Problems of recruitment and retention of health care professionals
Many westernised countries face ongoing difficulties in the recruitment and retention of adequate numbers of health professionals in remote and rural communities1,2. In the UK, the general shortage of doctors3 and nurses4 is exacerbated by fewer medical graduates entering general practice: 'the key discipline of rural health care'5. The proportion of women in the medical workforce (especially general practice), is increasing6, and there is a move among male as well as female professionals towards part-time work7. The traditional model of rural healthcare, provided by relatively few professionals working long hours, is changing because of: the introduction of new models of out-of-hours care; restrictions on working hours imposed by the European Working Time Directive, and by the demands of the professionals themselves for the clearer personal/professional delineation now enjoyed by their urban counterparts8. While new models evolve, there is insecurity among healthcare professionals about committing to rural work, which is likely to further exacerbate recruitment and retention difficulties. Given the growing challenge of adequately staffing UK rural health services, it is important to understand the characteristics of the present workforce, its stability, and opportunities and threats to rural recruitment and retention.
International perspective
International research has been partially successful in characterising the rural healthcare workforce. Retrospective surveys from Australia and north America have suggested that the most important predictors of recruitment of health professionals to rural areas are the individual having been born or educated in a rural location9,10 and exposure to rural healthcare during training11.
More recently, research considering retention has identified a range of professional and personal reasons for remaining in a rural area, such as access to continuing professional education, and good relationships with peers12 and patients13. Personal reasons include: partner having a rural background and 'spousal contentedness'14,15; adoption of a rural 'lifestyle'; successful integration into local communities16; and educational opportunities for children13.
Scotland
A Scottish consultation exercise suggested these internationally accepted determinants of recruitment and retention apply in Scotland, but this has not been verified by empirical research. The general lack of research into Scottish rural healthcare17 may reflect the comparatively small scale of Scotland's remoteness, the relatively recent recruitment and retention crisis, or a perception among centrally-based policymakers and politicians that rural areas are of low priority.
We were interested to explore the extent to which themes around rural working, demonstrated in the international literature, also apply in areas of the UK. This was achieved by carrying out a survey of primary healthcare professionals in the Scottish Highlands, the most sparsely populated area of the UK (Fig 1).
Figure 1: Map showing Highland in relation to the United Kingdom.
Methods
Setting
The Scottish Highlands was self-selected for the study because the survey was commissioned by the Highland Primary Care Trust, the administrative organisation for primary healthcare in the north of Scotland at the time of this study. The Highlands makes up one-third of Scotland's land area (9800 square miles) and has just 4% of the country's population (209 000). Approximately one-quarter of the population (42 000) live in Inverness. The area is ideal for investigating the rural workforce due to its population sparsity and the inclusion of small towns and Inverness, allowing urban/rural comparisons.
Sample
Following ethical approval, a postal survey was conducted between May and July 2003 of all 2070 primary healthcare health professionals working in Highland health board area. The sample included full- and part-time staff: 1764 employed by Highland Primary Care Trust (community-based nurses; midwives; allied health professionals, such as physiotherapists; mental health professionals; and doctors); 224 professionals employed directly in general practice (general practitioners and practice-based nurses); and 82 dental professionals (dentists and dental nurses). Trust employees were mailed via the payroll department of the Trust, and general practice professionals were mailed directly from Highlands and Islands Health Research Institute (HIHRI). Anonymised questionnaires were returned to HIHRI.
The questionnaire
The questionnaire (Appendix I), explored themes identified from the literature as being related to recruitment and retention (place of birth and education; intentions to stay/leave their current location; professional isolation; access to amenities; and perceptions of belonging to the local community). The questionnaire was piloted in a neighbouring Primary Care Trust area. One reminder mailing was carried out.
Analysis
Data were entered into Access 2000 software and analysed using Stata vers.8.0. The main independent variables were 'living location' and 'working location'; each classified into three categories based on those defined by the Scottish Household Survey Classification18: 'urban areas', with populations between 10 000 and 125 000; 'small towns' (3 000 to 10 000) and 'rural areas' (<3000). Population sizes were ascertained using 2001 Scottish census data. By this classification, the only 'urban area' in Highland is Inverness. These six categories were then simplified for analysis into three 'location types': working and living in Inverness or a small town (for the purposes of this study, referred to as 'urban'); working in Inverness or a small town but living in a rural area (commuters); and, working in a rural area and living anywhere (rural). Results are presented as percentages. Chi-square tests were used to assess the statistical significance of differences between groups in the frequency distribution of categorical variables, unless the expected cell size was less than five, when Fisher's exact test was used.
Results
Response rates
Of the 2070 questionnaires sent, 40 were excluded because the person was no longer employed in Highland. Of the remaining 2030 questionnaires, 1077 were returned complete (53%). The response rates for the four mailing groups were as follows: Trust employees (of whom the majority are nurses and professionals allied to medicine), 57%; practice nurses, 50%; GPs, 57%; and dentists, 40%. The proportions of respondents in the four main professional groups were as follows: nursing 54% (including practice nurses, district nurses, midwives and health visitors); medical 17.6% (including general practitioners and community-based doctors); allied health professions 14.4%; dentistry 4.3% (including dentists and dental nurses).
Analyses involving comparisons among location types include only those 1050 respondents (52% of total) whose place of residence and work-place could be classified according to their population sizes (Table 1). Thirty-eight per cent of respondents worked and lived in Inverness or a small town; 25% were 'commuters' (work in Inverness/small town and live in a rural area), and the remaining 37% worked in 'rural' areas. Of those working in a rural area, 18% travelled from Inverness or a small town.
Table 1: Demographic characteristics by location type
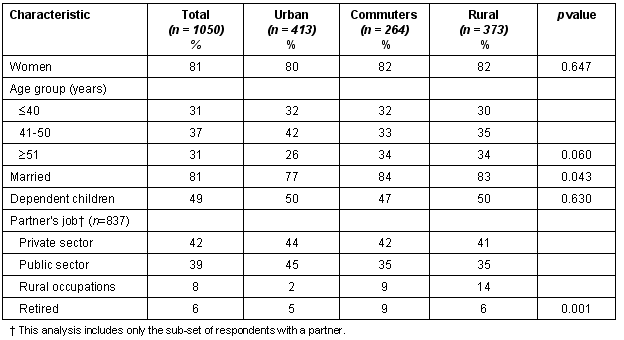
Eighty-one percent of respondents were women (93% of nurses, 52% of doctors; 33% of dentists and dental nurses; and 91% of professionals allied to medicine). One third of respondents were over 50 years, with a higher proportion of older respondents living in rural areas. Eighty-one percent were married (again, higher for those living in rural areas), and half had at least one dependent child. Of those living in rural areas, partners or spouses were more likely to have rural occupations such as crofting and estate work, and more likely to be retired than partners of urban dwellers.
Ninety-nine per cent of respondents gave their ethnic group as 'white', with two-thirds born in Scotland, and one-quarter in England or Wales (Table 2). Three-quarters completed their secondary education in Scotland, one-fifth in England or Wales and the remainder elsewhere; and those proportions were similar for place of professional training. Compared with the other professional groups, nurses were more likely to have been born (p = 0.00), educated (p = 0.00) and trained (p = 0.00) in Scotland. Professionals living in rural areas were more likely to have been born outside Scotland and to have completed their secondary education and professional training outside Scotland, compared with those living in Inverness or small towns.
Table 2: Rural background by location type
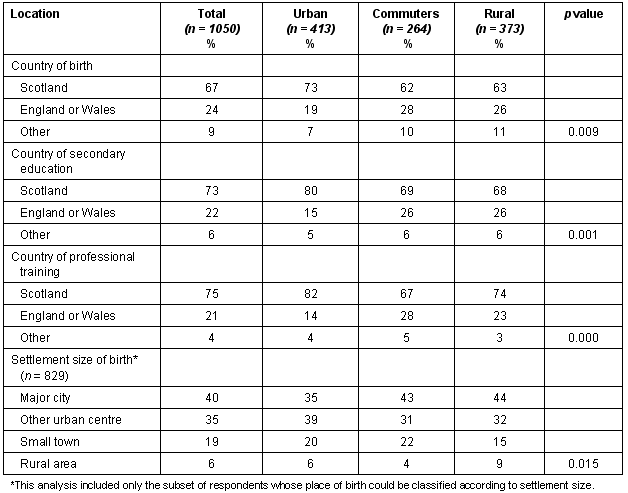
Of the 829 respondents with a birth-place that could be classified according to settlement size, three-quarters were born in major cities or other urban centres (with no difference between our three location types); 19% in small towns, and 6% in rural areas. However, compared with respondents working in Inverness/small towns, those working in rural areas were more likely to have been born in rural areas, and less likely to have been born in small towns. Of the 53 respondents who were born in a rural area, 47% currently work in a rural area. Compared with dentists (15%) and doctors (12%), a higher proportion of nurses (30%) and professionals allied to medicine (24%) were born in rural areas or small towns (p = 0.00).
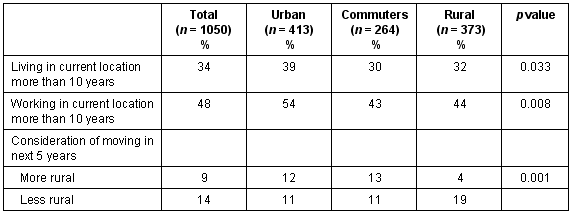
Approximately one-third (34%) had lived in their current location for more than 10 years and that proportion was higher for the urban group compared with rural dwellers (Table 3). Similarly, the urban dwellers were more likely to have been in their current job for more than 10 years. One-quarter said that they would consider moving from their current location within the next 5 years, with no difference between location types. Eighty-two per cent of those working in a rural area who had considered moving, said they would like to move to a less rural area, compared with 46% of commuters.
Table 3: Stability of the workforce
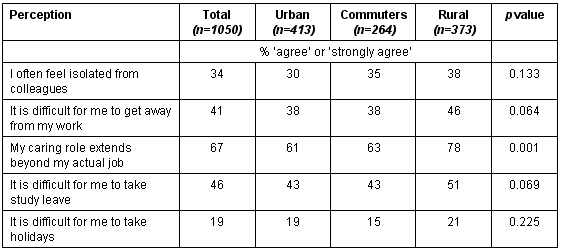
Respondents were asked to indicate the extent to which they agreed with five statements relating to professional isolation and work pressure (Table 4). Isolation, an extended caring role and a perceived inability to get away from work for holidays and study leave were surprisingly common in urban as well as rural workers. For each of five statements, those who both lived and worked in rural areas perceived greater difficulty than those in other location types. When we compared the perceived isolation of the different professional groups, we found that although the doctors were most likely to perceive that their caring role extended beyond their work (p = 0.00), professional allied to medicine were most likely to feel professionally isolated and to encounter difficulties getting away for study leave.
Respondents were also asked to state whether they felt part of the community they live in. Eighty-one per cent said that they did; 19% said 'no' or 'not sure'. The proportion that felt part of the community was higher for those working in rural areas (86%) than for urban residents (81%). The group stating that they feel least part of the community was the commuters (75%), p = 0.00.
Table 4: Perceptions of jobs and locations: professional isolation
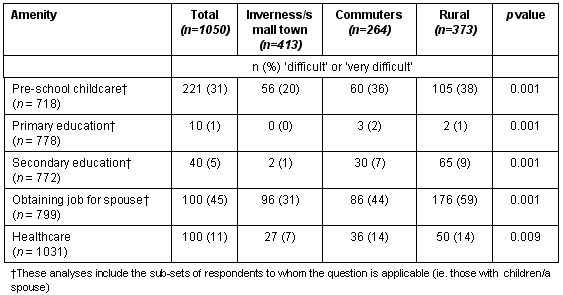
Respondents indicated their perceived ease of access to five amenities and services: children's education (preschool, primary and secondary); access to a job for spouse; and health care (Table 5). The amenities that were most difficult to reach were preschool care and spouse's job. With the one exception of access to primary education, access was perceived to be most difficult by the professionals working in rural areas. In general, commuters perceived similar problems of reaching services to those working in rural areas. There was no relationship between difficulty accessing amenities and intention to leave an area within the following 5 years, except for accessing health care (16% of those who perceived problems accessing health care had considered moving, compared with 10% of those who did not perceive problems).
Table 5: Access to amenities
Discussion
Rural background as a predictor of rural working
Rural background was a predictor of rural working for participants in this survey of the Scottish Highlands. This finding agrees with the international literature which has consistently shown a positive association between rural origins and rural working. For general practice19,20 and nursing21, it has been suggested that rural origins should be taken into account when selecting students for training. The other element of 'rural background' which is positively associated with rural working, is educational exposure to rural issues9,22 and rural educational programs have been established in Australia and North America11 to boost the rural workforce. In the UK, the few existing rural educational placements have been instigated relatively recently23 and exposure to rural matters depends heavily on the personal enthusiasms and initiatives of practitioners. We therefore did not explore educational exposure.
In the present study, rural workers were more likely to have been born and educated outside Scotland, compared with those working in towns. The apparent bolstering of the rural workforce by professionals from other regions has not been described previously and may be specific to the UK. In contrast with North America and Australia, whose rural areas are relatively deprived24, rural areas of the UK, especially Scotland, are widely perceived to offer a high quality of life and a chance to escape from 'the rat-race'. In Highland, for example, 14% of the population were born in England and Wales compared with 8% in Scotland as a whole. Nurses and professionals allied to medicine were more likely to be born in rural areas than doctors and dentists which may reflect that they are more likely to be local to Highland.
Professional isolation and access to amenities
Respondents working in rural areas perceive themselves to be more isolated and to have poorer access to services and amenities than those in Inverness and small towns. Professional isolation, lack of opportunity for professional development and poor access to basic amenities are important barriers to recruiting and retaining health professionals in rural areas25. As expected, a perception that the caring role extended beyond actual work was commonest among the doctors. Somewhat surprisingly, professionals allied to medicine were more likely than other groups to feel professionally isolated: this may reflect the fact that in rural areas, there is likely to be just one representative of each allied profession (eg physiotherapy, occupational therapy). Although our survey was not designed to test the causal relationship between these factors and recruitment and retention, we have shown that they are disproportionately problematic for professionals working in rural areas. Perceived difficulty accessing amenities did not predict intention to leave an area, suggesting that access is just one of a number of factors contributing to that decision.
Adoption of a rural lifestyle
Adoption of rural lifestyle and integration into the community are associated with retention of healthcare professionals in rural areas16 and in Australia, communities have been actively involved in the recruitment process26. Most of our respondents said that they felt part of their community, commuters less so than either urban- or rural-dwellers. Our failure to demonstrate a rural/urban difference might reflect that although Inverness is officially a city (since 2001), it is relatively small and shares some features of rural areas, such as easy access to rural leisure pursuits and long drive times to major urban centres.
Stability of workforce
The Highland primary care workforce is stable: half the respondents have been at their current workplace for more than 10 years. However, compared with Inverness, rural workers had been at their current location for a shorter time, suggesting a relatively rapid turnover in rural areas. In addition, the relatively old age of professional in Highland (30% over 50 years) means that increasing numbers of the workforce will retire over the next decade. At the same time, aging of the general population of rural areas of Scotland an increasing dependency ratios (scoping study) will put added pressure on health services.
The perspective of female professionals
Most previous research into recruitment and retention of rural health professionals has focussed on doctors, who are predominantly male14. A recent Scottish study showed that female medical students are, in principle, keen to work in rural areas21 and given the increasing 'feminisation' of the medical workforce6,27, it is particularly important to consider the issues facing female professionals in rural areas. Studies that have looked at the perspective of female professionals suggest that, although women are equally concerned about professional issues28,29 their decision to stay in a rural area is strongly influenced by family considerations, the option of flexible working, and the availability of childcare30. The negative aspects of rural working demonstrated by our survey, such as poor access to childcare and isolation, will arguably disproportionately affect women, who are still expected to assume the greater role in childcare.
Study's strengths and limitations
Our survey has the main advantage over previous research that it includes all professional groups, rather than focusing only on doctors. The study has limitations. First, in order to maximise the response rate, we chose to keep the questionnaire short and therefore some complex issues, such as community-belonging are only superficially explored. Second, because of the need for anonymity we have no information about the non-responders (except whether they are an employee of the Primary Care Trust, a GP, a dentist or a Practice Nurse) and we cannot guarantee that our respondent-group is representative of the sample. Third, there are some inherent problems of defining rural and urban. Here, we classified Inverness as 'urban' because it is the only major centre of population in Highland (our study area). However, Inverness is a small city lacking in some features typical of larger cities, such as significant areas of social deprivation and therefore contrasts with our 'rural' areas may be tenuous. In addition, differences in classification systems make international comparisons difficult - according to the Commonwealth of Australia's rural classification, Inverness would be classified as a large rural centre, rather than an urban area.
Policy implications
Our survey confirms, in the UK, the association between rural background and rural working and highlights the contribution of healthcare professionals from other parts of the UK to the Scottish rural workforce. It also suggests the importance of isolation and lack of access to amenities for those working in rural areas.
Recent Scottish policy documents emphasise the importance of equity of access31 as well as the challenges of providing healthcare in remote and rural areas. If policy makers are interested in addressing the shortage of health professionals in rural areas, we suggest that the following strategies could be considered. First, rural origins could be taken into account when selecting individuals to train for the health professions, especially in the educational institutions that supply a large proportion of professionals to rural areas. Second, active recruitment initiatives should extend to England and Wales. Third, innovative solutions to reducing professional isolation and easing access to educational opportunities, such as greater use of information technology and expansion of distance learning programs should be encouraged. Fourth, policy makers should be aware that the predominance of women in the rural workforce will mean that for many, access to amenities and services will be important.
Conclusion
Our survey has been successful in providing a snapshot of the workforce in one rural area of Scotland. If repeated in 5 years time, it would be possible to monitor temporal trends and to test some of the hypotheses generated.
Acknowledgements
The authors thank the health professionals for completing the questionnaires. We are grateful to Highland Primary Care Trust for funding the study and to Ken Proctor for his advice. We would also like to thank Fiona Ryan for her careful data entry and David Godden for his helpful comments on the manuscript.
References
1. James R, Dowell A, Cormack D. New Zealand rural general practitioners 1999 survey - part 1: an overview of the rural doctor workforce and their concerns. New Zealand Medical Journal 2001; 114: 492-495.
2. Rourke J, Newbery P, Topps D. Training an adequate number of rural family physicians. Canadian Family Physician 2000; 46: 1245.
3. Sibbald B, Bojke C, Gravelle H. National survey of job satisfaction and retirement intentions among general practitioners in England. BMJ 2003; 326: 22-26.
4. Finlayson B, Dixon J, Meadows S, Blair G. Mind the gap: the extent of the NHS nursing shortage. BMJ 2002; 325: 538-541.
5. Talley RC. Graduate medical education and rural health care. Academic Medicine 1990; 65(12): S22-S25.
6. Denekens JP. The impact of feminisation on general practice. Acta Clinica Belgica 2002; 57: 5-10.
7. French F, Needham G, Walker K, Scott A. Towards a flexible workforce - a basis for change. Aberdeen: NHS Scotland, 2003.
8. Farmer J, Lauder W, Richards HM, Sharkey S. Dr John has gone: assessing health professionals' contribution to remote rural community sustainability. Social Sciences in Medicine 2003; 57: 673-686.
9. Rabinowitz HK, Diamond JJ, Hojat M, Hazelwood CE. Demographic, educational and economic factors related to recruitment and retention of physicians in rural Pennsylvania. Journal of Rural Health 1999; 15: 212-218.
10. Brooks RG, Walsh M, Mardon RE, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: a review of the literature. Academic Medicine 2002; 77: 790-798.
11. Dunabin J, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. Rural and Remote Health 3: 212. (Online) 2003. Available: http://rrh.org.au/ (Accessed 28 February 2005).
12. Huntley B. Factors influencing recruitment and retention: why RNs work in rural and remote area hospitals. Australian Journal of Advanced Nursing 1994; 12: 14-19.
13. Scammon DL, Williams SD. Understanding physicians' decisions to practice in rural areas as a basis for developing recruitment and retention strategies. Journal of Ambulatory Care Marketing 1994; 5: 85-100.
14. Sempowski IP, Godwin M, Seguin R. Physicians who stay versus physicians who go: results of a cross-sectional survey of Ontario rural physicians. Canadian Journal of Rural Medicine 2002; 7: 173-179.
15. MacPhee M, Scott J. The role of social support networks for rural hospital nurses: supporting and sustaining the rural nursing workforce. Journal of Nursing Administration 2002; 32: 264-272.
16. Cutchin MP. Physician retention in rural communities: the perspective of experiential place integration. Health and Place 1997; 3: 25-41.
17. Godden DJ, Richards HM. Health research in remote and rural Scotland: what is out there? Scottish Medical Journal 2003; 48: 10-12.
18. Scottish Executive Environment and Rural Development Department. Living In Scotland: an Urban-Rural Analysis of the Scottish Household survey. Edinburgh: Scottish Executive, 2003.
19. Blackman JR. Pre-doctoral education for rural practice. In: JP Geyman, TE Norris, LG Hart (Eds). Textbook of Rural Medicine. New York: McGraw-Hill, 2001; 359-367.
20. Hegney D, McCarthy A, Rogers-Clark C, Gorman D. Why nurses are attracted to rural and remote practice. Australian Journal of Rural Health 2002; 10: 178-186.
21. Laven GA, Beilby JJ, Wilkinson D, McElroy HJ. Factors associated with rural practice among Australian trained general practitioners. Medical Journal of Australia 2003; 179: 75-79.
22. Wilkinson D, Laven G, Pratt N, Beilby J. Impact of undergraduate and postgraduate rural training, and medical school entry criteria on rural practice among Australian general practitioners: national study of 2414 doctors. Medical Education 2003; 37: 809.
23. Farmer J, Iverson L, Bond C, Duthie I. Medical students' orientation towards rural general practice: results from an exploratory study of a Scottish cohort. Education for Primary Care 2003; 14: 463-467.
24. Rosenblatt RA. The health of rural people and the communities and environments in which they live. In: JP Geyman, TE Norris, LG Hart (Eds). Textbook of rural medicine. New York: McGraw-Hill, 2000; 1-3.
25. Hays R, Wynd S, Veitch C, Crossland L. Getting the balance right? GPs who chose to stay in rural practice. Australian Journal of Rural Health 2003; 11: 193-198.
26. Veitch C, Harte J, Hays R, Pashen D, Clark S. Community participation in the recruitment and retention of rural doctors: methodological and logistical considerations. Australian Journal of Rural Health 1999; 7: 206-211.
27. Roberts JH. The feminisation of medicine. BMJ Career Focus 2005; 330: 13-15.
28. Wainer J, Bryant L, Strasser R. Sustainable rural practice for female general practitioners. Australian Journal of Rural Health 2001; 9(1): S43-S48.
29. Elley R. Women in rural general practice: the stresses and rewards. New Zealand Medical Journal 2001; 114: 358-360.
30. Ellsbury KE, Baldwin LM, Johnson KE, Runyan SJH. Gender-related factors in the recruitment of physicians in the rural Northwest. Journal of the American Board of Family Practice 2002; 15: 391-400.
31. Scottish Executive. Availability of Services in Rural Scotland. Edinburgh: Scottish Executive; 2002.
Abstract
Introduction: Many westernised countries face ongoing difficulties in the recruitment and retention of health professionals in remote and rural communities. Predictors of rural working have been identified by the international literature, and include: the individual having been born or educated in a rural location; exposure to rural healthcare during training; access to continuing professional education; good relationships with peers; spousal contentedness; adoption of a rural 'lifestyle'; successful integration into local communities; and educational opportunities for children. However, those themes remain unverified in the UK.
The present study aimed to ascertain whether the internationally identified determinants of recruitment and retention of the rural health workforce apply in the Highlands of Scotland, which includes the most sparsely populated area of the UK mainland, as well as an urban area.
Methods: In 2003, a questionnaire was sent to all 2070 primary healthcare professionals working in the Highlands (which makes up one-third of Scotland's land area (9800 square miles) and has just 4% of the country's population (209 000)). Approximately one-quarter of the Highland's population live in Inverness. The area is ideal for investigating the rural workforce due to its population sparsity and the inclusion of small towns and Inverness, allowing urban/rural comparisons. The questionnaire asked about places of birth and education; intentions to stay/leave current location; professional isolation; access to amenities; and perceptions of belonging to the local community.
Results: The response rate was 53%. Compared with respondents working in urban areas, those working in rural areas were more likely to have been born in rural areas. Professionals living in rural areas were more likely to have been born outside Scotland and to have completed their secondary education and professional training outside Scotland, compared with those living in urban areas. Approximately one-third (34%) had lived in their current location for more than 10 years, and that proportion was higher for the urban group compared with rural dwellers. Similarly, the urban dwellers were more likely to have been in their current job for more than 10 years. Respondents' perceptions of being isolated, of their caring roles extending beyond their work; and of an inability to get away from work for holidays and study leave, were more common among rural dwellers. Eighty-one percent of respondents said that they felt part of their community and that proportion was higher for those working in rural areas, than for urban residents. Respondents indicated their perceived ease of access to five amenities and services: children's education (preschool, primary and secondary); access to a job for spouse; and health care. With the one exception of access to primary education, access was perceived to be most difficult by the professionals working in rural areas.
Conclusions: Our survey confirms, in the UK, the association between rural background and rural working, and highlights the contribution of healthcare professionals from other parts of the UK to the Scottish rural workforce. It also suggests that professional isolation and perceived lack of access to amenities are important issues for those working in rural areas.
Keywords: Highlands, recruitment and retention, rural workforce, Scotland.




