Except for skin cancer, breast cancer is the most frequent malignancy affecting women across all racial and ethnic groups. In 2012 an estimated 226 870 new cases of invasive breast cancer along with 63 300 new cases of non-invasive cancer occurred among women in the USA1. In spite of advances in medical technology leading to earlier diagnosis and treatment, breast cancer is the second leading cause of death in women, closely following lung cancer1. An estimated 39 510 breast cancer deaths were expected among women in the USA in 2012. In the USA, breast cancer death rates have steadily decreased in women since 1990, with larger decreases in younger women from 2004 to 2008. During this period, rates decreased 3.1% per year in women younger than 50 years and 2.1% per year in women aged 50 years and older. The decrease in breast cancer death rates reflects progress in earlier detection, improved treatment and, possibly, decreased incidence1.
Cancer stage at diagnosis has a tremendous impact on type of treatment, recovery and survival. In most cases, the earlier the cancer is detected and treated, the higher the survival rate for the patient. The surveillance, epidemiology and end results (SEER) of the overall relative 5-year survival rate (female) of cancer patients (all races) who received diagnosis at different stages in the progression of the disease from 2002 to 2008 was 98.4% for localized, 83.9% for regional, 23.8% for distant or late stages and 50.7% for unknown or unstaged cancers2.
To improve access to screening services, the US Congress passed the Breast and Cervical Cancer Mortality Prevention Act 1990 (Public Law 101-354), which guided the Centers for Disease Control and Prevention in establishing the National Breast and Cervical Cancer Early Detection Program3. The program operates in all 50 states, the District of Columbia, six US territories, and 12 Native American/Alaska Native organizations. In Missouri, the Breast and Cervical Cancer Control Program, now called the Show Me Healthy Women program, started in 1992. The goal of the program is to reduce breast and cervical cancer mortality and morbidity by increasing the availability of cancer screening for early detection of breast or cervical cancer among women in high-risk populations. High-risk women include women whose income is less than 200% of the federal poverty level, those aged less than 65 years, those with little or no health insurance, and women with disabilities4. Various studies have indicated disparities in access to health services.
The purpose of this research was to examine the impact of spatial access to healthcare services on late detection of female breast cancer diagnosis in Missouri, taking into account access and travel time by road to the nearest mammography center and/or hospital. Easy access and shorter distances are necessary to ensure prompt and adequate access to healthcare services is available to all cancer patients, regardless of place of residence and economic situation. Access is defined as an individual's ability to obtain medical services on a timely and financially affordable basis. Factors determining ease of access include availability of healthcare facilities and transportation to them as well as reasonable hours of operation5.
Study design
A cross-sectional retrospective study of female breast cancer incidence in the state of Missouri was employed, using county as the unit of analysis. A geographic information system (GIS) network analysis was used to calculate distance time travel to the nearest healthcare facility.
Data sources and study population
The sample was restricted to Missouri women who were diagnosed with breast cancer and whose cases had been reported to the Missouri Cancer Registry and Research Center (MRC-ARC). The cancer incidence cases covered the period 2003-2008 and were analyzed in two broad 3-year time periods: 2003-2005 and 2006-2008. Cancer cases were categorized into two main groups: 'early' (defined as in situ and localized stages) and 'late' (defined as regional and distant stages). Variables included stage at diagnosis, age, race, county of patient's residence, and year of diagnosis. Socioeconomic status is known to be a powerful predictor of health and wellbeing6-9. However, cancer registries do not collect information on patient socioeconomic status such as educational attainment, income and poverty. Other data sources were used which provide an indirect way of identifying the socioeconomic status of the counties in which diagnosed patients live as well as the distance that patient has to travel to access detection services. This includes the Beale Code or Rural Urban Continuum Code, referencing (TIGER) cartographic boundary, Environmental Systems Research Institute StreetMap, and locations of healthcare facilities, including mammography screening centers.
Analysis
A total of 29 410 cases of breast cancer were diagnosed during the period under consideration. Of these, 874 cases (approximately 3%) were excluded because of missing patient data, including stage at diagnosis, race, and/or place of residence. Two race classifications, Caucasian (white) and African-American (black), were used because these are the major racial groups in the state of Missouri. Analysis was performed on 28 536 cases. Table 1 provides summary descriptive statistics on the study population. Year of diagnosis was categorized into two periods, 2003-2005 and 2006-2008, to assess the differences between the two races. The rural-urban continuum code was used to categorize all the 115 counties into rural-urban types (Fig1). In addition, a new rural-urban type was derived using the SEER grouping as shown in Table 2.
A geostatistical analysis technique was used to calculate proportions of late-stage diagnosis in each county, ie to assess patterns, trends, relationships and geographical distribution of breast cancer diagnosis in Missouri. Network analysis travel time is considered the best measure of distance and therefore an excellent measure of access to healthcare services10,11. Network analysis also provides the benefit of determining the least-cost network paths between a particular origin and destinations. To determine the centroid of each county, each county feature polygon was converted to points. Network analysis also provides the closest facility function, which is travel time zones or service areas of less than 15 minutes, 15-30 minutes, 30-45 minutes, 40-60 minutes, 60-75 minutes and more than 75 minutes around each county centroid (origins) and healthcare facilities (destinations). This calculation took into account access to various types of healthcare service such as hospitals, mammography centers, federally qualified health centers and critical access hospitals in each county. Finally, a thematic layer was generated and overlaid on the county map layer to estimate travel time from each county centroid to the nearest health facility and the impact of spatial isolation on stage at diagnosis.
Table 1: Distribution of study population diagnoses?
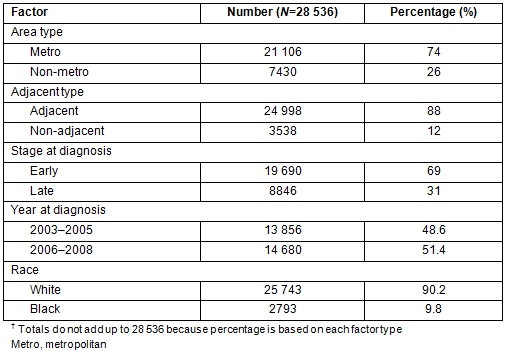
Table 2: Rural-urban continuum code classification
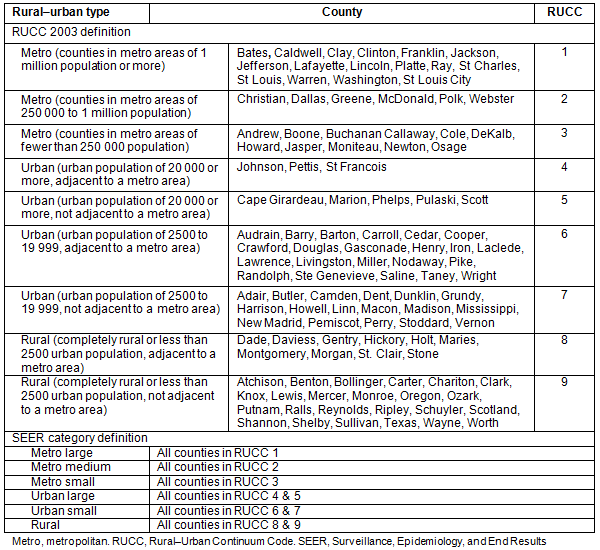
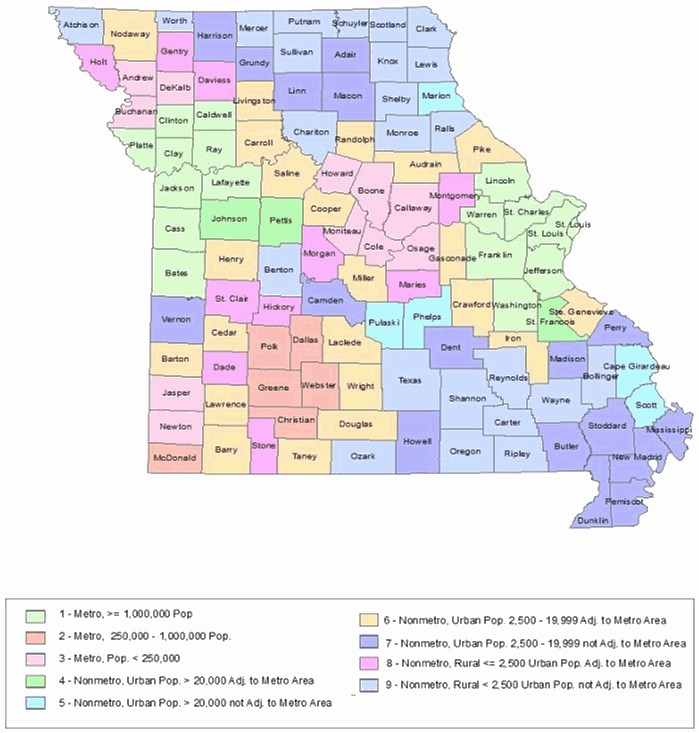
Figure 1: Rural-Urban Continuum Code classification.
Ethics approval
This study did not require review by the University of Missouri Institutional Review Board because existing publicly de-identified cancer data was used.
Of the 28 536 women diagnosed with known breast cancer stages in the study population, 25 743 (90.2%) were white and 2793 (9.8%) were African-American. The small number of black women diagnosed is due to the small number of African-Americans in the state. Overall, between 2003 and 2008 the breast cancer incidence rate in Missouri was 289.6 per 100 000 women.
Figures 2 and 3 present the changes in the proportion of late-stage diagnosis over the study period between the two main racial groups and rural-urban types. Although more white than black women were diagnosed with breast cancer, the racial distribution of the data into black, white and place of residence revealed a large disparity across regions of residence and late stage at diagnosis. Among African-Americans, from 2003-2005 more than 50% of all late-stage diagnoses occurred in metropolitan (metro) medium (55.6%) and completely rural counties (66.7%). Metro small (42.3%), urban large (47.4%) and urban small (44.9%) counties recorded more than 40% of late-stage diagnoses. Most of the diagnoses of white women were reported in urban small (32.2%) and rural (32.3%) counties. Between 2006 and 2008, again, the proportion of late-stage diagnoses among black women was the highest. More than 40% of all black late-stage diagnosis cases were in metro small and urban small counties, whereas for white women most of the late-stage diagnoses occurred in completely rural and urban small areas.
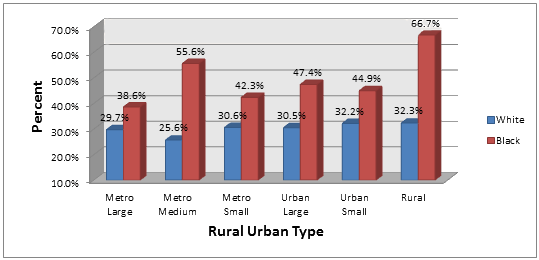
Figure 2: Advanced breast cancer distribution by race and county size, 2003-2005.
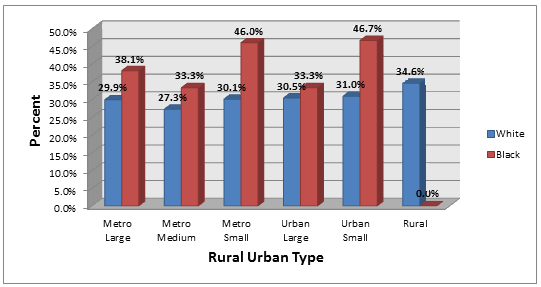
Figure 3: Advanced breast cancer distribution by race and county size, 2006-2008.
Impact of travel time on diagnosis
Figure 4 shows the location of hospitals in Missouri and travel time in minutes from the centroid of each county to the nearest hospital. In general, accessibility to hospitals is fairly distributed among all counties. Women from disadvantaged non-metro areas have the same level of access to hospitals to those in metro areas if they are within a travel time of 15-30 minutes. Women residing in 22 out of the 115 counties have to travel between 45 and 75 minutes for medical care. Of those 22 counties, 13 (Benton, Clark, Carter, Hickory, Knox, Lewis, Mercer, Morgan, Oregon, Ozark, Reynolds, Shannon and Shelby) are considered rural, six (Crawford, Douglass, Iron, Mississippi, Taney and Wright) are urban small and three (Christian, Dallas and Webster) are metro medium.There are approximately 180 cancer screening facilities throughout the state that provide free cancer screenings. Compared to the location of hospitals (Fig4), however, access to mammography services is not evenly distributed (Fig5). For instance, while the St Louis City and County area is served by more than 20 mammography centers, women in some counties do not have access to a single center. The travel distance from each county centroid to the nearest mammography facility revealed that women living in 19 non-metro rural and four metro counties have a travel time of more than 45 minutes one way by car for mammography services (Fig5). Out of the 19 non-metro counties, nine (Carter, Clark, Mercer, Montgomery, Ozark, Reynolds, Shannon, Texas and Worth) are located in completely rural areas. Another nine (Camden, Cooper, Dunklin, Gasconade, Harrison, Nodaway, Perry, Saline and Taney) are urban small counties, while Pulaski is classified as an urban large county. The four metro counties Franklin, Lincoln and Warren are considered as metro large counties, while McDonald is classified as a metro medium county. Clark, Carter, Mercer, Ozark, Reynolds, Shannon and Taney counties are non-metro regions that do not have access to hospital and mammography services (Figs 4,5).
Compared with the existing pattern of hospitals and mammography services the map of locations of critical access hospitals (CAHs; Fig6) shows that women located in the south central and southern part of the state are required to travel the longest distance (more than 75 minutes) one way for their medical care. However, with the exception of part of the southwest regions in which women have to travel over 75 minutes for healthcare services (federally qualified health center; Fig7), access is available in both metro and non-metro counties within a travel time of 30 minutes (Fig7).
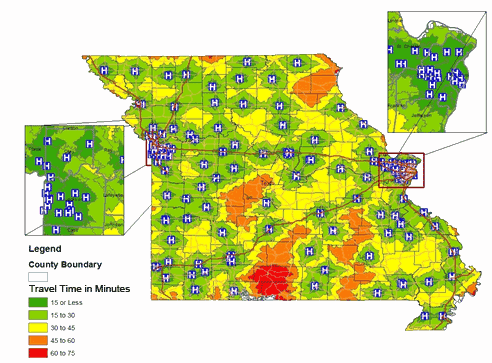
Figure 4: Travel time to nearest hospital in Missouri.
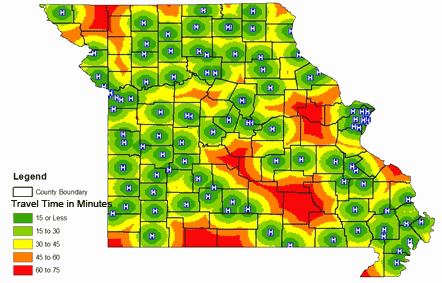
Figure 5: Travel time to nearest mammography center in Missouri.
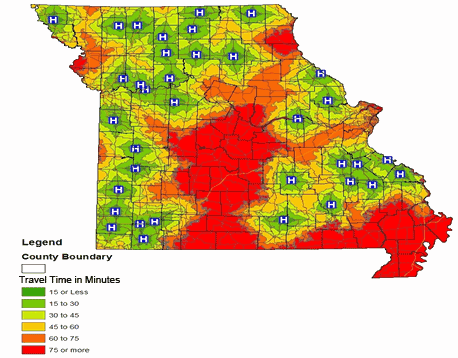
Figure 6: Travel time to nearest critical access hospital in Missouri.
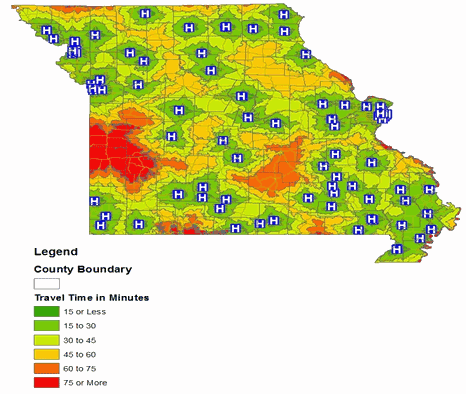
Figure 7: Travel time to nearest federally qualified health center in Missouri.
Discussion
Previous studies conducted in the USA and internationally have shown that geographic information systems (GIS) provide an effective way of identifying access to healthcare services in the community. Wang et al12, Owen et al13 and Oppong and Hodgson14 have all applied GIS techniques to better understand and address issues affecting access to health services in various countries. Wang et al12 used spatial analysis methods to create a measure of spatial access to primary care and mammography clinics on late-stage breast cancer diagnosis in Illinois. Findings from the study indicated that spatial access to primary care doctors and travel time are critically important in achieving high rates of early breast cancer detection in Illinois and surrounding states. Consequently, living in areas with poor geographical access to primary care physicians increases the likelihood of late-stage diagnosis for breast cancer12.
This study contributes to the use of GIS in addressing access to health care by looking at how geographical place of location and travel time affect stage at breast cancer diagnosis in Missouri. This study's analysis shows that geographical differences exist between metro and non-metro areas in terms of access, distance traveled to the nearest healthcare facility and stage at breast cancer diagnosis. For example the GIS results on hospital location showed that women from most non-metro areas have almost the same level of access to hospitals to those in metro areas when distance traveled was considered. Unlike hospitals, mammography screening centers are unevenly distributed. Women residing mostly in completely rural to small urban counties (based on the degree of urbanization and adjacency to a metropolitan areas) have to travel the longest distances. Counties such as Mercer, Nodaway, Ozark, Shannon, Texas and Worth do not have a single screening center. Women in these counties have to travel a distance of more than 60 minutes minimum one way if they are to benefit from the Show Me Healthy Women program free breast screening and cervical cancer services. This finding highlights the predicament of women in these counties regarding access to breast cancer screening services in Missouri. In contrast, counties such as Boone, Jackson and St Louis City and County have an abundance of healthcare facilities within a maximum of 30 minutes travel.
Almost one-fifth of the US population lives in a rural area15. In 1997, Congress established critical access hospitals (CAHs) to strengthen rural health care infrastructure. CAHs are to improve rural health care access for patients residing in rural areas16. Federally qualified health centers are community-based health centers that serve populations with limited access to health care. These include low income populations, the uninsured, those with limited English proficiency etc16. Federally qualified health centers are required to provide a detailed scope of primary health care as well as supportive services to all patients, regardless of their ability to pay. Even though the purpose of these facilities is to bridge the disparity gap in health care access between rural and urban areas, almost all the rural counties in Missouri do not have a single type of these facilities to promote equal health care access.
Disparities in breast cancer between white and black women have been well documented over the years17,18. Racial disparities, especially in access, diagnosis, treatment and survival of breast cancer among different racial and ethnic groups, have been identified as major factors impacting cancer incidence and mortality. African-American women are known to have lower incidence and prevalence rates of breast cancer than white women, but they have a higher mortality rate and a lower survival rate1,19. Causes for these disparities have been linked to social, behavioral and economic factors such as persistent inequalities in access to care, unhealthy environments and racial discrimination12,20-25. In Missouri, the African-American population is overwhelmingly located in larger population counties such as Boone, Cole, Greene, Jackson, and St Louis City and County. Results from this study revealed that the percentage of late breast cancer diagnosis for African-American women was always higher than that for white women in all rural-urban types of residence even though the majority of cases diagnosed with cancer reported to the Missouri Cancer Registry were white women.
Aside from racial differences in stage at diagnosis and distance travel time to the closest health facility, the present study's findings suggest that, overall, women located in rural non-metro counties are at risk of being diagnosed with more-advanced breast cancer than those dwelling in metro counties. Another important finding the authors want to address is the proportion of late-stage diagnosis among black women between 2006 and 2008. The study analysis indicated that percentage of black women diagnosed in rural counties during this period was zero. However, this could be because the proportions of black women diagnosed were either unstaged or of an unknown stage, or even part of the missing data, and hence were excluded from the analysis.
Place of residence and neighborhood socioeconomic characteristics are usually considered to affect health outcomes and quality of life. For cancer patients, studies have shown that individuals living in rural and poor areas are more likely not to utilize cancer screening services and tend to be diagnosed at a later stage compared with individuals living in affluent areas7. McLafferty and Wang8, Wang et al12., Campbell et al20 and Campbell et al22 reported that higher risk of late-stage cancer diagnosis is prevalent among rural residents who face long distances in accessing cancer screening services.
In contrast to the above findings, Henry et al6, Henry et al7, and Warner and Gomez26 found a weak association between geographic place of measures and differences in the risk of late-stage breast cancer. Similarly, a study in New Hampshire examining breast cancer stage at diagnosis and geographic access to mammography screening from 1998 to 2004 concluded that most women living in New Hampshire have good geographical access to mammography, and no indication was found that travel time or travel distance to mammography significantly affected stage at breast cancer diagnosis27. Health insurance, age and marital status were the major factors associated with later-stage breast cancer27. This study corroborates previous findings7,8,12,20,21 that limited availability of mammography screening center and other health services, and long-distance travel, may be barriers to women in rural areas to receive timely diagnoses for breast cancer.
Limitations
A major limitation of this study is that cancer registries do not collect patient information about socioeconomic status such as level of education, income and poverty. Hence, these important variables were not included in the analysis. Also, county centroid rather than actual addresses of cancer patients was used to measure distance travel to the closest healthcare facility available in each county. This was done to protect patient privacy and confidentiality.
Breast cancer remains the leading cause of mortality among women across all racial and ethnic groups in the USA. The findings from this study have highlighted the distribution of female breast cancer between 2003 and 2008 in Missouri. Results on access and travel distance to the nearest healthcare facility have indicated that women living in areas with limited access are more likely to be diagnosed with late-stage breast cancer. The approach used in the study has provided useful information on provision of healthcare access and accessibility regarding what healthcare services are needed, where and for whom coverage is lacking. This analysis can serve as a guide to policy-makers in the state of Missouri about deliberation on healthcare resource allocation as well as developing strategies and prioritizing targets aimed at improving access to healthcare services to all Missourians regardless of geographical location. Finally, due to the importance of socioeconomic factors on health and wellbeing, and acknowledgement in the Breast and Cervical Cancer Mortality Prevention Act that socioeconomic factors increase the risk of late-stage cancer detection, it is recommended that cancer registries collect data on education, ethnicity and poverty. Incorporating more socioeconomic variables into a spatial model like this one would enhance the ability of policy-makers to identify specific locations that would greatly benefit from access to additional cancer screening resources.
References
1. American Cancer Society. Cancer facts and figures 2012. Atlanta, GA: American Cancer Society, Inc., 2012.
2. National Cancer Institute. Surveillance, Epidemiology, and End Results (SEER) (SEER). Stage distribution and 5-year relative survival by stage at diagnosis for 2002-2008, all races, females 2012. (Online). Available: http://seer.cancer.gov/statfacts/html/breast.html (Accessed 11 April 2012).
3. Centers for Disease Control and Prevention. National Breast and Cervical Cancer Early Detection Program. (Online) 2011. Available: http://www.cdc.gov/cancer/nbccedp/legislation/law.htm (Accessed 11 April 2012).
4. Department of Health and Senior Services. Show Me Healthy Women. (Online) 2011. Available: http://health.mo.gov/living/healthcondiseases/chronic/showmehealthywomen/pdf/SMHWFactSheet.pdf (Accessed 11 April 2012).
5. Jonas S, Goldsteen R, Goldsteen K. An introduction to the U.S. health care system. New York: Springer Publishing, 2007.
6. Henry KA, Boscoe FP, Johnson CJ, Goldberg DW, Sherman R, Cockburn M. Breast cancer stage at diagnosis: is travel time important? Journal of Community Health 2011; 36: 933-942.
7. Henry KA, Sherman R, Roche LA. Colorectal cancer stage at diagnosis and socioeconomic characteristics in New Jersey. Health and Place 2009; 15: 505-513.
8. McLafferty S, Wang F. Rural reversal? Cancer 2009; 115: 2755-2764.
9. Merkin SS, Stevenson L, Powe N. Geographic socioeconomic status, race, and advanced stage breast cancer in New York City. American Journal of Public Health 2002; 92(1): 64-70.
10. Shalid R, Bertazzon S, Knudtson ML, Ghali WA. Comparison of distance measures in spatial analytical modeling for health service planning. BMC Health Services Research 2009; 9: 200.
11. Apparicio P, Abdelmajid M, Riva M, Shearmur R. Comparing alternative approaches to measuring the geographical accessibility of urban health services: distance types and aggregation-error issues. International Journal of Health Geographics 2008; 7: 7.
12. Wang F, McLafferty S, Escamilla V, Luo L. Late-stage breast cancer diagnosis and health care access in Illinois. Professional Geographer 2008; 60(1): 54-69.
13. Owen KK, Obregón EJ, Jacobsen KH. A geographic analysis of access to health services in rural Guatemala. International Health 2010; 2(2): 143-149.
14. Oppong JR, Hodgson MJ. Spatial accessibility to health care facilities in Suhum District, Ghana. Professional Geographer 2005; 46(2): 199-209.
15. Berk M, Feldman J, Schur C, Gupta J. Satisfaction with practice and decision to relocate. Bethesda: NORC Walsh Center for Rural Health Analysis, 2009.
16. US Department of Health and Senior Services. A manual for effective collaboration between critical access hospital and federally qualified health centers. (Online) 2010. Available: http://www.hrsa.gov/ruralhealth/pdf/qhcmanual042010.pdf (Accessed 13 April 2012).
17. Mackillop WJ, Zhang-Salomons J, Boyd CJ, Groome PA. Association between community income and cancer incidence in Canada and the United States. Cancer 2000; 89: 901-912.
18. Mackinnon J, Duncan R, Huang Y, Lee D, Fleming L, Voti L, et al. Detecting an association between socioeconomic status and late stage breast cancer using spatial analysis and area-based measures. Cancer Epidemiology, Biomarkers & Prevention 2007; 16 (4): 756-762.
19. Komen for the Cure. Racial facts for life: racial and ethnic differences. (Online) 2012. Available: http://ww5.komen.org/uploadedFiles/Content_Binaries/806-373a.pdf (Accessed 13 April 2012).
20. Campbell NC, Elliot AM, Sharp L, Ritchie LD, Cassidy J, Little J. Rural factors and survival from cancer: analysis of Scottish cancer registrations. British Journal of Cancer 2000; 82(11): 1863-1866.
21. Campbell RT, Li X, Dolecek TA, Barrett RE, Weaver KE, Warnecke RB. Economic, racial and ethnic disparities in breast cancer in the US: towards a more comprehensive mode. Health and Place 2009; 15: 870-879.
22. Campbell B, Staley D, Matas M. Who misses appointments? An empirical analysis. Cancer Journal of Psychiatry 1991; 36: 223-225.
23. Jordan H, Roderick P, Martin D, Barnett S. Distance, rurality and the need for care: access to health services in South West England. International Journal of Health Geographics 2004; 3: 21.
24. Cromley RG, Cromley EK. Chloropleth map legend design for visualizing community health disparities. International Journal of Health Geographics 2009; 8: 52.
25. Peters HD, Anu G, Gerry B, Damian GW, William RB, Hafizur R. Poverty and access to health care in developing countries, Annual N.Y. Academy of Sciences 2008; 1136: 161-171.
26. Warner ET, Gomez SL. Impact of neighborhood racial composition and metropolitan residential segregation on disparities in breast cancer stage at diagnosis and survival between black and white women in California. Journal of Community Health 2010; 35(4): 398-408.
27. Celaya MO, Berke EM, Onega TL, Gui J, Riddle BL, Cherala SS, et al. Breast cancer stage at diagnosis and geographic access to mammography screening (New Hampshire, 1998-2004). Rural and Remote Health 10: 1361. (Online) 2012. Available: www.rrh.org.au (Accessed 22 May 2012).



