Australia is the sixth largest nation in the world, with a total area of more than 7 million km2, and a very low population density of just three people/km21. This makes Australia one of the least densely populated countries on earth. Some parts of Australia are even less densely populated. The Northern Territory, for example, has been recorded to hold 0.2 people/km21. Much of Australia (45%) is desert, and this is the main reason why most of the population is concentrated on or around coastal areas1.
Australians have generally enjoyed good dental health. The overall toll of poor oral health has reduced sharply during the 20th century with the introduction of fluoridated water and better understanding of dental disease. But the health gains have not been equally shared across all socioeconomic groups2. It has been acknowledged by Australia's National Oral Health Plan that low income earners are at a greater risk of dental disease compared to more affluent Australians3.
Aboriginal and Torres Strait Islander people experience significantly higher levels of dental disease compared to all other groups4. Rural residents are less likely to follow a prevention-oriented pattern of dental attendance5. It has also been found that concession card holders are less likely to visit a dentist on a regular basis and have a higher rate of dental disease4. Poor dental health has been found to be more prevalent among those without private health insurance3.
Ryan and Whelan have noted an increase in the disadvantaged population in outer urban areas of major capital cities. These areas are often characterised by low-cost housing and poor provision of services such as public transport6. There is evidence that mobility rates decrease as area socioeconomic disadvantage rises6.
Nationally, access to oral health care is available through several clinical pathways. The majority (about 85%) of dental care is provided in a private practice pathway. When seeing a dentist privately, a patient is responsible for meeting the cost of service provided. In some cases the cost of treatment in this pathway is partially paid for by private health insurance, when available. Prevalence of privately insured persons varies from year to year, but at the present time about 45% of the population is covered7. Market forces set the costs of care in this pathway; there is no government interference in the market, although there is some effect of insurance-driven schemes on the fee-for-service model within some practices.
Low income earners are able to obtain subsidised dental care through a large network of public dental clinics across Australia8. In this pathway the cost associated with provision of dental care is taxpayer subsidised by between 25% and 100% of the benchmark Department of Veteran's Affairs fee, depending on patient income9. The level of subsidy varies between Australian states and territories. In some cases levels of subsidy can differ between population groups9. The federal fee schedule has been reported to be between 20% and 40% less than a similar mix of care in the private pathway10.
In addition to the above pathways, Aboriginal and Torres Strait Islander people are able to access oral health care through a network of Aboriginal medical services clinics. Generally, services provided at these clinics are free of charge to the patient11.
Caries and periodontitis have been identified as the two most common diseases that result in chronic damage to oral health. If not identified early, these two diseases can have a cumulative cost to individuals and taxpayers. Easy and timely access to preventive dental care could help to identify problems early, thereby reducing the severity and cost of treatment12. Many Australians understand the importance of seeing a dentist regularly but not all are able do so. Up to 33% of the Australian population are likely to have untreated dental decay5, while people with inadequate dentition (fewer than 21 teeth) account for up to 34% of Australian adults5. Historically, demand for subsidised dental care has outstripped the ability of the public system to provide care, resulting in waiting lists, with wait times of in some cases 24 months10.
The aim of this study was to gauge the potential for reducing national dental waiting lists through geographical advantage, which could arise from subcontracting the delivery of subsidised dental care out to the existing network of private dental clinics across Australia.
Waiting list data
All waiting list data (number of people waiting to receive non-emergency dental care) for each state and territory were collected from websites or confirmed through direct communication with various jurisdictional bodies. The Northern Territory declined to participate. The data were collected for a single time point (mid-2012). This time point was chosen specifically because of its proximity in time to the available Census 2011 data.
Eligible population
Previous research found a close correlation between the 'unemployed' and 'not in the labour force' Census 2011 data and the distribution of eligible (for subsidised dental care) population, as provided by the Department of Human Services13. Eligibility for subsidised dental care was found to be about 75% of the total 'unemployed' or 'not in the labour force' sample obtained from the Australian Bureau of Statistics. Eligibility criteria do differ slightly between states.
This retrospective study collected the 'unemployed' and 'not in the labour force' Census 2011 data from the ABS website (Statistical Area Level 2) to represent the eligible population (n=4 746 422) for subsidised dental care across Australia.
Government and private practice locations
Physical address (and the longitude and latitude) for each dental practice in Australia (collated from a number of open sources) as at August 2012 was obtained from previously published research and formed the basis of practice locations8.
Geographic analysis
The Statistical Area 2 (SA2) is a unit of statistical geography that contains one or more Statistical Areas 1 (SA1s). In urban settings SA2s mostly follow officially gazetted suburb dimensions. In rural areas SA2s can outline a functional zone with socioeconomic links. Geography is also a consideration in SA2 design. When combined, SA2s cover the whole of the continent without gaps or overlaps14.
Quantum Geographic Information System v2.8.1 (QGIS; http://www.qgis.org) was used to map and analyse the distribution of the eligible population and waiting list patients across Australia by SA2, and to correlate this with the locations of government and private dental clinics.
Ethics approval
This retrospective study analysed statistical data and previously published literature. No individual-level data were used and no identification of patients was possible with the grouped data provided. Thus ethics approval was not required.
There are 373 259 people on the national waiting list. The total numbers of patients currently waitlisted for public dental care in the Australian Capital Territory, New South Wales, Queensland, South Australia, Tasmania, Victoria and Western Australia were obtained from state dental health services websites or through written requests for data to the relevant department (Tables 1, 2). The Northern Territory did not report its data and offers of participation were declined. Notwithstanding this, it is estimated that the number of people on the Northern Territory public dental waiting list would be very small compared with other states and territories.
There are 4.75 million people in Australia eligible for subsidised dental care. The eligible population comprises those residing within metropolitan areas (n=2.84 million) and those residing outside metropolitan areas (n=1.90 million). In this study, a metropolitan area was defined as being within a 50 km radius of the general post office of one of the capital cities. The centroid was calculated for each of the SA2s, and the numbers of eligible people within a 5 km radius of a government clinic, and within a 5 km radius of a government or private clinic in a metropolitan area, were calculated (Table 1). A similar calculation was performed for the eligible population residing outside metropolitan areas (Table 2). For this second group an additional range to 50 km was recorded. Essentially if a centroid fell within the predetermined distance then the population of that SA2 would be counted as 'residing within' that distance. The calculations were cumulative (ie eligible population residing within a 50 km radius also included those residing within a 5 km radius).
Seventy two percent (weighted average) of the eligible population and about 142 000 of those on the waiting list are residing in metropolitan areas and are located within a 5 km range of a government dental clinic. When both government and private clinics are considered, 97% of the eligible population, and 191 000 of those on the waiting list residing in metropolitan areas, are found to be within 5 km of a dental clinic, representing a 25% improvement in geographical accessibility (Table 1).
In contrast, only 38% (weighted average) of the eligible population, and 66 000 of those on the waiting list residing outside metropolitan areas, are located within 5 km of a government dental clinic. When availability of private dental clinics is taken into account, 64% of the eligible population, and 112 000 of those on the waiting list, are within 5 km of a dental clinic, representing a potential 59% improvement in accessibility (Table 2).
The Northern Territory had the lowest percentage of population eligible for subsidised care, at 15% (Table 3), and had the lowest accessibility, with only 19% of the eligible city residents residing within 5 km and only 4% of the eligible rural residents located within 50 km of a government dental clinic. The Northern Territory figures are in stark contrast with the findings for New South Wales where 82% of the eligible metropolitan population are residing within 5 km of a government dental clinic. Country residents in New South Wales have also enjoyed better access to subsidised dental care, compared to people in the Northern Territory (and all other states), with almost all (97%) residing within 50 km of a government dental clinic. Twenty one percent of the total New South Wales population are eligible for subsidised dental care (Table 3). This figure is comparable with those of other states and territories.
The results show that 96% (weighted average) coverage of the eligible population, and 168 000 people that are on the waiting list, can be achieved for most states and territories when the service area radius of both government and private dental clinics located outside metropolitan areas is increased to 50 km (Fig1).
Table 1: Distribution within metropolitan areas of the Australian population eligible for subsidised dental care
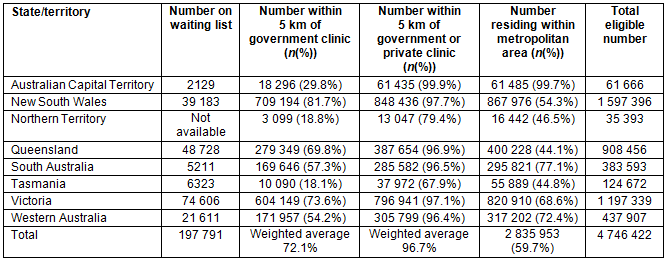
Table 2: Distribution outside metropolitan areas of the Australian population eligible for subsidised dental care
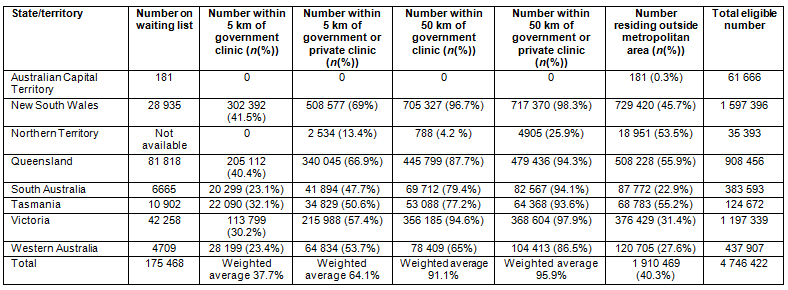
Table 3: Australian state and territory population and dental subsidy eligibility data
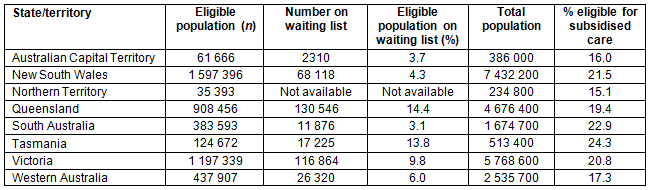
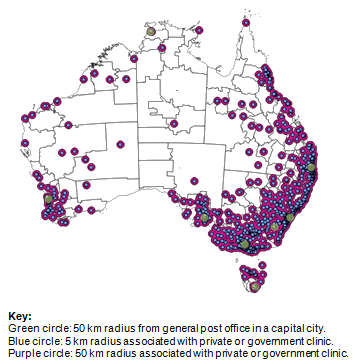
Figure 1: Geographic coverage: 50 km radius from government and private dental clinics in Australia.
Discussion
Good dental health is fundamental to a person's overall health, wellbeing and quality of life. Thus, timely access to primary oral healthcare services is critical in reducing the burden of dental disease on individuals and communities. Preventive dental care reduces the incidence of disease, facilitates early detection of problems and reduces the need for extensive restorative or emergency treatments at a later stage15.
The present study examined a time-point distribution of the eligible (for subsidised dental care) population and those on the waiting lists across Australia, and calculated expected improvement in geographical accessibility to basic dental care and the potential impact on the national waiting list, should private dental clinics be considered for a more permanent role as a safety net for those eligible for subsidised dental care. The potential improvement in geographical access (and thus the capacity of the public dental care system) can be enjoyed by a significant percentage of those on the national dental waiting list, and is therefore likely to have a positive effect on the average waiting time for routine dental care.
Interpretation of results
Distance has often been identified as one of the main barriers to obtaining health-related services16. However, it should be remembered that the distance a person is willing able to travel to obtain a health-related service may differ depending on the setting.
Distance needs to be considered in the context of everyday travel activities for a particular community. For example, 5 km of travel for a city resident with a low income using several modes of public transport can be considered a significant distance. The same distance in a country setting may not be seen as excessive, perhaps because town centres are generally smaller, with the majority of services often available close to the town centre. Use of public transport is more likely to involve a single mode of transport. When thought of in these terms, it is easier to see why prioritisation of trips to see a dentist for routine care differs with place of residence.
This reasoning formed the basis for nominating a 5 km travel distance to attend a dental clinic for city residents, and a 5 km (to allow for comparison) and 50 km range for those residing outside a metropolitan area.
The present study's model found that people on the waiting lists in all Australian states and territories could benefit from the reduction in travel distance, should they have the option of choosing to obtain subsidised dental care through either a government or private dental clinic. The highest increase in the availability and/or spatial accessibility of dental care (up by 59%) was noted for those residing outside metropolitan areas. This is a significant finding considering that rural and remote residents are consistently at a disadvantage compared to their metropolitan counterparts when it comes to accessing health-related services5.
Impact of distance on dental health
A person's place of residence, and more precisely travel distance to dental services, has been found to have a significant impact on the rate of hospitalisation for potentially preventable dental conditions. The rate of hospitalisation was shown to increase markedly with the increase in distance to dental services12.
Key statistics and issues
The number of people eligible for subsidised dental care (4.7 million) represents 20% of the total population of Australia (24 million). Those on the waiting list (Table 3) represent 10% of the total population eligible for subsidised dental care or 1.6% of the total population of Australia. An annual report published by the Dental Health Services of Western Australia states that, in 2012-2013, 18% of the eligible population actually received subsidised dental care17. Although the figures for other states and territories are unknown they are expected to be similar. Although this represents an underutilisation of care by the eligible population, the wait times to see a dentist for non-urgent dental care can be up to 24 months17. It is of concern to consider a scenario where all (or even increased proportions) of all those persons eligible for public care would demand and utilise subsidised care. With such long existing waiting lists, it is clear that public services and resources alone would not cope with increased demand for service.
When this is considered in the context of the current economic climate, namely the end of the mining boom, rising rate of unemployment and an ageing population, future increase in demand for subsidised dental care is a real possibility. Thus a more permanent arrangement utilising existing networks of private dental clinics may need to be considered, especially for those residing in rural and remote areas of Australia.
National Partnership Agreement
In 2012 the Commonwealth Government committed A$1.3 billion over several years to state and territory governments to support additional dental services for adults under the National Partnership Agreement (NPA). The measure is aimed at reducing long wait times to see a public dentist by providing eligible public dental patients with an authority to seek limited treatment from a private dentist, thus also improving access to dental care services, especially for rural residents14.
The current NPA for public dental patients ended in March 2015 and a cut-down 12-month extension was put in place. The second NPA was originally scheduled to start on 1 July 2014, but the federal budget proposed its deferral until 2015-201614.
Although early reports suggest that the NPA has had some success in reducing the states' dental waiting lists and has improved access to primary oral healthcare services, the initiative is deemed too new to determine with any degree of certainty whether the effect will be long lasting, cost-effective or sustainable18.
Economic considerations
Rolling out taxpayer-subsidised government dental clinics and supporting infrastructure in regional areas is expensive, requires extensive consultation, may not be viable, and may not reach many eligible people due to the relatively low population density of most regional centres in Australia. The solution needs to be effective and sustainable, and preferably benefit other layers of communities.
Locations of private dental clinics have been shown to be driven by market forces and the economy8. In a lot of cases private dental services cannot be sustained in many rural and remote areas, in part due to lack of dentists, high costs and low population density19.
The dental labour force in Australia is likely to continue to grow. Currently around 500 new dentists graduate from Australian universities every year20. This is a 100% increase on 2005 numbers. The new graduates are expected to have an impact of the numbers of practising dentists across the country, which is projected to increase by about 50% to around 15 000 by the 202020. The number of dentists per 100 000 population is also expected to rise to around 28% in the next 4-5 years20.
The increased number of dentists in Australia is already having an impact on the ability of new graduates to secure employment21, while a significant number of those with jobs consider themselves to be underemployed21. This situation is likely to result in downward pressure on remuneration within the sector.
It seems that an ongoing arrangement with the private sector in rural and remote areas could be the answer to the current and expected future growth in demand for subsidised dental care. In line with the opportunities afforded by the NPA, small-scale elements of this type of arrangement currently operate in some locations, and an expansion of this strategy may need to be considered. If appropriate safeguards are implemented, it might be possible for regional private patients, public patients and taxpayers to benefit from such an arrangement. A long-term agreement to provide a predetermined set of dental services to public patients may provide the extra financial incentive needed for private clinics to remain open (or for new clinics to open) in rural and remote centres. This approach may improve primary health services availability for the general population, offer a much-needed safety net for the geographically disadvantaged low income earners, and provide a welcome reprieve for the taxpayer with respect to capital expenditure and the cost of subsidising more expensive emergency dental care.
Dental health plays an integral part in the overall health of an individual and by extension in communities. Prevention and early detection of dental problems can minimise the need for complex and often expensive restorative work, and therefore reduce demand on the public healthcare system.
The present research found that utilisation of the existing network of private dental clinics across Australia to deliver subsidised dental care could dramatically reduce the national dental waiting list, increase geographic reach and possibly make good oral health a more realistic goal to achieve for the economically disadvantaged members of Australian communities.
Previous experience with the Chronic Disease Dental Scheme shows that writing an 'open cheque' in terms of the types of services that can be provided to treat public patients in a private setting can be very expensive17 and may not necessarily yield the desired results. A framework with appropriate safeguards in place that would allow for subsidised dental services delivery at private clinics has the potential to reduce waiting lists, improve access for greater eligible population and increase service availability in rural and remote areas for entire communities where existing socioeconomic dynamics do not otherwise foster private practice set-up. Improvement in access to primary dental care could help promote preventive treatment by simplifying the process to obtaining such care and making it more affordable.
References
1. World Population Review. Australia population 2016. (Internet) 2015. Available: http://worldpopulationreview.com/countries/australia-population (Accessed 18 October 2015).
2. Turrell G, Stanley L, de Looper M, Oldenburg B. Health Inequalities in Australia: morbidity, health behaviours, risk factors and health service use. (Internet) 2006. Available: http://www.aihw.gov.au/WorkArea/DownloadAsset.aspx?id=6442459734 (Accessed 18 October 2015).
3. Australian Dental Association. Socioeconomic status and oral health. (Internet) 2006. Available: http://www.ada.org.au/app_cmslib/media/lib/0702/m44818_v1_socioeconomic%20status%20and%20oral%20healthsep_06.pdf (Accessed 18 October 2015).
4. McAuliffe A, Nanda-Paul S, Dooland M. Inequities in oral health. National oral health plan. (Internet) 2004. Available: http://oralhealthplan.com.au/inequities-oral-health (Accessed 17 October 2015).
5. Australian Research Centre for Population Oral Health. Geographic variation in oral health and use of dental services in the Australian population 2004-06. (Internet) 2009. Available: http://www.aihw.gov.au/WorkArea/DownloadAsset.aspx?id=6442455420 (Accessed 10 October 2015).
6. Ryan C, Whelan S. Locational disadvantage, socio-economic status and mobility behaviour - evidence from Australia. (Internet) 2006. Available: https://www.melbourneinstitute.com/downloads/hilda/Bibliography/Conference_Papers/Whelan_ACE10.pdf (Accessed 20 October 2015).
7. Kruger E, Tennant M, George R. Application of geographic information systems to the analysis of private dental practices distributed in Western Australia. Rural and Remote Health (Internet) 2011 11: 1736. Available: www.rrh.org.au (Accessed 10 October 2015).
8. Tennant M, Kruger E. A national audit of Australian dental practice distribution: do all Australians get a fair deal? International Dental Journal 2013; 63: 177-182. https://doi.org/10.1111/idj.12027
9. Australian Dental Association. Inquiry into adult dental services in Australia. (Internet) 2013. Available: http://www.ada.org.au/App_CmsLib/Media/Lib/1304/M578038_v1_635018044353624420.pdf (Accessed 20 February 2014).
10. Dyson K, Kruger E, Tennant M. Networked remote area dental services: a viable, sustainable approach to oral health care in challenging environments. Australian Journal of Rural Health 2012; 20(6): 334-338. https://doi.org/10.1111/j.1440-1584.2012.01318.x
11. Chrisopoulos S, Beckwith K, Harford JE. Oral health and dental care in Australia: key facts and figures 2011. (Internet) 2011. Available: http://www.aihw.gov.au/publication-detail/?id=10737420710 (Accessed 18 October 2015).
12. Dudko Y, Kruger E, Tennant M. Geographic distribution of point-in-time access to subsidised dental services in Western Australia. Australian Journal of Primary Health (in press).
13. Kruger E, Tennant M. Socioeconomic disadvantages and oral-health-related hospital admissions: a 10-year analysis. British Dental Journal 2016; 29 July. https://doi.org/10.1038/bdjopen.2016.4
14. Metropolitan Health Service. Annual report 2012-13. (Internet) 2013. Available: http://ww2.health.wa.gov.au/~/media/Files/Corporate/Reports%20and%20publications/Annual%20reports/annual_reports_2013_MHS.ashx (Accessed 12 September 2015).
15. Rural Dental Action Group. Dental Health Survey 2006. (Internet) 2006. Available: http://www.ncoss.org.au/bookshelf/health/submissions/RDAG%20summary%202006.pdf (Accessed 2 October 2015).
16. Dental Health Services. Annual report 2014. (Internet) 2014. Available: http://www.dental.wa.gov.au/about/DHS%20Annual%20Report%20June%202014.pdf (Accessed 30 October 2015).
17. Dudko Y, Kruger E, Tennant M. National dental waitlists: what would it take to reset to zero? Australian Health Review 2016; 40(3): 277-281. https://doi.org/10.1071/AH15025
18. Willie-Stephens J, Kruger E, Tennant M. Public and private dental services in NSW: a geographic information system analysis of access to care for 7 million Australians. NSW Public Health Bulletin 2014; 24(4): 164-170.
19. Dudko Y, Kruger E, Tennant M. Is mix of care influenced by the provider environment? A comparison of four care pathways in oral health. Australian Health Review 2015; 39: 51-55. https://doi.org/10.1071/AH14064
20. Australian Research Centre for Population Oral Health. Dentist labour force projections, 2005-2020. (Internet) 2008. Available: https://www.adelaide.edu.au/arcpoh/downloads/publications/reports/research/2001-2008/report-42.pdf (Accessed 22 October 2016).
21. Preiss B. Many dentists, but not enough holes. (Internet) 2013. Available: http://www.smh.com.au/national/tertiary-education/many-dentists-but-not-enough-holes-20130111-2clas.html (Accessed 22 October 2016).


