Individuals living in rural communities tend to have poorer health outcomes than their urban counterparts, differences that stem from transportation difficulties, higher unemployment rates and more poverty, a different personal and community culture, some unique health beliefs, as well as limited access to some essential services including palliative care1-3. Palliative care is defined as a philosophy and a unique set of care processes that aim to enhance quality of life at the end of life in order to provide a 'good death' for people, and their families, when death is inevitable4. Given that quality palliative care is now considered a basic human right5, efforts are needed to improve palliative care services in rural communities. A number of definitions of rural community have been put forward, mostly related to geography including population density, size, and distance to an urban center. In Canada, a rural community has been defined as one where individuals live in towns or municipalities outside the commuting zone of larger centers (with populations of 10 000 or more)6.
Indeed, palliative care is influenced by geographical setting, in that gaps exist in rural palliative care related to access, coordination of care, and availability to specialized education and healthcare providers3. Robinson et al3 propose that palliative care in rural communities needs to be understood on the basis of the nature and strengths of these communities. However, many changes have occurred within the system over the past couple of decades that have challenged the strength of these communities and palliative care provision, particularly related to the nursing role. From 1994 to 2004, the location of death (LOD) for many palliative care clients shifted rapidly and substantially from hospital to home7. The shift to home-based palliative care provision and regionalization of services began as money-saving strategies with the goal of better integration and less duplication of services8,9. However, MacLeod et al8 indicate that a reduction in services, particularly in rural and remote areas of Canada, has actually occurred, and this reduction has come with new challenges and consequences that have not been fully acknowledged. Moreover, Stajduhar et al10 state that healthcare system features and cost constraints influence access to end-of-life care due to shortages of staff, beds, supplies, and equipment; time pressures; competing demands such as higher caseloads; rationing or priority-setting care; and increased care responsibilities being put onto family caregivers. Also, there is concern now evident about giving 'too much' home-care service too soon in end-of-life illness trajectories. All of these factors affect rural and urban nurses' ability to determine the need for and provide that amount of service at end-of-life11.
Rural community nurses, in particular, have been confronted with new and existing challenges as a result of these system changes, ones that have complicated their already demanding role in providing palliative care since they have a key role in the coordination and delivery of palliative care services in rural settings. These challenges include separating their personal and professional lives despite living in small communities where they are highly visible, and working in isolated areas while having little opportunity for continuing education8,12-14.
Moreover, the influence of the physical nature of rural communities, along with additional rural aspects of each residential setting can create additional challenges for rural nurses providing palliative care. The physical manifestations of palliative care provided in the home include factors that are unique as compared to the hospital setting15. Factors such as home design, travel time to visit home-care clients, and whether family members or friends are capable of providing home care are important to consider when examining how palliative care is provided in the home.
The purpose of this study was to explore nurses' experiences of providing palliative care in rural communities with a particular focus on the impact of the physical residential setting. This study is a follow-up to previous investigations that examined the practice patterns, self-efficacy in providing palliative care, extent of interdisciplinary collaboration, satisfaction, and perceived barriers and facilitators to providing effective palliative care for nurses working in rural communities in Ontario, Canada14,16. In the first study, a cross-sectional survey of rural and urban nurses showed that rural nurses spent more time travelling and were more confident in their ability to provide palliative care14. Moreover, both rural and urban nurses reported moderate job satisfaction and moderate satisfaction with the level of interdisciplinary collaboration in their practice. This follow-up study sought to explore the perceptions of rural nurses by using qualitative methodology to gain a deeper sense of their experiences in light of the physical aspects of their work environment and residential setting that influenced the way they cared for clients who were dying in the community.
As indicated, this study utilized a qualitative descriptive design to explore nurses' experiences providing palliative care in rural communities17. This specific design was appropriate for this study because it facilitated the gathering of rich, contextual data related to rural nurse experiences of providing palliative care to rural clients with a particular focus on the physical nature of rural communities.
Setting and sample
The nursing organization of Victorian Order of Nurses (VON) is Canada's largest, national, not-for-profit, charitable home and community care organization. In Ontario, this nursing organization offers a variety of services, largely nursing and professional services as well as other community support services, First Nations and Inuit services, volunteer services, and health promotion and education.
Rural and urban VON nurses who completed the initial survey (N=159) were asked if they would be willing to participate in a follow-up interview14. Out of the pool of nurses who agreed (N=35), we sought the perspectives of rural nurses only for this follow-up study (N=24). The nurses selected for a potential interview had self-designated as being 'highly rural'; or rather, all of their clients lived in a community that was (a) at least 80 km away from the nearest large city with a population of 100 000 or more; (b) sparsely inhabited (less than 150 persons per square kilometer); or (c) viewed as having a total area population of 10 000 or less13,14,18.
Once a consent form was signed by each nurse who was willing to participate in a follow-up interview, a telephone interview was scheduled. A trained interviewer conducted the interviews with each nurse (N=21), using a semi-structured interview guide. Questions focused on eliciting information on the nurses' experiences of providing palliative care to rural clients living in the community (Table 1).
Table 1: Interview guide questions

Each 30-60 minute interview was recorded and transcribed. Interview data were organized and analyzed by NVivo v8.0 (QSR International Ltd, Thousand Oaks, CA, USA). Important concepts that emerged from the data were labeled, coded, and then categorized17,19. Initial coding of each transcript was done independently by two individuals to foster credibility and dependability. Any discrepancies were reviewed by the two investigators and discussed until consensus was reached.
A number of methods was used to improve the credibility of the findings. Member checking or 'recycling interpretation' was done with each participant, whereby after each interview, informants were asked to review a 2 page summary of key findings and provide comments relating to the investigators' interpretation of their interview data20. Investigator triangulation was used to minimize any idiosyncratic biases.
By the 21st interview, if not somewhat before, data saturation was reached; that is, no new major ideas or themes were emerging through the later interviews. The 21 interviews were consistent with the general guideline for reaching data saturation typically with 20-30 interviews21.
Ethics approval
This study was approved by the McMaster University Research Ethics Board and the Victorian Order of Nurses Research Ethics Board with whom we partnered to access community nurses (REB 09-272). Written consent to participate in a 1 hour interview was obtained from each participating nurse.
Characteristics of the sample
All of the participants were female, with 90% Registered Nurses and 10% Registered Practical Nurses (Table 2). Almost half of the nurses worked part-time (43%) and the majority worked directly with clients (90%). Two-thirds had over 11 years of rural nursing experience and 77% were over 46 years of age. The majority (76%) reported that they had received some training in palliative care.
Table 2: Characteristics of the sample

Participants were from rural communities in six regions across Ontario: Grey-Bruce (n=4), Porcupine (n=3), Perth-Huron (n=3), Thunder Bay (n=2), Chatham-Kent (n=3), and Hastings-Prince Edward (n=6). The populations of these regions ranged from 84 159 (population density: 0.3/km2; Porcupine) to 155 970 (population density: 22.2/km2; Hastings-Prince Edward)22.
Nature of rural nursing
Nurses described the characteristics of working in a rural community and how it influenced their perception of their role (see Table 3). Many stated that they 'have always lived there' and that they had a strong sense of community and trust with its members, a circumstance that, for the most part, was viewed positively by them as illustrated by this quote:
... you often have in the country what you don't have in the city because you have neighbors that know each other, whether they're just on the rural routes or they're in the little towns like XXX and XXX. People know each other and help each other when they know somebody is sick. I had a young mother that was diagnosed [with cancer] right after her second child was born and lived another four years. But the tiny community of XXX, there wasn't a night that somebody didn't bring a meal or look after her children if needed ... you could in some ways be more isolated in a city area than you are out in the country. (Nurse 2)
Despite the close-knit community in their rural settings, these nurses also reported many challenges. Some nurses expressed concerns about the lack of anonymity of clients since the communities were so small. Some nurses felt that working in a rural community was isolating, especially for nurses who cover large areas on their own with little possible physical or practical support from others:
It's very difficult for us here because it's a small community. Right now there are very few nurses working and we work out of our homes, so there's very little interaction between the nurses for that reason. And CCAC [Community Care Access Center] is the agency that accesses us, but we don't have much communication with them either. Like we report to them but as far as the way it used to be years ago when I started doing home care, it's certainly not as good a system as it used to be ... where we used to all work out of the same office and had a lot of interaction and a lot of communication ... Well we don't have that much contact with other services because they're not involved at the same times as us ... there are no team meetings or anything like that, we work on our own. (Nurse 2)
Many nurses commented about system changes that have occurred over the years, ones that have impacted on their work life and the quality of care that is provided to clients in rural communities. These concerns were partly due to centralization of home-care services. Specifically, the nurses reported that there has been an increase in the quantity of their work while the work quality has declined because more patients are being seen daily but in shorter timeframes. One nurse alternatively stated that she was working less with clients because of increased responsibilities being put on informal caregivers as clients are being discharged sooner from home-care nursing, and with fewer nursing visits prior to this discharge. She also indicated that there is more driving, paperwork, voicemails, and faxes to be addressed in their own unpaid time, as well as increased gas prices with no increased mileage compensation and less personal support worker (PSW) care provision. Personal support worker care is now confined to bathing only, not homemaking or shopping. Moreover, most nurses reported that there was a loss of registered nursing staff over the past 10-15 years, a change that has increased the workload of remaining nurses, with one nurse reporting that her vacation time was denied because there were no nurses to 'cover for her' while she was away:
We're so busy right now because we have had so many staff quit, we're on skeleton crew, in fact none of us are going to be able to get summer holidays we've been told ... and they [nursing agency] took away our pagers so we have to check our voicemail every 30 minutes, lots of the time when we're driving in the car ... it's just really gone bad and we don't need the stress ... there's more and more paperwork for us, unbelievable, like on an average night I am getting over 50 sheets on my fax ... and it's invading my privacy now, I had a friend over at 9:00 at night and my fax machine kept going off, good thing I live alone. (Nurse 8)
Nursing role in providing palliative care in rural communities
Nurses universally highlighted the key role that they have in providing palliative care to clients living in rural communities. One nurse explained:
Well as a home-care nurse we actually cover quite an area here, we cover five towns to the reservation ... and there are small settlements and a lot of isolated areas, farms and homes, so it's rural. So we are the sole caregiver when it comes to palliative care. Often they [clients] are referred to us and then as their condition worsens and they require more care it's up to us to coordinate the services and meet the needs as they change, we need to educate the family on what's coming, explain their choices as to whether or not they want to stay at home or be admitted later on. So I think we play a large role actually. (Nurse 12)
In this regard, nurses described themselves as 'jacks of all trades', as they needed to be a generalist but also needed the specialized skills to deliver palliative care effectively since they were the only ones available to do that. As one nurse stated:
We are all generalists, we are not specialists. So we have to juggle time, distance, weather and skill levels. And I would think in an urban setting the first thing that would come to mind is that you must have a lot more specialists down there so that if I'm stuck on something I would have somebody to call to or ask to come to see the client. (Nurse 1)
Nurses described various ways that a client would be designated as 'palliative'. There were some instances when patients and/or their families could request a palliative care designation. Although most of the time a physician was responsible for the designation of clients as palliative, these nurses stated that their own assessments were also important. However, it was often nurses who had to 'break bad news' to patients and their family members. One nurse elaborated:
Okay, they [physicians] stopped the treatment and that means that they [clients] are palliative and the condition deteriorates and the family is saying to us, 'What is this? Are we looking at them dying now? What's happening here?' So I often find that some patients are left in the dark. I don't know if that's because they don't ask the questions of the doctors or whatever. But we are often the ones that are saying: okay, we're moving into a situation where you are looking at more of an end-stage palliative, you have to start making decisions on how you want to do this. (Nurse 5)
Along with providing education and preparing clients and their family members for what to expect during the end-of-life period, nurses also stated that they provide psychosocial and spiritual support and direct hands-on or physical care to clients. For the most part though, nurses were involved in assessing the capacity and needs of both the client and one or more family members caring for the client and also in determining what resources are needed to assist them. Nurse 1 highlighted, 'What I do is I coordinate the pain and symptom management of the client as well as deal with providing family support ... I see myself as kind of a quarterback.' Nurse 6 added: 'I think our role is to be a facilitator for them to get the services that they need to do the assessment, to find out what physically the person needs and then help them get that.'
Quite often, nurses expressed frustration about the challenges of accessing resources and supplies that were needed to provide optimal palliative care, as one nurse described:
You have a client that declines suddenly and needs a hospital bed for whatever reasons suddenly, you may have to wait a week for that bed to be delivered. Now if family wants it sooner they have to pay for shipping charges themselves to get here, which annoys the heck out of me. (Nurse 15)
Nurses stated that they would use 'palliative symptom control kits' in their practices and felt these kits facilitated optimal palliative care and provided 'easy access' to medications that were needed in emergency situations or during times when physicians were not easily available to them (eg evenings, weekends). However, nurses stated that these kits needed to be tailored to the distances between homes, pharmacies, and doctors; sometimes they would 'stock up' on medications and keep them in the trunks of their cars if they felt they might need additional supplies to cover weekends or unexpected increased demands of the clients.
Nurses also had to work with others, and they described their relationships with other healthcare providers (eg physicians, case managers, social workers, occupational therapists (OT), physiotherapists (PT), chaplaincy, advanced practice nurses). Some were described more favorably than others, and they learned to seek out new ones in urban centers to provide consultation for them if needed. They expressed concern, however, about any case managers' initial assessments being conducted over the phone and not in person, describing this effort as 'disjointed'. When this happened, sometimes nurses would be confronted unexpectedly by extreme filth or poverty in client homes, since they were the first ones to actually visit clients in their homes, thereby creating additional challenges for them in their care provision.
In the more isolated rural areas though, nurses tended to work alone with little involvement from other disciplines:
Sometimes we run across doctors who don't really seem aware of their clients. We might phone and ask them things. There was a lady who had a catheter and had something like ALS [amyotrophic lateral sclerosis] and she kept getting infections. So the one time I was there I had to keep phoning the doctors' office and kept getting an antibiotic. And he said, 'What are her symptoms?' and I said 'Basically she has a UTI [urinary tract infection]', and he just gave me a prescription. I mean he didn't offer to go see her, he just relied on what the nurse told him and he was happy to prescribe a pill. (Nurse 7)
Nurses stated that the most common motives for palliative clients transitioning across settings of care (eg home to hospital, hospital to home, home to long-term care or hospice beds) were crisis-initiated, or due to exhausted caregivers, and/or unmanaged pain. Case managers helped facilitate the transitioning process when they were available to the nurses. Nurses also stated that having a strong, trusting and open relationship with family members enabled smoother transitions as well. Yet barriers would often impede smooth transitions, such as a lack of beds in hospitals, limited other options available to them, and bad weather that created unsafe driving conditions.
Nurses often described transitions across settings of care as 'disjointed' with a 'lack of communication among all the services'. They stated that the lack of family physicians in remote settings was an issue, especially when patients were transitioned back home from hospital without a 'most responsible physician'. One nurse identified that patients' own financial resources or family members, who can assist with care provision/supervision in the home, helped when patients could no longer manage living alone at home.
Nurses stated that often clients who were dying in the community but wished to be transferred to the local hospital could not because it was 'too small to absorb all' and they stated that in these cases, they needed to support families and clients so they could die in their own homes. To do this, nurses would draw from services provided by local churches and service clubs to help meet client and family member care needs at home. One nurse described:
Well it certainly is beneficial to have other services involved because there's lots of needs for these clients for introducing services, you can see that it's a big help. They have home making through Red Cross here and that really helps the family be able to cope and keep the clients at home as long as they possibly can. (Nurse 2)
Ultimately, nurses tried to meet a number of goals in providing quality palliative care to clients and their family members. They viewed a 'good death' as: (a) fulfilling the wishes of both the client and their family members (eg client dies in location of preference); (b) maintaining dignity of client and family; (c) keeping clients and family informed about disease progression and what to expect in the future as end-of-life draws near; (c) keeping clients comfortable and pain-free; and (d) achieving a peaceful death. If a 'good death' occurred, then they felt satisfied in their nursing role in providing palliative care to their rural clients.
Impact of physical residential setting on nurses' provision of palliative care
Many nurses described how physical aspects of working in a rural setting impeded their care provision to clients who were dying in the community. The most common issues that were addressed were the long distances that they travelled to visit clients while, at the same time, having to deal with bad weather when making these trips. One nurse stated that she has travelled in dangerous conditions to visit with families who needed her:
In the rural setting, sometimes you have to drive in some pretty bad weather. One day it was a really bad storm and I had a difficult time even getting there, it was freezing rain, it was a very bad storm, the mom [of a dying child] had paged in and said her daughter was in really bad pain and needed her pain pump increased. So I went, almost put my car in the ditch but I went. Because it [her pain] was so bad I ended up staying there probably 4 hours with her. (Nurse 17)
Nurses described the challenges of managing the distances between clients and how it limited the number of clients they could care for within their work shift:
I'm a visiting palliative care nurse and XXX is a rather large rural area so there's a lot of driving involved. So you spend a lot of time in the car, which, if you are in the city you could use more effectively probably. Although there are some benefits to having time between clients to think about and run things through your head. But yeah, the rural area does come with its own unique set of challenges. (Nurse 14)
Sometimes the physical layout of the home also created challenges to providing care to clients, and at times concern over client safety was raised:
... the one home of the 54 year old with breast cancer, part of the problem was that house was a fire hazard I thought, extremely cluttered and, had an old brick stove back by the door. Boy, if you'd ever started a fire I don't know how you would get out with the old window panes and all this type of thing. (Nurse 20)
Nurses described challenges related to accessing equipment and the increased wasting of intravenous medications when orders change, because deliveries arrived from urban centers only weekly. One nurse reported there is less equipment available to them that is in good working order (eg the one oximeter that was donated by a local pharmacist now needs repairs; a nurse purchased her own tympanic thermometer versus using the existing mercury one). Another nurse commented on the challenges of accessing supplies:
... supplies come down from XXX every Tuesday so that's a little bit of a barrier. One lady we got on a Friday and she died on Sunday, and we never did end up getting the supplies we needed for her. So we try to keep some supplies in our car trunk at all times. But our supplies only come down once a week. Sometimes if the caseworkers are on holidays we have gone one or two weeks without supplies which happened last Christmas. And so that's a little frustrating, running out of sterile gloves, running out of saline, running out of dressing trays, running out of catheters. You sure don't want to get too many ostomies because they are so specific with what supplies they need. So I'm just saying, other than what we have left over here, we do not have many supplies. (Nurse 14)
Some nurses stated that they would find supplies on their own time and purchase these supplies if they felt clients really needed them. For example, one nurse elaborated:
So say you have a client that really needs some Boost [nutrition supplementation] or something and I will say, 'Well is there anybody that can pick that up for you?' And they will say 'We really don't have anybody'. So lots of times I would just go to the grocery store and take it to them on my way there, they just couldn't, there's still a lot of seniors in the community but only one person drives, so that's a bit of a challenge. (Nurse 7)
Many clients that they cared for lived in isolated areas with little support from others; some of these settings were quite impoverished as well, which complicated care delivery. One nurse vividly described her experience of taking on additional tasks for clients, such as doing their laundry at the nurse's own home, in order to meet the client's care needs; and sometimes these activities occurred outside of nurses' working hours:
And there was one lady who had a cottage-like home, 24 kilometers out in the bush outside of town ... in the spring she had an MI [myocardial infarction] so they weren't able to do any more chemotherapy ... so they sent her home with a tube feeding, living out there all by herself and in this little cottage home, the mice had gone through her clothing and sheets ... she just had one of those twin tub washing machines and I ended up after a visit, I said 'Just give me your sheets' and I brought them home myself and actually just did them in my laundry. It took about two weeks for CCAC to realize she needed a PSW there to help her. But the sad thing with that situation was, she was living all alone, way out in the bush with a wood stove. And I was really her support system for weeks and months and so was the PSW that ended up going in there. But at the end she did not want to go into the hospital and she did not have the strength to even put the wood into her wood fire. She was a very, very stoic brave lady and she didn't have a good relationship with her stepdaughter who lived in the south. So on a Friday I realized she was really poor, the PSW actually was kind enough - they could slap her hands if they want to - but she actually went down there morning and night and stoked the fire because she lived maybe 10 kilometers away. And she did so that this lady was not freezing in her bed, she didn't have back-up heating or anything. And she refused to go into hospital until her stepdaughter arrived. And then she went into hospital that Monday morning and she passed away on the Wednesday. (Nurse 4)
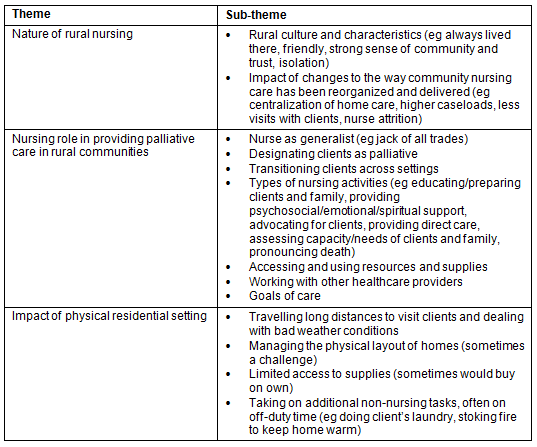
Table 3: Themes and sub-themes emerging from data
Discussion
The findings from this qualitative study highlight the relatively unique experiences of nurses providing palliative care to clients and family members in rural communities as well as the impact of the physical aspects of the residential care setting imposed on them. These findings add to the growing body of knowledge of rural nurses' experiences of providing palliative care in communities that are under-serviced in some areas such as healthcare services and often plagued with a range of challenges in providing optimal palliative care.
Most notably, this study highlights the extreme measures that nurses would take, above and beyond their normal duties, to ensure that individuals who were dying in their home would receive compassionate end-of-life care while working within the physical constraints of the residential setting. Verderber and Refuerzo state that 'palliative architecture holds the power to re-validate the invalid as a human being; it can redefine an explicit role for architecture and for healthcare in providing essential aid in support of medical, emotional, and spiritual care.' (p. 4)23.
The shifting of the LOD from hospital to home raises unique challenges due to the spatial characteristics in which current patient treatment or care takes place. One such challenge, noted by many of the nurses interviewed, is the geographic isolation of rural homes. This isolation can result in lack of personal hygiene, fire hazards, and issues of accessibility, due partly to a reduced frequency of nurse visits. This is not surprising; as Jacobs states, a city's street is safer and better cared for when watched by many neighbors, is well lit, and continuously visited by people walking along its sidewalks24. Patients in hospitals benefit from similar qualities: continuous visitation and constant monitoring made possible by the proximity of caregivers in the area; however, this is not commonplace in rural home settings as supported by these study findings.
The layout of the home is also critically important to consider in residential settings when providing palliative care25. Domestic floor plans of the 19th and 20th century systemize access through their use of separate rooms connected by corridors dedicated to circulation15. Rooms become isolated spaces, accessed by single doors along hallways. If a patient is weak, navigating narrow halls and reaching distant rooms becomes a hazard, especially when they are living alone. This design also complicates the logistics of the visiting nurse, such as her having to move equipment within the home.
Finally, these study findings highlight the underserviced nature of rural communities in terms of providing optimal palliative care and how nurses would draw from urban centers to meet their needs. Crooks et al state that although increased acknowledgement is being given to palliative care needs of increased numbers of persons over age 65 who are living longer, little attention has been given to the consequences of the variation of service delivery and availability between urban and rural areas26. They suggest a secondary palliative care hub as a practical solution to extending the interdisciplinary collaboration and services available in urban centers to rural ones where they are lacking. Its primary goal is to harmonize the current imbalance in the services that exists between the two.
There are limitations to this study. First, data were collected in one province of Canada so results may be different in other provinces and/or countries. This study addressed the perspective of nurses only but would be enriched by hearing first-hand the experiences of clients and family members. Future work is also needed to explore perceptions of PSWs, physicians and other care providers in terms of what they identify as barriers and enablers to providing high-quality palliative care to individuals living in rural communities. Also, nurses were sampled from only one nursing agency with a particular culture of community involvement of its own; hence, the results may not be reflective of all community nurses who work in rural areas.
In summary, the findings from this study add to the growing body of literature on the experiences of nurses working in rural communities in terms of the provision of palliative care and the influence of the physical residential setting there. Nurses described their experiences of working in a rural community and, more specifically, their role in providing palliative care to clients dying in rural communities. These findings are important since nurses have a major role in caring for community-dwelling clients who are dying, but they are confronted with many obstacles along the way. As such, these results should help inform future decisions on how to improve rural residents' access to important palliative services and ways to support them work within the rural community.
Acknowledgements
This study was funded by a Canadian Institutes of Health Research (CIHR) Interdisciplinary Capacity Enhancement (ICE) Team Grant. The authors are grateful for the willingness of the Victorian Order of Nurses for their participation in this project and for their commitment to improving palliative care in the community. This project benefited greatly from the enthusiasm and expertise of Janet Lovegrove.
References
1. Goodridge D, Duggleby W. Using a quality framework to assess rural palliative care. Journal of Palliative Care 2010; 26(3): 141-151.
2. Public Health Agency of Canada (PHAC). Summary Report. How healthy are rural Canadians? An assessment of their health status and health determinants. Ottawa, Ontario: Canadian Institute for Health Information, 2006.
3. Robinson C, Pesut B, Bottorff J, Mowry A, Broughton S, Fyles G. Rural palliative care: a comprehensive review. Journal of Palliative Medicine 2009; 12(3): 253-258.
4. Kehl K, Moving toward peace: an analysis of the concept of a good death. American Journal of Hospice and Palliative Medicine 2006; 23(4): 227-284.
5. Brennan F. Palliative care as an international human right. Journal of Pain Symptom Management 2007; 33: 494-499.
6. Statistics Canada (2012). Rural and Small Town Canada Analysis Bulletin 2012; 9(1): 1-38.
7. Wilson D, Truman C, Thomas R, Fainsinger R, Kovacs-Burns K, Froggatt K, et al. The rapidly changing location of death in Canada, 1994-2004. Social Science and Medicine 2009; 68: 1752-1758.
8. MacLeod M, Browne A, Leipert B. Issues for nurses in rural and remote Canada. Australian Journal of Rural Health 1998; 6(2): 72-78.
9. Williams A, Caron M, McMillan M, Litkowich A, Rutter N, Hartman A, et al. An evaluation of contracted palliative care home care services in Ontario, Canada. Evaluation and Program Planning 2001; 24: 23-31.
10. Stajduhar K, Funk L, Roberts D, McLeod B, Cloutier-Fisher D, Wilkinson C, et al. Home care nurses' decisions about the need for and amount of service at the end of life. Journal of Advanced Nursing 2010; 67(2): 276-286.
11. Gallagher E, Alcock D, Diem E, Angus D, Medves J. Ethical dilemmas in home care case management. Journal of Healthcare Management 2002; 47: 85-96.
12. Hunsberger M, Baumann A, Blythe J, Crea M. (). Sustaining the rural workforce: nursing perspectives on worklife challenges. Journal of Rural Health 2009; 25(1): 17-25.
13. MacLeod M, Kulig J, Stewart N, Pitblado R. (2004). The nature of nursing practice in rural and remote Canada. Available: http://www.cfhi-fcass.ca/Migrated/PDF/ResearchReports/OGC/macleod_final.pdf. (Accessed 22 May 2013).
14. Kaasalainen S, Brazil K, Wilson D, Willison K, Marshall D, Taniguchi A, et al. Palliative care nursing in rural and urban community settings: a comparative analysis. International Journal of Palliative Nursing 2011; 17(7): 344-352.
15. Evans R, Translations from drawing to building: figures, doors, and passages. London: AA Publications, 2005.
16. Kaasalainen S, Brazil K, Williams A, Wilson D, Willison K, Marshall D, et al. Barriers and enablers to providing palliative care in rural communities: a nursing perspective. Journal of Rural and Community Development, 2013; 7(4): 4-19.
17. Sandelowski M. Whatever happened to qualitative description? Research in Nursing & Health 2000; 23: 334-340.
18. Wilson D, Fillion L, Thomas R, Justice C, Vignette AM, Bhardwaj P. Planning and providing for a good death using rural French-Canadian and English-Canadian insights. Reviews in the Neurosciences (Special Issue) 2009; 20(3-4): 313-319.
19. Patton MQ. Qualitative research and evaluation methods, 3rd edn. Thousand Oaks, CA: Sage Publications, 2002.
20. Crabtree B, Miller W. Doing qualitative research, 2nd edn. London: Sage Publications, 1999.
21. Strauss A, Corbin J. Basics of qualitative research: techniques and procedures for developing grounded theory, 2nd edn. Thousand Oaks, CA: Sage Publications, 1998.
22. City-data.com. Available: http://www.city-data.com/canada/Chatham-Kent-Health-Unit.html (Accessed 23 May 2013).
23. Verderber S, Refuerzo B. Innovations in hospice architecture. Abingdon, Oxon: Taylor & Francis Group, 2006.
24. Jacobs J. The death and life of great American cities. New York: Random House, 1961.
25. Granger F. Vitruvius, on architecture. London: W. Heinemann Ltd, 1934.
26. Crooks V, Schurrman N, Cinnamon J, Castleden H, Johnston R. Refining a location analysis using a mixed methods approach: community readiness as a key factor in siting rural palliative care services. Journal of Mixed Methods Research 2011; 5(1): 77-95.

