The purpose of this introductory article is to set the scene and raise some of the issues which need discussion and debate. It is not a comprehensive overview, but rather a personal reflection, intended to stimulate a response.
I will do this by touching briefly on the following:
- The statistics
- The human side
- The carers
- The response
- Issues in prevention and treatment
The statistics
The statistics are well known to most people, and are mind-boggling in their magnitude. Can we grasp the many zeros in the figures that are infected or have died? In 2001, it was estimated that 4.7 million South Africans were living with HIV and AIDS1. Do any of us really need to see any more?
By way of example I offer no more than the prevalence trends amongst women attending antenatal clinics in my own country, South Africa, which illustrate the steadily increasing magnitude of the problem.
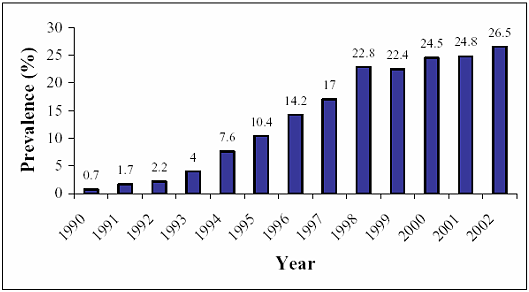
Figure 1: HIV Prevalence trends among antenatal clinic attendees in South Africa: 1990-2002 (From National HIV and Syphilis Antenatal Sero-Prevalence Survey in South Africa: 20021.)
The human side
It is important to give the figures a human face. There are many more stories than we will ever have time or space for. We will share just two (See Part II by Dr Ani Etokidem and Dr Ndifreke Udonwa).
Many issues arise when one considers the situation of rural people in Africa. The lack of rural employment and the difficulties of subsistence farming in a modern economy lead to a continued dependence on migrant labour, in itself a legacy of apartheid and colonialism. This negatively influences family stability, and is often associated with a reality of two families or at least two partners - one in the city and one back home. Together with this, polygamous marriages still flourish in many ethnic groups and the traditional patriarchal society typically seen in rural areas deprives many women of the ability to determine their own future and protect themselves from infection. Tribal traditions have been eroded or destroyed by Christianity, without an adequate replacement system to deal with sexual immorality, which was harshly punished under the old law.
Burial societies and funeral schemes flourish in this new world of AIDS. Many people living in rural areas report that weekends are exhausting due to the number of funerals, at which attendance is expected by everyone in the local community. There is a sense of 'damned if you do, damned if you don't': if you do attend the funerals you have no time to yourself but if you do not you are shunned by the community. The deaths particularly affect the young adult group, with a consequent 'missing generation' becoming noticeable; the society is made up of the old (grandparents) and the young (grandchildren).
The status of the obese has risen enormously - if you are fat you visibly declare that you do not have AIDS. This has serious implications in terms of other health problems! This is evidence of the stigma that still exists. It is manifest in the whispers if anyone is ill, regarding what might be wrong compared to what is stated to be wrong, and the whispers after anyone dies, for the cause is seldom declared forthrightly. For the loved ones who are left behind, the truth may be discovered very late, with a consequent sense of betrayal. As one friend expressed it, the person who dies may rest in peace, but those who remain live with anger.
The carers
The healthcare system in almost all cases is struggling to cope with the pandemic, being inadequately resourced, both in material and human resources. The result of this is that health workers often become increasingly callous and are no longer able to give the care that is needed, beyond the purely physical. This is also a consequence of the absence of care for the carers. To quote one rural colleague:
I do not think that those who are not exposed to the reality of AIDS on a daily basis, and nevertheless have to work with these people can ever imagine the ambivalent feelings and emotions that haunt us. As the epidemic grows I can see more doctors becoming thoroughly discouraged and deciding to move on to safer areas.
Dealing with AIDS patients also stirs up all kinds of emotions in the carer, many of which we would prefer to avoid. This is something I myself have had to confront (see box):

The response
Doctors' responses to the problem are variable, but seem to be grouped into certain strategies. Some doctors try to ignore it; this may have worked in the past, but it is now becoming increasingly difficult. Some become pre-occupied by it - they cannot think or talk about anything else, and every problem is approached with HIV in mind. Others run away from it, either by going into specialities which will remove them from dealing with it directly, or, more typically, by emigrating to a developed country where the prevalence is low enough that they will not have to face it often and where resources are sufficient for AIDS to be treated as another chronic illness. Many doctors, however, learn to live with it and develop coping strategies of one kind or another, often without consciously thinking about it and usually without help or support.
For some, there is a conscious re-examination of motives for practice:
I sometimes have inner conflict in times of emergency. Do you wait for the gloves or visors to arrive, addressing first your own safety, or do you start what needs to be done, hoping that the necessary items will soon arrive. This leads to an examination of motives for practising in such an area, and often throws us back on to our own view of the world, or spirituality. (A rural doctor, pers. comm.)
Internationally, responses of health professionals and governments are also varied. For some there is a reaction of shock and horror at the problem, with the underlying premise that 'it could never happen to us'. (The lesson of Europe, which said this of the massacres in Africa till Kosovo erupted, has not been learnt.) For others there is a distancing of themselves from the issue - it is 'not our problem' - except to the extent to which something has to be done about the refugees in the country concerned. For many there is the response of paternalism; 'shame, poor things, let us send them some money' (which is also a way of avoiding having to deal with the real issues that the AIDS pandemic raises.) Unfortunately this grant-making is usually on their own terms, for example the Bush AIDS Rescue plan for Africa. For some, sadly, Africa is simply written off (yet again): 'nothing good can come out of Africa'. Fortunately there is a substantial minority of people all over the world who genuinely engage with the problem and seek to make a meaningful contribution in partnership with people in developing countries.
Issues in prevention and treatment
AIDS is a global problem; it cannot be ignored by any health professional, society or government. The burden of AIDS in Africa is substantially a result of the socioeconomic and political realities of the past and present, with the global power relationships and the continued exploitation of developing countries by developed nations. (This aspect of the HIV crisis is discussed further in Part IV by Dr John Gillies.) Money without fundamental change is meaningless. The World Trade Organisation has let Africa down again2. 'Free' drugs without restructuring of the global pharmaceutical industry have limited value.
There are lessons in Africa which are important. The relative successes in Uganda are one example3,4.
An oft quoted Chinese proverb states, 'Give a man a fish and you feed him for a day; teach him how to fish and you feed him for his life'. (And if you teach him well enough he can teach others to fish.) But what happens if the lake is in a controlled game reserve and the man is not allowed to enter without paying a fee, or the water has been polluted and the fish are poisonous, or the corrupt police confiscate his fish for arbitrary reasons etc.
Simplistic prevention strategies are no more effective than simplistic treatment strategies. There is a need for fundamental change, on both sides of the developed-developing world divide.
References
1. Department of Health. National HIV and Syphilis Antenatal Sero-Prevalence Survey in South Africa: 2002. (Online) 2003. Available: http://www.doh.gov.za/docs/reports/2002/hiv-syphilis.pdf (Accessed 13 May 2004).
2. South African Press Association (SAPA). WTO talks collapse over North-South rift. (Online)15 Sep 2003. Available: http://iafrica.com/news/worldnews/270695.htm (Accessed 13 May 2004).
3. Hankins C. Changes in patterns of risk. AIDS Care. 1998; 10 Suppl 2: S147-S153.
4. Okware S, Opio A, Musinguzi J, Waibale P. Fighting HIV/AIDS: is success possible? Bulletin of the World Health Organization 2001; 79: 1113-1120.
____________________
This article concludes with the 2003 WONCA World Rural Health Congress' concluding 'Santiago de Compostela Statement on HIV/AIDS' as adopted on September 2003 at the Congress. It is offered here as a suggested way forward.


