Introduction
Background
People living in rural and remote areas of Australia have similar health experiences and concerns, irrespective of location. Access to local health services is limited and residents frequently have to travel significant distances or wait for an appropriate health provider to visit their local area. In rural and remote Queensland, Australia, sustainable health services are challenged by low population density, large travelling distances, culturally diverse communities, high prevalence of chronic disease, poor retention of allied health professionals and the prolonged wet season1.
Rural communities require more diverse health services than in the past including promotive, preventative, chronic and social health care2. Their health is poorer than their urban counterparts3-5 and their health priorities and preferred management of specific problems also differ. Recently identified health priorities of rural residents include health care and support for children and young people and healthy ageing3.
Adolescent health
Adolescence is generally viewed as a period of optimum health. However, morbidity and mortality rates during adolescence remain high due to violence, injury and mental health disorders6. Young people are exposed to many of the serious risks to health earlier in life than they were in the past and often engage in behaviours that negatively impact their health status. These include substance use and abuse, premature and unprotected sexual behaviour, eating disorders, delinquency and violence, stress, depression and suicide6,7.
The key areas for concern in adolescent health in Queensland include the rising number of mental health problems and disorders; alcohol, tobacco and other drug use; suicide, attempted suicide and self harm; inappropriate nutrition and physical inactivity8. In Queensland, although deaths related to transport and intentional self-harm have reduced, overall death rates for young people from external causes during the past 9 years remain high9-14.
Rural and urban adolescents report similar health concerns about the use of alcohol, sexual health, stress and depression. However, rural adolescents are more concerned about suicide and teenage pregnancy than their urban counterparts15. Rural females report teenage pregnancy to result from limited suitable entertainment, recreational and sporting activities, 'getting drunk', a belief that it 'would not happen to you', believing that contraception was the males' responsibility and males not wanting to use condoms15,16.
Young rural males perceive stress and depression to be precursors of suicide. Depression is linked to limited access to educational, recreational and employment opportunities and can lead to suicide16. The relationship between unemployment and youth suicide in Australia was established in 1999 by Morrell et al17. In addition, rural and remote areas have higher than urban suicide rates, higher incidences of morbidity and mortality, including hearing loss, from injury associated with machinery and animals4,18 and respiratory illnesses and certain cancers from exposure to farm chemicals18.
School Based Youth Health Nurse Program
A School Based Youth Health Nurse (SBYHN) program, a joint project between Queensland Health and Education Queensland, was introduced in 1998. Through this program nurses work with students, school staff and parents to address health and wellbeing related concerns and problems. Previous work[19] identified the roles and responsibilities of SBYHN in metropolitan and provincial areas of south-east Queensland. These roles include support, referral, health promotion and marketing through individual confidential consultations and health promoting activities, predominantly health education and health information displays. The majority of clients accessing individual consultations were females aged 13 to 16 years. Health issues addressed during consultations were predominantly psychosocial (approximately 75%), others included medical, sexual and sexuality issues, health surveillance and risk-taking behaviours19.
Referral of young people to appropriate health services is a major part of the SBYHN role. As young people living in rural and remote locations may have limited access to health professionals it is important to identify the role of the SBYHN in providing health services and referral to young people in these areas.
Purpose of the study
The purpose of this research was to explore the role of SBYHN in provincial, rural and remote areas of Queensland, to identify those health concerns about which young people in these areas consult the SBYHN, and to examine SBYHN perception of the availability and accessibility of appropriate health services.
Method
Study design
A descriptive cross-sectional self-report, self-administered survey was conducted. This methodology was chosen because surveys are economical methods of data collection and allow in-depth exploration of previously unexplored areas20.
Ethical approval
Ethical approval was granted from the Queensland University of Technology, two of Queensland's three Health Zones (HZ) and individual Health Service Districts (HSD) in the remaining Health Zone. Queensland is divided into three HZ, within each HZ there are a between 11 and 16 HSD.
Sample
Seventy-one SBYHN were eligible to participate in the study. Forty four completed the survey (62%). Of these, 27 (61%) were from provincial, 11 (25%) from rural and 6 (14%) from remote areas. The Accessibility/Remoteness Index of Australia21 was used to determine geographical location.
The majority of respondents were female (n = 40, 91%) with a mean age of 40.8 years (SD 7.15, range 23-54 years) and married or in a defacto relationship (n = 33, 75%). The highest nursing qualifications of nearly half were postgraduate (n = 20, 45%); 18% (n = 8) had a tertiary degree/diploma and 36% (n = 16) held post registration certificates and/or a general hospital certificate. Nursing and child health experience ranged from 4 to 33 years (Mean 18.6 years, SD 7.2) and zero to 20 years (Mean 3.2, SD 3.7) respectively. Half the SBYHN (n = 25, 57%) had previous adolescent experience. Nearly half had been in the SBYHN program for more than 2 years (n = 21, 48%); 11 (25%) had less than 12 months and 12 (27%) had between one and 2 years experience.
Instrument
An instrument was developed from previous research by the author's examination of the roles, responsibilities, challenges and rewards of SBYHN in metropolitan and provincial areas19 and an extensive search of CINAHL and MEDLINE literature targeting the challenges of health professionals in rural and remote areas. A questionnaire was developed, examined by an expert panel of five SBYHN, one with managerial and two with rural and remote nursing experience, to determine content and face validity20. Identified issues were addressed, one section was revised and another area expanded to ensure accurate information was gathered. Panel members were satisfied with these changes.
The final instrument consisted of six sections. Areas addressed in this paper include demographic information; youth health concerns; youth health service provision in provincial, rural and remote areas; accessibility and availability of services; appropriateness of the SBYHN in addressing health concerns; and management of health concerns when services are unavailable.
Procedure
Upon receipt of ethical approval, information about the study was posted to all relevant key personnel in each eligible HSD. A package containing an invitation to participate in the study, a plain language information sheet, a questionnaire and reply paid envelope was posted to each eligible SBYHN. Reminder letters were posted 3 weeks later.
Data entry and analysis: Data were entered into SPSS vers. 11.5 (SPSS Inc; Chicago, IL, USA), searched for outliers and irregularities and 10% of cases randomly checked for data entry reliability. Data were split into the two geographical areas of interest (provincial, and, rural and remote) and examined descriptively by frequency and percentage of responses.
Results
The findings are presented in two sections. In the first section the health concerns that young people consult SBYHN about are identified. Additionally the following is described:
- SBYHN perception of their appropriateness in addressing particular health concerns.
- Most appropriate health professional to address particular health concerns.
- Availability of the most appropriate health professional.
The second section addresses SBYHN management of young peoples' problems when appropriate health services were unavailable.
Health concerns young people discuss with SBYHN during individual confidential consultations
Participants described psychological, drug and alcohol, family conflict, sexual and reproductive health, nutritional and social and isolation concerns of young people which led to consultations with SBYHN (Table 1).
Table 1: Reasons for consultation with SBYHN and SBYHN perception of the appropriateness of the service to meet this health need
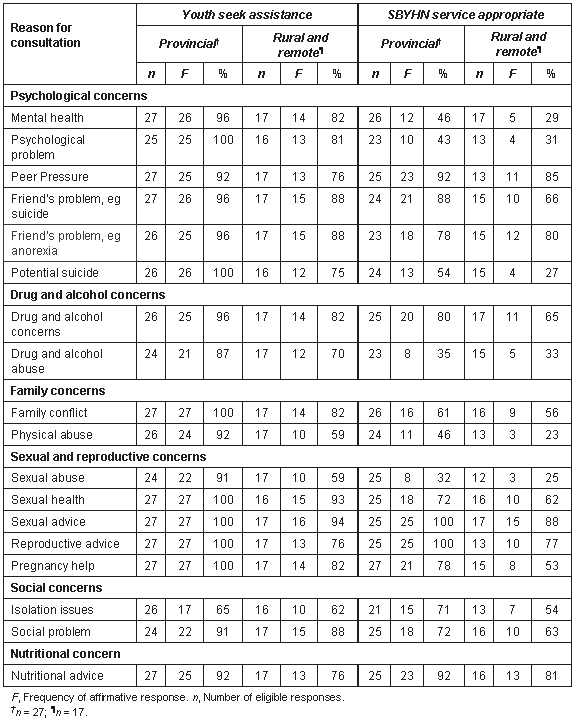
Psychological concerns: Psychological concerns, including mental health, psychological problems, peer pressure, anorexia and suicide, were identified by the majority of SBYHN as reasons for consultation, with many indicating that the service was appropriate to deal with these issues. However, for those who did not consider the SBYHN service appropriate, Child and Youth Mental Health Services (CYMHS) were identified most frequently as the appropriate service to address these concerns. Other frequently reported services were psychologists, general practitioners and Indigenous health workers. Less than half these services were available locally. Some locally available services had long waiting lists; others required parental consent for young people to access the service, making it inaccessible to those not wanting parental involvement. Remote areas were more likely to have a visiting service available and other services required travelling great distances.
Drug and alcohol concerns: The majority of SBYHN indicated that young people consulted them for concerns related to alcohol and drug use and abuse. Respondents considered the service appropriate to deal with general concerns related to drug and alcohol use, but only one-third considered the service appropriate to deal with alcohol abuse problems. Most SBYHN who did not consider themselves the most appropriate for this health concern identified the Alcohol, Tobacco and Other Drugs Service (ATODS) as appropriate. However ATODS were available locally in less than one-third of provincial and rural areas and were unavailable locally in remote areas. Again, young people in remote areas had to either travel long distances or to wait for a visiting service.
Family conflict concerns: SBYHN identified family conflict as a reason for consultation; with over half indicating that the service was appropriate to deal with this issue. Concerning physical and sexual abuse, however, less than half of the respondents considered the service appropriate. SBYHN who did not agree they were appropriate for young people to approach most frequently identified the Department of Family Services as the appropriate service. In provincial and rural areas, sexual assault/abuse services were also recommended frequently. Police and Indigenous health workers were recommended most frequently by SBYHN in remote areas. Access was available locally for the most frequently recommended service.
Sexual and reproductive health concerns: Issues related to sexual health and reproductive concerns included sexual health advice, reproductive advice and pregnancy help, with the majority of SBYHN indicating that young people consulted them for these reasons. The SBYHN service was considered to be appropriate by the majority of respondents. SBYHN in provincial and rural areas who did not consider SBYHN appropriate to address these concerns identified sexual health clinics and Family Planning Services (FPS) as the appropriate services. However, these services were not available in all provincial or rural areas. Most remote area SBYHN recommended locally available GPs. Again, remote areas used visiting services, and young people in provincial and rural areas were required to travel 30 to 100 km for recommended services.
Social and isolation concerns: Isolation issues and social problems were identified as reasons for consultation, and over half of the respondents indicated that the service was appropriate to meet these needs. Youth workers were most frequently reported to be the appropriate person to address these concerns in provincial areas by those SBYHN who did not consider SBYHN appropriate. In rural and remote areas, social workers were recommended frequently. Indigenous health workers were only recommended in rural and remote areas.
Nutrition concerns: Nutritional advice was identified as a reason for consultation with the majority of nurses indicating this issue as a reason for consultation and commenting that the service was appropriate to deal with this issue. SBYHN who did not perceive themselves the appropriate health professional to address nutritional concerns recommended dieticians/nutritionists. However, dieticians/nutritionists were available locally in 29% of the provincial areas where they were recommended, in 17% of rural areas and unavailable in remote areas.
Methods used by SBYHN when health services were unavailable or young people were reluctant to attend the recommended service
Meeting young peoples' needs when services are unavailable: As the availability of allied health services in rural and remote areas is inadequate1,5 SBYHN were asked how they met client needs in these instances. The most frequently reported methods were:
- Phone counselling (n = 22, 26%)
- Using available generalist services (n = 15, 18%)
- Supporting and monitoring the young person until the service is available (n = 9, 11%)
- Accepting the health service limitations in the area and doing the best possible for the young person n = 7, 8%).
- Only five respondents (6%) reported adequate referral services were available.
Most SBYHN had advocated for the required services (n = 36, 86%), twenty-one (84%) from provincial, 10 (91%) from rural and 5 (83%) from remote areas. This was most frequently accomplished through contacting the needed service (n = 17, 35%), the SBYHN Program (n = 12, 25%) and gaining community support (n = 11, 23%). Four SBYHN (8%) had successfully obtained the required service; three from provincial areas and one from a rural area.
With the limited health service support available it was thought that SBYHN might find themselves in a position where they operated outside their prescribed scope of practice (SOP). More than half SBYHN reported this experience (n = 26, 62%); 17 (65%) from provincial, 5 (50%) from rural and 4 (67%) from remote areas. The 26 experiences described included:
- Managing young people who were depressed and suicidal
- Managing young people in an abusive family situation, both physical and/or sexual
- Acting on behalf of young people without parental consent
- Transporting young people to the service without parental consent
- Assistance with pregnancy testing.
Sometimes it is difficult for young people to access allied health services without parental consent22, limiting access to a particular service, and sometimes a young person may be reluctant to attend the recommended service. SBYHN were asked if they had experienced situations where a young person refused to attend the referred service and, if so, how they dealt with these situations. Overall, most SBYHN had dealt with similar situations (n = 38, 86%); 24 (89%) from provincial areas, 8 (73%) rural and 6 (100%) from remote areas. To overcome these deficits SBYHN reported ensuring ongoing support (n = 13, 18%), offering alternative services (n = 11, 16%) and advising young people that their problem/s was out of the SBYHN SOP and specialist help was necessary (n = 7, 10%).
Discussion
The SBYHN program was introduced to address the health and wellbeing concerns and problems of young people in Queensland State high schools23. Young people consult SBYHN through individual confidential consultations about many of the key areas for concern regarding youth health in Queensland, rising levels of mental health problems and disorders; alcohol, tobacco and other drug use; suicide, attempted suicide and self harm; inappropriate nutrition and physical inactivity8. The strength of the school nurse relationship with the students in the school setting can provide an alternative arena to general practice and clinic based services for care, consultation and health promotion24. In rural and remote areas, school based nurses are in an ideal position to provide assessment, referral and intervention programs in the school setting25.
The findings from this study suggests that young people consult SBYHN on a wide range of issues and that SBYHN, provide health information, support young people and facilitate access to referral services. This referral role is an important part of SBYHN practice, however, referral services are not available in all instances.
As expected, provincial SBYHN reported better access to and more varied referral services than those available in other areas. Variety of, and distances to, referral services reduced in rural areas. In remote areas there were more referrals to Indigenous health workers, GPs and visiting services with visits ranging from 2 to 6 weekly. Many referral services SBYHN recommended were not readily available.
When recommended services are absent or unavailable, SBYHN use a variety of methods to assist young people. Locally available services requiring parental consent for a young person to access the service created additional difficulties for young people who may not want parental involvement in the particular problem/concern. Klein found a third of young people, more frequently girls, missed needed care through not wanting to tell their parents26. Most SBYHN had experienced young people refusing to attend a recommended service for this reason. To overcome these difficulties, SBYHN provided ongoing support, suggested alternative services that could assist the young person, and tried to encourage the young person to attend the recommended service. As access to health care reduces risky behaviours, improves health and is an indicator of equity27 these young people are significantly disadvantaged.
The lack of available suitable health services and/or the need for parental consent places SBYHN in a precarious position. They have a young person in need who cannot access necessary assistance. More than half of the respondents had experienced this and felt that they had operated outside their prescribed scope of practice.
Nurses must practice in a safe and competent manner and are responsible for maintaining the competence necessary for current practice28. SBYHN in rural and remote areas can find themselves in a difficult position. They have the trust of a young person who informs them of a potentially life threatening situation, but have neither access to appropriate healthcare for that person, nor the necessary skill to manage, sometimes even in the short term, the person's immediate healthcare needs.
Conclusions and recommendations
Introducing SBYHN into State high schools has provided young people with non-restrictive, confidential access to a health professional, supporting and referring young people with Queensland's key adolescent health concerns. However, their effectiveness is often restricted by limited access to appropriate referral services. Many services are unavailable locally, or only on a visiting basis, challenging SBYHN to support a young person until an appropriate appointment is available, the service visits the town or the young person agrees to access the service. SBYHN are in a position where their practice may extend beyond their scope, a situation which places both the client and the nurse in a vulnerable situation.
To address the gap between SBYHN scope of practice and young people's needs in provincial and, rural and remote areas, the role and scope of SBYHN requires further debate. It must be recognized that SBYHN are practicing at an advanced level and that a broad and comprehensive educational preparation is needed to enable these nurses to meet the wide range of health needs identified.
In addition, the role of the SBYHN in identifying health problems among young people, and facilitating access to referral services cannot be over emphasized. In many ways SBYHN act as a community based medium through which young people can express their health concerns in a safe environment and be enabled to seek further assistance if necessary. However, appropriate services are not always available.
Therefore, the availability of services in rural and remote regions needs consideration. As rural youth are more vulnerable to a number of health concerns, it is imperative that services are available for them. In addition, the issue of parental consent remains a barrier to young people seeking health services and it may be timely for the community to debate this issue. SBYHN are in an ideal position promote health and provide advice to young people, and with adequate referral services would contribute significantly to the improved health of this population.
Limitations
This is a novel nursing role. Previous research has not examined the referral role of SBYHN in provincial, rural and remote areas. The sample for this study was small. However, the response rate was good, 62%, and representative of SBYHN in Queensland. The instrument used, a self report questionnaire, could have limitations; however the tool was based on previous work with metropolitan and provincial SBYHN and validated by a panel of experts. These points need to be considered when considering the findings.
Acknowledgements
This study was supported by a grant from the Queensland University of Technology, Scholarship in the Professions and we thank them for their financial assistance. The authors would like to acknowledge and thank the School Based Youth Health Nurses who participated in this study.
References
1. Bushy A. International perspectives on rural nursing: Australia, Canada, USA. Australian Journal of Rural Health 2002; 10: 104-111.
2. Mahnken J. Rural nursing and health care reforms: building a social model of health. Rural and Remote Health 1; 104. (Online) 2001. Available: http://rrh.org.au (accessed 8 June 2004).
3. Battye K, McTaggart K. Development of a model for sustainable delivery of outreach allied health services to remote north-west Queensland, Australia. Rural and Remote Health 3; 194. (Online) 2003. Available: http://rrh.org.au(accessed 8 June 2004).
4. The National Rural Health Policy Forum & The National Rural Health Alliance. Healthy horizons 1999-2003: a framework for improving the health of rural, regional and remote Australians. Canberra: The Australian Health Ministers' Conference; 1999.
5. Sheahan B. Remote communities, child telepsychiatry & primary health care. Youth Studies Australia 2002; 21: 52.
6. Irwin J, Charles E, Burg S, Uhler Cart C. America's adolescents: where have we been, where are we going? Journal of Adolescent Health 2002; 31: 91-121.
7. De Leo D, Evans R. Suicide in Queensland, 1996-1998: Mortality rates and related data. Brisbane: Australian Institute for Suicide Research and Prevention, 2002.
8. Queensland Government. A strategic policy framework for children's and young people's health 2002-2007. Brisbane: Queensland Government, Queensland Health, 2002.
9. Australian Bureau of Statistics. Causes of Death, Australia, 2000. Catalogue no. 3303.0. Canberra: Australian Bureau of Statistics, 2001.
10. Australian Bureau of Statistics. Causes of Death, Australia, 1994. Catalogue no. 3303.0. Canberra: Australian Bureau of Statistics, 1995.
11. Australian Bureau of Statistics. Causes of Death, Australia, 1995. Catalogue no. 3303.0. Canberra: Australian Bureau of Statistics, 1996.
12. Australian Bureau of Statistics. Causes of Death, Australia, 1996. Catalogue no. 3303.0. Canberra: Australian Bureau of Statistics, 1997.
13. Australian Bureau of Statistics. Causes of Death, Australia, 1997. Catalogue no. 3303.0. Canberra: Australian Bureau of Statistics, 1998.
14. Australian Bureau of Statistics. Causes of Death, Australia, 1998. Catalogue no. 3303.0. Canberra: Australian Bureau of Statistics, 1999.
15. Quine S, Bernard D, Booth M, Kang M, Usherwood T, Bennett D. Health and access issues among Australian adolescents: a rural-urban comparison. Rural and Remote Health 3: 245. (Online) 2003. Available: http://rrh.org.au (Accessed 8 June 2004).
16. Patterson I, Pegg S. Nothing to do: the relationship between 'leisure boredom' and alcohol and drug addiction. Is there a link to youth suicide in rural Australia? Youth Studies Australia 1999; 18: 24-29.
17. Morrell S, Taylor R, Quine S, Kerr C, Wester J. A case-control study of employment status and mortality in a cohort of Australian young people. Medical Journal of Australia 1999; 49: 383-392.
18. Von Essen S, McCurdy S. Health and safety risks in production agriculture. Western Journal of Medicine 1998; 169: 214-220.
19. Barnes M, Courtney M, Pratt J, Walsh A. School-Based Youth Health Nurses: Roles, Responsiblities, Challenges, and Rewards. Public Health Nursing 2004; 21(4): 316-322.
20. Polit D, Hungler B. Nursing research: principles and methods. New York: Lippincott, 1999; 332-333.
21. Information and Research Branch Department of Health and Aged Care. Accessibility/remoteness Index of Australia (ARIA). Adelaide: The University of Adelaide, 1999.
22. Booth M, Bernard D, Quine S et al. Access to health care among Australian adolescents young people's perspectives and their sociodemographic distribution. Journal of Adolescent Health 2004; 34: 97-103.
23. Education Queensland. School-based youth health nurse program. (Online) 2001. Available: http://education.qld.gov.au/curriculum/advocacy/access/equity/students/inclusion/supportive/cgp-nurse.html (accessed 15 December 2004).
24. Rote S. Healthy futures. Nursing Standard 1997; 11: 17.
25. Lamb J, Puskar K, Sereika S, Corcoran M. School-based intervention to promote coping in rural teens. American Journal of Maternal and Child Nursing 1998; 23: 187-194.
26. Klein J, Wilson K, McNulty M, Kapphahn C, Collins K. Access to medical care for adolescents: results from the 1997 Commonwealth Fund Survey of the Health of Adolescent Girls. Journal of Adolescent Health. 1999; 25: 120-130.
27. Klein J, Slap G, Elster B et al. Access to health care for adolescents. Journal of Adolescent Health 1992; 13: 162-170.
28. Australian Nursing Council. Code of professional conduct for nurses in Australia. Dickson, ACT: Australian Nursing Council, 2003.



