Rural circumstances are contributing factors to the higher incidence of adolescent pregnancy in rural areas compared to urban locations1,2. Access to and delivery of health care in rural areas are influenced by healthcare professional shortages3-5; distance from health services4,6,7; isolation from more populated areas; limited financial means to cover driving expenses to health appointments or for birth control and other resources8,9; familiarity with healthcare providers8; lack of anonymity, privacy, and confidentiality in personal, family, and professional contexts5; and religiosity10. While Ontario's public health mandate is to provide sexual health programs or services in schools, rural schools may have less support due to fewer rural staff, which can result in decreased delivery of sexual health education programs11. These circumstances interact and affect each other to make delivery of and access to rural health care problematic for rural female adolescents in particular because they must be more dependent on local rather than distant services and resources.
Rural women tend to have more children than urban women, have their first child at a younger age, and have lower incomes than rural men5,12,13. An unexpected pregnancy may worsen a rural female adolescent's ability to continue her education or advance her future. Adolescent pregnancy also poses physical and psychological health risks to both the young mother14,15 and her child16. In addition, children of teenage mothers have a greater chance of having a child during their own adolescent years, thereby continuing the cycle of adolescent pregnancy17,18. Thus, exploring the rural female adolescent sexual decision-making process regarding decisions about pregnancy is important because of the far-reaching implications of adolescent pregnancy for rural female adolescents, their families, and rural communities6,19.
Given the higher incidence of adolescent pregnancy in rural areas, the purpose of this study was to understand how rural female adolescents make decisions regarding sexual intercourse and pregnancy, and how they view rural factors and circumstances, such as geographical location, economic resources, and available health care, that impact this decision-making process.
Methodology
This research was conducted using constructivist grounded theory methodology as described by Charmaz20. Constructivism is a worldview that assumes that there are many realities and that the participant and researcher co-construct knowledge21. Schreiber and Stern22 suggest that grounded theory is ideal for understanding the social processes that occur in human interactions, and that it is especially useful for under-researched phenomena, making it appropriate for this study. In this study, rural female adolescents' decision-making regarding sexual intercourse and pregnancy was regarded as a process influenced by their rural context.
Participant sampling
A purposive sample of eight participants was used for this study. Inclusion criteria were self-identification as female between the ages of 16 and 19 years, having lived in rural areas of Ontario with a population less than 30 000 for the majority of their adolescence with a minimum of 1 year, heterosexual, unmarried, and not in a common law relationship. Participants who had been pregnant and/or had given birth were also invited to participate in the study. Adolescent females currently living in a city were included in the study provided they had lived rurally for a minimum of 1 year.
Participant recruitment
Study advertisements, such as tear-off flyers and brochures, were placed in various locations in rural Ontario such as rural health units, hospital lobbies, shopping malls, theatres, and stores that were relevant and available to rural adolescent females. Flyers were also posted at Western University to recruit female adolescents who had left their rural hometown to pursue their education.
Data collection strategies
Research participants were obtained through initial sampling (from criteria developed prior to the study) and theoretical sampling (by collecting data that better inform the categories emerging from the data)20. A total of eight adolescents participated in the study and were interviewed by the same female interviewer. Four of these participants were re-interviewed to better saturate the data for a total of 12 conducted interviews. Six out of eight of the initial interviews were in person and took place at Western University and in a public library and medical center in small towns. The other two participants were interviewed by telephone, as were the four participants who were re-interviewed. All participants were required to sign a consent form. To respect participants' privacy, participants aged 16 and 17 years did not require parental consent because of the highly sensitive and personal nature of the study.
Interviews involved open-ended questions to explore participants' experience living in a rural or small town as a female adolescent; access to sexual health education, information, and care; decision-making regarding engaging in sexual intercourse; decision-making experiences regarding pregnancy; and factors that affect personal, family, and community expectations about sexual intercourse and pregnancy. Particular emphasis was placed on exploring how the rural context affects rural female adolescents' experiences regarding such sexual decision-making. Interviews of 1-2 hours were audio-recorded and transcribed verbatim. Field notes were also used to record observations and perceptions about participants and the researchers' assumptions before, during, or after an interview20.
Data analysis
Data analysis followed the three coding guidelines for constructivist grounded theory as set out by Charmaz20: coding transcribed interviews20,23, sorting recurring codes into more abstract categories with the use of constant comparison analysis and theoretical sampling20,23, and developing and testing hypotheses about the emerging theory during ongoing data collection and analysis23. Memos were written to record pre-existing assumptions; thoughts, feelings and questions that surfaced during data collection and analysis; and methodological choices23. QSR International NVivo v10 qualitative data analysis software (QSR International; http://www.qsrinternational.com) was used to manage transcript data coding20,24.
Approaches for creating authenticity
Charmaz's20 four quality criteria - credibility, originality, resonance, and usefulness - were used to create authenticity. Attempting credibility involved becoming familiar with the research topic, employing investigator triangulation, and gathering sufficient data. Originality addresses whether the research offers innovative insights and an elaboration of current ideas found in the literature; as this study's research questions have rarely been examined in other studies, findings will significantly add to the current literature. Attempting resonance involved ensuring that analytic categories represent the complete gathered data; in this study, theoretical sampling was used to ensure that categories were fully elaborated, refined, and included many participant viewpoints.
Finally, usefulness of research is defined as whether it contributes to current knowledge and to creating a better world. Through publications and presentations, findings from this research will contribute to the current literature and help to inform rural healthcare practices and sexual health promotion initiatives.
Ethics approval
This study was approved by the Health Sciences Research Ethics Board (HSREB) at Western University (approval no. 103894).
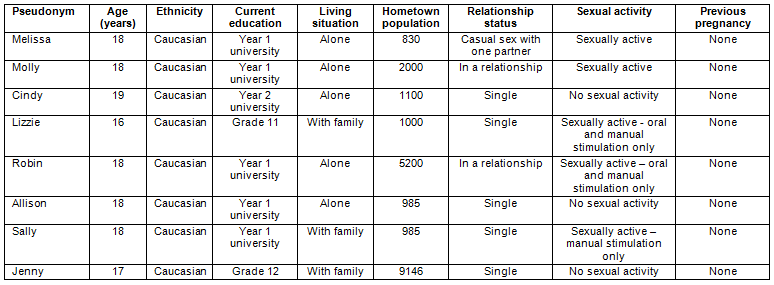
Demographic information, relationship status, and brief sexual history of study participants are shown in Table 1. Participants are referred to by their pseudonyms to protect their identities.
Table 1: Participant demographics
The core sexual decision-making process that participants engaged in, Prioritizing Influences, consisted of prioritizing four key influences: personal values and circumstances, family's values and expectations, friends' influences, and community influences (Fig1). The process of prioritizing involved assessing the influences present in their lives, evaluating the advantages and drawbacks of each decision, and, finally, prioritizing which influence affected them the most. These influences and the sexual decision-making process were embedded in and significantly affected by the rural context.
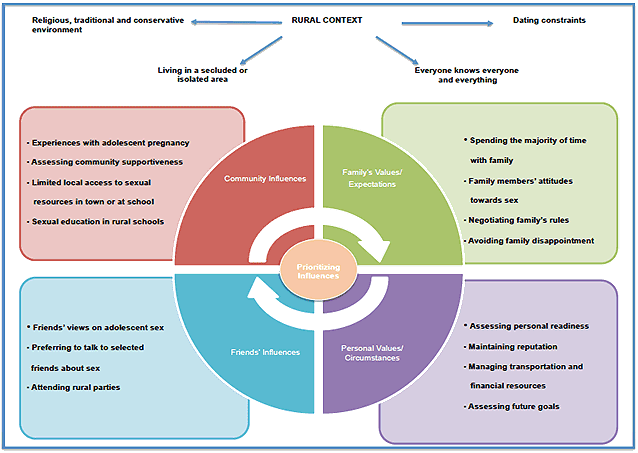
Figure 1: Rural female adolescents' sexual decision-making process.
The rural context
The process that rural female adolescents experience in sexual decision-making is situated in and influenced by the rural context.
Living in a secluded or isolated area: Participants reported that living in a rural area presented several challenges in the form of seclusion or isolation, which created distance between rural female adolescents and available opportunities. For instance, friends and romantic partners lived far away, there were limited entertainment options, less local sexual and reproductive services and resources, and more time spent with their families. Driving was reported as a necessity for all participants due to the distance between people, health services, and activities. However, the ability to drive was dependent on having a driver's license, finances for fuel expenses, access to a vehicle, and challenging weather conditions. As Melissa explained, 'It's expensive to go everywhere so you kind of think twice about going out before you do.'
Everyone knowing everyone and everything: Participants explained that it is common for rural community members to know each other well, and that it may be difficult for rural female adolescents to keep their sexual decision-making private. For instance, Lizzie stated that community members might be aware of who adolescents are dating or sleeping with and who is pregnant or has a sexually transmitted infection. Such gossip was very prevalent in participants' rural communities and community members' judgmental attitudes could make adolescents question or feel guilty about their sexual or reproductive choices. When rural female adolescents' privacy and anonymity are reduced, their sexual decision-making process can be compromised. For example, they might choose to not see a healthcare provider out of fear that they will run into someone they know in the waiting room. Robin explained that 'People would be scared to ... get ... condoms because they would run into people that they know.' Participants also explained that some rural female adolescents who are pregnant may drop out of school due to gossip.
Religious, traditional, and conservative environment: All participants explained that their hometowns had a religious Christian presence of various denominations with many community members who subscribed to traditional and conservative values: 'Almost everybody goes to a church and they have some ... kind of, um, religious upbringing ... to stay abstinent 'til you're married [Jenny].' These values were likely to influence them to delay sexual intercourse until marriage or avoid accessing contraception out of fear of being judged negatively by community members or excluded from their community if they chose to engage in premarital sex: 'A lot of times it would be the parents [who] would tell their kids to not talk to me and not go anywhere near me because I'm a bad influence [if I were sexually active][Jenny].'
Dating constraints: Participants stated that visibility, community interest, and judgment can affect a rural female adolescent's choices to date and engage in sexual activity because she may not feel comfortable being the talk of the town. Allison commented on the 'quality of male people around here'. With fewer partners to choose from, Cindy said that female adolescents tended to broaden the age range of their partners, and that often an older male adolescent would date a younger female adolescent and that 'the girls who were dating older guys almost always got pregnant.'
Personal values and circumstances
Assessing personal readiness: Assessing personal readiness was a subjective experience for participants based on their age, availability of a sexual partner, and personal beliefs regarding premarital sex. The availability of alcohol and/or drugs at a rural party could impact their decision to engage in sexual activity as could pressure from a male. Religious beliefs played a significant role in the sexual decision-making for some participants. For instance, Cindy stated, 'Being Christian, I believe that sex is for marriage.' Others were more concerned with waiting for the right person, and not necessarily for marriage.
Maintaining reputation: Participants noted that in a rural town, making certain decisions, such as engaging in sexual activity outside of a relationship or marriage, can negatively impact a rural female adolescent's reputation, as Melissa explained: 'Where I'm from, like, the people that sleep around have a very BAD reputation ... and it gets around and, because it's such a small town, EVERYBODY knows about it.' Participants also explained that, due to decreased availability of rural employment, finding a job in their rural town was highly dependent on their connections, and an adolescent's reputation is taken seriously. If a rural female adolescent has a reputation for being sexually active, it may be difficult for her to find employment because she may be deemed promiscuous and irresponsible. Furthermore, this reputation can cause loss of friends if other parents decide that she might be a negative influence on their children.
Managing transportation and financial resources: If participants wanted birth control services, they would likely have to tell their parents in order to either have the parent drive them or secure access to a car to drive themselves. As Melissa explained, 'You can't get ANYTHING. ... Nothing's accessible to you. ... So everything has to be driven to.' This is problematic for rural female adolescents who do not feel comfortable telling their parents about their sexual health appointment, decisions, or activities, and, thus, their commitment to access sexual health services could be minimized or eliminated. Participants noted that they also needed to finance drives to the pharmacy, health clinic, or store to buy contraceptives, condoms, monthly birth control pills, the 'morning after' pill, or a pregnancy test without their parents' knowledge, or if they drove to a different town to avoid being recognized by their community members while buying these items.
Assessing future goals: Preventing pregnancy was a specific concern for participants because they wanted to wait until they had finished their education and were settled in future careers. As Molly said, 'It would be a lot longer [after pregnancy] to try to finish your degree if you EVEN went back to it.' Robin observed that many rural female adolescents who get pregnant, 'have not gone to post-secondary education [and] some of them haven't even ... graduated secondary education.' Participants noted that these young women experienced fewer employment opportunities and life choices.
Family's values and expectations
Spending the majority of time with family: Melissa explained, 'There's a lot of people who are really close with their families and if ... [their families] would think badly of a decision like ... having sex randomly ... you're less likely to do it.' However, time spent with family did not necessarily mean that the family was close, consulted, or sought out regarding sexual decision-making. For example, Sally mentioned that she spent a lot of time with her family but never felt close enough to talk to them about sex.
Family members' attitudes towards sex: Family members' openness regarding sexual health affected whether participants would approach them for help with relationships or sexual-health-related questions. However, participants were reluctant to talk to their family about sexual activity unless it was serious like a pregnancy or a medical concern that might warrant the need for birth control or treatment. This reduced their likelihood of obtaining sexual information from their most accessible resource in their rural town: their parents. Some participants came from families that did not discuss sex at all, and talking to their families for information on sexual activity was not an option for them. For example, Sally mentioned that 'My family ... would NEVER give us information on [sex]. ... That was such a taboo subject.'
Negotiating family's rules: A rural female adolescent's family's rules could impact her sexual decision-making process by influencing her ability to make her own decisions, limiting her options, and shaping values regarding sexuality in the rural context. For instance, Robin mentioned that 'I never realized why [my mom] was strict until, like, I realized that there was that part of town where [adolescent pregnancy] happens.' Although Melissa's parents let her attend parties, they never let her spend the night because they believed that those who slept over had a higher likelihood of engaging in sexual activity. In this situation, Melissa's parents both limited and gave her the freedom to make her own sexual decisions while she was at parties by placing rules around her attendance such as with a curfew.
Avoiding family disappointment: In a rural environment in which family closeness is highly regarded and in which families spend the majority of their time together, participants explained that disappointing their family would be particularly difficult and meaningful, and priority would be placed on avoiding family disappointment. For instance, Cindy explained that when her family referred to people living together before marriage as 'shacked up,' it gave premarital sex a 'negative connotation' and that 'You don't wanna do something that's negative.' Similarly, Jenny said that if she had decided to engage in sexual activity before marriage, 'it would be very devastating' to her parents and that 'they would cry over it and pray for me a lot.'
Friends' influences
Friends' views on adolescent sex: Participants' most immediate friend groups tended to have similar interests and values regarding adolescent sexual activity. Jenny stated that her church friends were a primary influence on her decisions regarding sexual activity rather than her friends from school because of shared values and increased time spent with one another. Furthermore, Molly explained that having friends who were sexually active normalized adolescent sexual activity for her, and this affected her personal readiness to engage in sexual activity at a younger age than she had originally planned.
Preferring to talk to selected friends about sex: Participants mentioned that they considered their friends as resources for sexual information, especially if they came from families that did not discuss sexual activity. Sally explained, '[Friends were] how I found what sex WAS! I didn't know ANYTHING from home.' However, participants noted that their friends could not always to be trusted with private information due to the consequences of this information for reputations, employment, friendships, and other areas of life.
Attending rural parties: Parties in rural towns were described as often located in isolated areas, unsupervised, and a convenient place to engage in sexual activity, which was often a decision facilitated by alcohol or drug use. Participants explained that rural female adolescents who decided to engage in sexual activity at a party might be making a decision in the moment that they were unable to prepare for ahead of time by, for example, having condoms available, due to distance and compromised transportation.
It was very common to have large age gaps at parties because there are fewer people in rural areas in general. As Robin explained, 'In order for [the party] to be successful ... they really had to widen the age group.' Participants noted that it was not unusual, therefore, for there to be a significant age variance at a rural party and to have younger female adolescents engaging in sexual activity with older male adolescents who may be more sexually experienced and persistent.
Community influences
Experiences with adolescent pregnancy: Every participant had known several females who had experienced an adolescent pregnancy. Participants explained that it was also not unusual for a rural female to become pregnant during her adolescent years, while still in school, as young as in grade seven, and sometimes by an older male adolescent. Cindy stated that 'At one point there was 22 girls in my school who were pregnant. ... It wasn't unusual to be a ... high school student with a ... child.' Seeing other rural female adolescents' pregnancy experiences influenced participants' decisions to engage in safe sexual intercourse or to postpone sexual intercourse because they saw the difficulties that these young women endured, including dropping out or staying in school amidst gossip, struggling to raise their child with limited resources, or having to give their child up for adoption.
Assessing community supportiveness: Participants explained that, in some ways, they felt that community members were not supportive of rural female adolescents' decisions to engage in sexual activity. For instance, Allison explained that, even though she did not go to a Catholic school, she still found that 'it was a struggle to get the high school to stop teaching abstinence as a sexual education program' due to the high religiosity in her town. Allison felt it would be easier to make decisions regarding sexual health if the topic were openly discussed. However, while some adults in rural communities remained 'old fashioned,' Sally noted that times are slowly changing, and that more parents do not have a problem with safe, premarital adolescent sexual activity.
Limited local access to sexual resources in town or at school: Due to the limited local access to sexual resources in a rural town - specifically to preferred female healthcare professionals - sexual health resources at school can sometimes be the only ones available to rural female adolescents. Each participant had varying levels of sexual health resources in town or at school, for example a guidance counselor, community health nurse, or sexual health nurse. Having access to a sexual health nurse at school was not always helpful to rural female adolescents because of the high visibility at school and the ease of gossip spreading. Appointments outside of school, however, would require skipping class and risking parents finding out.
Sexual education in rural schools: The way that sexual education was taught at school was often highly dependent on the school's values and articulation of the curriculum, and on the teacher's approach to the topic. If it was not taught properly or at all, the students may have missed their only opportunity to learn about safe sexual activity. Melissa explained that many students attended Catholic school in her rural community, not because they were religious, but because it was the closest school to them, and other school options were too far away. Therefore, some students might receive abstinence education at a Catholic school even though they did not subscribe to these beliefs and would prefer other forms of sexual education.
Discussion
Barriers and facilitators to rural female adolescents' sexual decision-making
Participants in the study listed several barriers to sexual decision-making in a rural town, which echoed barriers to sexual health services found by other researchers, such as religiosity, transportation difficulties, boredom due to limited leisure activities, social exclusion due to sexual behavior and/or reputation, future prospects and goals, high visibility and familiarity, and scarcity of discreet services25-30. Participants in this study also identified several novel supportive factors that helped them cope with sexual decision-making barriers within the rural context, such as distance from a boyfriend if they did not wish to be sexually active, the flexibility of some health professionals in making appointments due to difficulty of travel, and informed and dedicated sexual health teachers, especially if parents and other rural services and resources were inaccessible. While researchers agree that sexual health education is an important sexual decision-making facilitator31,32, this study highlights that participants themselves also believe in the importance sexual health education and are open to it if it is taught effectively and informatively.
Recommendations to facilitate rural female adolescents' sexual decision-making
These study findings can help address sexual health issues in rural schools, rural communities, and with rural female adolescents.
Rural schools: To improve rural adolescent sexual health education, it is important that teachers tailor the sexual health curriculum to their rural community33. For instance, if there is a higher prevalence of adolescent pregnancy in a school, teachers could make pregnancy prevention the main focus of their sexual health education program. Furthermore, knowing what rural services are available, including reputable educational websites and help lines when in-person services are inaccessible, would be particularly useful for rural female adolescents. Teachers who work in rural schools that do not allow sexual education may be able to distribute general health information, such as trustworthy health websites, that include a section on sexual health information. Rural teachers can also consult with a local public health nurse or sexual health promoter to help facilitate teaching sexual education.
Another approach in rural schools is to increase students' sexual health literacy34. Based on participants' explanations, improved sexual health literacy for adolescents living in a rural environment could include knowing where and how to anonymously access accurate sexual health information and resources; effectively communicating sexual and reproductive needs with rural health professionals, partners, family members, and peers; and making and adhering to informed sexual decisions that are appropriate to their values and desires.
Availability of adolescent sexual health information and resources in rural schools would allow for increased access to healthcare providers, information on sexual health, and resources such as condoms and birth control in under-resourced communities19,35. However, while having access to sexual health services in rural schools can be helpful, the study's results indicate that the type of resource provided is also important. For example, having a public health nurse rather than a sexual health nurse at schools could facilitate anonymity regarding the services being sought, reduce rumors, and may be more accepted in schools not offering sexual education.
Rural towns: Sexual healthcare resources need to be local and accessible after school and on weekends and need to emphasize confidential access without family involvement to adolescents. In addition, rural female adolescents would benefit from enhanced access to female health practitioners to discuss reproductive issues36.
As rural communities are often religiously inclined, the church may act as a resource for rural populations, such as female adolescents, who have compromised health resources37. Parish nurses, registered nurses who work within a faith community, could provide sexual health information38. Small rural parishes that may not be able to afford parish nurses could consider sharing the cost of one nurse. Collaboration between health and religious staff could include open discussion with leaders of faith communities, such as ministers, on adolescent values and sexual health choices and options in order to help rural female adolescents make informed sexual decisions.
Due to the lack of services and resources in rural towns, rural assets such as strong family connections should be emphasized. Families can be an immediate resource for sexual health information if the family is accepting of discussing sexual health openly and is knowledgeable themselves39. One option to encourage open family discussion about sexual activity and relationships is a rural nurse-led family session that could help to provide parents with sexual health information and discussion opportunities related to how to approach this topic with their children, and including adolescent perceptions regarding confidentiality and sexuality33,40.
Rural female adolescents: Another critical aspect of sexual health promotion involves empowering rural female adolescents, for example by helping them to determine or identify their values regarding sexual activity. Although it is important for both males and females to have an understanding of each other's sexual values and preferences, and to encourage such dialogue between the two sexes, as participants noted, additional female-specific sessions that involve empowerment regarding sexual decision-making would be very useful. These sessions could be led by public health nurses, health promoters or teachers.
Telehealth and the internet have become increasingly popular methods of obtaining health care in rural areas due to their ability to increase healthcare access to isolated rural individuals and to lower travel costs for health care41. Through telehealth, a rural female adolescent could obtain quick and confidential access to a healthcare professional and sexuality-related information. When available at home, at the library, or at school, the internet can also be a confidential source of sexual health information, especially with the use of smart phones42. However, the internet may not provide sufficient, adequate, or reliable information on sexuality, when used on its own42,43, and should thus be used in concert with more reliable sexual health information from a healthcare provider or health educator.
Text messaging can also be used as a way for adolescents to access sexual health information and services, and it has been used successfully among at-risk adolescents in San Francisco43. The option of text messaging services with health professionals may be preferable to looking up information on the internet in rural areas that do not have good internet access. Text messaging also has the potential to provide immediate contact with a health professional, quick answers to sexual health questions, and the benefit of not having to travel for this information.
Strengths and limitations
This study contributes to the knowledge on rural female adolescent health and sexual health promotion by incorporating the views and experiences of rural female adolescents, who are rarely included in research. In addition, this study is one of the first to explore sexual decision-making process by rural female adolescents in Canada. Furthermore, a methodological strength for this study is the measures to ensure authenticity.
Limitations of this study include not having had an opportunity to interview a participant who had been pregnant and/or given birth for her perspectives regarding pre-pregnancy sexual decision-making; not having been able to interview most participants in their hometowns, which limited the understanding of participants' rural contexts; interviewing some participants in person and some by telephone; and participants not being of culturally diverse backgrounds.
Suggestions for future research include investigating the same topic with younger rural adolescent age groups, such as ages 13-16 years, rural male adolescents, lesbian, gay, bisexual and transgender youth, and with adolescents from other rural cultures, such as Aboriginal or immigrant adolescents. Furthermore, it would be beneficial to explore adolescents', teachers', and parents' views of sexual education and knowledge of sexual health; the impact of adolescent pregnancies in rural communities; sexual health education in rural public schools and rural religious schools, such as Catholic and Mennonite schools; rural healthcare providers' unique insights regarding rural adolescents' sexual health; and the potential sexual exploitation of rural female adolescents by older male adolescents. Telehealth, social media, and sexual health promotion initiatives in rural schools and communities should also be evaluated regarding their impact on adolescent sexual decision-making and sexual health literacy. Finally, more literature related to adolescent sexual behavior needs to be disaggregated for gender and geographical location (ie rural versus urban) to advance gendered understanding about rural youth sexual health and other health related topics.
This study reveals important new and preliminary information about rural female adolescents' sexual decision-making process and factors that influence this process, both positively and negatively. Recommendations provided may help to ameliorate rural female adolescents' sexual decision-making experiences and ensure that these females are empowered and knowledgeable to make sexual decisions that are appropriate for them.
References
1. Best Start. Teen pregnancy prevention: exploring out of school approaches. Toronto, ON: Best Start, Ontario's Maternal, Newborn and Early Child Development Resource Centre, 2008.
2. Ministry of Health and Long-Term Care. Initial report on public health. (Internet) 2009. Available: http://www.health.gov.on.ca/en/public/publications/pubhealth/init_report/ (Accessed 14 January 2016).
3. Leipert B, Leach B, Thurston W. Introduction: connecting rural women's health across time, locales, and disciplines. In: B Leipert, B Leach, W Thurston (Eds). Rural women's health. Toronto, ON: University of Toronto Press, 2012; pp. 3-25.
4. Romanow R. Rural and remote communities. In: R Romanow (Ed). Building on values: the future of health care in Canada. Final report. Ottawa, ON: Commission on the Future of Health Care in Canada, 2002.
5. Sutherns R. So close yet so far: rurality as a determinant of women's health. Canadian Woman Studies 2005; 24(4): 117-122.
6. Canadian Institute for Health Information. How healthy are rural Canadians? An assessment of their health status and health determinants. Ottowa, ON: Canadian Institute for Health Information, 2006.
7. Wong ST, Regan S. Patient perspectives on primary health care in rural communities: effects of geography on access, continuity and efficiency. Rural and Remote Health 9(1142): 1-12. (Internet) 2009. Available: www.rrh.org.au (Accessed 20 August 2014).
8. Leipert B, Matsui D, Rieder M. Women and pharmacologic therapy in rural and remote Canada. Canadian Journal of Rural Medicine 2006; 11(4): 296-300.
9. Leipert B, Landry T, Leach B. Closing the gap: rural women's organizations and rural women's health in Canada. In: B Leipert, B Leach, W Thurston (Eds). Rural women's health. Toronto, ON: University of Toronto Press, 2012; pp. 62-79.
10. Hemingway D, McLennan C. Harnessing information and communication technology to build an online community of northern/rural women. Canadian Woman Studies 2005; 24(4): 161-166.
11. Riddell T, Ford-Gilboe M, Leipert B. Strategies used by rural women to stop, avoid, or escape from intimate partner violence. Health Care for Women International 2009; 30(1): 134-159.
12. Ministry of Health Promotion. School health: guidance document. (Internet) 2010. Available: http://www.mhp.gov.on.ca/en/healthy-communities/public-health/guidance-docs/SchoolHealth.pdf (Accessed 4 August 2014).
13. Ostry A. Children, youth, and young adults and the gap in health status between urban and rural Canadians. In: J Kulig, A Williams (Eds). Health in rural Canada. Vancouver, BC: UBC Press, 2012; pp. 44-59.
14. Dryburgh HB. Teenage pregnancy 1997 data. Health Reports 2000; 12(1): 9-19.
15. Paranjothy S, Broughton H, Adappa R, Fone D. Teenage pregnancy: who suffers? Archives of Disease in Childhood 2009; 94(3): 239-245.
16. Chen XK, Wen SW, Fleming N, Demissie K, Rhoads GG, Walker M. Teenage pregnancy and adverse birth outcomes: a large population based retrospective cohort study. International Journal of Epidemiology 2007; 36(2): 368-373.
17. East PL, Reyes BT, Horn EJ. Association between adolescent pregnancy and a family history of teenage births. Perspectives on Sexual and Reproductive Health 2007; 39(2): 108-115.
18. Wellings K. Causes and consequences of teenage pregnancy. In: P Baker, K Guthrie, C Hutchinson, R Kane, K Wellings (Eds). Teenage pregnancy and reproductive health. London: Royal College of Obstetricians and Gynaecologists, 2007; pp. 69-80.
19. Varpalotai A. A web of support for rural girls: a school/community healthcare partnership. Canadian Woman Studies 2005; 24(4): 153-159.
20. Charmaz K. Constructing grounded theory, 2nd ed. London: Sage, 2014.
21. Denzin N, Lincoln Y. The discipline and practice of qualitative research. In: N Denzin, Y Lincoln (Eds). The Sage handbook of qualitative research. Thousand Oaks, CA: Sage Publications, 2005.
22. Schreiber RS, Stern PN. Using grounded theory in nursing. New York, NY: Springer Publishing Company; 2001.
23. Schreiber RS. The 'how to' of grounded theory: avoiding the pitfalls. In: RS Schreiber, PN Stern (Eds). Using grounded theory in nursing. New York, NY: Springer Publishing Company, 2001; pp. 55-83.
24. Richards L. Data alive! The thinking behind NVivo. Qualitative Health Research 1999; 9(3): 412-428.
25. Craig G, Stanley N. Visibility, immobility and stigma: young people's use of sexual health services in rural areas. Children and Society 2006; 20(3): 171-182.
26. Shoveller J, Johnson J, Prkachin K, Patrick D. 'Around here, they roll up the sidewalks at night': a qualitative study of youth living in a rural Canadian community. Health & Place 2007; 13(4): 826-838.
27. Bell J. Why embarrassment inhibits the acquisition and use of condoms: a qualitative approach to understanding risky sexual behaviour. Journal of Adolescence 2009; 32: 379-391.
28. Docherty A. Accessing sexual health services in rural Scotland. British Journal of School Nursing 2010; 5(2): 78-86.
29. Elliott B, Larson J. Adolescents in mid-sized and rural communities: foregone care, perceived barriers, and risk factors. Journal of Adolescent Health 2004; 35(4): 303-309.
30. Garside R, Ayres R, Owen M, Pearson V, Rozen J. Anonymity and confidentiality: rural teenagers' concerns when accessing sexual health services. Journal and Family Planning and Reproductive Health Care 2002; 28(1): 23-26.
31. Banister E, Begoray D, Daly L. Responding to adolescent women's reproductive health concerns: empowering clients through health literacy. Health Care for Women International 2011; 32(4): 344-354.
32. Sex Information and Education Council of Canada. Sexual health education in the schools: questions and answers, 3rd edition. (Internet) 2010. Available: http://www.sieccan.org/pdf/she_q&a_3rd.pdf (Accessed 23 November 2012).
33. Varpalotai A, Leipert B. Rural schools/rural communities: partnerships between physical and health educators and public health nurses. In: E Singleton, A Varpalotai, (Eds). Stones in the sneakers: active theory for secondary school physical and health educators. London, ON: Althouse Press, 2006; pp. 203-222.
34. Ratzan R, Parker S, Lurie N. Health literacy: a policy challenge for advancing high-quality health care. Health Affairs 2003; 22(4): 147-153.
35. Leipert B. Rural women's health issues in Canada: an overview and implications for policy and research. Canadian Woman Studies 2005; 24(4): 109-116.
36. Plunkett R, Leipert B. Women's health promotion in the rural church: a Canadian perspective. Journal of Religion and Health 2013; 52(3): 877-889.
37. International Parish Nurse Resource Centre. Parish nursing fact sheet. (Internet) 2009. Available: https://www.queenscare.org/files/qc/pdfs/ParishNursingFactSheet0311.pdf (Accessed 24 September 2014).
38. Wang J, Simoni P, Wu Y. Human papillomavirus (HPV) in rural adolescent females: knowledge, protected sex, and sexual risk behaviors. Online Journal of Rural Nursing and Health Care 2006; 6(1): 74-88.
39. Kennedy E, MacPhee C. Access to confidential sexual health services. The Canadian Nurse 2006; 102(7): 29-31.
40. Gagnon MP, Duplantie J, Fortin JP, Landry R. Implementing telehealth to support medical practice in rural/remote regions: what are the conditions for success? Implementation Science 2006; 1(18): 1-8.
41. Campbell L. Grrls plugged in: how Canadian rural young women are using the internet. Canadian Woman Studies 2005; 24(4): 167-170.
42. Sutherns R, McPhedran M, Haworth-Brockman M. Rural, remote, and northern women's health: policy and research directions: final summary report. Winnipeg, MB: Centres of Excellence for Women's Health, 2004.
43. Levine D, McCright J, Dobkin L, Woodruff A, Klausner J. SEX INFO: a sexual health text messaging service for San Francisco youth. American Journal of Public Health 2008; 98: 393-395.



