Access to health care in Australia is recognised as a fundamental human right1, but limited health service access in non-metropolitan areas remains a significant issue2. Rural health services globally experience similar issues with transport, communication, infrastructure and health workforce shortages3. In Australia, a comparison of health indicators between geographic populations reveals higher mortality and poorer health outcomes in non-metropolitan areas4. Geographic disproportion in health service provision has chiefly contributed to these well established inequities in health outcomes for rural and remote populations5. Improved access to health care in regional areas can be a mechanism to ensure the populations of these communities are as healthy as other Australians6, and contribute to sustainable economic development and protection of the natural environment7.
Medical practitioners, oral health practitioners, mental health professionals and allied health professionals are substantially fewer per capita in rural and remote Australia compared to major cities8. Issues with recruitment and retention of health practitioners in rural and remote communities are significant contributors to health workforce mal-distribution9. Attracting and retaining allied health professionals in rural areas is also a recognised problem internationally10.
Promoting health professions to rural secondary students and undergraduate rural clinical placements have been suggested as strategies to address workforce shortages11,12. Students originating from rural and remote areas are more likely to return to work in these communities8, and rural clinical placements contribute to subsequent rural practice12. The phenomenon of student transition is a common factor and an important consideration for the success of both these strategies.
Previous research and government investment in rural health workforce development in Australia have largely focused on the medical profession13. An assumption of transferability to allied health is not consistent with research findings, with discipline-specific strategies considered more effective14. Preliminary investigation revealed a paucity of research quantifying the impact of strategies used to address low distribution of allied health professionals in rural areas. Resources directed at this issue may not be guided by best practice initiatives or evaluated to direct future investment. Recognising these factors, a comprehensive review was undertaken with the following objective:
To identify barriers and enablers from an Australian perspective for rural and remote students accessing allied health undergraduate tertiary education, and allied health undergraduate students participating in rural and remote clinical placements.
Terminology
Within the published literature there is no Australian or international standard definition of allied health15, nor consensus on which professions constitute the Australian allied health workforce16. For the purpose of this review, allied health practitioners are defined as tertiary qualified mainstream healthcare providers including audiology, dietetics, occupational therapy, optometry, orthoptics, orthotics and prosthetics, pharmacy, physiotherapy, podiatry, psychology, radiography, social work, speech pathology and Aboriginal and Torres Strait Islander health workers15,17. Allied health professions do not include medical doctors and nurses15,17.
The terms 'rural', 'remote', 'regional', 'country' and 'isolated' have different definitions and connotations across government departments, professional agencies and service providers. For the purpose of this review the terms 'rural' and 'remote' are used throughout. Furthermore, to achieve the review objective a consistent interpretation of 'rural' and 'remote' was required. Several classification systems are utilised in Australia; for the purpose of this review, the Australian Standard Geographical Classification (ASGC) Remoteness Structure was used18. 'Rural' and 'remote' included inner and outer regional Australia, and remote and very remote Australia18.
An initial keyword search of the Cochrane Library was completed in August 2012. One systematic review relevant to the objective of this study was identified, although from an international perspective. Grobler et al. (2009) found no studies that met their inclusion criteria of well-designed research minimising bias and confounding and evaluating interventions to increase the proportion of health professionals in rural areas19. With an absence of randomised controlled trials19, an integrative approach to this review was therefore considered appropriate to enable comparison of a range of methodologies20.
It was not the purpose of this study to conduct a systematic review and the findings should not be considered in this context. Rather, a broad review of existing literature is presented to account for professional diversity and to draw on a variety of data sources. A search of the empirical literature was conducted together with review of theoretical publications, including public health strategies and policy documents. Evidence quality grading was not attempted with conclusions subsequently intended as broad policy considerations and research directions.
Electronic database keyword searches of CINAHL, Medline, ERIC, PsychInfo and Scopus were performed in August 2012 using Boolean phrases: 'rural student' AND 'allied health' AND 'tertiary education' OR 'services' OR 'placement' OR 'fieldwork' OR 'support' OR 'transition, as well as 'Indigenous education' OR 'health career promotion'. Selection criteria included Australian research in English, full text available online, keywords in title or abstract, year of publication from 1990 to 2012, and with inclusion of rural contexts and allied health professions.
A single researcher reviewed titles and abstracts for articles with a primary focus relevant to the review objective. Publications not inclusive of allied health disciplines or rural and remote contexts were excluded. No specific restrictions were placed on research design. A total of 28 empirical publications met these selection criteria. Transcripts were assessed and themes categorised by application of a constant comparative analytic strategy. This was performed by an iterative review of transcripts, thematic analysis and accrual, and identifying recurring key words and summary concepts between transcripts. This material was organised into broad categorical themes with the progression assessed and confirmed by a second researcher.
For theoretical sources, and grey literature including informally published material available in the public sphere, Google searches were performed using a variety of search terms applicable to the review objective. Searches were restricted to the Australian context with a total of 22 grey literature publications included for review. An iterative process was applied with texts selected based on relevance to themes from the empirical literature.
For the purpose of interpretation and presentation of data, a process of thematic analysis was employed. This comprised organising and finalising themes by identification of patterns within selected texts using the process of constant comparison previously indicated. These themes were then described in detail, integrating citations from both empirical and grey literature. Subsequent analysis of themes by interpretation of relevance to the review objective generated opportunities for future policy, program and research initiatives. The report was subsequently condensed with findings presented in the following results and summarising conclusion.
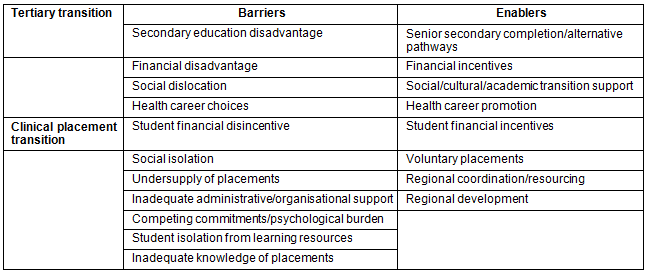
A summary of the empirical publications included for review is provided in Table 1. To align with the two-part study objective, themes arising from the reviewed empirical and theoretical sources were divided into two components. The first component categorises barriers and enablers for rural and remote students accessing allied health undergraduate tertiary education, termed tertiary transition. The second component categorises barriers and enablers for allied health undergraduates participating in rural and remote clinical placements, termed clinical placement transition. These themes are summarised in Table 2.
Interpretation of these results is presented in the following thematic analysis with direct relevance to rural and remote health policy, research and education in Australia.
Table 1: Summary of empirical publications
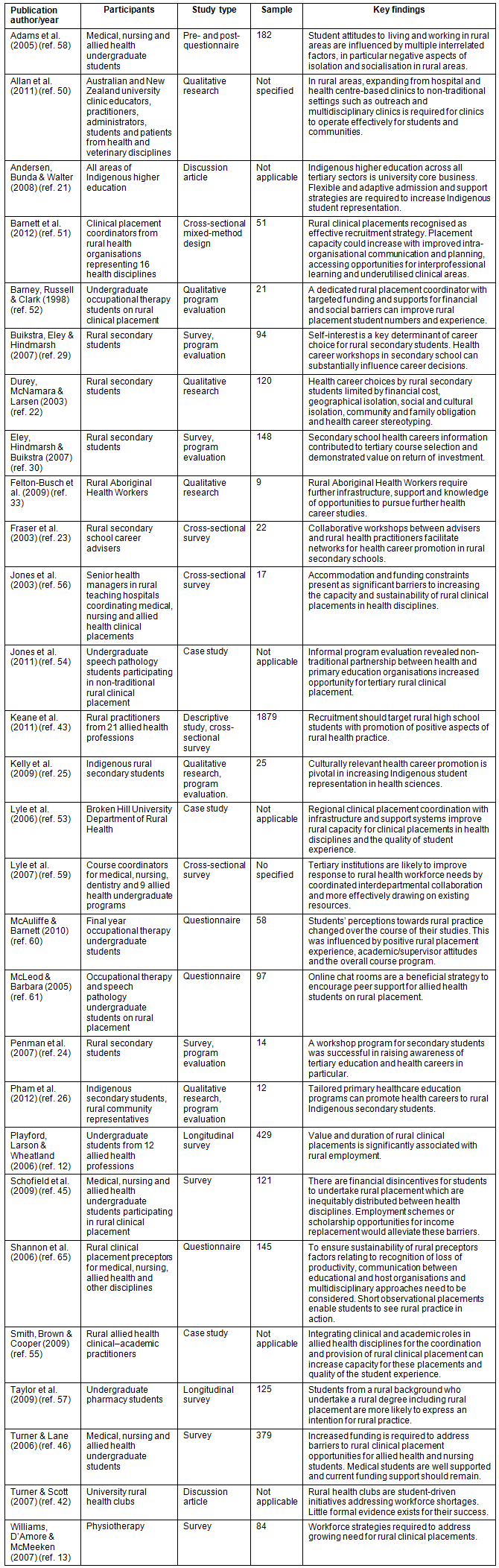 Table 2: Summary of review themes
Table 2: Summary of review themes
Tertiary transition
A review of the empirical literature on barriers for rural and remote students accessing allied health undergraduate degrees revealed themes relevant to all rural origin students commencing higher education. These include secondary education disadvantage, financial disadvantage and social dislocation. However, a fourth theme, a lack of consideration of health careers in the first instance, is specific to health disciplines.
Barrier - secondary education disadvantage: Secondary education disadvantage is a recognised barrier for rural and remote students accessing tertiary education21. The combination of rurality and low socioeconomic status generates the greatest educational disadvantage22. Research specific to allied health describes this disadvantage as originating from restricted subject choices, a comparative lack of peer pressure for academic performance, difficulty accessing senior secondary facilities23, inadequate career counselling with inappropriate subject selection23,24 and high tertiary entrance scores relative to perceived academic ability22,24. School completion and academic performance were also cited as barriers21,25,26.
The Bradley Review, a review of Australian higher education commissioned by the Australian Government, cites previous educational performance as a barrier to higher education for students from rural and remote, Aboriginal and Torres Strait Islander and low-socioeconomic backgrounds27. This report highlights the under-representation of rural and remote students in paramedical sciences specifically27. A report commissioned by the Department of Education, Employment and Workplace Relations elaborates on the mechanisms for this trend28. Gale et al. (2010) describe schooling standards as reproducing the structures of inequality, with students from low socioeconomic, rural and remote and Indigenous backgrounds differentially prepared by primary and secondary schooling for higher education28.
Barrier - financial disadvantage: The financial burden of university education was cited in the selected empirical publications as a barrier for rural and remote secondary students considering allied health careers21,22,24,29,30. This was framed as both the additional costs of relocation to urban centres for university29 and higher rates of low socioeconomic status in rural and remote populations contributing to reduced capacity for university education21,29.
The Senate Standing Committee on Rural and Regional Affairs and Transport described the financial cost of relocation as the greatest barrier for rural and remote students attending the tertiary course of their choice31. Similarly, the Bradley Review emphasises the additional financial assistance required to ensure these students successfully complete higher education, in comparison to their urban peers27. Furthermore, the National Rural Health Alliance Inc. (NRHA) cites the cost of relocation, accommodation and living expenses as primary barriers for rural and remote students attending undergraduate tertiary education, specifically for health disciplines32.
Barrier - social dislocation: The theme of social dislocation from the empirical literature included separation from family supports and social networks24,30,33, community loyalty and connection to place discouraging relocation for study purposes22, and Indigenous cultural isolation and alienation in the university environment and health curriculum21,26.
Gale et al. (2010) also detail the intricacies of social and cultural adaptations in the experience of relocation from rural and remote communities to urban centres for higher education purposes28. This process of transition is depicted as presenting the following broad challenges:
- developing skills for independent living
- negotiating unfamiliar transport systems and orientating to large educational institutions
- losing contact with family and longstanding community and peer relationships
- establishing new social networks28.
Barrier - lack of consideration of health careers: The empirical literature describes this phenomenon as the result of the unique characteristics of rural and Indigenous culture, including connection to place, obligation to community and perception of gender norms21-23,25,26,33, insufficient career guidance and promotion of the variety of health careers by educational institutions22-26,30, and insufficient student exposure to local role models from an undersupply of health practitioners in non-metropolitan areas21-23,25,30.
For tertiary education in general, the Bradley Review describes the aspirations of rural and remote students as not inclusive of higher education due to a lack of awareness of the long-term benefits27. Gale et al. (2010) identify origins of inhibitors to higher education aspirations for this student population as:
- limited exposure to information about university courses, and careers requiring a university qualification
- apprehension resulting from inadequate or misinformation on the university experience
- teacher expectations of academic potential expressed through career counselling advice28.
The Bradley Review describes the task of improving equity of representation in higher education of rural and remote students as difficult, with solutions not immediately obvious27 . However, this comprehensive review revealed the following practical enabling solutions; with a focus on allied health undergraduate qualifications.
Enabler - secondary completion and alternative pathways: Senior secondary completion with attainment of sufficient academic achievement for admission to allied health qualifications is an essential first step in improving representation of rural and remote students, and particularly Aboriginal and Torres Strait Islander students, in these courses21,26.
A practical solution to barriers to secondary school completion and academic outcomes for rural and remote students is recognition of this disadvantage by higher education institutions through admission policies and alternative pathways21. There are currently specific admission quota requirements for rural and remote origin students to qualifications in medicine34. Extending this across allied health would support greater representation of rural origin students in these courses35-37. The Bradley Review also describes a range of innovations for recognising disadvantage in tertiary admission processes, ultimately recommending further investigation by the Australian Government to determine equitable methodologies for university admissions27.
Enabler - financial incentives: Greater financial incentives are recommended in the empirical literature to increase representation of rural and remote origin students completing allied health undergraduate qualifications22,24. The Australian Government introduced legislation in 2011 in response to the Review of Student Income Support Reforms38. This increased the financial support for students from rural areas moving away for tertiary education. This was in addition to income support reforms for tertiary students passed by the Australian Parliament in 2010 in response to recommendations from the Bradley Review, with an emphasis on students from rural areas32,39.
The National Rural Health Alliance (NRHA) and Services for Australian Rural and Remote Allied Health (SARRAH) have welcomed these reforms, but continue to advocate for further enhancements to Commonwealth undergraduate scholarships in allied health disciplines32,37. The NRHA also suggested improved marketing of financial support opportunities for rural and remote students considering higher education in health disciplines35. Subsequently, an advertising campaign was released by the Australian Government in 2011 targeting regional students and their families with information on the Student Income Support Reforms40.
Enabler - transition support: The review of empirical literature also elicited a theme of university transition support to enable successful completion of allied health undergraduate qualifications for rural origin students21,22. This theme included remediating strategies for the social and cultural barriers already discussed. For Aboriginal and Torres Strait Islander students in particular, Andersen et al. (2008) describe the potential for universities to take a leadership role in improving tertiary participation and qualification completion rates of this student population21. They describe multi-level strategies to create supportive environments for Aboriginal and Torres Strait Islander students and academic staff, ultimately establishing Indigenous higher education as core university business21.
The theoretical literature also advocates for the role and potential benefits of rural health clubs in universities for supporting cultural and academic transition of rural origin students35,41. However, there is an apparent lack of research evaluating these programs, with little formal evidence for their success42. In fact, a counter-intuitive research outcome illustrates involvement with rural health clubs is not associated with rural employment13.
Enabler - health career promotion: A high proportion of publications from this review describe the potential and proven effectiveness of health career promotion for increasing rural and remote student participation in allied health qualifications22-26,29,30,43. The following are recommendations for characteristics of health career promotion strategies derived from these publications:
- accessible and relevant health career promotion programs inclusive of information on the range of health professions, with sensitivity to social and cultural context in rural Australia22,24,30
- exposure of students to health careers prior to senior secondary school to ensure appropriate subject selection24,29,30,43
- emphasis on cultural safety in health career promotion for Aboriginal and Torres Strait Islander students, emphasising health careers in the context of family and community loyalty and beliefs25,26
- utilising local health practitioners and allied health students as role models for health career promotion, and as ongoing mentors for rural and remote secondary students considering health professions22,23
- improving networking between rural high school career advisors and health professionals, and better resourcing career advisors by schools and higher education institutions for accurate information on allied health undergraduate admissions23.
This theme is recognised broadly in the theoretical literature. The Bradley Review describes awareness of higher education and an aspiration to participate as core components of increasing tertiary representation of disadvantaged student populations27. Specifically relevant to allied health, the NRHA call for greater representation of health professions as viable career options to rural and remote secondary students35,37. The additional potential of media campaigns to drive greater interest in health professions in rural communities is also discussed44.
The NRHA and SARRAH also call for extension of the role of university departments of rural health by provision of allied health programs32,37. This would not only improve visibility of allied health qualifications in rural communities, but also reduce barriers associated with distance from community of origin.
Clinical placement transition
A review of empirical literature on barriers to transition for allied health students accessing rural and remote clinical placements revealed themes consistent with tertiary transition. These include financial disincentive, social isolation and inadequate knowledge of available opportunities. Further barriers included an undersupply of rural placements in allied health, inadequate placement administrative and organisational support, competing family commitments and psychological burden for students, and student isolation from peer and professional support and learning resources. These barriers highlight issues of access to placements, as well as describing potential for positive experiences contributing to future rural practice intention.
Barrier - student financial disincentive: Financial issues are cited in empirical publications as particularly concerning for students considering rural placements. These issues include potential loss of employment earnings, accommodation costs and transportation requirements13,45,46. Schofield et al. (2009) extrapolate this to highlight the risks of a system exposing students to a reduction in earnings, as financial problems frequently contribute to university withdrawal45. Although lost earnings of clinical placement supervisors have been investigated, there is little information on the magnitude of lost earnings for participating students45.
Turner and Lane (2006) indicate allied health students receive substantially less travel reimbursement and paid accommodation on rural placement compared to medical students46. The financial burden for students undertaking rural clinical placements in allied health is recognised by SARRAH, which currently brokers the Australian Government Department of Health and Aging scholarships for rural clinical placements47. Both SARRAH and NRHA advocate for greater investment in this scholarship program to match the incentives provided to medical students48.
Barrier - social isolation: Selected empirical publications cite social isolation as contributing to rural clinical placement refusal or placement dissatisfaction13,45,46. Issues of social isolation on rural clinical placement are described in unpublished literature as pertaining to separation from family and friends, and adjustment to rural cultural characteristics49.
Barrier - undersupply of rural clinical placements: An undersupply of rural clinical placements is described in the empirical literature as a fundamental barrier to allied health students participating in these attachments13,46,50-54. This is a critical finding as rural allied health clinical placements are an identified means of increasing recruitment to rural areas13,45,46,52,53,55-61.
Suggested mechanisms for this shortfall include:
- limited capacity of rural allied health practitioners to supervise students on placement50,51,53,54
- inadequate funding and poor coordination between sponsoring universities and health organisations46,53
- under-utilisation of non-traditional placement opportunities and inter-sectoral collaboration54,55.
Health Workforce Australia (HWA) describes insufficient infrastructure and human resources as contributing to shortages of clinical placements across all disciplines and geographic locations62. In the rural context, this issue continues despite clear recognition for some years of the undersupply of rural clinical placements in allied health by the NRHA63 and SARRAH64.
Barrier - inadequate administrative and organisational support: Challenges with administrative and organisational support for rural clinical placements in allied health are represented in the empirical literature as arising from both the health and higher education sectors46,51,53,56,59. The dual consequence of insufficient placement opportunities and unsatisfactory placement experiences is described51,56. Causal factors suggested include inadequate or unsustainable funding for health and higher education organisations52,53,56,59, and inadequate communication and feedback mechanisms between institutions providing rural placements38,43,51,53,59,65.
Insufficient inter-sectoral collaboration and administrative support are cited by HWA as impacting on growth of clinical placements nationally, irrespective of location62. As rural placements are often in competition with urban settings for allied health students49,64, non-metropolitan communities are at a distinct disadvantage. There appears to be debate between higher education institutions and public sector health organisations as to funding and human resource responsibilities for coordination of allied health clinical placements63,64. In the unpublished literature there is also evidence of contention regarding disparity between support for medical student training in rural clinical schools, and the comparatively lesser funding incentives for allied health rural clinical placements36,63,64.
Barrier - competing commitments and psychological burden: Turner and Lane (2006) describe difficulties organising care for dependents and psychological burden for students associated with preparing for clinical placement, as reasons for allied health students refusing a rural attachment46. The National Rural Health Student Network (NRHSN) describes the inequitable expectation for many allied health students to organise their own rural clinical placements, in comparison to the coordinated preparation for other disciplines36. This is recognised through the call for greater emphasis and funding support for rural allied health placement coordinators63,64.
Barrier - student isolation from learning resources: Barney, Russell and Clark (1998) and McLeod and Barbara (2005) describe isolation from peer and professional support and resources as detracting from the learning outcomes and satisfaction experienced by allied health students on rural clinical placement52,61. Similarly, inadequate access to information technology, teaching resources and simulation devices has been identified by SARRAH as an issue for rural placement supervisors supporting the learning objectives of allied health students64.
Barrier - inadequate knowledge of rural clinical placements: A lack of information on the availability of rural clinical placements was cited by Barney, Russell and Clarke (1998) and Turner and Lane (2006) as a barrier to uptake of these attachments for allied health students46,52. This is an important insight relevant to the task of ensuring exposure of metropolitan-based allied health students to rural practice, as a means of achieving positive attitudes to employment in rural and remote communities.
Health Workforce Australia emphasises the importance of removing barriers to growth and uptake of clinical placements for those professions required to meet the health needs of the Australian population62. A shortage of allied health professionals in rural and remote Australia necessitates examination of current and potential enablers for the uptake of rural clinical placements in allied health, given the positive correlation between these experiences and future rural practice. The research publications considered in this study describe the following recommended and proven solutions.
Enabler - student financial incentives: Barney, Russell and Clark (1998) describe strategies to overcome financial barriers to allied health rural placements to improve uptake and perceived quality of placements offered52. These include free accommodation and reimbursement of travel costs52. Schofield et al. (2009) specifically address issues related to loss of student income45. They recommend casual employment registers, employment transfer programs, or scholarship for income replacement as potential incentives to address wage loss for allied health students on rural clinical placement45.
In the theoretical literature SARRAH, the NRHA and the NRHSN have called for increased government commitment to existing scholarship programs for allied health students participating in rural clinical placements36,63,64. Increased scholarship support is proposed as a method of alleviating the impact of travel, accommodation and social isolation issues contributing to reduced uptake or poor experiences of rural clinical placements in allied health64.
Enabler - voluntary placements: Despite ambiguity surrounding some characteristics of rural placements, Playford, Larson and Wheatland (2006) found a strong association between voluntary clinical placements and future rural practice for both nursing and allied health students12. However, there appears to be contradictory findings as to the ideal characteristics of rural placements to advance future rural practice12. Further research is suggested to adequately understand what constitutes positive placement experiences with sufficient confidence to make policy recommendations12,60.
Enabler - regional coordination and resourcing: Regional coordination and investment in infrastructure and support systems is described in the empirical literature as improving both the quality of rural clinical placements and regional capacity for allied health students52,53. Lyle et al. (2006) present a case study of regional clinical placement coordination across all health disciplines53. They detail improved student placement numbers and increased breadth of clinical experience as a result of centralised coordination, streamlined administration and commitment to inter-sectoral collaboration53.
On a broader scale, Barnett et al. (2012) recognise the competition for rural clinical placements across the health disciplines as compromising the quality of student learning and contributing to clinical supervisor burnout51. To minimise these negative outcomes, Barnett et al. (2012) advocate for greater collaboration between universities, faculty and health organisations in relation to student placement data, interdisciplinary learning and placement opportunities51. The authors call for not only regional planning as described by Lyle et al. (2006), but also statewide and national planning efforts to maximise the quality and capacity of rural clinical placements in health53.
The potential for jointly funded teaching positions and inter-professional learning in rural settings to improve rural placement experiences and availability is investigated by Smith, Brown and Cooper (2009)55. The authors present a model for multidisciplinary allied health clinical-academic practice55. Their case study illustrates the potential for these initiatives to achieve better rural health outcomes by:
- improved collaboration between higher education institutions and local health services
- responsiveness of clinical placements to community needs
- improved rural placement experiences for students
- identifiable career progression for rural health practitioners
- increased research capacity in rural areas, and increased capacity for rural clinical placements55.
Further opportunities for increasing availability of rural placements in allied health utilising inter-sectoral collaboration include university outreach clinics50 and community-led non-traditional partnerships54. Appropriate accommodation options and availability of information technology and telecommunications are also conducive to allied health student uptake of rural clinical placements and subsequent positive experiences52,55,56,59,61.
Embedded in the depiction of these programs is adequate, sustained and appropriately utilised funding. Congruent with research publications, the theoretical literature advocates for increased funding for provision of rural placements in allied health, and greater shared financial investment for inter-sectoral coordination63,64. Increasing the number of joint clinical-academic allied health preceptors in rural areas is also recognised in the unpublished literature as improving the quality of support for allied health students on rural placement63.
In recognition of the issues with clinical placement coordination in all geographic locations, HWA introduced Integrated Regional Clinical Training Networks66. These networks were established with the intention of increasing the availability and quality of clinical placements in the health professions67.
Enabler - regional development: Jones et al. (2003) present regional development and promotion of viable communities as fundamental to ensuring rural placements in health disciplines are both available and meaningful56. In essence, the retention of services in rural hospitals is required to provide teaching environments for student placements56. Beyond the domain of health, the imperative for regional development is recognised at a national level with broader social considerations. For instance, Regional Development Australia is an initiative recognising the importance of strengthening regional communities to ensure their economic, social and environmental sustainability in the future68.
This review is intended to assist policy and program development for growth of the rural allied health workforce in Australia, as well as identify knowledge deficits to guide future research endeavours. Although applicability of findings to an international context may be limited, recommendations from this study may engender consideration of allied health student transition support strategies for rural and remote areas globally.
Based on the findings of this review, policy directions for consideration at the national level incorporating Australian Government initiatives to support the recruitment of allied health practitioners to rural and remote areas in Australia should include:
- pursuit of a standardised national allied health definition and classification of rurality to achieve clarity and equity for professional and student support, and to strengthen workforce data collection methods
- continued emphasis on regional development in support of viable communities and health services in rural and remote areas
- policy support for inter-sectoral collaboration through identification of common goals and non-competitive resource allocation for mutually beneficial outcomes in the health and higher education sectors. Specific strategies may include funding opportunities for tertiary education and health organisation collaboratives for rural placement coordinators and clinical/academic supervisors for improved capacity, sustainability and quality of placement experiences
- ongoing development and evaluation of specific programs in support of secondary education quality and completion in rural and remote areas
- investigation of equitable tertiary admission processes or alternative pathways for university entrants addressing under-representation of rural origin students, and specifically for allied health disciplines
- evidence-based and contemporary transition support programs for rural and remote allied health undergraduates, particularly for Aboriginal and Torres Strait Islander students
- recognition of the role of allied health in contributing to the well-being of rural and remote populations, achieved through parity with medical and nursing financial incentives for rural origin students, and resourcing of rural clinical training.
Relevant to higher education and health sectors at a state jurisdictional level, this comprehensive review has revealed program and research recommendations. These include:
- health career promotion initiatives based on local identified needs
- regional coordination of rural clinical placements in allied health
- further investigation of social and cultural motivations for health career choices by rural origin students
- development of a valid and reliable measure of the impact of rural clinical placements in allied health
- investigation of the attributes of rural clinical placements creating positive experiences for participating allied health students.
Beyond recognition of social and cultural implications, there appears to be comparatively little formal investigation within empirical or theoretical literature for transition interpretations and experiences of students themselves. Initiatives addressing transition issues for rural and remote origin allied health students or undergraduates on rural clinical placement may not be adequately influenced by the opinions and perspectives of the target population. To achieve meaningful change in representation of allied health practitioners in rural and remote Australia, and ultimately more equitable health outcomes for regional communities, future research should privilege the perspective of these students.
Acknowledgements
This work was supported by the University of Tasmania, Centre for Rural Health.
References
1. Humphreys JS. Key considerations in delivering appropriate and accessible health care for rural and remote populations: discussant overview. Australian Journal of Rural Health 2009; 17(1): 34-38.
2. World Health Organization. Increasing access to health workers in rural and remote areas through improved retention: global policy recommendations. Geneva, Switzerland: World Health Organization, 2010.
3. Australian Institute of Health and Welfare. Rural health: demography. 2012. Canberra, ACT: Australian Institute of Health and Welfare, 2012.
4. Strasser R, Neusy A-J. Context counts: training health workers in and for rural and remote areas. Bulletin of the World Health Organization 2010; 88(10): 777-782.
5. Dunbar J, Reddy P. Integration and coordination of care. Australian Journal of Rural Health 2009; 17(1): 27-33.
6. Standing Council on Health. National strategic framework for rural and remote health. Canberra, ACT: Commonwealth of Australia, 2012.
7. Australian Institute of Health and Welfare. Rural, regional and remote health: indicators of health status and determinants of health. Canberra, ACT: Australian Institute of Health and Welfare, 2008.
8. Department of Health and Ageing. Report on the audit of health workforce in rural and regional Australia. Canberra, ACT: Department of Health and Ageing, 2008.
9. Allan J, Ball P, Alston M. 'You have to face your mistakes in the street': the contextual keys that shape health service access and health workers' experiences in rural areas. Rural and Remote Health 8(1): 835.(Online) 2008. Available: www.rrh.org.au (Accessed 13 March 2014).
10. Schoo A, Stagnitti K, Dunbar J. A conceptual model for recruitment and retention: allied health workforce enhancement in Western Victoria, Australia. Rural and Remote Health 5(4): 477. (Online) 2005. Available: www.rrh.org.au (Accessed 13 March 2014).
11. Alexander C, Fraser J. The promotion of health careers to high school students in the New England Health Area: the views of high school careers advisers. Australian Journal of Rural Health 2001; 9(4): 145-149.
12. Playford D, Larson A, Wheatland B. Going country: rural student placement factors associated with future rural employment in nursing and allied health. Australian Journal of Rural Health 2006; 14(1): 14-19.
13. Williams E, D'Amore W, McMeeken J. Physiotherapy in rural and regional practice. Australian Journal of Rural Health 2007; 1S: 380-386.
14. Baldwin A, Agho A. Student recruitment in allied health educational programs: the importance of initial source of contact. Journal of Allied Health 2003; 32(2):65-70.
15. Turnbull C, Grimmer-Somers K, Kumar S, May E, Law D, Ashworth E. Allied, scientific and complementary health professionals: a new model for Australian allied health. Australian Health Review 2009; 33(1): 27-37.
16. Australian Health Workforce Advisory Committee. The Australian allied health workforce: an overview of workforce planning issues. Sydney, NSW: Australian Health Workforce Advisory Committee, 2006.
17. Lowe S, Adams R, O'Kane A. A framework for the categorization of the Australian health professional workforce. Canberra, ACT: Services for Australian Rural and Remote Allied Health, 2007.
18. Australian Bureau of Statistics. Statistical geography: remoteness structure. (Online). 2011. Available: http://www.abs.gov.au/websitedbs/D3310114.nsf/home/remoteness+structure (Accessed 6 December 2012).
19. Grobler L, Marais BJ, Mabunda SA, Marindi PN, Reuter H, Volmink J. Interventions for increasing the proportion of health professionals practising in rural and other underserved areas. Cochrane Database of Systematic Reviews 2009; 2.
20. Whittemore R, Knafl K. The integrative review: updated methodology. Journal of Advanced Nursing 2005; 52(5): 546-553.
21. Andersen C, Bunda T, Walter M. Indigenous higher education: the role of universities in releasing the potential. Australian Journal of Indigenous Education 2008; 37(2008): 1-8.
22. Durey A, McNamara B, Larson A. Towards a health career for rural and remote students: cultural and structural barriers influencing choices. Australian Journal of Rural Health 2003; 11(3): 145-150.
23. Fraser J, Alexander C, Simpkins B, Temperley J. Health career promotion in the New England area of New South Wales: a program to support high school career advisers. Australian Journal of Rural Health 2003; 11(4): 199-204.
24. Penman J, Ellis B, White F, Misan G. Evaluating the effectiveness of a university health sciences experience program for regional Year 10 students. Australian Journal of Rural Health 2007; 15(6): 352-359.
25. Kelly H, Robinson A, Drysdale M, Chesters J, Faulkner S, Ellender I, et al. 'It's not about me, it's about the community': culturally relevant health career promotion for Indigenous students in Australia. Australian Journal of Indigenous Education 2009; 38(2009): 19-26.
26. Pham X, Page P, Sivamalai S, Woolley T. The benefits of a tailor-made pilot primary health-care course for Indigenous high school students in remote Queensland. Australian Journal of Rural Health 2012; 20(3): 113-118.
27. Bradley D, Noonan P, Nugent H, Scales B. Review of Australian higher education: final report [Bradley Review]. Canberra, ACT: Department of Education, Employment and Workplace Relations, 2008.
28. Gale T, Tranter D, Bills D, Hattam R, Comber B. Interventions early in school as a means to improve higher education outcomes for disadvantaged (particularly low SES) students. Component A: A review of the Australian and international literature. Underdale, SA: National Centre Student Equity in Higher Education, 2010.
29. Buikstra E, Eley RM, Hindmarsh N. Informing rural and remote students about careers in health: factors influencing career decisions. Australian Journal of Rural Health 2007; 15(5): 289-295.
30. Eley RM, Hindmarsh N, Buikstra E. Informing rural and remote students about careers in health: the effect of Health Careers Workshops on course selection. Australian Journal of Rural Health 2007; 15(1): 59-64.
31. Rural and Regional Affairs and Transport References Committee. Rural and regional access to secondary and tertiary education opportunities. Canberra, ACT: Australian Senate, 2009.
32. National Rural Health Alliance Inc. Fact sheet 6: Further education and health. Canberra, ACT: National Rural Health Alliance, 2010.
33. Felton-Busch CM, Solomon SD, McBain KE, De La Rue S. Barriers to advanced education for indigenous Australian health workers: an exploratory study. Education for Health 2009; 22(2): 187.
34. National Rural Health Student Network. Ensuring a sustainable future health workforce for rural and remote Australia. Victoria: National Rural Health Student Network, 2010.
35. National Rural Health Alliance Inc. Twenty steps to equal health by 2020: The NRHA's 20-point plan for improving health services and health workforce in rural and remote areas. Canberra, ACT: National Rural Health Student Network, 2012.
36. National Rural Health Student Network. National priorities paper: Summary paper 2011-2012. Victoria: National Rural Health Student Network, 2012.
37. Services for Australian Rural and Remote Allied Health. Submission to Health Workforce Australia: rural and remote health workforce innovation and reform strategy. Canberra, ACT: Services for Australian Rural and Remote Allied Health, 2011.
38. Dow K. Review of student income support reforms. Canberra, ACT: Department of Industry, Innovation, Science, Research and Tertiary Education, 2011.
39. Department of Industry, Innovation, Science, Research and Tertiary Education. Student Income Support Reforms. Canberra, ACT: Department of Industry, Innovation, Science, Research and Tertiary Education, 2012.
40. Department of Industry, Innovation, Science, Research and Tertiary Education. Regional Student Income Support Campaign Materials. Canberra, ACT: Department of Industry, Innovation, Science, Research and Tertiary Education, 2012.
41. Services for Australian Rural and Remote Allied Health. Student rural health clubs and professional support. Canberra, ACT: Services for Australian Rural and Remote Allied Health, 2012.
42. Turner JV, Scott LM. University rural health clubs: nurturing the future Australian rural workforce. Rural and Remote Health 7(3): 649. (Online) 2007. Available: www.rrh.org.au (Accessed 13 March 2014).
43. Keane S, Smith T, Lincoln M, Fisher K. Survey of the rural allied health workforce in New South Wales to inform recruitment and retention. Australian Journal of Rural Health 2011; 19(1): 38-44.
44. McKinstry C, Kenny A. Promoting health careers to rural students. Presented at 11th National Rural Health Conference, Perth, Western Australia. Canberra, ACT: National Rural Health Alliance, 2011.
45. Schofield D, Keane S, Fletcher S, Shrestha R, Percival R. Loss of income and levels of scholarship support for students on rural clinical placements: a survey of medical, nursing and allied health students. Australian Journal of Rural Health 2009; 17(3): 134-140.
46. Turner JV, Lane J. Early barriers for university rural clinical placements. Education for Health 2006; 19(3): 375-379.
47. Services for Australian Rural and Remote Allied Health. Clinical placement. Canberra, ACT: Services for Australian Rural and Remote Allied Health, 2012.
48. National Rural Health Alliance. Submission to Health Workforce Australia to provide comment on the National Health Workforce Innovation and Reform Strategic Framework for Action (Framework). Canberra, ACT: National Rural Health Alliance, 2011.
49. Humphreys N, White S. Undergraduate physiotherapy students' expectations and preconceptions of rural clinical placements. Presented at NSW Rural and Remote Health Conference, Albury, NSW, 2010.
50. Allan J, O'Meara P, Pope R, Higgs J, Kent J. The role of context in establishing university clinics. Health & Social Care in the Community 2011; 19(2): 217-224.
51. Barnett T, Walker LE, Jacob E, Missen K, Cross MD, Shahwan-Akl L. Expanding the clinical placement capacity of rural hospitals in Australia: displacing Peta to place Paul? Nurse Education Today 2012; 32(5): 485-489.
52. Barney T, Russell M, Clark M. Evaluation of the provision of fieldwork training through a rural student unit. Australian Journal of Rural Health 1998; 6(4): 202-207.
53. Lyle D, Morris J, Garne D, Jones D, Pitt M, Walker T, et al. Value adding through regional coordination of rural placements for all health disciplines: the Broken Hill experience. Australian Journal of Rural Health 2006; 14(6): 244-248.
54. Jones D, Grant-Thomson D, Bourne E, Clark P, Beck H, Lyle D. Model for rural and remote speech pathology student placements: using non-traditional sites and partnerships. Australian Journal of Rural Health 2011; 19(1): 52-53.
55. Smith T, Brown L, Cooper R. A multidisciplinary model of rural allied health clinical-academic practice: a case study. Journal of Allied Health 2009; 38(4): 236-241.
56. Jones GI, Alford KA, Russell UJ, Simmons D. Removing the roadblocks to medical and health student training in rural hospitals in Victoria. Australian Journal of Rural Health 2003; 11(5): 218-223.
57. Taylor SJ, Maharaj P, Williams K, Sheldrake C. Pharmacy students' intention to practise in a rural setting: measuring the impact of a rural curriculum, rural campus and rural placement on a predominantly metropolitan student cohort. Australian Journal of Rural Health 2009; 17(6): 305-309.
58. Adams ME, Dollard J, Hollins J, Petkov J. Development of a questionnaire measuring student attitudes to working and living in rural areas. Rural and Remote Health 5(1): 327. (Online) 2005. Available: www.rrh.org.au (Accessed 13 March 2014).
59. Lyle D, Klineberg I, Taylor S, Jolly N, Fuller J, Canalese J. Harnessing a university to address rural health workforce shortages in Australia. Australian Journal of Rural Health 2007; 15(4): 227-233.
60. McAuliffe T, Barnett F. Perceptions towards rural and remote practice: a study of final year occupational therapy students studying in a regional university in Australia. Australian Occupational Therapy Journal 2010; 57(5): 293-300.
61. McLeod S, Barbara A. Online technology in rural health: supporting students to overcome the tyranny of distance. Australian Journal of Rural Health 2005; 13(5): 276-281.
62. Health Workforce Australia. Mapping clinical placements: capturing opportunities for growth. Adelaide, SA: Health Workforce Australia, 2011.
63. National Rural Health Alliance. Under pressure and under-valued: allied health professionals in rural and remote areas. Canberra, ACT: National Rural Health Alliance, 2004.
64. Lowe S. SARRAH issues paper: clinical education for allied health students and rural clinical placements. Canberra, ACT: Services for Australian Rural and Remote Allied Health, 2007.
65. Shannon SJ, Walker-Jeffreys M, Newbury JW, Cayetano T, Brown K, Petkov J. Rural clinician opinion on being a preceptor. Rural and Remote Health 6(1): 490. (Online) 2006. Available: www.rrh.org.au (Accessed 13 March 2014).
66. Health Workforce Australia. National Clinical Supervision Support Framework. Adelaide, SA: Health Workforce Australia, 2011.
67. Health Workforce Australia. Integrated regional clinical training networks. Adelaide, SA: Health Workforce Australia, 2012.
68. Department of Regional Affairs, Local Government, Arts and Sport. Regional Development Australia. Canberra, ACT: Department of Regional Australia, Local Government, Arts and Sport, 2011.

