The health of people living in rural areas is worse across all indicators, as reflected in higher morbidity and mortality rates and lower life expectancy1. In Australia, various factors contribute to this greater burden of disease including the demographic profile of the rural population, particularly the higher proportion of Aboriginal and Torres Strait Islander (hereafter Aboriginal) Australians with poorer health status and more social and environmental disadvantage2. Lifestyle and behavioural risk factors, environmental risks related to, for example, occupation and road accidents resulting in injury or death, geographic isolation and reduced access to services also contribute to health disparities between rural and urban populations3. Despite reforms, health services generally remain focused on specialised acute care in metropolitan centres. More upstream approaches are also required including prevention, high quality primary care, population health initiatives and offering more services to disadvantaged populations including Aboriginal Australians in rural and remote areas4,5.
Attracting health professionals to work in rural locations in Australia and elsewhere has long been a challenge that is well documented. The problem is not one of supply but of distribution, which has generated a plethora of research on how to mitigate the mal-distribution of the health workforce to improve services to these populations4. Our definition of 'rural' follows that reported in journal articles and mainly refers to towns and settlements outside metropolitan areas including regional centres. Workforce retention refers to the minimum length of stay between commencement and termination of employment whereas turnover is the proportion of employees whose service terminates within a given period6,7.
With substantial government investment to attract doctors to rural areas in Australia, including pre-vocational and vocational medical training, calls are increasing from the nursing and allied health sectors for more equity and better investment in their training on the grounds of need to meet shortages in the rural workforce4. Nurses are the largest group, comprising about 60% of the current health workforce, have the lowest turnover and greatest stability in rural practice with a relatively high median length of service in their current position4,6. With the exception of Aboriginal health practitioners, registered allied health practitioners (AHPs) make up a smaller percentage of the rural health workforce with the lowest proportion per 100 000 population working in remote/very remote areas, usually the areas of greatest need4,8. Across Australia, rural communities are experiencing shortages of AHPs, with ongoing recruitment difficulties and high staff turnover9. While 150.5 registered psychologists per 100 000 population work in major cities, only 47.8 per 100 000 population work in remote areas; 62.9 occupational therapists (OTs) per 100,000 population work in cities, which drops to 23.1 per 100 000 population in remote areas8. AHPs are also twice as likely as doctors or nurses to leave rural practice10.
AHPs play an important role in both upstream (health promotion and disease prevention) and downstream (treatment of disease) approaches to rural health care. Profiles of AHPs across disciplines in 2011-2012 identified more women than men with the average employment age between 37 and 47 years. The highest percentage of full-time equivalent (FTE) practitioners were employed in the major cities with the exception of Aboriginal health practitioners8. AHPs must meet the standards and eligibility criteria set out by the national boards for each profession to register and practise in Australia8. While an AHP is a 'trained professional who works in the healthcare team to support a person's medical care', consensus is lacking on who constitutes the allied health workforce8,11. Table 1 outlines the overlapping but inconsistent list of professions included by the Allied Health Professions Australia and the National Registration and Accreditation Scheme introduced in 20108,12.
During a broader literature review conducted by the authors on the rural health workforce, a rural pipeline was identified as a promising model for recruiting and retaining rural practitioners13. The idea of the rural pipeline emerged in the medical literature as a career pathway for medical doctors, conceptualised as a career continuum starting at school and ending in a committed, appropriately trained and supported rural doctor14,15. It involves a multifaceted, integrated sequence of tailored interventions made over time to support a particular individual to develop as a motivated and well-trained rural health practitioner16.
In this article we will consider how the concept of a rural pipeline can be used to enhance recruitment and retention of AHPs in Australia. We take into account the multifaceted nature of the issue, acknowledging the diverse professional and social needs within and between AHPs and their different career pathways. With this in mind, we adapt the rural pipeline to focus on AHPs who enter at any stage of their career to work in rural areas. We draw on the literature to identify barriers to AHP recruitment and retention and identify strategies to encourage and support AHPs from educational, financial, organisational, professional and social perspectives with a view to improving recruitment and retention at different stages along the pipeline.
Table 1: Allied health professions in Australia
Rural pipeline
The conventional rural pipeline starts at school where students are exposed to information about health careers to foster aspirations to apply for entry to health professional training after finishing school. It mainly applies to 'locally' trained (home-grown) health professionals who are targeted from secondary school4. In the undergraduate stage, the aspiring health professional is exposed to a curriculum and rural placements that encourage intention to practise rurally15. The adapted pipeline for AHPs recognises that graduates who choose rural practice need to be retained in the system. Once fully registered, health professionals are 'career professionals' who can then be recruited into the rural health professional workforce and hopefully retained13.
Adapting and extending the pipeline in this way harnesses the potential offered by AHPs who enter at different stages of their career and through different pathways including FIFO (fly-in, fly-out) workers. FIFO work is described as work in isolated environments far from home, making daily commuting impractical or virtually impossible. This type of work is particularly prevalent in mining and resource industries in Australia to deliver various services, including health, to remote communities17. Other pathways include overseas trained AHPs entering rural practice; locums; AHPs re-entering the rural workforce after years away; those who contribute to rural and remote health care through, for example telehealth; AHPs who, as they get older, move to rural areas (sea/tree change); and assistants who support health AHPs clinically (Fig1).
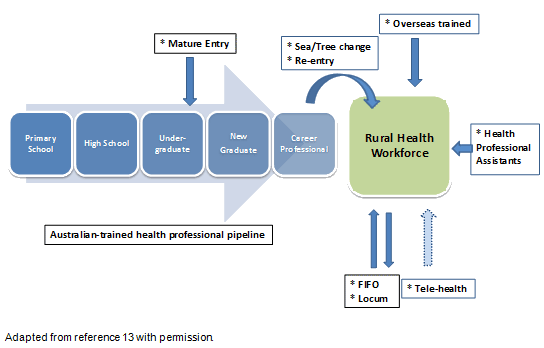
Figure 1: The extended rural pipeline.
The pipeline approach to increasing the rural health workforce extends the concept of short-term recruitment (placement/employment) to include long-term strategies to nurture potential professionals (Fig2). Once employed in rural locations, retention strategies are needed to increase longevity in the rural area and reduce staff turnover6. Humphreys et al's conceptual framework informed this approach identifying educational, financial/economic, professional/organisational, social (family and personal) and external factors (location and community) that impact on recruitment and retention of AHPs6. Flexible and integrated strategies for AHPs can then be developed to address specific factors including taking into account the broad social context.
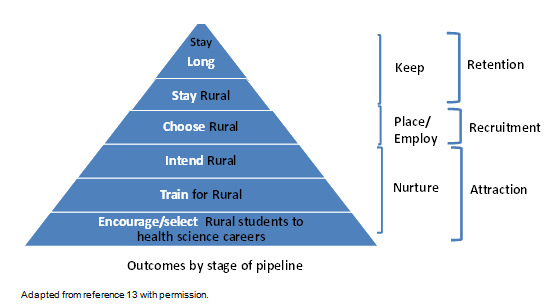
Figure 2: Relationship of the extended 'pipeline' to the recruitment and retention of rural allied health practitioners.
Factors impacting on allied health practitioner recruitment and retention at various stages along the extended rural pipeline
Educational factors: Little evidence from 2008 onwards was found of tertiary allied health schools selecting students at rural secondary schools to enrol in their courses despite suggestions that recruitment strategies should target this cohort18. Resources are available to target potential medical students from school through structured contact between rural high schools and the medical profession to inspire students to make rural career choices. These choices were then supported through medical school and into rural general practice15.
Strategies to attract students interested in allied health and feed into this point on the rural pipeline include engaging rural career advisors. As key stakeholders they can raise rural secondary students' awareness of health professions as a career choice worth considering19. In one example, 90% of rural students participating in a health career workshop claimed it influenced their career selection20. Other recruitment strategies include delivering information at school about health careers interactively (rather than passively via brochures or flyers), targeting rural high school students in promoting rural health careers and highlighting the positive aspects of rural practice such as diversity and autonomy18,21. These approaches also provide opportunities to establish partnerships between schools and the higher education sector and, in the current climate of digital technology, can make use of social media as a promotion strategy to attract this cohort to rural practice.
Rural content in curriculum Once at university, adequate exposure to rural content in undergraduate curricula can influence allied health students' career choices and be a potential entry point into the rural pipeline for rural and urban students14. However, many allied health courses are located at city universities despite evidence that courses based at regional universities are effective in attracting rural allied health students to rural practice. A national study identified that rural pharmacy students were more likely to enter rural practice if they had attended regional or rural pharmacy schools22 and social work courses at regional universities attracted and retained local social workers to practise in that region23.
Rural placements Supervised clinical placements in rural areas are a component of undergraduate education that offer allied health students hands-on experience to learn about rural issues and practice24. However, effective preparation of students and the quality of these placements was identified as more important than rural placements per se23,25.This includes offering practical skills in coursework on rural practice, adequate training in interprofessional care, mentoring, more education on management and organisational skills during training, and working with an inspiring and effective academic educator and fieldwork supervisor26-28. As a potential point of entry on the pipeline, students with positive experiences of rural placement were more likely to want to practise rurally24,29. For example, OT undergraduate students who were exposed to a rural location and a good rural fieldwork experience increased their positive perceptions of rural and remote practice from 60% to 79% over the course of the program26,30. Pharmacists were more likely to practise rurally if they had undertaken a rural internship and were four times more likely to have undertaken one if they had lived in a rural area as child and attended a rural university31. One innovative marketing strategy used a DVD developed from interviews with rural and remote health professionals to promote rural practice to pharmacy students. Findings from fourth year students showed over 50% had considered rural practice before seeing the DVD and 37% indicated that the DVD had increased their awareness of rural pharmacy practice32.
Financial/economic factors: For AHPs in the workforce, financial incentives are already a recruitment strategy along the pipeline. However, such strategies were not always successful in increasing the number of health professionals working in underserved areas with suggestions that other incentives such as good working conditions and affordable housing may be more effective6,33,34. A study of 1879 AHPs in rural New South Wales in Australia found that the most significant factors influencing recruitment and retention included work-life balance, the nature of work and location. Income, housing affordability and cost of living were not rated as highly18. However, recent findings from a case-managed rural health professionals' program in Australia to recruit nurses and AHPs found that financial support was a key incentive to participate in the program35.
Organisational factors: Organisational factors including poor health service management were a key theme impacting particularly on retention6. This suggests the need to adequately educate and prepare health service managers to undertake human resource functions relevant to all stages of recruitment and retention along the extended rural pipeline6. Inter-sectoral and interdisciplinary collaboration was identified as one way to address the issue by applying human resource knowledge, expertise and strategies to the rural health workforce sector36. Improving organisational support was important if AHPs were to maintain necessary skills for rural practice6,37.
Urban-centric policy and planning for health professionals often fails to address relevant issues for rural practice that can negatively affect recruitment and retention along the pipeline. These include the impact of professional isolation, the need to increase access to continuing professional development to better prepare and support rural practitioners and the value of recruiting locally - factors that can significantly influence retention4. This raises the question of what constitutes a reasonable retention rate for rural health professionals. According to rural health service managers, 2 years of rural practice for AHPs is reasonable10, suggesting that short-term as well as long-term approaches to retention are needed.
Professional factors: Taking into account professional differences along the pipeline highlights the need to go beyond a one-size-fits-all approach. A study of rural dieticians in New South Wales found that the majority were new graduates where one third remained in their position for less than 6 months38. In another AHP study, of those who did choose rural practice, Gen Y (those born in the 1980s and 1990s) were the hardest to retain, often staying no longer than 2 years11. Keane et al's study of rural AHPs in New South Wales reported 70% were female and 60% had a rural background. While participants generally reported high job satisfaction, the workforce was also ageing18. A national study of the rural and remote pharmacy workforce supported findings that pharmacists were generally older and were also likely to work outside hospitals than were pharmacists in urban settings22. The Careers in Rural Health Tracking Survey suggested that health professionals preferred to work in urban locations early in their career but would consider rural practice later in life39. Poor recruitment and retention rates were noted in some disciplines more than others, including podiatry and dietetics38,40. These findings suggest the need for recruitment and retention strategies that specifically target different cohorts along the pipeline.
Improving professional development along the pipeline is another strategy to increase retention, although it is not always accessed by AHPs, with one study citing poor uptake by rural physiotherapists41. Nonetheless, limited opportunities for professional development have negatively affected retention of rural AHPs where a study of rural dieticians noted the need for mentoring, education and training in specialised areas such as cancer37. Other evidence indicated that an e-mentoring program using technology combined with good communication was an effective way to reduce the isolation for rural physiotherapists and provide professional support42. Strategies to target retention more specifically include introducing a professional development allowance for AHPs to attend education and training activities such as financial support for travel and accommodation, increasing the use of information communication technology including telehealth to reduce professional isolation, invite second opinions and increase job satisfaction42-44.
Career pathways Offering AHPs incentives to alleviate professional barriers at all stages along the rural pipeline is effective45. Barriers include limited opportunities for advancement, better career opportunities elsewhere, isolation, long hours including extensive travel, problems with management, little job satisfaction and a lack of flexibility around the mix between public and private rural practice45-47. This can be offset by developing strategies based on evidence of what AHPs value and offering a balanced view where the challenges of rural practice are offset by its benefits48. For example, OTs valued autonomy, team work, diversity, a flexible work schedule, increased client contact, experience gained and rural lifestyle28. Others valued the model of care. Findings from a survey of AHPs in rural New South Wales found 46% of positions were in the public sector, 40% were private, 11% of AHPs worked across multiple sectors and 18% were self-employed18. Targeted rural pipeline strategies are needed to meet AHPs with different disciplinary and demographic profiles working in public and private sectors. For example, more young AHPs worked in the public sector and require mentoring, management support and career opportunities18.
The Rural Health Professionals Program (RHPP) established in 2012 coordinated various marketing strategies to attract nursing and allied health professionals from Australia and approved overseas locations to rural areas. Eligible candidates were case managed and matched with employers, free of charge. Candidates recruited under this program received case-managed funds to support their retention for up to 2 years including psychosocial support, professional development opportunities, mentoring and spousal employment assistance. Early findings showed that 46% of RHPP recruits had never lived in rural or remote Australia and 100 recruits (N=349) moved from practising in the city to work in rural and remote locations. However, the authors acknowledge it was too early to determine the effect of the program on longer term retention outcomes35.
Recruitment strategies along the pipeline can also focus on different cohorts of AHWs including FIFO workers, the sea/tree changers, those who enter rural practice later in life, and those with different cultural and linguistic backgrounds. Current literature focuses mainly on overseas trained doctors and nurses rather than AHPs49,50. Targeting career grade for AHPs is also important as it impacts on retention - the more senior the grade, the more likely the health professional is to stay11.
Social factors: Innovative and relevant marketing strategies that reflect diversity within and between allied health professions are called for to increase recruitment and retention along the rural pipeline. Evidence suggests strategies need to target social as well as professional factors including differential needs for age, discipline, life stage, gender, nature of work and location9,51. For example, retention strategies for early career AHPs should target the first year of rural employment as younger AHPs are less likely to stay in a rural area40.
Rural location, lifestyle and social support including family and friends in rural settings were positive indicators of recruitment and retention of AHPs along the pipeline. Pharmacists were attracted to practise in rural areas not just because of business and job opportunities but also because of the quality of rural life22. This increased with opportunities for community-based pharmacy and if their spouse/partner had a non-metropolitan background31. The friendliness of community, slower pace of life, a sense of adventure and recreation, work-life balance, adequate time off, involvement in community activities and feeling that the services they offered as AHPs were valued by the community were all important factors10,52-54. However, sometimes these were counter-balanced by the nature of rural practice with blurred boundaries between professional and social life, a sense of accountability to the community particularly when working in smaller communities, a lack of privacy and challenges around confidentiality9,51.
The rural health pipeline adapted for AHPs has emerged as a useful conceptual tool in recruitment and retention. Evidence from studies of rural AHPs indicates a flexible approach is needed to acknowledge the complexity of the issue, address diversity within and between professions and meet AHPs' professional and social needs. By avoiding a one-size-fits-all approach, the extended rural pipeline opens the door to developing recruitment and retention strategies that reflect the various stages AHPs enter rural practice along with differences in age, gender, professional needs, social context, cultural background and career stage.
Adopting an integrated, collaborative, inter-sectoral, sustained approach to develop and implement creative ways to improve AHP recruitment and retention offers an opportunity to share disciplinary and industry knowledge, skills and expertise and build capacity across sectors in this context. Rural background is well documented as a predictor for choosing rural practice. However, inspiring city-based allied health students and AHPs to become rural practitioners requires offering a balanced rather than deficit perspective of rural practice as an attractive option and positive step in a career trajectory that can begin at any stage along the extended rural pipeline48. The challenge is to ensure there is enough political will and resources available to implement and sustain strategies to improve recruitment and retention outcomes of rural AHPs.
Acknowledgements
Funding for this review was provided by Rural Health West. We would like to acknowledge the support of Dr John Wood in preparing this manuscript.
References
1. Begg S, Vos T, Goss J, Barker B, Stevenson C, Stanley L, et al. The burden of disease and injury in Australia. Report No. PHE 82. Canberra, ACT: AIHW, 2007.
2. Pink B, Allbon P. The health and welfare of Aboriginal and Torres Strait Islander people. Canberra, ACT: AIHW, ABS, 2008.
3. Standing Council on Health. National strategic framework for Rural and Remote Health. (Online). 2012. Available: http://www.ruralhealthaustralia.gov.au/internet/rha/publishing.nsf/Content/NSFRRH-homepage (Accessed 9 August 2013).
4. Mason J. Review of Australian Government health workforce programs. (Online) 2013. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/review-australian-government-health-workforce-programs (Accessed 14 August 2013).
5. Productivity Commission. Australia's health workforce, research report. (Online). 2006. Available: http://www.pc.gov.au/projects/study/health-workforce/docs/finalreport (Accessed 19 August 2013).
6. Humphreys J, Wakerman J, Pashen D, Buykx P. Retention strategies and incentives for health workers in rural and remote areas: what works? (Online) 2009. Available: http://aphcri.anu.edu.au/projects/network/retention-strategies-and-incentives-health-workers-rural-and-remote-areas-what. (Accessed 12 August 2013).
7. Waldman J. Change your metrics: if you get what you measure, then measure what you want - retention. Journal of Medical Practice Management 2006; 22(1): 13-19.
8. Australian Institute of Health and Welfare. Allied health workforce 2012. National health workforce series no. 5. Cat. no. HWL 51. Canberra, ACT: AIHW, 2013.
9. Humphreys J, Chisholm M, Russell D. Rural allied health workforce retention in Victoria: modelling the benefits of increased length of stay and reduced staff turnover. Melbourne, VIC: Victorian Department of Health, 2010.
10. Campbell N, McAllister L, Eley D. The influence of motivation in recruitment and retention of rural and remote allied health professionals: a literature review. Rural and Remote Health 12: 1900. (Online) 2012. Available: www.rrh.org.au (Accessed 12 August 2013).
11. Whitford D, Smith T, Newbury J. The South Australian Allied Health Workforce survey: helping to fill the evidence gap in primary health workforce planning. Australian Journal of Primary Health 2012; 18(3): 234-241.
12. Allied Health Professionals Australia. Allied Health Professionals Australia (AHPA) is the national voice of allied health in Australia. (Online). Available: http://www.ahpa.com.au/ (Accessed 14 August 2013).
13. Katzenellenbogen J, Durey A, Haigh M, Woods J. Critical success factors for recruiting and retaining health professionals to primary health care in rural and remote locations: contemporary review of the literature. Perth, WA; Rural Health West, 2013.
14. Fisher KA, Fraser JD. Rural health career pathways: research themes in recruitment and retention. Australian Health Review 2010; 34(3): 292-296.
15. Henry JA, Edwards BJ, Crotty B. Why do medical graduates choose rural careers? Rural and Remote Health 9(1): 1083. (Online) 2009. Available: www.rrh.org.au (Accessed 12 August 2013).
16. Bell E. Creating 'the rural pathway': Australia's university departments of rural health and rural clinical schools. International Journal of Child Health and Huan Development 2011; 4(1): 135-144.
17. Australian Bureau of Statistics. 6105.0 - Australian Labour Market Statistics, July 2013. Canberra, ACT: ABS, 2014.
18. Keane S, Smith T, Lincoln M, Fisher K. Survey of the rural allied health workforce in New South Wales to inform recruitment and retention. Australian Journal of Rural Health 2011; 19(1): 38-44.
19. Fraser J, Alexander C, Simpkins B, Temperley J. Health career promotion in the New England area of New South Wales: a program to support high school career advisors. Australian Journal of Rural Health 2003; 11(4): 199-204.
20. Eley R, Hindmarsh N, Buikstra E. Informing rural and remote students about careers in health: the effect of health careers workshops on course selection. Australian Journal of Rural Health 2007 15(1): 59-64.
21. Durey A, McNamara B, Larson A. Towards a health career for rural and remote students: cultural and structural barriers influencing choices. Australian Journal of Rural Health 2003; 11(3): 145-150.
22. Smith JD, White C, Roufeil L, Veitch C, Pont L, Patel B, et al. A national study into the rural and remote pharmacist workforce. Rural and Remote Health 13(2): 2214. (Online) 2013. Available: www.rrh.org.au (Accessed 13 August 2013).
23. Brown G, Green R. Inspiring rural practice: Australian and international perspectives. Rural Social Work and Community Practice 2009; 14(1): 63-70.
24. Dalton LM, Routley GK, Peek KJ. Rural placements in Tasmania: do experiential placements and background influence undergraduate health science student's attitudes toward rural practice? Rural and Remote Health 8(3): 962. (Online) 2008. Available: www.rrh.org.au (Accessed 14 August 2013).
25. Brockwell D, Wielandt T, Clark M. Four years after graduation: occupational therapists' work destinations and perceptions of preparedness for practice. Australian Journal of Rural Health 2009; 17(2): 71-6.
26. McAuliffe T, Barnett F. Factors influencing occupational therapy students' perceptions of rural and remote practice. Rural and Remote Health 9(1): 1078. (Online) 2009. Available: www.rrh.org.au (Accessed 12 August 2013).
27. Schofield D, Fuller J, Wagner S, Friis L, Tyrell B. Multidisciplinary management of complex care. Australian Journal of Rural Health 2009; 17(1): 45-8.
28. Wielandt PM, Taylor E. Understanding rural practice: implications for occupational therapy education in Canada. Rural and Remote Health 10(3): 1488. (Online) 2010. Available: www.rrh.org.au (Accessed 12 August 2013).
29. Charles G, Bainbridge L, Copeman-Stewart K, Kassam R, Tiffin S. Impact of an interprofessional rural health care practice education experience on students and communities. Journal of Allied Health 2008; 37(3): 127-131.
30. McAuliffe T, Barnett F. Perceptions towards rural and remote practice: a study of final year occupational therapy students studying in a regional university in Australia. Australian Occupational Therapy Journal 2010; 57(5): 293-300.
31. Fleming CA, Spark MJ. Factors influencing the selection of rural practice locations for early career pharmacists in Victoria. Australian Journal of Rural Health 2011; 19(6): 290-297.
32. Peterson GM, Fitzmaurice KD, Rasiah RL, Kruup H. Marketing of rural and remote pharmacy practice via the digital medium. Journal of Clinical Pharmacy and Therapeutics 2010; 35(4): 409-414.
33. Barnighausen T, Bloom DE. Financial incentives for return of service in underserved areas: a systematic review. BMC Health Services Research 2009; 9: 86.
34. Buykx P, Humphreys J, Wakerman J, Pashen D. Systematic review of effective retention incentives for health workers in rural and remote areas: towards evidence-based policy. Australian Journal of Rural Health 2010; 18(3): 102-109.
35. Morell A, Kiem S, Millsteed M, Pollice A. Attraction, recruitment and distribution of health professionals in rural and remote Australia: early results of the Rural Health Professionals Program. Human Resources for Health 2014; 12: 15.
36. Allan J, Ball P. Developing a competitive advantage: considerations from Australia for the recruitment and retention of rural and remote primary health workers. Australian Journal of Primary Health 2008; 14(1): 106-112.
37. Kiss NK, Davidson W, Taylor K. Mentoring and professional support programs in cancer nutrition for regional dietitians. Cancer Forum 2011; 35(2): 122-125.
38. Brown L, Williams L, Capra S. Going rural but not staying long: recruitment and retention issues for the rural dietetic workforce in Australia. Nutrition and Dietetics 2010; 67(4): 294-302.
39. Schofield D, Keane S, Fletcher S, Shrestha R, Percival R. Loss of income and levels of scholarship support for students on rural clinical placements: a survey of medical, nursing and allied health students. Australian Journal of Rural Health 2009; 17(3): 134-140.
40. Chisholm M, Russell D, Humphreys J. Measuring rural allied health workforce turnover and retention: what are the patterns, determinants and costs? Australian Journal of Rural Health 2011 19(2): 81-88.
41. Minisini M, Sheppard LA, Jones A. Self-efficacy beliefs and confidence of rural physiotherapists to undertake specialist paediatric caseloads: a paediatric example. Rural and Remote Health 10(4): 1426. (Online) 2010. Available: www.rrh.org.au (Accessed 14 August 2013).
42. Stewart S, Carpenter C. Electronic mentoring: an innovative approach to providing clinical support. International Journal of Therapy and Rehabilitation 2009; 16(4): 199-206.
43. Gagnon MP, Pollender H, Trepanier A, Duplaa E, Ly BA. Supporting health professionals through information and communication technologies: a systematic review of the effects of information and communication technologies on recruitment and retention. Telemedicine Journal and E-Health 2011; 17(4): 269-274.
44. Mills E, Airey C, Yee KC. Generation Y in healthcare: the need for new socio-technical consideration for future technology design in healthcare. Studies in Health Technology and Informatics 2007; 130: 169-179.
45. Roots RK, Li LC. Recruitment and retention of occupational therapists and physiotherapists in rural regions: a meta-synthesis. BMC Health Services Research 2013; 13: 59.
46. Brown LJ, Mitchell LJ, Williams LT, Macdonald-Wicks L, Capra S. Private practice in rural areas: an untapped opportunity for dietitians. Australian Journal of Rural Health 2011; 19(4): 191-196.
47. O'Toole K, Schoo A, Stagnitti K, Cuss K. Rethinking policies for the retention of allied health professionals in rural areas: a social relations approach. Health Policy 2008; 87(3): 326-832.
48. Bourke L, Humphreys J, Taylor J, Wakerman J. From 'problem-describing' to 'problem-solving': challenging the 'deficit' view of remote and rural health. Australian Journal of Rural Health 2010; 18(6): 205-209.
49. Dywili S, Bonner A, Anderson J, O'Brien L. Experience of overseas-trained health professionals in rural and remote areas of destination countries: a literature review. Australian Journal of Rural Health 2012; 20(4): 175-184.
50. Le Q, Kilpatrick S. Vietnamese-born health professionals: negotiating work and life in rural Australia. Rural and Remote Health 8(4): 1062. (Online) 2008. Available: www.rrh.org.au (Accessed 14 August 2013).
51. Schofield D, Fletcher S, Fuller J, Birden H, Page S. Where do students in the health professions want to work? Human Resources for Health 2009; 7(1): 74.
52. Keane S, Lincoln M, Rolfe M, Smith T. Retention of the rural allied health workforce in New South Wales: a comparison of public and private practitioners. BMC Health Services Research 2013; 13: 32.
53. Keane S, Lincoln M, Smith T. Retention of allied health professionals in rural New South Wales: a thematic analysis of focus group discussions. BMC Health Services Research 2012; 12: 175.
54. Williams E, D'Amore W, McMeeken J. Physiotherapy in rural and regional Australia. Australian Journal of Rural Health 2007; 15(6): 380-386.



