Tackling health inequalities is a global challenge. Around half the world's population live in rural and/or remote areas, but only 38% of these have access to nurses, while the supply of doctors is lower and more patchy1.
To address the problem of the unequal geographical distribution of health workers, several countries have adopted specific policies designed to attract and retain these professionals, doctors included, in rural and/or remote areas. International experience shows that access to and uptake of health services is dependent on health equity strategies, whereby efforts are made to recruit and retain professionals in more vulnerable areas to provide their populations with health care1-4.
Maciel Filho5 has reported on government initiatives from some countries to boost the recruitment and retention of doctors in areas that are far from big cities and/or hard to access. Colombia, Peru, Costa Rica, Mexico, and Ecuador have all introduced compulsory social service. In Colombia in particular, universities are important actors in this process, since the new university curriculum has made this social service - better known as 'the rural year' (el año rural) - a prerequisite for obtaining a medical license.
Mexico's work in this field is more consolidated, because Mexico first introduced this social service in 1945, via rural cooperatives. For would-be doctors to obtain their license, they must first spend 12 months at a designated location. Meanwhile, in Chile, medical career paths are established according to the specific features of the target areas, such as their geographical distance and risks, and the physical and financial infrastructure available for the work, while also providing professional development opportunities. In Australia, scholarships are available for students of medicine willing to gain experience at rural or remote locations5,6.
The form these measures take can be more incentive-oriented or more coercive in nature, covering regulations, education, selection, and financial support1,2. Most of them are aligned with WHO's recommendations to improve the retention of health workers in rural and remote areas7.
The reality around the world is that there are disparities in healthcare, shortages of health workers, and a poor distribution of the existing workforce. Recognizing this fact, many countries are developing joint strategies to assure equitable health care based on global perspectives on health8,9. One of the strategies being pursued is the organized migration of health workers from countries with more health professionals to those with a shortage10,11.
A notable case in Latin America was Venezuela's Inside the Neighborhood Mission (Misión Barrio Adentro), a program created in 2003 to strengthen primary health care in cooperation with Cuba. Thanks to this program, primary healthcare coverage has been expanded, with the training and deployment of health teams made up of doctors, nurses, dentists, and other professionals. It has also served to decentralize the offer of health services and foster their uptake by the population12-14.
Wilson et al (2009)2 have argued that more detailed research is needed to assess programs where foreign doctors are recruited to cover shortfalls in given areas. Although such initiatives may alleviate the problems in the short term, the terms of the international agreements must be considered, as well as language issues, cultural barriers, ethical issues, and the experience of doctors and service users.
In Brazil, the challenge of providing a proportionate offer of health professionals, especially doctors, throughout the country has been addressed in a number of government interventions5,15. According to Maciel Filho5, the country's efforts to attract and retain health workers to its inland regions; small and mid-sized municipalities; and rural, remote, hard-to-access, and socially vulnerable areas date back to the 1960s.
Basically, two key initiatives have been taken in Brazil this century. The first was the Inland Health Care Program (Programa de Interiorização do Trabalho em Saúde), which ran from 2001 to 2004. Its aim was to foster primary health care through the Family Health Program, improving the distribution and training of doctors and nurses in order to assure their presence in municipalities in inland parts of the country, which are often poor and remote. Unfortunately, only 469 doctors were provided through the program5. The other government initiative is the Valuing Primary Healthcare Program (Programa de Valorização da Atenção Básica, PROVAB), introduced by Inter-Ministerial Directive 2087 on 1 September 2011, with the aim of getting doctors, nurses, dentists, and other health workers to spend a year working in primary health care in areas with a shortage of these professionals. Newly graduated doctors receive a monthly stipend and potentially an extra 10% on their grade in their medical residency exam. Although it has helped attract doctors to remote areas, PROVAB has failed to attain the numbers necessary to meet the needs of the target municipalities because of the limited interest shown by medical professionals. In 2012, 4671 health professionals - doctors, nurses, and dentists - were selected as part of the PROVAB program. However, only 617 were actually hired, and only 381 of these were doctors. Most of them (67%) were deployed in the Northeast Region of the country16. In 2013, the program hired 3800 doctors, who were allocated in 1300 different municipalities17.
Until recently, the difficulty of attracting and retaining doctors and other health workers to remote/rural areas, areas far from big cities, and small municipalities remained. This has hampered the supply of health services and thereby entrenched the inequitable access to health services by different portions of the population. Several studies have identified a marked inequality between different regions of Brazil when it comes to access to health services18,19.
There is a marked disparity in the concentration of doctors in different regions and states, and between state capitals and other parts of states20. According to the Federal Board of Medicine (FBM) 'two of the major regions of the country are below the national rate: the North, with 1.01, and the Northeast, where there are 1.2 doctors per thousand inhabitants. The best placed region is the Southeast, with a ratio of 2.67, followed by the South, with 2.09, and the Central West, with 2.05'(p. 36)21. In other words, the South and Central West regions are the closest to the national average, while the North and Northeast regions have the fewest doctors per inhabitant; the best supplied region is the Southeast Region, where there are more doctors than the national average20,21.
A study by Girardi22 to identify the shortage of primary healthcare doctors shows that the shortfall is far more marked in municipalities in the North Region of Brazil (the Amazon region). The study also shows significant disparities in the distribution of these professionals between state capitals and other parts of states.
This study focuses specifically on the provision of medical professionals in the remotest areas of Brazil inhabited by the most isolated peoples: indigenous groups and maroon communities. According to the 2010 census, the native Brazilian indigenous population comprises 517 383 people, occupying 505 indigenous reserves in forest and rural lands, covering 12.5% of the national territory. They belong to 250 ethnic groups and speak 274 different languages; about half of them live in the reserves in northern Brazil (Amazon region)23. The indigenous health subsystem is organized into 34 Indigenous Health Districts (Distritos Sanitários Especiais Indígenas, DSEIs).
Throughout the Americas, when runaway slaves formed rural maroon communities, the places they chose were typically hard to access - normally remote and inhospitable24. More than 3000 maroon communities are currently estimated to remain in Brazil. The first step for their official recognition is certification by the government agency Fundação Cultural Palmares, based on an anthropological report. In November 2014 there were 2431 certified maroon communities in 801 municipalities in Brazil25. Both maroon communities and native indigenous populations live in very remote, often vulnerable rural settings with limited access to health services26,27.
This report describes the implementation of the Mais Médicos program and maps out the provision of doctors in the country in 2014, comparing it with the corresponding data for 2013, focusing on their distribution in rural, remote, and socially vulnerable settings.
To analyze the implementation of the Mais Médicos program, we mapped out the provision of doctors in the country, comparing their supply per municipality in 2014 with the corresponding data for 2013. It was difficult to determine exactly how many doctors were working in each of the 5570 municipalities in July 2013, as there is no reliable baseline for the number of physicians in Brazil. We opted to use the information from the FBM published in February 201321. The National Register of Health Establishments (Cadastro Nacional de Estabelecimentos de Saúde, CNES) system was another potential source of data, but three main problems precluded its use:
- Completeness of the databases: the professionals themselves entered data into the FBM database, which had 415 206 doctors registered. The data on the CNES database are provided by the municipal health authorities. There were 315 965 doctors on the CNES database in June 2013. A plausible hypothesis is that the CNES data is out of date, as there are no penalties for municipalities that fail to keep them updated.
- Quality of information: CNES is a complex information system that stores different types of administrative data on the national health system (Sistema Único de Saúde). The data are entered by employees working at the country's 5570 municipal health departments. The quality of the information varies greatly, as does the timeliness of updates. The data on the FBM database are entered by the doctors themselves, who are more likely to provide reliable information for their professional license.
- Credibility and transparency for medical professionals: by working with the FBM database, access to which was made available to us promptly upon request, we were able to ensure the transparency and credibility of the study results for medical professionals. While it is possible to access the CNES database from the Ministry of Health website, the procedures are complex and require multiple interpretations and decoding operations.
One limitation of the FBM database is the lack of precision in the determination of the number of doctors per municipality, since it classifies doctors by the mailing address they register. Another point is that the FBM does not provide data on every municipality, with the information gap being particularly marked in municipalities with a smaller population. In order to extrapolate the data for areas where none was available (28%), we imputed the regional medians (North, Northeast, Central West, Southeast, and South) for the different categories of municipality (<5000 inhabitants; 5001-10 000 inhabitants; 10 001-20 000 inhabitants; 20 001-50 000 inhabitants, >50 000 inhabitants). We used medians to prevent extreme values from biasing the data. When we plotted the trend line, we found that the imputed data hardly altered the distribution of the values for the states. Since the FBM data were published, five new municipalities have been created, to which we have assigned the same ratio of doctors per thousand inhabitants as were in the municipality of origin.
To prepare the maps, the ratio of one doctor per thousand inhabitants was taken as the parameter of reference, as set forth in Ministry of Health Directive 1101 of 200228. In the legends for the maps, the municipalities in the highest category (green) are the ones that have this or a higher doctor-to-population ratio. The municipalities marked red are in the lowest category, with less than 0.1 doctors per thousand inhabitants, which corresponds to one-tenth of the number recommended in the legislation. The computer program used to prepare the maps and legends was TabWin v3.6 (Datasus; http:// www.datasus.gov.br/tabwin).
Ethics approval
The study was approved by the Research Ethics Board of the University of Brasilia (Parecer #399.461 - CAAE 21688313.9.0000.0030).
Program implementation in priority areas
The Mais Médicos program was instituted by Provisional Measure 621 on 8 July 201329, and Law 12.871 of 22 October 201330. It introduced long- and short-term measures designed to cover shortfalls in the supply of doctors at primary healthcare units and to diminish regional inequalities in health.
In the short term, the program offers 3-year contracts to attract doctors to work in primary health care in municipalities in inland, rural, and remote areas, and the outskirts of big cities31. In its first public call (July 2013) 3511 municipalities applied to join the program, requesting a total of 15 460 doctors for the primary healthcare units. Although the program prioritizes the recruitment of Brazilian professionals, only 1096 doctors registered in Brazil enrolled and were hired, while another 522 places were taken by physicians who had trained abroad, together filling 10.5% of the vacancies. These doctors were sent to work in 579 municipalities, or 16.4% of the municipalities that originally requested doctors32. As a result, a technical cooperation agreement was signed with the Pan-American Health Organization to create a partnership between Brazil and Cuba for positions not filled by Brazilian doctors to be taken by Cubans. The influx of doctors from Cuba and other countries has been strongly opposed by medical entities in Brazil, which have filed two injunctions, claiming it is unconstitutional33.
The doctors enrolled under the program receive a monthly stipend paid by the Ministry of Health, while the municipality where they work is responsible for covering their food and housing costs, as well as any transportation costs they incur in exercising their professional activities. The contracts are for 3 years, and can be renewed for another 3 years.
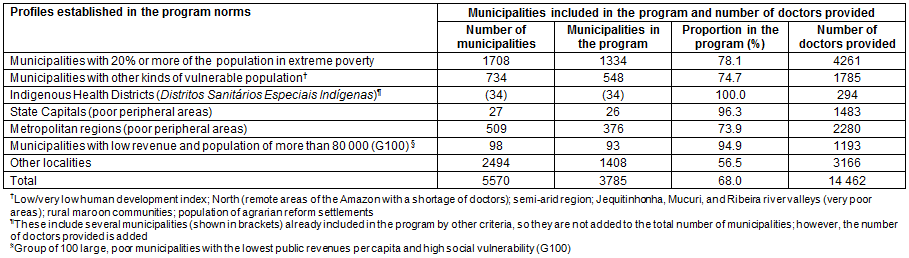
Initially, the priority municipalities for participation in the program were ones that had 20% or more of their population living in extreme poverty, or were located in poor peripheral areas around big cities, or had more than 80 000 inhabitants and the lowest levels of public revenue per capita, or had Amerindians living in indigenous reserves (forest/rural) covered by DSEIs31. Subsequently, municipalities with other characteristics were included: those with a low or very low human development index, or situated in the semiarid region in the Northeast Region of the country, or in the North Region (remote areas of the Amazon), or in the Jequitinhonha, Mucuri, and Ribeira river valleys (areas of extreme poverty); municipalities with rural maroon communities or agrarian reform settlements were also made eligible34,35. Table 1 shows the vulnerability profile of the 5570 Brazilian municipalities according to the above-mentioned criteria.
The long-term measures of the Mais Médicos program are geared towards improving the medical education in the country by increasing the supply of medical courses, as well as providing for more places on degree courses and medical residencies. By January 2015 almost 4400 new places had been created on medical courses - 1400 at public institutions and 3000 at private ones - while 39 municipalities had been selected to host new medical schools36. In parallel, there are also investments in infrastructure, with the primary healthcare units at all the participating municipalities receiving new equipment and refurbishments.
Table 1: Distribution of municipalities and participation in the Mais Médicos program, according to the profiles of vulnerability defined in the regulations for the program, Brazil, 2013-2014
Mapping the provision of doctors for rural, remote, and socially vulnerable areas
In the 12-month period from July 2013 to July 2014, there were five separate public calls for doctors to join the program, which attracted a total of 14 462 professionals, corresponding to 93.5% of the doctors demanded; all the 3785 participating municipalities (68.0% of the total) received doctors (Table 1). According to the data analyzed for this report, 1846 (12.8%) were Brazilians who trained in Brazil and were registered with the FBM; 456 (3.1%) were Brazilians who had trained abroad and were not registered in the country; 11 429 (79.0%) were from the technical cooperation agreement with Cuba, and 731 (5.1%) were foreigners of other nationalities, mainly Venezuelans and Argentineans. All the doctors who earned their degrees abroad received a Ministry of Health Registration number (Registro do Ministério da Saúde) to work in primary health care in a specific municipality for the 36-month duration of the program.
The professionals from the program were deployed in areas identified as having a shortage of doctors, namely rural and remote areas far from big cities, areas with traditional indigenous, river-dependent, and maroon communities, and socially vulnerable urban areas. Table 1 shows the 3785 municipalities that are covered by the program and their vulnerability profiles. Each of the 34 DSEIs includes several municipalities already listed in the program under another profile, so they were not added to the total of municipalities, but the number of doctors allocated to the DSEIs was added. Most of the municipalities included in the program (more than 70%) fitted into at least one of the priority profiles, but more than half of the 'Other localities' were also included.
If we compare the doctor-to-inhabitant ratio per municipality before and after the Mais Médicos program, we can see that in the February 2013 baseline, there was a marked concentration of doctors in the South, Southeast, and Central West regions (Fig1). There were 374 municipalities, mostly in the North and Northeast regions, that had fewer than 0.1 doctors per thousand inhabitants, which is ten times lower than the ratio established by the Ministry of Health22.
When we analyzed the scenario 12 months after the introduction of Mais Médicos, we found a significant increase in the supply of doctors in the target municipalities (Fig2), especially in the most critical regions. More than 80% of the municipalities in the North and around 73% of the municipalities in the Northeast - the two regions with the most critical shortage of medical professionals - received doctors from the program. The number of municipalities with fewer than 0.1 doctors per thousand inhabitants decreased from 374 to 95, which represents a 75% reduction. Eighty-one of the 95 municipalities remaining in the lowest category (85%) did not enroll for the program. The increase in the ratio of doctors per inhabitant in areas with a scarcity of such professionals has helped counterbalance the inequality of access to health care, one of the objectives of the legislation.
A total of 294 doctors were deployed to cover all the 34 DSEIs included in the program (100%). We calculated a ratio of 0.45 doctors per thousand indigenous people for this population group, but with significant differences between different DSEIs. The most highly populated was found to have 0.04 doctors per thousand inhabitants, while the least populated had 2.02. These values are only for the doctors from the 'Mais Médicos program' serving the indigenous people registered in a national database called the Indigenous Healthcare Information System (Sistema de Informações da Atenção à Saúde Indígena); there were no data available on the number of doctors serving in DSEIs before the program37.
Table 2 shows the distribution of municipalities with certified maroon communities, by region and number of doctors provided. The 801 municipalities in question received 3390 new doctors thanks to this program - around 23% of the total. Before Mais Médicos, there were already no municipalities with maroon communities in the Central West or South regions with fewer than 0.1 doctors per thousand inhabitants. By the end of the period under study, there was a significant decrease in the number of municipalities with maroon communities with fewer than 0.1 doctors per thousand inhabitants, with the largest drop occurring in the North Region: from 18.3% to 2.4% municipalities (decrease of 87%).
In 2014, more than 30% of the municipalities with maroon communities in the richest regions (Southeast, South and Central West) had more than one doctor per thousand inhabitants, whereas in the North and Northeast fewer than 7% of the municipalities reached that goal. Essentially, although regional inequalities have decreased, they have not been eliminated.
Table 2: Distribution of municipalities with certified maroon communities according to the region and the doctor-to-inhabitant ratio before and after the Mais Médicos program, Brazil, 2013-2014
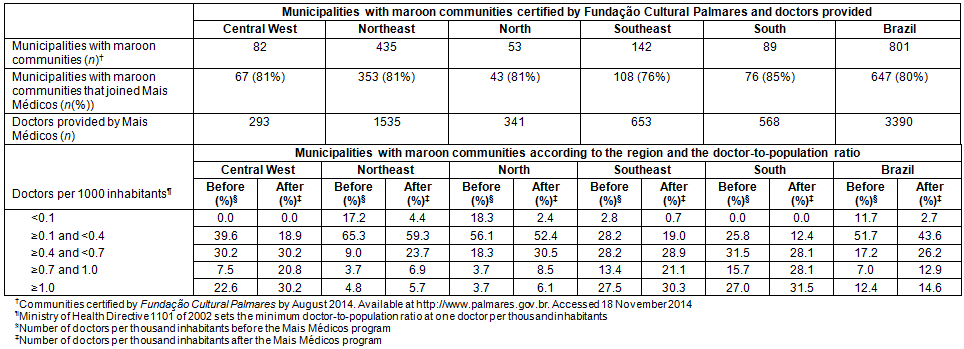
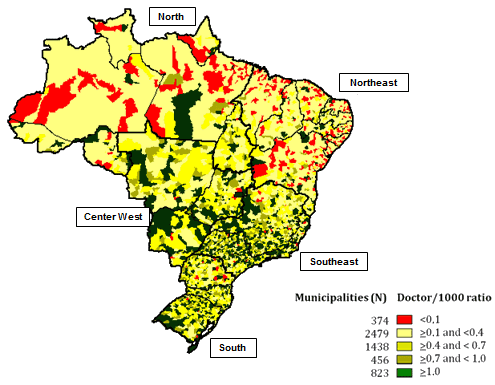
Figure 1: Distribution of municipalities according to the number of doctors per thousand inhabitants prior to the Mais Médicos program, Brazil, 2013.
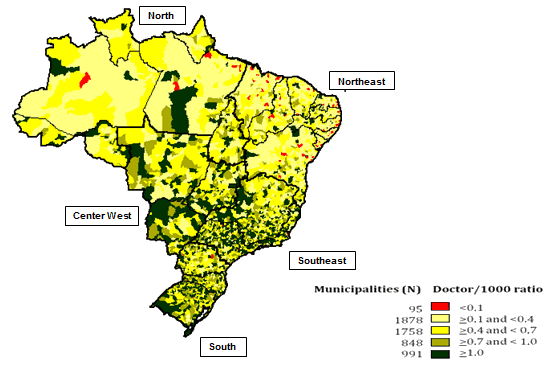
Figure 2: Distribution of municipalities according to the number of doctors per thousand inhabitants after the Mais Médicos program, Brazil, 2014.
Discussion
The strategies adopted by the Brazilian government since the 1960s have not been successful in spreading the supply of healthcare services inland or achieving a more equitable distribution of health workers, especially doctors, as evidenced by the data available until 2013.
Dolea et al and Wilson et al have undertaken critical reviews of the development of international interventions in recent years. They warn that although coercive strategies may relieve the recruitment problem in the short run, there is no evidence of the sustainability of their positive results over time. They add that doctors who do a residency in family health and gain experience in rural areas are more likely to work in these areas after graduating1,2.
Some studies1-3,38 have identified the factors that health professionals see as hampering and/or preventing their staying in rural areas, which include academic isolation, lack of local support, poor physical or limited infrastructure at the healthcare units, limited employment opportunities for their spouse/partner, family issues such as lifestyle options and access to educational and leisure services, and poor housing.
Another finding of some studies1,2 is that the inclusion of rural residencies in medical school curricula and the provision of grants for doctors to work in rural areas can effectively contribute to the retention of doctors in these areas. The origin of medical professionals also has an influence: doctors originally from rural and/or inland parts are often more inclined to work in such areas. One of the Mais Médicos program actions promotes profound changes in medical education: new medical schools were created in smaller interior towns and precocious insertion of students into primary health care in poor areas is mandatory39.
One limitation of this study is the fact that it analyzes secondary data, and is therefore unable to assess the aspects that may impinge on the retention of professionals in places where they are assigned to work under the Mais Médicos program. Undergoing projects and future studies based on primary data to investigate the retention of doctors in rural areas of Brazil could fill this gap.
This study analyzes the introduction of the Mais Médicos program in Brazil by mapping out the distribution of doctors in the country, demonstrating that when it comes to rural and remote areas, two priority target groups - indigenous groups (DSEIs) and maroon communities - have particularly benefitted from the deployment of new doctors. These populations live in very remote, often vulnerable rural settings with limited access to health services26,27.
Based on the data presented here, we can state that the Mais Médicos program has provided greater access to health services by population groups that have traditionally been deprived of such services, thanks to the government strategy to provide a more equitable supply of primary healthcare services.
This initial analysis shows that the Mais Médicos program has achieved positive indicators in the short term, assuring the presence of doctors in primary healthcare teams in rural, remote, hard-to-access, and socially and economically vulnerable areas. However, substitution of the currently working foreign professionals with doctors newly graduated from Brazilian schools of medicine under new curriculum guidelines and a more systematic integration with the public health system are targets yet to be attained in the mid- and long term. Currently, the professionals are working under 3-year contracts, renewable for a further 3 years, but there is no guarantee that these will be renewed. It is therefore important to discuss the sustainability of this government initiative, meaning continued coverage for population groups that have historically been overlooked.
Acknowledgements
This research project was funded by the Brazilian National Research Council (CNPq) and the Science and Technology Department (DECIT) under Public Call no. 41/2013, protocol 405103/2013-1, coordinated by Dr Leonor Maria Pacheco Santos (University of Brasilia). The authors are grateful to Professor Sandra Maria Chaves dos Santos (Federal University of Bahia) and Professor Mauro Niskier Sanchez (University of Brasilia), who collaborated in the project preparation for grant application.
References
1. Dolea C, Stormont L, Braichet JM. Evaluated strategies to increase attraction and retention of health workers in remote and rural areas. Bulletin of the World Health Organization 2010; 88: 379-385.
2. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health (Internet) 2009; 9: 1060. Available: www.rrh.org.au (Accessed 18 December 2015).
3. Strasser R, Neusy AJ. Context counts: training health workers in and for rural and remote areas. Bulletin of the World Health Organization 2010; 88(10): 777-782.
4. Huicho L, Dieleman M, Campbell J, Codjia L, Balabanova D, Dussault G, et al. Increasing access to health workers in underserved areas: a conceptual framework for measuring results. Bulletin of the World Health Organization 2010; 88(5): 357-363.
5. Maciel Filho R. Estratégias para Distribuição e Fixação de Médicos em Sistemas Nacionais de Saúde. (Tese de Doutorado em Política, Planejamento e Administração em Saúde). Rio de Janeiro: Universidade Estadual do Rio de Janeiro, Instituto de Medicina Social e Preventiva, 2007.
6. Carvalho MS. Programa de Valorização dos Profissionais da Atenção Básica: um olhar implicado sobre sua implantação. (Dissertação de Mestrado). Brasília: Universidade de Brasília, Pós Graduação em Saúde Coletiva, 2013.
7. Rourke J. WHO recommendations to improve retention of rural and remote health workers - important for all countries. Rural and Remote Health (Internet) 2010; 10: 1654. Available: www.rrh.org.au (Accessed 19 December 2015).
8. Forcier MB, Simoens S, Giuffrida A. Impact, regulation and health policy implications of physician migration in OECD countries. Human Resources for Health (Internet) 2004; 2: 12. Available: http://human-resources-health.biomedcentral.com/articles/10.1186/1478-4491-2-12 (Accessed 21 December 2015).
9. Miguelote VRS, Fortes MT, Fagundes M, Varella TC. Distribuição da Força de Trabalho: equidade e negociação. Physis Revista de Saúde Coletiva 2008; 18(2): 317-338.
10. Frenk J, Chen L, Bhutta ZA, Cohen J, Crisp N, Evans T, et al. Health professionals for a new century: transforming education to strengthen health systems in an interdependent world. Lancet; 2010; 376: 1923-1958.
11. Scheffler RM, Liu JX, Kinfu Y, Dal Poz MR. Forecasting the global shortage of physicians: an economic- and needs-based approach. Bulletin of the World Health Organization 2008; 86(7): 516-523.
12. Aguirre V. Barrio Adentro en Salud: un proyecto político y social de la República Bolivariana de Venezuela. Salud Colectiva (Internet) 2008; 4(2): 221-238. Available: http://www.scielo.org.ar/scielo.php?script=sci_arttext&pid=S1851-82652008000200011 (Accessed 22 December 2015).
13. Briggs CL, Mantini-Brigg C. 'Misión Barrio Adentro': Medicina Social, Movimientos Sociales de los Pobres y Nuevas Coaliciones en Venezuela. Salud Colectiva (Internet) 2007; 3(2): 159-176. Available: http://www.scielo.org.ar/scielo.php?script=sci_arttext&pid=S1851-82652007000200005 (Accessed 22 December 2015).
14. Henrique F, Da Ros MA, Goronzi TA, Soares GB, Gama LA. Modelo de atenção primária à saúde na Venezuela, Misión Barrio Adentro I: 2003-2006. Trabalho, Educação e Saúde. 2014; 12(2): 305-326.
15. Oliveira FP, Vanni T, Pinto HA, Santos STR, Figueiredo AM, Araújo SQ, et al. Mais Médicos: um programa brasileiro em uma perspectiva internacional. Interface (Botucatu) (Internet) 2015; 19(54): 623-634 Available: http://www.scielo.br/scielo.php?pid=S1414-32832015000300623&script=sci_arttext (Accessed 5 March 2016).
16. Carvalho MS, Sousa MF. Como o Brasil tem enfrentado o tema provimento de médicos? Interface (Botucatu) (Internet) 2013; 17(47): 913-926. Available: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1414-32832013000400012 (Accessed 17 December 2015).
17. Ministério da Saúde. Pacto Nacional pela Saúde (Internet) 2013. Available: http://bvsms.saude.gov.br/bvs/publicacoes/pacto_nacional_saude_mais_medicos.pdf . (Accessed 18 December 2015).
18. Tomasi E, Fachini LA, Thumé E, Piccini RX, Osorio A, Silveira DS, et al. Características da utilização de serviços de atenção básica à saúde nas regiões Sul e Nordeste do Brasil: diferenças por modelo de atenção. Ciência e Saúde Coletiva 2011; 16(11): 4395-4404.
19. Campos FE, Machado MH, Girardi SN. A fixação de profissionais de saúde em regiões de necessidades. Divulgação em Saúde para Debate, Rio de Janeiro. (Internet) 2009; 44: 13-24. Available: http://www.cnts.org.br/public/arquivos/Artigo_Campos.pdf (Accessed 3 January 2016).
20. Nogueira RP. Mercado de trabajo en salud. Conceptos y medidas. Educación Médica y Salud (Internet) 1986; 20(4): 524-532. Available: http://pesquisa.bvsalud.org/portal/resource/pt/pah-16631 (Accessed 28 December 2015).
21. Conselho Regional de Medicina do Estado de São Paulo. CREMESP, Demografia Médica no Brasil, v. 2/Coordenação de Mário Scheffer; Equipe de pesquisa: Alex Cassenote, Aureliano Biancarelli. São Paulo: Conselho Regional de Medicina do Estado de São Paulo: Conselho Federal de Medicina, 2013.
22. Girardi S. Construção do índice de escassez de profissionais de saúde para apoio à Política Nacional de Promoção da Segurança Assistencial em Saúde. Estação de Pesquisa Sinais de Mercado. Núcleo de Saúde da Comunidade. (Internet) 2010; Available: https://www.nescon.medicina.ufmg.br/biblioteca/imagem/2443.pdf (Accessed 22 December 2015).
23. Instituto Brasileiro de Geografia e Estatística. Censo Demográfico 2010: Características Gerais dos Indígenas - Resultados do Universo (Internet) 2010. Available: http://biblioteca.ibge.gov.br/visualizacao/periodicos/95/cd_2010_indigenas_universo.pdf (Accessed 12 January 2016).
24. Price R. Maroon societies: rebel slave communities in the Americas. (Internet) 1979. Available: http://www.folklife.si.edu/resources/maroon/educational_guide/23.htm (Accessed 5 March 2016).
25. Ministério da Cultura. Quadro Geral de Comunidades remanescentes de quilombos (Internet) 2014. Available: http://www.palmares.gov.br/wp-content/uploads/crqs/lista-das-crqs-certificadas-ate-27-11-2014.pdf (Accessed 18 February 2015).
26. Oliveira SKM, Silveira JCS, Pereira MM, Freitas DA. Saúde em comunidade rural quilombola: relato de experiência sob o prisma dos atributos da atenção primária à saúde. Motricidade (Internet) 2012; 8(2): 83-88. Available: http://www.redalyc.org/articulo.oa?id=273023568011 (Accessed 8 January 2016).
27. Garnelo L. Política de Saúde Indígena no Brasil: notas sobre as tendências atuais do processo de implantação do subsistema de atenção à saúde. In: L Garnelo, Saúde Indígena: uma introdução ao tema. Brasilia: MEC-SECADI, 2012.
28. Ministério da Saúde. Portaria Ministerial n.º 1101/GM, de 12 de junho de 2002. Dispõe sobre os parâmetros de cobertura assistencial no âmbito do Sistema Único de Saúde - SUS. Brasilia: Diário Oficial da União, 13 July 2002; section 1:36.
29. Presidência da República. Medida Provisória nº 621, de 8 de julho de 2013 (a). Institui o 'Programa Mais Médicos' e dá outras providências. Brasilia: Diário Oficial da União, 9 July 2013; section 3.
30. Presidência da República. Lei nº 12.871, de 22 de outubro de 2013(b). Institui o Programa Mais Médicos, altera as Leis no 8.745, de 9 de dezembro de 1993, e no 6.932, de 7 de julho de 1981, e dá outras providências. (Internet) 2013. Available: http://www.planalto.gov.br/ccivil_03/_ato2011-2014/2013/Lei/L12871.htm (Accessed 2 January 2016).
31. Ministério da Saúde. Portaria Interministerial No 1.369, de 8 de Julho de 2013. Dispõe sobre a implementação do 'Projeto Mais Médicos para o Brasil. Brasilia: Diário Oficial União, 9 July 2013; section 1:49.
32. Portal da Saúde. Mais Médicos: 1.618 profissionais confirmam participação na primeira seleção do programa. (Internet) 2013. Available: http://portalsaude.saude.gov.br/index.php/cidadao/principal/agencia-saude/noticias-anteriores-agencia-saude/5297-mais-medicos-1-618-profissionais-confirmam-participacao-na-primeira-selecao-do-programa (Accessed 6 January 2016).
33. Supremo Tribunal Federal. Ação Direta de Inconstitucionalidade nº 5.035. (Internet) 2013. Available: http://www.stf.jus.br/portal/peticaoInicial/verPeticaoInicial.asp?base=ADIN&s1=m%E9dico&processo=5035 (Accessed 20 January 2016).
34. Ministério da Saúde. Edital No 22, de 31 de Março de 2014. Dispõe sobre a Adesão de municípios no Projeto Mais Médicos para o Brasil. Secretaria de Gestão do Trabalho e Educação em Saúde. Brasilia: Diário Oficial União, 1 April 2014; section 3:140.
35. Ministério da Saúde. Edital No 01, de 15 de Janeiro de 2015. Dispõe sobre a Adesão de municípios no Projeto Mais Médicos para o Brasil. Secretaria de Gestão do Trabalho e Educação em Saúde. Brasilia: Diário Oficial União, 16 January 2015; section 3:120.
36. Universidade Aberta do SUS. Mais Médicos; abertas inscrições de propostas para novos cursos de medicina. (Internet) 2015. Available: http://www.unasus.gov.br/noticia/mais-medicos-abertas-inscricoes-de-propostas-para-novos-cursos-de-medicina (Accessed 18 January 2016).
37. Ministério da Saúde. Sistema de Informação da Atenção à Saúde Indígena. Relatório de dados populacionais de 2013, por DSEI. Available: http://zip.net/bvqXhj (Accessed 27 January 2016).
38. Perpétuo IHO, Oliveira AC, Ribeiro MM, Rodrigues RB. A categoria profissional dos médicos: fatores condicionantes da sua atração e fixação na Atenção Primária à Saúde em Minas Gerais. (Internet) 2009. Available: https://www.nescon.medicina.ufmg.br/biblioteca/imagem/3065.pdf (Accessed 17 December 2015).
39. Costa AM, Girardi SN, Rocha VXM, Almeida ER, Santos LMP. Mais (e melhores) Médicos. Tempus, Actas de Saúde Coletiva (Internet) 2015; 9(4): 175-181. Available: http://tempus.unb.br/index.php/tempus/article/view/1810. (Accessed 5 March 2016).
