Introduction
Contact dermatitis of the hands, or hand dermatitis (HD), represents one of the most frequent occupational diseases and is particularly common among working nurses1. Previous studies have also highlighted the problems of HD among nursing students or apprentice nurses in Australia2, Japan3, Denmark4, the Netherlands5 and Germany6. To date, however, no research of this nature has been undertaken in mainland China and published in English. Given that there are at least 1.2 million working nurses7 and approximately 40 000 nursing students graduating every year in China8, they represent a vastly understudied cohort. Similarly, rural populations are often neglected in international research. Of the aforementioned nursing student studies, only two were conducted in rural locations2,3, only one of which was Asian3. Although the booming Chinese economy has brought increased wealth to many metropolitan areas such as Beijing and Shanghai in recent years, industrialisation has not been uniform throughout the country. In this regard, many rural regions have been largely overlooked and a bias towards urban development continues in China, as throughout the world. Given the absence of Chinese student nurse data and the general scarcity of rural nursing research, a preliminary study of HD within a rural, Chinese nursing school was conducted, for what appears to be the first time.
Although medical examinations for HD are expensive, inconvenient and generally impractical, self-reporting questionnaires have been shown to be sufficiently accurate for the detection of HD among large groups1,9. For example, Smit et al.1 demonstrated that the sensitivity and specificity of their HD questionnaire was 100% and 64%, respectively. Similar findings have been seen in other studies9. Simion et al.10 also reported that questionnaires may even offer supplementary information on skin diseases, beyond that of clinical examination. Given these factors, we considered that an epidemiological investigation of HD among Chinese student nurses would be most appropriately undertaken using a previously-validated, questionnaire-based methodology.
Methods
The research protocol was initially reviewed and approved by a Chinese university ethics committee and conducted in accordance with ethical guidelines appropriate to China. A convenience sample of students was selected from a typical hospital-based nursing school in the rural area of Shijiazhuang city. Shijiazhuang is located in Hebei province, and is approximately 280 km south of Beijing. Most Chinese nurses (approximately 99%) are educated in vocational nursing schools, many of which are attached to hospitals7. As such, our study group was deemed to be representative of the wider population of student nurses throughout the country. The study protocol involved an anonymous questionnaire and informed consent was implied when students completed and returned this document. The three-page survey form included both demographic items (such as age, sex, year of study) and HD-related questions. All questions were adapted from previous investigations of nursing students2-6. The English-language version was translated into Chinese by a team of experienced, bilingual healthcare professionals. It was then assessed for accuracy and clarity within a Chinese nursing setting by experienced nursing professionals, before being back-translated into English and rechecked by the original author. Regarding HD, a positive case was defined when one or more specific symptoms occurred in the past 12 months and had persisted for more than 3 weeks or had reoccurred5. Other skin disease questions were asked, with any affirmative response (except HD) considered a positive case for that particular disease.
Questionnaires were distributed to a convenience sample of both grades from the nursing school and collected on the same day. A complete cross-section was obtained by recruiting all students. Data was then entered into a common spreadsheet before being analysed by statistical software. Students were categorised according to their year of study within the nursing school. Statistical differences in prevalence by year of study were calculated using Fisher's exact test for discrete variables and One-way Analysis of Variance (ANOVA) for continuous variables. Statistical associations between HD and demographic items were investigated using the c2 test. Where statistical association with HD were identified, simple logistic regression was also performed to establish a basic risk magnitude. These results were expressed as crude Odds Ratios (OR) with 95% Confidence Intervals (95%CI). Probability values below 0.05 were regarded as statistically significant throughout all analyses.
Results
We recruited a complete cross-sectional cohort of 57 rural nursing students from a university-based nursing school in Hebei Province, China. All of them completed the questionnaire and the group consisted entirely of females. Nursing students at the university of the present study first begin hospital duties in their second year and become completely hospital-based in the third year. As such, the school contained no 1st year students. However, there were 27 students from the 2nd year (47.4%) and 30 from the 3rd year (52.6%). Their average age ranged from 20.6 to 21.5 years (a statistically significant difference: p < 0.01). There were no tobacco smokers at all. Alcohol consumption was also rare among our Chinese nursing students, with only the 2nd years reporting any (14.8%, p < 0.05).
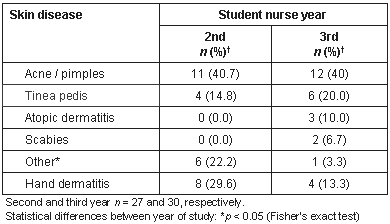
Approximately one-quarter (25.9%) of the 2nd year nurses had previously worked as a nurse or nursing assistant, and this figure dropped to 3.3% in the 3rd year group (a statistically significant difference: p < 0.05). A higher proportion of 3rd year nurses (26.7%) stated that they had suffered from allergies as a child (2nd year, 11.1%). This was in contrast to a family history of allergic disease, which was reported by 29.6% of the 2nd years and only 23.3% of the 3rd year students (Table 1). HD prevalence fell from 29.6% in the 2nd year to 13.3% in the 3rd year and averaged 21.1% across both (a non-significant difference). Systemic allergic disease among family members was found to be statistically associated with HD during this study (p < 0.05). By simple logistic regression, the risk of HD was elevated 4-fold (OR 4.0, 95% CI: 1.0-15.9). The prevalence of miscellaneous skin diseases varied between the two groups as follows: acne or pimples (40.0% to 40.7%), tinea pedis (14.8% to 20.0%) atopic dermatitis (0.0% to 10.0%), skin rashes (0.0% to 6.7%) and other diseases (3.3% to 22.2%: P < 0.05). The average rates for these conditions were as follows: acne or pimples (40.4%), tinea pedis (17.5%), atopic dermatitis (5.3%), skin rashes (3.5%) and other skin diseases (12.3%) (Table 2).
Table 1: Nursing student demographics
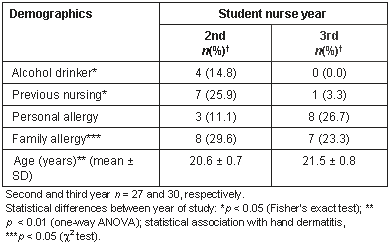
Table 2: Nursing students' skin disease
Discussion
With an overall prevalence of 21.1%, the rural Chinese students suffered less HD than a previous investigation of their Danish counterparts (32% to 39%)4. A different study conducted in the Netherlands also reported a higher rate among working hospital nurses (47.7%)1. Alternatively, the Chinese students' prevalence rate was higher than other investigations of German (3.6% to 9%)6, Dutch (13.5%)5 and Australian (18.5%)2 nursing students. HD among the Chinese cohort was, however, quite similar to previous research conducted in Japan, where 23.8% of the nursing students reported HD occurring over the past 12 months3. Although the prevalence of HD among Chinese nursing students fell between 2nd and 3rd years of nursing study, this decrease was not statistically significant. Regarding rurality, the HD prevalence rate among Chinese students (21.1%) was higher than a similar study from north-eastern Australia (18.5%)2, but lower than another rural investigation conducted in Japan (23.8%)3. Interestingly, HD research conducted in more urban nursing schools has shown the prevalence to range widely, from 3.6% to 39%4-6.
Given this seemingly wide range of variables, it was decided to calculate an average HD rate with respect to rurality. This was achieved by first dividing the results of previous studies (including the present) into either urban or rural subgroups. Prevalence rates in each subgroup (urban or rural) were then added and the total divided by the number of studies. Studies with two different prevalence rates had both rates included and the result divided by two. This was undertaken because both studies indicating two separate results4,6 had, in fact, evaluated HD in two separate groups. As a group, it appears therefore, that rural nursing students suffer HD at a rate slightly higher than their urban counterparts (Table 3). Among them, Chinese nursing students seem to suffer HD at the average rate for their geographical subgroup.
Table 3: Nursing student hand dermatitis prevalence and rurality

The reasons contributing to this result and the complicity of rural environments in HD development are difficult to explain. In one sense, interactions between allergic disease and HD are well known11. It has also been shown that rural people tend to suffer fewer allergies such as hay fever and asthma12,13. Furthermore, childhood farm environments may confer a protective effect against allergic disease in later life14. This latter result probably arises due to a higher environmental exposure to bacterial compounds during farm work13. Interestingly, the prevalence of allergic disease among the rural Chinese nursing students (11.1% to 26.7%) was lower than that documented among their rural counterparts in Australia (43.1% to 46.8%)2 and Japan (33.9% to 47.7%)3. One possible reason for this may relate to the relative lack of industrialisation in rural China when compared with rural areas of Australia and Japan. Intrinsic differences in nursing practice between mainland China and other parts of the world may also have influenced the present study's overall results. For example, nurse burnout has already been documented in China15, suggesting that certain occupational issues such as staffing levels may be problematic. Whether this can be extrapolated to nursing students is difficult to ascertain, however, and needs to be explored in larger epidemiological studies.
Statistical analysis revealed that a family history of systemic allergic disease was significantly associated with the presence of HD during our study. Although systemic allergy is known to be a risk factor in the development of HD among nursing students2,3,5, the contribution of family history of allergic disease has not been reported previously in either rural or urban research, and deserves to be evaluated in larger studies. The importance of this new risk factor is difficult to definitively ascertain, however, because the present sample size was small and no other demographic items were shown to be statistically associated with HD development. Furthermore, the overall rate of allergy among the Chinese cohort (19.3%), was somewhere between that reported by Dutch (11.7%)5, Japanese (39.1%)3 and Australian nursing students (44.8%)2. All of these previous studies showed personal allergy (rather than family allergy) to be an important risk factor for HD. Such results seem to indicate that systemic allergic disease, either among the individual or the family, is an important predictor of HD among student nurses, regardless of ethnicity or rurality. With regard to other skin diseases, our investigation showed that the prevalence of acne among rural Chinese (40.4%) was similar to a previous study of rural Australian nursing students (41.8%)2, although their rate of self-reported tinea pedis was somewhat higher (17.5% vs 7.0%). Again, a larger study of Chinese nursing students will be needed to clarify the significance of this result.
Conclusions
Overall, our preliminary study showed that HD affects rural Chinese nursing students at rates similar to their Japanese counterparts, but higher than other investigations from Germany, Holland and Australia. Regarding rurality, the HD prevalence rate among Chinese students was higher than a similar study from north-eastern Australia, but lower than another rural investigation conducted in Japan. Alternative research undertaken within urban nursing schools has shown the prevalence to range more widely than within our study. However, the generalisability of these results with respect to the wider population of student nurses in mainland China is difficult to ascertain. In one sense, the Shijiazhuang cohort was considered typical of Chinese student nurses, because the majority are trained in hospitals such as that of the present study. However, the present sample size only represented a fraction of the total number of student nurses in mainland China. As such, it must be remembered that this study was intended only as a preliminary investigation, and the results must be treated with caution. Another issue is that the present study's definition of HD may have differed from researchers in other countries and, more importantly, among student nurses in other countries. Again, this suggests that the international comparison of our results should be undertaken cautiously.
Nevertheless, it appears that HD among rural Chinese nursing students has been documented for the first time in English. This preliminary study has also demonstrated that the basic concept for researching rural nursing students is feasible in mainland China. The identification of family allergic disease as a possible HD risk factor was novel, and is worthy of further investigation in larger studies. Further research is now needed to clarify the aetiology of HD among larger student-nurse cohorts, and to evaluate the complicity of newly identified risk factors, such as family allergy.
Acknowledgements
We are grateful to all the student nurses who completed our questionnaire and to Dr Sa Tang from the University of Yamanashi, Japan, for her assistance with the questionnaire translation. Derek R Smith was the recipient of a Japan Society for the Promotion of Science (JSPS) post-doctoral fellowship throughout this project.
References
1. Smit HA, Coenraads PJ, Lavrijsen APM, Nater JP. Evaluation of a self-administered questionnaire on hand dermatitis. Contact Dermatitis 1992; 26: 11-16.
2. Smith DR, Leggat PA. Hand dermatitis among female nursing students in tropical Australia. Nursing and Health Sciences 2004; 6: 109-113.
3. Smith DR, Sato M, Mizutani T, Miyajima T, Yamagata Z. A questionnaire survey of hand dermatitis among Japanese nursing students. Environmental Dermatology 2002; 9: 139-145.
4. Held E, Wolff C, Gyntelberg F, Agner T. Prevention of work-related skin problems in student auxiliary nurses. Contact Dermatitis 2001; 44: 297-303.
5. Smit HA, van Rijssen A, Vandenbroucke JP, Coenraads PJ. Susceptibility to and incidence of hand dermatitis in a cohort of apprentice hairdressers and nurses. Scandinavian Journal of Work Environment and Health 1994; 20: 113-121.
6. Gebhardt M, Seidel A, Bartsch R. Expression of atopic criteria in a population of medical nurses and hairdressers at the beginning of vocational training. Current Problems in Dermatology 1995; 23: 56-63.
7. Xu Y, Xu Z, Zhang J. The nursing education system in the People's Republic of China: Evolution, structure and reform. International Nursing Review 2000; 47: 207-217.
8. Chan S, Wong F. Development of basic nursing education in China and Hong Kong. Journal of Advanced Nursing 1999; 29: 1300-1307.
9. Berg M. Evaluation of a questionnaire used in dermatological epidemiology. Discrepancy between self-reported symptoms and objective signs. Acta Dermato Venereologica (Stockholm) 1991; Suppl.156: 13-17.
10. Simion FA, Rhein LD, Morrison BM et al. Self-perceived sensory responses to soap and synthetic detergent bars correlate with clinical signs of irritation. Journal of the American Academy of Dermatology 1995; 32: 205-211.
11. Meding B, Swanbeck G. Predictive factors for hand eczema. Contact Dermatitis 1990; 23: 154-161.
12. Riedler J, Eder W, Oberfeld G, Schreuer M. Austrian children living on a farm have less hay fever, asthma and allergic sensitisation. Clinical and Experimental Allergy 2000; 30: 194-200.
13. Von Ehrenstein OS, Von Mutius E, Illi S, Baumann L, Bohm O, Von Kries R. Reduced risk of hay fever and asthma among children of farmers. Clinical and Experimental Allergy 2000; 30: 187-193.
14. Kilpelainen M, Terho EO, Helenius H, Koskenvuo M. Farm environment in childhood prevents the development of allergies. Clinical and Experimental Allergy 2000; 30: 201-208.
15. Sun WY, Ling GP, Chen P, Shan L. Burnout among nurses in the People's Republic of China. International Journal of Occupational and Environmental Health 1996; 2: 274-279.
Abstract
Introduction: Although hand dermatitis (HD) is known to affect nursing students worldwide, no studies of this disease have yet been conducted in China. Similarly, rural populations are often neglected in international research.
Methods: A preliminary study of female students from both grades of a hospital-based nursing school was conducted in Hebei Province, China, approximately 280 km south of Beijing. There were 27 students from the 2nd year of the course (47.4%) and 30 students from the 3rd year (52.6%). The study protocol involved an anonymous questionnaire distributed to a convenience sample of both grades from the nursing school. Statistical differences in prevalence by year of study were calculated using Fisher's exact test for discrete variables and One-way Analysis of Variance (ANOVA) for continuous variables. Statistical associations between HD and demographic items were investigated using the c2 test. Where statistical association with HD were identified, simple logistic regression was also performed to establish a basic risk magnitude. Results were compared with similar populations of student nurses from previous studies in Australia, Japan, Denmark, the Netherlands and Germany.
Results: HD prevalence fell from 29.6% in the 2nd year to 13.3% in the 3rd year and averaged 21.1% across both grades. Systemic allergic disease among family members was found to be statistically associated with HD (p < 0.05). Overall, our preliminary study showed that HD probably affects Chinese nursing students at rates similar to that of their Japanese counterparts, but at a higher rate than students in other investigations from Germany, Holland and Australia. The identification of familial allergic disease as a possible risk factor for HD was also novel.
Conclusion: The investigation was conducted as a preliminary investigation, and as such, our results need to be treated with caution. Further research is recommended to more carefully elucidate the prevalence of HD among larger groups of Chinese nursing students.
Keywords: allergic disease, China, hand dermatitis, epidemiology, risk factor, student nurse.
You might also be interested in:
2017 - Rural multidisciplinary training: opportunity to focus on interprofessional rapport-building

