Access to basic health service remains limited in many rural communities within developing countries. To address the lack of health manpower in remote rural areas, villagers are trained and equipped as lay health workers. These health workers are involved in a variety of healthcare programs, such as provision of first aid, promotion of immunization, breastfeeding assistance, environmental sanitation, and community-based infectious disease surveillance1-3.
Laos is situated in South-East Asia, and considered to be one of the world's least developed countries4. The gross national income (GNI) per capita was US$1130 over the year of 2011 (January to December)5. Lay health workers in Laos are called village health volunteers (VHVs). The Lao health authorities depend on VHVs to perform various ongoing tasks, which include conducting community-based surveillance for vital events and basic illnesses such as malaria, aiding in health workers' outreach activities, providing basic first aid treatment, providing health education to communities, and referring patients to healthcare facilities. Health professionals working for a health center or district health office are responsible for supervising VHVs, and it is to these supervisors that VHVs are expected to report monthly regarding their community-based surveillance activities.
One of the challenges faced by the healthcare system in Laos is the lack of integration of the care provided by government medical workers and VHVs. This is particularly evident in the lack or delay of regular monthly reporting of community-based surveillance data by VHVs6,7. This problem makes it difficult to estimate morbidity and mortality nationwide. It also makes it difficult to identify vital events such as pregnancies, births, and deaths that occur outside the reaches of healthcare facilities. Furthermore, because of poor access to geographically remote areas, VHVs experience delays and difficulties in contacting their supervisors to seek advice.
There is evidence to suggest that strategies employing mobile phones can improve healthcare delivery in resource-limited settings8-10. While most relevant studies aimed at improving patient adherence to medication regimens by focusing on communication between health professionals and patients, few focused on communication between health professionals and lay health workers. The latter communications are critical in bridging the gap between the government healthcare system and geographically remote communities.
The current study assessed whether the establishment of a mobile phone communications network between VHVs and their supervisors improved the quality and timeliness of healthcare provision and vital event surveillance reporting in a rural district of Laos.
Study site and population
This study was conducted in Xepone district, Savannakhet province in central Laos (Fig1). The Xepone district is located 500 km from the national capital, Vientiane, and borders Vietnam. Of a total of 134 districts in Laos, Xepone is among the 47 poorest districts in the country in terms of household income and access to education and health services, water and roads11. In 2008, ethnic minorities comprised 75% of the total district population of approximately 45 000. One district hospital and 10 health centers represent the total governmental medical treatment facilities provided for patients in this population. Illnesses such as malaria, diarrhea, and respiratory infections are commonly reported from these healthcare facilities. No private medical treatment facility exists in the district. The Xepone district health office governs these facilities and also supervises VHVs who belong to the 27 villages located in the catchment area of the district hospital. In the remaining 131 villages, health centers supervise VHVs.
The VHV program has been in place in the district since the 1990s. Village executives generally select two or three VHVs from the community of each village who are then trained by health professionals. Village health volunteers are not government employees, nor are they paid on a regular basis by any other entity. However, opportunities exist for VHVs to receive an irregular allowance from vertical programs including the National Immunization Program and the National Malaria Control Program when they attend training or help to conduct an outreach activity. Although the range of typical VHV activities differs according to the requirements and characteristics of each village, all villages in the district are involved in community-based surveillance for vital events.
In accordance with the national health information system, VHVs are requested to complete monthly surveillance reports for vital events at the end of each month; the data are transmitted to the ministry via the health centers and the district- and provincial health offices. In cases where no vital events occur, VHVs are requested to submit a report to that effect.
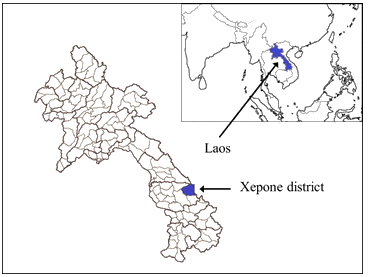
Figure 1: Map of Laos showing the Xepone district.
Intervention
In July 2009, a 2-day workshop was attended by 11 VHV supervisors (representing each health center and the district health office) and 154 VHVs. One representative VHV from each village was invited. At the workshop, the objective of the present study was introduced and mobile phones were given to each participating VHV and supervisor. VHVs were trained until competent in the use of the provided phone. They were instructed to use the phone ad libitum for their VHV work and to share the phone with other VHVs in their villages. During the workshop, VHVs were recommended to deliver monthly reports to supervisors via mobile phone when unable to attend face-to-face supervisory meetings. VHVs were also told that those who find phone use difficult are exempt from the mobile phone-based reporting.
One month after distribution of phones, VHVs who attended the workshop were invited for a one-day follow-up workshop, and various problems that they encountered were addressed, such as loss or breakage of phones, or forgetting of phone-use skills taught at the workshop. Pre-paid cards for phone use (containing the value of 25,000 Lao Kip, equivalent to nearly US$3) were distributed to each VHV on a monthly basis at each supervisory meeting. When VHVs were not able to attend a monthly meeting, they received a pre-paid card from their supervisors on other occasions. During the course of the present study, the authors contacted supervisors several times to provide guidance.
Data collection
During this study, supervisors were responsible for checking whether and how VHVs submitted each monthly report of vital event surveillance. Additionally, supervisors recorded information pertaining to the phone calls they made to and received from VHVs. Information recorded included phone call date, phone call purpose, and village name. Other data collected in this study included general characteristics of VHVs and the availability of phone signal and electricity in their villages, which were collected by interviews with VHVs. Additionally, during the 1-day follow-up workshop VHVs were asked how they coped with the absence of phone signal/electricity in their villages.
Data analysis
The primary outcome in this study was the submission rate of monthly reports of vital event surveillance. This was calculated as the number of villages from which a report was submitted, divided by the total number of villages. The difference in report submission rates was determined by comparing the rate of submission at 1 month before phone distribution with the rates of submission 6 months and 12 months after phone distribution. This was analyzed by the McNemar test. For subgroup analyses, villages were categorized into four groups, according to availability of phone signal and electricity supply. Additionally, differences between means of submitting monthly reports at 1 month before and 6 or 12 months after phone distribution were analyzed by χ2 test. Statistical analysis was performed with Statistical Package for the Social Sciences v17 (SPSS Inc.; www.spss.com). A p value of <0.05 was accepted as statistically significant.
Ethics approval
This study was approved by the Ethics Committee of the Graduate School of Medicine, University of Tokyo, Japan (No. 2168) and the National Ethics Committee for Health Research, Ministry of Health, Lao PDR (No. 172/NECHR). Verbal and written consent was obtained from participants. The participants were aware that their participation would be voluntary and that all data obtained would be confidential. Mobile phones were given to VHVs and not collected after the study.
Characteristics of VHVs and villages
Of a total of 158 representative VHVs, 154 VHVs participated in the study, of which 89.6% were men. VHV median age was 33.5 years, ranging from 18 to 60 years. Educational attainment was mostly primary level (83.1%). The majority (65.6%) reported that they had never used a mobile phone.
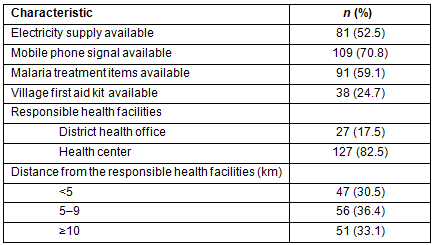
Table 1 shows the characteristics of the study villages. Of a total of 154 villages, phone signal was available in 109 villages (70.8%) and electricity supply was available in 81 villages (52.6%).
Table 1: Characteristics of study villages (N=154)
Phone call content
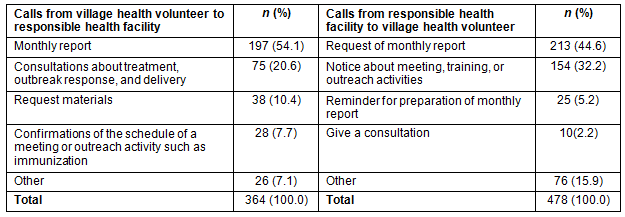
During the 6-month period after the mobile phone distribution, a total of 842 calls were made between VHVs and their supervisors (Table 2). VHVs made 364 calls to supervisors; the most common purpose was regular reporting (54.1%), followed by consultation on a variety of topics including malaria case treatment, vitamin A distribution, and delivery (20.6%). Supervisors made 478 calls to VHVs with the most frequent purpose being to request a monthly report (44.6%) and the next most frequent purpose being to inform VHVs of scheduled upcoming activities (32.2%), such as meetings, training or outreach events including immunizations and health check-ups.
Table 2: Content of phone calls between village health volunteers and their supervisors during 6 months after phone distribution
Monthly report submission frequency
Compared to 1 month prior to phone distribution, the number of villages from which monthly reports were submitted significantly increased from 79 (51.3%) to 127 (82.5%) half a year after the phone distribution (Table 3). The increase was maintained one year after the phone distribution (n=125, 81.2%); Of the 127 villages from which monthly reports were submitted at half a year after phone distribution, 106 submitted monthly reports at 1 year. In contrast, in a group of 36 villages without both phone signal and electricity, there was no increase in the number of villages from which a monthly report was submitted.
One month before the distribution of phones, most reports were made by VHVs during a visit to their supervisors, and reporting by phone was rare (Table 4). In contrast, at both the half-year and one-year post-phone distribution time points, the mobile phone was the most commonly used method for monthly surveillance reporting.
Table 3: Change in frequency of report submission between baseline and half/1-year follow-up
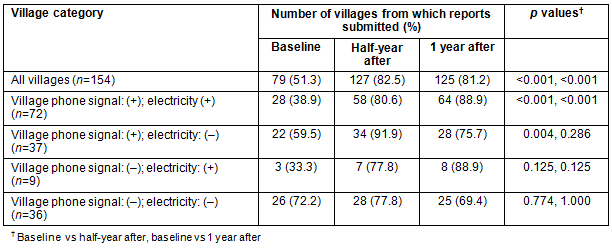
Table 4: Change in means of monthly reporting between baseline and half/1-year follow-up
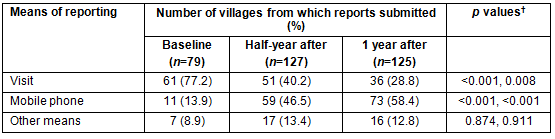
Experiences of VHVs living in a village without phone signal/electricity
Some of the VHVs living in villages without electricity were able to charge their mobile phones by a car battery which is usually used for charging an electronic torch. Some of the VHVs who live in villages without phone signal had little difficulty in using their phones because signal was available at a neighboring village or at a mountain where they work.
This study established a mobile phone communication network between lay health workers and their supervisors, in order to facilitate reporting, the seeking of advice, medical supply requests, and informing schedule for outreach activities. After phone distribution, there was a significant increase in the proportion of VHVs who submitted monthly reports of vital event surveillance.
The observed increase in report submission is of great importance, because vital event surveillance plays a crucial role in aiding government health staff to identify and monitor pregnant women. This in turn promotes delivery of antenatal care services in rural areas, where low utilization has long been a major challenge for the health sector of Laos12,13.
This study provides evidence that the creation of a new mode of communication between VHVs and their supervisors via provision of mobile phones, accompanied by VHV training on mobile phone use, led to a significant increase in frequency of VHV monthly reporting of vital events. However, merely providing VHVs with phones is unlikely to promote VHV reporting. Mobile phones with pre-paid cards were also distributed to VHV supervisors who displayed motivation to participate. Results indicated that supervisors called VHVs to encourage them to submit their monthly surveillance reports. This study's findings were supported by previous studies examining factors influencing lay health worker performance, which have suggested that supportive supervision is essential for sustaining motivation in lay health workers14. The authors believe that the observed increase in reporting was dependent on input and support from the VHV supervisors.
VHVs consulted their supervisors for advice via mobile phone, particularly regarding treatment of common illnesses (eg malaria). VHVs in malaria-endemic villages are trained by the National Malaria Control Program to enable VHVs to rapidly diagnose and treat malaria at the community level, using a diagnostic kit and the available anti-malaria medicines. However, previous studies assessing VHV performance on malaria case management have suggested that some VHVs need monitoring and further case management training15,16. Phone consultation observed in this study, therefore, has the potential to improve malaria case management by VHVs.
Phones were also used to inform the schedule of outreach activities such as planned immunizations and medical check-ups. One study reported that one reason for low immunization coverage in rural Laos was lack of community awareness of village immunization schedules, which results in people being absent from the village during the event17. In this study, health workers informed VHVs of the schedule in advance by phone. Because of this notification, VHVs were afforded the time to informing community people of the events, which have the potential to increase community participation in immunization and health check-ups.
Despite the positive impact of the present intervention, the potential for negative impact should also be noted: after the phone distribution, there was a significant decrease in VHV reports by face-to-face visits with their supervisor. VHVs are recommended to make their monthly reports by visiting their supervisors. In contrast to the study hypothesis that distributed phones would be used for monthly reporting only in cases where VHVs were unable to report by visit, some VHVs chose to report by phone rather than by their accustomed visits, presumably due to ease and convenience. Investigation of this phenomenon is required when scaling-up the present intervention for use in other areas in Laos.
Within the geographical area covered in this study, phone signal and electricity supply were not necessarily available in every village. Results showed that an increase in report submission at 1 year post-intervention was not observed in a group of 36 villages where neither signal nor electricity was available. This may be due to absence of phone signal or electricity. However, baseline differences should be taken into account. The report submission rate was already high in the group before the intervention. It should also be noted that the absence of phone signal/electricity did not necessarily prevent VHVs from using a mobile phone. As shown in the results, some of them were able to overcome the barrier by using a car battery or by making a phone call from an area where signal is available.
The application of phone-based reporting to countries other than Laos is feasible since mobile phone signal has become widely available even in rural areas of many developing countries18. An additional feasibility factor is that implementation cost may not be a critical barrier: mobile phone ownership is increasingly common in individuals in rural areas19, thus the provision of phones to health volunteers may prove unnecessary in other locations.
In conclusion, the establishment of a mobile phone network spanning village health volunteers and their supervisors led to increased monthly report submission and more timely consultations, via improvement of communication between health volunteers and supervisors. This study provides evidence that improved communication has the potential to translate into better health outcomes among community people.
Acknowledgement
This study was supported by the grants for the Research Institute of Humanity and Nature and the National Center for Global Health and Medicine (22-7), Japan.
References
1. Oum S, Chandramohan D, Cairncross S. Community-based surveillance: a pilot study from rural Cambodia. Tropical Medicine & International Health 2005; 10(7): 689-697.
2. Corluka A, Walker DG, Lewin S, Glenton C, Scheel IB. Are vaccination programmes delivered by lay health workers cost-effective? A systematic review. Human Resources for Health 2009; 7(81): 1-13.
3. Lewin S, Munabi-Babigumira S, Glenton C, Daniels K, Bosch-Capblanch X, van Wyk BE, et al. Lay health workers in primary and community health care for maternal and child health and the management of infectious diseases. The Cochrane Database of Systematic Reviews 2010; (3): CD004015.
4. United Nations. Handbook on the least developed country category: inclusion, graduation and special support measures. New York: United Nations, 2008.
5. UNICEF. At a glance: Lao People's Democratic Republic. (Online). Available: http://www.unicef.org/infobycountry/laopdr_statistics.html (Accessed 23 June 2013).
6. Pongvongsa T, Nonaka D, Kobayashi J, Mizoue T, Phongmany P, Moji K. Determinants of monthly reporting by village health volunteers in a poor rural district of Lao PDR. Southeast Asian Journal of Tropical Medicine and Public Health 2011; 42(5): 1269-1281.
7. Jorgensen P, Nambanya S, Gopinath D, Hongvanthong B, Luangphengsouk K, Bell D, et al. High heterogeneity in Plasmodium falciparum risk illustrates the need for detailed mapping to guide resource allocation: a new malaria risk map of the Lao People's Democratic Republic. Malaria Journal 2010; 9(1): 59.
8. Hoffman JA, Cunningham JR, Suleh AJ, Sundsmo A, Dekker D, Vago F, et al. Mobile direct observation treatment for tuberculosis patients: a technical feasibility pilot using mobile phones in Nairobi, Kenya. American Journal of Preventive Medicine 2010; 39(1): 78-80.
9. Lester RT, Ritvo P, Mills EJ, Kariri A, Karanja S, Chung MH, et al. Effects of a mobile phone short message service on antiretroviral treatment adherence in Kenya (WelTel Kenya1): a randomised trial. Lancet 2010; 376(9755): 1838-1845.
10. Pop-Eleches C, Thirumurthy H, Habyarimana JP, Zivin JG, Goldstein MP, de Walque D, et al. Mobile phone technologies improve adherence to antiretroviral treatment in a resource-limited setting: a randomized controlled trial of text message reminders. AIDS 2011; 25(6): 825-834.
11. International Monetary Fund. Lao People's Democratic Republic: poverty reduction strategy paper December 2004 IMF country report no. 04/393. Washington D.C.: International Monetary Fund, 2004.
12. Phathammavong O, Ali M, Souksavat S, Chounramany K, Kuroiwa C. Antenatal care among ethnic populations in Louang Namtha Province, Lao PDR. Southeast Asian Journal of Tropical Medicine and Public Health 2010; 41(3): 705-716.
13. Ye Y, Yoshida Y, Harun-Or-Rashid M, Sakamoto J. Factors affecting the utilization of antenatal care services among women in Kham District, Xiengkhouang province, Lao PDR. Nagoya Journal of Medical Science 2010; 72(1-2): 23-33.
14. Lehmann U, Sanders D. Community health workers: what do we know about them? The state of the evidence on programmes, activities, costs and impact on health outcomes of using community health workers. Geneva: World Health Organization, 2007.
15. Mayxay M, Pongvongsa T, Phompida S, Phetsouvanh R, White NJ, Newton PN. Diagnosis and management of malaria by rural community health providers in the Lao People's Democratic Republic (Laos). Tropical Medicine & International Health 2007; 12(4): 540-546.
16. Phommanivong V, Thongkham K, Deyer G, Rene JP, Barennes H. An assessment of early diagnosis and treatment of malaria by village health volunteers in the Lao PDR. Malaria Journal 2010; 9: 347.
17. Maekawa M, Douangmala S, Sakisaka K, Takahashi K, Phathammavong O, Xeuatvongsa A, et al. Factors affecting routine immunization coverage among children aged 12-59 months in Lao PDR after regional polio eradication in western Pacific region. Bioscience Trends 2007; 1(1): 43-51.
18. Kaplan WA. Can the ubiquitous power of mobile phones be used to improve health outcomes in developing countries? Global Health 2006; 2: 9.
19. Lester R, Karanja S. Mobile phones: exceptional tools for HIV/AIDS, health, and crisis management. The Lancet Infectious Diseases 2008; 8(12): 738-739.



