Telemedicine is the use of electronic information communication technologies to support health care in remote areas1. The remote exchange of data between a patient and healthcare professionals helps to facilitate the diagnosis and management of diseases and helps in monitoring and following up chronic health conditions. Previous research has supported the feasibility2, cost-effectiveness3,4, and usefulness of teleconsultations5. However, there is still a debate on the benefits and effectiveness of telemedicine applications in some disciplines and the evidence on the value of telemedicine in managing chronic diseases is contradictory5. Moreover, its effect on patients' perception using self reported measures such as quality of life, psychological outcomes, patient satisfaction, and acceptability of services is still unclear.
Compared to other telemedicine applications, telenephrology has been underutilized and under-researched. Little information is available on the impacts of telenephrology, particularly in low- and middle-income countries, and most of the research on telenephrology has originated in North America and Europe6. Telenephrology has been applied in different settings using different methods for different purposes such as interactive video to monitor patients undergoing hemodialysis7, email links with health facilities to send high-resolution digital images8, websites with technical support that allows a secure and fast exchange of medical data9, and videoconferencing providing nephrology services to remote communities10.
Previous research has shown a relatively high rate of late referrals of patients with kidney disease11. Poor access to specialized services and costly travelling have been reported as main reasons for discontinuation of follow-up care by patients10,11. Having timely access and referral to specialist nephrology services for patients with chronic kidney disease through the telenephrology is expected to result in better outcomes.
In rural and remote areas of Jordan, because of the scarcity of specialists most patients with kidney diseases are treated by general practitioners. Other patients need to travel to receive medical attention in tertiary hospitals in big cities like Amman, the capital city of Jordan. Because of geographic distance and costly travel, a telemedicine initiative was undertaken through the Jordan Healthcare Initiative to facilitate access to quality healthcare services for patients and clinicians from two remote hospitals in northern and southern regions in Jordan to specialists at a tertiary hospital in Amman. This study was conducted to assess the impact of live interactive telenephrology consultations on diagnosis and disease management and on patient quality of life and time- and cost savings.
Jordan Healthcare Initiative
Two teleclinics have been successfully implemented and are fully operational in two remote hospitals in Jordan: Mafraq Governmental Hospital in the north and Queen Rania Hospital in the south of Jordan. The two clinics connect patients from the north and south of Jordan with specialists at Prince Hamzah Hospital in Amman.
Study population and design
The study design and methods have been discussed in previous publications12,13. In brief, a pre-test-post-test one-group design was used to evaluate the process and outcomes of the teleconsultations that took place in the period between September 2013 and January 2014. This study focused on the evaluation of telenephrology and its impact. All consecutive patients who attended or were referred to the teleclinics for suspected kidney disease or for follow-up of chronic kidney disease in both hospitals during the study period were included in the study. For each patient, the physician or the nurse in the remote hospital filled the consultation request form and scheduled an appointment for the patient in the teleclinic within 1 week of the patient's first visit. On the day of the visit to the teleclinic, and at the end of consultation session, the study team (two nurses in each hospital) interviewed patients using face-to-face interview and filled all study questionnaires. The quality-of-life questionnaires were filled again 8 weeks after the last visit to the clinic using phone interview. The sample size that was needed to detect a medium effect size in the change of quality of life for patients with kidney disease after receiving the teleconsultation at a power of 80% and level of significance of 0.05 was calculated to be 53 subjects.
Data collection
Different aspects were assessed in the evaluation process. All questionnaires and forms used in this study were identified based on the review of the relevant studies. English questionnaires were translated into Arabic using a forward-backward translation method and were subsequently adapted to the Jordanian culture. The questionnaires were pilot tested on 10 patients and the necessary changes were made. All nurses were trained on data collection methods including phone interview and face-to-face interview, on ethical aspects of research conduct, and on all study procedures.
Consultation request form
This form was filled for each patient during the initial visit by the physician or the trained nurse in the remote hospitals and a copy was sent to the specialists in the main hospital by fax or email. The form included information for demographic purposes, the patient's chief complaint, disease or condition category, medical history, current medications, and provisional diagnosis and treatment plan. All necessary and available documents such as lab results that may have helped to diagnose, treat or follow up the patient were sent to the specialist.
Record form
This form was filled by the physicians or trained nurses in the remote hospitals at the end of the consultation. The record form included information about the final diagnosis and proper treatment plan as agreed upon by the physician and the specialist. A change in diagnosis was defined as whether the nephrologist's diagnosis was different from that of the referring physician's diagnosis at the completion of the initial consultation. A change in disease management was defined as whether the nephrologist's recommended treatment plan was different from that recommended by the referring physician.
Patient perception and satisfaction questionnaire
The questionnaire has been described elsewhere12,13. A structured questionnaire was filled using face-to-face interview at the end of the teleconsultation session to assess patient perception and satisfaction with the telemedicine application and determine its effect on the quality of care and health outcomes. The questionnaire, consisting of 15 items, was divided into different sections to give a complete picture of different domains including medical improvement, time- and cost savings, the telemedicine preparation, proper case management, and diagnosis and treatment. A Likert scale of five responses was used to rate the individual items in each domain, with higher scores indicating better satisfaction. The total satisfaction score was calculated by summing the responses of all individual items in the questionnaire and transforming to a score on a 0-100 scale, with higher scores indicating better satisfaction.
Quality-of-life questionnaires
One generic quality of life questionnaire (the Arabic version of the short form (SF8) questionnaire)14 and selected questions from the Kidney Disease Quality of Life survey (KDQOL) were used to assess quality of life15. The questionnaires were filled in the same day of the teleconsultation using face-to-face interview and the same questionnaires were filled 8 weeks later using phone interview, to assess the changes in quality of life as a result of teleconsultation.
The SF8 has been translated to more than 30 languages, and used in a number of countries with good reliability and validity14. The SF8 consists of eight items, each representing one health profile dimension: general health perception, physical functioning, role functioning-physical, bodily pain, vitality, social functioning, mental health, and role functioning-emotional. Each item of the SF8 was assessed using a 5- or 6-point Likert scale. Selected questions from the KDQOL that are relevant to patients with kidney disease (such as symptoms, burden of illness, social interaction, staff encouragement, and patient satisfaction) were chosen. Some items about general health, activity limits, ability to accomplish desired tasks, depression and anxiety, energy level, and social activities were not selected because they were already included in the SF8 questionnaire. Questions on sexual function were not selected for cultural reasons. The items in the questionnaire were grouped into three subscales. The Burden of Kidney Disease subscale included items about how much kidney disease interferes with daily life, takes up time, causes frustration, or makes the respondent feel like a burden. The Symptoms and Problems subscale included items about how bothered a respondent feels by itchy or dry skin, faintness/dizziness, and lack of appetite. The Effects of Kidney Disease on Daily Life subscale includes items about how bothered the respondent feels by fluid limits, diet restrictions, and stress or worries caused by kidney disease. Convergent and divergent validity and reliability of the KDQOL subscales have been established and confirmed in different studies16.
Each item of the SF8 and KDQOL was scored on a 0-100 range and the domains and total scores were then calculated. The lowest and highest possible scores were 0 and 100, respectively, with high scores defining a more favorable health state and better quality of life. The psychometric properties for both questionnaires were studied in this study using the pre-test data. Cronbach alpha coefficient for the SF8 questionnaire was 0.92, indicating high internal consistency. The correlations between each item in the SF8 questionnaire and its hypothesized scale exceeded the criterion of 0.40. For all subscales of KDQOL, Cronbach alpha coefficients exceeded the minimum criterion of 0.70 and ranged from 0.73 to 0.92, indicating high internal consistency.
Statistical analysis
Data were described and analyzed using the Statistical Package for the Social Sciences v20 (IBM; http://www.spss.com). Data were described using means, standard deviations, or percentages wherever appropriate. Improvement in quality of life after telemedicine application compared to the baseline was analyzed using paired t-test. A p-value of less than 0.05 was considered statistically significant.
Ethics approval
Ethical approval was obtained from the institutional review board at Jordan University of Science and Technology, approval number 20130228. Written informed consent was obtained from all participants.
Patient characteristics
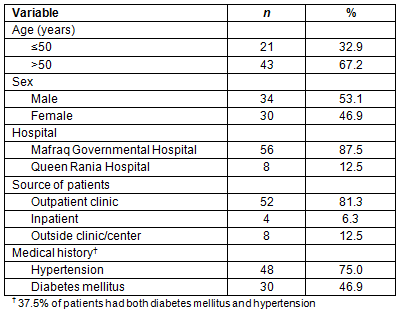
A total of 71 patients were eligible to be included in the study. Of those, 64 (90.1%) patients (34 males and 30 females) agreed to participate in the study and were included in this study. Table 1 shows demographic and clinical characteristics. The age of patients ranged from 16 to 90 years with a mean of 54.1 years (standard deviation (SD) 19.0 years) year. Less than one-third of patients (30.3%) were younger than 45 years. The majority (87.5%) of telenephrology consultations were done at Mafraq Governmental Hospital. About 75% of patients were referred from the outpatient clinics in the same hospitals. About 75.0% of patients had hypertension, 46.9% had diabetes mellitus, and 37.5% of patients had both diabetes mellitus and hypertension.
Table 1: Characteristics of patients who attended telenephrology clinics in two Jordanian hospitals, September 2013 - January 2014
Impact of telenephrology consultations on diagnosis and treatment plan
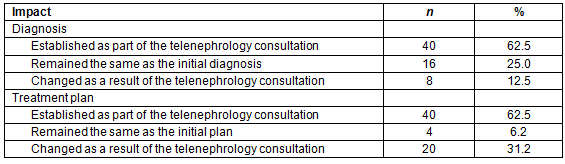
Establishing or helping in diagnosis or treatment plan was the main reason for teleconsultations in all patients. As perceived by the referring providers, final diagnosis was established as part of the telenephrology consultations in 62.5% of patients and changed from that of the referring provider in 12.5% of patients (Table 2). The treatment plan changed from that of the referring provider for 31.2% of patients. The referring providers perceived that the communication with the specialist helped them to reach the diagnosis and the treatment plan in all consultations.
Table 2: Impact of telenephrology consultations on changes in diagnosis and treatment plan according to the perceptions of referring providers
Patient perception of the time- and cost saving and their satisfaction
If the telenephrology clinic were not an option, patients perceived that they would take 21.0 hours for each potential visit to the specialist clinic. About 28% of patients stated that they needed to take a day off from work to visit the specialist clinic. On average, patients perceived that the cost would be 73.0 JD (1 US$ = 0.71 JD) per visit if they needed to visit the specialist clinic and receive care at the main hospital in Amman.
All patients perceived that their visit to the telenephrology clinics needed less travel time when compared to visiting the specialist clinic in the referral hospital. The vast majority of patients stated that their visits to teleclinics were associated with less waiting time and lower cost (96.9% and 98.4%, respectively) when compared to their previous visits to the specialist clinics in the referral hospital. The waiting time ranged from 1 to 90 minutes with a mean (SD) of 26.2 (16.6) minutes. The teleconsultation times ranged from 5 minutes to 75 minutes with a mean of 17.8 (10.5) minutes.
While none of the patients perceived that it was easy to access the specialist clinic in Amman, all patients stated that it was easy to access the telenephrology clinic. When patients were asked about what they would do if the telenephrology were not available, 85.9% reported that they would travel to see the specialist and the rest (14.1%) reported that they would see the general practitioner in the same hospital. The total satisfaction score of patients with the services received ranged from 71.2 to 100 with a mean (SD) of 96.8 (4.8), indicating a high level of satisfaction.
Impact of telenephrology consultations on quality of life
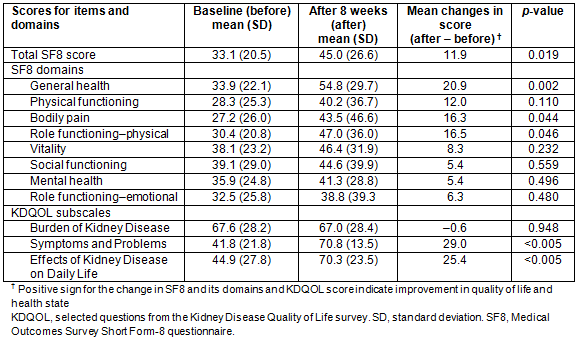
Table 3 shows the changes in the quality of life after 2 months of telenephrology consultations. After 2 months of consultations, the mean SF8 score increased significantly from 33.1 to 45.0 (p<0.019), which implies that the telenephrology consultations might result in an overall improvement in quality of life and in a more favorable health state. Of the eight individual domains of SF8, only the general health, bodily pain, and role functioning-physical items had improved significantly after 2 months of telenephrology consultations. Of the three subscales of KDQOL, there were significant increases in the scores of Symptoms and Problems subscale and Effects of Kidney Disease on Daily Life subscale. This means that, as a result of teleconsultations, patients were less bothered by itchy or dry skin, faintness/dizziness, and lack of appetite, and less bothered by fluid limits, diet restrictions, and stress or worries caused by kidney disease. However, there was no significant improvement in the Burden of Kidney Disease subscale.
Table 3: Changes in quality of life among patients after 2 months of telenephrology consultations, as measured by the SF8 questionnaire and its domains and KDQOL
Discussion
People in the remote and rural areas of Jordan don't have timely access to specialized nephrology services because of shortages in the number of nephrologists and concentration of these specialists in big cities. Therefore, many patients in these areas need to travel long distances to reach specialized services in tertiary hospitals in Amman. For the two areas in the present study (Mafraq and Wadi Mousa), the travel distances were more than 100 km. For most cases in any specialty, patients wait 30-45 days for an appointment to see the specialist. Telemedicine is one option to improve access to these services and it can offer a cost-effective, time-efficient means of expanding health care coverage to underserved areas2-5. Previous evaluations of telemedicine applications in Jordan showed that telecardiology and teledermatology would improve access to health care, help to reach proper diagnosis and establish a treatment plan, and improve quality of life12,13. The present study evaluated telemedicine application in nephrology.
The study showed that all patients perceived that their visit to the telenephrology clinics needed less travel time. The vast majority of patients stated that their visits to teleclinics were associated with less waiting time and lower cost (96.9% and 98.4%, respectively) compared to what happens if they visit nephrologists in Amman. Moreover, costly travels might be avoided because all patients included in this study were managed locally, without any need to refer them to hospitals in Amman.
About 14.1% of patients stated that they would visit a general practitioner if telemedicine was not available. This option has implications for diagnosis and treatment since the study showed that final diagnosis and treatment plan changed from that of the referring provider in 12.5% and 31.2% of patients, respectively. Therefore, it is expected that the diagnosis and the treatment plan will be less likely to be appropriately established for these 14% who would not have attended the specialist center.
Overall, patient quality of life improved significantly after 2 months of telenephrology consultations as measured by SF8. Specifically, only aspects of quality of life related to the general health, bodily pain and role functioning-physical items improved significantly. Some aspects of the quality of life such as social functioning, mental health, and role functioning-emotional items showed no significant improvement. It seems that teleconsultations resulted in an improvement in physical component of quality of life but not in emotional quality of life. It is worth mentioning that the general health, bodily pain and role functioning-physical domains belong to a physical component and social functioning, mental health, and role functioning-emotional domains belong to mental components according the procedures recommended by the developers17,18. The improvement in physical, but not emotional, quality of life might be explained by the fact that the emotional quality of life might need a longer time to improve and the 2 months of follow-up were not enough for the changes to occur. A study assessing long-term impact of teleconsultations is needed to capture the impact on emotional health.
Moreover, the quality of life measured by KDQOL showed that patients were less bothered by the disease symptoms (Symptoms and Problems subscale) and by restrictions on daily activities (Effects of Kidney Disease on Daily Life subscale) after teleconsultations. However, there was no improvement in the Burden of Kidney Disease subscale, which measures how much kidney disease interferes with daily life, and makes the respondent feel like a burden. Similarly, the short period of evaluation did not give an opportunity to detect the impact of teleconsultations on the burden of kidney disease. The finding of positive impact of teleconsultations on quality of life is consistent with the findings of other studies that have examined the effect of telemedicine on health-related quality of life in patients with different health problems and showed that telemedicine is beneficial19,20. However, the changes in the quality of life after telenephrology application might be for other reasons. A large randomized clinical trial is recommended to provide better evidence.
This study was not intended to compare telenephrology to in-person nephrology care because telenephrology may still be superior to nephrology care provided by non-specialists. One of the main limitations in this study is inherited in the design itself. In this design patients were not compared to a control group or a group who was not treated by telenephrology.
Telenephrology care in remote areas of Jordan would improve access to health care, help physicians to reach a proper diagnosis and establish a treatment plan, and improve quality of life. If expanded to remote and rural areas in Jordan, telenephrology is expected to improve the care and the outcomes for patients with kidney problems. A study with a comparison group of patients who used the in-person nephrology care would provide stronger evidence on the effectiveness of telenephrology care.
Acknowledgements
The research was supported by Cisco Systems, Inc., USA. The funder had no role in the study design, data collection and analysis, interpretation of data, decision to publish, or preparation of the manuscript.
References
1. Institute of Medicine, Committee on Evaluating Clinical Applications of Telemedicine. Telemedicine: a guide to assessing telecommunications in health care. Washington, DC: National Academy Press, 1996.
2. Scalvini S, Tridico C, Glisenti F, Giordano A, Pirini S, Peduzzi P, et al. The SUMMA Project: a feasibility study on telemedicine in selected Italian areas. Telemedicine Journal and e-Health 2009, 15(3): 1-9.
3. Whitten PS, Mair FS, Haycox A, May CR, Williams TL, Hellmich S. Systematic review of cost effectiveness studies of telemedicine interventions. British Medical Journal 2002; 324(7351): 1434-1437.
4. Larsen F, Gjerdrum E, Obstfelder A, Lundvoll L. Implementing telemedicine services in northern Norway: barriers and facilitators. Journal of Telemedicine and Telecare 2003; 9(S1): 17-18.
5. Wootton R. Twenty years of telemedicine in chronic disease management - an evidence synthesis. Journal of Telemedicine and Telecare 2012; 18(4): 211-220.
6. Blinkhorn TM. Telehealth in nephrology health care: a review. Renal Society of Australasia Journal 2012; 8(3): 132-139.
7. Moncrief JW. Telemedicine in the care of the end-stage renal disease patient. Advances in Renal Replacement Therapy 1998; 5(4): 286-291.
8. Graham LE, Zimmerman M, Vassallo DJ, Patterson V, Swinfen P, Swinfen R, Wootton R. Telemedicine - the way ahead for medicine in the developing world. Tropical Doctor 2003; 33(1): 36-38.
9. Alamartine E, Thibaudin D, Maillard N, Sauron C, Mehdi M, Broyet C, et al. Telemedicine: an unfruitful experience of tele-expertise in nephrology. Presse Medicale 2010; 39(5): e112-116.
10. Campbell M, Akbari A, Amos S, Keyes C. Feasibility of providing nephrology services to remote communities with videoconferencing. Journal of Telemedicine and Telecare 2012; 18(1): 13-16.
11. Jungers P, Joly D, Nguyen-Khoa T, Mothu N, Bassilios N, Grünfeld JP. Continued late referral of patients with chronic kidney disease. Causes, consequences, and approaches to improvement. Presse Medicale 2006; 35(1 Pt 1): 17-22.
12. Al Quran HA, Khader YS, Ellauzi ZM, Shdaifat A. Effect of real-time teledermatology on diagnosis, treatment and clinical improvement. Journal of Telemedicine and Telecare 2015; 21(2): 93-99.
13. Khader YS, Jarrah MI, Al-Shudifat AE, Shdaifat A, Aljanabi H, Al-Fakeh SI, et al. Telecardiology application in Jordan: its impact on diagnosis and disease management, patients' quality of life, and time- and cost-savings. International Journal of Telemedicine and Applications 2014; 2014: 819-837.
14. Ware J, Kosinski M, Dewey J, Gandek B. How to score and interpret single-item health status measures: a manual for users of the SF-8 Health Survey. Lincoln, RI: Quality Metric, 2001.
15. Hays RD, Kallich JD, Mapes DL, Coons SJ, Carter WB. Development of the kidney disease quality of life (KDQOL) instrument. Quality of Life Research 1994; 3(5): 329-338
16. Kalantar-Zadeh K, Unruh M. Health related quality of life in patients with chronic kidney disease. International Urology and Nephrology 2005; 37: 367-378.
17. Ware J, Kosinski M, Bayliss M, McHorney CA, Rogers WH, Raczek A. Comparison of methods for the scoring and statistical analysis of SF-36 health profile and summary measures: summary of results from the medical outcomes study. Medical Care 1995; 33(Suppl 4): 264-279.
18. Ware J, Kosinski M, Keller S. SF-36 Physical and Mental Summary Scales: a user's manual. Boston, MA: The Health Institute, New England Medical Center, 1994.
19. Clark RA, Inglis SC, McAlister FA, Cleland JGF, Stewart S. Telemonitoring or structured telephone support programmes for patients with chronic heart failure: systematic review and meta-analysis. British Medical Journal 2007; 334: 942-945.
20. Inglis SC, Clark RA, McAlister FA, Ball J, Lewinter C, Cullington D, et al. Structured telephone support or telemonitoring programmes for patients with chronic heart failure. The Cochrane Database of Systematic Reviews 2010: CD007228.
