Introduction
The problem of emergency department (ED) overcrowding is a major issue for emergency medicine in Australasia1. Interventions to reduce crowding are commonly aimed at reducing the ED length of stay (EDLOS). Studies have looked at multifaceted interventions, including changes in staff profiles and work policies, which have successfully reduced EDLOS2,3. One study in the USA that examined triage by a senior doctor found reduced EDLOS but with an increased cost4. Several UK studies examining early screening by senior staff have shown a decrease in medical and surgical admissions5-7. Recent work in a rural ED in Australia has indicated that the presence of an emergency physician in the department decreases both waiting time by triage category and access block8. This study looks at the effect of having a specialist emergency physician working in the ED at night. The authors are not aware of any published literature in Australasia that directly addresses this question.
Tamworth Base Hospital is a 262 bed public hospital in rural New South Wales (NSW), Australia. Five emergency physicians who are all Fellows of the Australasian College for Emergency Medicine (FACEM) run the ED, which has an annual census of approximately 37 000 and an 18% admission rate. Night shift in the ED runs from 2230 hours until 0800 hours and is staffed by two doctors, usually a resident medical officer (RMO) and a career medical officer (CMO) or locum. During these shifts pathology tests can be ordered and the radiographer, inpatient registrars and consultants can be contacted at home to provide a service or consultation if required. The use of these essential, external services contribute to the additional cost of patient care above the baseline operational costs of the department.
Due to a staff shortage in January and February of 2002, two emergency physicians worked seven consecutive night shifts. Each of these night shifts was staffed by one emergency physician and one intern (postgraduate year one). This situation led opportunistically to the generation of the null hypothesis that there was no significant difference in ED waiting times, EDLOS, admissions, diagnostic investigations and consultations between those shifts when an emergency physician was present and those shifts when they were not.
Methods
A retrospective analysis of the ED information system (EDIS) database was used to obtain the data for this study. The compilation of an EDIS database has been used by most NSW public hospital emergency departments since 1995. The Area Health Service Ethics Committee was consulted and considered that neither formal approval nor individual informed consent was required for the study.
A comparison was made between two cohorts of patients. Group A consisted of patients seen during a period of seven night shifts between 28 January and 4 February 2002 when an emergency physician was one of the two night shift doctors on duty. The second doctor on these shifts was an intern. The emergency physician was involved both in seeing patients and supervising the intern. Group B consisted of patients seen on the night shift on the same dates of the previous year, between 28 January and 4 February 2001. There were two doctors rostered on these night shifts, an RMO and a CMO or locum. It was found that there were three multi-trauma patients in Group B and none in Group A. Therefore, these three patients were excluded from Group B in order to moderate the potential bias caused by major trauma, which involves surgical registrar review, consultant call-back and radiographer call-back.
The information collected from the EDIS database consisted of age, gender, triage category, diagnosis, waiting time, EDLOS, pathology tests ordered, X-rays ordered, specialist consultations, admissions, and representations for the same complaint within 7 days. Waiting time was the time between arrival and being seen by a doctor. EDLOS was the time between being seen by a doctor and disposition from the department. De-identified information was transferred from the original database and entered into a Microsoft EXCEL spreadsheet.
The two groups were first compared in terms of the independent variables of age, gender, triage category and diagnosis category using appropriate statistical tests to see whether or not they were similar in these characteristics. Triage categories for the two cohorts ranged from 2 (in need of treatment within 10 min of arrival) to 5 (patients who have a less urgent condition in need of treatment within two hours)9. The diagnoses entered by the doctor on the EDIS database for each patient were grouped into sixteen logical categories according to the disease of injury type.
Having compared the independent variables, the waiting time and EDLOS for the two groups were described in terms of median and 25th-75th percentiles because they were not normally distributed. The non-parametric Wilcoxon Rank Sum test was used to test the statistical significance of the differences in these times between the two groups. The number of admissions, pathology tests, X-rays, call-backs, telephone consultations and re-presentations (scheduled and unscheduled) were also compared and assessed for their statistical significance using either c2 analysis or the Fisher's exact test, as appropriate. For those patients who had pathology tests ordered, the number and cost of tests per patient was compared again using the Wilcoxon rank sum test.
Results
The results of the comparison of the independent variables of age, gender and triage category are shown (Table 1) and the age distribution is shown (Fig 1). The distribution of patients across these 'diagnosis categories' for Group A and Group B is shown (Fig 2). It is apparent that there was no statistically significant difference for any of these variables (p > 0.05) and that the two groups were, therefore, comparable.
Table 1: Comparison of independent variables for group A and group B
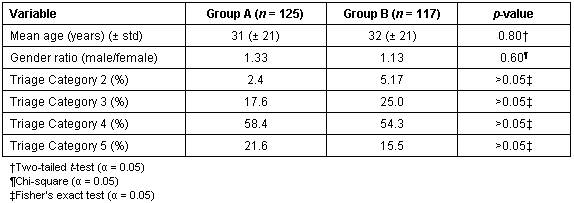
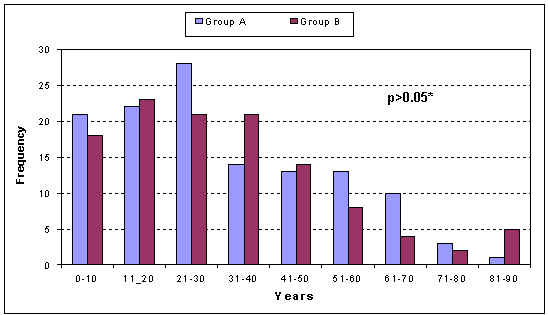
Figure 1: Age distribution for group A and group B (two-tailed t-test [α = 0.05]).
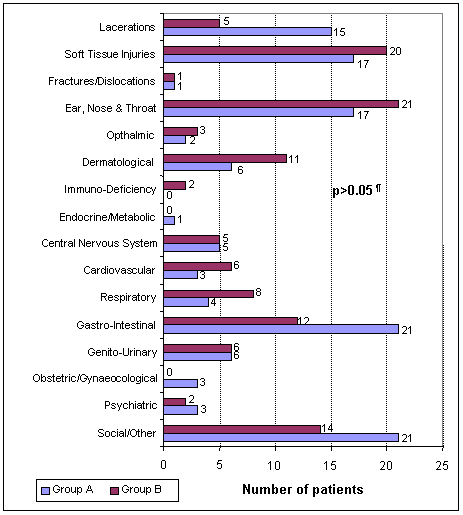
Figure 2: Diagnosis categories for group A and group B patients (Mann-Whitney U test [α = 0.05]).
The results of the analysis of waiting times and EDLOS are shown (Table 2), demonstrating that there was a significant improvement in EDLOS when an emergency physician was present. Table 3 compares admissions, diagnostic tests, consultations and representations for each group. The number of admissions is significantly smaller in Group A, the emergency physician group. Similar numbers of patients had pathology tests performed in each group but the median number of tests per patient was significantly less in Group A. The number of X-ray examinations performed in the two groups was similar, however, the total cost of pathology tests and X-ray examinations was significantly less in Group A.
Table 2: Comparison of waiting time and ED length of stay

Table 3: Comparison of the outcome factors for the two groups
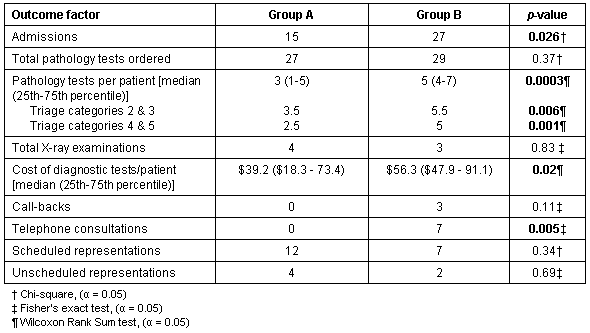
In order to assess the effect that different triage categories may have had on outcome measures in each group, both groups were divided into those patients in triage categories 2 and 3 and those categorised as 4 or 5. The Wilcoxon rank sum test was again used to test for statistically significant differences in EDLOS and the median number of pathology tests ordered per patient. This was found to further verify the differences between Groups A & B (p < 0.05 in all cases).
Specialist consultations were divided into call-backs, when the registrar or consultant attends the hospital and a fee is incurred, and telephone consultations. There were significantly fewer telephone consultations in the emergency physician group. Further, when re-presentations within 7 days were divided into scheduled and unscheduled, it was found that there was no significant difference in either between the two groups.
Discussion
This study demonstrated that there were a number of statistically significant differences in outcome measures between those shifts when there was an emergency physician present in the ED and when there was not. The two groups of patients compared were deemed comparable on the basis of age, sex, triage category and diagnosis category. Each period of time included in the study consisted of seven consecutive night shifts and so had an equal distribution of weekdays and weekends. The samples were taken from the same time of year to avoid seasonal variations of illnesses. There were no identifiable changes in departmental procedures and protocols between the two study periods that would account for these differences, and the retrospective study design eliminated the influence of a performance bias by the staff.
The potential effect on the data of excluding the three multi-trauma patients from group B is acknowledged and may be regarded as problematic. However, when a trauma case is in the department, specialists and registrars are called in and so it can be argued that the impact on the rostered medical staff in the ED should not be great. There is a greater impact on the nursing staff, although this too is moderated by the night supervisor and intensive care unit nurses being called if necessary. The authors believe that the considerable difference between the outcome variables in each group could not reasonably be attributed solely to this effect.
Median waiting time to see a doctor was similar for the two groups, at approximately 1 h. It was evident that a number of patients seen after 2230 hours, the time that the night shift begins, had presented before this time, some perhaps several hours before. It is felt that this 'existing wait' rendered absolute waiting time an unreliable outcome measure.
EDLOS is a commonly used variable in studies addressing the problem of ED overcrowding. Our results showed that the presence of an emergency physician in the ED at night is associated with a significantly shorter EDLOS. At Tamworth Base Hospital there is generally no problem with access block, so the times are thought, therefore, to accurately reflect the time taken for ED treatment.
There was a large difference in the ordering of pathology tests between the two groups. Although similar numbers of patients underwent testing, the median number of tests per patient was five in Group B and only three in Group A. This finding is in agreement with previous studies investigating the seniority of staff and pathology tests ordered10,11. It is likely that this outcome reflects the emergency physicians training and better clinical judgement in the ordering of diagnostic tests. This result is also evident in the reduced cost of tests shown for the emergency physician group. It was not within the scope of this study to investigate whether or not further investigations by GP or inpatient teams were requested at a later date.
There were no call-backs or phone consultations when the emergency physician was in attendance, which has implications for the cost of patient care. Not surprisingly, it appears that the emergency physicians are more self-reliant and assured in their decision making than the RMOs, CMOs or locums.
Unscheduled re-presentations were included in the study as a marker of adverse health outcome. There were a considerable number of both scheduled and unscheduled re-presentations in both groups, but no statistically significant difference was found. There is evidence from other previous studies that a substantial proportion of return ED visits are the result of quality of care issues such as deficient medical management, poor patient education and insufficient arranged follow up12,13. Although this is a commonly used variable, its importance in this rural-based study may be questionable. In Tamworth and surrounding rural areas where GP services are limited, patients being discharged from the ED are often advised to return if their condition deteriorates, hence adding to the unscheduled re-presentation numbers. Further, in both 2001 and 2002 the time of year over which the comparison was made coincided with the annual Tamworth Country Music Festival. As a result, re-presentations for suture removal and dressing changes were more common than usual because of the transient increase in the town's population. Perhaps, for future reference, a more reliable outcome measure than representation would be a telephone interview a few days after discharge to gauge patient satisfaction. Clearly, this was not possible in this retrospective study and so no more accurate measure of quality of care was applied.
The lower number of pathology tests, consultations and admissions in Group A implies a cost saving. There are, of course, many other factors to be considered when evaluating cost, including staff time, dressings, minor treatments, pharmacy, and the differing pay rates of different doctors and other staff. A complete cost analysis is beyond the scope of this study, however.
The shifts studied involved only two emergency physicians in one rural base hospital so the results may not be generalisable to all emergency physicians or all departments. The emergency physicians had more years of experience than the other doctors in the study and may have been more familiar with hospital protocol and the availability of community services. Further, the results represent an emergency physician to total doctor ratio of 1:2, which would not be common in larger hospital ED where a greater proportion of junior doctors would be expected.
Conclusion
This retrospective case record review was opportunistic, as occasions when it is possible to compare ED outcomes with and without an emergency physician in attendance do not arise frequently, especially in rural hospitals. While it is acknowledged that the study reported in this article includes only small sample sizes, and that there were other limitations, as discussed above, it is strongly indicative that the presence of more senior, experienced staff in a rural ED at night is associated with a reduction in EDLOS, admissions, pathology tests per patient, and telephone consultations. For further confirmation of these findings it is recommended that a larger multi-centre trial be undertaken.
This study did not take into account the comparative cost of care with and without an emergency physician in attendance, although some of the findings are certainly suggestive of a cost saving. It is obvious that there is cost differential between employing a registrar or staff specialist compared to a more junior doctor; however, without detailed analysis of all the costs it is difficult to know if the additional expense would be balanced by the resultant cost saving. It is recommended that, should a larger study be possible in the future, financial cost as well as quality of care should be included as outcome measures.
This article must be considered in the light of recent findings about the improvement in access block with the presence of an emergency physician in the rural ED8 and comments about the affect of access block on job satisfaction and career longevity of emergency physicians14. As mentioned earlier, Tamworth Base Hospital does not have a problem with access block and so this could not be used reliably as an outcome factor. However, the findings of this study seem to further substantiate the case for the presence of a staff specialist in the ED, within the limits of available staffing, on other grounds. In addition, rural emergency departments often have a relatively 'flat' administrative profile and a frontline presence has been observed to promote the perception of consultants as clinical leaders, role models and mentors for younger doctors14.
References
1. Richardson DB. Reducing patient time in the emergency department. Medical Journal of Australia 2003; 79: 516-517.
2. Cardin S, Afilalo M, Lang E et al. Intervention to decrease emergency department crowding: does it have an effect on return visits and hospital readmissions. Annals of Emergency Medicine 2003; 41: 173-185.
3. Cobelas C, Cooper C, Ell M, Hawthorne G, Kennedy M, Leach D. Quality management and the emergency services enhancement program. Journal of Quality Clinical Practice 2001; 21: 80-85.
4. Partovi SN, Nelson BK, Bryan ED, Walsh MJ. Faculty triage shortens emergency department length of stay. Academic Emergency Medicine 2001; 8: 990-5.
5. Gaskell DJ, Crosby DL, Fenn N, Lewis PA, Roberts CJ, Roberts SM. Improving the primary management of emergency surgical admissions: a controlled trial. Annals of the Royal College of Surgeons England 1995; 77(Suppl): 239-241.
6. Wanklyn P, Hosker H, Pearson S, Belfield P. Slowing the rate of acute medical admissions. Journal of the Royal College of Physicians, 1997; 31: 173-176.
7. Cochrane RA, Edwards AT, Crosby DL et al. Senior surgeons and radiologists should assess emergency patients on presentation: a prospective randomised controlled trial. Journal of the Royal College of Surgeons 1998; 43: 324-327.
8. O'Connor AE, Lockney AL, Sloan PM, McGrail MR. Does the presence of an emergency physician improve access based quality indicators in a rural emergency department? Emergency Medicine 2004; 16: 55-58.
9. NSW Health. How triage works - the five triage categories. Online (2005). Available: http://www.health.nsw.gov.au/hospitalinfo/categs.html (Accessed April 2005).
10. Knott JC, Meyer AD. Impact of blood testing on patient disposition from the emergency department. Emergency Medicine 2003; 15: 121-125.
11. Dale J, Lang H, Roberts JA, Green J, Glucksman E. Cost effectiveness of treating primary care patients in accident and emergency: a comparison between general practitioners, senior house officers, and registrars. BMJ 1996; 312: 1340-1344.
12. Hu SC. Analysis of patient revisits to the emergency department. American Journal of Emergency Medicine 1992; 10: 366-370.
13. Keith KD, Bocka JJ, Kobernick MS, Krome RL, Ross MA. Emergency department revisits. Annals of Emergency Medicine 1989; 18: 964-968.
14. Green D. How long do emergency physicians' careers last? - The Tom Hamilton Lecture 2001. Emergency Medicine 2002; 14: 1-7.




