Health care has always been a complicated issue, for both advanced and emerging countries. When a nation such as India strives to provide medical coverage for its people, it faces not only the inherent complications of medicine, but also the associated costs of paying for and supplying the necessary tools, equipment and training for its practitioners. Without a stable operational model, unifying geographically scattered patients, facilities and practitioners is a daunting endeavor. Often, facilities are located in areas that are accessible only to high-income individuals, whereas low-income brackets are left to fend for themselves with facilities that are ill-funded and under-supplied. As a result, clustered and niche sociodemographic areas emerge, and those unable to procure the necessary monies and transportation to the proper facilities are forced to leave their health to chance.
Uncontrolled population growth and disorganized urbanization as well as a lack of affordable, available and accessible medical facilities has put pressure on India's rural population to find its health resources in local remedies or by make do with scarce supplies. These practices often result in the detrimental and fatal state of many patients who succumb to ailments that could have been treated.
A few programs initiated by the Indian Government have:
... finally brought some infectious diseases under control, but the nation's ability to meet the basic medical needs of its citizens remains abysmal. Despite robust economic growth over the past two decades, the infant mortality rate is three times higher than China's and seven times greater than that of the US Of the 2 million Indians in need of heart surgery, fewer than 5% get it. Seventy percent of India's 12 million blind people could be cured by a simple surgery - if it were available to them.
Although India boasts 750 000 doctors and 1.1 million nurses, practitioner density is about one-fourth what it is in the US and less than half that of China ... nominal per capita income is only $1,500 a year, patients typically have to pay 60% of health care expenses from their own pockets1.
Background
The aforementioned issues of availability and affordability in India led a few organizations to resort to the implementation of the hub and spoke model (HSM) in health care. At a high level, the fundamental tenets of HSM are to improve access to services and meet clients' needs. The model is derived from the visualization of a wheel and its central hub. The hub, or the center of the wheel, serves as the central operational headquarters of the overall mechanism. The activities vital to an enterprise's operation are located at the hub, which allows for capitalization of more specialized practices in the spokes.
Although Delta Airlines pioneered the use of the HSM in 19552, it was Bertrand Dawson, a physician of the Royal Army Medical Corps, who suggested the use of an approach similar to HSM in health care in 1920. At that time, he referred to it as 'a hierarchical system which proceeded from the simple to the complex'3.
'Domiciliary services would revolve around doctor, pharmacist, and nurse' in 'Primary health centres staffed by general practitioners, laboratories and inpatient accommodation.' These are followed by 'Secondary health centres which would provide a full range of general and specialized medical services.' These secondary health centers would relate to university hospitals where the most difficult cases could be managed. Supplementary health centers would deal with 'patients suffering from other conditions such as mental and infectious diseases'4.
'The scheme would require a new pattern of medical administration, to ensure 'unity of purpose at all levels'. It was proposed that there should be a single health authority to unify and control all health services'3 (Fig1).
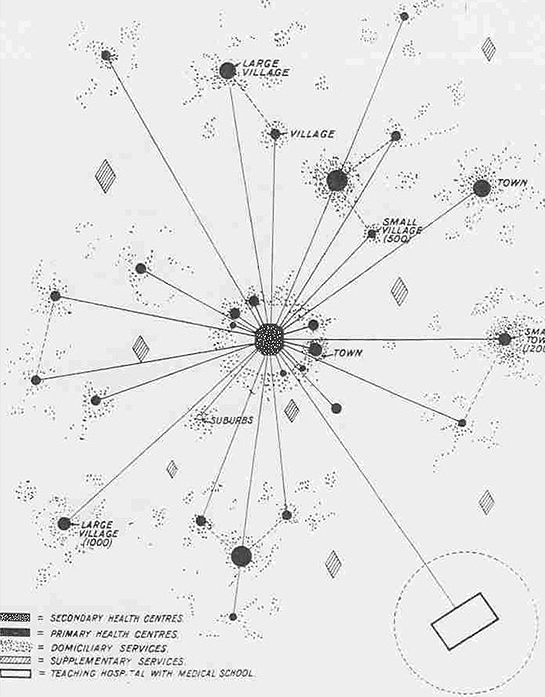
Figure 1: Chairman Lord Dawson's hierarchical system, London 19204.
Contemporary HSM experts also agree with Dr Dawson that:
On a larger level what this entails is the authorization for the larger, more established core units to essentially support the lesser ones while still allowing for the regulation and control of the overall 'wheel' movements5.
HSM offers large market coverage with efficient use of resources and flexibility in workload distribution. However, capacity limitations and changes at the hub could have a domino effect on the spokes that could be disadvantageous to the network.
Although the model can be applied to nearly any operational enterprise, its usefulness and overall efficiency is inherently driven by the core users' abilities to coordinate logistical operations within its entire practice5.
Thereby, ICT-enabled HSM becomes necessary to help resolve potential logistical issues arising from the absence of such a concept.
Role of ICT
In India, rural-urban connectivity is a major issue: 'The physical accessibility of public or private healthcare facilities is a challenge in rural areas'6. The innovativeness of ICT-enabled HSM lies in its emphasis on healthcare availability to populations spread over vast geographic areas without adding expensive infrastructure. It eliminates the need for travel unless necessary by ensuring that rural clinics (RCs) (spokes) take care of basic treatment and that patients would only need to travel to the urban hospital (UH) (hub) for specialized care.
ICT system set-up
The ICT-enabled HSM incorporates the use of cloud computing over a secured network. The healthcare workers at the RCs are provided with handheld devices or laptops connected to a secure network. These devices can be equipped with:
- wireless network cards designed to work in low connectivity areas and without the need for any phone or ethernet wires
- software with defined procedures and process flows
- various security features (antivirus, password protection, data encryption)
- communication capabilities (email and text) (Fig2).
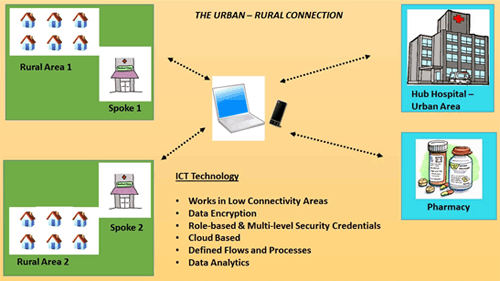
Figure 2: Example of system set-up depicting the urban-rural connection.
Data integrity
Patient information is stored on a community cloud7. The community, in this case, is the organization, the RC and the UH. Only those users with approved credentials can share and access the information securely within the network using a laptop or a mobile device. These devices are equipped with antivirus software to protect the information from any type of data breach (hacking, phishing etc). This way, patient information is kept confidential, but details can be made available in case of referrals or escalations. Patient medical records are encrypted and only shared over a secured network via directed exchange8. Within the software, the security credentials are multi-layered (requiring the user to enter their password to perform important steps), and the access privileges are role based (a doctor could have access to features such as sharing information with the UH that a nurse might not have). Some companies train their health workers to respect information confidentiality and penalize workers who do not comply9.
Patient advantages
The companies implementing the HSM have strong connections to a network of doctors and facilities that provide subsidized prices and reduced treatment fees to patients, eliminating the need to shop for facilities in the first place.
Dr Herzlinger further explains this aspect of the HSM's connectivity:
Some cancer care in India is delivered in a hub and spoke model. At the hub, they use very advanced surgical techniques for treating cancer. The spokes are the cancer centers where they do chemotherapy, radiation and rehabilitation. Anything you can do locally should be done locally10.
Most rural Indians are daily wageworkers who make about 174 rupees a day (approximately $3)11. Considering this, it is important to acknowledge that the HSM approach saves the patient a lot of travel time, waiting time, money and an otherwise unnecessary trip to the UH. Since the rural-urban hospitals are within the HSM network, the fees charged by the UH for secondary and tertiary diagnoses to the patients will also be discounted. The spokes are constantly in touch with the hub hospital, and doctors can update the spokes about a patient's case. The ICT-enabled HSM network also connects patients to pharmacies for discounted medicines.
Discussion
Using the HSM approach:
Hub hospitals in urban centers assemble the most advanced technologies and highly specialized surgical and diagnostic skills. Smaller hospitals and clinics in outlying towns are equipped with lower-level technologies and operated by non-specialist physicians, assisted by nurses and support staff. Providers at the spokes treat patients who have straightforward needs. They refer those with more complex issues back to the hub or use telemedicine technologies to consult with hub specialists on treatments12.
This tightly coordinated web cuts equipment and expertise costs. It also creates specialists at the hubs who, while performing high volumes of focused procedures, develop the skills that will improve quality13.
The advantage of having expensive and specialized equipment and practitioners at fixed centralized locations is that they alleviate the pressure for smaller healthcare facilities to spend their limited resources on equipment that is not frequently used but still critical for health care.
By contrast, hospitals in the US are spread out and uncoordinated, duplicating care in many places without high enough volume in any of them to provide the critical mass to make the procedures affordable. Similarly, an MRI machine might be used four to five times a day in the US but 15 to 20 times a day in the Indian hospitals. We have to make the equipment sweat!13
In the cases of the more successful privatized hospitals, India, as well as the rest of the world, is paying careful attention to this 'configured networks of care and facilities in a hub-and-spoke design'12. One of the primary benefits of HSM that is being revealed in India is that 'This allows for a more-orderly progression of care and rational allocation of often-scarce resources'12.
Thus, success is being found in India when practising medical facilities centralize their assets and diversify their more benign practices in the lower cost ambulatory locales. The end result is a lower centralized cost, as providers only procure the equipment and resources they need. Moreover, the Indian population, in general, is able to access greater coverage for fulfilling their basic healthcare needs.
Reasons for success
Attracting and retaining doctors: No matter how efficient a hospital may be, it cannot be deemed successful if its doctors and nurses are incompetent or unable to perform their primary tasks. As such, Indian hospitals operating under the HSM are actually retaining and attracting capable doctors who are keenly interested in 'high volume and sheer variety of cases that attract talent to these hospitals'. Also, 'doctors can build their capabilities faster in [HSM hospitals] ... in turn, [this] contributes to the high quality of outcomes at these hospitals'14.
Nurturing and updating treatment protocols: Perhaps most unique to India's HSM success is its incorporation of developed protocols for both mundane tasks and highly complex procedures. Knee and hip replacements, as well as cardiac and cancer surgeries, all have itemized procedures that are adhered to despite being executed in facilities outside of the central hub. According to the data found, 'One in 200 angioplasty patients in the US will require emergency surgery and half of those patients will die, only two out of 40 000 angioplasty patients at CARE [HSM] Hospitals have required emergency surgery and just one has died on the operating table since the hospital's inception in 1997'15.
Creating specialties in esoteric practices of medicine: Similar to retaining doctors, part of the allure for HSM facilities is that due to the sheer volume of patients from rural areas arriving for care and treatment at the hub, doctors are able to 'focus on specific types of medical problems. As volumes increase, relatively rare conditions are treated often enough that doctors become world-class experts in those areas'15. As the patients access either hubs or ambulatory facilities, the doctors become subject matter experts in varying fields simply through sheer exposure to the volume of patients.
Assessing thriftiness: Arguably the greatest cost saving, and subsequently the most successful aspect of HSM-practising Indian facilities, is their staunch position on being thrifty. 'The goal is to maximize the number of patients treated rather than the number of procedures conducted'5. This aspect is achieved through measures that can be seen as both 'innovative and remarkably mundane'. Medical practitioners often reuse equipment and resources that would be discarded in other nations. Cleaned and sterilized, hand tools and hardware are recycled and redistributed in urban and rural centers rather than adding to unnecessary costs by importing more supplies. This thrifty approach not only saves money and other resources but also allows facilities to treat patients rather than offload them due to a lack of viable utilities.
Technological contribution: Rural India is known for poor roads and communication infrastructure. Due to the high set-up costs, telephones and faxes are few and far between. Using a courier service to send patient information may prove costly in terms of money, data confidentiality, report errors, and time.
ICT eliminates the dependencies on paper, courier services and other methods. Data transfer between hubs and spokes takes negligible time (less than a minute), and each patient's report is sent individually; therefore, the chance of a report error is practically zero. India has 27 million landline users compared to 960 million mobile phone users (urban 557 million, rural 403 million)16, so the probability of finding mobile phones is higher than finding courier services in a rural area. India takes the top spot amongst 148 countries in terms of affordability of ICT technology17. Hence, the implementation of ICT in HSM should be an easy choice. Since most companies are using cloud-based platforms, '[this helps] to reduce infrastructure cost. Scaling up becomes easier on a cloud environment'18.
The HSM is also efficacious in disseminating information for health awareness, immunizations or precautions to be taken during epidemics (such as Ebola). Companies implementing the HSM have helped create and sustain thousands of rural jobs, both direct and indirect.
HSM is an effective mechanism that allows for greater distribution while minimizing costs when paired with ICT. There are many areas in emerging nations in Africa and South America where healthcare accessibility is limited. This also holds true for remote areas in advanced nations such as Sweden, Finland, Russia, Australia, Canada and the USA where there is limited access due to weather conditions and other factors. HSM paired with ICT will effectively service such regions, reducing unnecessary travel and other related costs. 'You don't need a PhD in economics to figure out this model is a lot cheaper and probably a lot more convenient for patients'10.
Many Indian healthcare companies such as iKure, Vaatsalya Healthcare, Smile Merchants (Dental), Apollo Hospitals and Care Hospitals are demonstrating that using HSM paired with ICT not only allows for treatment of medical conditions but also lowers costs and improves availability, making health care accessible and affordable to the nation.
Acknowledgements
The author would like to express special thanks to the management team at iKure (www.ikure.in and www.ikuretechsoft.com) (Sujay Santra - Founder & CEO, and Dr Tirumala Santra Mandal, Public Relations Corporate Communications Manager), who walked him through the implementation of iKure's hub and spoke model and for sharing their company's information.
References
1. Govindarajan V, Ramamurti R. Delivering world-class health care, affordably. Harvard Business Review (Internet) 2013; 2. Available: http://hbr.org/2013/11/delivering-world-class-health-care-affordably/ar/1 (Accessed 26 February 2014).
2. Delta Flight Museum. History - Delta First in the Air, 1955. (Internet). Available: https://www.deltamuseum.org/exhibits/delta-history/first-in-the-air (Accessed 7 August 2015).
3. Rivett G. The Development of the London Hospital System. 1823-2015 (Internet) 2015. Available: http://www.nhshistory.net/regions_&_districts.htm (Accessed 2 August 2015).
4. Dawson B. Interim report on the future provision of medical and allied services. Great Britain, Ministry of Health. (Internet) 1920. Available: http://www.nhshistory.net/Dawson%20report.html (Accessed 2 August 2015).
5. Herzlinger R, Ghorawat A, Krishnan M, Saggi N. Hub and spoke, healthcare global, and additional focused factory models for cancer care. Harvard Business School Case 313-030. (Internet) 2012. Available: http://www.hbs.edu/faculty/Pages/item.aspx?num=42927 (Accessed 19 May 2014).
6. Aitken M, Backliwal A, Chang M, Udeshi A. Understanding healthcare access in India. What is the current state? IMS Institute for Healthcare Informatics (Internet) 2013; 2. Available: http://www.imshealth.com/deployedfiles/imshealth/Global/Content/Corporate/IMS%20Institute/India/Understanding_Healthcare_Access_in_India.pdf (Accessed 20 January 2014).
7. Community Cloud. Techopedia. Available: http://www.techopedia.com/definition/26559/community-cloud (Accessed 29 May 2015).
8. Directed Exchange. Health Information Exchange. What is HIE? Available: http://www.healthit.gov/providers-professionals/health-information-exchange/what-hie (Accessed 28 May 2015).
9. Section 43(b), The Information Technology Act, 2000. Ministry of Law, Justice and Company Affairs, Government of India. Available: http://deity.gov.in/sites/upload_files/dit/files/downloads/itact2000/itbill2000.pdf (Accessed 21 May 2015).
10. Dunn L. What the US can learn from healthcare delivery overseas: Q&A with Harvard Business School's Regina E. Herzlinger. Becker Hospital Review, Online Edition (Internet) 2013. Available: http://www.beckershospitalreview.com/hospital-management-administration/what-the-us-can-learn-from-healthcare-delivery-overseas-qaa-with-harvard-business-schools-regina-e-herzlinger.html (Accessed 19 May 2014).
11. Prabhu N. MNREGA wage rate hiked to Rs. 174 a day. The Hindu, Online Edition (Internet) 2015. Available: http://www.thehindu.com/news/national/karnataka/mnrega-wage-rate-hiked-to-rs-174-a-day/article4715162.ece (Accessed 25 May 2015).
12. Govindarajan V. Reviving the health of health-care. Business Today, Online Edition (Internet) 2014. Available: http://businesstoday.intoday.in/story/vijay-govindarajan-on-healthacre-in-india/1/201864.html (Accessed 7 July 2014).
13. Ramamurti R, Govindarajan V. India's secret to low-cost health care. Harvard Business Review (Internet) 2013. Available: http://blogs.hbr.org/2013/10/indias-secret-to-low-cost-health-care (Accessed 1 March 2014).
14. Govindarajan V, Ramamurti R. Delivering world-class health care, affordably. Harvard Business Review (Internet) 2013; 4. Available: http://hbr.org/2013/11/delivering-world-class-health-care-affordably/ar/1 (Accessed 26 February 2014).
15. Govindarajan V, Ramamurti R. Delivering world-class health care, affordably. Harvard Business Review (Internet) 2013; 5. Available: http://hbr.org/2013/11/delivering-world-class-health-care-affordably/ar/1 (Accessed 26 February 2014).
16. Telecom Regulatory Authority of India. Highlights of Telecom Subscription Data (Internet) 2015; 1. Available: http://www.trai.gov.in/WriteReadData/PressRealease/Document/PR-TSD-Feb-10042015.pdf (Accessed 19 August 2015).
17. Networked Readiness Index (4th pillar: Affordability). Global Information Technology Report (Internet) 2015. Available: http://www3.weforum.org/docs/GITR15/IND.pdf (Accessed 19 August 2015).
18. Mishra D. A cure for health ailments in rural areas. Business Standard, Online Edition (Internet) 2013. Available: http://www.business-standard.com/article/companies/a-cure-for-health-ailments-in-rural-areas-113111800016_1.html (Accessed 2 June 2014).
Correction: A correction was made to the Acknowledgements on 15 February 2015.
