in the Introduction). The five national laws are the Mountain Village Activation Act 2011, the Isolated Island Activation Act 2012, the Peninsular Areas Development Act 2012, the Act on Special Measures for Promotion for Independence for Underpopulated Areas 2012, and the Act on the Promotion of the Improvement of Basic Conditions of Agriculture, Forestry and Other Business in Hilly and Mountainous Areas 2011.
Descriptive statistics and correlation analysis were conducted with IBM SPSS Statistics v21 (http://www-01.ibm.com/software/jp/analytics/spss/products/statistics/). The ROC analysis was performed with MedCalc v12 (http://www.medcalc.org/). Logistic regression analysis was done with STATA v12.1 (http://www.stata.com/).
Ethics approval
Patient data in this study was collected by local governments and used in an anonymous form with permissions from the governments. This study was approved as a study that can be conducted without individual informed consent by the Ethics Committee of Epidemiological Research, Hiroshima University (Epi-412).
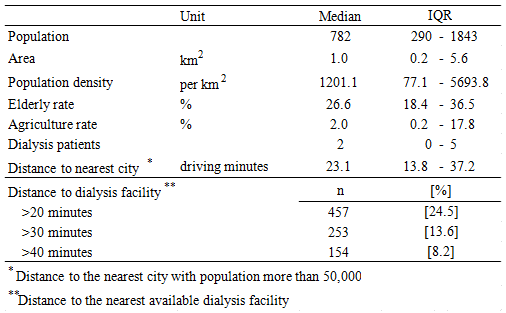
The study area is shown (Figs1,2). Basic statistics of the 1867 communities are given (Table 1). In 75% of these communities, dialysis patients live within a 20 min drive of their treating facility.
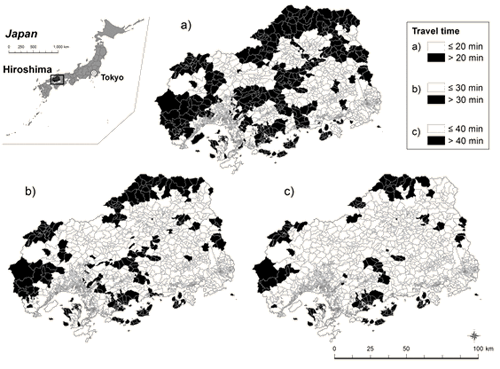
Figure 1: Hiroshima prefecture and its communities (census blocks)
classified according to driving time to the nearest available dialysis facility.
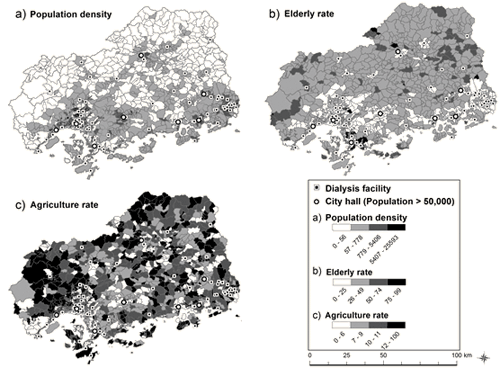
Figure 2: Hiroshima prefecture and its communities
(census blocks) classified according to rural parameters.
Table 1: Characteristics of the communities studied (N=1867)
Results of correlation analysis between a rural/remote parameter and the average driving time of dialysis patients are shown (Table 2). Driving time was negatively correlated with population and population density, and positively correlated with elderly rate, agriculture rate, and distance to nearest city.
Results of ROC analysis are shown (Table 3). Low-access levels were defined as >20 min, >30 min and >40 min driving time. At each level, rural/remote parameters showed good sensitivities. Most specificities, however, were lower than the sensitivities, and as a consequence, positive predictive values were less than 50% in most of the parameters.
Changing the level of 'low access' had a moderate impact on sensitivities and specificities (Table 3). Sensitivities in all the five parameters increased and specificities in four parameters slightly decreased when the cut-off of driving time for 'low access' increased from 20 min to 40 min. However, the sensitivity and specificity in the 'all' parameter and area under curves were stable throughout the three levels of 'low access'. Positive predictive values decreased and negative predictive values increased when the cut-off increased, reflecting the decrease in the proportion of 'low access' communities among all communities. Overall, the level of 'low access' did not have a large impact on the predictive power of each parameter.
The effects of expansion of geographic unit are shown (Fig3). Here, low-access was defined as >30 min driving time. The proportion of low-access communities within a boundary substantially changed when municipalities were merged into secondary healthcare areas (Fig3a,3b). Among the municipalities, the proportion of population living in the low-access communities among the entire population ranged from 0 to 100%. When the geographic unit was expanded to secondary healthcare area, the proportion ranged from 0.9% to 19.9%. This means the expanded border is less accurate in demarcating low-access population than the original version. In the administrative rural area, which is medically and financially supported by the prefecture government due to its 'underservedness', the proportion was 30%.
Table 2: Correlation between travel time of dialysis patients
and community rural/remote parameter (N=1867)
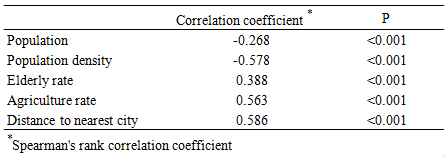
Table 3: Optimal cut-off value and predictive power of rural/remote parameter to
identify low access communities defined as >20, >30, >40 min driving time to dialysis facility
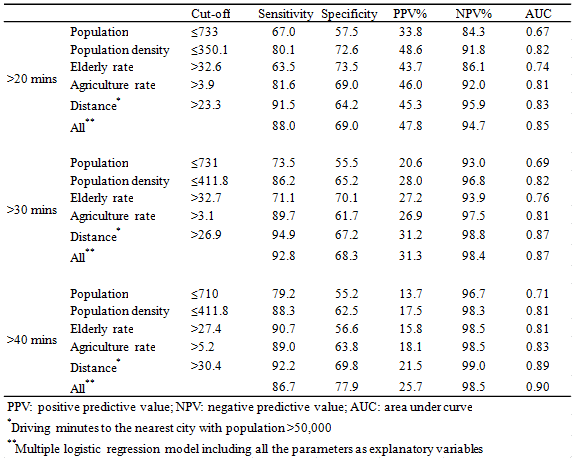
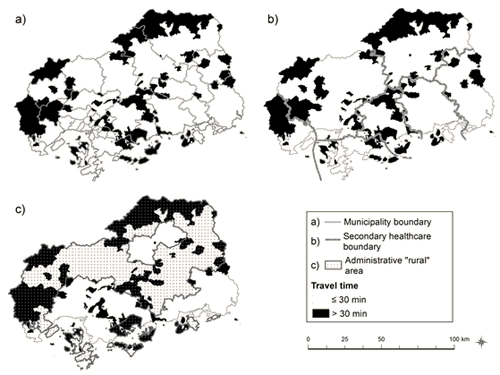
Figure 3: Effects of expansion of the geographic unit: (a) Low-access communities (>30 min)
within each municipality; (b) secondary healthcare area; and (c) administrative rural border.
Discussion
The rural/remote parameters examined in this study correlated well with geographic accessibility to dialysis facilities. By setting an optimal cut-off value, each parameter or combination of parameters seemed to work as a predictor of low-access areas. However, in any definition of rural/remote, and in any definition of low-access, a substantial proportion of low-access communities was excluded from rural areas. In addition, a large number of high-access communities was included in rural areas. Furthermore, the accuracy of the term low-access deteriorated markedly when the geographic unit expanded.
The results suggest that no matter how carefully rural parameters are used, it is not possible to perfectly identify low-access areas. More precisely, where these areas are can only be speculated upon. The size of geographic unit determines the extent to which an area can be described as 'low-access'. Policy-makers may need to take into account the limitations of the rural definition and the geographic unit when they make a decision on rural health policies1,3,4.
There has been an attempt to create a universally applicable definition of what constitutes rurality8. In practical terms, however, each country uses a different definition of what is rural, and this makes rural health research difficult at an international level21,22. The USA, England, Canada and Australia have their own definitions of 'rural', so researchers in these countries study rural health on the basis of those definitions1-4,9. Even within a country, there is no uniform definition of what is rural. In the USA, for example, there are several such definitions3,23. Some health services and epidemiological studies have shown that differences in rural definitions create a critical difference in study results24-26. Many researchers and policy analysts have acknowledged this, and agree that the choice of a definition depends on the purpose for which it is used1,3,4.
The subjects of this study are limited to dialysis patients in Hiroshima Prefecture. The direct application of the results is therefore limited to this part of Japan. If patients with other diseases or in other areas had been studied, the results would have been different. Primary-care facilities, for example, would have been distributed more equitably than dialysis facilities27. Moreover, the cut-off values for a 'long' commuting time are arbitrary. The results of this study should thus be applied cautiously to other settings.
Dialysis costs more than treatment modalities for other chronic diseases so the economic status of a patient can influence his or her access28,29. In Japan, however, the financial burden of dialysis therapy for patients has been minimized. In addition to universal health insurance coverage supported by the government30,31, there is special public financial support available for those certified as 'renal disabled'. With the support system, the co-payment for dialysis therapy for a 'renal disabled' patient is totally exempted or reduced to ¥10,000 (US$100) per month, depending on household income.
The concept of access incorporates financial accessibility, health resource availability and geographic accessibility32. The commuting time used in this study cannot be equated with access, but remains a part of it. However, as mentioned above, patients with end-stage renal disease in Japan have very limited financial barriers to dialysis care. Therefore the availability of human and material dialysis resources and the distance to those resources (both which were measured and included in the concept 'commuting time' in this study), are critical in determining dialysis patients' access to dialysis facilities.
All certified renal disabled people in Hiroshima were included11,12, and the authors' preliminary survey demonstrated that almost all dialysis patients in the prefecture were certified renal disabled. According to the annual report of the Japanese Society for Dialysis Therapy, 7132 patients in Hiroshima were receiving dialysis in 201033, which is close to this study's 7374 patients.
The distribution of patients in this study may be biased by the unique nature of dialysis care in Japan. Dialysis patients in rural areas can relocate to urban areas in order to shorten their commuting time to the dialysis facility, because commuting is literally a matter of life and death. The authors have previously reported, based on the same data, that the prevalence of dialysis patients was lower among rural/remote residents than among urban residents, which suggests that relocation of dialysis patients did occur12.
Past studies have suggested the usefulness of GIS as a model for calculating commuting time of dialysis patients14-16,34-36. Conventional models, however, assume that a patient commutes to the nearest facility in linear or road distance14,34-36. These models are likely to overestimate the geographic accessibility of patients. The capacity-distance model used in this study incorporated both geographic accessibility and facility capacity11,12. The model can simulate access of patients in a more realistic manner than the model without facility capacity37. The capacity-distance model has potential to be applied to people in other parts of the world whose medical conditions require regular commuting.
The geographic unit used in this study is the second-smallest census block. Municipality, secondary healthcare area, and prefecture have often been used as geographic units in policy analyses in Japan38-42. The census block is the smallest available geographic unit that can be connected to census data. There are more than 1800 census blocks in Hiroshima. The use of census blocks enabled the present study's analysis of the distribution of low access areas to be more precise than for municipalities (n=35), secondary healthcare areas (n=7) or administrative rural/urban areas (n=2).
In order to distribute health resource equitably and efficiently, policy-makers need to accurately identify underserved areas. For the construction of data that can be used for such outreach policies, it is necessary to measure access itself and find true low-access areas, rather than, as a surrogate, to designate some areas as rural or remote based on conventional geographic, demographic, economic and distance parameters. The geographic unit of analysis should be as small as possible. In analysis for prefecture-level policy-making, census blocks or even smaller areas are suitable as the unit, rather than the municipality and secondary healthcare area that have been used traditionally.
Acknowledgements
The authors thank the Hiroshima Dialysis Association and the Hiroshima Association of Dialysis Patients, which supported this study. The software used in this study was supplied by the Higher Education Grant Program of ESRI Japan Corp (Tokyo, Japan).
References
1. Minore B, Hill M, Puglise I, Gauld T. Rurality literature review. Ottawa, ON: Centre for Rural and Northern Health Research, Lakehead University, 2008.
2. Australian Institute of Health and Welfare. Rural, regional and remote health: a guide to remoteness classifications. In: Rural Health Series. Canberra, ACT: Australian Institute of Health and Welfare, 2004.
3. Hart LG, Larson EH, Lishner DM. Rural definitions for health policy and research. American Journal of Public Health 2005, 95: 1149-1155.
4. Plessis VD, Beshiri R, Bollman RD, Clemenson H. Definitions of "rural". In: Agriculture and Rural Working Paper series. Ottawa, ON: Statistics Canada, Agriculture Division, 2002.
5. Matsumoto M, Inoue K, Kajii E, Takeuchi K. Retention of physicians in rural Japan: concerted efforts of the government, prefectures, municipalities and medical schools. Rural and Remote Health 10: 1432. (Online) 2010. Available: www.rrh.org.au (Accessed 20 August 2013).
6. Community Empowerment Office, Hiroshima Prefecture. Chu-sankan-chi no shitei joukyo [Current status of administrative rural areas]. Hiroshima: Community Empowerment Office, 2006.
7. Statistics Bureau, Ministry of Internal Affairs and Communications. Japan standard industrial classiffication. (Online) 1996-2008. Available: http://www.stat.go.jp/english/data/kokusei/2000/terms.htm (Accessed 20 August 2013).
8. Directorate for Public Governance and Territorial Development. OECD regional typology. Paris: OECD, 2010; 1-5.
9. Commission for Rural Communities. Defining rural England. Cheltenham, England: CRC, 2007.
10. Matsumoto M, Okayama M, Kajii E. Rural doctors' satisfaction in Japan: a nationwide survey. Australian Journal of Rural Health 2004, 12: 40-48.
11. Matsumoto M, Ogawa T, Kashima S, Takeuchi K. The impact of rural hospital closures on equity of commuting time for haemodialysis patients: simulation analysis using the capacity-distance model. International Journal of Health Geographics 2012, 11: 28.
12. Kashima S, Matsumoto M, Ogawa T, Eboshida A, Takeuchi K. The impact of travel time on geographic distribution of dialysis patients. PLoS One 2012, 7: e47753.
13. Disability and Welfare Section, Hiroshima City. A physician's guide for disability certification. Hiroshima: City of Hiroshima, 2004.
14. Ayyalasomayajula B, Wiebe N, Hemmelgarn BR, Bello A, Manns B, Klarenbach S et al. A novel technique to optimize facility locations of new nephrology services for remote areas. Clinical Journal of American Society of Nephrology 2011, 6: 2157-2164.
15. Judge A, Caskey FJ, Welton NJ, Ansell D, Tomson CR, Roderick PJ et al. Inequalities in rates of renal replacement therapy in England: does it matter who you are or where you live? Nephrology Dialysis Transplantion 2011, 27: 1598-607.
16. White P, James V, Ansell D, Lodhi V, Donovan KL. Equity of access to dialysis facilities in Wales. QJM 2006, 99: 445-452.
17. Youden WJ. Index for rating diagnostic tests. Cancer 1950, 3: 32-35.
18. DeLong ER, DeLong DM, Clarke-Pearson DL. Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 1988, 44: 837-845.
19. Tabaei BP, Herman WH. A multivariate logistic regression equation to screen for diabetes: development and validation. Diabetes Care 2002, 25: 1999-2003.
20. Tabaei BP, Engelgau MM, Herman WH. A multivariate logistic regression equation to screen for dysglycaemia: development and validation. Diabetic Medicine 2005; 22: 599-605.
21. Farmer J, Clark A, Munoz SA. Is a global rural and remote health research agenda desirable or is context supreme? Australian Journal of Rural Health 2010, 18: 96-101.
22. Matsumoto M, Bowman R, Worley P. A guide to reporting studies in rural and remote health. Rural and Remote Health 12: 2312. (Online) 2012. Available: www.rrh.org.au (Accessed 20 August 2013).
23. Vanderboom CP, Madigan EA. Federal definitions of rurality and the impact on nursing research. Research in Nursing & Health 2007, 30: 175-184.
24. Matsumoto M, Inoue K, Kajii E. Definition of "rural" determines the placement outcomes of a rural medical education program: analysis of Jichi Medical University graduates. Journal of Rural Health 2010, 26: 234-239.
25. Hall SA, Kaufman JS, Ricketts TC. Defining urban and rural areas in U.S. epidemiologic studies. Journal of Urban Health 2006, 83: 162-175.
26. West AN, Lee RE, Shambaugh-Miller MD, Bair BD, Mueller KJ, Lilly RS et al. Defining "rural" for veterans' health care planning. Journal of Rural Health 2010, 26: 301-309.
27. Matsumoto M, Inoue K, Bowman R, Kajii E. Self-employment, specialty choice, and geographical distribution of physicians in Japan: A comparison with the United States. Health Policy 2010, 96: 239-244.
28. Rodriguez RA, Sen S, Mehta K, Moody-Ayers S, Bacchetti P, O'Hare AM. Geography matters: relationships among urban residential segregation, dialysis facilities, and patient outcomes. Annals of Internal Medicine 2007, 146: 493-501.
29. Hossain MP, Goyder EC, Rigby JE, El Nahas M. CKD and poverty: a growing global challenge. American Journal of Kidney Diseases 2009, 53: 166-174.
30. Hashimoto H, Ikegami N, Shibuya K, Izumida N, Noguchi H, Yasunaga H et al. Cost containment and quality of care in Japan: is there a trade-off? Lancet 2011, 378: 1174-1182.
31. Ikegami N, Yoo BK, Hashimoto H, Matsumoto M, Ogata H, Babazono A et al. Japanese universal health coverage: evolution, achievements, and challenges. Lancet 2011, 378: 1106-1115.
32. Hall AG, Lemak CH, Steingraber H, Schaffer S. Expanding the definition of access: it isn't just about health insurance. Journal of Health Care for Poor and Underserved 2008, 19: 625-638.
33. The Japanese Society for Dialysis Therapy. Current status of chronic dialysis therapy in Japan. (Online) 2007. Available: http://docs.jsdt.or.jp/overview/ (Accessed 20 August 2013).
34. Rucker D, Hemmelgarn BR, Lin M, Manns BJ, Klarenbach SW, Ayyalasomayajula B et al. Quality of care and mortality are worse in chronic kidney disease patients living in remote areas. Kidney International 2011, 79: 210-217.
35. Toubiana L, Richard JB, Landais P. Geographical information system for end-stage renal disease: SIGNe, an aid to public health decision making. Nephrology Dialysis Transplantion 2005, 20: 273-277.
36. Salgado TM, Moles R, Benrimoj SI, Fernandez-Llimos F. Designing a model to minimize inequities in hemodialysis facilities distribution. Geospatial Health 2011, 6: 5-12.
37. Fryer GE Jr, Drisko J, Krugman RD, Vojir CP, Prochazka A, Miyoshi TJ et al. Multi-method assessment of access to primary medical care in rural Colorado. Journal of Rural Health 1999, 15: 113-121.
38. Kobayashi Y, Takaki H. Geographic distribution of physicians in Japan. Lancet 1992, 340: 1391-1393.
39. Tanihara S, Kobayashi Y, Une H, Kawachi I. Urbanization and physician maldistribution: a longitudinal study in Japan. BMC Health Services Research 2011; 11: 260.
40. Matsumoto M, Inoue K, Bowman R, Noguchi S, Toyokawa S, Kajii E. Geographical distributions of physicians in Japan and US: Impact of healthcare system on physician dispersal pattern. Health Policy 2010, 96: 255-261.
41. Matsumoto M, Inoue K, Farmer J, Inada H, Kajii E. Geographic distribution of primary care physicians in Japan and Britain. Health & Place 2010, 16: 164-166.
42. Takita M, Tanaka Y, Matsumura T, Kishi Y, Kodama Y, Nishimura T et al. Regional social system for specialized medical care in hematologic malignancies: a pilot study. Rural and Remote Health 9: 1106. (Online) 2009. Available: www.rrh.org.au (Accessed 20 August 2013).

