The earthquake-tsunami on 26 December 2004 was one of the most severe natural disasters to hit Indonesia1. It was reported that 126 741 persons were killed, 93 285 went missing, 500 000 lost their abodes, and 750 000 were suddenly unemployed2. The emergency health sector was also reduced to chaos3,4, with 517 health facilities destroyed5. Local health personnel played a minimal role in the response to the disaster, with about 245 health workers confirmed dead and 413 missing. The World Bank estimated the overall loss to the health sector at about $91.9 million, with $131.14 million being required for health facility reconstruction6,7. However, the full impact of the earthquake-tsunami was unknown8.
Apart from damage, ecological disruption, loss of human life, and worsened health status, people were exposed to high levels of immediate and long-term stress, for years9-12. WHO reported that up to 50.0% of the tsunami-affected people in Aceh experienced significant psychological distress and 5-10% developed diagnosable stress-related psychiatric disorders9,13.
After the tsunami, the Indonesian government, working with national and international organizations, launched a national disaster preparedness policy, including the management of mental health and psychosocial problems in tsunami-affected Aceh communities. The Community Mental Health Nurse Program (CMHNP), started in 2006, aimed to (1) provide psychosocial and mental health services for communities impacted by disasters and conflicts, (2) increase community participation in community mental healthcare dealing with disasters and conflicts, and (3) encourage community members to prepare for potential disasters and promote good mental health among communities in disaster-affected areas14-20. Medical doctors, nursing staff and community health workers with mental health training provide mobile outreach services in rural areas, which include treatment, education, and support, targeted at patients, their families and community members21.
Aceh is a disaster-prone area, highly vulnerable to natural hazards such as floods and earthquakes9,14-20,22. Therefore, household and community disaster preparedness is an essential mitigation strategy to protect human lives from the adverse health impacts of natural disaster high-risk areas23. There have been few population-based studies of disaster preparedness among people in the tsunami-affected areas in Aceh. Therefore, this study aimed to assess knowledge of disasters and disaster preparedness of the community members, which were the outcome indicators of the CMHNP.
Study setting, design and samples
This community-based descriptive household survey study was conducted in Aceh, in September and October 2014. The study population comprised community members representing three selected districts strongly affected by the tsunami: Aceh Besar on the west coast, Banda Aceh on the north coast, and Pidie on the east coast (Fig1). The inclusion criteria were (1) community member aged 18-70 years, living in the study area, who had experienced the earthquake-tsunami disaster, (2) voluntary participation in the study, (3) ability to communicate in Bahasa Indonesia. Community members who were deaf, sick at the time of data collection, and migrants from outside Aceh or who resided in the community after the rehabilitation and reconstruction of Aceh, were excluded.
In this study, the unit of analysis was the individual household. Sample size was calculated using the single proportion formula24, with 95% confidence interval. The sample size was based on 50.0% of population having good levels of disaster preparedness, since there was no published literature regarding the proportion of disaster preparedness among community members in these earthquake-tsunami areas. Precision was set at 5.0%, and sample size calculated as 384. The sample size was multiplied by the maximum design effect for clustering of two to give a sample of 768. To allow for an 8% non-response rate, the final sample size was 830. There were 220 villages in 17 subdistricts in three tsunami-affected areas. Of these, 40 villages were randomly selected using two-stage probability proportional to size sampling. For each village, systematic random sampling was used to select 20-21 representative household community members for interview by starting from the centre of the village and moving left to select every other household. One representative was selected for one household. The total study sample was 827, yielding a response rate of 99.6% (827/830).
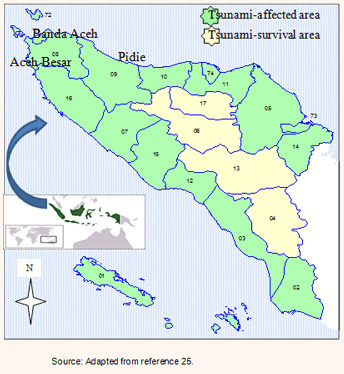
Figure 1: Map of Aceh, Indonesia, showing tsunami-affected and tsunami-survival areas25.
Survey instrument
The household survey instrument developed by the researchers comprised three parts. Part I consisted of 11 questions regarding the respondent's baseline characteristics, including sex, age, marital status, family type, religion, ethnicity, previous abode/history, education, occupation, households with children aged less than 12 years, and households with physically dependent members.
Part II comprised 23 dichotomous items with 'true/yes', or 'false/no' format, to assess the community members' disaster knowledge. A score of 1 was given for a correct answer and a score of 0 for an incorrect answer. A score of up to 60% of the total score was 'poor', 61-80% 'moderate', and more than 80% 'good'. Cronbach's alpha was 0.748 for knowledge of disasters.
Part III dealt with community disaster preparedness, and consisted of a 17-item questionnaire measuring community-related disaster preparedness (three items), disaster information for the family (six items), and disaster supply kit/vehicle at home (eight items). Responses were rated on a three-point rating scale: 0='never', 1='sometimes', and 2='always'. A score of 0-20 (≤60% of total score) was 'low', 21-27 (61-80% of total score) 'moderate', and 28-34 (?80% of total score) 'good'. Cronbach's alpha was 0.901.
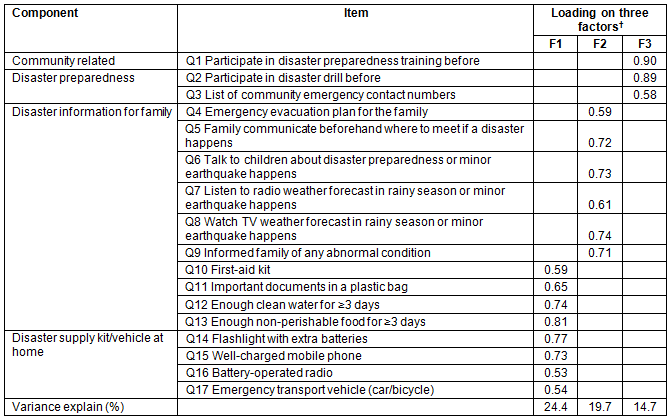
All 17 items of the three components (community-related disaster preparedness, disaster information for the family, disaster supply kit/vehicle at home) were included in the analysis. The most highly rated factor was disaster supply kit/vehicle at home (factor loading 0.53-0.81), followed by disaster information for the family (factor loading 0.59-0.74), and community-related disaster preparedness (factor loading 0.58-0.90) (Table 1).
The study questionnaire was back-translated (Bahasa Indonesia-English-Bahasa Indonesia); the final version was pre-tested with 30 samples and revised before data collection in the main study.
Table 1: Factor analysis for 17-item disaster preparedness survey using principal component extraction with varimax rotation (n=827)
Data collection
Ten research assistants who were postgraduate students in the Disaster Management Program at Syiah Kuala University Aceh, Indonesia were trained for 1 day on the informed consent process and interviewing participants. These research assistants also were trained how to deal with community members who have tsunami experience. All participating community members were interviewed and survey forms were filled out by trained research assistants. Each research assistant received onsite supervision from the principal investigator who has been teaching in disaster management in Kuala University Aceh for more than 10 years and also working as a public health professional in Aceh for more than 30 years. All research assistants were familiar in dealing with community members. During data collection, no potential acute mental health issues caused by the data collection process were found. All respondents' answers were kept confidential and discussed only among team members and solely for research purposes.
Data analysis
Study data were edited, coded, and entered into the Statistical Package for the Social Sciences for Windows v18 (SPSS; http://www.spss.com). The general characteristics and other study variables were described by number, percentage, mean, and standard deviation. Factor analysis was used to analyze explanatory factors for the disaster-preparedness questionnaire.
Ethics approval
This study was approved by the Ethical Review Committee of the Faculty of Public Health, Mahidol University (COA. No. MUPH 2014-188; 2014 Sep 18), and permission was provided by the Aceh Government of Indonesia (ND. NO. 875.1/1003, Tanggal 23 Mei 2014).
General characteristics
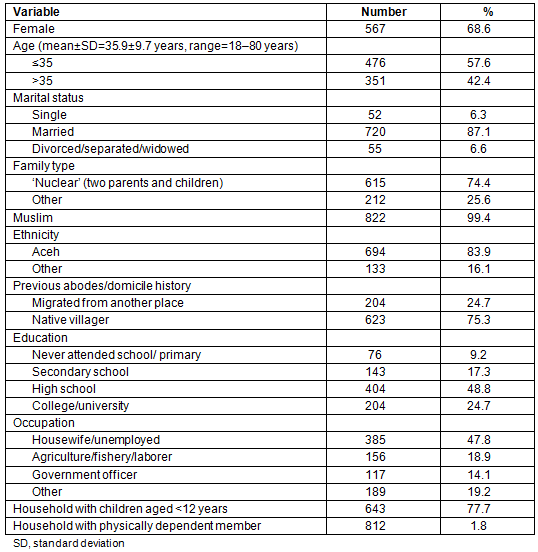
Of the 827 community members, 68.6% were female, 57.6% were aged 35 years or less, 87.1% were married, 74.4% were from 'nuclear families' (two parents and their children), 99.4% were Muslim and 83.9% were of Aceh ethnicity. Native villagers constituted 75.3% of the sample, 48.8% had finished high school, 47.8% were housewives or unemployed. A total of 77.7% were in households with children aged less than 12 years and 1.8% were from households with physically dependent members (Table 2).
Table 2: General characteristics of surveyed community members in Aceh Besar, Banda Aceh and Pidie, Indonesia (n=827)
Prevalence of knowledge of disasters, and good disaster preparedness
About 57.6% of community members had good disaster knowledge. Only 26.0% had a good level of disaster preparedness (Table 3). Both knowledge of disaster and disaster preparedness of the community members did not achieve the target of the CMHNP outcome indicators (<60.0%) (Table 4). Details for knowledge of disasters is shown in Table 5. The main problems of disaster knowledge were that only 52.1% of community members reported having a battery-operated radio at home, while 56.7% reported storage of enough fresh meat for at least 3 days at home. A total of 66.9% reported turning off mains water before evacuation and 68.3% reported being able to indicate the location of an emergency warning system in the community (Table 5).
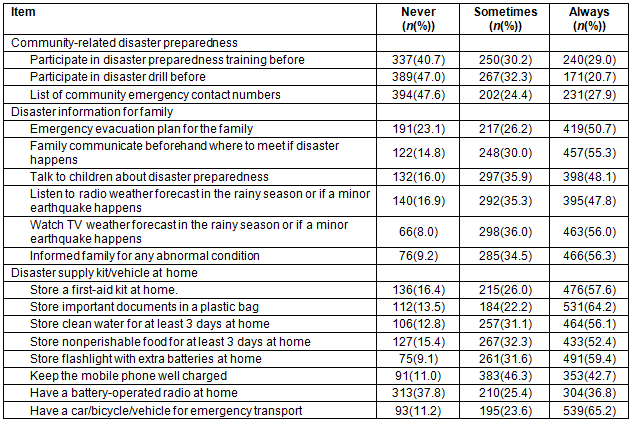
Table 6 shows the components of disaster preparedness. For the community-related disaster preparedness component, only 20.7% reported that they had always participated in previous disaster drills, 27.9% always had a list of community emergency contact numbers and 29.0% had always participated in disaster preparedness training.
Regarding disaster information for the family, 47.8% reported always listening to radio forecasts in the rainy season or about the occurrence of a minor earthquake, 48.1% always talked to children about disaster preparedness, 50.7% reported always having an emergency evacuation plan for the family and 55.3% reported always communicating to family beforehand where to meet if a disaster happens.
In the last component, disaster supply kit/vehicle at home, 36.8% reported that they always had a battery-operated radio at home, 42.7% reported always keeping the mobile phone well charged, 52.4% reported always storing enough non-perishable food for at least 3 days at home and 56.1% reported that they always stored enough clean water for at least 3 days at home.
Table 3: Prevalence of knowledge of disasters, and disaster preparedness of surveyed community members in Aceh Besar, Banda Aceh and Pidie, Indonesia (n=827)
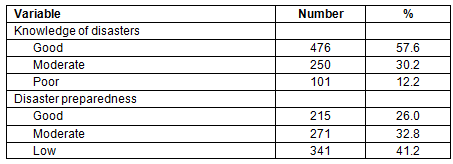
Table 4: Target and actual community member indicators of the Community Mental Health Nurse Program, Aceh, Indonesia

Table 5: Disaster knowledge among community members in Aceh Besar, Banda Aceh and Pidie, Indonesia (n=827)
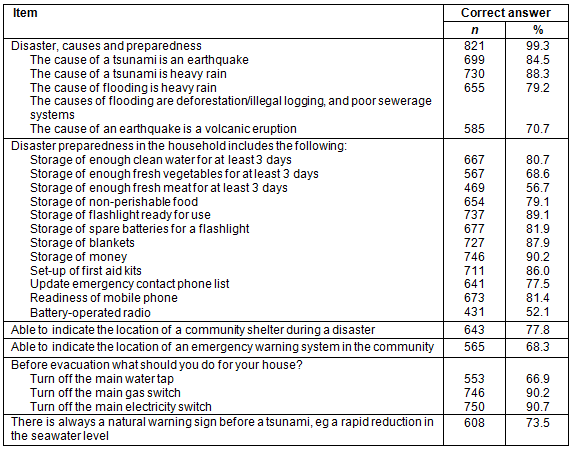
Table 6: Level of disaster preparedness among surveyed community members in Aceh Besar, Banda Aceh and Pidie, Indonesia (n=827)
Discussion
Although the community members in the study areas had direct experiences of a tsunami, the proportions of people with good knowledge of disaster (57.6%), and good disaster preparedness (26.0%) were much lower than the Aceh government target indicators, which were set at 70%. Only half of the community members had good levels of knowledge, in particular poor knowledge of disaster preparedness in relation to the storage of items. There may be too many items to remember.
This study included only community members in the tsunami-affected areas, unlike a previous study, which included samples from both tsunami-affected and non-affected areas in coastal Aceh26. That study found that people with direct experience of the tsunami had higher mean scores for knowledge, individual emergency planning and resource mobilization than those with indirect experience26. Another study from Thailand27 reported that people who experienced loss from the 2004 tsunami were more likely to participate in community activities and respond to earthquake hazards. The actual experience of loss can increase levels of disaster preparedness among these people. The finding in Aceh is inconsistent with the study in Thailand. One possible explanation is that Thailand has a clearer policy for disaster preparedness, drills and training. In the tsunami-prone areas, there are clear signposts, assembly points, forecasting, early-warning systems, and awareness of potential disaster risks and knowledge of disaster preparedness is actively promoted. People were encouraged by the village headman and staff to participate in disaster drills twice a year. In addition, the villagers are more likely to participate in community activities since disaster risk reduction is not just an individual effort. It can be fostered by social networking27.
The study found that the community-education intervention was ineffective. The educational intervention by the community mental health nurse, focusing on disaster preparedness and mental health status, seemed to be a common occurrence for the community members; this was the first evaluation of this national program. Since 2009, the CMHNP had not been re-orientated, and did not reflect the mental health promotion activities of the CMHNP, with no integration into routine public health service delivery to ensure the sustainability of the program28. Therefore, it is necessary to understand the culturally specific coping mechanisms of the Acehnese. They were quite familiar with the tsunami event. Many community members believed that the tsunami disaster was 'a punishment from God' due to the long-lasting civil war and their bad behavior. Therefore, they may have paid less attention to the community mental health nurses. The communities' strong religious faith had helped them to mitigate their pain, and accept and overcome negative events throughout their lives29. Like Buddhists in Thailand, they interpreted the tsunami disaster according to the 'law of karma', or cause and effect. They believed that life is to a certain extent predetermined and the result of one's own intent and actions30.
At present, few studies have reported on public health disaster preparedness in Banda Aceh. Well-prepared communities are more likely to participate in disaster recovery efforts, to deliver services more effectively, and to shorten the necessary disaster response28. A well-prepared health system can reduce disaster risk, but a response capacity is needed, especially an information system. The CMHNP might not be the best way to help communities prepare for a disaster, because of the large populations involved. Community participation and networking are also required.
Study limitations
The results of this study relied on self-reports, so there may be some reporting bias regarding disaster preparedness among community members. There were no baseline data regarding the evaluation of knowledge of disaster and disaster preparedness status in the study areas. Also, Aceh has up to eight local languages; there might be differential interpretations of questions and responses among community members.
This study provides baseline data for some outcome indicators of the CMHNP, but does enable assessment of the program's effectiveness. Disaster preparedness and knowledge of disaster education should be promoted and supported in remote rural Acehnese communities. Working at the community level can reduce the negative impact of disasters, such as injuries and loss of life, property damage and social disruption; however, the best way to manage the negative impact remains unresolved. Community participation may be needed, together with the establishment of networks to strengthen community capacity in the affected areas; this may be a more effective focus for the CMHNP. Qualitative research is recommended to elicit more detail about the quality of disaster preparedness and the disaster knowledge of community members.
Acknowledgements
The authors acknowledge the Governor of Aceh State, Republic of Indonesia, and the Human Resource Development Board of Aceh, who provided financial support during this study. They also gratefully acknowledge Universitas Muhammadiyah Aceh, Universitas Syiah Kuala Darussalam Banda Aceh, in particular Nazli Ismail, PhD for his commitment to leading the research team during the workshop and data collection. They are extremely grateful to Aceh Health Office, District Health Office, and the research participants, who in an intensely personal and collective disaster gave freely of their time and information. This study was partially supported by the China Medical Board, Faculty of Public Health, Mahidol University.
References
1. Carballo M, Daita S, Hernandez M. Impact of the Tsunami on healthcare systems. Journal of the Royal Society of Medicine 2005; 98: 390-395. http://dx.doi.org/10.1258/jrsm.98.9.390
2. Agency for the Rehabilitation and Reconstruction of Aceh and Nias. Strengthening the narrative of community life: two year report. Banda Aceh: Agency for the Rehabilitation and Reconstruction of Aceh and Nias, 2007.
3. Garfield R, Hamid AY. Tsunami response: a year later. Postdisaster nursing in Aceh, Indonesia. American Journal of Nursing 2006; 106(1): 76-79. http://dx.doi.org/10.1097/00000446-200601000-00036
4. World Health Organization. Mental health in emergencies: mental and social aspects of health of populations exposed to extreme stressor. Geneva: World Health Organization, 2003.
5. Agency for the Rehabilitation and Reconstruction of Aceh and Nias. Enriching the construction of the recovery: annual report 2007. Banda Aceh: Agency for the Rehabilitation and Reconstruction of Aceh and Nias, 2008.
6. Bappenas and World Bank. Indonesia: preliminary damage and loss assessment. (Internet) 2014. Available: http://www.unep.org/tsunami/reports/damage_assessment.pdf (Accessed 10 March 2014).
7. Bappenas and the International Donor Community. Indonesia, notes on reconstruction, the December 26, 2004 natural disaster. (Internet) 2005. Available: http://www.preventionweb.net/files/2165_VL323115.pdf (Accessed 10 March 2014).
8. United Nations Office for the Coordination of Humanitarian Affairs. Indonesia earthquake and tsunami: situation report no. 38. (Internet) 2005. Available:http://reliefweb.int/report/indonesia/indonesia-earthquake-and-tsunami-situation-report-no-38 (Accessed 12 February 2014).
9. World Health Organization. WHO recommendation for mental health in Aceh. Banda Aceh; Ministry of Health, Republic of Indonesia, 2005.
10. Boothby N, Veatch M. Community mental health treatment, protection and promotion for women and children in Aceh: findings from an evaluation of programs supported by the Health Service Program. Columbia University: JSI Research and Training Institute, Inc. and Program on Forced Migration and Health, 2007.
11. McEntire DA, Myers A. Preparing community for disaster issues and process for government readiness. Disaster Prevention and Management 2004; 13: 140-152. http://dx.doi.org/10.1108/09653560410534289
12. Tillman P. Disaster preparedness for nurses: a teaching guide. Journal of Continuing Education in Nursing 42: 404-408. http://dx.doi.org/10.3928/00220124-20110502-02
13. American Red Cross. Disaster cycle services, fiscal year 2013. (Internet) 2013. Available: http://www.redcross.org/about-us/publications (Accessed 19 March 2014).
14. Prasetiyawan, Viora E, Maramis A, Keliat BA. Mental health model of care programmes after the tsunami in Aceh, Indonesia. International Review of Psychiatry 2006; 18: 559-562. http://dx.doi.org/10.1080/09540260601039959
15. Putra A, Petpichetchian W, Maneewat K. Review: public health nurses' roles and competencies in disaster management. Nurse Media Journal of Nursing 2011; 1: 1-14.
16. Jakeway CC, Larosa G, Cary A, Schoenfisch S. The role of public health nurses in emergency preparedness and response: a position paper of the association of state and territorial directors of nursing. Public Health Nursing 2008: 25: 353-361. http://dx.doi.org/10.1111/j.1525-1446.2008.00716.x
17. Langan JC, James DC. Preparing nurses for disaster management. Upper Saddle River, New Jersey: Pearson Education, 2005.
18. Michelle C, Keith E, Craig D, Tony M, Frank T, Linda W, et al. Household disaster preparedness and information sources: rapid cluster survey after a storm in New South Wales, Australia. BMC Public Health 2008; 8: 195. http://dx.doi.org/10.1186/1471-2458-8-195
19. Kapucu N. Culture of preparedness: household disaster preparedness. Disaster Prevention and Management 2008; 17: 526-535. http://dx.doi.org/10.1108/09653560810901773
20. Robins SP. Organizational behavior (9th Edn). Upper Saddle River, New Jersey: Prentice-Hall, 2001.
21. Ng C, Herrman H, Chiu E, Singh B. Community mental health care in the Asia-Pacific region: using current best-practice models to inform future policy. World Psychiatry 2009; 8: 49-55. http://dx.doi.org/10.1002/j.2051-5545.2009.tb00211.x
22. Souza R, Bernatsky S, Reyes R, de Jong K. Mental health status of vulnerable tsunami-affected communities: a survey in Aceh Province, Indonesia. Journal of Traumatic Stress 2007; 20: 263-269. http://dx.doi.org/10.1002/jts.20207
23. Tomio J, Sato H, Matsuda Y, Koga T, Mizumura H. Household and community disaster preparedness in a Japanese provincial city: a population-based household survey. Advances in Anthropology 2014; 4: 68-77. http://dx.doi.org/10.4236/aa.2014.42010
24. Daniel WW, Cross CL. Biostatistics: a foundation for analysis in the health sciences. New York: John Wiley and Sons, 2013.
25. Tsunami and Disaster Mitigation Research Center. Tsunami and Disaster Mitigation Research Center. (Internet) 2012. Available: http://tdmrc.unsyiah.ac.id/en/ (Accessed 10 February 2014).
26. Rachmalia MNS, Hatthakit U, Chaowalit A. Tsunami preparedness of people living in affected and non-affected areas: a comparative study in coastal area in Aceh, Indonesia. Australasian Emergency Nursing Journal 2011; 14: 17-25. http://dx.doi.org/10.1016/j.aenj.2010.10.006
27. Witvorapong N, Muttarak R, Pothisiri W. Social participation and disaster risk reduction behaviors in tsunami prone areas. PLoS ONE 2015; 10(7): e0130862. http://dx.doi.org/10.1371/journal.pone.0130862
28. Ardalan A, Mowafi H, Malekafzali Ardakani H, Abolhasanai F, Zanganeh AM, Safizadeh H, et al. Effectiveness of a primary health care program on urban and rural community disaster preparedness, islamic republic of Iran: a community intervention trial. Disaster Medicine and Public Health Preparedness 2013; 7: 481-490. http://dx.doi.org/10.1017/dmp.2013.93
29. Domínguez G. Ten years after the tsunami: how has Aceh changed? (Internet) 2014. Available: http://www.dw.com/en/ten-years-after-the-tsunami-how-has-aceh-changed/a-18149958 (Accessed 14 January 2015).
30. Van Griensven F, Chakkraband MLS, Thienkrua W, Pengjuntr W, Lopes Cardozo B, Tantipiwatanaskul P, et al. Mental health problems among adults in tsunami-affected areas in southern Thailand. Journal of the American Medical Association 2006; 296: 537-548. http://dx.doi.org/10.1001/jama.296.5.537





